Abstract
During cardiac operations, weaning from cardiopulmonary bypass (CPB) may prove challenging as a result of superimposed acute right ventricular dysfunction in the setting of elevated pulmonary vascular resistance (PVR). The aim of this study was to retrospectively evaluate the effect of inhaled milrinone versus inhaled iloprost in patients with persistent pulmonary hypertension following discontinuation of CPB. Eighteen patients with elevated PVR post-bypass were administered inhaled milrinone at a cumulative dose of 50 μg kg−1. These patients were retrospectively matched with 18 patients who were administered 20 μg of inhaled iloprost. Both drugs were administered through a disposable aerosol-generating jet nebulizer device and inhaled for a 15-min period. Hemodynamic measurements were performed before and after cessation of the inhalation period. Both inhaled milrinone and inhaled iloprost induced significant reductions in mean pulmonary artery pressure and PVR and significant increases in cardiac index in patients with post-CPB pulmonary hypertension. The favorable effect of both agents on the pulmonary vasculature was confirmed by echocardiographic measurements. Both agents were devoid of systemic side effects, since mean arterial pressure and systemic vascular resistance were not affected. A decrease in intrapulmonary shunt by inhalation of both agents was also demonstrated. Pulmonary vasodilatation attributed to iloprost seems to be of greater magnitude and of longer duration as compared to that of inhaled milrinone. Both substances proved to be selective pulmonary vasodilators. The greater magnitude and of longer duration vasodilatation attributed to iloprost may be due to its longer duration of action.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pulmonary hypertension (PH) can occur after cardiac surgery and is mainly associated with the pulmonary endothelial inflammatory response to extracorporeal circulation [1]. Therefore, weaning from cardiopulmonary bypass (CPB) may prove particularly challenging as a result of superimposed acute right ventricular dysfunction in the setting of the elevated pulmonary vascular resistance (PVR). The risk is particularly high in patients undergoing heart valve surgery. In this patient population, preexisting PH can be further exacerbated by the endothelial dysfunction induced by CPB, thus increasing patients’ morbidity and mortality [2, 3].
In this context, several pharmacologic agents have been used to reduce the occurrence of PH post-CPB [4]. Intravenous vasodilators (such as nitrates or prostaglandins) attenuate PH, but associated systemic hypotension with escalating dosage due to lack of pulmonary selectivity is the limiting factor [5]. Furthermore, hypoxemia may occur with intravenous agents due to worsening of intrapulmonary shunt caused by inhibition of hypoxic pulmonary vasoconstriction and indiscriminate vasodilatation of both ventilated and non-ventilated alveoli [6]. On the contrary, agents administered by inhalation seem to selectively target the pulmonary circulation, thus effectively decreasing pulmonary arterial pressure without causing systemic hypotension [7]. In the past, inhaled nitric oxide was advocated as a selective pulmonary vasodilator. However, there are major drawbacks to its use. Nitric oxide can be a highly toxic molecule due to the production of methemoglobin and higher oxides of nitrogen and, therefore, specialized monitoring as well as close vigilance with repeated measurements of concentration is required [8]. Moreover, sophisticated delivery systems may make application difficult and significant financial investment in administration is mandatory. Finally, some patients are non-responders, whereas in strong responders, there is a risk of rebound pulmonary hypertension when administration is abruptly withdrawn, which can worsen right ventricular dysfunction [9]. Therefore, research in recent years has been directed towards alternative inhaled agents for the management of PH, such as inhaled iloprost and inhaled milrinone. For both agents, there have been reports of their use in the context of post-CPB PH, with encouraging results [10,11,12,13].
The aim of this study was to retrospectively evaluate the effect of inhaled milrinone versus inhaled iloprost on hemodynamic and oxygenation parameters in patients with valvular heart disease and preoperative PH who underwent elective cardiac surgery and who presented with persistent PH following discontinuation of CPB. Both agents were administered after weaning from extracorporeal circulation in an attempt to manage post-CPB elevation of pulmonary arterial pressure and to prevent the occurrence of acute right ventricular failure.
