Abstract
Background
This study aimed to comprehensively analyze the relationship between serum potassium (K+) levels and the risk of de novo cardiac arrhythmias in left ventricular assist device (LVAD) recipients.
Methods
We performed a retrospective study using the INTERMACS registry. Data was collected on adult patients with available K+ measurements taken 1-month post-LVAD implantation. K+ levels were the main exposure of interest and were analyzed as a continuous and categorical variable (quartiles of baseline K+ distribution). The main outcome of interest was the occurrence of de novo arrhythmia events, either sustained (ventricular [VA] or supraventricular arrhythmia [SVA]) or not sustained (atrial fibrillation/flutter [AF]). All-cause mortality was evaluated as the secondary outcome. Multivariable adjusted time-dependent Cox regression models and natural splines were used to describe the relationship between the exposure and outcomes of interest.
Results
10,570 patients met our inclusion criteria. A significant and consistent relationship was observed between the lowest quartile of longitudinal K+ and the risk of arrhythmic events (HR 1.28, 95% CI 1.08, 1.53, p = 0.005) as well as in the highest K+ quartile (HR 1.24, 95% CI 1.02, 1.49, p = 0.027).
A similar relationship was confirmed in the stratified analysis of arrhythmia types for SVAs and AF. The data were reflected in a U shaped relationship. Similarly, the highest and lowest quartiles of longitudinal K+ were independently associated with a significant increase in the HR of death, which was reflected by a U shaped relationship.
Conclusions
Our study reveals a significant U shaped relationship between low and high K + levels and cardiac arrhythmias in LVAD patients, particularly SVAs and AF. Both high and low K + levels negatively impacted patient survival.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Left ventricular assist device (LVAD) implantation has become increasingly common in patients with end-stage heart failure due to the donor organ supply shortage and the improved survival associated with second- and third-generation mechanical circulatory support (MCS) devices [1]. LVADs are being used more frequently as a destination therapy, and the life expectancy of patients remaining on MCS devices is increasing [1].
Cardiac arrhythmias, both supraventricular arrhythmias (SVAs) and ventricular arrhythmias (VAs), are a frequent complication observed in LVAD recipients [2]. Recent estimates suggest an incidence rate of up to 4.7 events per patient-year, making arrhythmias the third most common complication in this population, after bleeding and infections [3]. Although systemic circulation is well supported in LVAD patients, these arrhythmias can lead to detrimental symptoms and potentially fatal outcomes. The impact of these arrhythmias on patient survival is debated [2]. However, recent reports indicate that they may independently contribute to increased patient mortality [4].
Various factors contribute to the development of arrhythmias and electrolyte disorders, with serum potassium (K+) imbalances identified as a significant predictor [5]. Alterations in K+ levels, such as hypokalemia, have been associated with poorer clinical outcomes [6] and increased risk of ventricular arrhythmias [7] and mortality [8] among heart failure patients.
To date, no studies have directly assessed the relationship between K+ imbalances and arrhythmias in LVAD recipients or their impact on patient survival. In addition, most previous research has focused on VAs. This study aimed to comprehensively analyze the relationship between K+ levels and the risk of cardiac arrhythmias in LVAD recipients. In addition, we aimed to evaluate the prognostic impact of K+ alterations on patient outcomes. Our findings may contribute to improving the current understanding of the pathophysiology of arrhythmias in LVAD patients and could potentially guide the development of preventive and therapeutic strategies to improve patient outcomes.
Materials and methods
Study population
The INTERMACS (Interagency Registry for Mechanically Assisted Circulatory Support) registry is a large prospective North American database that collects data on patients who undergo LVAD implantations [9]. A full description of the registry has been previously published [9]. After LVAD implantation, patients are monitored until death, explant, or heart transplantation.
We included adult patients (i.e., older than 17) who underwent permanent continuous flow (CF) LVAD implantation and had at least one K+ measurement during their follow-up. To ensure we only selected stable LVAD patients, we only collected data from 1-month post-LVAD implantations. Those with missing K+, serum creatinine (SCr), or blood pressure (BP) follow-up measurements were excluded from the analysis (Fig. 1).
The data, analytical methods, and study materials used are available via the Biological Specimen and Data Repository Information Coordinating Center [10]. The Institutional Review Board of the University of Verona approved our research protocol (n 21/2022). Written informed consent was obtained from all patients by the participating INTERMACS centers.
Data collection
Demographic, examination, laboratory, medication, and comorbid conditions data were collected. The estimated glomerular filtration rate (eGFR) was calculated from SCr using the race-free equation recommended by the National Kidney Foundation and the American Society of Nephrology Task Force [11]. Mean arterial pressure (MAP) was estimated using a formula in which diastolic BP is doubled and added to the systolic BP, with the sum then being divided by 3. All collected data are presented in Tables 1 and S1.
