Abstract
Purpose
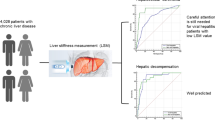
To retrospectively evaluate the prognostic role of liver stiffness (LS) measurement using magnetic resonance elastography (MRE) in patients with compensated chronic liver disease (cCLD).
Methods
We enrolled 217 patients with cCLD who underwent MRE. After mean follow-up of 45.0 ± 17.6 months, cumulative incidence (CI) of hepatocellular carcinoma (HCC) occurrence, development of decompensation and overall survival (OS) were estimated using the Kaplan-Meier method. Prognostic factors were evaluated using the Cox proportional hazard regression model.
Results
During the follow-up period, HCC occurred in 33 patients, and 1-, 3- and 5-year CIs of HCC occurrence were 3.8%, 14.8% and 18.9%, respectively. The LS value was a significant predictive factor for HCC occurrence [p < 0.001, hazard ratio (HR) = 1.59 per unit (1.25-2.03)]. Eighteen patients experienced hepatic decompensation, and 1-, 3- and 5-year CIs of decompensation were 2.8%, 7.3% and 11.3%, respectively. The LS value was also significantly associated with decompensation development [p < 0.001, HR = 2.02 per unit (1.37-2.98)]. Fourteen patients died, and 1-, 3- and 5-year OSs were 99.1%, 98.0% and 89.8%, respectively. The LS value was demonstrated to be a significant affecting factor for OS [p = 0.008, HR = 1.39 per unit (1.10-1.78)].
Conclusions
LS obtained from MRE was a significant predictive factor for the development of decompensation, HCC occurrence and OS in cCLD patients.
Key Points
• Liver stiffness (LS) values obtained from MRE can provide prognostic information.
• The LS value was a significant predictive factor for occurrence of hepatocellular carcinoma.
• The LS value was significantly associated with development of hepatic decompensation.
• Survival of compensated chronic liver disease patients was affected by the LS value.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Chronic liver disease caused by viral infections such as the hepatitis B and hepatitis C virus, alcoholic liver diseases and non-alcoholic fatty liver disease is a major health problem worldwide, which often leads to morbidity and mortality for those who contract this disease [1,2,3]. Furthermore, chronic liver disease can progress into liver cirrhosis as the end result of liver damage, which has also been demonstrated to be associated with significant morbidity and mortality [4, 5]. However, it is important to note that there are two distinct stages of cirrhosis with disparate clinical outcomes: compensated and decompensated cirrhosis [6]. Most of the morbidity and mortality in patients with chronic liver disease can be attributed to the transition from a compensated to a decompensated state, with the probability of developing into decompensation varying between 4% and 12% per year [7,8,9]. As a majority of deaths in patients with chronic liver disease are due to the progression into a decompensated state and the development of portal hypertension-related complications such as variceal bleeding and hepatorenal syndrome, identification of the risk factors that can predict the development of decompensation in patients with compensated chronic liver disease is of crucial importance. In addition, chronic liver disease and the presence of advanced fibrosis or cirrhosis are well-known risk factors for developing hepatocellular carcinoma (HCC), which is one of the most common malignant tumours and the third most common cause of cancer-related death worldwide [10, 11]. Therefore, assessment of the risk of developing HCC in patients with chronic liver disease is of critical importance for patient management, as it can allow the implementation of the most optimal preventive management strategies that may modify the disease course [12].
