Abstract
Purpose
This study aimed to evaluate the feasibility and safety of laparoscopic resection of abdominal neuroblastoma by comparing operative and long-term oncologic outcomes between open and laparoscopic surgeries.
Methods
This single-center retrospective study included patients who underwent laparoscopic tumor resection, between January 2000 and June 2021, with a maximum tumor diameter of ≤ 60 mm and without image-defined risk factors (IDRFs) at surgery. Data from 35 abdominal neuroblastoma resections were reviewed and compared between the laparotomy and laparoscopic groups.
Results
Nineteen patients underwent laparotomy and 16 had laparoscopic tumor resection. All laparoscopic surgeries achieved complete resection without conversion to open surgery. Median blood loss was significantly lower in the laparoscopic group (0.6 mL/kg) than in the laparotomy group (8.4 mL/kg) (P < 0.0001). There were two locoregional recurrences in the laparoscopic group and two metastatic recurrences in the laparotomy group. Five-year overall survival was 93.8% in both groups.
Conclusion
Laparoscopic resection of abdominal neuroblastomas in children is a feasible and safe procedure for tumors ≤ 60 mm in diameter with no IDRFs at surgery, with long-term outcomes equivalent to laparotomy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Surgical resection of neuroblastoma plays an important role in local control and the prompt transition to subsequent treatments [1, 2]. As laparoscopic surgery is generally associated with rapid recovery and is less invasive than laparotomy, laparoscopic neuroblastoma resection has gradually become a common procedure [3, 4]. A few retrospective studies have compared laparoscopic and open surgeries for abdominal neuroblastomas in small cohorts [2, 5, 6], but the backgrounds of the two groups differed in tumor size [5, 6]. Moreover, because most laparoscopic surgeries have been performed in recent years with relatively shorter follow-up periods [2, 6], long-term oncologic outcomes cannot be validated precisely.
Since 2009, image-defined risk factors (IDRFs) have been introduced by the International Neuroblastoma Risk Group (INRG) Taskforce to predict the surgical risks of localized neuroblastoma [7, 8]. It has been reported that neuroblastoma without IDRFs was associated with a significantly lower risk of surgical complications [1, 9]; since there is no encasement of vessels, tumor dissection from the surrounding tissues can be performed using standard laparoscopic procedures. Beginning in January 2000, laparoscopic resection of abdominal neuroblastoma has been performed at our hospital. This is the first study to evaluate the feasibility and safety of laparoscopic resection of neuroblastoma, by comparing operative and long-term oncologic outcomes with open resection of neuroblastoma with the same tumor characteristics.
Methods
This was a retrospective study conducted at Osaka Women’s and Children’s Hospital in Japan. In our hospital, the use of the laparoscopic approach was determined by the attending surgeons, taking into account the availability of staff expertise for pediatric laparoscopic surgery. For tumors with a maximum tumor diameter of ≤ 60 mm and without image-defined risk factors (IDRFs) at surgery, some attending surgeons selected the laparoscopic approach for the neuroblastoma tumor. Between January 2000 and July 2021, 34 children underwent resection of abdominal neuroblastoma with a maximum tumor diameter of ≤ 60 mm and no IDRFs at the time of surgery. Laparoscopic resection of the neuroblastoma was performed using three to five ports. Preoperative clinical data and intraoperative and postoperative results of these patients were retrospectively reviewed using medical charts. Preoperative clinical data included tumor location, tumor size, tumor volume, INRG staging system, and laparotomy history. Tumor size was evaluated based on the largest diameter as assessed using the latest preoperative computed tomography (CT). The tumor volume was calculated based on the length, width, and depth of the tumor from cross-sectional imaging using the following formula to calculate ellipsoid volume: π/6 × length × width × depth. IDRFs were defined according to the original Monclair report published in 2009 [7]. According to a new guideline for assessing IDRFs published in 2011 [10], tumor contact with renal vessels is considered IDRF positive. In the present study, tumor contact with renal vessels was considered IDRF-negative, and thus only tumor encasement of renal vessels was considered IDRF-positive. Intraoperative and postoperative outcomes included operative time, intraoperative bleeding amount, need for blood transfusion, time to start postoperative feeding, postoperative complications, and oncologic outcomes, such as relapse and mortality. The clinical factors and operative and oncologic outcomes of the laparotomy and laparoscopic groups were compared.