Methods
Study population
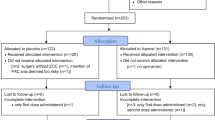
After approval by the Hospital’s Ethics Committee, the authors retrospectively reviewed the files of patients with preoperatively diagnosed severe PH, subjected to elective cardiac operations from March 2011 until June 2014. Patients were considered to have severe PH if systolic pulmonary arterial pressure (SPAP) was greater than 55 mmHg or mean pulmonary arterial pressure (MPAP) was greater than 25 mmHg, as estimated by preoperative transthoracic or transesophageal echocardiography. Full intraoperative hemodynamic and echocardiographic data were available for 48 patients with severe PH. Inclusion criteria for the retrospective analysis were a post-bypass MPAP > 25 mmHg and post-bypass PVR > 200 dyn s cm−5 from the readings of a pulmonary artery catheter at the initial attempt of discontinuation from CPB. From the files of patients examined, the authors identified 18 patients who fulfilled inclusion criteria and in whom inhaled iloprost was administered after cessation of extracorporeal circulation to treat PH. These patients were retrospectively matched for type of operation with patients who had also presented with post-bypass PH and in whom inhaled milrinone had been administered to treat elevated pulmonary arterial pressure post-bypass. Patients’ written informed consent had been obtained from all patients preoperatively for administration of either drug. All patients were free of comorbidities that could affect the occurrence of pulmonary hypertension, such as thromboembolic disease, chronic obstructive pulmonary disease, or renal and liver disease, thus ensuring that elevated pulmonary pressure was exclusively due to left heart pathology. Exclusion criteria from the retrospective analysis were a left ventricular ejection fraction of less than 35% and emergency or redo surgery.
Anesthesia, monitoring, and surgery
On the morning of the operation, patients received their regular doses of cardiac medications. Premedication, monitoring, and anesthesia and mechanical ventilation were standardized. Apart from the standard monitoring including a pulmonary artery catheter, a multifrequency 2.9- to 8-MHz transesophageal echocardiography probe was placed in the patients’ esophagus after induction for transoesophageal echocardiography monitoring. The presence of PH was confirmed by the pulmonary artery catheter after anesthetic induction. At separation from CPB, a low dose of dobutamine (3–5 μg kg min−1) was commenced in both groups with the aim to support both ventricles and to achieve a predefined goal of hemodynamic stability of cardiac index (CI) of ≥2.5 L min−1 m−2.
Inhaler administration protocol
Inhaled milrinone or iloprost was administered through a jet nebulizer device for aerozol generation (Aeroneb Pro Micropump Nebulizer, Aerogen Ltd, Galway, Ireland) attached to the ventilatory circuit, near the endotracheal tube. The concentration of milrinone used in the inhaled milrinone group was 1 mg mL−1 and the cumulative dose administered was 50 μg kg−1. Iloprost concentration was 10 μg mL−1 and administered at a cumulative dose of 20 μg. Duration of administration for both agents was 15 min approximately (Fig. 1).
Data measurements
Variables measured or calculated included CI, measured in triplicate by the thermodilution method, mean arterial pressure (MAP), MPAP, right atrial pressure (RAP), pulmonary capillary wedge pressure (PCWP), transpulmonary pressure gradient (TPG), systemic vascular resistance (SVR), and PVR. PVR/SVR and MPAP/MAP ratios were also calculated. The intrapulmonary shunt fraction (IPSF) was calculated using a standard formula.Footnote 1 For the echocardiographic evaluation of right ventricular function, tricuspid annular systolic velocity (TAVsyst) and tricuspid annular plane systolic excursion (TAPSE) were used as surrogates. TAVsyst was obtained in the four-chamber view, using the pulse-wave tissue Doppler and colour-coded tissue Doppler imaging protocol, while the maximal velocity at the tricuspid valve annulus during the ejection phase of the right ventricular was measured. The sample volume was placed at the junction of the right ventricular free wall and the anterior leaflet of the tricuspid valve. TAPSE was also measured in the four-chamber view as the distance between the end-diastolic and end-systolic position of the outer port of the tricuspid annulus. Additional parameters examined included the need for use of further inotropic or vasopressor support post-CPB, a requirement for reinitiation of CPB or for use of intraaortic balloon pump as well as Intensive Care Unit (ICU) stay and hospital stay.
Hemodynamic measurements were performed after discontinuation of CPB and before inhalation (T 0), 20 min after the start of inhalation (T 1), 40 min after the start of inhalation (T 2), and 60 min after the start of inhalation (T 3). TAVsyst was evaluated at T 0 and T 2 timepoints.
