Abstract
Magnetic resonance neurography (also called MRN or MR neurography) refers to MR imaging dedicated to the peripheral nerves. It is a technique that enhances selective multiplanar visualisation of the peripheral nerve and pathology by encompassing a combination of two-dimensional, three-dimensional and diffusion imaging pulse sequences. Referring physicians who seek imaging techniques that can depict and diagnose peripheral nerve pathologies superior to conventional MR imaging are driving the demand for MRN. This article reviews the pathophysiology of peripheral nerves in common practice scenarios, technical considerations of MRN, current indications of MRN, normal and abnormal neuromuscular appearances, and imaging pitfalls. Finally, the emerging utility of diffusion-weighted and diffusion tensor imaging is discussed and future directions are highlighted.
Key points
• Lesion relationship to neural architecture is more conspicuous on MRN than MRI.
• 3D multiplanar imaging technique is essential for pre-surgical planning.
• Nerve injuries can be classified on MRN using Sunderland’s classification.
• DTI provides quantitative information and insight into intraneural integrity and pathophysiology.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Magnetic resonance neurography (also called MRN or MR neurography) refers to MR imaging dedicated to the peripheral nerves. It is a technique that enhances selective multiplanar visualisation of the peripheral nerve and pathology by encompassing a combination of two-dimensional (2D), three-dimensional (3D) and diffusion imaging pulse sequences [1]. While large perineural lesions and denervation muscle changes are quite apparent on conventional MRI, the relationship of lesions to the nerve architecture is more conspicuous on MRN [2, 3] (Fig. 1). Direct depiction of neuromuscular imaging alterations is highly valuable because it is helpful for both referring physicians and patients to objectively visualise the consequences of neuromuscular pathology (Fig. 2) [4, 5]. This article reviews the pathophysiology of common peripheral nerve abnormalities, describes technical considerations of MRN, discusses current indications for MRN, and highlights normal and abnormal neuromuscular appearances and imaging pitfalls on MRN examinations. Finally, the emerging utility of diffusion-weighted imaging (DWI) is discussed and future directions are highlighted.
A 23-year-old woman with prior right leg and ankle injury and tendon surgery presenting with ipsilateral foot weakness and pain. (A) Sagittal proton density-weighted (PDW) image shows heterogeneous soft tissue thickening along the course of the tibial nerve (small arrows) with adjacent susceptibility artefacts. Denervation changes are seen as hyperintense signals in the plantar muscles (large arrow). (B) Three-dimensional magnetic resonance neurography (MRN) image shows high-grade tibial nerve injury and large neuroma in continuity (Sunderland class IV) demonstrated by a heterogeneously thickened nerve segment (small arrows). Notice the hyperintense but otherwise normal-calibre medial and lateral plantar nerves (large arrows). (C) Inverted scale trace maximum intensity projection (MIP) image from diffusion tensor imaging (DTI) confirms the neuroma in continuity with selective depiction of abnormally hypointense nerve (small arrows) and muscle denervation changes (large arrows)
A 63-year-old man with foot drop and clinically suspected right-sided sciatic neuropathy or radiculopathy. Electrophysiology revealed right tibial and sural neuropathy. Magnetic resonance neurography (MRN) of the right thigh, knee and lumbosacral (LS) plexus was performed to better localise and characterise the lesion. The nerves appeared normal in the thigh and knee (not shown). The LS plexus MRN image reveals an abnormally thickened and hyperintense right lateral femoral cutaneous nerve (small arrow), femoral nerve (medium arrow) and obturator nerve (large arrow). The left-sided plexus shows a normal appearance. The final diagnosis was multifocal inflammatory motor-sensory neuropathy
Peripheral neuromuscular anatomy and variations
The peripheral nerves have a uniform but complex architecture (Fig. 3). The axon, a basic building block, is covered by connective tissue layers known as the endoneurium, perineurium and epineurium [6]. In young adults, although there is tight compact appearance of the nerve with uniformly thick fascicles, more intraneural fat accumulates and prominent intraneural vessels appear with increasing age [7]. Asymptomatic streaky fatty infiltration of the muscles can be seen with aging, e.g. in gluteus maximus, pronator quadratus, semimembranosus, plantar foot and supinator muscles [8, 9].