Continuous data are expressed as medians with interquartile range values. Group comparisons were analyzed using Fisher’s exact test, Mann–Whitney U test, or Welch’s t test, accordingly. Long-term results (disease-free survival, overall survival, and locoregional recurrence) were analyzed using Kaplan–Meier analysis and log-rank test. All analyses were performed using GraphPad Prism 8 (GraphPad Software, Inc., San Diego, CA, USA). Statistical significance was set at P < 0.05.
Results
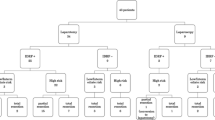
Within the 34-patient study group, there were 19 resections performed by laparotomy and 16 resections performed laparoscopically (one patient in the laparoscopic group had bilateral neuroblastomas). Comparisons of patient characteristics between the laparotomy and laparoscopic groups are shown in Table 1. There were no significant differences between the laparotomy and laparoscopic groups in sex, age at surgery, weight at surgery, history of surgery, primary tumor site, the largest diameter of the tumor, tumor volume, presence of contact with renal vessels, INRG staging system, and INRG risk group. Neoadjuvant chemotherapy was performed for nine patients in the laparotomy group and three in the laparoscopic group. Three IDRF-positive cases (L2) were effectively treated with neoadjuvant chemotherapy and were found to be IDRF-negative at the time of surgery.
All patients in the laparoscopic group underwent complete resection without open conversion. Comparisons of the operative and oncologic outcomes between the laparotomy and laparoscopic groups are shown in Table 2. The median blood loss was significantly lower in the laparoscopic group (0.6 mL/kg) than in the laparotomy group (8.4 mL/kg) (P < 0.0001). There were no significant differences in the operative time and need for blood transfusions between the laparotomy and laparoscopic groups. One patient in the laparotomy group had an abdominal incisional hernia; however, no intra- or postoperative complications (greater than Grade II severity, according to the Clavien–Dindo classification) were observed in either group. The median time to start postoperative feeding was significantly shorter in the laparoscopic group (1 day) than in the laparotomy group (2 days) (P = 0.001). The median follow-up periods were 160 and 69 months in the laparotomy and laparoscopic groups, respectively (P = 0.053). During the follow-up period, locoregional recurrence was observed in two cases in the laparoscopic group. One local recurrence occurred 17 months after secondary resection for a contralateral right tumor in a patient with bilateral neuroblastoma, and one regional lymph node recurrence occurred 5 months after surgery. There were two metastatic recurrences in the laparotomy group. Five-year overall survival was 93.8% in both groups (P = 0.759) (Fig. 1).
One patient in the laparotomy group died 13 months after surgery due to intracranial hypertension caused by central nervous system metastases. Another patient in the laparotomy group died 74 months after surgery due to fibrous pericarditis caused by treatment-related renal failure. In addition, one patient in the laparoscopic group died 10 months after surgery due to pneumonia caused by chronic graft-versus-host disease. All of these patients were classified into the high-risk group. Patients in the very-low to intermediate-risk groups, in both the laparotomy and laparoscopic groups, were still alive at the last follow-up.
Discussion
Laparoscopic resection is not suitable for all abdominal neuroblastomas, because achieving complete resection is dependent on tumor size and relationship with the surrounding organs and vessels. Our criteria for laparoscopic resection were a tumor size ≤ 60 mm in its largest diameter and no IDRFs at the time of surgery. Therefore, we selected neuroblastoma cases using these criteria to compare the operative and oncologic outcomes of the two different surgical approaches.