Exposure and outcomes of interest
Time-updated K+ during follow-up was the exposure of interest. Second, K+ disorders (hypokalemia [HoK] or hyperkalemia [HerK]) and the coefficient of variation of potassium (K+ CV) were evaluated for their association with the outcomes of interest. HoK was defined as K+ < 3.5 mmol/L, and HerK was defined as K+ > 5.0 mmol/L. The K+ CV, defined as the ratio between the standard deviation (SD) and the mean of all K+ values during follow-up, was used as measure of K+ variability. The main outcome of interest was the occurrence of new onset arrhythmia events. The INTERMACS registry defines adverse events as any documented sustained arrhythmia (either sustained VAs or sustained SVAs)that results in clinical compromise (e.g., abnormal ventricular assist device function, reduced urine output, pre-syncope or syncope, angina, and shortness of breath) or necessitates hospitalization or treatment, such as medication, defibrillation, cardioversion, implantable cardioverter defibrillator (ICD) therapy (e.g., shocks or anti-tachycardia pacing), or arrhythmia ablation procedures.
Separately, we used ECG monitoring data collected during patients follow-ups to identify new instances of supraventricular arrhythmia (SVA) events [atrial fibrillation or atrial flutter (AF)], both with and without clinical symptoms, in patients who did not show AF in their baseline ECG. All arrhythmic events were analyzed both as a composite event and separately. All-cause mortality was investigated as a secondary outcome.
Statistical analysis
Continuous variables were reported as means and standard deviations (SDs) or medians and interquartile ranges (IQRs). Categorical variables were reported as frequencies and percentages. Continuous variables were compared using the Student's t test or the Mann–Whitney U test, as appropriate. Categorical variables were compared using the Chi-squared test. The normality of variable distribution was evaluated via the visual inspection of histograms and Q–Q plots.
The baseline study population data were presented according to K+ quartiles. Time-dependent (TD) Cox regression models were used to estimate the hazard ratios (HRs) and 95% confidence intervals (CIs) of the associations between K+ quartiles, time-updated during follow-up, and the outcomes of interest. Potential confounders were included in several hierarchical models: Model 1 was unadjusted; Model 2 included age, sex, and race; Model 3 included all the covariates in Model 2 plus body mass index (BMI), eGFR, and MAP; Model 4 included all the covariates in Model 3 plus comorbidities and early adverse events post-LVAD implantation; Model 5 included all the covariates in Model 5 plus medications. Given that K+ levels, MAP, eGFR, and medication used can change over time, we treated these variables as time-varying in the Cox proportional hazards regression models.
Survival time was defined as the time from the first K+ measurement, taken 1-month post-LVAD implantation, to new-onset cardiac arrhythmia event, death, or the end of follow-up. All living patients were censored after 5 years of follow-up. Patients who underwent LVAD explant due to recovery or heart transplantation were also censored at the time of MCS device removal.
The continuous relationship between K+ and the outcomes of interest was investigated using K+ as natural splines in multivariable-adjusted TD Cox regression models. We performed a Kaplan–Meier (KM) survival analysis on the primary and secondary outcomes of interest, comparing baseline K+ quartiles. The log-rank test was used to test for differences in survival.
Multivariable adjusted logistic regression models were used to describe the association between new-onset cardiac arrhythmia events (VAs, SVAs, and AF) and mortality. The same covariates used in the previous models plus late adverse event post-LVAD implantation were included to control for confounders.
To evaluate the effect modification by the history of arrhythmia before LVAD implantation on the relationship between K+ levels and new-onset cardiac arrhythmia events, a stratified analysis and an interaction test were performed.
As a sensitivity analysis, we investigated the relationship between K+ disorders (HoK and HerK), updated over time during follow-up, and the outcomes of interest using TD Cox regression models. The same covariates used in the main analysis were included in the multivariable models for confounding control.
Natural splines in multivariable adjusted logistic regression models were used to evaluate the relationship between K+ CV levels and the occurrence of new-onset cardiac arrhythmia event and death. These associations were explored in three separate subgroups of the study population based on their average K+ values during follow-up. The percentiles of the average K+ distribution during follow-up were used to define the following groups: below the 25th percentile, between the 25th and 75th percentiles, and above the 75th percentile.
We used the R software (version 4.1.1, R Foundation for Statistical Computing Platform) for all analyses and calculations. A two-tailed p value < 0.05 was considered statistically significant.
Results
Baseline study population characteristics
Overall, 10,570 patients were enrolled in the study, contributing a total of 26,502 study visits. Each patient had a median of 2 visits (IQR 2), with a median interval of 4.5 months (IQR 3.9) between visits.
The type of LVAD was available for 9652 patients. Most patients (N = 7749) received axial-type LVADs, while 1903 patients received centrifugal-type LVADs. Baseline descriptive characteristics are reported in Table 1. Patients in the highest K+ quartile were older, with a higher prevalence of males and whites. Comorbidities exhibited a homogeneous distribution across the K+ quartiles, except for coronary artery disease, peripheral vascular disease, and severe diabetes, which were more prevalent in patients with higher K+ levels. The use of beta-blocker as renin–angiotensin system inhibitor therapies was more frequently observed in patients with higher K+ levels, whereas diuretic therapy use was more prevalent in patients with lower K+ levels.