Pathophysiology of neuropathy as it pertains to imaging
The most common causes of peripheral neuropathy include trauma and entrapment. Traumatic nerve injury can occur because of stretch, crush or penetration, traditionally graded based on Seddon’s classification. The degree of injury is further stratified based on Sunderland’s I–V classification system, which aids in management planning (Table 1) [10,11,12]. Classes IV and V lead to significant nerve dysfunction and usually require surgical treatment. Nerve compression due to entrapment results in blockage of endoneurial fluid flow and vascular congestion. Over time, the unrelieved compression leads to myelin and axonal damage, nerve infarction and fibrosis. If the insult is relieved, the nerve heals by axonal regeneration and immature myelin formation [13, 14]. Body and tissue response may also include intraneural fat proliferation, which is particularly observed in diabetes mellitus, where the overall nerve calibre increases despite fascicular atrophy [15]. During healing, regeneration proceeds slowly from the spinal anterior horn cells or site of injury to the muscle end plate up to a rate of 1 mm/day for smaller nerves and 5 mm/day for the larger nerves [6, 16, 17]. Typical examples of repeated degeneration and regeneration of peripheral nerves are seen in the histology models of Charcot-Marie-Tooth disease (CMT) [18].
Electrophysiology versus imaging
Electrophysiology (EP) has long been considered the reference standard for neuropathy diagnosis and nerve regeneration. However, its limitations must be recognized. EP can be falsely negative in neurapraxia and, additionally, despite complete nerve transection in higher class injuries, it may take up to 7 days to detect a significant decrease or absence of sensory and/or motor nerve responses [19, 20]. Further limitations of EP procedures include difficulty in lesion localisation and physical discomfort to the patients.
Ultrasound (US) is excellent for evaluating superficial nerves and in interrogating large areas of extremities rapidly [21]. Increasingly, US is being employed for the diagnosis and follow-up of various neuropathies using the diagnostic criteria of nerve and/or fascicular enlargement [22]. MRN provides excellent spatial resolution (0.3–0.5 mm in-plane on 2D imaging and 0.9–1.5 mm isotropic on 3D imaging) [23]. It allows easy identification and characterisation of obliquely coursing peripheral nerves [24]. Due to its superior contrast resolution compared with US, signal alterations in nerves and muscles are much more conspicuous and the diagnosis of neuropathy on MRN can be accomplished using multiple different criteria even if the nerve is not enlarged (Table 2). Multiple MRN studies have shown moderate to excellent interobserver performance in determination of T2 nerve signal, nerve-to-vessel signal intensity ratio and nerve calibre with the intraclass coefficient ranging from 0.84 to 0.94 for larger nerves, such as sciatic and ulnar, and 0.56 to 0.72 for smaller ones [25,26,27]. Apart from lesion localisation and intraneural tissue characterisation (Table 3), MRN allows grading of the acuity or chronicity of muscle denervation, classifies nerve injury, detects polyneuropathies and aids in planning of subsequent image-guided perineural or intramuscular injections. In vivo neural regeneration studies on humans using MRI are being published, and decreasing muscle and nerve hyperintensity has been shown to correlate with nerve regeneration and functional improvement [28, 29]. Current indications of MRN are listed in Supplementary Table 4.
Technical considerations of magnetic resonance neurography (MRN)
Pulse sequences
The basic goal for all imaging sequences employed for MRN is to produce high-resolution scans with superior contrast and/or uniform fat saturation while simultaneously suppressing pulsation and breathing artefacts. Since nerves have longer T2 signals (e.g. 80– 100 ms) [30], and are often surrounded by bright fat, the preferred imaging sequence includes fast or turbo spin echo (FSE/TSE) with spectral saturation using the adiabatic inversion pulse and Dixon technique [31]. The echo time should be kept above 60 ms, specifically to enhance the endoneurial fluid signal while minimizing signals from surrounding tissues with shorter T2 signals, such as muscle [32]. Furthermore, when used with diffusion tensor imaging (DTI) acquisitions, tighter echo spacing (e.g. <0.7 ms) and higher bandwidth reduce ghosting artefacts [33]. Recent advancements including modulated refocusing flip angles [34] combined with extended echo train lengths and parallel imaging have enabled 3D T2-weighted acquisitions using FSE/TSE for volumetric visualisation of the nerves in clinically feasible scan times [23, 35]. In addition, signal suppression of adjacent vessels can be accomplished by addition of motion-sensitizing driven equilibrium or diffusion moment [36,37,38] enabling visualisation of small nerves in the extremities and skull base. Contrast imaging is used in cases suspected of tumours or infections and for characterisation of atypical polyneuropathies. The suggested MRN protocols are highlighted in Supplementary Tables 5 and 6.
Scanners and coils
MRN can be performed on both 1.5 T and 3 T scanners, but when available, 3 T is preferred due to the increased SNR and faster 3D [39]. In addition, fascicular detail is much more conspicuous on 3 T, especially on the axial images, which are important to characterise and localise the neuropathies [40]. An exception to this is the presence of metallic implants, where 1.5 T imaging is preferred to minimize artefacts. For superior spatial resolution, a joint specific receiver coil should be used in a periarticular location, e.g. during carpal tunnel or cubital tunnel imaging [7]. The dedicated joint coil can be combined with a surface (flex) coil to evaluate the nerve over a longer distance. For plexus imaging, the anterior torso coil is combined with the spine coil to achieve a homogeneous signal.
