Abstract
Introduction
Bicruciate retaining (BCR) total knee arthroplasty (TKA) was designed to simulate natural knee kinematics and improve proprioception by retaining both the ACL and PCL. While the prospect of the design appears favorable to patients, previous designs have demonstrated modest survivorship rates compared to traditional designs. This study aims to report the early functional outcomes and implant survivorship of a novel BCR design.
Materials and methods
A multi-center, retrospective study was conducted identifying BCR TKA patients from 2016 to 2017. Patient demographics, quality outcomes, and post-operative complications were collected. A Kaplan–Meier analysis was used to evaluate revision-free survival.
Results
One-hundred thirty-three patients with a mean follow-up time of 2.35 ± 0.25 years (range: 2.00–2.87 years) were identified. Patients receiving BCR TKA were, on average, 61.46 ± 9.27 years-old, obese (BMI = 31.80 ± 6.01 kg/m2), predominantly white (71.4%), and female (69.9%). The device was most often implanted using standard instruments (85.7%) compared to computer-assisted navigation (13.5%). Average length-of-stay was 1.77 ± 0.97 days. Six patients had a reoperation; three (2.5%) full revisions occurred for: infection (n = 1), arthrofibrosis (n = 1), and ACL rupture (n = 1); one (0.8%) tibial revision occurred for: arthrofibrosis; two (1.5%) liner exchanges occurred for: infection (n = 1) and arthrofibrosis (n = 1). Kaplan–Meier survivorship analysis of cumulative failure at 2-year showed a survival rate of 96.2% (95% confidence interval, 91.2–98.4%) for all-cause reoperation, 97.3% (91.6–99.1%) for aseptic revision, and 100% for mechanical failure.
Conclusion
Survivorship was 96.2% for all-cause reoperation, 97.3% for aseptic revision, and 100% for mechanical implant failure at 2-years. This novel BCR TKA demonstrated no implant-related complications and excellent survivorship outcomes over 2 years with comparable revision rates to those previously reported in the literature.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
While total knee arthroplasty (TKA) remains a highly successful procedure with excellent patient reported outcomes, up to 20% of patients may remain unsatisfied with their knee replacement [1, 2]. In an attempt to address patient dissatisfaction, more nuanced implant designs such as the bicruciate retaining (BCR) TKA were developed to simulate more natural knee kinematics and improve proprioception by retaining both the anterior (ACL) and posterior cruciate ligaments (PCL) [3,4,5,6,7,8,9]. Prior studies have shown that BCR TKA may be preferable over traditional TKA systems [10, 11]. A proportion of patients who receive a TKA may be indicated for a BCR prosthesis, provided that they have an intact ACL and PCL [12].
While BCR TKA may provide greater satisfaction with perceived advantages over other knee systems, some studies have demonstrated modest survivorship rates in previous BCR designs that were inferior to traditional TKA designs [13,14,15,16,17]. Some of the limitations of previous BCR designs that may have contributed to implant failure in earlier studies include limited flexion as a result of constrained polyethylene and non-anatomic implant designs, poor tibial implant strength and fixation features, polyethylene wear, and technical difficulties in surgical technique [18, 19].
A novel BCR design (Journey II XR, Smith & Nephew) was developed in an attempt to address these concerns through kinematic features and a wide range of sizes. Currently, no prior studies that have evaluated the performance or durability of this novel design. Therefore, the aim of this study is to report the short-term functional outcomes and implant survivorship of a novel BCR design.