Previous studies on laparoscopic resection for neuroblastoma have focused on the tumor size and the presence of vascular encasement [2,3,4,5,6, 9, 11, 12]. The maximum tumor size that can be treated using laparoscopic excision remains unclear. Laparoscopic surgery was thought to be effective only for adrenal neuroblastomas with diameters of < 20 mm [11]. With improvements in surgical instruments and clinical experience with laparoscopic surgery, the use of this approach for neuroblastoma resection has gradually increased. Some reports have supported laparoscopic excision for abdominal neuroblastomas of ≤ 40–60 mm [2,3,4,5,6, 9, 12, 13]. In this study, all patients underwent successful laparoscopic resection with a tumor size ≤ 60 mm in its largest diameter. These results are consistent with those of previous studies. However, as Kawano et al. claimed that tumor size was significantly related to patient height [4], further study may be required to assess the consideration of patient height as an indicator of tumor size and procedure selection. Additionally, in this study, the maximum tumor volume in the laparoscopic group was 63.5 mL. Gabra et al. recently reported that tumor volume > 75 mL is a risk factor for conversion and complications according to the International Society of Pediatric Oncology Europe Neuroblastoma Surgeons Group (SIOPEN) multicentric study of data for patients with neuroblastoma who underwent laparoscopic neuroblastoma resection between 2005 and 2018 [14]. These findings support our results.
The primary indication for laparoscopic resection of abdominal neuroblastomas may be the absence of vascular encasement [2, 6, 9]. In the present study, although none of the cases had IDRFs (vascular encasement) at surgery, 50% of the laparoscopic cases had tumor contact with the renal vessels. As the laparoscopic group had no operative complications, including renal infarction or open conversion, contact of the tumor with renal vessels might be considered as an inclusion criterion for the indication of laparoscopic neuroblastoma resection. However, Tanaka et al. [9] demonstrated that two of their five cases involving tumor contact with renal vessels developed partial renal infarction, and the other cases with deformation or subtotal encasement of the inferior vena cava by the tumor resulted in open conversions. Vascular encasement should be avoided for laparoscopic neuroblastoma resection, however, a prospective study is needed to determine the indication of the laparoscopic approach in tumors with renal vessel contact.
In the present study, one patient in the laparoscopic group had an IDRF (encasement of the renal artery) at diagnosis. The disappearance of his IDRF was achieved with the use of neoadjuvant chemotherapy. He safely underwent laparoscopic resection with no intraoperative or postoperative complications. However, it has been reported that Stage L2 tumors (IDRF present at diagnosis) may have a potential risk for surgical complications, even after IDRF reduction by neoadjuvant chemotherapy [14, 15]. Therefore, laparoscopic resection in these cases should be performed carefully to avoid surrounding organ or vessel injury to structures that may be adherent to the tumor due to chemotherapeutic effects.
Our results demonstrated that the amount of bleeding was significantly lower in the laparoscopic group than in the laparotomy group. We theorize that dissection and the identification of vascular injury were performed more precisely during laparoscopic surgery because of the laparoscope’s magnification. Additionally, compression by pneumoperitoneum insufflation can minimize the oozing of blood. Our data support the advantages of laparoscopic surgery in terms of decreasing the amount of bleeding, as demonstrated by Shirota et al. [2].
Another advantage of laparoscopic surgery may be its reduced invasiveness and rapid recovery [3]. Our results demonstrated a significantly shorter time to start postoperative feeding in the laparoscopic group. Moreover, all patients in the laparoscopic group started oral feeding within two days after surgery. These results were supported by the previous study by Shirota et al. [2]. Motivated by these findings, laparoscopic neuroblastoma resection may contribute to the rapid transition to subsequent cancer treatment.
Two locoregional recurrences occurred in the laparoscopic group. One patient developed regional lymph node recurrence five months after surgery, although there were no swollen lymph nodes preoperatively. Meanwhile, local recurrence occurred in a patient with bilateral neuroblastoma and trisomy 2p at the secondary resection site 17 months after laparoscopic tumor resection. Pederiva et al. reported that bilateral neuroblastomas are extremely rare and are represented by synchronous primaries or contralateral metastases of a unilateral tumor [16]. When the contralateral right tumor was a result of metastasis of the left tumor, it was not considered local recurrence but metastatic recurrence. Therefore, the main factors associated with local recurrence could not be identified.
