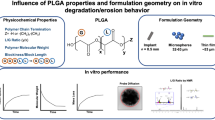
Abstract
In this study, poly(d,l-lactide-co-glycolide), PLGA, was developed as an in situ forming implants (ISFIs) to improve the therapeutic efficiency and to devoid the adverse effects of the Paclitaxel (PTX). ISFIs have received considerable attention as localized drug delivery systems. Different molecular weights of PLGA (502H, 503H, and 504H) were examined as an ISFI for PTX. In vitro experiments showed that PTX was released from PLGA over the course of 28 days. The profile of PTX release demonstrated a slow diffusion-controlled phase and afterward a more express degradation-controlled phase. The zero-order, first-order, Higuchi’s, and Weibull models were applied to drug release data in order to elucidate release mechanisms and kinetics. Therefore, to confirm the results of PTX release, the process of the polymer degradation is evaluated for the direct determination of the monomers, glycolic acid, and lactic acid, via a novel HPLC method and measurement of pH.
Graphic abstract

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Recently, an innovative ISFI has been developed that may be injected as a liquid that subsequently solidifies in situ [1,2,3]. In this case, the injectable implant system is comprised of a water-insoluble biodegradable polymer dissolved in a pharmaceutically acceptable water-miscible solvent. Upon intramuscular or subcutaneous injection into an aqueous environment, the biocompatible water-soluble solvent diffuses out of the polymer, while water diffuses into the polymer matrix. Due to the polymer’s insolubility in water, it coagulates or precipitates upon contact with water, thus resulting in a solid polymeric implant. Accordingly, the effective dosage formulation formed that could avoid surgical incision [4]. Also, the advantages of ISFIs are the less stressful preparation conditions and the less complicated preparation [5, 6].
Recently, in the pharmaceutical applications and medical devices, PLGA polymer as biodegradable implants has been broadly developed [7,8,9]. This polymer due to its biocompatibility, biodegradability, and safety, approval by the Food and Drug Administration (FDA) for human use, has attracted great interest [10,11,12,13]. PLGA implants can be loaded with different kinds of drugs [1, 14,15,16]. Drugs with small molecular weight, for example, anticancer drugs, antibiotics, analgesics, antiviral drugs, and steroids, have been loaded into PLGA polymer for implants preparation [17, 18]. Anticancer drugs, for example, 2-methoxyestradiol, PTX, and doxorubicin, can be delivered by the biodegradable implants for the treatment of cancer [19, 20].
PTX against a wide variety of tumors, for instance, ovarian cancer, lung cancer, breast cancer, and head and neck carcinomas, has shown significant activity [21]. PTX is mainly limited for the productively clinical application owing to its low solubility in water and many acceptable pharmaceutical solvents and subsequently low therapeutic index. Therefore, there is a need to develop favorable formulations for the administration of PTX [22].
Several studies have been carried out using different materials to achieve the controlled release of PTX from surgical implants of various forms. For example, Wang et al. fabricated PLGA 50:50 (MW 45,000:75,000) microspheres by spray-drying and reported the in vitro release of PTX [23]. Li et al. used implants based on polyphosphoester p(DAPG-EOP) polymer which released PTX close to 100 days in vitro [24]. Ong et al. synthesized PLGA foams for controlled release of PTX in the postsurgical chemotherapy against glioblastoma multiforme [25]. Von Eckardstein et al. used a nitrosoureas liquid crystalline cubic phase encapsulating carboplatin and PTX and reported a reduction in tumor sizes in F98 rat brains [26]. Elkharraz et al. worked with injectable PTX-loaded implants made of glycerol tripalmitate [27]. However, very high initial drug burst release or delayed-release followed by a burst, or inappropriate for postsurgical implantation in the resection cavity, is shortcoming of most of these devices. Hence, to resolve this problem, we need an alternative notable method.
In our previous works [28, 29], we have studied the effect of HSA microparticles (mHSA), aqueous stability of PTX in different release media, and different molecular weight of PLGA on the PTX release profile of the in situ forming PLGA systems. Based on our previous investigations on PLGA microsphere [28,29,30], in this study, we used PLGA to prepare ISFIs for delivery of PTX, which exhibit a minimal initial burst, near zero-order release kinetics, and efficient implant-ability. The overall objects of the present study are as follows:
-
1.
Preparation of ISFIs based on PLGA for PTX release with three different formulations.