Imaging pitfalls
Significant pulsation artefacts from vessels can obscure the nerve or cause it to be too bright due to overlap. Shorter echo spacing and re-orientation of the phase encoding gradient can help mitigate this artefact. Suboptimal fat suppression or magic angle artefact can lead to spurious differences in the signal intensity of the peripheral nerves. The presence of metal artefacts can obscure the local anatomy. Suboptimal fat suppression and low bandwidth can result in significant ghosting artefacts on diffusion imaging [41]. Finally, patient movement and off-centre imaging can potentially degrade imaging.
MRN imaging findings
Normal neuromuscular appearances
Normal peripheral nerves show uniform contour, a similar calibre to adjacent arteries and accompanying nerves, side-to-side symmetry and minimal visible branching [42]. The fascicular detail is conspicuous in axial images in extremity peripheral nerves measuring more than 3 mm. The outer epineurium and perineurium exhibit thin uniform hypointense linings. On contrast imaging, only the dorsal nerve root ganglion exhibits any appreciable enhancement [6].
Abnormal neuromuscular appearances
Pathological nerves show one or a combination of findings (Table 2), including nerve and/or fascicular signal alterations or discontinuity, altered calibre, irregular contour, intra- or perineural tumour or scarring, and abnormal enhancement (Fig. 2) [2, 5]. MRN can indirectly demonstrate intraneural pathophysiology as illustrated in Table 3 [42,43,44]. DTI further supplements anatomical MRN diagnostic accuracy. Breckwoldt et al. showed that in upper extremity neuropathy, T2W images and DTI perform similarly in isolation while a combination of MRN plus DTI results in increased diagnostic accuracy (area under the curve = 0.97) [44]. Muscle denervation oedema and/or atrophy are important findings in the diagnosis of neuropathy [2, 27]. As a rule, denervation changes occur distal to the site of insult and muscle signal alterations are diffuse without haemorrhage or fascial oedema. The injured nerves exhibit hyperintense signal on T2W images within 24 h of the insult [28, 45]. Sunderland Class I–III injuries demonstrate a uniform hyperintense signal and class I injury is short-lived with absent muscle signal alterations. Class IV injury shows a heterogeneous nerve signal with a focal fascicular abnormality and neuroma in continuity (Figs. 1 and 4). Class V injury shows a discontinuous nerve with end-bulb neuroma. Studies are needed to show if DTI can further supplement the differentiation of class I–IV injuries. MRN aids in characterisation of the lesions causing nerve entrapment, such as haematoma, ganglion, bony callous, etc. and demonstrates their relationship to the nerve in terms of its axial location, longitudinal extent or fascicular involvement [2, 6, 7]. Nerve and/or fascicular hyperintensity is maximum adjacent to the site of entrapment, which aids in lesion localisation. For example, sciatic nerve hyperintensity is most pronounced at the sciatic notch in the setting of piriformis syndrome. The increasing nerve calibre distinguishes severe from mild cases of neuropathy and DTI can also aid in the severity assessment [26, 46]. Commonly, the nerve enlarges proximal to the site of entrapment. If one also identifies distal nerve enlargement or ‘triple B sign’ (progressive nerve signal change from ‘bright to black to bright’ across the entrapment site), there is likely severe nerve impingement or constriction that would typically require surgery (Fig. 5) [47, 48]. Peripheral nerves can be affected by a variety of tumours and tumour-like conditions (Fig. 6) [49, 50]. MRN and DTI can characterise the relationship of various lesions with nerve fascicles (Table 3) [51, 52].
Prior penetrating injury with Sunderland class IV and III injuries. Axial T2 SPAIR image shows a neuroma in continuity of the common peroneal nerve with loss of fascicular detail (large arrow) in keeping with a class IV injury. Notice the enlarged tibial nerve with hyperintense, albeit preserved fascicular detail (small arrow) in keeping with a class III injury. The patient underwent surgical reconstruction of the common peroneal nerve
Carpal tunnel syndrome and triple B sign. Coronal magnetic resonance neurography (MRN) image shows proximal and distal enlargement and abnormal hyperintensity (large arrows) of the median nerve across the transverse carpal ligament with flattening and decreased signal at the impingement site (small arrow)
Benign peripheral nerve sheath tumour. A 45-year-old man with left shoulder swelling. (A) Coronal magnetic resonance neurography (MRN) image shows a large peripheral nerve sheath tumour (large arrow) displacing the nerves anteriorly and superiorly (small arrow). (B) Corresponding ADC map shows a high ADC value of 2.5–2.7 × 10–3 mm2/s in keeping with a benign peripheral nerve sheath tumour. The tumour was stable for more than 2 years
Interpretation pitfalls
For accurate reporting, it is essential to be familiar with the expected regions of T2 hyperintensity related to magic-angle artefacts. These include the greater sciatic notch for the sciatic nerve, genu of the femoral nerve and at turning points (e.g. lateral femoral cutaneous nerve at anterior superior iliac spine, C8 nerve at thoracic outlet, deep branch of ulnar nerve dorsal to the carpal tunnel and medial plantar nerve across the tarsal tunnel) [7]. It is important to evaluate the spatial extension of T2 signal alterations to be confident of neuropathy [53]. Mild hyperintensity of the nerves on T2W images can be seen in asymptomatic subjects [54]. Anatomical nerve branching variations are common. For example, sciatic variations are seen in about 6–25% of the population but only a minority develop piriformis syndrome.
