Abstract
Introduction
Impaired ankle dorsiflexion (ADF) is known to increase forefoot pressure, which is associated to various pathologies affecting the foot and ankle. M. gastrocnemius tightness (MGT) is its most common cause. Up to date we are missing a standardized examination procedure, norm values, and a valid decision pathway to diagnose impaired ADF and MGT. The aim of this study was to define norm values for ADF using a standardized examination procedure. These were used to define a decision pathway to diagnose impaired ADF and MGT.
Materials and methods
64 young, asymptomatic subjects were examined. Based on a standardized examination procedure, bilateral ADF, both with the knee extended and flexed, non-weight bearing and weight bearing, was assessed by three investigators. Inter-rater test reliability and norm values for ADF were calculated. Side differences were analyzed. ADF differences between the knee extended and flexed were calculated.
Results
The standardized examination procedure revealed high ICC values (0.876–0.915). ADF values with the knee extended for the left/right limb were 22.7° ± 5.9° [95 % CI 21.2°–24.3°]/23.4° ± 6.5° [95 % CI 21.7°–25.1°] non-weight bearing and 33.3° ± 5.5° [95 % CI 31.9°–34.7°]/33.6° ± 5.6° [95 % CI 32.1°–35.0°] weight bearing. Physiological side differences with the knee extended were <6° (95 % CI). Knee flexion resulted in an approximate ADF increase of 10°.
Conclusions
Based on an extensive systematic approach, physiological values for ADF were assessed in a large asymptomatic population. This allowed the definition of a decision pathway to diagnose impaired ADF and MGT. Patients presenting with pathologies associated with impaired ADF should be examined according to the herein presented examination protocol. This systematic approach provides a consistent definition of impaired ADF and MGT, which is the prerequisite to study the effectiveness of treatment strategies for MGT.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Impaired ankle dorsiflexion (ADF) is hypothesized to increase forefoot pressure [1–3]. This can lead to various problems of the foot and ankle, including metatarsalgia [4, 5], plantar fasciitis [6], Achilles tendinopathy [7], and plantar ulceration [8]. The most common cause for reduced ADF is a tightness of the M. gastrocnemius (MGT) [9, 10]. MGT has gained increased attention in the literature. Despite the rising number of studies reporting on treatment strategies [11], there is no consensus on how to diagnose MGT. Currently there is no standardized examination procedure and no consistent definition of physiological norm values [12–15]. However, this is the prerequisite to diagnose impaired ADF and MGT as well as initiate treatment.
MGT is characterized by impaired ADF with the knee extended. Knee flexion results in an increase of ADF. Although this principle forms the basis for any test addressing MGT, published examination procedures differ significantly. These vary in various aspects, including the force applied to the ankle [16–18], the measurement device [19], and the anatomical measurement landmarks used [12, 20, 21]. Obviously, every one of these parameters has a pronounced impact on the degree of ADF measured. Because of those variations, we are missing a consistent definition of physiological and pathological norm values. Currently, definitions for impaired ADF vary from less than 0° to less than 10° [14, 22–24].
To put it into a nutshell, we are missing a consistent diagnostic algorithm for MGT. Consequently, the indication for treatment is unclear. As an example we analyzed the indication for therapy of the 18 trials included in the most recent systematic review on the effectiveness of M. gastrocnemius recession. One-third of the studies did not mention the degree of ADF necessitating therapy. Only three papers gave details on the testing procedure [11, 15]. Therefore, the validity and comparability of outcome studies on gastrocnemius recession are limited. We strongly believe that the prerequisite for any study on the efficacy of gastrocnemius recession is to clearly define the indication. This necessitates a standardized examination procedure. Based on this, norm values must be defined.
The aim of this study was to apply a standardized examination procedure [12] to a large collective of young, asymptomatic individuals to identify norm values for ADF. Based on these, we intended to define a decision pathway to diagnose impaired ankle dorsiflexion and M. gastrocnemius tightness.
Materials and methods
Study population
64 healthy, asymptomatic individuals meeting the criteria presented in Table 1 were included. The local ethics committee approved the study (#007–14)
Testing procedure
The standardized testing procedure was defined in a previous study [12]. ADF was assessed bilaterally for each subject, non-weight bearing and weight bearing, both with the knee extended and flexed. Three investigators performed all measurements independently: senior consultant foot and ankle surgery (HP), 5th year resident orthopedic surgery (SFB), final year medical student (FS). The investigators were blinded to each other’s results. The order of examination was changed randomly in between the subjects. A standard goniometer (MDF Instruments USA, Inc. Malibu, CA, USA) with 2° increments and 20 cm length was used.
