Abstract
Background
Stoma formation is a commonly performed procedure both during and following colorectal surgery. When designed correctly, stomas can dramatically improve patients’ quality of life, but the reverse may occur when complications arise. Given the significant negative impact of complications following stoma formation, understanding risk factors that may be mitigated pre-operatively is important.
Method
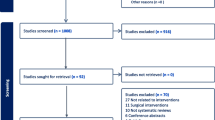
A systematic search of publications using MEDLINE, CINAHL, and Cochrane databases was conducted in May 2022. Data was extracted and a narrative synthesis undertaken. The evidence-based librarianship (EBL) checklist assessed the methodological quality of the included studies. The systematic review includes various research designs such as randomised controlled trials (RCT), case–control studies, and observational cohort studies written in English. Reviews, conference papers, opinion papers, and those including participants < 18 years old were excluded. No restrictions on the date of publication and study setting were applied.
Results
This review included 17 studies, conducted between 2001 and 2020. The study designs were prospective audit, prospective analysis, retrospective analysis, longitudinal analysis and multivariate analysis of self-reported questionaires/surveys. Twenty-two possible risk factors for the development of stoma complications following stoma formation were identified. These include demographical risk factors, underlying medical condition, type of surgery, elective vs emergency surgery, stoma factors, surgical factors, indications for surgery and factors which may impact healing. Furthermore, high BMI, emergency surgery, and stoma type were identified as the most frequently occurring risk factors.
Conclusion
Given the large number of risk factors identified, the implementation of a risk stratification tool may decrease the incidence and prevalence of stoma complication development. This, in turn, would decrease the associated healthcare-related costs, and negative impact on mortality, length of stay and quality of life.

Similar content being viewed by others
Data availability
Due to the study design being a systematic review, supporting data is not available.
Change history
20 October 2023
A Correction to this paper has been published: https://doi.org/10.1007/s00384-023-04549-9
References
Mulita F, Lotfollahzadeh S (2022) Intestinal Stoma. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan. PMID: 33351447
Shabbir J, Britton DC (2010) Stoma complications: a literature overview. Colorectal Dis 12:958–964. https://doi.org/10.1111/j.1463-1318.2009.02006.x
Pandiaraja J, Chakkarapani R, Arumugam S (2021) A study on patterns, indications, and complications of an enteric stoma. J Fam Med Prim Care 10(9):3277–3282. https://doi.org/10.4103/jfmpc.jfmpc_123_21
Qureshi A, Cunningham J, Hemandas A (2018) Emergency stomas; should non-colorectal surgeons be doing it? Gastroenterol Hepatol Bed Bench 11(4):306–312. PMID: 30425809; PMCID: PMC6204250
Zewude WC, Derese T, Suga Y, Teklewold B (2021) Quality of life in patients living with stoma. Ethiop J Health Sci 31(5):993–1000. PMID: 35221616; PMCID: PMC8843156. https://doi.org/10.4314/ejhs.v31i5.11
Liao C, Qin Y (2014) Factors associated with stoma quality of life among stoma patients. Int J Nurs Sci 1(2):196-201, ISSN 2352-0132. https://doi.org/10.1016/j.ijnss.2014.05.007
Malik T, Lee MJ, Harikrishnan AB (2018) The incidence of stoma related morbidity - a systematic review of randomised controlled trials. Ann R Coll Surg Engl 100(7):501–508. https://doi.org/10.1308/rcsann.2018.0126. Epub 2018 Aug 16. PMID: 30112948; PMCID: PMC6214073
Krishnamurty DM, Blatnik J, Mutch M (2017) Stoma complications. Clin Colon Rectal Surg 30(3):193–200. https://doi.org/10.1055/s-0037-1598160. Epub 2017 May 22. PMID: 28684937; PMCID: PMC5498161
Koc U, Karaman K, Gomceli I, Dalgic T, Ozer I, Ulas M, Ercan M, Bostanci E, Akoglu M (2017) A retrospective analysis of factors affecting early stoma complications. Ostomy Wound Manage 63(1):28–32. PMID: 28112647