Diffuse polyneuropathies
Diffuse or systemic neuropathies can be hereditary (CMT disease) or acquired due to a multitude of causes, and idiopathic (Fig. 2). While their diagnosis is primarily based on clinical findings and laboratory testing, electrophysiology and MRN supplement the diagnosis [53]. CMT manifests with symmetrical early-age neuropathy problems, high plantar arches, positive family history and symmetrically reduced nerve conduction velocities. MRI may incidentally exhibit substantial symmetrical thickening of nerves (CMT type I-demyelinating variety) or milder thickening (type II-axonal type). MRN and DTI increase conspicuity of the nerve lesions and can detect superimposed entrapment(s) [55,56,57].
Most acquired neuropathies, however, produce asymmetrical findings. One such common condition, chronic inflammatory demyelinating neuropathy (CIDP), usually shows a downhill course and typical albuminocytological dissociation. MRN shows significant thickening and hyperintensity of nerves in the lower limbs > upper limbs and no substantial enhancement [58]. Multifocal motor neuropathy presents with pure motor neuron weakness. Typically, ganglioside M1 antibodies are identified on serology and MRN shows mild to moderate thickening and hyperintensity of the upper limb or brachial plexus nerves [59]. In radiation neuropathy, MRN shows diffuse nerve thickening and T2 hyperintensity localised to the radiation field with regional oedematous muscle changes in acute-to-subacute stages. Nerve kinking from fibrosis is seen in chronic stages [7]. Diabetes mellitus is a common cause of peripheral polyneuropathy, and diabetic amyotrophy is a common differential finding of radiculopathy in adult patients. On MRN, a diffuse increased signal in bilateral sciatic and tibial nerves can be seen in the lower limbs, with nerve thickening and DTI parameter alterations [60,61,62]. In diabetic amyotrophy, MRN shows bilateral prominent and hyperintense lumbosacral (L4-S2) nerve roots and paraspinal branches and femoral and/or sciatic nerves. While local infections can affect the nerves, Mycobacterium leprae is a known neurotropic pathogen. MRN can show moderate to marked thickening of the nerves with perineural oedema and/or intraneural abscess. Finally, polyneuropathy can occur due to amyloidosis, especially in the setting of underlying paraproteinemia. It manifests as diffuse thickening of the nerves and fascicles with nodularity and mixed or predominantly hyperintense signal foci [63].
Role of diffusion imaging
DWI and DTI application in the peripheral nerve system is challenging because of the need for high spatial resolution over the long nerve course, low water proton content of the nerves and relatively limited diffusion within them. On qualitative evaluation, the signal in the neuropathic nerve is often more conspicuous on DWI trace images compared with T2W images. The quantitative evaluation generates fractional anisotropy (FA) and apparent diffusion coefficient (ADC) [64]. Research has shown an age- and location-dependency of FA values. Neuropathy leads to increased ADC and decreased FA. Quantitative data from the initial animal studies has shown FA increases towards normalcy with nerve regeneration [65]. DTI generates tractography (Fig. 7), and it is important to understand that the fibres seen on tractography are not anatomically identical to the individual fascicles. However, if fascicles are compressed, oedematous or interrupted, correspondingly, the fibres on tractography are thinned, distorted or interrupted [66].