Materials and methods
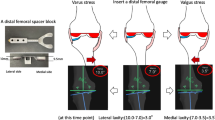
This is a multi-institution, multi-surgeon, retrospective study that analyzed patients at ten institutions who underwent complex primary TKA between 2016 and 2017 using a novel BCR TKA implant (Smith&Nephew Journey II XR, Memphis, TN, USA) (Fig. 1). This implant combines a kinematic design of the femoral cruciate retaining (CR) TKA with the BCR tibial implant to allow for retention of both the ACL and PCL. To our knowledge, it is currently the only TKA BCR design available on the market. The BCR system features a tibial baseplate with an asymmetric notch that is positioned more anteriorly on its medial side to accept the ACL footprint and provide greater coverage while not limiting the capacity for rotation. The tibial component also features a non-symetrical tibial tray with two independently designed medial and lateral inserts. Furthermore, the tibia has a continuous keel and optimized anterior bridge to provide greater fixation and implant strength. In addition, the femoral component utilizes a kinematic design that can be matched with various tibial baseplate sizes. Appropriate institutional review board (IRB) approval was obtained at every institution participating in this study. All procedures were performed by fellowship-trained, high-volume arthroplasty surgeons at their respective institutions. All cases that qualified for inclusion by each surgeon were reported in the present study. Each participating surgeon was past the associated learning curve for all cases included in the present study. In general, a standard medial parapatellar arthrotomy was used when feasible, however, surgical approach and decision-making were left to the surgeon’s discretion. Patients were included in this study if they received this specific BCR TKA system and had a minimum of 2-year follow-up data to evaluate short to mid-term outcomes. Exclusion criteria included any patients under the age of 18, those with severe deformity or flexion contraction as determined by preoperative radiographs as well as those who received other knee implant systems or did not have a minimum of 2-year follow-up data available for review.
Patient demographics and surgical data were reviewed from each institution's respective electronic medical record system and manually recorded onto a centralized electronic medical database (OpenClinica, Waltham, MA). Baseline patient demographics (i.e. age, gender, body mass index (BMI), race, smoking status, prior arthroscopies) and surgical data (i.e. operative laterality, indication for index procedure, surgical approach, and use of intraoperative technology) were collected from the date of each patient’s index surgery (Table 1). Patient outcomes were collected at routine follow-up appointments with data being reported at the date of the last clinical follow-up. Assessed outcomes included operative time, lengths of stay, intraoperative complications, discharge disposition, 90-day readmissions, 90-day emergency department (ED) visits, reoperations, and revision surgery (Table 2). In addition, patient reported outcome measures (PROMs) such as the Forgotten Joint Score (FJS-12) and the Knee Injury and Osteoarthritis Outcome Score (KOOS) at 2 year follow-up were included (Table 3). Reoperation was defined as any case in which the indexed knee was taken back to the operating room (OR) and reopened for a post-operative complication. Revision surgery included cases in which the femoral, tibial, or both components of the implant were explanted and/or exchanged. All-cause reoperation included any case taken back to the OR and had surgery performed on the index knee [e.g. irrigation, debridement and modular component exchange with implant retention (DAIR), extensor mechanism repair, patellar removal, etc.], whereas aseptic reoperation excluded cases performed for infectious causes. Mechanical implant failure was defined as any case in which revision surgery was performed for failure of an implant component (e.g. aseptic loosening, migration, implant fracture).
Survivorship was analyzed and presented graphically using the Kaplan–Meier method. Outcomes and survivorship data were calculated using the time of the latest follow-up. Patients who died with the implant in situ and/or were lost to follow-up were considered censored at the date of death and last follow-up, respectively. All data was analyzed with descriptive statistics using SPSS v.25.0 (IBM Corp., Armonk, NY, USA).
Results
Overall, 445 patients were enrolled in this retrospective study. Patients who had inadequate 2-year follow-up (306 patients) or received a different implant (6 patients) were excluded. Ultimately, there were 133 knees identified to be eligible for this study, having undergone primary TKA throughout the study period using the evaluated BCR system. On average, there were 2.35 ± 0.25 years (range 2.00–2.87 years) follow-up time. The cohort was predominately female (69.9%) with a mean age of 61.46 ± 9.27 years, obese (BMI 31.80 ± 6.01 kg/m2), white (71.4%), and were mostly non-smokers (58.6%). Over a third of the patients in this study (38.3%) had a history of a prior knee arthroscopy procedure. Of the 133 cases, the majority were indicated for osteoarthritis of the knee (97.0%), underwent the medial parapatellar approach (90.1%), and utilized standard instrumentation (85.7%). Navigation or robotic assistance was utilized in 13.5% of cases (Table 1).
