Abstract
Introduction
This study aimed to highlight that atlantoaxial rotatory fixation (AARF) can be related to neurosurgery procedures in children, with an afterward demonstration of good results after halo-gravity traction and C1–C2 stabilization using the Harms technique.
Case description
To the best of our knowledge, this is the first case to report a 4-year-old boy who presented with AARF after a posterior fossa craniotomy to treat a cerebellar astrocytoma. At our medical facility, AARF was diagnosed using plain radiography and computed tomography imaging. The patient was treated with continuous cranial traction for 14 days. Initially, we detected that the patient had no C1 posterior arch or C2 spinous process; therefore, the best option was to perform the Harms technique. Postoperatively, the patient was placed in a cervical collar for 4 weeks. At the 4-year postoperative follow-up, the patient was doing well and had not developed any complications.
Conclusion
Herein, we report a case in which AARF can be developed after neurosurgical procedure. Surgical techniques used for atlantoaxial subluxation should be carefully selected. In our case, the Harms technique after cranial traction was an excellent option for correcting and stabilizing the abnormal neck position. However, further studies are required to determine the best technique to use in the pediatric population.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
AARF is characterized by cervical pain and limited neck motion. It was first described by Bell in 1930 and classified by Fielding and Hawkins in 1977 into four types according to the severity of displacement and the anterior or posterior position of the atlas in relation to the axis [1]. This condition has also been reported in patients following otorhinolaryngological or head and neck surgeries and those with disorders such as rheumatoid arthritis, Down syndrome, and Morquio syndrome [2,3,4,5,6]. To the best of our knowledge, this is the first case of AARF associated with postoperative complications following neurosurgery.
Case presentation
History
A 4-year-old boy was admitted to our medical facility with a complaint of abnormal neck position since he had undergone surgery of the posterior fossa for excision of a cerebellar astrocytoma 5 months earlier under the care of another medical facility. The patient was in a prone position on a horseshoe headrest, and it is worth noting that the other medical team reported no surgical or positioning accident. The patient was treated as if he had torticollis or muscle contractions.
Examination and diagnosis
The patient presented with left anterior fixed rotation of the neck, also known as the Cock Robin position, and limited rotation, flexion, extension, and lateralization of the cervical spine. The patient had no neurological deficits or cervical pain.
Three-dimensional computed tomography (CT) showed a type 3, left, anterior, and fixed atlantoaxial rotatory subluxation according to the Fielding and Hawkins classification (Fig. 1A) and C2–C3 subluxation. The posterior arch of the atlas (C1), spinous process, and part of the C2 lamina were surgically removed (Fig. 1B). Due to the craniovertebral instability and the uncertain risk of the dynamic X-ray maneuvers, the diagnosis was based solely on the CT scan.
Presence of AARF condition. Three-dimensional computed tomography of the cervical spine demonstrating a type 3, left, anterior, fixed atlantoaxial rotatory subluxation. C2–C3 subluxation is also evident, without any commitment of neurovascular structures (A). Previous removal of the posterior arch of the atlas (C1), spinous process, and part of the C2 lamina can be seen (B)
Halo-gravity traction
Immediately after diagnosis, the patient was placed in continuous cranial halo traction, either in a walker or an adapted bed (Fig. 2A). Traction began at 2 kg and was increased by 250 g every 2 days. On the 14th day, we observed the alignment of the neck position, and radiography showed reduced joint subluxation and distraction between the posterior elements of C1 and C2 (Fig. 2B). The patient initially received analgesics, and over time, he tolerated the traction very well even without analgesics.
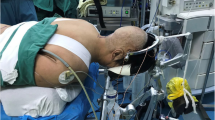
Performance of halo-gravity traction. Radiography of the cervical spine demonstrates the presence of a halo traction device, placed immediately after diagnosis of AARF to perform continuous cranial traction (A). Patient during the treatment with a halo traction walker (B). Radiography of the cervical spine after 14 days shows neck position alignment and reduction of joint subluxation and distraction between the posterior elements of C1 and C2 (C). AARF, atlantoaxial rotatory fixation. (C) Postoperative plain radiography showing atlantoaxial fixation using the Goel and Harms technique, which consists of C1–C2 stabilization with polyaxial screws and rods. The cervical spine appears satisfactorily aligned after hardware placement comprising C1–C2
Operation and postoperative course
On the 15th day, C1–C2 stabilization was performed using the Harms technique (Fig. 2C). The absence of C1–C2 posterior elements precluded using any posterior cervical wiring technique. We chose to perform only decortication of the C1–C2 articular surfaces because of insufficient bone exposure.
On postoperative day 2, the patient was discharged, used a Philadelphia collar for 4 weeks, and underwent a further investigation of collagen disorders and other medical conditions, but nothing was found. He showed progress after 3 months without cervical pain or any other complaint, except for limited head rotation. Radiological follow-up with plain radiographs alone is recommended because it has a much lower patient dose than CT [7]. Comparing the preoperative (Fig. 3A) and postoperative (Fig. 3B) images, we observed a reduction in the abnormal neck position presented previously. Eight years postoperatively, the patient did not present with any new deformities and maintained atlantoaxial stability (Fig. 4).
Postoperative images of the patient 8 years after surgery. The patient presents no deformities in the coronal plane (A) and adequate atlantoaxial fusion in the transoral anteroposterior image (B). In the lateral view, no new deformities in the sagittal plane are seen, and atlantoaxial stability is seen in the neural (C), extension (D), and flexion (E) images
Discussion
To the best of our knowledge, this is the first case of AARF associated with postoperative complications following neurosurgery. As his parents affirmed that they noted the abnormal position of his head immediately after the surgery, we hypothesized that he developed the C1–C2 subluxation during any step of the cranial procedure.