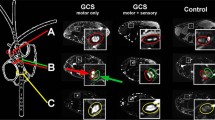
Representative images illustrating the current status of diffusion tensor imaging (DTI) and maximum possible image quality employing diffusion weighted and diffusion tensor imaging in the corresponding anatomical regions. (A) Oblique coronal 3D diffusion-weighted PSIF image of the facial region with an overlaid tractograpy image in a healthy volunteer shows the right inferior alveolar nerve within its intra-osseous course through the mandible (image generated on Syngovia, Siemens, Erlangen, Germany). (B) The tractography fibres can also be overlaid onto a 3-dimensional (3D) model that was created by acquiring a 3D MRI data set using ultra-short echo time sequence. It can help in planning complex orthodontic surgery with visualisation of the important neurogenic structures. (C) Virtual anatomical images from a fusion of diffusion-weighted and high-resolution morphological magnetic resonance neurography (MRN) images allow photorealistic representations of the true in vivo anatomy in an individual
Impact of MRN and future directions
Dedicated nerve imaging has been shown to impact both diagnostic thinking and therapeutic management of patients suspected of having peripheral neuropathy [67,68,69]. In a recent study, MRN was shown to reduce unnecessary surgeries by 17% and MRN increased the confidence of the surgeon in the diagnosis and management of neuropathy [67]. MRN accuracy is well reported [70]; however, technical developments continue and outcome studies using homogeneous and larger patient populations are still needed. Cost analysis would be useful to determine the overall burden of this emerging imaging modality.
Conclusion
MRN is a useful modality for direct demonstration of neuromuscular pathology and characterisation and is playing an increasingly important role in the management of various peripheral nerve disorders.
References
Howe FA, Filler AG, Bell BA, Griffiths JR (1992) Magnetic resonance neurography. Magn Reson Med 28:328–338
Filler AG, Kliot M, Howe FA, Hayes CE, Saunders DE, Goodkin R et al (1996) Application of magnetic resonance neurography in the evaluation of patients with peripheral nerve pathology. J Neurosurg 85:299–309
Mauermann ML, Amrami KK, Kuntz NL, Spinner RJ, Dyck PJ, Bosch EP et al (2009) Longitudinal study of intraneural perineurioma –a benign, focal hypertrophic neuropathy of youth. Brain 132:2265–2276
Thawait SK, Wang K, Subhawong TK, Williams EH, Hashemi SS, Machado AJ et al (2012) Peripheral nerve surgery: the role of high-resolution MR neurography. AJNR Am J Neuroradiol 33:203–210
Baumer P, Kele H, Kretschmer T, Koenig R, Pedro M, Bendszus M et al (2014) Thoracic outlet syndrome in 3T MR neurography-fibrous bands causing discernible lesions of the lower brachial plexus. Eur Radiol 24:756–761
Filler AG, Maravilla KR, Tsuruda JS (2004) MR neurography and muscle MR imaging for image diagnosis of disorders affecting the peripheral nerves and musculature. Neurol Clin 22:643–682, vi–vii
Subhawong TK, Wang KC, Thawait SK, Williams EH, Hashemi SS, Machado AJ et al (2012) High resolution imaging of tunnels by magnetic resonance neurography. Skeletal Radiol 41:15–31
Gyftopoulos S, Rosenberg ZS, Petchprapa C (2010) Increased MR signal intensity in the pronator quadratus muscle: Does it always indicate anterior interosseous neuropathy? AJR Am J Roentgenol 194:490–493
Schmid DT, Hodler J, Mengiardi B, Pfirrmann CW, Espinosa N, Zanetti M (2009) Fatty muscle atrophy: prevalence in the hindfoot muscles on MR images of asymptomatic volunteers and patients with foot pain. Radiology 253:160–166
Sunderland S (1951) A classification of peripheral nerve injuries producing loss of function. Brain 74:491–516
Chhabra A, Ahlawat S, Belzberg A, Andreseik G (2014) Peripheral nerve injury grading simplified on MR neurography: As referenced to Seddon and Sunderland classifications. Indian J Radiol Imaging 24:217–224
Cox B, Zuniga JR, Panchal N, Cheng J, Chhabra A (2016) Magnetic resonance neurography in the management of peripheral trigeminal neuropathy: experience in a tertiary care centre. Eur Radiol 26:3392–3400
Menorca RM, Fussell TS, Elfar JC (2013) Nerve physiology: mechanisms of injury and recovery. Hand Clin 29:317–330
Li X, Shen J, Chen J, Wang X, Liu Q, Liang B (2008) Magnetic resonance imaging evaluation of acute crush injury of rabbit sciatic nerve: correlation with histology. Can Assoc Radiol J 59:123–130