This series demonstrated a mean operative time of 99.98 ± 24.28 min. All cases underwent full femur, tibia, and liner implantation. Patients on average had a 1.77 ± 0.97 days length of stay and were most commonly discharged to home with services (74.4%). The only intraoperative complication was an iatrogenic medial tibial plateau fracture, which resulted in ORIF and subsequent removal of fixation hardware. Furthermore, the cohort demonstrated 2 (1.5%) 90-day ED visits, one for prepatellar bursitis and one for VTE. Eleven (8.3%) patients were readmitted within 90-days. Of these, seven patients (5.3%) experienced knee stiffness, two patients (1.5%) experienced worsening pain, one patient (0.8%) experienced wound drainage, and one patient (0.8%) had cardiac complications (Table 2).
Overall, six out of 133 cases (4.5%) required a reoperation procedure. Two were (2.5%) full revisions due to infection (n = 1) and arthrofibrosis (n = 1), while one was a tibial revision to a conventional CR TKA secondary to ACL tear (n = 1). There was also one (0.8%) tibial revision for arthrofibrosis, and two (1.5%) tibial polyethylene liner exchanges for infection (n = 1) and arthrofibrosis (n = 1). Kaplan–Meier survivorship analysis of cumulative failure at 2-year showed a survival rate for all-cause reoperation of 96.2% (95% confidence interval, 91.2%-98.4%). Mean time to all-cause reoperation was 647 (range 539–796) days (Fig. 2). Mean time to all-cause reoperation was 697 (range 637–796) days (Fig. 3). Kaplan–Meier survivorship analysis of cumulative failure at 2-years showed a survival rate for aseptic implant revision of 97.3% (91.6–99.1%). Kaplan–Meier survivorship analysis of cumulative failure at 2-year showed a survival rate for mechanical implant failure of 100% (Fig. 4).
Patients in our cohort demonstrated a mean FJS-12 score of 55.52 ± 29.25 at 2 years postoperatively. In addition, KOOS collected at 2 years postoperatively demonstrated a mean symptoms score of 49.17 ± 20.05; stiffness score of 43.74 ± 16.90; pain score of 49.95 ± 15.67; function of daily living score of 56.37 ± 16.64; function of sports score of 24.60 ± 22.35; and quality of life score of 27.86 ± 18.53. A complete overview of PROMs data can be found in Table 3.
Discussion
The bicruciate-retaining TKA design was first developed over half a century ago in an attempt to preserve native knee kinematics and improve proprioception through the retention of both the ACL and PCL [3,4,5,6,7,8,9, 20]. Proponents of the BCR design have claimed it could possibly narrow the gap of patients still unsatisfied with their TKA. However, the promise of this improved implant design has been challenged with concerns regarding surgical exposure, implant fixation and durability, and ACL evaluation [18, 19, 21]. The aim of this current study is to evaluate and report the short-term functional outcomes and implant survivorship of a novel BCR design.
In this study, the Kaplan–Meier survivorship analysis for implant revision in patients who received the novel BCR implant showed a 97.3% survival rate for aseptic implant revision, and 100% survival rate for mechanical implant failure at 2 years. This reported survivorship of this BCR implant appears to be a substantial improvement over its predecessors. While early first-generation BCR TKAs were reported to have survival rates of 84–89% at a mean follow-up of 3.5 years, newer BCR implants have undergone significant refinement and improvement since then [22]. Mid-term follow-up of a more recent design had a reported survivorship for implant revision of 95% at 10 years, and 82% survivorship at 22-year follow-up. [22]. While the implant reported in this study certainly requires longer term follow-up studies to evaluate its durability, these early survivorship results appear promising.