Measurement landmarks
Similar anatomical measurement landmarks were applied for both non-weight bearing and weight bearing examination:
Y-axis: Distal long axis of the fibular marked prior to testing (a line connecting the center of the lateral malleolus with the center of the fibula 10 cm proximally) [25, 26].
X-axis: Plantar aspect of the foot (non-weight bearing)/the floor (weight bearing).
Non-weight bearing
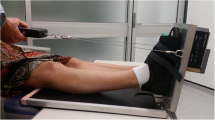
Two examiners conducted the test. The subject was placed in supine position. One investigator applied maximum force to the forefoot for maximum ADF with one hand, while assuring a subtalar neutral position with the other hand. The other examiner performed ADF measurements, both with the knee fully extended (Fig. 1A1) and 90° flexed (Fig. 1A2).
Illustration of the non-weight bearing and weight bearing testing procedure. A1 Non-weight bearing examination with the knee extended; A2 non-weight bearing examination with the knee flexed (approx. 90°, min 20°); B1 weight bearing examination with the knee extended; B2 weight bearing examination with the knee at least 20° flexed
Weight bearing
One examiner conducted the test. The subject performed a lunge stance in front of a wall. The foot to be measured was the rear foot. It was centered (2nd toe and heal) on a previously marked line perpendicular to the wall. The subject was allowed to hold onto the wall to stabilize their stance. In order to achieve maximum ADF the participant was asked to move the hip towards the wall until just before heel lift off. ADF measurements were performed both, with the knee fully extended (Fig. 1B1) and at least 20° flexed (Fig. 1B2) [12].
Data assessed
Standard demographics (gender, age, BMI) were recorded following informed consent. ADF measurements were conducted bilateral, with the knee extended and flexed, non-weight bearing and weight bearing. Three investigators conducted the measurements separately and the inter-rater reliability was assessed. ADF differences between the right and left side as well as the knee extended and flexed were calculated.
Outcome variables
The primary outcome parameter were the ADF measurements (norm values). Secondary outcome parameters were inter-rater test reliability, secondary values generated from the ADF measurements, i.e., side- and knee position differences, and the influence of the demographic parameters on the ADF norm values.
Statistics
Inter-rater test reliability was assessed using the interclass correlation coefficient (ICC; 1.1). ICC values can range from 0 to 1, with 1 being perfect agreement. Values greater than 0.7 are generally considered acceptable [27, 28]. The ICC was calculated for all possible combinations of investigators.
To obtain reliable ADF norm values, subjects demonstrating a disproportionate inter-rater variance were excluded from further analysis. Therefore, the maximum difference of ADF between the three investigators was calculated for each measurement. Based on these values we calculated the 95 % CI. Subjects were excluded, if any measurement exceeded the 95 % CI of the inter-rater variance.
In the following, standard descriptive statistics were calculated. Possible gender, side, or test (non-weight bearing/weight bearing) differences were assessed using the Students t test (independent/paired, where appropriate). A Pearson correlation coefficient was used to test the influence of age and BMI on ADF. The symmetry between the left and right ankle (knee extended) was calculated using the Bland–Altman levels of agreement analysis. ADF differences between the knee extended and flexed, for both non-weight bearing and weight bearing, were assessed by standard descriptive statistics and a MANOVA. p values less than 0.05 indicated statistical significance. Statistics were computed using SPSS Vs. 21 (IBM Company).
Results
64 healthy, asymptomatic subjects with a mean age of 28.3 ± 4.0 years (58 % female) were included. The mean BMI was 22.7 ± 3.0.
Inter-rater test reliability (ICC)
The overall ICC ranged from 0.876 to 0.915 for non-weight bearing and from 0.851 to 0.901 for weight bearing examination (Table 2). Calculating ICC values for all rater combinations separately (HP-SFB, HP-FS, SFB-FS) revealed higher ICC values for the more experienced raters with a mean ICC (±SD) of 0.903 ± 0.023 (HP-SFB). The mean ICC with the student was 0.862 ± 0.035 (FS-HP) and 0.867 ± 0.029 (FS-SFB). The complete analysis is presented in Supplement 1.