Liver stiffness (LS) measurement using transient elastography (TE) (Fibroscan; Echosense, Paris, France) has been confirmed to be an effective tool for the staging of liver fibrosis and the diagnosis of liver cirrhosis in patients with chronic liver disease [13,14,15]. In addition to the diagnosis of cirrhosis and the staging of liver fibrosis, the LS value obtained using TE can also be a significant predictive factor for both the development of hepatic decompensation [12, 16, 17] and the occurrence of HCC [18,19,20]. Another non-invasive method that has garnered attention is magnetic resonance elastography (MRE) of the liver typically used for the assessment of the viscoelastic properties of the liver [21, 22], which can be a successful quantitative method for the non-invasive diagnosis of liver cirrhosis as well as the staging of liver fibrosis [23, 24]. Indeed, several studies have shown that MRE can outperform TE for hepatic fibrosis staging and that it has better reproducibility for liver fibrosis [25,26,27]. In addition to 2D-MRE using gradient echo, which has been widely used in clinical practice, the LS value could also be measured by magnetisation tagged MRI, and spin-echo based MRE has been recently introduced and widened the applicability of MRE [28,29,30]. Indeed, MRE has also been feasible with 3-T MR systems, which have been gaining popularity nowadays [31]. Therefore, we hypothesised that the LS value obtained using MRE might also have the potential to provide important prognostic information in patients with chronic liver disease. Even though a previous study had reported that the LS value obtained using MRE was independently associated with decompensated liver disease [32], the prognostic role of MRE has not been fully evaluated, especially regarding HCC occurrence and the overall survival of patients with compensated chronic liver disease. Therefore, the purpose of our study was to retrospectively evaluate the prognostic role of the LS value obtained using MRE to predict the development of hepatic decompensation and the occurrence of HCC as well as overall survival in patients with compensated chronic liver disease.
Patients and methods
Patients
Our Institutional Review Board (IRB) approved this retrospective study and the requirement for written informed consent was waived. We examined all consecutive patients who underwent MRE at Seoul National University Hospital between January 2010 and December 2013. Most of the MRE examinations were performed in the outpatient setting and were requested at the physician’s discretion. The most common reasons for MRE examinations included the follow-up of known cirrhosis, evaluation of abnormal liver function tests and the assessment of a liver mass. The inclusion criteria of this study were as follows: (1) patients with chronic liver disease with Child-Pugh class A liver function without ascites; (2) no previous history of HCC treatment; (3) no previous history of hepatic decompensation (i.e., no previous history of variceal bleeding, spontaneous bacterial peritonitis, hepatic encephalopathy or hepatorenal syndrome) [7]; (4) no concomitant serious medical illness other than liver disease; (5) available follow-up medical records and/or imaging studies. Initially, we found 235 patients who underwent MRE examinations during the study period and had Child-Pugh class A liver function without a previous history of decompensation or HCC treatment. Among them, 11 patients were excluded for the following reasons: immediate follow-up loss after MRE examination (n = 3) and concomitant medical illness (congestive heart failure, n = 3; chronic renal failure with dialysis, n = 5). Seven additional patients were also excluded for suboptimal image quality of MRE owing to failure to generate a satisfactory mechanical wave through the abdomen. Finally, 217 patients comprised the study population. The baseline characteristics of the 217 patients are summarised in Table 1, and the laboratory tests were obtained within 6 months from MRE examination (mean interval, 6.5 days; range, 0 to 118 days). Among the 217 patients, 22 (10.1%) underwent liver biopsy to evaluate the aetiology of the liver disease within 6 months from the MRE examination.
MR elastography protocol and analysis
All liver MR imaging including MRE was obtained using a 1.5-T whole-body MR unit (Signa HDx; GE Healthcare, Milwaukee, WI) with an eight-channel torso phased-array coil centred over the liver. For 2D-MRE, a cylindrical passive longitudinal pneumatic actuator with 19-cm diameter and 1.5-cm thickness (MR-touch; GE Healthcare, Milwaukee, WI) was placed against the right anterior chest wall to generate 60-Hz vibrations; the detailed MRE parameters are provided in the supplementary data.
Two abdominal radiologists (DHL and WC with 9 years and 7 years of experience in liver MR and MRE, respectively) who were blinded to the clinical outcome measured the LS and spleen stiffness (SS) values using MRE (Fig. 1). Both radiologists first evaluated the image showing wave propagation to ensure generation of appropriate wave propagation, and detailed information regarding the measurement procedures is also given in the supplementary data.