Pritchett et al. described the functional outcomes and survivorship of the largest and most long-term series of 489 BCR implants [13]. The authors reported the Kaplan–Meier survivorship, at a mean follow-up of 23 years, to be 89% with revision for any reason as the endpoint. Of their 21 revisions, patients were most commonly revised for polyethylene wear, aseptic loosening, and infection [13]. Although in our series, there was one case of revision for infection, the remaining three revisions occurred for either arthrofibrosis or ligamentous tear. Post-operative ACL tear and bone block fracture are inherent drawbacks of the BCR design, however, given that the incidence was found to be 0.8% in our cohort, this complication is of minimal concern. Our series contained no incidence of aseptic loosening, polyethylene wear or implant fracture, resulting in 100% survivorship for mechanical implant failure at two years.
Post-operative stiffness has also been an established complication following BCR TKA. A review of the literature by Zhou et al. found that no studies included were able to demonstrate full restoration of native knee kinematics during exercises such as squatting and downhill walking following BCR TKA [23]. Boese et al. [24] reported that BCR TKA with a second-generation implant provided higher mean range of motion in flexion postoperatively compared to earlier models, though overall post-operative results between studies were conflicting. In a comparison study of 100 patients who underwent BCR TKA against 100 patients who underwent PS TKA, Lavoie et al. reported that post-operative stiffness occurs more frequently and with greater magnitude following BCR TKA compared to PS TKA. This, however, was only found to hold true in patients when preoperative flexion was less than 130 degrees [25]. In the current study, 7 patients (5.3%) had a 90-day readmission for knee stiffness, with two patients (1.5%) ultimately requiring revision for arthrofibrosis [25]. Nevertheless, these rates are on par with those noted in the literature, with arthrofibrosis developing in approximately 3–4% of patients undergoing TKA [26, 27].
In our analysis, the BCR implant demonstrated a mean FJS-12 score of 55.52 ± 29.25 at 2 year follow-up. Similarly, in a recently published randomized control trial, Troelsen et al. [28] evaluated PROMs in patients undergoing TKA with BCR versus CR implants. Their analysis demonstrated mean FJS-12 scores of 62 ± 28 at 2 year follow-up in their BCR cohort. Their results showed no significant differences in mean improvement of FJS-12 scores preoperatively to 2 years postoperatively between the two cohorts, though their study was underpowered to detect clinically relevant differences. Nevertheless, our findings coincide with recently published data and argue in favor of improved patient satisfaction.
Overall, this novel BCR design appears to achieve excellent results by addressing many of the concerns of older designs. A major concern with bicruciate-retaining implants was with the tibial component fixation due to the limited contact surface available for stability, resulting in liner wear and loosening [20]. Neither of these complications were observed in our cohort, resulting in excellent short-term survivorship.
Limitations
The current study is not without its limitations. The most important limitation to this study is that of the 445 patients followed in this study, only 30% had adequate follow-up to report. This impacts the ability of the survivorship analysis to accurately predict the performance of the implant over time. Another limitation is the retrospective study design and reliance on manual chart review, which inherently predisposes our results to selection bias and possibly data collection error. In addition, prior literature has documented the need for appropriate preoperative imaging and examination to help manage the difficult nature of malalignment and deformity associated with BCR TKA. Sabatini et al. [29] reported on inclusion criteria for second-generation BCR designs involving coronal deformity less than 15 degrees and flexion contracture that results in no more than a 10 degree loss in range of motion. Further analyses using this novel design may benefit from examining outcomes of patients who meet these criteria. Furthermore, we may have inadequately controlled for confounding variables due to the lack of a control group, although this is an inherent bias of retrospective studies. While clinical outcomes of prior BCR implant studies were used for comparison, the lack of consistency in patient selection and ACL evaluation makes it difficult to perform any direct comparisons. Additionally, the BCR implant chosen is limited in its ability to correct major deformity and severe flexion contraction or hyperextension. Consequently, our analysis could not account for patients who underwent TKA with severe deformity or large tibial bony defects. Finally, given the 2-year follow-up, long-term performance of this BCR knee design is lacking. Yet, our follow-up time still provides the longest-term follow-up of this implant in the literature.
Conclusion
This study demonstrates this novel bicruciate-retaining TKA system to have excellent early survivorship, with very low rates for reoperation, implant revision, and no mechanical implant failure. While these short-term results appear promising, further long-term outcome studies are necessary ultimately determine this device’s durability and patient outcomes.