Norm values
As pointed out above, subjects demonstrating an inter-rater variance exceeding the 95 % CI interval were excluded from further analysis. This corresponded to an inter-rater difference of ≥10°, which was observed in 5 subjects. In order to assess the physiological ADF, the values of the remaining 59 subjects were calculated as the mean of all three investigators for each measurement.
The descriptive statistics for the mean ADF are presented in Table 3. No gender differences were found. No side differences were found but for non-weight bearing knee flexed measurements (p 0.002). The weight bearing examination resulted in a significantly higher ADF for all measurements compared to non-weight bearing. Age did not influence ADF. Higher BMI scores were only associated with significantly lower values for ADF when tested non-weight bearing. The corresponding Pearson correlation coefficients for the right leg were −0.389 (p 0.002) with the knee extended and −0.313 (p 0.016) with the knee flexed. For the left leg the correlation coefficients were −0.410 (p 0.001) with the knee extended and −0.304 (p 0.019) with the knee flexed.
Symmetry right and left ankle
The summary of the Bland–Altman level of agreement analysis is presented in Table 4. Figure 2 illustrates the Bland–Altman plots. Overall an average bias of 0.6°/0.3° for the non-weight bearing/weight bearing examination was present for the right limb. Considering the 95 % confidence interval revealed a physiological ADF side difference for the knee extended <6°.
Blande-Altman plot representing the asymmetry of dorsiflexion between the right and left ankle with the knee extended. Each subject is represented by a data point. The y-axis shows the difference between the right and left ankle. The mean ADF of the right and left ankle is plotted on the x-axis. Values above zero indicate greater ADF on the right side. The thin solid line represents the level of agreement between both ankles, i.e., mean difference between the right and left ankle. The dashed lines represents ±1SD, the thick solid line the lower and upper bounds of the 95 % confidence interval
Differences of ADF with the knee extended and flexed
The differences between the knee extended and flexed for non-weight bearing and weight bearing are presented in Table 5. Overall, a mean gain in ADF of approximately 10° was observed by flexing the knee. The MANOVA showed no significant influence of the testing condition (non-weight bearing/weight bearing). The model revealed a side and an interaction effect on ADF. Still, the mean difference varied around approximately 10° ADF.
Discussion
The key to diagnose impaired ADF and MGT is the application of a standardized examination protocol. Up to now, multiplicities of different testing procedures have been described. These differ in various aspects, all of which have a pronounced impact on the measured values of ADF. The most distinct aspects are the force applied to the ankle, the anatomical measurement landmarks and the measurement device. ADF can be assessed non-weight bearing [16, 29], weight bearing [17, 30] or instrumented [18, 31]. Measurement landmarks applied for the y-axis were the fibula [17, 32], the tibia [33, 34], or the Achilles tendon [35, 36]. The x-axis was either defined by the plantar surface of the foot [32, 37] or the fifth metatarsal bone [29, 38]. Finally, devices used to measure ADF were a mobile app [35], digital inclinometer [34, 35], measuring tape [39, 40], custom made devices [18, 31, 41], or a standard goniometer [16, 42, 43]. This hinders the definition of physiological and pathological norm values. Therefore, the authors strongly believe that the community should agree on one standardized examination procedure.
In a previous study, the authors laid the foundation for a standardized non-weight bearing and weight bearing examination procedure [12]. This protocol was applied herein. The advantages of this procedure have been discusses in detail [12]. In brief, the examination protocol is highly standardized and demonstrates a high inter-rater reliability. Moreover, reproducible landmarks are used, no special equipment is needed and it can be conducted in a timely manner. Therefore, it is highly applicable for the daily routine.
