Abstract
Purpose
To evaluate the ovarian reserve after laparoscopic cystectomy with suturing in patients with endometriomas.
Methods
A total of 80 women with unilateral or bilateral endometriomas underwent laparoscopic cystectomy using sutures for hemostasis after the excision of ovarian cysts. Serum levels of antimullerian hormone (AMH) and FSH were measured at the day 3 of menstrual cycles preoperatively, 6 and 12 months postoperatively.
Results
In the bilateral endometrioma group, serum AMH level decreased significantly from the baseline (4.68 ± 2.87 ng/ml) to 6 months (3.05 ± 1.99 ng/ml) and 12 months (2.26 ± 1.88 ng/ml) postoperatively, whereas the FSH level increased significantly from baseline to 12 months postoperatively (P < 0.05). Those patients with unilateral endometriomas also had lower levels of AMH in 6 and 12 months after operation. When compared between unilateral and bilateral endometrioma group, the rate of AMH decline 6 and 12 months and the rate of FSH increase 12 months postoperatively reached statistical significance (P < 0.05).
Conclusions
The changes of the AMH and FSH values suggest that the ovarian reserve is obviously reduced in spite of suturing technology used as a method of hemostasis after stripping ovarian endometriomas, especially in those with bilateral cysts. The protective effect of the ovarian suturing for ovarian reserve may be marginal.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Endometriosis is a common disease in which the endometrial glands and stroma are found outside the uterine cavity, and endometrioma is defined as the presence of an ovarian cyst with ectopic endometriotic tissues. Laparoscopic ovarian cystectomy is currently the most valid approach in treatment of endometriomas [1, 2]. However, there are concerns about the ovarian reserve damage during surgery including the removal of healthy ovarian tissue adjacent to the cyst capsule and the thermal damage of ovarian follicles by use of bipolar coagulation for hemostasis purposes [3]. Some investigators propose that the ovarian reserve was less reduced in sutured ovaries than in those electrocoagulated, they suggest suturing technology can be a better choice after stripping ovarian endometriomas [4, 5].
To investigate the extent of ovarian reserve impairment, the antimullerian hormone (AMH) was recommended as the most reliable marker, and its production was reported to be stable throughout the menstrual cycle [6]. To the best of our knowledge, few studies have assessed the impairment on ovarian reserve induced by laparoscopic excision using serum AMH levels. The aim of this prospective study was to evaluate the impact of laparoscopic cystectomy with ovarian suturing for endometrioma on ovarian reserve as measured by serum AMH levels.
Materials and methods
Patients
Between January 2012 and December 2013, 80 patients aged between 21 and 35 years with ovarian endometriomas requiring surgical removal were enrolled in the study. The diagnoses of unilateral and bilateral cystectomy (at least 4 cm) were observed for two menstrual cycles by ultrasound on day 3 of each cycle. The treatment protocol was approved by the Ethics Committee of Jinhua Municipal Central Hospital, and informed consent was obtained from all patients. The exclusion criteria were as follows: patients with polycystic ovarian syndrome according to the Rotterdam criteria, previous ovarian surgery, premature ovarian failure, ovarian malignant diseases, intake of hormonal medications within 3 months before enrollment, and any other endocrine disorders such as hyperprolactinemia, congenital adrenal hyperplasia or Cushing’s syndrome.
Laparoscopic cystectomy techniques
The laparoscopic cystectomy operations were performed under general anesthesia by the same team of experienced surgeons. After adhesiolysis and mobilization of the ovary, we identified the cleavage plane between the cyst capsule and the normal ovarian tissue. Then, two grasping forceps were used to gently strip the cyst wall from the ovary. Meticulous reconstruction and hemostasis were performed by using 3-0 polyglactin without bipolar forceps electrocoagulation. All endometrioma specimens obtained from operation were submitted for pathology examination.
Hormone measurements
Venous blood samples were drawn from the patients at day 3 of menstrual cycles preoperatively, 6 and 12 months postoperatively. Serum AMH level was analyzed with an enzyme-linked immunosorbent assay (ELISA) [Diagnostic Systems Laboratories (DSL), USA]. The intra-assay and inter-assay coefficients of variation for AMH was 9.4 and 7.2 %, respectively, with a detection limit of 0.006 ng/ml. Serum FSH level was measured using an Immulite 2000 immunoassay system (Diagnostic Products, Los Angeles, CA), with a detection limit of 0.1 mIU/ml.