Association between K + levels and arrhythmia
During a median follow-up of 9.6 (IQR 17.6) months, 1700 (16.1%) patients experienced new-onset cardiac arrhythmia events, with a 5-year event-free survival probability of 61.1% (95% CI: 58.7, 63.6; Fig. 2A. Patients in the lowest baseline K+ quartiles displayed a lower probability of new-onset arrhythmic events; however, this was not statistically significant (log-rank p value = 0.3; Fig. 2A).
Kaplan–Meier survival curves for de novo arrhythmia event A and all-cause mortality B based on quartiles of baseline K+. Results are displayed up to 5 years. The overall 5-year survival was 61.1% (95% CI 58.7, 63.6) for de novo arrhythmia event and 45.3% (95% CI 43.1, 47.6) for all-cause mortality. Q, quartile of serum K+
After sequentially adjusting for confounders, a significant and consistent relationship was observed between the lowest quartile of longitudinal K+ and the risk of arrhythmic events (HR 1.28, 95% CI 1.08, 1.53, p = 0.005; Table 2) as well as in the highest K+ quartile (HR 1.24, 95% CI 1.02, 1.49, p = 0.027; Table 2).
When the relationship between longitudinal K+ and arrhythmia was explored as a natural spline in a TD Cox regression model, both low and high K+ levels were associated with an increased log-hazard of arrhythmic events (p value nonlinear < 0.001; Fig. 3A). A similar association was confirmed in the stratified analysis of arrhythmia types (Table S2); however, this was only seen for SVAs and AF, where the lowest and highest quartiles of longitudinal K+ were associated with an increased HR. This was reflected in a U-shaped relationship (SVA, p value nonlinear = 0.034; AF, p value nonlinear = 0.001) when K+ was analyzed as a spline (Fig. 4).
Continuous relationship between K+ and arrhythmia event (A) and all-cause mortality (B). Multivariable time-dependent adjusted model, adjusted to age, sex, race, MAP, BMI, eGFR, CAD, NYHA class, history of arrhythmias, major stroke, cerebrovascular disease, PVD, severe diabetes, liver disease, respiratory disease, early adverse events, medications; MAP, eGFR and medications treated as time-varying covariates
Continuous relationship between K+ and sustained ventricular arrhythmia (A), sustained supraventricular arrhythmia (B) and atrial fibrillation/flutter (C). Multivariable time-dependent adjusted model, adjusted to age, sex, race, MAP, BMI, eGFR, CAD, NYHA class, history of arrhythmias, major stroke, cerebrovascular disease, PVD, severe diabetes, liver disease, respiratory disease, early adverse events, medications; MAP, eGFR and medications treated as time-varying covariates
Stratified analysis by the history of arrhythmias before LVAD implantation suggested an effect modification on the relationship between K+ levels and the risk of new-onset arrhythmic event (Table S3).
In the sensitivity analysis, only HerK was significantly associated with an increased hazard ratio (HR) for new-onset cardiac arrhythmias (HR 1.34, 95% CI 1.00–1.79, p = 0.047; Table S4). Although an increased hazard for cardiac arrhythmias was also observed with HoK, it did not reach statistical significance in the multivariable adjusted model (HR 1.20, 95% CI 0.97–1.50, p = 0.100; Table S4).
When exploring the relationship between K+ variability and arrhythmias, the association between K+ CV and the new-onset of cardiac arrhythmia event was not consistent across all subgroup of the average K+ distribution (Figure S1). An increase in K+ CV was associated with an increased risk of new-onset cardiac arrhythmia events only in patients with average K+ values between the 25th and 75th percentiles.
New-onset cardiac arrhythmia events were independent predictors of mortality (Table S5). This association was only confirmed for sustained arrhythmia event: VA (OR 1.45, 95% CI 1.16, 1.80, p < 0.001) and SVA (OR 1.40, 95% CI 1.05, 1.85, p < 0.001).
Association between K+ levels and mortality
During a median follow-up of 11.4 (IQR 20.3) months, 2,447 (23.2%) of the patients died, with a 5-year event-free survival probability of 45.3% (95% CI: 43.1, 47.6; Fig. 2B). Both low and high baseline K+ levels were associated with lower survival probability (Fig. 2B, log-rank p value = 0.004). The highest and lowest quartiles of longitudinal K+ were independently associated with a significant increase in the HR of death (Table 3), which was reflected by a U shaped relationship (p value nonlinear < 0.001, Fig. 3B).
Similar findings were observed in the sensitivity analysis, where both HoK and HerK were associated with an increased mortality risk (Table S6). Higher K+ variability was associated with increased log odds of death. This result was consistent across all subgroups of the average K+ distribution (Figure S1).
