Abstract
GPA with pituitary involvement is a rare condition which is prone to be misdiagnosed. The aim of this study was to summarize clinical features of pituitary involvement in GPA and facilitate early diagnosis. Twelve GPA patients were retrospectively analyzed at a single hospital between 2000 and 2017. A literature review was conducted to compare previous findings with our clinical results. The incidence rate of pituitary involvement in GPA was 3.9% (12/304) without sexual predilection. Other impairments included ear, nose and throat (n = 12), oculi (n = 10), lung (n = 6), meninges (n = 4), kidney (n = 3), and skin (n = 2). Antineutrophil cytoplasmic antibodies (ANCA) were positive in all patients with lung or kidney involvement (n = 6/6), while ANCA were negative in almost all patients without lung or kidney involvement (n = 5/6). Endocrine abnormalities included central diabetes insipidus (CDI, n = 11/12) hypogonadotropic hypogonadism (n = 6/11), adrenocorticotropic hormone deficiency (n = 4/7), thyroid-stimulating hormone deficiency (n = 5/11), and growth hormone deficiency (n = 3/9). Enlarged pituitary gland (n = 6), absence of posterior hyperintense signal on T1-weighed images (n = 11) and hypertrophic cranial pachymeningitis (n = 4) were common radiological manifestations. After treatment, nine patients experienced remission but one died. Pituitary images of 3/4 patients showed size of pituitary lesions decreased. CDI was not alleviated and hypopituitarism remained in two patients. Pituitary involvement in GPA can occur at any time throughout the course of disease, including at the initial presentation. GPA could not be excluded based on negative-ANCA in patients with pituitary abnormality alone. CDI and hypogonadotropic hypogonadism are dominant endocrine abnormalities. Systemic diseases may alleviate and pituitary images may improve after treatment, though the recovery of pituitary function is rare.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Granulomatosis with polyangiitis (GPA) is characterized by necrotizing granulomatous vasculitis affecting small to medium vessels. The typical manifestation is a triad syndrome, including lesions of ear, nose and throat (ENT), pulmonary vasculitis and glomerulonephritis. Central nervous system (CNS) involvement occurs in 7–11% of patients [1]. Patients usually present with hypertrophic cranial pachymeningitis (HCP), stroke, encephalitis, and epilepsy.
Pituitary involvement is a rare manifestation. It was first described by Ahlstrom in 1953 [2]. From 1983 to 2017, 26 case reports [3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28] and 2 retrospective cohort studies [29, 30] were published on PubMed. Central diabetes insipidus (CDI) and hypogonadotropic hypogonadism were the prominent endocrine features in patients with pituitary involvement [29,30,31]. A correct diagnosis is difficult to determine without positive-ANCA or a typical triad syndrome in GPA patients with pituitary involvement. Furthermore, many cases are inclined to be misdiagnosed as lymphocytic hypophysitis, pituitary abscess or tuberculosis. In this retrospective clinical study, clinical features of 12 cases of patients with GPA and pituitary involvement were reviewed. Additionally, a literature review was conducted to compare previous findings with data from our study and to ascertain clinical features of pituitary involvement in GPA patients.
Methods
Patient cohort and inclusion criteria
Patients with GPA and pituitary involvement, admitted to Peking Union Medical College Hospital (PUMCH) between January 2000 and December 2017, were evaluated in this retrospective study. The query terms used to search pituitary involvement in GPA were “pituitary involvement”, “hypopituitarism”, “panhypopituitarism”, “pituitary neoplasm”, and “diabetes insipidus”. The included patients met all of the following criteria: (1) patients were diagnosed with GPA according to the 2017 ACR/EULAR classification criteria [32]; (2) pituitary involvement, including CDI, and/or hypopituitarism, and/or abnormalities in pituitary magnetic resonance images (MRIs); (3) other causes of pituitary dysfunction could be excluded, such as infection and tumor. Two authors (Gu Y and Sun XF) independently investigated the medical records of patients who appeared to meet the inclusion criteria and they filled out data collection forms. Any discrepancy between the two authors was resolved by discussion with a third author (Mao JF).
Laboratory examination and hormonal assessment
The erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) were measured on admission. Antineutrophil cytoplasmic antibodies (ANCA) were measured by indirect immunofluorescence as well as proteinase 3 (PR3) and myeloperoxidase (MPO) antigen-specific immunometric assays. Lumbar puncture was conducted and cerebrospinal fluid was collected for routine and biochemistry tests.