Arumugam PJ, Bevan L, Macdonald L, Watkins AJ, Morgan AR, Beynon J, Carr ND (2003) A prospective audit of stomas-analysis of risk factors and complications and their management. Colorectal Dis 5:49–52. https://doi.org/10.1046/j.1463-1318.2003.00403.x
Persson E, Berndtsson I, Carlsson E, Hallén A-M, Lindholm E (2010) Stoma-related complications and stoma size – a 2-year follow up. Colorectal Dis 12:971–976. https://doi.org/10.1111/j.1463-1318.2009.01941.x
Parmar KL, Zammit M, Smith A, Kenyon D, Lees NP (2011) A prospective audit of early stoma complications in colorectal cancer treatment throughout the Greater Manchester and Cheshire colorectal cancer network. Colorectal Dis 13:935–938. https://doi.org/10.1111/j.1463-1318.2010.02325.x
Harilingam M, Sebastian J, Twum-Barima C, Boshnaq M, Mangam S, Khushal A et al (2015) Patient-related factors influence the risk of developing intestinal stoma complications in early post-operative period. ANZ J Surg 87(10):E116–E120. https://doi.org/10.1111/ans.13397
Glynn L (2006) A critical appraisal tool for library and information research. Emerald Insight 24(3):387–399
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Coroş MF, Sorlea S, Hintea A, Georgescu R, Crăciun C, Pascarenco G (2016) Indications of a defunctioning stoma in colorectal anastomosis–our experience and review of the literature. Chirurgia 111(2):138–143
John B, Kim M-Y, Forgrave D (2019) Risk factors associated with peristomal skin complications: Integrative literature review. J Nurs Educ Pract 9(7). https://doi.org/10.5430/jnep.v9n7p82
Vogel I, Shinkwin M, van der Storm SL, Torkington J, Cornish AJ, Tanis PJ, Hompes R, Bemelman WA (2022) Overall readmissions and readmissions related to dehydration after creation of an ileostomy: a systematic review and meta-analysis. Tech Coloproctol 26(5):333–349. https://doi.org/10.1007/s10151-022-02580-6
Zelga P, Kluska P, Zelga M, Piasecka-Zelga J, Dziki A (2021) Patient-related factors associated with stoma and peristomal complications following fecal ostomy surgery: a scoping review. J Wound Ostomy Continence Nurs 48(5):415–430. https://doi.org/10.1097/WON.0000000000000796
Formijne Jonkers HA, Draaisma WA, Roskott AM, van Overbeeke AJ, Broeders IA, Consten EC (2012) Early complications after stoma formation: a prospective cohort study in 100 patients with 1-year follow-up. Int J Colorectal Dis 27(8):1095–1099. https://doi.org/10.1007/s00384-012-1413-y
Lee HJ, Park SJ, Min BS, Cheon JH, Kim TI, Kim NK, Kim WH, Hong SP (2014) The role of primary colectomy after successful endoscopic stenting in patients with obstructive metastatic colorectal cancer. Dis Colon Rectum 57(6):694–699. https://doi.org/10.1097/DCR.0000000000000061
Pinto I, Queirós S, Queirós C, Silva C, Santos C, Brito M (2017) Risk factors associated with the development of elimination stoma and peristomal skin complications. Rev Enferm Ref IV Série(15):155–166
Khor BY, McSorley ST, Horgan PG, McMillan DC (2017) The relationship between systemic inflammation and stoma formation following anterior resection for rectal cancer: A cross-sectional study. Int J Surg 37:79–84. https://doi.org/10.1016/j.ijsu.2016.12.010
EuroSurg Collaborative (2018) Body mass index and complications following major gastrointestinal surgery: a prospective, international cohort study and meta-analysis. Colorectal Dis 20(8):0215–0225. https://doi.org/10.1111/codi.14292
Krebs B, Ivanecz A, Potrc S, Horvat M (2019) Factors affecting the morbidity and mortality of diverting stoma closure: retrospective cohort analysis of twelve-year period. Radiol Oncol 53(3):331–336. https://doi.org/10.2478/raon-2019-0037
van Ommeren-Olijve SJ, Burbach JPM, Furnée EJB, Dutch Snapshot Research Group (2020) Risk factors for non-closure of an intended temporary defunctioning stoma after emergency resection of left-sided obstructive colon cancer. Int J Colorectal Dis 35(6):1087–1093. https://doi.org/10.1007/s00384-020-03559-1
Saghir JH, McKenzie FD, Leckie DM, McCourtney JS, Finlay IG, McKee RF, Anderson JH (2001) Factors that predict complications after construction of a stoma: a retrospective study. Eur J Surg 167(7):531–534. https://doi.org/10.1080/110241501316914911. PMID: 11560389
Cottam J, Richards K, Hasted A, Blackman A (2007) Results of a nationwide prospective audit of stoma complications within 3 weeks of surgery. Colorectal Dis 9(9):834–838. https://doi.org/10.1111/j.1463-1318.2007.01213.x. Epub 2007 Aug 2 PMID: 17672873