Statistical analysis
Sample size calculation was based on expected changes in MPAP post-inhalation, as these had been demonstrated in a previous study by our team [10]. We estimated that approximately 16 patients should be included in each group to detect a difference of 30% in MPAP post-inhalation between the two groups with a power of 0.80 an alpha error of 0.05. Variables were tested for normality of distributions with the Kolmogorov–Smirnov test. Comparisons of numeric data between the two groups were performed with the unpaired t test or the Wilcoxon rank sum test for independent samples, depending on whether the variables followed a normal or non-normal distribution. The Chi-square test or Fisher’s exact test as appropriate was used for comparisons of categorical data. Echocardiographic comparisons within the same group were performed with the paired t test. Hemodynamic variables over time were analyzed with two-factor mixed design analysis of variance with repeated measures for one factor (time). The two factors were the inhaled agent group and time. If a significant effect was found, post-hoc comparisons were carried out to assess at which timepoint the two groups were different. Results are expressed as mean ± SD or as median (25th–75th percentiles) depending on normality of distributions and as frequency for categorical variables. A value of p < 0.05 was considered as statistically significant. Data were analyzed with the SigmaPlot for Windows v.11.0 statistical software (Systat Software, Inc., San Jose, CA).
Results
Demographic, preoperative, and intraoperative characteristics of the two groups are presented in Table 1 and were similar between groups. Median patient age was 73.5 (range 50–83 years) and all patients included in the retrospective analysis underwent mitral valve replacement with mitral stenosis as primary indication for surgery in 23 patients and mitral regurgitation in the remaining 13 patients. Of the 36 patients analyzed, 10 patients underwent concurrent aortic valve replacement due to grade III–IV aortic regurgitation and 13 patients underwent coronary artery bypass surgery due to coexisting coronary artery disease. All patients presented with preoperative severe PH, with SPAP 74.7 ± 13.4 mmHg.
At weaning from extracorporeal circulation, all patients presented evidence of severe PH, with MPAP 41.1 ± 4.2 mmHg and PVR 376 ± 94 dyn s cm−5. On echocardiographic examination, echocardiographic evidence of impaired right ventricular function (such as global or localised hypokinesis of the free right ventricular wall combined with right ventricular distension or increasing tricuspid insufficiency) was also present [14]. The high MPAP and the echocardiographic indices of right ventricular decompensation were the cut-off point for the inhaled agent administration on top of the standard dobutamine support. The effect of inhaled agents on hemodynamic parameters is presented in Table 2. Baseline (T 0) hemodynamic values were comparable between the two groups. Both agents induced selective pulmonary dilatation with a reduction of MPAP at the end of the inhalation period in comparison with baseline (T 1). The reduction in MPAP was still evident for both agents 40 and 60 min after the start of the inhalation (T 2 and T 3, respectively). However, at T 2 and T 3, the effect of inhaled iloprost on MPAP was more prominent.
A decrease in PVR was also observed, which was longer acting for inhaled iloprost, as patients of this group presented reduced PVR in comparison with baseline even 1 h after the start of inhalation, while in the inhaled milrinone group, PVR values at T 3, although lower, were no significantly different from baseline. In a direct comparison, no differences in the degree of pulmonary vasodilatation induced by either agent were observed, except for T 3, where PVR were significantly lower in the inhaled iloprost group in comparison with the inhaled milrinone group.
MPAP/MAP ratios were found to decrease significantly over time as compared to baseline in both groups. Forty and 60 min after the start of inhalation, MPAP/MAP ratios in the inhaled iloprost group were lower in comparison with the inhaled milrinone group (Fig. 2). Similarly, PVR/SVR ratios decreased over time in both groups. However, in the inhaled iloprost group, the decrease in PVR/SVR ratio was evident for the whole period of observation, whereas in the inhaled milrinone group, PVR/SVR ratio returned to baseline values 60 min after the start of inhalation being significantly higher as compared to the inhaled iloprost group (Fig. 3). TPG also decreased, although in the milrinone group, values were not significantly different from baseline 60 min after the start of inhalation. CI improved in both groups with increased values throughout the observation period in comparison with baseline, except for T 3 in the inhaled milrinone group, where CI was no longer different from baseline. No differences in CI were demonstrated between the two groups apart from the end of the observation period (T 3), where CI was significantly higher in the inhaled iloprost group as compared to the inhaled milrinone group. Systemic blood pressure (MAP) and vascular resistance (SVR) were not affected by either agent. Finally, IPSF was reduced by the inhalation of both agents in comparison with baseline with no significant differences between the two groups at any timepoint (Table 2). As far as echocardiography is concerned, TAVsyst and TAPSE increased in both groups 40 min after commencement of inhaler administration (Table 2; Fig. 4).