Thakkar RS, Del Grande F, Thawait GK et al (2012) Spectrum of high-resolution MRI findings in diabetic neuropathy. AJR Am J Roentgenol 199:407–412
Cudlip SA, Howe FA, Griffiths JR, Bell BA (2002) Magnetic resonance neurography of peripheral nerve following experimental crush injury, and correlation with functional deficit. J Neurosurg 96:755–759
Gulati AK (1996) Peripheral nerve regeneration through short- and long-term degenerated nerve transplants. Brain Res 742:265–270
Hsieh SY, Kuo HC, Chu CC, Lin KP, Huang CC (2004) Charcot-Marie-Tooth disease type 1A: a clinical, electrophysiological, pathological, and genetic study. Chang Gung Med J 27:300–306
Chung T, Prasad K, Lloyd TE (2014) Peripheral neuropathy: clinical and electrophysiological considerations. Neuroimaging Clin N Am 24:49–65
Feinberg J (2006) EMG: myths and facts. HSS J 2:19–21
Padua L, Liotta G, Di Pasquale A, Granata G, Pazzaglia C, Caliandro P et al (2012) Contribution of ultrasound in the assessment of nerve diseases. Eur J Neurol 19:47–54
Di Pasquale A, Morino S, Loreti S, Bucci E, Vanacore N, Antonini G (2015) Peripheral nerve ultrasound changes in CIDP and correlations with nerve conduction velocity. Neurology 84:803–809
Chhabra A, Lee PP, Bizzell C, Soldatos T (2011) 3 Tesla MR neurography – technique, interpretation, and pitfalls. Skeletal Radiol 40:1249–1260
Delaney H, Bencardino J, Rosenberg ZS (2014) Magnetic resonance neurography of the pelvis and lumbosacral plexus. Neuroimaging Clin N Am 24:127–150
Chhabra A, Del Grande F, Soldatos T, Chalian M, Belzberg AJ, Williams EH et al (2013) Meralgia paresthetica: 3-Tesla magnetic resonance neurography. Skeletal Radiol 42:803–808
Bäumer P, Dombert T, Staub F, Kaestel T, Bartsch AJ, Heiland S et al (2011) Ulnar neuropathy at the elbow: MR neurography – nerve T2 signal increase and caliber. Radiology 260:199–206
Chhabra A, Chalian M, Soldatos T, Andreisek G, Faridian-Aragh N, Williams E et al (2012) 3-T high-resolution MR neurography of sciatic neuropathy. AJR Am J Roentgenol 198:W357–W364
Bendszus M, Wessig C, Solymosi L, Reiners K, Koltzenburg M (2004) MRI of peripheral nerve degeneration and regeneration: correlation with electrophysiology and histology. Exp Neurol 188:171–177
Viddeleer AR, Sijens PE, van Ooijen PM, Kuypers PD, Hovius SE, De Deyn PP et al (2016) Quantitative STIR of muscle for monitoring nerve regeneration. J Magn Reson Imaging 44:401–410
Stanisz GJ, Midha R, Munro CA, Henkelman RM (2001) MR properties of rat sciatic nerve following trauma. Magn Reson Med 45:415–420
Madhuranthakam AJ, Yu H, Shimakawa A et al (2010) T(2)-weighted 3D fast spin echo imaging with water-fat separation in a single acquisition. J Magn Reson Imaging 32:745–751
Gatehouse PD, Bydder GM (2003) Magnetic resonance imaging of short T2 components in tissue. Clin Radiol 58:1–19
Ishida G, Oishi M, Morii K, Hasegawa K, Saito A, Sato M et al (2015) Application of brain diffusion-weighted imaging performed using readout segmentation of long variable echo trains. No Shinkei Geka 43:31–40
Busse RF, Hariharan H, Vu A, Brittain JH (2006) Fast spin echo sequences with very long echo trains: design of variable refocusing flip angle schedules and generation of clinical T2 contrast. Magn Reson Med 55:1030–1037
Vargas MI, Viallon M, Nguyen D, Beaulieu JY, Delavelle J, Becker M (2010) New approaches in imaging of the brachial plexus. Eur J Radiol 74:403–410
Madhuranthakam AJ, Lenkinski RE (2015) Technical advancements in MR Neurography. Semin Musculoskelet Radiol 19:86–93
Kasper JM, Wadhwa V, Scott KM, Rozen S, Xi Y, Chhabra A (2015) SHINKEI – a novel 3D isotropic MR neurography technique: technical advantages over 3DIRTSE-based imaging. Eur Radiol 25:1672–1677
Chhabra A, Soldatos T, Subhawong TK, Machado AJ, Thawait SK, Wang KC et al (2011) The application of three-dimensional diffusion-weighted PSIF technique in peripheral nerve imaging of the distal extremities. J Magn Reson Imaging 34:962–967
Merkle EM, Dale BM, Barboriak DP (2007) Gain in signal-to-noise for first-pass contrast-enhanced abdominal MR angiography at 3 Tesla over standard 1.5 Tesla: prediction with a computer model. Acad Radiol 14:795–803
Bäumer P, Kele H, Xia A, Weiler M, Schwarz D, Bendszus M et al (2016) Posterior interosseous neuropathy: Supinator syndrome vs fascicular radial neuropathy. Neurology 87:1884–1891