The atlantoaxial joint is a unique articulation that is the cornerstone of the upper cervical spine and allows a large degree of head rotation. However, attempts to establish diagnostic criteria for AARF have not yet been successful because such pathological rotation occurs within the physiological range of motion [4].
The atlantoaxial joint is responsible for 60% of cervical rotation, the atlantooccipital joint for 5–10%, and the remaining rotation is shared by the subaxial segments [3]. The pathological definition of AARF is not described by the static angular relationship between C1 and C2; however, in the abnormal form, C1 is related to C2 during the movement cycles in axial rotation [3].
Part III of Pang and Li’s study of AARF [8] describes a slight tendency for younger children to have a more severe C1–C2 interlock, and the severity was related to the length of pretreatment time, although this difference was not statistically significant.
We performed continuous cranial traction because such treatment aims to stabilize the joint and stimulate normal sagittal and coronal alignment before arthrodesis, eventually avoiding adverse events [9].
In the only prospective study on AARF [8], a subsequent C1–C2 fusion was performed in patients whose condition was refractory to conservative treatment or irreducible to halo traction. Pang and Li [8] also reported a high recurrence rate of chronic AARF, mainly of type 3 of Fielding and Hawkings, and considered this to be associated with conservative treatment involving the long-term use of a halo vest; therefore, we decided to perform surgery. Because our patient had no C1 posterior arch or C2 spinous process, fusion using transarticular screws or the Goel and Laheri [10] and Harms and Melcher technique [11] would be an option with C1 lateral mass and C2 pedicle screws. This was the treatment of choice, followed by the use of a cervical collar for 4 weeks.
Conclusion
Early diagnosis and treatment prevent the development of AARF; however, when this condition settles, surgical treatment is indicated, potentially preceded by traction using a cranial halo. Finally, the surgical technique to be used in each case should be carefully selected, considering the anatomical and bone conditions as well as the surgeon’s experience with each technique.
Data availability
Not applicable.
Materials availability
Not applicable.
References
Fielding J, Hawkins R (1977) Atlanto-axial rotatory fixation. (Fixed rotatory subluxation: JBJS. J Bone Joint Surg 59:37–44
Tauchi R, Imagama S, Ito Z et al (2014) Atlantoaxial rotatory fixation in a child after bilateral otoplastic surgery. Eur J Orthop Surg Traumatol : Orthop Traumatol 24 Suppl 1. https://doi.org/10.1007/S00590-013-1254-6
Pang D, Li V (2004) Atlantoaxial rotatory fixation: part 1–biomechanics of normal rotation at the atlantoaxial joint in children. Neurosurgery 55:614–625. https://doi.org/10.1227/01.NEU.0000134386.31806.A6
Kelly EJ, Herbert KJ, Crotty EJ, O’Connor TPF (1998) Atlantoaxial subluxation after otoplasty. Plast Reconstr Surg 102:543–544. https://doi.org/10.1097/00006534-199808000-00040
Meza Escobar L, Osterhoff G, Ossendorf C et al (2012) Traumatic atlantoaxial rotatory subluxation in an adolescent: a case report. J Med Case Rep 6. https://doi.org/10.1186/1752-1947-6-27
Deichmueller CMC, Welkoborsky HJ (2010) Grisel’s syndrome–a rare complication following “small” operations and infections in the ENT region. Eur Arch Otorhinolaryngol 267:1467–1473. https://doi.org/10.1007/S00405-010-1241-Z
Don S (2004) Radiosensitivity of children: potential for overexposure in CR and DR and magnitude of doses in ordinary radiographic examinations. Pediatr Radiol 34 Suppl 3. https://doi.org/10.1007/S00247-004-1266-9
Pang D, Li V (2005) Atlantoaxial rotatory fixation: part 3-a prospective study of the clinical manifestation, diagnosis, management, and outcome of children with alantoaxial rotatory fixation. Neurosurgery 57:954–971. https://doi.org/10.1227/01.NEU.0000180052.81699.81
Ahmed R, Traynelis VC, Menezes AH (2008) Fusions at the craniovertebral junction. Childs Nerv Syst 24:1209–1224. https://doi.org/10.1007/S00381-008-0607-7
Goel A, Laheri V (1994) Plate and screw fixation for atlanto-axial subluxation. Acta Neurochir (Wien) 129:47–53. https://doi.org/10.1007/BF01400872
Harms J, Melcher RP (2001) Posterior C1-C2 fusion with polyaxial screw and rod fixation. Spine (Phila Pa 1976) 26:2467–2471. https://doi.org/10.1097/00007632-200111150-00014
Author information
Authors and Affiliations
Contributions
Vinicius de Meldau Benites: Conceptualization, writing the original draft, data acquisition, editing, and reviewing. Marcos Devanir Silva da Costa: Review and editing. Sergio Cavalheiro: Supervision, review, and editing.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Research Ethics Committee of the Universidade Federal de São Paulo, São Paulo, Brazil. Informed consent was obtained from all the guardians.
Consent for publication
Informed consent was obtained from the guardians for publication.
Conflict of interest
No competing interests to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
de Meldau Benites, V., da Costa, M.D.S. & Cavalheiro, S. Posterior C1–C2 fusion for atlantoaxial rotatory fixation after posterior fossa craniotomy in a 4-year old: a case report. Childs Nerv Syst 39, 1647–1651 (2023). https://doi.org/10.1007/s00381-023-05862-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-023-05862-y