CDI was diagnosed by polyuria (24 h urine volume > 3 l) with a good response to desmopressin therapy. Hypogonadotropic hypogonadism was defined as low level of serum testosterone or estradiol accompanied with inappropriately low or normal luteinizing hormone (LH) and follicle-stimulating hormone (FSH) levels. Thyroid-stimulating hormone (TSH) deficiency was defined as a low serum-free thyroxin level (< 1.04 ng/dl) associated with an inappropriately low or normal serum TSH level. Adrenocorticotropic hormone (ACTH) deficiency was defined as a morning cortisol value of less than 5 µg/dl (8am) associated with an inappropriately low or normal ACTH level. Growth hormone (GH) deficiency was defined as insulin-like growth factor (IGF-1) level lower than age-matched normal range. No one underwent stimulation tests.
Radiological assessment
Magnetic resonance images were used to evaluate the pituitary gland and sella turcica. The abnormalities of MRIs were defined by the reports from radiologists. The dimensions of the pituitary gland, gadolinium enhancement, posterior hyperintense signal of pituitary on T1-weighed images (T1WI) with or without HCP, and involvement of adjacent tissue were summarized.
Activity of GPA
The Birmingham vasculitis activity score (BVAS) was calculated at the onset of pituitary dysfunction and at the conclusion of follow-up. Two authors (Gu Y and Sun XF) independently evaluated BVAS of patients according to BVAS version 3.0 [33]. Disagreements were resolved by consensus.
Treatment and prognosis
Immunosuppressive therapy and hormone replacement therapy were administrated. The follow-up times (from discharge to the last out-patient visit) and activity of GPA (BVAS) at the conclusion of follow-up were recorded. Pituitary hormones and pituitary MRIs of some patients were repeatedly measured during follow-up.
Statistical analysis
The descriptive results were presented as percentages and ranges if necessary.
Search strategy for literature review
We used the terms “granulomatosis with polyangiitis” or “Wegener’s granulomatosis” and “diabetes insipidus” or “hypopituitarism” or “pituitary abnormality” to identify the relevant articles between 1983 and 2017 on PubMed. The language of evaluated articles was limited to English. Inclusion criteria were defined as follows: (1) diagnosis of GPA was based upon the 2017 ACR/EULAR classification criteria; (2) pituitaries with abnormalities in function and/or morphology; (3) cases with well-documented clinical information. Patients with secondary vasculitis or other autoimmune diseases, such as drug-induced vasculitis or autoimmune thyroiditis, were excluded. The applicable cases were selected by two investigators (Zhang T and Peng M) independently. Discrepancies were resolved by discussing with an additional author (Shi JH).
Results
Patient characteristics
Among 304 patients diagnosed with GPA between January 2000 and December 2017 in the PUMCH administration database, 12 (3.9%) inpatients were identified as having pituitary dysfunction related to GPA. Half of them were female. The average age at the onset of GPA was 48 years (range 19–64 years).
Clinical manifestations
Two patients presented with polydipsia and polyuria as their first symptoms. Other patients presented with initial symptoms of headache (n = 4), hearing loss (n = 1), blurred vision (n = 1), conjunctivitis (n = 1), ophthalmodynia (n = 1), fever and expectoration (n = 1) and dry cough (n = 1). The lag time between occurrence of initial symptom presentation and pituitary dysfunction ranged from 0 to 103 months. The BVAS, calculated when pituitary symptoms emerged, ranged between 0 and 27. During the course of GPA, ENT manifestations appeared in all patients. Other organ involvement included ocular impairment in ten patients (83.3%), CNS (other structures of CNS except pituitary) involvement in seven patients (58.3%, including 4 patients with HCP), lower respiratory tract involvement in five patients (41.7%), albuminuria in two patients (16.7%), and skin ulceration in two patients (16.7%). Demographics and clinical characteristics are summarized in Table 1.
Laboratory findings
Inflammatory markers, including erythrocyte sedimentation rate and C-reactive protein, increased in 11 patients (91.7%). Seven patients were ANCA-positive (Table 1). All patients with lung or kidney involvement were ANCA-positive (patients 1, 2, 3, 5, 7, and 12). All patients without lung and kidney involvement were ANCA-negative, except Patient 8 who had a low titer of p-ANCA 1:10. Six patients presented with increased cerebrospinal fluid (CSF) pressure (> 180 mmH2O). In general, CSF biochemical markers were normal aside from slightly increased protein (n = 6) and glucose levels (n = 2).
Hormonal evaluation
Central diabetes insipidus presented in 11 patients (91.7%) and all of them responded well to desmopressin. Hypogonadotropic hypogonadism was confirmed in 6/11 patients (54.5%). TSH deficiency was noted in 5/11 patients (45.5%). ACTH deficiency was identified in 4/7 patients (57.1%) before glucocorticoid treatment started. GH deficiency was found in 3/9 patients (33.3%). Prolactin was slightly elevated in 1/11 patients. The hormonal evaluation data are outlined in Supplemental Table 1.