Statistics
Statistical analysis was performed using SPSS version 13.0. Paired sample t test was used to compare the differences in AMH and FSH levels before and after the operation within the same group. Independent t test was used to compare the AMH and FSH levels between unilateral and bilateral endometriomas groups. Data were presented as mean ± SD and P < 0.05 was considered statistically significant.
Results
Initially, 80 women were included in this study. The mean age of our cohort was 29.1 years (rage 21–35 years). Eight women got pregnant and four lost to follow-up. Thus, 68 women formed the final study group, of whom 36 had unilateral and 32 had bilateral endometriomas.
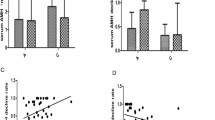
The median level of baseline serum AMH was 5.02 ± 3.05 ng/ml in unilateral endometrioma group, which thereafter decreased to 4.43 ± 2.13 and 4.07 ± 2.06 ng/ml at 6 and 12 month postoperatively. However, the trend of decrease in AMH level was not statistically significant. While in the bilateral endometrioma group, the serum AMH level significant decreased in 6 and 12 postoperative month as compared to baseline serum AMH level (P < 0.05 and P < 0.01) (Table 1). The level of baseline serum FSH was 5.36 ± 1.81 mIU/ml, it remained approximately unchanged after 6 and 12 months postoperatively (P > 0.05) in unilateral endometrioma group. In the bilateral endometrioma group, the serum FSH level slightly decreased in the 6th postoperative month (P > 0.05), then significantly decreased in the 12th postoperative month (8.26 ± 1.88 mIU/ml, P < 0.05) compared to baseline samples (Table 2).
There was no difference in preoperative serum AMH and FSH levels between the unilateral and bilateral endometrioma group. Postoperatively, the serum AMH level in the bilateral endometrioma group was significantly lower than in the unilateral endometrioma group during 6 months (3.05 ± 1.99 vs 4.43 ± 2.13 ng/ml, P < 0.05) and 12 months (2.26 ± 1.88 vs 4.07 ± 2.06 ng/ml, P < 0.05) postoperatively. On the other hand, the serum FSH level in the bilateral endometrioma group was significantly higher than in the unilateral endometrioma group during the 12th postoperative month (8.26 ± 1.88 vs 5.49 ± 2.06 mIU/ml, P < 0.05), there was no significant difference in serum FSH levels between two groups during the 6th postoperative month.
Discussion
Laparoscopic cystectomy is considered the optimal treatment for endometriomas, because it allows a more complete removal of the lesion and is associated with lower incidence of recurrence compared with other methods. Nonetheless, it is still under debate whether the ovarian tissue is damaged during surgery. We performed the stripping technique by the same experienced laparoscopists with high cautiousness and used suture instead of bipolar electrocoagulation for hemostasis. The aim of the study was to observe whether the ovarian reserve could be maintained similar to the preoperative level.
AMH, a member of the transforming growth factor-β family, is secreted by granulose cells in preantral and early antral follicles [7]. It was first reported in 1981 by Donohoe [8], because the serum AMH level is considered an indication for the size of the growing follicle pool, the utility of AMH measurement as an ideal estimator of ovarian function has recently developed. Basal FSH level is the most widely used marker of ovarian reserve. With combined use of AMH and FSH evaluation, we prospectively investigated the ovarian reserve of 80 patients after the excision of endometriomas cysts.