Discussion
Our study demonstrated a significant U-shaped relationship between low and high K+ levels and the occurrence of cardiac arrhythmias in LVAD patients. This relationship was particularly significant for SVAs (which comprises both atrial tachycardias, AF and atrial flutter) and AF (which have been identified by ECG recordings, see method section). As expected, both high and low K+ levels exhibited an unfavorable prognostic impact on LVAD patient survival. Sustained arrhythmic events occurring after LVAD implantation negatively impacted patient survival.
The existing literature has extensively reported on the relationship between K+ imbalances and cardiac arrhythmias [12,13,14]. K+ plays a crucial role in maintaining normal cardiac electrical activity [15]. Abnormal K+ levels can disrupt the balance of ion channels responsible for the cardiac electrical conduction system, causing arrhythmias [16, 17]. It is widely acknowledged that K+ imbalances adversely impact patient survival [8, 18]. Fluctuations in K+ levels can disturb the normal cardiac rhythm and increase a patient’s susceptibility to life-threatening arrhythmias [7].
While the use of LVADs is becoming increasingly common among individuals with severe heart failure, limited studies have investigated the relationship between K+ levels and the risk of arrhythmias and/or mortality in LVAD recipients [19, 20]. The most compelling evidence comes from a study conducted by Ziv et al., where a broad spectrum of electrolyte imbalances, including K+, calcium, and magnesium, were demonstrated to be independent predictors of VAs in a cohort of 100 LVAD patients [20]. However, conversely to our study, Ziv et al. [20] included the early post-LVAD implantation period in their analysis. Most VAs occur during this period. This period is likely influenced by “mechanical” factors, such as suctioning events, myocardial irritation due to inflow cannula insertion, QT prolongation, and the use of pro-arrhythmogenic drugs like ino-vasopressors immediately following implantation [21,22,23]. Such factors may have influenced the conclusions drawn by Ziv et al. [20].
Our study aimed to comprehensively examine the association between K+ levels and the risk of late cardiac arrhythmias, sustained or non-sustained, in LVAD patients. To address the issue observed in the study by Ziv et al. [20], we focused solely on arrhythmias that occurred at least 1-month post-LVAD implantation.
Our analysis confirmed the elevated prevalence of late arrhythmic events within the LVAD patient population and identified a significant association between K+ levels, the risk of new-onset arrhythmic events, and patient survival. The findings highlight a robust connection between low K+ levels and the risk of late arrhythmias, particularly SVAs and AF. However, a U-shaped relationship more accurately characterizes the relationship between K+ levels and arrhythmias.
Notably, this relationship holds true primarily in patients without a history of arrhythmia before LVAD implantation. When stratifying by the presence or absence of arrhythmia history before LVAD implantation, we found that the association between abnormal K+ levels and new arrhythmic events remained significant only in patients without a prior history of arrhythmias. In contrast, this association was not significant in patients with a prior history of arrhythmias. The interaction between K+ levels and arrhythmia history approached significance (p = 0.07), suggesting that the presence of pre-existing arrhythmias may modulate the heart's sensitivity to K+ fluctuations. This finding highlights the complex interplay between electrolyte balance and arrhythmic risk in this patient population and underscores the need for tailored K+ management strategies based on individual arrhythmic history. Further studies are warranted to elucidate the underlying mechanisms and to explore potential therapeutic implications.
Not only do high or low K+ levels influence the risk of arrhythmia, but fluctuations in K+ levels can also contribute to the onset of new arrhythmic events and impact patient survival. Our analyses show that an increase in K+ level variability significantly raises the risk of new arrhythmic events, especially in patients with consistently normal K+ levels. This increased risk was not observed in patients with consistently high or low K+ levels. These findings suggest that the variability in K+ levels, rather than the absolute values, plays a crucial role in the genesis of cardiac arrhythmias in patients with LVADs. In addition, a more predictable relationship was observed between K+ level variability and the risk of death, regardless of the absolute serum K+ values. Fluctuations in K+ levels appear to be more harmful than consistently high or low levels because the heart has more difficulty adapting to rapid and frequent changes. These fluctuations can destabilize the membrane potentials of cardiac cells, interfere with repolarization, cause electrolyte imbalances, and induce cellular stress. The continuous need for K+ level adjustments prevents the heart from maintaining electrical and mechanical stability, thus increasing the risk of arrhythmias and compromising patient survival.