A second period of CPB was required for one patient in the inhaled iloprost group and two patients in the inhaled milrinone group. These patients were successfully weaned thereafter with support by an increase in dobutamine dose (7 μg kg min−1). Two patients in the inhaled iloprost group and four patients in the inhaled milrinone group required the addition of noradrenaline during transfer to ICU with gradual discontinuation of vasopressor support afterwards. No patient required the insertion of an intraaortic balloon pump. In both groups, there were repeated sessions of the inhaled agent during the patients’ stay in the ICU, especially during the first 24 h, to deal with episodes of elevated PVR occurring postoperatively. The requirement for repeated sessions of iloprost administration was less frequent for iloprost than for milrinone. Moreover, differences in time from end of CPB to extubation, ICU stay, and hospital stay were not significantly different between groups and there was not in-hospital mortality in the patients studied.
Discussion
According to our results, both inhaled milrinone and inhaled iloprost proved to be selective pulmonary vasodilators in patients with post-CPB PH, since they induced significant reductions in MPAP, PVR, and TPG and significant increases in CI. The favorable effect of both agents on the pulmonary vasculature was confirmed by both hemodynamic and echocardiographic measurements. At the same time, both agents were devoid of systemic side effects, since MAP and SVR were not affected. These facts were confirmed by the calculation of MPAP/MAP ratios and PVR/SVR ratios over time in both groups. Improvement in oxygenation as expressed by a decrease in intrapulmonary shunt by inhalation of both agents was also demonstrated. Notably, pulmonary vasodilatation attributed to iloprost seems to be of greater magnitude and of longer duration as compared to that of inhaled milrinone.
The systemic inflammatory response induced by extracorporeal circulation is manifested as increased pulmonary capillary permeability, decreased pulmonary compliance and elevated PVR, which compromises right ventricular work and may ultimately lead to acute right ventricular decompensation [15, 16]. Patients with mitral valve disease who develop PH due to the chronic increase of left atrial pressure and pulmonary vascular remodeling are particularly prone to the risk of exacerbation of PH and development of acute ventricular dysfunction post-CPB [3, 17, 18]. Over the years, intravenous vasodilators have been used to decrease the incidence of post-CPB PH, but the lack of pulmonary selectivity limits their applicability, since the invariably ensuing systemic hypotension not only compromises the systemic circulation but also may further exacerbate right ventricular coronary perfusion and performance [19]. Therefore, pulmonary vasodilators administered by inhalation have become more popular in this context because of the theoretical advance of systemic circulation preservation.
Our findings regarding the use of the two inhaled agents are consistent with previous studies in animals and humans. All patients participating in the present study presented with hemodynamic evidence of elevated PVR at weaning from CPB as well as echocardiographic evidence of imminent impairment of right ventricular performance (low TAVsyst and TAPSE). We demonstrated selective pulmonary vasodilatation and improved indices of right ventricular function on echocardiography by both inhaled iloprost and inhaled milrinone, while both agents were devoid of significant side effects on the systemic circulation. To the best of our knowledge, the two inhaled agents have not been compared before in experimental or clinical settings.
Inhaled prostanoids are among the pharmacologic interventions that have been used aiming at targeting post-CPB pulmonary hypertension [7]. Iloprost is a stable prostacyclin analog, whose delivery via aerosolization caused selective vasodilatation of the pulmonary vasculature, sparing the systemic circulation both in primary and secondary PH contexts [20,21,22,23,24]. On the other hand, milrinone increases myocardial and vascular smooth muscle cyclic AMP (c-AMP) concentration through inhibition of phosphodiesterase III, acting as an inodilator [25]. Its delivery through the intravenous route has previously been shown to ameliorate ventricular dysfunction and facilitate separation from CPB [26]. However, the high incidence of systemic hypotension associated with its intravenous administration often requires support of the systemic circulation by vasoactive agents [27]. In this light, inhalation of milrinone was proposed as an alternative route of administration with its first description by Haraldsson et al. in postcardiac surgical patients with PH [28]. Ever since, there have been several reports of its use in experimental and clinical settings [13, 29,30,31].