Chang et al. [9] believed that a surgery-related ovarian impairment really exists, but it partially recovered up to 3 months postoperatively. As a result, some investigators suggest delaying the follow-up intervals to observe whether the decreased AMH levels could be fully recovered. In our study, the serum AMH level continuously decreased after 6 and 12 months postoperatively as compared to baseline samples in the unilateral endometrioma group, though this reduction was not statistically significant. On the other hand, this difference reached statistical difference during the similar time frame (P < 0.05 and P < 0.01) in the bilateral endometrioma group. Although there were no data about serum AMH level 3 months after surgery, our data showed that the decrease of the serum AMH level is not temporary but sustained over 6–12 months. The results indicate that laparoscopic cystectomy can lead to a irreversible damage to ovarian reserve especially in bilaterality group, which was also supported by the increase trend of FSH in the bilateral endometrioma group 12 months postoperatively (P < 0.05) in our study. The findings of the current data are in line with the study by Raffi and Ferrero [10, 11]. Hwu et al. [12] also demonstrated that the serum AMH level in endometrioma patients with previous cystectomy was significantly lower than those without previous cystectomy. In our study, the difference between the postoperative and preoperative groups did not reach statistical significance in patients operated for a unilateral endometriomas, which could be explained by the normal contralateral ovary compensating for the ovarian function [13] and was not the case in bilateral endometrioma group as evident from the results of our study (Table 2).
Two studies that reported ovarian reserve was not affected by laparoscopic cystectomy [14, 15]. However, we found both articles had the common characteristic about short-term follow-up intervals (1 month postoperatively), limited number of patients, and relatively small sample of bilateral endometrioma patients. As a matter of fact, Alper et al. [15] showed that the serum AMH level deceased 1 month postoperatively. Unfortunately, the difference did not reach statistical significance. In his study, a total of 16 patients were included, of which only one had bilateral endometriomas. Therefore, their conclusions need to be further investigated empirically. Recent study [16] showed that, even when performed by experienced laparoscopists with every effort to be atraumatic, the laparoscopic cystectomy reduced the ovarian reserve. The causes of the decrease serum AMH level postoperatively might as follows: sutures elevate intraovarian pressure with ischemic regions produce additional damage of healthy tissue, although the thermal destruction to ovarian stroma and vascularization induced by bipolar electrocoagulation is more extensive. The presence of ovarian tissue adjacent to the lesion has been documented in many pathologic specimens indicating the inevitable removal of healthy tissue during laparoscopic stripping technique [14, 17]. A difficult striping procedure due to severe adhesion and multiple endometrioma cysts aggravates ovarian impairment. The inflammation-mediated injury following operation may cause ovarian damage resulting in decreased ovarian reserve. Thus, several techniques had been proposed for preserving ovarian reserve during surgery such as the combined cystectomy plus ablation of the remaining 10–20 % close to ovarian hilus [18], a three-step approach [19], injection of vasopressin around the cyst wall [20], and the ultrasound-guided puncture with methotrexate [21], or alcohol [22]. Further clinical trials are mandatory to evaluate the effect of these suggestions.
Current data suggest a progressive decline in ovarian reserve following cystectomy surgery in spite of suturing technology used as a method of hemostasis. In patients with a unilateral endometrioma, the impact of surgery on future fertility may be minimal, while excision of bilateral endometrioma can be great. The negative impact of this procedure on ovarian reserve should be fully considered before operation.
References
Dan H, Limin F (2013) Laparoscopic ovarian cystectomy versus fenestration/coagulation or laser vaporization for the treatment of endometriomas: a meta-analysis of randomized controlled trials. Gynecol Obstet Invest 76(2):75–82
Hart R, Hickey M, Maouris P, Buckett W, Garry R (2005) Excisional surgery versus ablative surgery for ovarian endometriomata: a Cochrane Review. Hum Reprod 20:3000–3007