Radiological evaluation
Pituitary MRIs were conducted in all patients. Six patients had enlarged pituitary glands with heights exceeding 8 mm. Six pituitaries revealed homogenous enhancement and two showed peripheral enhancement and central cystic hypo-intensive images. One patient presented with heterogeneous enhancement in the pituitary gland. The posterior hyperintense signal was absent in 11/12 patients. Only Patient 6 had a normal posterior hyperintense signal and normal urine volume during the follow-up. HCP was found in four patients (Fig. 1). The pituitary lesions could invade cavernous sinus (n = 5) and compress the optic chiasma (n = 1). The main features of pituitary MRIs are summarized in Table 2.
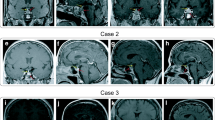
HCP and pituitary enlargement in Patient 4 and Patient 6. Patient 4 (a–c): sagittal T1WI scan (a) shows an enlarged pituitary gland (1.99 × 0.93 × 1.13 cm) with heterogeneous enhancement after gadolinium administration (b). The thickened meninges (white arrow), invading bilateral cavernous sinus, indicate HCP (c). Patient 6 (d–f): sagittal T1WI scan (d), enhancement sagittal (e) and coronal T1WI (f) show thickened meninges occupying the sella turcica region completely (white arrow)
Pathology of pituitary
Seven patients underwent biopsy, including lung (n = 2, Patient 1, 2), nasal sinus (n = 2, Patient 8, 11), mastoid process (n = 1, Patient 10), pituitary (n = 1, Patient 6), skin (n = 1, Patient 1), and bronchial mucosa (n = 1, Patient 12). Pituitary biopsy in Patient 6 revealed polyclonal B and T lymphocytes infiltration (Fig. 2), supporting the diagnosis of lymphocytic hypophysitis.
Treatment and follow-up
All patients were treated with corticosteroids (Table 3). Four patients received pulse therapy (methylprednisolone 500–1000 mg/day, intravenously administrated for 3 days, followed by high-dose corticosteroids). The remaining eight patients received high-dose corticosteroids (equivalent to prednisone 0.8–1 mg/kg/day). Cyclophosphamide and other immunosuppressive agents were administrated for all patients, such as ciclosporin (n = 2), tacrolimus (n = 2), methotrexate (n = 1), mycophenolate mofetil (n = 1) and leflunomide (n = 1). Patient 1 received rituximab therapy due to his poor response to the conventional therapy. The follow-up periods ranged from 1 to 133 months. Nine patients remained in remission (BVAS = 0–2) at the end of follow-up under low-dose corticosteroids with or without immunosuppressive agents. Patient 8 died 1 month following discharge due to severe intracranial hypertension. Patient 12 was diagnosed with myelodysplastic syndrome related to long-term use of cyclophosphamide after 133 months. Patient 10 was unable to be contacted for follow-up.
Desmopressin was given to all patients with CDI. Patient 2 received levothyroxine for replacement therapy. No growth or sex hormone replacement was given. During the follow-up, all patients with CDI were still on desmopressin treatment. Pituitary hormones, retested in two patients, did not recover to normal range after immunosuppressive treatment. Pituitary MRIs were reevaluated in four patients, and the size of lesions decreased in three patients but increased in one patient.
Literature review
Between 1983 and 2017, 51 cases (2 case series and 26 case reports) of GPA with pituitary involvement have been published on PubMed (Supplemental Tables 2 and 3). The average age at the diagnosis of pituitary dysfunction was 42 years (range 16–77 years) with female predilection (74.5%). The pituitary dysfunction preceded additional organ involvement in 10 patients (15.7%) [4, 5, 7, 15, 18,19,20, 23, 30], was concomitant in 16 patients (31.3%) [5, 8, 12,13,14, 16, 18, 24, 26, 28,29,30], and appeared subsequently in 25 patients (49.0%) [3, 4, 6, 9,10,11, 17, 21, 22, 25,26,27, 29, 30].
The ANCA-positive rate was 91.3% in the literature review. However, ANCA assessment was performed at different times over the course of GPA. ENT (84.3%) were the most common involved organs, followed by lung (51.0%), kidney (39.2%), oculi (31.5%), peripheral nerve system (19.6%), skin (15.7%), and gastrointestinal tract (3.9%). CDI (86%, 43/50) was the most frequent endocrine abnormality and one patient was undergoing dialysis at the beginning of the study. Other pituitary dysfunction included, listed in decreasing frequency, hypogonadotropic hypogonadism (68.3%, 28/41), TSH deficiency (51.2%, 22/43), ACTH deficiency (48.1%, 13/27), hyperprolactinemia (42.5%, 17/40), and GH deficiency (28.1%, 9/32). Due to cyclophosphamide administration, sex hormone was not measured in two patients. ACTH of 16 patients could not be evaluated due to the administration of glucocorticoid in these patients. Pituitary MRIs of 48 patients were available. The common lesions included enlarged pituitary glands (91.1%, 41/45), pituitary glands enhanced after gadolinium injection on T1WI (93.8%, 30/32), and absence of posterior hyperintense signal of pituitary on T1WI (84.6%, 22/26). The clinical manifestations, hormone evaluation and pituitary MRIs are shown in Supplemental Table 2.