The fact that, according to our results, the pulmonary vasodilatation achieved by inhaled iloprost was of greater magnitude as compared to that achieved by inhaled milrinone could be due to several reasons; first, in the current study, our practice was to administer milrinone after separation from CPB. In a previous study that compared pre- to post-CPB inhaled milrinone administration, pre-CPB inhaled milrinone was shown to be more advantageous in comparison with post-CPB inhalation, since patients exposed to milrinone before extracorporeal circulation presented lower MPAP as compared to when administration occurred after CPB [13]. The former group also presented a lower need for use of an intraaortic balloon pump, reinitiation of CPB or requirement for inotropic support following separation from extracorporeal circulation. This most possibly shows that the administration of inhaled milrinone before CPB may be more effective in preventing the reperfusion syndrome associated with the perfusion pump, since a more uniform distribution of the drug can be achieved when the lungs are still mechanically ventilated and have not been subjected to CPB-related atelectases that could diminish milrinone’s favorable action [32]. Similarly, in another study, it was shown that preoperative delivery of inhaled milrinone in cardiac surgical patients was capable of attenuating the inflammatory response to CPB [33]. Therefore, post-CPB inhalation of milrinone, as in our study, may provide a temporary relief of PH but may not be able to induce a more sustained vasodilatory response, which probably would have been the case if it had been administered preoperatively or prior to the initiation of CPB.
Another reason for the more sustained pulmonary vasodilatation in the inhaled iloprost group observed in our study could also be the longer duration of action of inhaled iloprost, which has been shown to last up to 120 min [20]. In addition, other yet unknown mechanisms affecting vascular remodeling may be involved in ensuring iloprost’s sustained beneficial effects, even after the cessation of its administration and may not be related merely to vasodilatation [34]. Inhaled iloprost has also been found to increase the clearance of endothelin in the pulmonary circulation, an effect also possibly related to its sustained beneficial effects [35].
The effect of inhaled iloprost on the CI was also of greater magnitude as compared to that of inhaled milrinone. Apart from the effect on the pulmonary vasculature which favorably affects cardiac output, direct positive inotropic effects for iloprost have been documented in experimental and in vitro studies [36]. However, it remains unclear whether these effects are clinically significant.
As far as inhaled milrinone is concerned and consistent with the results of our report, in the Haraldsson study, twenty min after milrinone inhalation, patients’ hemodynamic values returned to baseline, indicating that inhaled milrinone was effective but rather short-acting [28]. Similarly, the effect of inhaled milrinone was rather short-living in the Sablotzki study, since 30 min after termination of milrinone inhalation, MPAP had returned to baseline values [30]. In addition, in a recent multicentre trial, the intraoperative use of inhaled milrinone as compared to placebo in high risk cardiac surgical patients with PH resulted in modest hemodynamic benefits that did not translate into improvement of clinically relevant endpoints [37]. Although that study might have been underpowered as the authors suggested, the effect of inhaled milrinone is likely to be small. Perhaps, alternative modalities of administration, such as different dosing schemes or repeated inhalation sessions should be explored to achieve more sustained hemodynamic benefits. Co-aerolization could also be an option since there are promising reports in experimental and clinical settings showing effectiveness of combined therapy in attenuating PH to a greater degree than sole administration of each factor [28, 38]. Perhaps a combined approach might be advantageous by targeting multiple sites of action, namely the milrinone-mediated c-AMP pathway and iloprost-related endothelin clearance, since levels of endothelin-1 have been shown to correlate with postoperative complications after cardiac surgery [39].
A favorable effect of both agents on intrapulmonary shunts was observed, which is in accordance with experimental and clinical studies on PH that demonstrated improvement in oxygenation by inhalation of both inhaled iloprost and milrinone [32, 40]. This is due to the fact that delivery of these agents through inhalation produces selective vasodilatation of pulmonary vessels adjacent to well-ventilated areas, thus leading to better matching of ventilation/perfusion and decrease of intrapulmonary shunt.
Finally, regarding cost concerns in our study, although inhaler milrinone is slightly cheaper than inhaler iloprost, iloprost’s slightly higher cost may not be a major drawback, since there was a requirement for less frequent sessions of inhaled iloprost postoperatively due to its more sustained duration of action.