Busacca M, Vignali M (2008) Endometrioma excision and ovarian reserve: a dangerous relation. J Minim Invasive Gynecool 16:142–148
Fedele L, Bianchi S, Zanconato G, Bergamini V, Berlanda N (2004) Bipolar electrocoagulation versus suture of solitary ovary after laparoscopic excision of ovarian endometriomas. J Am Assoc Gynecol Laparoscop 11:344–347
Li CZ, Liu B, Wen ZQ, Sun Q (2009) The impact of electrocoagulation on ovarian reserve after laparoscopic excision of ovarian cysts: a prospective clinical study of 191 patients. Fertil Steril 92:1428–1435
Seifer DB, Maclaughlin DT (2007) Mullerian inhibiting substance is an ovarian growth factor of emerging clinical significance. Fertil Steril 88:539–546
Weenen C, Laven JS, Von Bergh AR, Cranfield M, Groome NP, Visser JA, Kramer P, Fauser BC, Themmen AP (2004) Anti-Mullerian hormone expression pattern in the human ovary: potential implications for initial and cyclic follicle recruitment. Mol Hum Reprod 10:77–83
Hutson J, Ikawa H, Donahoe PK (1981) The ontogeny of Mullerian inhibiting substance in the gonads of the chicken. J Pediatr Surg 16:822–827
Chang HJ, Han H, Lee JR, Jee BC, Lee BI, Suh CS, Kim SH (2010) Impact of laparoscopic cystectomy on ovarian reserve: serial changes of serum anti-Mullerian hormone levels. Fertil Steril 94:343–349
Raffi F, Metwally M, Amer S (2012) The impact of excision of ovarian endometrioma on ovarian reserve: a systematic review and meta-analysis. J Clin Endocrinol Metab 97(9):3146–3154
Ferrero S, Venturini PL, Gillott DJ, Remorgida V, Leone Roberti Maggiore U (2012) Hemostasis by bipolar coagulation versus suture after surgical stripping of bilateral ovarian endometriomas: a randomized controlled trial. J Min Inv Gynecol 19:722–730
Hwu YM, Wu FS, Li SH, Sun FJ, Lin MH, Lee RK (2011) The impact of endometrioma and laparoscopic cystectomy on serum anti-Müllerian hormone levels. Reprod Biol Endocrinol 9:80
Urman B, Alper E, Yakin K, Oktem O, Aksoy S, Alatas C, Mercan R, Ata B (2013) Removal of unilateral endometriomas is associated with immediate and sustained reduction in ovarian reserve. Reprod Biomed Online 27:212–216
Ercan CM, Sakinci M, Duru NK, Alanbay I, Karasahin KE, Baser I (2010) Antimullerian hormone levels after laparoscopic endometrioma stripping surgery. Gynecol Endocrinol 26:468–472
Alper E, Oktem O, Palaoglu E, Peker K, Yakin K, Urman B (2009) The impact of laparoscopic ovarian cystectomy on ovarian reserve as assessed by antral follicle count and serum AMH levels. Fertil Steril 92:S59
Biacchiardi CP, Piane LD, Camanni M, Deltetto F, Delpiano EM, Marchino GL, Gennarelli G, Revelli A (2011) Laparoscopic stripping of endometriomas negatively affects ovarian follicular reserve even if performed by experienced surgeons. Reprod Biomed Online 23(6):740–746
Alborzi S, Foroughinia L, Kumar PV, Asadi N, Alborzi S (2009) A comparison of histopathologic findings of ovarian tissue inadvertently excised with endometrioma and other kinds of benign ovarian cyst in patients undergoing laparoscopy versus laparotomy. Fertil Steril 92:2004–2007
Donnez J, Lousse JC, Jadoul P, Donnez O, Squifflet J (2010) Laparoscopic management of endometriomas using a combined technique of excisional (cystectomy) and ablative surgery. Fertil Steril 94:28–32
Tsolakidis D, Pados G, Vavilis D, Athanatos D, Tsalikis T, Giannakou A, Tarlatzis BC (2010) The impact on ovarian reserve after laparoscopic ovarian cystectomy versus three-stage management inpatients with endometriomas: a prospective randomized study. Fertil Steril 94:71–77
Saeki A, Matsumoto T, Ikuma K, Tanase Y, Inaba F, Oku H, Kuno A (2010) The vasopressin injection technique for laparoscopic excision of ovarian endometrioma: a technique to reduce the use of coagulation. J Minim Invasive Gynecol 17:176–179
Agostini A, De Lapparent T, Collette E, Capelle M, Cravello L, Blanc B (2007) In situ methotrexate injection for treatment of recurrent endometriotic cysts. Eur J Obstet Gynecol Reprod Biol 130:129–131
Hsieh CL, Shiau CS, Lo LM, Hsieh TT, Chang MY (2009) Effectiveness of ultrasound-guided aspiration and sclerotherapy with 95 % ethanol for treatment of recurrent ovarian endometriomas. Fertil Steril 91:2709–2713
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Shao, MJ., Hu, M., He, YQ. et al. AMH trend after laparoscopic cystectomy and ovarian suturing in patients with endometriomas. Arch Gynecol Obstet 293, 1049–1052 (2016). https://doi.org/10.1007/s00404-015-3926-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-015-3926-4