Strengths of this study include the reporting of data on long-term outcomes. Since all patients in the very- low to intermediate-risk groups were alive during the follow-up period, outcomes in these risk groups may be excellent regardless of the surgical approach. Also, in contrast to previous comparative studies [5, 6], similar backgrounds in terms of tumor size and IDRFs at surgery were assigned to both groups in the present study. Moreover, the criteria for laparoscopic neuroblastoma resection in our hospital are considered appropriate and generally accepted according to previous reports [2, 4,5,6, 9].
This study had some limitations, however. First, selection bias could not be excluded because of the single-center retrospective design. Second, the number of patients in each group was small. There were only six high-risk patients in the laparotomy group and two in the laparoscopic group. Therefore, further comparative studies between laparotomy and laparoscopic approaches for abdominal neuroblastoma in high-risk groups are required to better assess their long-term outcomes.
Conclusion
In this study, complete laparoscopic resection of neuroblastoma was successful in all cases, without intraoperative and postoperative complications or conversion to open surgery, with less blood loss and a shorter time to start postoperative feeding than laparotomy. We conclude that laparoscopic resection of abdominal neuroblastomas in children is a feasible and safe procedure, with long-term outcomes equivalent to those of laparotomy for the resection of tumors ≤ 60 mm in diameter with no IDRFs at the time of surgery.
Data Availability
The data that support the fndings of this study are available from the corresponding author, M.Z., upon reasonable request.
References
Yoneda A, Nishikawa M, Uehara S, Oue T, Usui N, Inoue M, Fukuzawa M, Okuyama H (2016) Can image-defined risk factors predict surgical complications in localized neuroblastoma? Eur J Pediatr Surg 26:117–122. https://doi.org/10.1055/s-0035-1566100
Shirota C, Tainaka T, Uchida H, Hinoki A, Chiba K, Tanaka Y (2017) Laparoscopic resection of neuroblastomas in low- to high-risk patients without image-defined risk factors is safe and feasible. BMC Pediatr 17:71. https://doi.org/10.1186/s12887-017-0826-8
Iwanaka T, Kawashima H, Uchida H (2007) The laparoscopic approach of neuroblastoma. Semin Pediatr Surg 16:259–265. https://doi.org/10.1053/j.sempedsurg.2007.06.008
Kawano T, Souzaki R, Sumida W, Shimojima N, Hishiki T, Kinoshita Y, Uchida H, Tajiri T, Yoneda A, Oue T, Kuroda T, Hirobe S, Koshinaga T, Hiyama E, Nio M, Inomata Y, Taguchi T, Ieiri S (2021) Current thoracoscopic approach for mediastinal neuroblastoma in Japan-results from nationwide multicenter survey. Pediatr Surg Int 37:1651–1658. https://doi.org/10.1007/s00383-021-04998-9
Yao W, Dong K, Li K, Zheng S, Xiao X (2018) Comparison of long-term prognosis of laparoscopic and open adrenalectomy for local adrenal neuroblastoma in children. Pediatr Surg Int 34:851–856. https://doi.org/10.1007/s00383-018-4294-5
Kelleher CM, Smithson L, Nguyen LL, Casadiego G, Nasr A, Irwin MS, Gerstle JT (2013) Clinical outcomes in children with adrenal neuroblastoma undergoing open versus laparoscopic adrenalectomy. J Pediatr Sur 48:1727–1732. https://doi.org/10.1016/j.jpedsurg.2013.03.056
Monclair T, Brodeur GM, Ambros PF, Brisse HJ, Cecchetto G, Holmes K, Kaneko M, London WB, Matthay KK, Nuchtern JG, von Schweinitz D, Simon T, Cohn SL, Pearson AD (2009) The international neuroblastoma risk group (INRG) staging system: an INRG task force report. J Clin Oncol 27:298–330. https://doi.org/10.1200/JCO.2008.16.6876