The significant impact of K+ alterations on SVAs observed in our study raises questions about the underlying mechanisms driving this. While VAs, particularly hypokalemia-related, are widely associated with K+ disorders in the general population and are the most common arrhythmia reported in LVAD patients [12, 24, 25], our findings did not reveal a significant link between K+ levels and the risk of VAs. However, they did confirm a relationship between high and low K+ levels and the risk of SVAs. Finding a rationale that could justify or clarify these results is challenging. Moreover, the lack of other studies that have investigated this issue in LVAD patients makes comparisons difficult. The only available evidence, gathered from a limited sample of 100 patients, does not differentiate between high and low K+ values and encompasses both the early post-LVAD implantation period and the later period [20]. It is possible that there is a problem in the detection of VAs related to INTERMACS registry, which does not include ICDs routine reading results and defines adverse events only documented arrhythmia that results in clinical compromise. Considering this particular characteristic of the registry, it is possible that HypoK was associated with a low number of clinically impactful VAs. We further propose that factors, whether mechanical or comorbidities rather than altered K+ levels, are responsible for late VAs in LVAD patients. However, further research is needed to elucidate the precise mechanisms linking K+ levels to specific types of arrhythmias in LVAD patients. The mechanisms by which SVAs have a negative effect on LVAD patients’ prognosis are still not precisely defined, however several hypothesis may be advanced. SVAs are associated with an increased risk of right ventricular failure [26] and thromboembolic events [27] that may explain the higher mortality. These complications represent 30.9% of the late adverse events in our study (Table S1).
Another interesting hypothesis is provided by Deshmukh A et al. [28]. LVADs are able to induce a beneficial atrial electroanatomical remodelling by both reducing the atrial pressure and unloading the left ventricle, and by improving the patients’ neurohormonal status. The atrial size is strictly related to the risk of SVAs [29, 30], and indeed the favourable atrial remodelling results in a reduction in the SVAs occurrence in LVAD patients [28] similarly to what happens in case of cardiac resynchronization therapy [31, 32]. As hypothesized by Deshmukh et al., it is possible that the increased mortality associated with SVAs is due to an insufficient unloading of the ventricles provided by the LVAD. In the context of electrolytes imbalance, a large atrial size could exponentially increase the risk of SVAs which therefore could be an indirect sign of an inadequate mechanical circulatory support. Another hypothesis that could explain the association between SVAs and increased mortality in LVAD is the association between SVAs and sepsis. Patients with sepsis have a higher probability of SVAs [33]. Furthermore, it has been demonstrated a U-shaped relationship of mortality due to sepsis and K+ levels [34]. In the context of sepsis, which is responsible for 48.5% of late adverse events in our study, K+ imbalance could be another (together with sepsis) predisposing factor for SVAs.
Based on our findings, it appears there is a range of K+ values within which LVAD patients may experience a relatively lower risk of arrhythmic events. However, although the range of K+ levels is quite broad (3.7–6.1 mmol/L) for sustained SVAs, it is narrower (3.9–0.3 mmol/L) for AF. This data becomes more significant when viewed in the context of the impact of sustained and non-sustained arrhythmic events on the mortality risk of LVAD patients.
These findings may have some important implications, particularly for CF-LVAD patients who do not have an implantable cardioverter defibrillator (subcutaneous or intracavitary ICD). The American Heart Association and European Society of Cardiology recommend ICD implantation for patients who experience sustained VAs; however, their recommendations are vague in cases where primary prevention ICD may be needed, advising individualized approaches are used [35, 36]. Furthermore, recent studies have reported that ICD demonstrates a lack of beneficial effects on the mortality of CF-LVAD patients [37, 38]. Moreover, ICD implantation in LVAD patients is associated with a significant risk of infection and bleeding [36]. Using a stricter K+ range to determine ICD eligibility might limit the occurrence of potentially fatal sustained VAs in these patients, as well as other complications associated with ICD implantation.
A U-shaped relationship characterizes the association between K+ levels and mortality risk. We observed that K+ values below 3.9 mmol/L and above 4.5 mmol/L (in the quartile analysis) or below 4 mmol/L and above 4.9 mmol/L (in the analysis where K+ was a continuous spline variable) were significantly associated with an increased risk of death. There are several potential mechanisms behind these observations. Very low K+ levels may impact cardiac function and increase the risk of arrhythmias and other complications [24, 39], while excessively high K+ levels could disrupt normal cardiac electrical activity, contributing to adverse outcomes [12]. The association between survival and K+ levels can also be viewed within the context of CKD and eGFR adjustments, the detrimental roles of which have been considered major prognostic determinants [40,41,42,43]. Therefore, even moderately altered K+ levels are dangerous in LVAD patients. The U-shaped relationship suggests that maintaining K+ levels within an optimal range is crucial for reducing the risk of arrhythmic events or mortality in LVAD patients. K+ levels should be closely monitored and appropriately managed to ensure they remain within the desired therapeutic range. This might involve dietary adjustments, medication modifications, or other interventions to maintain K+ balance.
Our study has several strengths that contribute to improving the understanding of the relationship between K+ levels and the risk of late cardiac arrhythmias in LVAD patients. First, it is the first study to comprehensively investigate this association in a systematic manner, including both sustained and non-sustained VAs and SVAs. Second, our findings highlight the negative impact of K+ alterations, even mild ones, on patient prognoses. These insights emphasize the importance of closely monitoring and managing K+ levels in LVAD patients to improve outcomes.