-
2.
Biodegradation study of three different molecular weights of PLGA (low, medium, and high grade) on the release profile of the PTX from ISFI systems.
-
3.
The proposition of PTX release mechanism via relation among the PLGA degradation (amount of lactic acid (LA) and glycolic acid (GA)), pH, and release profile.
Materials and methods
Materials
PTX was a gift from nova spec (Norway), and PLGA copolymers (50:50; Resomer RG 502H, 503H, and 504H) were purchased from Boehringer Ingelheim; 7-epi-paclitaxel as an internal standard was supplied by LGC Standards (UK). Sodium hydroxide (NaOH), potassium dihydrogen phosphate (KH2PO4), dichloromethane (CH2Cl2), acetonitrile (CH3CN), and deionized water (H2O) as HPLC grade and N-methyl pyrrolidone (NMP) were purchased from Merck Chemicals (Germany). All the above materials were of the commercially highest grade.
Preparation of the ISFI systems
ISFIs were prepared by mixing PLGA copolymers (502H, 503H, 504H) and PTX with N-methyl-2-pyrrolidone (NMP) in two syringes until the formation of a clear solution: the 220 mg of PLGA and 3.33 mg of PTX with 432 mg of NMP solvent mixed (Scheme 1). The sample preparation was performed at ambient temperature, which was from three replicates.
Preparation of phosphate-buffered saline (PBS)
PBS solution was prepared according to US pharmacopeia conventions. Briefly, 13.6 g of potassium dihydrogen phosphate (0.1 mol) and 4.0 g of sodium hydroxide (0.1 mol) were separately dissolved in 500 mL of distilled water. Then, 250 mL of potassium dihydrogen phosphate solution, 173.5 mL of sodium hydroxide solution, and 500 mL distilled water were added in a 1 L flask. The pH of the flask solution was adjusted to 7.4 by hydrogen chloride or sodium hydroxide solutions (0.2 M), and distilled water was then added to the flask until the marker sign.
PTX release
ISFIs were incubated in 25 mL of PBS (pH 7.4) at a temperature of 37 °C to simulate physiological conditions. The PTX content release from the implant in the buffered solution was determined in triplicate using HPLC at specified sample collection times, and 25 mL of solution was removed from the vial and replaced with 25 mL of fresh PBS at 37 °C. Twenty-five milliliters of DCM was added to the collected sample of the buffered solution and it was decanted three times by decanter. The supernatant was then discarded after extraction in triplicate and the lower, and PTX-rich DCM phase was evaporated to dryness in the hood for 12 h. This method allowed for the recovery of greater than 93.76% of the drug. The dried PTX was then reconstituted in 5 mL of acetonitrile, and the concentrations of PTX were analyzed by using HPLC–UV assay. All the release experiments were conducted in triplicate.
PTX analysis
The HPLC–UV analysis was performed using an Agilent 1200 series system (Agilent Technologies, Palo Alto, CA, USA) consisted of a reverse-phase column (hichrom C18, Hichrom, UK) (length 150 mm, diameter 4.6 mm and particle size 5 µm), an isocratic pump (Iso Pump, G1310A), and an UV detector (VWD, G1314B). Detection was accomplished at 227 nm for all samples. Acetonitrile/water mixture (57:43 v/v) as the mobile phase with a flow rate of 0.8 mL/min was delivered at room temperature. A 20 µL aliquot of the samples was injected through the auto-injector. The concentrations of taxol and 7-epi-taxol were measured through calibration curves of them (0.01–10 mg/L). From three replicates, values were reported.
Determination of LA and GA
The HPLC–UV analysis was also performed using a new HPLC method for the determination of the monomer(s): d- and l-LA and d- and l-GA. The separation was achieved by simple method via a C18 analytical column (hichrom C18 250 mm × 4.6 mm i.d., 5 m), isocratic pump with flow rate 0.7 mL/min, UV 210 nm, and mobile phase 2% (v/v) methanol in phosphate-buffered (0.025 M, pH 7.4) containing 0.002 M tetra butyl ammonium hydroxide. The calibration curve was linear over the on-column concentration range of 1–1000 mg/L for LA and GA versus the integrated area of the related peaks of HPLC spectra. Reported values were from three replicates. The analytical method was successfully applied to the determined biodegradation of polymer in 1 month.
pH measurement
At the determined time points, the implants after incubation under a similar condition as the drug release study, the pH of the suspension was measured with a pH meter (Sartorius Basic Meter, Germany).