The majority of patients received glucocorticoid therapy (94.1%). Cyclophosphamide (n = 32) was the most widely used immunosuppressive agent, followed by methotrexate (n = 6), mycophenolate mofetil (n = 3), and acetazolamide (n = 3). In addition, other therapeutic strategies included rituximab (n = 7), infliximab (n = 5), intravenous immunoglobulin (n = 2), plasma exchange (n = 1), and 15-deoxyspergualin (n = 1). Following treatment, the systemic manifestations of GPA were alleviated in 27 patients and pituitary size decreased in 26 patients. However, endocrine abnormalities were improved in only a minor subset of patients, including decrease of urine volume (n = 9), improvement of hypogonadotropic hypogonadism (n = 5), increase in ACTH (n = 1, most patients were administrated with glucocorticoid), increase in TSH (n = 3), and decrease in prolactin (n = 5). The treatment and follow-up results are summarized in Supplemental Table 3.
Discussion
This study found that pituitary involvement occurred in 3.9% (12/304) patients with GPA. To our knowledge, this is the largest sample size from a tertiary academic hospital. Among these patients, the positive rate of ANCA was remarkably higher in patients with lung and/or kidney involvement compared to patients without. CDI and hypogonadotropic hypogonadism were the dominant endocrine abnormalities. Enlarged pituitary glands and the absence of posterior hyperintense signal on T1WI were common features on pituitary MRIs. After immunosuppressive treatment, the pituitary could decrease in dimensions, while CDI and hypopituitarism could not recover in most cases.
The incidence rate of pituitary involvement in GPA seemed to be underestimated due to the symptoms of hypopituitarism being closely associated with GPA systemic manifestations. The incidence rate of 3.9% was slightly higher than 1.1–1.3% previously reported in two case series reports [29, 30]. Pituitary involvement affected males and females equally in our center, but the majority of patients assessed in the literature review were female. The average age at the onset of GPA in our cohort was 48 years, which was similar to the studies from Mayo Clinic [30], French Vasculitis Study Group [29] and the literature review (48, 46, and 42 years, respectively).
The pathogenesis of pituitary involvement was speculated to be related to granuloma invasion from the adjacent organs (ENT, oculi, meninges), vasculitis of the pituitary gland itself, or granulomatous formation in situ [34]. Involvement rates of ENT, oculi and meninges (presented as HCP) were 100%, 83.3%, and 25%, respectively, in our participants, which were higher than the general GPA population (ENT 70–100% [35], oculi 50–58% [36], meninges/HCP 0.6–13.8% [37, 38]). In the literature review, we found that ENT impairment was common as well. Previous studies showed that ENT lesions were positively associated with CNS involvement [34, 37]. The above evidence supports granuloma extension from ENT, orbits and meninges as the main mechanism of pituitary involvement. Surprisingly, the only pituitary biopsy obtained from Patient 6 merely revealed lymphocyte infiltration. GPA was diagnosed according to clinical manifestations and positive-ANCA detection occurred subsequently, and lymphocytic hypophysitis was considered as a secondary response to GPA. This result expanded our knowledge on the pathology of pituitary involvement in GPA.
Pituitary involvement can occur at any time, before or after other organs are involved. Our literature review revealed that most of pituitary dysfunction occurs concurrently or following additional organ involvement (prior, concurrent, and post organ involvement percentages are 15.7%, 31.3%, and 49.0%, respectively). Nevertheless, pituitary impairment can be the only initial abnormality as well, which deserves more attention in the field. Polydipsia and polyuria were the first symptoms in two patients in our study. Patient 3 presented with polyuria and polydipsia, while her ANCA assessment was initially negative. Two months later, the patient visited the hospital for expectoration and exertional dyspnea. Computed tomography of chest revealed pulmonary opacities distributed along bronchovascular bundles (Fig. 3). Her ANCA reassessment resulted in a positive reading (p-ANCA 1:80 and MPO-ANCA 78 RU/ml), leading to the diagnosis of GPA. After treatment with glucocorticoids and cyclophosphamide, lesions in pituitary and lung resolved simultaneously, accompanied with negative-converted ANCA. For this reason, the diagnosis of GPA cannot be excluded in patients that only present with initial pituitary dysfunction. Conversely, the onset of pituitary dysfunction can lag behind the impairment of other organs for up to 103 months (Patient 7). A previous case report showed that pituitary abnormality could occur even when the disease was stable [39]. According to these results, pituitary involvement does not synchronize with additional organ involvement in GPA.