Despite these significant contributions, there are certain limitations in this study to consider. First, the retrospective nature of the study design introduced inherent biases and limited our ability to establish a causal relationship between K+ levels and arrhythmias. Second, it was not possible to characterize specific types of cardiac arrhythmias in detail. Doing so could provide further insights into the differential associations between arrhythmias and K+ levels. In addition, the analysis only focused on the late post-LVAD implantation period (at least 1 month after), which restricts our considerations to this subset of the population. This, together with the other eligibility criteria may have influenced our population’s survival time making it lower compared to that reported by recent scientific literature [44]. Future prospective studies using larger sample sizes that comprehensively characterize different arrhythmias are warranted. Alterations in K+ levels may also reflect the presence of underlying diseases, greater clinical instability, or increased use of medications, which could also impact patient prognoses.
In conclusion, our study provides compelling evidence of the significant relationship between K+ alterations and the risk of late cardiac arrhythmias in LVAD patients. The effect goes well beyond the classical definition of hypokalemia (< 3.5 mEq/L) and hyperkalemia (> 5.5 mEq/L), as even marginal reductions or increases in serum K+ levels were seen to adversely impact patient prognoses. This emphasizes the need for K+ levels to be carefully monitored and managed to maintain a balanced and optimal range for each individual patient. However, the importance of individualized care must be noted, as the optimal range of K+ levels may vary for each patient based on their specific clinical context and medical history. Regular follow-ups and collaboration between healthcare professionals are essential to assess and manage K+ levels effectively and mitigate the risk of adverse events, including arrhythmias and mortality. Further research is needed to elucidate the mechanisms and establish optimal strategies for maintaining K+ balance in this patient population.
Data availability
The dataset generated and analyzed during the current study is available in the Biological Specimen and Data Repository Information Coordinating Center [10].
References
Trachtenberg BH, Estep JD (2016) Roads, maps, and destinations: the journey of left ventricular assist device implantation in ambulatory patients with advanced heart failure. Curr Cardiol Rep 18:1–7. https://doi.org/10.1007/S11886-016-0785-Y/TABLES/1
Kadado AJ, Akar JG, Hummel JP (2018) Arrhythmias after left ventricular assist device implantation: incidence and management. Trends Cardiovasc Med 28:41–50. https://doi.org/10.1016/J.TCM.2017.07.002
Kirklin JK, Naftel DC, Kormos RL et al (2013) Fifth INTERMACS annual report: Risk factor analysis from more than 6,000 mechanical circulatory support patients. J Heart Lung Transplant 32:141–156. https://doi.org/10.1016/j.healun.2012.12.004
Jedeon Z, Cogswell R, Schultz J et al (2021) Association between early ventricular arrhythmias and mortality in destination vs. bridge patients on continuous flow LVAD support. Sci Rep 11:19196. https://doi.org/10.1038/S41598-021-98109-2
Hoppe LK, Muhlack DC, Koenig W et al (2018) Association of abnormal serum potassium levels with arrhythmias and cardiovascular mortality: a systematic review and meta-analysis of observational studies. Cardiovasc Drugs Ther 32:197–212. https://doi.org/10.1007/S10557-018-6783-0/FIGURES/3
Packer M (1990) Potential role of potassium as a determinant of morbidity and mortality in patients with systemic hypertension and congestive heart failure. Am J Cardiol. https://doi.org/10.1016/0002-9149(90)90251-U
Podrid PJ (1990) Potassium and ventricular arrhythmias. Am J Cardiol. https://doi.org/10.1016/0002-9149(90)90250-5
Cleland JGF, Dargie HJ, Robertson I et al (1987) Total body electrolyte composition in patients with heart failure: a comparison with normal subjects and patients with untreated hypertension. Br Heart J 58:230. https://doi.org/10.1136/HRT.58.3.230
Holman WL (2012) Interagency Registry for Mechanically Assisted Circulatory Support (INTERMACS): what have we learned and what will we learn? Circulation 126:1401–1406. https://doi.org/10.1161/CIRCULATIONAHA.112.097816
Coady SA, Mensah GA, Wagner EL et al (2017) Use of the national heart, lung, and blood institute data repository. N Engl J Med 376:1849. https://doi.org/10.1056/NEJMSA1603542
Delgado C, Baweja M, Crews DC et al (2022) A Unifying Approach for GFR Estimation: recommendations of the NKF-ASN task force on reassessing the inclusion of race in diagnosing kidney disease. Am J Kidney Dis 79:268-288.e1. https://doi.org/10.1053/J.AJKD.2021.08.003