To put our results into perspective, we identified studies using comparable landmarks and performing non-weight bearing or weight bearing tests. Non-weight bearing measurements revealed significantly lower ADF values [14, 21, 42]. Kim et al. [21] examined individuals in supine position and reported mean ADF values of approximately 11° ± 3° with the knee extended and 17° ± 4° with the knee flexed. A single investigator applied the force and conducted the measurements. Slightly higher values (knee extended: 13° ± 8°; knee flexed: 22° ± 11°) were reported by DiGiovanni and colleagues [14]. They used an equinometer and applied a standardized torque of 10 Nm. Rabin et al. [42] conducted non-weight bearing measurements with the subject in prone position. They reported ADF values of 25° ± 5° with the knee flexed. Again one investigator conducted the measurements and applied the force. One must assume that the force applied varied between these studies. Applying the torque while measuring will hamper the force produced by the investigator. Further, greater force can be applied with the subject in prone position. The use of a custom made device, which applies a defined torque, standardizes the force, but is not available to most physicians. Overall, these examples highlight the sensitivity of non-weight bearing measurements for the force applied to the ankle. This does not only explain the diverging values between the different studies, but again emphasizes the necessity of a standardized examination procedure.
Our study, in line with previous [32, 42], showed significantly higher values of ADF for weight bearing compared to non-weight bearing examination. This is most likely due to the greater torque acting on the ankle. The few studies applying a comparable weight bearing examination reported similar values [17, 43]. Munteanu et al. [17] conducted measurements using a clear acrylic plate apparatus and similar landmarks. They reported mean ADF values of 36° ± 5° with the knee extended. Konor et al. [43] reported mean values of 43° ± 6° with the knee flexed. In contrast to the non-weight bearing procedure, weight bearing examination with similar landmarks produces comparable results throughout studies. Taken together, the weight bearing procedure seems to feature a higher reliability. Moreover, previous studies demonstrated significantly higher ICC values for weight bearing measurements [17, 30, 32, 42, 44]. Therefore, the weight bearing examination seems to outmatch the non-weight bearing.
A further strength of this study was the large number of subjects enrolled. Various previous studies assessed ADF in less than 30 healthy subjects [17, 20, 30, 35, 43]. Moreover, we applied an extensive systematic approach to define ADF norm values. Not only did we assess ADF bilaterally with the knee extended and flexed, but also investigated the symmetry between the right and left ankle. The authors are not aware of any study applying a similar systematic approach. Only one study has assessed the side symmetry using a different test [45]. Hoch et al. [45] investigated ADF side differences in healthy volunteers using the lung test (weight bearing, knee flexed, toe-to-wall distance). They reported a bias of 0.1 cm (±2.8 cm; 95 % CI) on the right limb. Similar small physiological differences with a mean bias of 0.3° (±5.3°; 95 % CI) were found in our study. Consequently, an unilateral ADF reduction on the symptomatic side of more than 6° has to be considered highly suspicious for impairment.
Several limitations should be discussed. First, adjacent joints movements (e.g., subtalar and midtarsal joints) can bias the ADF measurements. Therefore, care was taken to assure neutral position of the subtalar and talonavicular joints during testing, as recommended in the literature [46–49]. Second, the herein used goniometer had 2° increments, which could add to measurement inaccuracy. Although other devices might be more accurate, the goniometer has to be considered the clinical gold standard [28]. Moreover, with respect to the high ICC, and narrow confidence intervals observed, we believe this tool to be sufficiently accurate. A final practical limitation is the disposal of two investigators conducting the non-weight bearing examination. In the clinical routine, usually only one physician examines the patient. Conducting non-weight bearing examination by a single investigator might increase measurement inaccuracy, as adjacent joint movements cannot be controlled, maximum force application and simultaneous execution of the measurement are hindered.
As outlined above, we applied a highly reliable and standardized test to a large collective of asymptomatic subjects. Bilateral values for ADF were measured for both, the knee extended and flexed, non-weight bearing and weight bearing. Based on this extensive examination procedure, we aimed at defining a decision pathway to diagnose impaired ankle dorsiflexion and M. gastrocnemius tightness (Fig. 3). The presented pathway is only valid if the herein outlined examination procedure and landmarks are applied. Any patient presenting with unilateral pathologies associated with impaired ADF (for example, plantar ulceration [8], metatarsalgia [4, 5], plantar fasciitis [6], or Achilles tendinopathy [7]) should be examined according to the following three steps:
-
1.
Measurements: Bilateral ADF, both with the knee fully extended and flexed, should be measured. For the reasons discussed above, the authors recommend to use the weight bearing protocol. Non-weight bearing examination should only be conducted in case the weight bearing test cannot be performed.
-
2.