Changes of pituitary and lung images in Patient 3. Polyuria, polydipsia accompanied with a mass in neurohypophysis (a) lead to a diagnosis of CDI. Patient 3 had a normal lung (b) and initial negative-ANCA. Two months later, pituitary was still enlarged (c). And expectoration, lung opacity (d) and positive serum ANCA (p-ANCA 1:80 and MPO-ANCA 78 RU/ml) resulted in diagnosis of GPA. After treatment, pituitary mass, lung opacity and positive ANCA disappeared (e, f). GPA granulomatosis with polyangiitis, CDI central diabetes insipidus
Positive ANCA seemed to be more closely related to lung or kidney rather than pituitary involvement. In our study, the diagnosis of six patients, whose lesions were limited to ENT, oculi and CNS, was difficult with negative-ANCA. But according to 2017 ACR/EULAR classification criteria, three patients (Patients 4, 6, and 9) were diagnosed with GPA due to severe nasal symptoms, hearing loss and oculi damages. Increased inflammation makers, HCP, response to immunosuppressive therapy and subsequent acquisition of positive ANCA supported the diagnosis as well. Another three patients were diagnosed with GPA because granulomatous lesions were discovered by biopsy at the nasal sinus (Patients 8, 11) and mastoid process (Patient 10). Our cohort study showed that all patients with lung and/or kidney involvement (6/12) were ANCA-positive, while patients with lesions limited to head and upper respiratory tract were almost ANCA-negative. GPA is traditionally classified into localized and systemic forms, according to the involved organs [40]. The former is localized to the upper respiratory tract with an ANCA-positive rate 50–80%. The latter involves kidney and/or lung with ANCA-positive rates above 90%. These findings provide further evidence that negative-ANCA does not exclude the diagnosis of GPA in patients with pituitary mass who do not have lung or kidney impairment.
Consistent with the literature review, CDI and hypogonadotropic hypogonadism were the most common endocrine presentations. Patients presented with CDI in almost all patients in our study. Life-threatening conditions such as dehydration and electrolyte disturbance can be caused by CDI. The pituitary–gonadal axis was mostly involved in patients with hypopituitarism. However, for patients with chronic disease, hypogonadotropic hypogonadism is difficult to identify based on symptoms, such as amenorrhea or low libido, since administration of cyclophosphamide directly impairs gonadal function as well. The pituitary–adrenal axis is also difficult to evaluate because levels of ACTH and cortisol are inevitably influenced by dosing of corticosteroids that surpass physiological levels. 4-Hydroxycyclophosphamide is a bioactive metabolite of cyclophosphamide. Studies have confirmed that severe hypothyroidism can reduce the concentration of 4-hydroxycyclophosphamide, potentially resulting in treatment failure [41]. Therefore, thyroid hormone replacement therapy is necessary. In our study, levothyroxine was prescribed to one patient who had a very low level of free thyroxine (FT4 = 0.547 ng/dl).
The typical MRIs of pituitary involvement in GPA showed enlarged pituitary gland, absence of posterior hyperintense signal on T1WI, HCP and lesions invading cavernous sinus. Most pituitary diseases present as pituitary enlargement, including adenoma and lymphocytic hypophysitis, and the diagnosis is determined by pituitary biopsy. HCP is considered as granulomatous inflammation of meninges in GPA [42]. It usually manifests with symptoms of headache and cranial nerves paralysis. HCP frequently invades the falx cerebri and tentorium cerebelli but is seldom around cavernous sinus [43]. When cavernous sinus is involved on imaging, pituitary impairment should be suspected (Fig. 1). Furthermore, sinusitis, mastoiditis and orbit mass in MRIs likely indicate a diagnosis of GPA. Enlarged pituitary glands can shrink after immunosuppressive treatment, which was confirmed in our study and literature review. However, for some patients with progressive disease, pituitary resection surgeries were needed to relieve the oppression of granulomatosis [7, 26, 30].