Our study has a few limitations. First, it was a retrospective unblinded non-controlled study and based on a small and rather not homogeneous cohort of patients. Although we observed a tendency for a lower rate of CPB reinitiation or for a reduced requirement of vasoactive drugs in the inhaled iloprost group, meaningful conclusions regarding clinically relevant outcomes cannot be reached by small retrospective studies. Furthermore, the more sustained hemodynamic effect of inhaled iloprost did not translate into shorter ICU and hospital stay, but the study was not powered to detect clinically relevant endpoints. Second, although the dosage of iloprost was within the range of the available literature, the optimal dosage for milrinone is not as well defined. We opted for a dose of 50 μg kg−1 which is based on personal experience and is in accordance with previous reports [13, 28, 30]. This dose might, however, still be low for a sustained hemodynamic effect. Perhaps, a higher dose could have resulted in more prominent effects and a comparison of different dosing schemes could be the subject of a future study. A third limitation might be considered the fact that since dobutamine has itself vasodilating properties, one could argue that its effects cannot be easily isolated from the inhaled agents. However, as mentioned before, our group of patients presented hemodynamic and echocardiographic signs of right ventricular deterioration despite dobutamine support and required the addition of the inhaler agent on top of the standard low-dose dobutamine regime. Finally, aerosol delivery of the inhaled drug makes it rather difficult to determine the exact dose of the agent reaching the alveolar space [41]. However, the delivery system we used is based on a vibrating mesh nebulizer, which is capable of producing a fine particle aerosol of consistently sized droplets and ensures deep lung deposition [42]. Moreover, consistency in mechanical ventilation with tidal volumes of ≥500 mL ensured that the dead space was cleared of aerosol, which improved drug delivery to the lower respiratory tract. In addition, slow inspiratory flow rates (40 L min−1) ensured long inspiratory times which, in turn, increased lung deposition at the intended site of action. Therefore, in spite of potential drug wastage in the nebulizer chamber, endotracheal tubing and ventilator, the use of the same system for delivery of both agents in addition to standardized mechanical ventilation settings ensured consistency between the two groups.
In conclusion, according to the results of the present retrospective study performed on a small group of patients, the administration of a specific dosing scheme of inhaled iloprost or inhaled milrinone at weaning from extracorporeal circulation resulted in selective pulmonary vasodilatation in patients with post-CPB PH following mitral valve surgery. The favorable effects of inhaled iloprost on right ventricular afterload were more pronounced and of longer duration as compared to those of inhaled milrinone. This is probably due to the fact that post-CPB administration of inhaled mirinone is not as effective as its pre-CPB administration. Alternatively, the more sustained effect of iloprost on the pulmonary circulation can be attributed to its longer duration of action. The more pronounced hemodynamic effects of inhaled iloprost and potential implications for clinical outcomes remain to be further elucidated in larger randomized trials.
Notes
For the calculation of intrapulmonary shunt fraction (IPSF) we used the formula Qs/Qt = CcO2-CaO2/CcO2-CvO2 by obtaining arterial and mixed venous blood gas measurements. (CcO2 = pulmonary capillary oxygen content; CaO2 = arterial oxygen content; CvO2 = mixed venous oxygen content). The alveolar gas equation was used to derive pulmonary capillary oxygen tension and pulmonary capillary blood was assumed to be fully saturated since FiO2 was > 0.21.
References
Ng CS, Wan S, Yim AP, Arifi AA (2002) Pulmonary dysfunction after cardiac surgery. Chest 121:1269–1277
Denault AY, Haddad F, Jacobsohn E, Deschamps A (2013) Perioperative right ventricular dysfunction. Curr Opin Anaesthesiol 26:71–81