Sung YH, Kwon I, Jo S, Park S (2010) Factors affecting ostomy-related complications in Korea. J Wound Ostomy Continence Nurs 37(2):166–172. https://doi.org/10.1097/WON.0b013e3181cf7b76. PMID: 20228659
Pittman JA (2011) Ostomy complications and associated risk factors: Development and testing of two instruments. Indiana University
Funahashi K, Suzuki T, Nagashima Y, Matsuda S, Koike J, Shiokawa H, Ushigome M, Arai K, Kaneko T, Kurihara A, Kaneko H (2014) Risk factors for parastomal hernia in Japanese patients with permanent colostomy. Surg Today 44(8):1465–1469. https://doi.org/10.1007/s00595-013-0721-3. Epub 2013 Sep 13. PMID: 24030376; PMCID: PMC4097204
Kozan R, Gültekin FA (2018) Controllable risk factor in the development of parastomal hernia; preoperative marking. Turk J Colorectal Dis 28(4):172–176. https://cms.galenos.com.tr/Uploads/Article_25536/turkishjcrd-28-172-En.pdf. Accessed 17 May 2022
Braumann C, Müller V, Knies M, Aufmesser B, Schwenk W, Koplin G (2019) Complications after ostomy surgery: emergencies and obese patients are at risk-data from the Berlin OStomy Study (BOSS). World J Surg 43(3):751–757. https://doi.org/10.1007/s00268-018-4846-9. PMID: 30426187
Jana K, Bera P, Mukhopadhyay A, Bhattacharya U (2020) Prospective evaluation of early local complications of stoma and their risk factors. Int Surg J 7(9):3024–3031
Pennings JP, Kwee TC, Hofman S, Viddeleer AR, Furnée EJB, van Ooijen PMA, de Haas RJ (2021) Clinical and radiologic predictors of parastomal hernia development after end colostomy. AJR Am J Roentgenol 216(1):94–103. https://doi.org/10.2214/AJR.19.22498. Epub 2020 Oct 29 PMID: 33119406
Ayik C, Özden D, Cenan D (2020) Ostomy complications, risk factors, and applied nursing care: a retrospective. Descriptive Study Wound Manag Prev 66(9):20–30 PMID: 32903201
Voegeli D, Karlsmark T, Eddes EH, Hansen HD, Zeeberg R, Hakan-Bloch J, Hedegaard CJ (2020) Factors influencing the incidence of peristomal skin complications: evidence from a multinational survey on living with a stoma. Gastrointest Nurs 18(Sup 4):S31–S38. https://doi.org/10.12968/gasn.2020.18.Sup4.S31
Shiraishi T, Nishizawa Y, Ikeda K, Tsukada Y, Sasaki T, Ito M (2020) Risk factors for parastomal hernia of loop stoma and relationships with other stoma complications in laparoscopic surgery era. BMC Surg 20(1):141. https://doi.org/10.1186/s12893-020-00802-y. PMID: 32571293; PMCID: PMC7310075
Carlsen E, Bergan A (1995) Technical aspects and complications of end ileostomies. World J Surg 19:632–636
Beck SJ (2011) Stoma issues in the obese patient. Clin Colon Rectal Surg 24(4):259–262. https://doi.org/10.1055/s-0031-1295689
Hildebrandt X, Ibrahim M, Peltzer N (2023) Cell death and inflammation during obesity: “Know my methods, WAT(son).” Cell Death Differ 30:279–292. https://doi.org/10.1038/s41418-022-01062-4
Holzer-Geissler JCJ, Schwingenschuh S, Zacharias M, Einsiedler J, Kainz S, Reisenegger P et al (2022) The impact of prolonged inflammation on wound healing. Biomedicines 10(4):856–866. https://www.mdpi.com/2227-9059/10/4/856. Accessed 17 May 2022
Author information
Authors and Affiliations
Contributions
Mai Chan: Conceptualization, Methodology, Software. Mai Chan, Pinar Avsar, Zena Moore, Declan Patton: Data curation, Writing- Original draft preparation. Pinar Avsar, Zena Moore, Declan Patton, Deborah McNamara, Tom O`Connor: Supervision. Mai Chan, Pinar Avsar: Software, Validation. Pinar Avsar, Zena Moore, Declan Patton, Deborah McNamara, Tom O`Connor: Writing- Reviewing and Editing.
Corresponding author
Ethics declarations
Conflict of interest
We declare that we have no conflict of interest statement.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The first author name was corrected.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chan, M.S., Moore, Z., Patton, D. et al. A systematic review of patient risk factors for complications following stoma formation among adults undergoing colorectal surgery. Int J Colorectal Dis 38, 238 (2023). https://doi.org/10.1007/s00384-023-04523-5
Accepted:
Published:
DOI: https://doi.org/10.1007/s00384-023-04523-5