Most patients remained in remission from GPA after immunosuppressive therapy, while hypopituitarism and CDI were not alleviated. The BVAS and its modifications were the most widely used tools for disease activity assessment in ANCA-associated vasculitis. The BVAS of seven patients decreased dramatically after treatment, indicating relief of GPA. Patient 1 experienced remission after rituximab infusion, while hypogonadotropic hypogonadism and TSH deficiency still remained after treatment. Irreversible hypopituitarism may be caused by permanent damage and fibrous tissue replacement in the pituitary. The damage to neurohypophysis is also irreversible, and desmopressin is needed for the foreseeable future. In the literature review, the improvement of CDI and hypopituitarism was rare as well. On the contrary, a case series revealed that 83% (5/6) of CDI patients recovered from the disease [30]. They concluded that early diagnosis and treatment potentially made a contribution to the resolution of CDI. Therefore, hormone replacement therapy for the duration of the patients’ lives would be necessary for most patients.
Several limitations of this study should be addressed. First, in this retrospective study, pituitary images were only reevaluated in four patients and two of them had repeated pituitary function during the follow-up. Second, only one patient received pituitary biopsy and the result showed polyclonal lymphocyte infiltration.
In conclusion, pituitary involvement in GPA can occur before or after other systemic impairment and even as the initial presentation. Almost all patients without lung or kidney impairment were ANCA-negative, while all patients with lung or/kidney impairment were ANCA-positive. These findings indicate that negative-ANCA cannot eliminate the diagnosis of GPA especially for patients without lung or kidney involvement. CDI and hypogonadotropic hypogonadism were the most common endocrine manifestations. Immunosuppressive treatment could notably improve systemic disease and pituitary imaging, while the reversal of anterior and posterior pituitary function was seldom obtained.
References
Choi HA, Lee MJ, Chung CS (2017) Characteristics of hypertrophic pachymeningitis in patients with granulomatosis with polyangiitis. J Neurol 264(4):724–732. https://doi.org/10.1007/s00415-017-8416-0
Ahlstrom CG, Liedholm K, Truedsson E (1953) Respirato-renal type of polyarteritis nodosa. Acta Med Scand 144(5):323–332
Tsuji H, Yoshifuji H, Fujii T, Matsuo T, Nakashima R, Imura Y, Yukawa N, Ohmura K, Sumiyoshi S, Mimori T (2017) Visceral disseminated varicella zoster virus infection after rituximab treatment for granulomatosis with polyangiitis. Mod Rheumatol 27(1):155–161. https://doi.org/10.3109/14397595.2014.948981
Esposito D, Trimpou P, Giugliano D, Dehlin M, Ragnarsson O (2017) Pituitary dysfunction in granulomatosis with polyangiitis. Pituitary 20(5):594–601. https://doi.org/10.1007/s11102-017-0811-0
Al-Fakhouri A, Manadan A, Gan J, Sreih AG (2014) Central diabetes insipidus as the presenting symptom of granulomatosis with polyangiitis. J Clin Rheumatol 20(3):151–154. https://doi.org/10.1097/rhu.0000000000000093
Slabu H, Arnason T (2013) Pituitary granulomatosis with polyangiitis. BMJ Case Rep. https://doi.org/10.1136/bcr-2013-008656
Pereira EA, Plaha P, Hofer M, Karavitaki N, Cudlip SA (2013) Hypophyseal Wegener’s granulomatosis presenting by visual field constriction without hypopituitarism. Clin Neurol Neurosurg 115(6):762–764. https://doi.org/10.1016/j.clineuro.2012.06.041
Kara O, Demirel F, Acar BC, Cakar N (2013) Wegener granulomatosis as an uncommon cause of panhypopituitarism in childhood. J Pediatr Endocrinol Metab JPEM 26(9–10):959–962. https://doi.org/10.1515/jpem-2013-0033
Tenorio Jimenez C, Montalvo Valdivieso A, Lopez Gallardo G, McGowan B (2011) Pituitary involvement in Wegener’s granulomatosis: unusual biochemical findings and severe malnutrition. BMJ Case Rep 1:1. https://doi.org/10.1136/bcr.02.2011.3850
Santoro SG, Guida AH, Furioso AE, Glikman P, Rogozinski AS (2011) Panhypopituitarism due to Wegener’s granulomatosis. Arq Bras Endocrinol Metab 55(7):481–485