An example showing the measurement of liver stiffness using MRE. a Anatomic imaging of a 56-year old male patient with chronic hepatitis B viral infection. b Confidence map of an elastogram. c Imaging showing wave propagation. d Free-drawn ROI excluding liver edge and large hepatic vessels placed on the elastogram
Follow-up for development of hepatic decompensation and HCC and for estimation of overall survival
The development of hepatic decompensation was defined as the occurrence of ascites, hepatic encephalopathy or variceal bleeding during the follow-up period [7, 32]. Surveillance for HCC was done in each patient with ultrasound (US) or contrast-enhanced computed tomography/MR every 3 or 6 months according to the patient’s risk of HCC development. HCCs were diagnosed based on the non-invasive criteria for the diagnosis of HCC defined by the European Association for the Study of the Liver (EASL) [33]. Overall survival was defined as the interval between the MRE examination and death or the last follow-up. Patients who underwent liver transplantations during the follow-up period after the MRE examination were censored from the study at the date of their transplantation.
Statistical analysis
The measurement reproducibility of the SS and LS values obtained from MRE between two readers was assessed by using intraclass correlation coefficients (ICCs) with their two-tailed p values. We considered an ICC value > 0.81 to indicate almost perfect agreement and values of 0.61-0.80, 0.41-0.60 and 0.21-0.40 to represent substantial, moderate and fair agreement, respectively.
The cumulative incidence of the development of hepatic decompensation and HCC occurrence was estimated using the Kaplan-Meier method. Univariate and multivariate analyses using the Cox proportional hazard regression model were performed to determine significant clinical and biological parameters predicting overall survival and the cumulative incidences of the development of decompensation and HCC occurrence. All statistical analyses were performed using SPSS version 23 (SPSS, Chicago, IL, USA). The optimal cut-off stiffness values obtained by MRE for predicting overall survival, development of hepatic decompensation and the occurrence of HCC were determined using the minimal p value approach based on the log-rank test statistic. For internal validation of the optimal cut-off stiffness values predicting overall survival, development of hepatic decompensation and the occurrence of HCC determined by the minimal p value approach, two-fold cross-validation was performed [34]. For the determination of the optimal cut-off stiffness value obtained by MRE and internal validation, we used SAS 9.2 version (SAS Institute Inc., Cary, NC, USA).
Results
LS and SS values obtained from MRE
LS values were successfully obtained from MRE examinations in 217 of 224 patients (96.9%, 217/224). Mean and median LS values obtained by MRE were 3.88 ± 1.81 kPa and 3.41 kPa, respectively, and ranged from 1.53 kPa to 11.5 kPa. Liver biopsy was done in 22 out of 217 patients, and the histopathological examination results, as well as LS and SS values obtained from MRE, were given in the supplementary data. Regarding the measurement reproducibility for LS value, the ICC was 0.986 [95% confidence interval (CI) = 0.982-0.990, p < 0.001], indicating almost perfect agreement. Mean and median SS values obtained by MRE were 5.52 ± 1.80 kPa and 5.32 kPa, respectively, and ranged from 1.80 kPa to 13.1 kPa. In terms of measurement reproducibility for the SS value, the ICC was 0.853 (95% CI, 0.849-0.857), also indicating almost perfect agreement.