Impaired ADF (knee extended): Less than 10° on the symptomatic side has to be considered impaired. This is in line with the literature [14] and the herein observed minimum values. Notably, the physiological lower limit (95 % CI) of ADF was 30° weight bearing (20° non-weight bearing). Consequently, values between 10° and 30° weight bearing (10°–20° non-weight bearing) have to be considered restricted. In those cases, the side symmetry should be taken into account. Side differences of less than 6° were found physiological (95 % CI). Therefore, if more than 5° of side asymmetry are present, ADF should then be considered impaired. ADF greater 30° is not impaired.
-
3.
M. gastrocnemius tightness: Once impaired ADF is diagnosed, one must identify the cause. MGT is present, if knee flexion results in an increase of ADF of approximately 10°. If knee flexion does not result in an increase of ADF, MGT is not present. Therefore, further diagnostics have to be conducted to identify the underlying pathology.
Overall, the herein presented study, for the first time, provides a standardized and detailed examination protocol to identify impaired ADF and MGT. Future studies should apply this decision pathway to diagnose impaired ADF and MGT and initiate treatment. This systematic approach will allow comparison of studies on the effectiveness of treatment strategies for M. gastrocnemius tightness.
References
You J-Y, Lee H-M, Luo H-J, Leu C-C, Cheng P-G, Wu S-K (2009) Gastrocnemius tightness on joint angle and work of lower extremity during gait. Clin Biomech (Bristol, Avon) 24(9):744–750. doi:10.1016/j.clinbiomech.2009.07.002
Aronow MS, Diaz-Doran V, Sullivan RJ, Adams DJ (2006) The effect of triceps surae contracture force on plantar foot pressure distribution. Foot Ankle Int 27(1):43–52
Chimera NJ, Castro M, Davis I, Manal K (2012) The effect of isolated gastrocnemius contracture and gastrocnemius recession on lower extremity kinematics and kinetics during stance. Clin Biomech (Bristol, Avon) 27(9):917–923. doi:10.1016/j.clinbiomech.2012.06.010
Irving DB, Cook JL, Menz HB (2006) Factors associated with chronic plantar heel pain: a systematic review. J Sci Med Sport 9(1-2):11–22. doi:10.1016/j.jsams.2006.02.004 (discussion 23–14)
Crawford F, Thomson C (2003) Interventions for treating plantar heel pain. The Cochrane database of systematic reviews (3):CD000416. doi:10.1002/14651858.CD000416
Pascual Huerta J (2014) The effect of the gastrocnemius on the plantar fascia. Foot Ankle Clin 19(4):701–718. doi:10.1016/j.fcl.2014.08.011
Gurdezi S, Kohls-Gatzoulis J, Solan MC (2013) Results of proximal medial gastrocnemius release for Achilles tendinopathy. Foot Ankle Int 34(10):1364–1369. doi:10.1177/1071100713488763
Laborde JM (2009) Midfoot ulcers treated with gastrocnemius-soleus recession. Foot Ankle Int 30(9):842–846. doi:10.3113/FAI.2009.0842
Hill RS (1995) Ankle equinus. Prevalence and linkage to common foot pathology. J Am Podiatr Med Assoc 85(6):295–300
Patel A, DiGiovanni B (2011) Association between plantar fasciitis and isolated contracture of the gastrocnemius. Foot Ankle Int 32(1):5–8. doi:10.3113/FAI.2011.0005
Cychosz CC, Phisitkul P, Belatti DA, Glazebrook MA, DiGiovanni CW (2015) Gastrocnemius recession for foot and ankle conditions in adults: Evidence-based recommendations. Foot Ankle Surg 21(2):77–85. doi:10.1016/j.fas.2015.02.001
Baumbach SF, Brumann M, Binder J, Mutschler W, Regauer M, Polzer H (2014) The influence of knee position on ankle dorsiflexion: a biometric study. BMC Musculoskelet Disord 15(1):246. doi:10.1186/1471-2474-15-246
Charles J, Scutter SD, Buckley J (2010) Static ankle joint equinus: toward a standard definition and diagnosis. J Am Podiatr Med Assoc 100(3):195–203