Barlas NB, Hassan HH, Al Badr FB, Bilal A (2011) Structural and functional involvement of pituitary gland in Wegener’s granulomatosis. Clin Neuroradiol 21(1):31–33. https://doi.org/10.1007/s00062-010-0037-2
Xue J, Wang H, Wu H, Jin Q (2009) Wegener’s granulomatosis complicated by central diabetes insipidus and peripheral neutrophy with normal pituitary in a patient. Rheumatol Int 29(10):1213–1217. https://doi.org/10.1007/s00296-008-0774-6
Yong TY, Li JY, Amato L, Mahadevan K, Phillips PJ, Coates PS, Coates PT (2008) Pituitary involvement in Wegener’s granulomatosis. Pituitary 11(1):77–84. https://doi.org/10.1007/s11102-007-0021-2
Thiryayi W, Donaldson MH, Border D, Tyagi A (2007) An enhancing pituitary lesion in a young woman: a diagnostic dilemma. J Clin Neurosci 14(3):286–288. https://doi.org/10.1016/j.jocn.2005.12.005
McIntyre EA, Perros P (2007) Fatal inflammatory hypophysitis. Pituitary 10(1):107–111. https://doi.org/10.1007/s11102-007-0016-z
Spisek R, Kolouchova E, Jensovsky J, Rusina R, Fendrych P, Plas J, Bartunkova J (2006) Combined CNS and pituitary involvement as a primary manifestation of Wegener granulomatosis. Clin Rheumatol 25(5):739–742. https://doi.org/10.1007/s10067-005-0065-5
Seror R, Mahr A, Ramanoelina J, Pagnoux C, Cohen P, Guillevin L (2006) Central nervous system involvement in Wegener granulomatosis. Medicine 85(1):54–65. https://doi.org/10.1097/01.md.0000200166.90373.41
Dutta P, Hayatbhat M, Bhansali A, Bambery P, Kakar N (2006) Wegener’s granulomatosis presenting as diabetes insipidus. Exp Clin Endocrinol Diabetes 114(9):533–536. https://doi.org/10.1055/s-2006-924122
Duzgun N, Morris Y, Gullu S, Gursoy A, Ensari A, Kumbasar OO, Duman M (2005) Diabetes insipidus presentation before renal and pulmonary features in a patient with Wegener’s granulomatosis. Rheumatol Int 26(1):80–82. https://doi.org/10.1007/s00296-005-0583-0
Tao J, Dong Y (2003) Pituitary involvement in Wegener’s granulomatosis: a case report and review of the literature. Chin Med J 116(11):1785–1788
Woywodt A, Knoblauch H, Kettritz R, Schneider W, Gobel U (2000) Sudden death and Wegener’s granulomatosis of the pituitary. Scand J Rheumatol 29(4):264–266
Goyal M, Kucharczyk W, Keystone E (2000) Granulomatous hypophysitis due to Wegener’s granulomatosis. AJNR Am J Neuroradiol 21(8):1466–1469
Miesen WM, Janssens EN, van Bommel EF (1999) Diabetes insipidus as the presenting symptom of Wegener’s granulomatosis. Nephrol Dial Transplant 14(2):426–429
Katzman GL, Langford CA, Sneller MC, Koby M, Patronas NJ (1999) Pituitary involvement by Wegener’s granulomatosis: a report of two cases. AJNR Am J Neuroradiol 20(3):519–523
Bertken RD, Cooper VR (1997) Wegener granulomatosis causing sellar mass, hydrocephalus, and global pituitary failure. West J Med 167(1):44–47
Roberts GA, Eren E, Sinclair H, Pelling M, Burns A, Bradford R, Maurice-Williams R, Black CM, Finer N, Bouloux PM (1995) Two cases of Wegener’s granulomatosis involving the pituitary. Clin Endocrinol 42(3):323–328
Czarnecki EJ, Spickler EM (1995) MR demonstration of Wegener granulomatosis of the infundibulum, a cause of diabetes insipidus. AJNR Am J Neuroradiol 16(4 Suppl):968–970
Hurst NP, Dunn NA, Chalmers TM (1983) Wegener’s granulomatosis complicated by diabetes insipidus. Ann Rheum Dis 42(5):600–601
De Parisot A, Puechal X, Langrand C, Raverot G, Gil H, Perard L, Le Guenno G, Berthier S, Tschirret O, Eschard JP, Vinzio S, Guillevin L, Seve P (2015) Pituitary involvement in granulomatosis with polyangiitis: report of 9 patients and review of the literature. Medicine 94(16):e748. https://doi.org/10.1097/md.0000000000000748
Kapoor E, Cartin-Ceba R, Specks U, Leavitt J, Erickson B, Erickson D (2014) Pituitary dysfunction in granulomatosis with polyangiitis: the Mayo Clinic experience. J Clin Endocrinol Metab 99(11):3988–3994. https://doi.org/10.1210/jc.2014-1962
Yong TY, Li JY (2014) Pituitary involvement in granulomatosis with polyangiitis. J Clin Rheumatol 20(3):123–124. https://doi.org/10.1097/RHU.0000000000000092
Yoo J, Kim HJ, Ahn SS, Jung SM, Song JJ, Park YB, Lee SW (2018) The utility of the ACR/EULAR 2017 provisional classification criteria for granulomatosis with polyangiitis in Korean patients with antineutrophil cytoplasmic antibody-associated vasculitis. Clin Exp Rheumatol 36 Suppl 111(2):85–87