Occurrence of HCC
During a mean and median follow-up period of 45.0 ± 17.6 months and 46.0 months, respectively, HCC occurred in 33 (15.2%) out of 217 patients. The estimated 1-, 3- and 5-year cumulative incidences of HCC occurrence were 3.8%, 14.8% and 18.9%, respectively (Fig. 2a). Predictive factors for the occurrence of HCC are summarised in Table 2. On multivariate analysis, patient age and LS values obtained by MRE [p < 0.001, hazard ratio (HR) = 1.59 per unit; 95% CI = 1.25-2.03] were revealed to be significant predictive factors for HCC occurrence in patients with compensated chronic liver disease. The optimal cut-off LS value to predict HCC occurrence was set at 4.44 kPa using the minimal p value approach with internally valid results (p < 0.001). The estimated 1-, 3- and 5-year cumulative incidences of HCC occurrence were 1.5%, 6.6% and 9.5% in 142 patients with LS values ≤ 4.44 kPa obtained by MRE, respectively, compared to 8.2%, 30.1% and 36.4%, respectively, in 75 patients with LS values greater than 4.44 kPa obtained by MRE. This difference was statistically significant (p < 0.001) (Fig. 2b).
Development of hepatic decompensation
During the follow-up period, hepatic decompensation developed in 18 (8.3%) out of 217 patients (occurrence of ascites in 12 patients and variceal bleeding in 6 patients). The estimated 1-, 3- and 5-year cumulative incidences of the development of decompensation were 2.8%, 7.3% and 11.3%, respectively (Fig. 3a). Predictive factors for the development of decompensation are summarised in Table 2. The LS value obtained by MRE was also revealed to be a significant predictive factor for the development of hepatic decompensation (p < 0.001, HR = 2.02 per unit; 95% CI = 1.37-2.98). The optimal cut-off LS value to predict the development of hepatic decompensation was set at 4.46 kPa using the minimal p value approach with internally valid results (p < 0.001). The estimated 1-, 3- and 5-year cumulative incidences of the development of decompensation were 0%, 0% and 1.8% in 143 patients with LS values ≤ 4.46 kPa obtained by MRE, respectively, compared to 8.3%, 20.6% and 26.5%, respectively, in 74 patients with LS values > 4.46 kPa obtained by MRE. This difference was statistically significant (p < 0.001) (Fig. 3b).
Overall survival outcomes
During the follow-up period, 14 out of 217 patients (6.5%) died, for which the cause of death was progression of HCC (n = 3), liver failure (n = 7), uncontrolled variceal bleeding (n = 3) and sepsis due to an upper arm infection (n = 1). In addition, 3 of the 217 patients (1.4%) underwent liver transplantations 14, 27 and 33 months after the MRE examination, respectively, due to persistent decompensation with liver failure (n = 2) and HCC (n = 1). The estimated 1-, 3- and 5-year overall survival rates after MRE examinations in the 217 patients with compensated chronic liver disease were 99.1%, 98.0% and 89.8%, respectively (Fig. 4a). Prognostic factors affecting overall survival are summarised in Table 3. The LS value obtained by MRE was shown to be a significant predictive factor for overall survival in patients with compensated chronic liver disease according to multivariate analysis (p = 0.008, HR = 1.39 per unit; 95% CI = 1.10-1.78) together with patient age. The optimal cut-off LS value to predict overall survival was set at 5.53 kPa using the minimal p value approach with internally valid results (p = 0.008) The estimated 1-, 3- and 5-year overall survival rates were 99.4%, 99.4% and 91.5% in 174 patients with LS values ≤ 5.53 kPa obtained by MRE, respectively, compared to 97.6%, 91.8% and 83.2%, respectively, in 43 patients with LS values > 5.53 kPa obtained by MRE. This difference was statistically significant (p = 0.005) (Fig. 4b).
Discussion
In our study, the LS value obtained from MRE was demonstrated to be a significant predictive factor for both the development of hepatic decompensation (p < 0.001, HR = 1.83 per unit; 95% CI = 1.34-2.49) and the occurrence of HCC (p < 0.001, HR = 1.46 per unit; 95% CI = 1.20-1.78) in patients with compensated chronic liver disease. In addition, the LS value obtained from MRE was revealed to be a significant factor affecting the patient’s overall survival (p = 0.006, HR = 1.40 per unit; 95% CI = 1.10-1.78). The optimal cut-off LS values measured using initial MRE in our study were set at 4.44 kPa for the occurrence of HCC, 4.46 kPa for the development of hepatic decompensation and 5.53 kPa for overall survival. Our study clearly showed that the LS values obtained from MRE can provide important prognostic information in patients with compensated chronic liver disease, i.e., increased LS values obtained from MRE can reflect the more advanced stage of fibrosis or the presence of cirrhosis. The presence of cirrhosis or advanced stage of fibrosis is a well-known risk factor for HCC occurrence as well as development of decompensation [33, 35].