Goyal A, Spertus JA, Gosch K et al (2012) Serum potassium levels and mortality in acute myocardial infarction. JAMA 307:157–164. https://doi.org/10.1001/JAMA.2011.1967
Krijthe BP, Heeringa J, Kors JA et al (2013) Serum potassium levels and the risk of atrial fibrillation: the Rotterdam Study. Int J Cardiol 168:5411–5415. https://doi.org/10.1016/j.ijcard.2013.08.048
Madias JE, Shah B, Chintalapally G et al (2000) Admission serum potassium in patients with acute myocardial infarction: its correlates and value as a determinant of in-hospital outcome. Chest 118:904–913. https://doi.org/10.1378/chest.118.4.904
Palmer BF, Clegg DJ (2016) Physiology and pathophysiology of potassium homeostasis. Adv Physiol Educ 40:480–490. https://doi.org/10.1152/ADVAN.00121.2016
Brown MJ, Brown DC, Murphy MB (1983) Hypokalemia from beta2-receptor stimulation by circulating epinephrine. N Engl J Med 309:1414–1419. https://doi.org/10.1056/NEJM198312083092303
Obeid AI, Verrier RL, Lown B (1978) Influence of glucose, insulin, and potassium on vulnerability to ventricular fibrillation in the canine heart. Circ Res 43:601–608. https://doi.org/10.1161/01.RES.43.4.601
Lombardi G, Gambaro G, Ferraro PM (2022) Serum potassium variability is associated with increased mortality in a large cohort of hospitalized patients. Nephrol Dial Transplant 37:1482–1487. https://doi.org/10.1093/NDT/GFAB211
Monreal G, Gerhardt MA (2007) Left ventricular assist device support induces acute changes in myocardial electrolytes in heart failure. ASAIO J 53:152–158. https://doi.org/10.1097/MAT.0B013E3180302A8B
Ziv O, Dizon J, Thosani A et al (2005) Effects of left ventricular assist device therapy on ventricular arrhythmias. J Am Coll Cardiol 45:1428–1434. https://doi.org/10.1016/J.JACC.2005.01.035
Harding JD, Piacentino V, Gaughan JP et al (2001) Electrophysiological alterations after mechanical circulatory support in patients with advanced cardiac failure. Circulation 104:1241–1247. https://doi.org/10.1161/HC3601.095718
Gopinathannair R, Cornwell WK, Dukes JW et al (2019) Device therapy and arrhythmia management in left ventricular assist device recipients: a scientific statement from the American heart association. Circulation 139:E967–E989. https://doi.org/10.1161/CIR.0000000000000673
Vollkron M, Voitl P, Ta J et al (2007) Suction events during left ventricular support and ventricular arrhythmias. J Heart Lung Transplant 26:819–825. https://doi.org/10.1016/J.HEALUN.2007.05.011
Keskin M, Kaya A, Tatlısu MA et al (2016) The effect of serum potassium level on in-hospital and long-term mortality in ST elevation myocardial infarction. Int J Cardiol 221:505–510. https://doi.org/10.1016/J.IJCARD.2016.07.024
Griffin JM, Katz JN (2014) The burden of ventricular arrhythmias following left ventricular assist device implantation. Arrhythm Electrophysiol Rev 3:145
Ozcan C, Deshmukh A (2020) Atrial arrhythmias in patients with left ventricular assist devices. Curr Opin Cardiol 35:276. https://doi.org/10.1097/HCO.0000000000000729
Keshav Chivukula V, Beckman J, Li S et al (2024) Atrial fibrillation increases thrombogenicity of LVAD therapy. Int J Artif Organs 47:329–337. https://doi.org/10.1177/03913988241251706
Deshmukh A, Kim G, Burke M et al (2017) Atrial arrhythmias and electroanatomical remodeling in patients with left ventricular assist devices. J Am Heart Assoc Cardiovasc Cerebrovasc Dis. https://doi.org/10.1161/JAHA.116.005340
Mulukutla S, Althouse AD, Jain SK, Saba S (2018) Increased left atrial size is associated with higher atrial fibrillation recurrence in patients treated with antiarrhythmic medications. Clin Cardiol 41:825. https://doi.org/10.1002/CLC.22964
Saadeh R, Abu Jaber B, Alzuqaili T et al (2024) (2024) The relationship of atrial fibrillation with left atrial size in patients with essential hypertension. Scie Rep 14:1–6. https://doi.org/10.1038/s41598-024-51875-1
Yu CM, Fang F, Zhang Q et al (2007) Improvement of atrial function and atrial reverse remodeling after cardiac resynchronization therapy for heart failure. J Am Coll Cardiol 50:778–785. https://doi.org/10.1016/J.JACC.2007.04.073
Fung JWH, Yip GWK, Zhang Q et al (2008) Improvement of left atrial function is associated with lower incidence of atrial fibrillation and mortality after cardiac resynchronization therapy. Heart Rhythm 5:780–786. https://doi.org/10.1016/J.HRTHM.2008.02.043
Walkey AJ, Wiener RS, Ghobrial JM et al (2011) Incident stroke and mortality associated with new-onset atrial fibrillation in patients hospitalized with severe sepsis. JAMA 306:2248–2255. https://doi.org/10.1001/JAMA.2011.1615
