Abstract
Congenital orbital teratomas are rare entities with few case reports detailing their prenatal and perinatal imaging features. We present the case of a congenital orbital teratoma initially detected as cystic lesion on prenatal ultrasound, with foetal and postnatal imaging showing evolution of characteristic MRI appearances. Knowledge of these appearances and the ability to diagnose these rare entities in foetal life can aid management and operative planning in the immediate postnatal period.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Teratomas are congenital tumours derived from the three germ layers. Although rare, the orbit is a recognised location for congenital teratoma [1].
Case report
We present a case of a congenital orbital teratoma, initially discovered as an incidental cystic lesion in the right orbit during antenatal ultrasound scan.
A foetal MRI performed at 27 weeks of gestation demonstrated a large, thin-walled, and well-defined cystic lesion within the right orbit, causing significant proptosis of the globe, stretching of the extraocular muscles and optic nerve, expansion, and remodelling of the bony orbit (Fig. 1A–C). At this time point, there were no visible septations, solid components, fat, or blood products demonstrated. The intracranial and the left orbital structures were normal.
A follow-up foetal MRI study was performed at 36 weeks of gestational age. This demonstrates significant structural changes of the cystic lesion in the right orbit, with reduction in the degree of proptosis, interval development of septations, and multiple small solid components posterior to the globe (Fig. 2A, B).
Post-processed 3D super-resolution-reconstructed (SRR) images were performed for both foetal MRI scans which provided further information regarding the transformation of the cyst between the 9 weeks interval, especially providing a clear overview of the volume of the lesion in relation to the whole head. This was particularly useful information during multidisciplinary meetings for delivery plan and also for parental counselling.
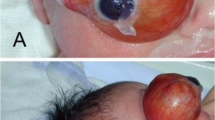
The baby was subsequently delivered via caesarean section at 38 weeks, with multidisciplinary assistance at birth, including obstetric, anaesthetic, and ophthalmology support to ensure maximal preservation of the affected eye (Fig. 3). On day 2 of life, approximately 7mls of straw-coloured fluid was sampled. At day 8 of life, a contrast-enhanced MRI head was performed with dedicated orbital sequences. This demonstrates a further reduction in the degree of proptosis and an increase in solid components, which showed contrast enhancement following gadolinium administration. Furthermore, T1-weighted fat-saturated images show regions of signal dropout within the orbital lesion consistent with macroscopic fat (Fig. 4A–D). The lesion was confined to the orbit with no evidence of any intracranial extension.
A–D T1-weighted images with (A and B) and without fat-saturation (C and D) demonstrate areas of signal dropout (arrows) within the right orbit consistent with macroscopic fat components. T1 fat-saturated post-contrast image demonstrates multiple solid enhancing components within the orbit. The degree of proptosis, and size of the cystic component, has reduced since the prenatal MRI imaging
At day 9 of life, exenteration was performed, with removal of the globe and excision of the orbital lesion as a single specimen. The orbital cavity was markedly expanded and distorted, with bony remodelling and widening of the optic canal.
Pathology examination (Fig. 5) revealed a firm grey tumour measuring approximately 3.5 cm in diameter, containing cystic and solid elements. The histology confirmed presence of mature tissue representing embryonic layers ectoderm, mesoderm, and endoderm. These included patches of mature neuroglial tissue, mesenchymal tissue comprising adipose and cartilage tissue, skin adnexal structures, and intestinal-type tissue. There were no immature elements or features of malignancy noted. The overall features are consistent with that of a mature (benign) cystic teratoma. The exenterated right eye showed no significant pathology.
Pathology confirming a mature benign cystic teratoma. A Macroscopic cut section showing a multi-loculated lesion with cystic change (asterisk) and surrounding solid elements. The lesion appears to be well contained within the peripheral inked resection margins. B Low magnification histology section of the lesion approximately representing the macroscopic image (A), showing cystic (asterisk) and solid elements. The solid part contained mature tissue derivatives from all three germ layers—ectoderm, mesoderm, and endoderm. C–F Higher magnification histology images showing neuroglial tissue (C), mesenchymal tissue (D) comprising cartilage (right) and adipose (left) tissue, skin adnexal structures including hair follicles (E), and intestinal-type epithelium (F). Other tissue such as collection of ganglionic cells, peripheral nerve, and skeletal muscle tissue were also present (not shown). There was no immature element noted. There is no evidence of malignancy
There were no immediate perioperative complications, and the patient went on to have oculoplastic reconstruction which is currently ongoing (Fig. 6).