Given that the risk and speed of the progression from fibrosis to compensated and decompensated cirrhosis define the prognosis in liver diseases, early detection of significant fibrosis using several non-invasive diagnostic tools and the application of preventive strategies is quite appealing as it can potentially improve the outcomes of patients with chronic liver disease [36]. Currently, TE has been the most widely used modality to assess the degree of liver fibrosis, and its diagnostic and prognostic values in patients with liver disease have been extensively evaluated and validated [13, 14, 37]. As an example, LS measurement using TE has been demonstrated to predict the risk of HCC occurrence [12, 18,19,20] as well as the development of hepatic decompensation [12, 16, 17]. In addition, Vergniol et al. reported that LS values obtained from TE were able to predict the 5-year survival of patients with chronic hepatitis C [37]. Given that LS obtained from MRE was also demonstrated in our study to provide prognostic information regarding HCC occurrence, development of hepatic decompensation and overall survival in patients with compensated chronic liver disease, we anticipate that the LS value obtained from MRE may also be used to stratify patient risk. However, MRE has several clear advantages over TE [38]. In contrast to TE that covers only a small portion of the liver, MRE measures liver stiffness across the entire liver and therefore may be more reliable [25, 26]. In addition, even though the accuracy and reproducibility of TE for the assessment of the stage of fibrosis are known to be high, the presence of steatosis, an increased BMI and a lower degree of hepatic fibrosis may significantly reduce the reproducibility of TE [39]. In this regard, the accuracy of liver fibrosis staging and the reproducibility of measurements using MRE have been reported to be significantly better than those of TE [25,26,27]. Furthermore, TE may have limitations in its application to obese patients or individuals with ascites [40]. However, the presence of ascites or obesity would not be a limiting factor for the performance of MRE, and the rate of successful LS measurement using MRE may be higher compared to ultrasound-based elastography such as TE [32]. Even though the accuracy and reproducibility of MRE are better than US-based elastography including TE, the presence of iron overload in the liver could be an important limitation in MRE for assessing the degree of liver fibrosis [41]. However, recently introduced spin-echo-based MRE might overcome the limitation of iron overload in the liver and could widen the applicability of MRE [30]. As the measured liver stiffness value could be altered by changing the used frequency, frequency selection would be important in performing MRE [42]. In addition, using multi-frequency MRE, viscosity of the liver could also be evaluated; therefore, multi-frequency MRE could have the potential to widen the clinical utility of MRE, especially for the evaluation of hepatic inflammation and fibrosis in the early stage of chronic liver disease [43, 44].
We also observed in our study that the cumulative incidence of HCC occurrence was significantly higher in patients with increased LS values obtained from MRE, with the optimal cut-off value to predict HCC occurrence set at 4.44 kPa. Most current guidelines for the management of HCCs recommend surveillance US with a 6-month interval to detect HCC at an early stage in patients at high risk [33, 45]. However, the reported sensitivity of US in detecting HCC within the Milan criteria in cirrhotic patients is only approximately 60% [46]. Furthermore, the sensitivity of surveillance US for HCC in patients with advanced liver cirrhosis, such as patients on a liver transplant list, is suboptimal; thus, triple-phase CT or dynamic MRI scans are more frequently used at many centres [47, 48]. Therefore, considering the higher incidence of HCC in patients with high LS values and lower sensitivity of US for the detection of HCC in advanced liver cirrhosis, we believe that the surveillance of HCC using CT or MR may be helpful for chronic liver disease patients with higher than 4.44 kPa LS values. In addition, MRE can easily be incorporated into standard liver MR examinations, with excellent diagnostic performance for the detection and evaluation of focal liver lesions. Indeed, performing MRE examinations in addition to routine liver MR only requires < 5 min of additional scan time without any risk related to the examination.