Availability of data and materials
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- BCR:
-
Bicruciate retaining
- CR:
-
Cruciate retaining
- TKA:
-
Total knee arthroplasty
- ACL:
-
Anterior cruciate ligament
- PCL:
-
Posterior cruciate ligament
- BMI:
-
Body mass index
- OR:
-
Operating room
- DAIR:
-
Debridement and modular component exchange with implant retention
- PROMs:
-
Patient reported outcome measures
- ED:
-
Emergency department
- FJS-12:
-
Forgotten Joint Score
- KOOS:
-
Knee Injury and Osteoarthritis Outcome Scores
References
NIH (2003) NIH Consensus Statement on total knee replacement. In: NIH consensus and state-of-the-science statements
Kahlenberg CA, Nwachukwu BU, McLawhorn AS et al (2018) Patient satisfaction after total knee replacement: a systematic review. HSS J Musculoskelet J Hosp Spec Surg 14:192–201. https://doi.org/10.1007/s11420-018-9614-8
Barrett TJ, Shi L, Parsley BS (2017) Bicruciate-retaining total knee arthroplasty, a promising technology, that’s not quite there. Ann Transl Med 5(Suppl 1):S17. https://doi.org/10.21037/atm.2017.03.77
Halewood C, Traynor A, Bellemans J et al (2015) Anteroposterior laxity after bicruciate-retaining total knee arthroplasty is closer to the native knee than ACL-resecting TKA: a biomechanical cadaver study. J Arthroplasty. https://doi.org/10.1016/j.arth.2015.06.021
Zumbrunn T, Varadarajan KM, Rubash HE et al (2015) Regaining native knee kinematics following joint arthroplasty: a novel biomimetic design with ACL and PCL preservation. J Arthroplasty. https://doi.org/10.1016/j.arth.2015.06.017
Wodowski AJ, Swigler CW, Liu H, Nord KM, Toy PC, Mihalko WM (2016) Proprioception and knee arthroplasty: a literature review. Orthop Clin N Am 47(2):301–309. https://doi.org/10.1016/j.ocl.2015.09.005
Cloutier JM (1983) Results of total knee arthroplasty with a non-constrained prosthesis. J Bone Jt Surg Ser A. https://doi.org/10.2106/00004623-198365070-00005
Komistek RD, Allain J, Anderson DT et al (2002) In vivo kinematics for subjects with and without an anterior cruciate ligament. Clin Orthop Related Res 404:315–325
Stiehl JB, Komistek RD, Cloutier JM, Dennis DA (2000) The cruciate ligaments in total knee arthroplasty: a kinematic analysis of 2 total knee arthroplasties. J Arthroplasty. https://doi.org/10.1054/arth.2000.4638
Pritchett JW (2011) Patients prefer a bicruciate-retaining or the medial pivot total knee prosthesis. J Arthroplasty. https://doi.org/10.1016/j.arth.2010.02.012
Pritchett JW (2004) Patient preferences in knee prostheses. J Bone Jt Surg Ser B. https://doi.org/10.1302/0301-620X.86B7.14991
De FD, Ries C, Foster M et al (2020) Indications for bi-cruciate retaining total knee replacement: an international survey of 346 knee surgeons. PLoS ONE. https://doi.org/10.1371/journal.pone.0234616
Pritchett JW (2015) Bicruciate-retaining total knee replacement provides satisfactory function and implant survivorship at 23 years. Clin Orthop Relat Res 473:2327–2333. https://doi.org/10.1007/s11999-015-4219-8
Sabouret P, Lavoie F, Cloutier J-M (2013) Total knee replacement with retention of both cruciate ligaments. Bone Jt J 95-B:917–922. https://doi.org/10.1302/0301-620X.95B7.30904
Pelt CE, Sandifer PA, Gililland JM et al (2019) Mean three-year survivorship of a new bicruciate-retaining total knee arthroplasty: are revisions still higher than expected? J Arthroplasty 34:1957–1962. https://doi.org/10.1016/j.arth.2019.04.030
Christensen JC, Brothers J, Stoddard GJ et al (2017) Higher frequency of reoperation with a new bicruciate-retaining total knee arthroplasty. Clin Orthop Relat Res 475:62–69. https://doi.org/10.1007/s11999-016-4812-5