Cohn SL, Pearson AD, London WB, Monclair T, Ambros PF, Brodeur GM, Faldum A, Hero B, Iehara T, Machin D, Mosseri V, Simon T, Garaventa A, Castel V, Matthay KK (2009) The international neuroblastoma risk group (INRG) classification system: an INRG task force report. J Clin Oncol 27(2):289–297. https://doi.org/10.1200/JCO.2008.16.6785
Tanaka Y, Kawashima H, Mori M, Fujiogi M, Suzuki K, Amano H, Morita K, Arakawa Y, Koh K, Oguma E, Iwanaka T, Uchida H (2016) Contraindications and image-defined risk factors in laparoscopic resection of abdominal neuroblastoma. Pediatr Surg Int 32:845–850. https://doi.org/10.1007/s00383-016-3932-z
Brisse HJ, McCarville MB, Granata C, Krug KB, Wootton Gorges SL, Kanegawa K, Giammarile F, Schmidt M, Shulkin BL, Matthay KK, Lewington VJ, Sarnacki S, Hero B, Kaneko M, London WB, Pearson AD, Cohn SL, Monclair T (2011) Guidelines for imaging and staging of neuroblastic tumors: consensus report from the international neuroblastoma risk group project. Radiology 261:243–257. https://doi.org/10.1148/radiol.11101352
Yamamoto H, Yoshida M, Sera Y (1996) Laparoscopic surgery for neuroblastoma identified by mass screening. J Pediatr Surg 31:385–388. https://doi.org/10.1016/s0022-3468(96)90743-5
Simon T, Haberle B, Hero B, von Schweinitz D, Berthold F (2013) Role of surgery in the treatment of patients with stage 4 neuroblastoma age 18 months or older at diagnosis. J Clin Oncol Off J Am Soc Clin Oncol 31:752–758. https://doi.org/10.1200/JCO.2012.45.9339
de Campos Vieira Abib S, Chui CH, Cox S, Abdelhafeez AH, Fernandez-Pineda I, Elgendy A, Karpelowsky J, Lobos P, Wijnen M, Fuchs J, Hayes A, Gerstle JT (2022) International society of paediatric surgical oncology (IPSO) surgical practice guidelines. Ecancermedicalscience 16:1356. https://doi.org/10.3332/2Fecancer.2022.1356
Gabra HO, Irtan S, Cross K, Lobos P, Froeba-Pohl A, Pio L, Virgone C, Guillén Burrieza G, Gómez Chacón Villalba J, Riccipetitoni G, Guérin F, Nightingale M, Heloury Y, Faraj S, Leclair M, Scalabre A, Mattioli G, Warmann SW, Fuchs J, Basta N, Bjørnland K, Matthyssens LE, Losty PD, Sarnacki S (2022) Minimally invasive surgery for neuroblastic tumours: a SIOPEN multicentre study: proposal for guidelines. Eur J Surg Oncol 48:283–291. https://doi.org/10.1016/j.ejso.2021.08.013
Yoneda A, Nishikawa M, Uehara S, Oue T, Usui N, Inoue M, Fukuzawa M, Okuyama H (2016) Can neoadjuvant chemotherapy reduce the surgical risks for localized neuroblastoma patients with image-defined risk factors at the time of diagnosis? Pediatr Surg Int 32:209–214. https://doi.org/10.1007/s00383-016-3858-5
Pederiva F, Andres A, Sastre A, Alves J, Martinez L, Tovar JA (2007) Bilateral adrenal neuroblastoma is different. Eur J Pediatr Surg 17:393–396. https://doi.org/10.1055/s-2007-965811
Acknowledgements
We would like to thank Editage (http://www.editage.com) for English language editing.
Funding
No funds, Grants, or other support were received.
Author information
Authors and Affiliations
Contributions
All authors contributed to the conception and design of the study. Data collection and analysis were performed by MZ. The first draft of the manuscript was written by MZ. The draft was reviewed and edited by NU, and all authors commented on the second version of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Study approval was granted by the institutional review board (IRB) of Osaka Women’s and Children’s Hospital (IRB number: 1567).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zenitani, M., Yoshida, M., Matsumoto, S. et al. Feasibility and safety of laparoscopic tumor resection in children with abdominal neuroblastomas. Pediatr Surg Int 39, 91 (2023). https://doi.org/10.1007/s00383-023-05371-8
Accepted:
Published:
DOI: https://doi.org/10.1007/s00383-023-05371-8