Our study has several limitations. First, owing to the retrospective study design, there is an inevitable risk of selection bias. Second, even though our cut-off LS values obtained from MRE for the prediction of the development of hepatic decompensation, occurrence of HCC and overall survival were internally valid, our study results need to be validated by other studies, particularly in Western populations, as the main etiology of chronic liver disease is different between our study population and Western populations (i.e., hepatitis B virus related in our study vs. alcohol or hepatitis C virus related in Western populations).
In conclusion, LS values obtained from MRE can provide significant prognostic information regarding the development of hepatic decompensation, the occurrence of HCC and overall survival in patients with compensated chronic liver disease; it thus may have a promising role in the management of patients with compensated chronic liver disease.
Abbreviations
- CI:
-
Confidence interval
- EASL:
-
European Association for the Study of the Liver
- HCC:
-
Hepatocellular carcinoma
- HR:
-
Hazard ratio
- ICC:
-
Intraclass correlation coefficient
- IRB:
-
Institutional review board
- kPa:
-
Kilopascal
- LS:
-
Liver stiffness
- MRE:
-
Magnetic resonance elastography
- SS:
-
Spleen stiffness
- TE:
-
Transient elastography
- US:
-
Ultrasound
References
Lozano R, Naghavi M, Foreman K et al (2012) Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380:2095–2128
Blachier M, Leleu H, Peck-Radosavljevic M, Valla DC, Roudot-Thoraval F (2013) The burden of liver disease in Europe: a review of available epidemiological data. J Hepatol 58:593–608
Chang W, Lee JM, Yoon JH et al (2016) Liver fibrosis staging with MR elastography: comparison of diagnostic performance between patients with chronic hepatitis B and those with other etiologic causes. Radiology 280:88–97
Manos MM, Leyden WA, Murphy RC, Terrault NA, Bell BP (2008) Limitations of conventionally derived chronic liver disease mortality rates: Results of a comprehensive assessment. Hepatology 47:1150–1157
Asrani SK, Larson JJ, Yawn B, Therneau TM, Kim WR (2013) Underestimation of liver-related mortality in the United States. Gastroenterology 145:375–382 e371-372
Garcia-Tsao G, Friedman S, Iredale J, Pinzani M (2010) Now there are many (stages) where before there was one: In search of a pathophysiological classification of cirrhosis. Hepatology 51:1445–1449
D'Amico G, Garcia-Tsao G, Pagliaro L (2006) Natural history and prognostic indicators of survival in cirrhosis: a systematic review of 118 studies. J Hepatol 44:217–231
Schuppan D, Afdhal NH (2008) Liver cirrhosis. Lancet 371:838–851
Fleming KM, Aithal GP, Card TR, West J (2010) The rate of decompensation and clinical progression of disease in people with cirrhosis: a cohort study. Aliment Pharmacol Ther 32:1343–1350
Parkin DM, Bray F, Ferlay J, Pisani P (2001) Estimating the world cancer burden: Globocan 2000. Int J Cancer 94:153–156
Lee DH, Lee JM, Lee JY et al (2014) Radiofrequency ablation of hepatocellular carcinoma as first-line treatment: long-term results and prognostic factors in 162 patients with cirrhosis. Radiology 270:900–909
Singh S, Fujii LL, Murad MH et al (2013) Liver stiffness is associated with risk of decompensation, liver cancer, and death in patients with chronic liver diseases: a systematic review and meta-analysis. Clin Gastroenterol Hepatol 11:1573–1584 e1571-1572; quiz e1588-1579