Osmani FA, Thakkar SC, Collins K, Schwarzkopf R (2017) The utility of bicruciate-retaining total knee arthroplasty. Arthroplast Today 3:61–66. https://doi.org/10.1016/j.artd.2016.11.004
Lombardi AV, Mcclanahan AJ, Berend KR (2015) The bicruciate-retaining TKA: two is better than one. Semin Arthroplasty. https://doi.org/10.1053/j.sart.2015.08.004
Mont MA, John M, Johnson A (2012) Bicruciate retaining arthroplasty. Surg Technol Int 22:236–242
Cherian JJ, Kapadia BH, Banerjee S et al (2014) Bicruciate-retaining total knee arthroplasty: a review special focus section 199. J Knee Surg 27:199–206. https://doi.org/10.1055/s-0034-1374812
Trecci A (2016) Bicruciate retaining. Ann Transl Med 4(7):128. https://doi.org/10.21037/atm.2016.01.27
Cloutier JM, Sabouret P, Deghrar A (1999) Total knee arthroplasty with retention of both cruciate ligaments: a nine to eleven-year follow-up study. J Bone Jt Surg Ser A 81:697–702. https://doi.org/10.2106/00004623-199905000-00011
Zhou C, Peng Y, An S et al (2021) Does contemporary bicruciate retaining total knee arthroplasty restore the native knee kinematics? A descriptive literature review. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-021-04116-3
Boese CK, Ebohon S, Ries C, De Faoite D (2021) Bi-cruciate retaining total knee arthroplasty: a systematic literature review of clinical outcomes. Arch Orthop Trauma Surg 141:293–304. https://doi.org/10.1007/s00402-020-03622-0
Lavoie F, Al-Shakfa F, Moore JR et al (2018) Postoperative stiffening after bicruciate-retaining total knee arthroplasty. J Knee Surg 31:453–458. https://doi.org/10.1055/s-0037-1604145
Diduch DR, Scuderi GR, Scott WN et al (1997) The efficacy of arthroscopy following total knee replacement. Arthroscopy 13:166–171. https://doi.org/10.1016/S0749-8063(97)90150-X
Parvizi J (2006) Management of stiffness following total knee arthroplasty. J Bone Jt Surg 88:175. https://doi.org/10.2106/jbjs.f.00608
Troelsen A, Ingelsrud LH, Thomsen MG et al (2020) Are there differences in micromotion on radiostereometric analysis between bicruciate and cruciate-retaining designs in TKA? A randomized controlled trial. Clin Orthop Relat Res 478:2045–2053. https://doi.org/10.1097/CORR.0000000000001077
Sabatini L, Barberis L, Camazzola D et al (2021) Bicruciate-retaining total knee arthroplasty: What’s new? World J Orthop 12:732–742. https://doi.org/10.5312/wjo.v12.i10.732
Funding
No funding was provided for this study.
Author information
Authors and Affiliations
Contributions
VS, DY, TC, TB, and AT equally contributed to this work, which included data collection, analysis, and manuscript preparation. RS oversaw the conceptualization of the project and made final edits prior to submission.
Corresponding author
Ethics declarations
Conflict of interest
V.S, D.Y, T.C, T.B, and A.T have nothing to disclose. R.S is a paid consultant for Intellijoint and Smith&Nephew and holds stock options in Gauss Surgical and PSI.
Ethical approval
The present study was conducted upon receiving approval from the institutional review board (IRB).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
Consent to publish was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Singh, V., Yeroushalmi, D., Christensen, T.H. et al. Early outcomes of a novel bicruciate-retaining knee system: a 2-year minimum retrospective cohort study. Arch Orthop Trauma Surg 143, 503–509 (2023). https://doi.org/10.1007/s00402-022-04351-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04351-2