Briongos Figuero S, Moya Mur JL, García-Lledó A, Centella T, Salido L, Aceña Navarro Á, García Martín A, García-Andrade I, Oliva E, Zamorano JL (2016) Predictors of persistent pulmonary hypertension after valve placement. Heart Vessel 31:1091–1099
Denault A, Deschamps A, Tardif JC, Lambert J, Perrault L (2010) Pulmonary hypertension in cardiac surgery. Curr Cardiol Rev 6:1–14
Schmid ER, Bürki C, Engel MH, Schmidlin D, Tornic M, Seifert B (1999) Inhaled nitric oxide versus intravenous vasodilators in severe pulmonary hypertension after cardiac surgery. Anesth Analg 89:1108–1115
Radermacher P, Santak B, Wüst HJ, Tarnow J, Falke KJ (1990) Prostacyclin for the treatment of pulmonary hypertension in the adult respiratory distress syndrome: effects on pulmonary capillary pressure and ventilation-perfusion distributions. Anesthesiology 72:238–244
De Wet CJ, Affleck DG, Jacobsohn E, Avidan MS, Tymkew H, Hill LL, Zanaboni PB, Moazami N, Smith JR (2004) Inhaled prostacyclin is safe, effective, and affordable in patients with pulmonary hypertension, right heart dysfunction, and refractory hypoxemia after cardiothoracic surgery. J Thorac Cardiovasc Surg 127:1058–1067
Tsukahara H, Ishida T, Mayumi M (1999) Gas-phase oxidation of nitric oxide: chemical kinetics and rate constant. Nitric Oxide 3:191–198
Miller OI, Tang SF, Keech A, Celermajer DS (1995) Rebound pulmonary hypertension on withdrawal from inhaled nitric oxide. Lancet 346:51–52
Theodoraki K, Rellia P, Thanopoulos A, Tsourelis L, Zarkalis D, Sfyrakis P, Antoniou T (2002) Inhaled iloprost controls pulmonary hypertension after cardiopulmonary bypass. Can J Anaesth 49:963–967
Sablotzki A, Czeslick E, Gruenig E, Friedrich I, Schubert S, Börgermann J, Hentschel T (2003) First experiences with the stable prostacyclin analog iloprost in the evaluation of heart transplant candidates with increased pulmonary vascular resistance. J Thorac Cardiovasc Surg 125:960–962
Denault AY, Lamarche Y, Couture P, Haddad F, Lambert J, Tardif JC, Perrault LP (2006) Inhaled milrinone: a new alternative in cardiac surgery? Semin Cardiothorac Vasc Anesth 10:346–360
Lamarche Y, Perrault LP, Maltais S, Tétreault K, Lambert J, Denault AY (2007) Preliminary experience with inhaled milrinone in cardiac surgery. Eur J Cardiothorac Surg 31:1081–1087
Amano H, Abe S, Hirose S, Waku R, Masuyama T, Sakuma M, Toyoda S, Taguchi I, Inoue T, Tei C (2017) Comparison of echocardiographic parameters to assess right ventricular function in pulmonary hypertension. Heart Vessel. doi:10.1007/s00380-017-0991-6
Dávila-Román VG, Waggoner AD, Hopkins WE, Barzilai B (1995) Right ventricular dysfunction in low output syndrome after cardiac operations: assessment by transesophageal echocardiography. Ann Thorac Surg 60:1081–1086
Strumpher J, Jacobsohn E (2011) Pulmonary hypertension and right ventricular dysfunction: physiology and perioperative management. J Cardiothorac Vasc Anesth 25:687–704
Vincens JJ, Temizer D, Post JR, Edmunds LH Jr, Herrmann HC (1995) Long-term outcome of cardiac surgery in patients with mitral stenosis and severe pulmonary hypertension. Circulation 92(9 Suppl):II137–II142
Magne J, Pibarot P, Sengupta PP, Donal E, Rosenhek R, Lancellotti P (2015) Pulmonary hypertension in valvular disease: a comprehensive review on pathophysiology to therapy from the HAVEC Group. JACC Cardiovasc Imaging 8:83–99
Goldstein JA (2002) Pathophysiology and management of right heart ischemia. J Am Coll Cardiol 40:841–853
Olschewski H (2009) Inhaled iloprost for the treatment of pulmonary hypertension. Eur Respir Rev 18:29–34
Kramm T, Eberle B, Guth S, Mayer E (2005) Inhaled iloprost to control residual pulmonary hypertension following pulmonary endarterectomy. Eur J Cardiothorac Surg 28:882–888
Rex S, Schaelte G, Metzelder S, Flier S, de Waal EE, Autschbach R, Rossaint R, Buhre W (2008) Inhaled iloprost to control pulmonary artery hypertension in patients undergoing mitral valve surgery: a prospective, randomized-controlled trial. Acta Anaesthesiol Scand 52:65–72
Theodoraki K, Tsiapras D, Tsourelis L, Zarkalis D, Sfirakis P, Kapetanakis E, Alivizatos P, Antoniou T (2006) Inhaled iloprost in eight heart transplant recipients presenting with post-bypass acute right ventricular dysfunction. Acta Anaesthesiol Scand 50:1213–1217
Antoniou T, Prokakis C, Athanasopoulos G, Thanopoulos A, Rellia P, Zarkalis D, Kogerakis N, Koletsis EN, Bairaktaris A (2012) Inhaled nitric oxide plus iloprost in the setting of post-left assist device heart dysfunction. Ann Thorac Surg 94:792–798