Castera L, Vergniol J, Foucher J et al (2005) Prospective comparison of transient elastography, Fibrotest, APRI, and liver biopsy for the assessment of fibrosis in chronic hepatitis C. Gastroenterology 128:343–350
Foucher J, Chanteloup E, Vergniol J et al (2006) Diagnosis of cirrhosis by transient elastography (FibroScan): a prospective study. Gut 55:403–408
Cassinotto C, Lapuyade B, Mouries A et al (2014) Non-invasive assessment of liver fibrosis with impulse elastography: comparison of Supersonic Shear Imaging with ARFI and FibroScan(R). J Hepatol 61:550–557
Robic MA, Procopet B, Metivier S et al (2011) Liver stiffness accurately predicts portal hypertension related complications in patients with chronic liver disease: a prospective study. J Hepatol 55:1017–1024
Corpechot C, Carrat F, Poujol-Robert A et al (2012) Noninvasive elastography-based assessment of liver fibrosis progression and prognosis in primary biliary cirrhosis. Hepatology 56:198–208
Jung KS, Kim SU, Ahn SH et al (2011) Risk assessment of hepatitis B virus-related hepatocellular carcinoma development using liver stiffness measurement (FibroScan). Hepatology 53:885–894
Wong GL, Chan HL, Wong CK et al (2014) Liver stiffness-based optimization of hepatocellular carcinoma risk score in patients with chronic hepatitis B. J Hepatol 60:339–345
Kim MN, Kim SU, Kim BK et al (2015) Increased risk of hepatocellular carcinoma in chronic hepatitis B patients with transient elastography-defined subclinical cirrhosis. Hepatology 61:1851–1859
Muthupillai R, Lomas DJ, Rossman PJ, Greenleaf JF, Manduca A, Ehman RL (1995) Magnetic resonance elastography by direct visualization of propagating acoustic strain waves. Science 269:1854–1857
Godfrey EM, Mannelli L, Griffin N, Lomas DJ (2013) Magnetic resonance elastography in the diagnosis of hepatic fibrosis. Semin Ultrasound CT MR 34:81–88
Huwart L, Sempoux C, Salameh N et al (2007) Liver fibrosis: noninvasive assessment with MR elastography versus aspartate aminotransferase-to-platelet ratio index. Radiology 245:458–466
Loomba R, Wolfson T, Ang B et al (2014) Magnetic resonance elastography predicts advanced fibrosis in patients with nonalcoholic fatty liver disease: a prospective study. Hepatology 60:1920–1928
Huwart L, Sempoux C, Vicaut E et al (2008) Magnetic resonance elastography for the noninvasive staging of liver fibrosis. Gastroenterology 135:32–40
Van Beers BE, Daire JL, Garteiser P (2015) New imaging techniques for liver diseases. J Hepatol 62:690–700
Lee DH, Lee JM, Yi NJ et al (2016) Hepatic stiffness measurement by using MR elastography: prognostic values after hepatic resection for hepatocellular carcinoma. Eur Radiol. https://doi.org/10.1007/s00330-016-4499-8
Chung S, Breton E, Mannelli L, Axel L (2011) Liver stiffness assessment by tagged MRI of cardiac-induced liver motion. Magn Reson Med 65:949–955
Mannelli L, Wilson GJ, Dubinsky TJ et al (2012) Assessment of the liver strain among cirrhotic and normal livers using tagged MRI. J Magn Reson Imaging 36:1490–1495
Mariappan YK, Dzyubak B, Glaser KJ et al (2017) Application of modified spin-echo-based sequences for hepatic MR elastography: Evaluation, comparison with the conventional gradient-echo sequence, and preliminary clinical experience. Radiology 282:390–398
Mannelli L, Godfrey E, Graves MJ et al (2012) Magnetic resonance elastography: feasibility of liver stiffness measurements in healthy volunteers at 3T. Clin Radiol 67:258–262
Asrani SK, Talwalkar JA, Kamath PS et al (2014) Role of magnetic resonance elastography in compensated and decompensated liver disease. J Hepatol 60:934–939