Tang J, Zhao P, Li Y et al (2024) The relationship between potassium levels and 28-day mortality in sepsis patients: secondary data analysis using the MIMIC-IV database. Heliyon. https://doi.org/10.1016/J.HELIYON.2024.E31753
Al-Khatib SM, Stevenson WG, Ackerman MJ et al (2018) 2017 AHA/ACC/HRS guideline for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: executive summary: a report of the American college of cardiology/American heart association task force on clinical practice guidelines and the heart rhythm society. Circulation 138:e210–e271. https://doi.org/10.1161/CIR.0000000000000548
Zeppenfeld K, Tfelt-Hansen J, De Riva M et al (2022) 2022 ESC Guidelines for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death. Eur Heart J 43:3997–4126. https://doi.org/10.1093/EURHEARTJ/EHAC262
Pausch J, Mersmann J, Bhadra OD et al (2023) Prognostic impact of implantable cardioverter defibrillators and associated adverse events in patients with continuous flow left ventricular assist devices. Front Cardiovasc Med. https://doi.org/10.3389/FCVM.2023.1158248
Rorris FP, Antonopoulos CN, Kyriakopoulos CP et al (2021) Implantable cardioverter defibrillators in left ventricular assist device patients: a systematic review and meta-analysis. J Heart Lung Transplant 40:1098–1106. https://doi.org/10.1016/J.HEALUN.2021.05.014
Lombardi G, Gambaro G, Ferraro PM (2022) Serum potassium disorders predict subsequent kidney injury: a retrospective observational cohort study of hospitalized patients. Kidney Blood Press Res 47:270–276. https://doi.org/10.1159/000521833
Dalia T, Chan W, Sauer AJ et al (2022) Outcomes in patients with chronic kidney disease and end-stage renal disease and durable left ventricular assist device: insights from the united states renal data system database. J Card Fail 28:1604–1614. https://doi.org/10.1016/J.CARDFAIL.2022.03.355
Ibrahim M, Saint CGR, Lacy S, Chaparro S (2021) Impact of renal dysfunction on outcomes after left ventricular assist device: a systematic review. Int J Heart Failure 3:69
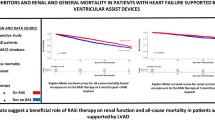
Lombardi G, Gambaro A, Ribichini FL et al (2023) RAS inhibitors and renal and general mortality in patients with heart failure supported by left ventricular assist devices: a registry study. Clin Res Cardiol 112:891–900. https://doi.org/10.1007/S00392-022-02136-6
Gambaro A, Lombardi G, Onorati F et al (2021) Heart, kidney and left ventricular assist device: a complex trio. Eur J Clin Invest. https://doi.org/10.1111/ECI.13662
Jorde UP, Saeed O, Koehl D et al (2024) The society of thoracic surgeons intermacs 2023 annual report: focus on magnetically levitated devices. Ann Thorac Surg 117:33–44. https://doi.org/10.1016/J.ATHORACSUR.2023.11.004
Acknowledgements
The authors thank the INTERMACS investigators, coordinators, and participating institutions for the data they provided for this registry. This manuscript was prepared using the INTERMACS research materials obtained from the NHLBI Biologic Specimen and Data Repository Information Coordinating Center and does not necessarily reflect the opinions or views of INTERMACS or the NHLBI.
The study was performed under the framework of the project PNRR for Mission 4, Component 2, Investment 1.4, funded by the European Union—NextGenerationEU, Notice: MUR Directorial Decree n. 341 of 15-03-2022, Project: “HEAL ITALIA”—“Health Extended Alliance for Innovative Therapies, Advanced Lab-research and Integrated Approaches of Precision Medicine Extended Partnership.”
Funding
This study was not funded.
Author information
Authors and Affiliations
Contributions
G.L., P.M.F., A.G. and G.G. contributed to the research idea and study design. G.L. contributed to data acquisition. G.L., E.D.T., A.G. and P.M.F. contributed to data analysis and interpretation. P.M.F., E.D.T. and G.L. contributed to statistical analysis. G.L. and A.G. drafted the paper. G.G., P.M.F., and F.L.R. contributed to supervision. Each author contributed important intellectual content during manuscript drafting of the overall work.
Corresponding author
Ethics declarations
Conflict of interest
P.M.F. received consultant fees from Allena Pharmaceuticals, Alnylam, AstraZeneca, Bayer, NovoNordisk, Otsuka Pharmaceuticals and royalties as an author for UpToDate. G.G received grant support from Fresenius Kabi, Roche Diagnostics and royalties as an author for UpToDate. All the other authors report no disclosures.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lombardi, G., Gambaro, A., Ferraro, P.M. et al. The relationship between serum potassium levels and cardiac arrhythmias in left ventricular assist device (LVAD) recipients: a comprehensive analysis and prognostic evaluation. Clin Res Cardiol (2024). https://doi.org/10.1007/s00392-024-02531-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00392-024-02531-1