DiGiovanni CW, Kuo R, Tejwani N, Price R, Hansen ST, Cziernecki J, Sangeorzan BJ (2002) Isolated gastrocnemius tightness. J Bone Joint Surg Am 84-A(6):962–970
Baumbach SF, Polzer H (2015) Letter to the editor on “Gastrocnemius recession for foot and ankle conditions in adults: Evidence-based recommendations”. Foot Ankle Surg. doi:10.1016/j.fas.2015.06.003
Bolívar YA, Munuera PV, Padillo JP (2013) Relationship between tightness of the posterior muscles of the lower limb and plantar fasciitis. Foot Ankle Int 34(1):42–48. doi:10.1177/1071100712459173
Munteanu SE, Strawhorn AB, Landorf KB, Bird AR, Murley GS (2009) A weight bearing technique for the measurement of ankle joint dorsiflexion with the knee extended is reliable. J Sci Med Sport 12(1):54–59. doi:10.1016/j.jsams.2007.06.009
Gatt A, Chockalingam N (2013) Validity and reliability of a new ankle dorsiflexion measurement device. Prosthet Orthot Int 37(4):289–297. doi:10.1177/0309364612465886
Gatt A, Chockalingam N (2011) Clinical assessment of ankle joint dorsiflexion: a review of measurement techniques. J Am Podiatr Med Assoc 101(1):59–69
Vohralik SL, Bowen AR, Burns J, Hiller CE, Nightingale EJ (2015) Reliability and validity of a smartphone app to measure joint range. Am J Phys Med Rehabil 94(4):325–330. doi:10.1097/PHM.0000000000000221
Kim PJ, Peace R, Mieras J, Thoms T, Freeman D, Page J (2011) Interrater and intrarater reliability in the measurement of ankle joint dorsiflexion is independent of examiner experience and technique used. J Am Podiatr Med Assoc 101(5):407–414
Phisitkul P, Rungprai C, Femino JE, Arunakul M, Amendola A (2014) Endoscopic Gastrocnemius Recession for the Treatment of Isolated Gastrocnemius Contracture: A Prospective Study on 320 Consecutive Patients. Foot Ankle Int. doi:10.1177/1071100714534215
Hamilton GA, Ford LA, Perez H, Rush SM (2005) Salvage of the neuropathic foot by using bone resection and tendon balancing: a retrospective review of 10 patients. J Foot Ankle Surg 44(1):37–43. doi:10.1053/j.jfas.2004.11.001
Duthon VB, Lübbeke A, Duc SR, Stern R, Assal M (2011) Noninsertional Achilles tendinopathy treated with gastrocnemius lengthening. Foot Ankle Int 32(4):375–379. doi:10.3113/FAI.2011.0375
Worrell TW, McCullough M, Pfeiffer A (1994) Effect of foot position on gastrocnemius/soleus stretching in subjects with normal flexibility. J Orthop Sports Phys Therapy 19(6):352–356. doi:10.2519/jospt.1994.19.6.352
Aström M, Arvidson T (1995) Alignment and joint motion in the normal foot. J Orthop Sports Phys Therapy 22(5):216–222. doi:10.2519/jospt.1995.22.5.216
Lahey MA, Downey RG, Saal FE (1983) Intraclass correlations: there is more than meets the eye. Psychol Bull 93(3):586–595
Martin RL, McPoil TG (2005) Reliability of ankle goniometric measurements: a literature review. J Am Podiatr Med Assoc 95(6):564–572
Krause DA, Cloud BA, Forster LA, Schrank JA, Hollman JH (2011) Measurement of ankle dorsiflexion: a comparison of active and passive techniques in multiple positions. J Sport Rehabil 20(3):333–344
Bennell KL, Talbot RC, Wajswelner H, Techovanich W, Kelly DH, Hall AJ (1998) Intra-rater and inter-rater reliability of a weight-bearing lunge measure of ankle dorsiflexion. Austr J Physiotherapy 44(3):175–180
Wilken J, Rao S, Estin M, Saltzman CL, Yack HJ (2011) A new device for assessing ankle dorsiflexion motion: reliability and validity. J Orthop Sports Phys Therapy 41(4):274–280. doi:10.2519/jospt.2011.3397
Baggett BD, Young G (1993) Ankle joint dorsiflexion. Establishment of a normal range. J Am Podiatr Med Assoc 83(5):251–254
Basnett CR, Hanish MJ, Wheeler TJ, Miriovsky DJ, Danielson EL, Barr JB, Grindstaff TL (2013) Ankle dorsiflexion range of motion influences dynamic balance in individuals with chronic ankle instability. Int J Sports Phys Therapy 8(2):121–128