European Association For The Study Of The L, European Organisation For R, Treatment Of C (2012) EASL-EORTC clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol 56:908–943
Faraggi D, Simon R (1996) A simulation study of cross-validation for selecting an optimal cutpoint in univariate survival analysis. Stat Med 15:2203–2213
El-Serag HB (2011) Hepatocellular carcinoma. N Engl J Med 365:1118–1127
Thiele M, Kjaergaard M, Thielsen P, Krag A (2015) Contemporary use of elastography in liver fibrosis and portal hypertension. Clin Physiol Funct Imaging. https://doi.org/10.1111/cpf.12297
Vergniol J, Foucher J, Terrebonne E et al (2011) Noninvasive tests for fibrosis and liver stiffness predict 5-year outcomes of patients with chronic hepatitis C. Gastroenterology 140:1970–1979 1979 e1971-1973
Srinivasa Babu A, Wells ML, Teytelboym OM et al (2016) Elastography in chronic liver disease: modalities, techniques, limitations, and future directions. Radiographics 36:1987–2006
Fraquelli M, Rigamonti C, Casazza G et al (2007) Reproducibility of transient elastography in the evaluation of liver fibrosis in patients with chronic liver disease. Gut 56:968–973
Llop E, Berzigotti A, Reig M et al (2012) Assessment of portal hypertension by transient elastography in patients with compensated cirrhosis and potentially resectable liver tumors. J Hepatol 56:103–108
Ferraioli G, Tinelli C, Dal Bello B et al (2012) Accuracy of real-time shear wave elastography for assessing liver fibrosis in chronic hepatitis C: a pilot study. Hepatology 56:2125–2133
Asbach P, Klatt D, Schlosser B et al (2010) Viscoelasticity-based staging of hepatic fibrosis with multifrequency MR elastography. Radiology 257:80–86
Asbach P, Klatt D, Hamhaber U et al (2008) Assessment of liver viscoelasticity using multifrequency MR elastography. Magn Reson Med 60:373–379
Yin M, Glaser KJ, Manduca A et al (2017) Distinguishing between Hepatic Inflammation and Fibrosis with MR Elastography. Radiology 284:694–705
Bruix J, Sherman M, American Association for the Study of Liver D (2011) Management of hepatocellular carcinoma: an update. Hepatology 53:1020–1022
Singal A, Volk ML, Waljee A et al (2009) Meta-analysis: surveillance with ultrasound for early-stage hepatocellular carcinoma in patients with cirrhosis. Aliment Pharmacol Ther 30:37–47
Van Thiel DH, Yong S, Li SD, Kennedy M, Brems J (2004) The development of de novo hepatocellular carcinoma in patients on a liver transplant list: frequency, size, and assessment of current screening methods. Liver Transpl 10:631–637
Yu NC, Chaudhari V, Raman SS et al (2011) CT and MRI improve detection of hepatocellular carcinoma, compared with ultrasound alone, in patients with cirrhosis. Clin Gastroenterol Hepatol 9:161–167
Funding
The authors state that there is no grant or fund supporting this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Jeong Min Lee.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Ethical approval
Institutional Review Board approval was obtained.
Informed consent
Written informed consent was waived by IRB.
Methodology
• Retrospective
• Observational
• Performed at one institution
Electronic supplementary material
ESM 1
(DOCX 25 kb)
Rights and permissions
About this article
Cite this article
Lee, D.H., Lee, J.M., Chang, W. et al. Prognostic Role of Liver Stiffness Measurements Using Magnetic Resonance Elastography in Patients with Compensated Chronic Liver Disease. Eur Radiol 28, 3513–3521 (2018). https://doi.org/10.1007/s00330-017-5278-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-017-5278-x