One year post-operative clinical photo demonstrating right periocular rehabilative status. The lids are comprised of orbicularis and skin only but will require further reconstruction. The posterior socket has been reconstructed from dermis fat grafts, which are now supporting a clear prosthetic shell. A painted prosthetic will be custom made for her. Further micro-fat pearl grafting will be performed to reduce facial asymmetry
Discussion
Teratomas are congenital germ cell tumours composed of all three germ cell layers (endoderm, ectoderm, mesoderm). Histopathological classification characterise as either mature teratoma, composed of fully differentiated cell types, or immature teratoma, containing undifferentiated tissues. Whereas mature teratomas generally behave as a benign tumour after complete resection, immature teratomas follow a more aggressive course with a greater propensity for recurrence [2].
This case posed a diagnostic challenge due to the findings of a large, thin-walled, and well-defined cystic orbital mass on initial MRI imaging, with no suggestion of solid, fatty, or haemorrhagic components at 27 weeks of gestation. The differential for these appearances is wide and includes congenital orbital cysts, venolymphatic malformations, and rare entities such as optic nerve sheath meningoceles [3]. The rapid metamorphosis from an orbital cystic lesion in foetal life, to the development of solid and enhancing components postnatally, has recently been reported separately [4], and this finding may reflect the natural history of orbital teratomas. This case demonstrates this transformation in utero, highlighting the importance of in utero MR imaging follow-up in the presence of undefined orbital cystic lesion, to improve diagnostic accuracy, to assist on parental counselling, and to guide for birth planning. Furthermore, this case highlights the importance of utilising dedicated postnatal MR orbital protocol, including the use of pre- and post-contrast T1-weighted images, both with and without fat saturation, to allow detection of macroscopic fat, a key feature of germ cell tumours.
Availability of data and materials
Not applicable.
References
Ahnoux-Zabsonre A, Sanou J, Lankoandé YF, Bouda C, Méda G, Lamien-Sanou A (2020) Prenatal exophthalmia revealing a postnatal orbital teratoma. Case Rep Ophthalmol Med 13(2020):1597353. https://doi.org/10.1155/2020/1597353
Mann JR, Gray ES, Thornton C, Raafat F, Robinson K, Collins GS, Gornall P, Huddart SN, Hale JP, Oakhill A (2008) UK children’s cancer study group experience. Mature and immature extracranial teratomas in children: the UK children’s cancer study group experience. J Clin Oncol 26(21):3590–3597. https://doi.org/10.1200/JCO.2008.16.0622
Pahwa S, Sharma S, Das CJ, Dhamija E, Agrawal S (2015) Intraorbital cystic lesions an imaging spectrum. Curr Probl Diagn Radiol 44(5):437–448. https://doi.org/10.1067/j.cpradiol.2015.03.003. (Epub 2015 Mar 17)
Moré GHM, Vieira J, Akaishi PMS, Cruz AAV (2020) Orbital teratoma MRI changes from fetal life to exenteration. Ophthalmic Plast Reconstr Surg 36(2):e58–e59. https://doi.org/10.1097/IOP.0000000000001430
Author information
Authors and Affiliations
Contributions
All the authors have made substantive contributions to the article and assume full responsibility for its content.
Corresponding author
Ethics declarations
Ethical approval
This is a retrospective case report, and ethical approval was not required. Parental consent was obtained for article submission and for permission to use the provided photographs.
Conflict of interest
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wheeler, M., Pergoretti, K., Gore, S. et al. Congenital orbital teratoma: A case report with foetal presentation. Childs Nerv Syst 38, 2217–2221 (2022). https://doi.org/10.1007/s00381-022-05576-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-022-05576-7