Mukhtyar C, Lee R, Brown D, Carruthers D, Dasgupta B, Dubey S, Flossmann O, Hall C, Hollywood J, Jayne D, Jones R, Lanyon P, Muir A, Scott D, Young L, Luqmani RA (2009) Modification and validation of the Birmingham Vasculitis Activity Score (version 3). Ann Rheum Dis 68(12):1827–1832. https://doi.org/10.1136/ard.2008.101279
Tumiati B, Zuccoli G, Pavone L, Buzio C (2005) ENT Wegener’s granulomatosis can hide severe central nervous system involvement. Clin Rheumatol 24(3):290–293. https://doi.org/10.1007/s10067-004-1025-1
Greco A, Marinelli C, Fusconi M, Macri GF, Gallo A, De Virgilio A, Zambetti G, de Vincentiis M (2016) Clinic manifestations in granulomatosis with polyangiitis. Int J Immunopathol Pharmacol 29(2):151–159. https://doi.org/10.1177/0394632015617063
Tarabishy AB, Schulte M, Papaliodis GN, Hoffman GS (2010) Wegener’s granulomatosis: clinical manifestations, differential diagnosis, and management of ocular and systemic disease. Surv Ophthalmol 55(5):429–444. https://doi.org/10.1016/j.survophthal.2009.12.003
Fragoulis GE, Lionaki S, Venetsanopoulou A, Vlachoyiannopoulos PG, Moutsopoulos HM, Tzioufas AG (2018) Central nervous system involvement in patients with granulomatosis with polyangiitis: a single-center retrospective study. Clin Rheumatol 37(3):737–747. https://doi.org/10.1007/s10067-017-3835-y
Nishino H, Rubino FA, DeRemee RA, Swanson JW, Parisi JE (1993) Neurological involvement in Wegener’s granulomatosis: an analysis of 324 consecutive patients at the Mayo Clinic. Ann Neurol 33(1):4–9. https://doi.org/10.1002/ana.410330103
Cunnington JR, Jois R, Zammit I, Scott D, Isaacs J (2009) Diabetes insipidus as a complication of Wegener’s granulomatosis and its treatment with biologic agents. Int J Rheumatol 2009:346136. https://doi.org/10.1155/2009/346136
Comarmond C, Cacoub P (2014) Granulomatosis with polyangiitis (Wegener): clinical aspects and treatment. Autoimmun Rev 13(11):1121–1125. https://doi.org/10.1016/j.autrev.2014.08.017
Jang SY, Dooley MA, Joy MS (2013) Impact of severe hypothyroidism on cyclophosphamide disposition and routes of metabolism and transport in a patient with treatment-resistant lupus nephritis. Ann Pharmacother 47(7–8):e35. https://doi.org/10.1345/aph.1S012
Yokoseki A, Saji E, Arakawa M, Kosaka T, Hokari M, Toyoshima Y, Okamoto K, Takeda S, Sanpei K, Kikuchi H, Hirohata S, Akazawa K, Kakita A, Takahashi H, Nishizawa M, Kawachi I (2014) Hypertrophic pachymeningitis: significance of myeloperoxidase anti-neutrophil cytoplasmic antibody. Brain 137(Pt 2):520–536. https://doi.org/10.1093/brain/awt314
Reinhold-Keller E, de Groot K, Holl-Ulrich K, Arlt AC, Heller M, Feller AC, Gross WL (2001) Severe CNS manifestations as the clinical hallmark in generalized Wegener’s granulomatosis consistently negative for antineutrophil cytoplasmic antibodies (ANCA). A report of 3 cases and a review of the literature. Clin Exp Rheumatol 19(5):541–549
Acknowledgements
We acknowledged all patients included in this retrospective study.
Funding
The national Key Research and Development Program of China (2016YFA0101003) and CAMS Innovation Fund for Medical Sciences (CIFMS) (2017-I2M-3-007).
Author information
Authors and Affiliations
Contributions
YG and JS contributed to the conception of study. YG, XS and JM collected and summarized clinical data. TZ, MP and JS performed the literature review and summarized the results. YG, JM drafted the manuscript and made tables and figures. All authors approved the manuscript as submitted and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors state they have no conflict of interest.
Ethical approval
The study was approved by the Peking Union Medical College Hospital Institutional Review Board (Reference number: 2013-9-322).
Informed consent
Informed consent for use of all patients’ medical records was obtained from every participant and/or their guardian.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gu, Y., Sun, X., Peng, M. et al. Pituitary involvement in patients with granulomatosis with polyangiitis: case series and literature review. Rheumatol Int 39, 1467–1476 (2019). https://doi.org/10.1007/s00296-019-04338-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-019-04338-0