Kang M-H, Lee D-K, Park K-H, Oh J-S (2015) Association of ankle kinematics and performance on the y-balance test with inclinometer measurements on the weight-bearing-lunge test. J Sport Rehabilit 24(1):62–67. doi:10.1123/jsr.2013-0117
Williams CM, Caserta AJ, Haines TP (2013) The TiltMeter app is a novel and accurate measurement tool for the weight bearing lunge test. J Sci Med Sport 16(5):392–395. doi:10.1016/j.jsams.2013.02.001
Burns J, Crosbie J (2005) Weight bearing ankle dorsiflexion range of motion in idiopathic pes cavus compared to normal and pes planus feet. Foot 15:91–94. doi:10.1016/j.foot.2005.03.003
Youdas JW, Krause DA, Egan KS, Therneau TM, Laskowski ER (2003) The effect of static stretching of the calf muscle-tendon unit on active ankle dorsiflexion range of motion. J Orthop Sports Phys Therapy 33(7):408–417. doi:10.2519/jospt.2003.33.7.408
Norkin CC, White DJ (2003) Measurement of joint motion: a guide to goniometry, 3rd edn. FA Davis, Philadelphia
Simondson D, Brock K, Cotton S (2012) Reliability and smallest real difference of the ankle lunge test post ankle fracture. Manual Therapy 17(1):34–38. doi:10.1016/j.math.2011.08.004
Hoch MC, Staton GS, Medina McKeon JM, Mattacola CG, Mckeon PO (2012) Dorsiflexion and dynamic postural control deficits are present in those with chronic ankle instability. J Sci Med Sport 15(6):574–579. doi:10.1016/j.jsams.2012.02.009
Purcell SB, Schuckman BE, Docherty CL, Schrader J, Poppy W (2009) Differences in ankle range of motion before and after exercise in 2 tape conditions. Am J Sports Med 37(2):383–389. doi:10.1177/0363546508325925
Rabin A, Kozol Z (2012) Weight bearing and Nonweight bearing Ankle Dorsiflexion Range of Motion: Are We Measuring the Same Thing? J Am Podiatr Med Assoc 12(5):406–411
Konor MM, Morton S, Eckerson JM, Grindstaff TL (2012) Reliability of three measures of ankle dorsiflexion range of motion. Int J Sports Phys Therapy 7(3):279–287
Menz HB, Tiedemann A, Kwan MM-S, Latt MD, Sherrington C, Lord SR (2003) Reliability of clinical tests of foot and ankle characteristics in older people. J Am Podiatr Med Assoc 93(5):380–387
Hoch MC, Mckeon PO (2011) Normative range of weight-bearing lunge test performance asymmetry in healthy adults. Manual Therapy 16(5):516–519. doi:10.1016/j.math.2011.02.012
Tiberio D (1987) Evaluation of functional ankle dorsiflexion using subtalar neutral position. A clinical report. Physical therapy 67(6):955–957
Tiberio D, Bohannon RW, Zito MA (1989) Effect of subtalar joint position on the measurement of maximum ankle dorsiflexic. Clin Biomech (Bristol, Avon) 4(3):189–191. doi:10.1016/0268-0033(89)90024-7
Bohannon RW, Tiberio D, Waters G (1991) Motion measured from forefoot and hindfoot landmarks during passive ankle dorsiflexion range of motion. J Orthop Sports Phys Therapy 13(1):20–22. doi:10.2519/jospt.1991.13.1.20
Johanson M, Baer J, Hovermale H, Phouthavong P (2008) Subtalar joint position during gastrocnemius stretching and ankle dorsiflexion range of motion. J Athlet Train 43(2):172–178. doi:10.4085/1062-6050-43.2.172
Acknowledgments
We would like to kindly thank Ms. Iveta Sklenarova for her help and support during the testing procedures.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The study has not received funding. The authors declare that they have no competing interests.
The paper has not been submitted to any other journal.
Rights and permissions
About this article
Cite this article
Baumbach, S.F., Braunstein, M., Seeliger, F. et al. Ankle dorsiflexion: what is normal? Development of a decision pathway for diagnosing impaired ankle dorsiflexion and M. gastrocnemius tightness. Arch Orthop Trauma Surg 136, 1203–1211 (2016). https://doi.org/10.1007/s00402-016-2513-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-016-2513-x