Chhabra A, Thakkar RS, Andreisek G, Chalian M, Belzberg AJ, Blakeley J et al (2013) Anatomic MR imaging and functional diffusion tensor imaging of peripheral nerve tumors and tumorlike conditions. AJNR Am J Neuroradiol 34:802–807
Soldatos T, Andreisek G, Thawait GK, Guggenberger R, Williams EH, Carrino JA et al (2013) High-resolution 3-T MR neurography of the lumbosacral plexus. Radiographics 33:967–987
Wadhwa V, Thakkar RS, Maragakis N, Höke A et al (2012) Sciatic nerve tumor and tumor-like lesions – uncommon pathologies. Skeletal Radiol 41:763–774
Breckwoldt MO, Stock C, Xia A, Heckel A, Bendszus M, Pham M et al (2015) Diffusion Tensor Imaging Adds Diagnostic Accuracy in Magnetic Resonance Neurography. Invest Radiol 50:498–504
van Ouwerkerk WJ, Strijers RL, Barkhof F, Umans U, Vandertop WP (2005) Detection of root avulsion in the dominant C7 obstetric brachial plexus lesion: experience with three-dimensional constructive interference in steady-state magnetic resonance imaging and electrophysiology. Neurosurgery 57:930–940
Breitenseher JB, Kranz G, Hold A, Berzaczy D, Nemec SF, Sycha T et al (2015) MR neurography of ulnar nerve entrapment at the cubital tunnel: a diffusion tensor imaging study. Eur Radiol 25:1911–1918
Sneag DB, Saltzman EB, Meister DW, Feinberg JH, Lee SK, Wolfe SW (2016) MRI bullseye sign: An indicator of peripheral nerve constriction in parsonage-turner syndrome. Muscle Nerve. doi:10.1002/mus.25480
Chhabra A (2014) Peripheral MR, neurography: approach to interpretation. Neuroimaging Clin N Am 24:79–89
Wasa J, Nishida Y, Tsukushi S, Shido Y, Sugiura H, Nakashima H et al (2010) MRI features in the differentiation of malignant peripheral nerve sheath tumors and neurofibromas. AJR Am J Roentgenol 194:1568–1574
Descamps MJ, Barrett L, Groves M, Yung L, Birch R, Murray NM et al (2006) Primary sciatic nerve lymphoma: a case report and review of the literature. J Neurol Neurosurg Psychiatry 77:1087–1089
Demehri S, Belzberg A, Blakeley J, Fayad LM (2014) Conventional and functional MR imaging of peripheral nerve sheath tumors: initial experience. AJNR Am J Neuroradiol 35:1615–1620
Schmidt M, Kasprian G, Amann G, Duscher D, Aszmann OC (2015) Diffusion tensor tractography for the surgical management of peripheral nerve sheath tumors. Neurosurg Focus 39, E17
Kästel T, Heiland S, Bäumer P, Bartsch AJ, Bendszus M, Pham M (2011) Magic angle effect: a relevant artifact in MR neurography at 3T? AJNR Am J Neuroradiol 32:821–827
Husarik DB, Saupe N, Pfirrmann CW, Jost B, Hodler J, Zanetti M (2009) Elbow nerves: MR findings in 60 asymptomatic subjects – normal anatomy, variants, and pitfalls. Radiology 252:148–156
Thawait SK, Chaudhry V, Thawait GK, Wang KC, Belzberg A, Carrino JA et al (2011) High-resolution MR neurography of diffuse peripheral nerve lesions. AJNR Am J Neuroradiol 32:1365–1372
Chhabra A, Carrino JA, Farahani SJ, Thawait GK, Sumner CJ, Wadhwa V et al (2016) Whole-body MR neurography: Prospective feasibility study in polyneuropathy and Charcot-Marie-Tooth disease. J Magn Reson Imaging 44:1513–1521
Vaeggemose M, Vaeth S, Pham M, Ringgaard S, Jensen UB, Tankisi H et al (2017) Magnetic Resonance Neurography and Diffusion Tensor Imaging of the peripheral nerves in patients with CMT Type 1A. Muscle Nerve. doi:10.1002/mus.25691
Trivedi JR, Phillips L, Chhabra A (2015) Hereditary and acquired polyneuropathy conditions of the peripheral nerves: clinical considerations and MR neurography imaging. Semin Musculoskelet Radiol 19:130–136
Staff NP, Amrami KK, Howe BM (2015) Magnetic resonance imaging abnormalities of peripheral nerve and muscle is common in amyotrophic lateral sclerosis and share features with multifocal motor neuropathy. Muscle Nerve 52:137–139
Pham M, Oikonomou D, Bäumer P, Bierhaus A, Heiland S, Humpert PM et al (2011) Proximal neuropathic lesions in distal symmetric diabetic polyneuropathy: findings of high-resolution magnetic resonance neurography. Diabetes Care 34:721–723
Vaeggemose M, Pham M, Ringgaard S, Tankisi H, Ejskjaer N, Heiland S et al (2017) Magnetic Resonance Neurography Visualises Abnormalities in Sciatic and Tibial Nerves in Patients with Type 1 Diabetes and Neuropathy. Diabetes. doi:10.2337/db16-1049
Wu C, Wang G, Zhao Y, Hao W, Zhao L, Zhang X et al (2016) Assessment of tibial and common peroneal nerves in diabetic peripheral neuropathy by diffusion tensor imaging: a case control study. Eur Radiol. doi:10.1007/s00330-016-4698-3