Levy JH, Bailey JM, Deeb GM (2002) Intravenous milrinone in cardiac surgery. Ann Thorac Surg 73:325–330
Feneck RO, Sherry KM, Withington PS, Oduro-Dominah A, European Milrinone Multicenter Trial Group (2001) Comparison of the hemodynamic effects of milrinone with dobutamine in patients after cardiac surgery. J Cardiothorac Vasc Anesth 15:306–315
Jeon Y, Ryu JH, Lim YJ, Kim CS, Bahk JH, Yoon SZ, Choi JY (2006) Comparative hemodynamic effects of vasopressin and norepinephrine after milrinone-induced hypotension in off-pump coronary artery bypass surgical patients. Eur J Cardiothorac Surg 29:952–956
Haraldsson A, Kieler-Jensen N, Ricksten SE (2001) The additive pulmonary vasodilatory effects of inhaled prostacyclin and inhaled milrinone in postcardiac surgical patients with pulmonary hypertension. Anesth Analg 93:1439–1445
Gelvez J, Fakioglu H, Olarte JL, Soliz A, Totapally BR, Torbati D (2004) Effect of aerosolized milrinone during drug-induced pulmonary hypertension in lambs. Pharmacol Res 50:87–91
Sablotzki A, Starzmann W, Scheubel R, Grond S, Czeslick EG (2005) Selective pulmonary vasodilation with inhaled aerosolized milrinone in heart transplant candidates. Can J Anaesth 52:1076–1082
Haglund NA, Burdorf A, Jones T, Shostrom V, Um J, Ryan T, Shillcutt S, Fischer P, Cox ZL, Raichlin E, Anderson DR, Lowes BD, Dumitru I (2015) Inhaled milrinone after left ventricular assist device implantation. J Card Fail 21:792–797
Lamarche Y, Malo O, Thorin E, Denault A, Carrier M, Roy J, Perrault LP (2005) Inhaled but not intravenous milrinone prevents pulmonary endothelial dysfunction alter cardiopulmonary bypass. J Thorac Cardiovasc Surg 130:83–92
Gong M, Lin XZ, Lu GT, Zheng LJ (2012) Preoperative inhalation of milrinone attenuates inflammation in patients undergoing cardiac surgery with cardiopulmonary bypass. Med Princ Pract 21:30–35
Höper MM, Voelkel NF, Bates TO, Allard JD, Horan M, Shepherd D, Tuder RM (1997) Prostaglandins induce vascular endothelial growth factor in a human monocytic cell line and rat lungs via cAMP. Am J Respir Cell Mol Biol 17:748–756
Wilkens H, Bauer M, Forestier N, König J, Eichler A, Schneider S, Schäfers HJ, Sybrecht GW (2003) Influence of inhaled iloprost on transpulmonary gradient of big endothelin in patients with pulmonary hypertension. Circulation 107:1509–1513
Fassina G, Tessari F, Dorigo P (1983) Possible inotropic effect of a stable analogue of PGI2 and of PGI2 on isolated guinea pig atria. Mechanism of action. Pharmacol Res Commun 15:735–749
Denault AY, Bussières JS, Arellano R, Finegan B, Gavra P, Haddad F, Nguyen AQ, Varin F, Fortier A, Levesque S, Shi Y, Elmi-Sarabi M, Tardif JC, Perrault LP, Lambert J (2016) A multicentre randomized controlled trial of inhaled milrinone in high-risk cardiac surgical patients. Can J Anaesth 63:1140–1153
Laflamme M, Perrault LP, Carrier M, Elmi-Sarabi M, Fortier A, Denault AY (2015) Preliminary experience with combined inhaled milrinone and prostacyclin in cardiac surgical patients with pulmonary hypertension. J Cardiothorac Vasc Anesth 29:38–45
Dorman BH, Bond BR, Clair MJ, Walker CA, Pinosky ML, Reeves ST, Kratz JM, Zellner JL, Crumbley AJ 3rd, Multani MM, Spinale FG (2000) Temporal synthesis and release of endothelin within the systemic and myocardial circulation during and after cardiopulmonary bypass: relation to postoperative recovery. J Cardiothorac Vasc Anesth 14:540–545
Sawheny E, Ellis AL, Kinasewitz GT (2013) Iloprost improves gas exchange in patients with pulmonary hypertension and ARDS. Chest 144:55–62
Thomas SH, O’Doherty MJ, Fidler HM, Page CJ, Treacher DF, Nunan TO (1993) Pulmonary deposition of a nebulised aerosol during mechanical ventilation. Thorax 48:154–159
Dhand R (2002) Nebulizers that use a vibrating mesh or plate with multiple apertures to generate aerosol. Respir Care 47:1406–1416
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Theodoraki, K., Thanopoulos, A., Rellia, P. et al. A retrospective comparison of inhaled milrinone and iloprost in post-bypass pulmonary hypertension. Heart Vessels 32, 1488–1497 (2017). https://doi.org/10.1007/s00380-017-1023-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-017-1023-2