Kollmer J, Hund E, Hornung B, Hegenbart U, Schönland SO, Kimmich C et al (2015) In vivo detection of nerve injury in familial amyloid polyneuropathy by magnetic resonance neurography. Brain 138:549–562
Guggenberger R et al (2012) Assessment of median nerve with MR neurography by using diffusion-tensor imaging: normative and pathologic diffusion values. Radiology 265:194–203
Boyer RB, Kelm ND, Riley DC, Sexton KW, Pollins AC, Shack RB et al (2015) 4.7-T diffusion tensor imaging of acute traumatic peripheral nerve injury. Neurosurg Focus 39:E9
Kasprian G et al (2015) Peripheral nerve tractography in soft tissue tumors: a preliminary 3-tesla diffusion tensor magnetic resonance imaging study. Muscle Nerve 51:338–345
Chhabra A, Belzberg AJ, Rosson GD, Thawait GK, Chalian M, Farahani SJ et al (2016) Impact of high resolution 3 tesla MR neurography (MRN) on diagnostic thinking and therapeutic patient management. Eur Radiol 26:1235–1244
Fisher S, Wadhwa V et al (2016) Clinical impact of magnetic resonance neurography in patients with brachial plexus neuropathies. Br J Radiol 89:20160503
Andreisek G, Burg D, Studer A, Weishaupt D (2008) Upper extremity peripheral neuropathies: role and impact of MR imaging on patient management. Eur Radiol 18:1953–1961
Kwee RM, Chhabra A, Wang KC, Marker DR, Carrino JA (2014) Accuracy of MRI in diagnosing peripheral nerve disease: a systematic review of the literature. AJR Am J Roentgenol 203:1303–1309
Acknowledgements
The authors acknowledge the contribution of Mr. Jon Garinn in editing this manuscript and Dr. Jaya Trivedi for editing the electrophysiology section of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Avneesh Chhabra, MD.
Conflict of interest
The authors of this manuscript declare relationships with the following companies
Avneesh Chhabra
AC has received prior research grants from GE-AUR (GERRAF), Siemens Medical Solutions, Gatewood Fellowship Award and Integra Life Sciences unrelated to this work. He serves as a research consultant with ICON Medical group. He also receives book royalties from Jaypee, Elsevier and Wolters Kluwer.
Ananth Madhuranthakam
None.
Gustav Andreisek
Gustav Andreisek was co-worker of a study that resulted in a US patent (USPTO Number 12/947,256). He has received grants from the Swiss National Science Foundation (SNCF), Holcim, MayenfischTtrust and Siemens. He is currently Co-PI or Sub-PI in several third party-funded clinical trials at the University of Zurich where renumeration is given to the department he works for (sponsors include: Millennium Pharmaceuticals, Eli Lilly, GlaxoSmithKline, Cytheris SA, Roche, BioChemics, Novartis, Bristol-Meyers Squibb, TopoTarget, Otsuka and Merck Sharp & Dohme). The department also receives grants from Bayer and Guerbet and has ongoing research collaborations with Siemens, GE and Philips. Gustav Andreisek has given workshops and talks at a congress which was sponsored by Mepha Pharma AG, Switzerland, and received a speaker fee. He also gives talks at Lunch symposia and CME courses, which are organized and sponsored by Guerbet AG, and receives speakers fees and travel reimbursements. He served as a consultant for Otsuka Pharmaceutical Europe Ltd and Siemens Healthcare AG, Germany, and received a consultancy fee and reimbursement of travel costs. Furthermore, he has been invited in the past by AGFA, Bracco, GE, Philips and Siemens for official company receptions at international radiological congresses (RSNA, ECR, SGR). As a book author, Gustav Andreisek receives royalties from Springer, Heidelberg and as author of CME articles, he receives royalties from Rheuma Schweiz.
The other authors declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Funding
The authors state that this work has not received any funding.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was not required for this study because it is a review article.
Ethical approval
Institutional Review Board approval was not required because it is a review article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(PPTX 49 kb)
Rights and permissions
About this article
Cite this article
Chhabra, A., Madhuranthakam, A.J. & Andreisek, G. Magnetic resonance neurography: current perspectives and literature review. Eur Radiol 28, 698–707 (2018). https://doi.org/10.1007/s00330-017-4976-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-017-4976-8