Mathematical models and equations
The zero-order, first-order, Higuchi’s, and Weibull models were used to investigate the PTX release kinetics [28, 29, 31]. In the zero-order model (Eq. 1), the drug release rate from its concentration is autonomous.
where the drug released portion at time t and drug release constant are, respectively, considered as F and k0. The natural log of the remained drug in the kinetics of the first-order drug release (Eq. 2) was plotted against time.
where the drug released portion at time t is regarded as F, while the drug release constant is kf. The Weibull model [32] is based on Weibull distribution theory [33] and represented by Eq. 3:
where td is the scale parameter defining the time scale of the process, F is the fraction of released drug at time t, and β is the shape parameter characterizing the release profile curve. In Higuchi’s model based on Fick’s law, the drug release from the insoluble matrix system is alike a square root (Eq. 4).
where F is the fraction of released drug at time t and kH is Higuchi’s dissolution constant.
Result and discussion
For PTX controlled-release systems, biodegradable implants based on PLGA are developed as the object of this study. Besides, to investigate the relation between the biodegradation of the prepared ISFIs and PTX release mechanism, different molecular weights of PLGA (low, medium, and high) have been recognized.
Preparation of ISFI
The injectable implant system was prepared via dissolving PLGA + PTX in NMP (Scheme 1). This can be one of the advantages of this system, non-wasting the drugs during the formulations. Upon intramuscular or subcutaneous injection into an aqueous environment, the NMP diffuses out of the PLGA, while water diffuses into the PLGA matrix. Due to the PLGA insolubility in water, it precipitates upon contact with water, thus resulting in a solid PLGA implant.
In vitro PTX release from ISFI
The results of the cumulative release are shown in Fig. 1. As shown in Fig. 1, these systems are provided for 28 days (672 h). The amount of burst release (initial 24 h) of PTX from ISFIs was determined as 31.65%, 36.13%, and 13.16% based on 502H (low molecular weight PLGA), 503H (medium molecular weight PLGA), and 504H (high molecular weight PLGA), respectively, which is comparable with previous similar work (Table 1). The results show that by increasing the molecular weight of PLGA, the initial burst release was considerably decreased. This phenomenon could be related to the increasing in the glass transition temperature (Tg) value with the molecular weight of PLGA that decreases the penetration rate of PTX [34]. That is related to the higher amount of functional group for the possible interaction with drug molecules in the higher molecular weight of PLGA, resulting in the raising of the Tg value of system. It should be noted that the measured value as initial release is related to the unloaded PTX during the formation of implant and drug-loaded on the surface and into the bulk implant.
In the following, the curve of the release for all three types of the system showed that the amount of PTX release is constant by the end of the fourth day. After this phase, in the third phase, the release rate of PTX was increased. According to its evolutionary curves, it showed triphasic release profile. These results are consistent with the previous research work [35, 36]. Initial burst release of PTX is affected by a number of factors such as the presence of initial interconnected pores, polymer swelling, polymer pore opening, and closing, and surface-associated and unload drug during formation. The second phase of release that typically referred to as the “lag phase” is controlled by surface erosion. In the third phase, as known the monomers in PLGA are connected to each other by ester bonds; after water penetration into the polymer and bulk erosion, the ester bonds are cleaved randomly by hydrolytic chain scission or hydrolysis, which is often shown rapid PTX release and follows apparent zero-order kinetics [37].
Kinetics for PTX release from ISFIs
The release data were examined using several models (zero-order, first-order, Weibull, and Higuchi) to disclose the kinetics of drug release in the third phase, as described previously (Table 2) [31]. The release data for ISFIs were best followed in initial burst release with Higuchi, and in leg and third phase with zero order. The relationship of PTX release with Higuchi and zero order can be used to define the drug dissolution from ISFIs, as seen in the case of some matrix tablets and transdermal systems [46,47,48].
Biodegradation study
Typically, the hydrolytic is a degradation mechanism in aliphatic polyester that is strongly supported by previous works [49,50,51]. For example, Vert et al., Visscher et al., and Ikada et al. reported an interesting study on the morphology of polymer and chemistry of the hydrolytic degradation mechanism [50, 52,53,54]. Water permeability and solubility (hydrophobicity/hydrophilicity), mechanism of hydrolysis (autocatalytic, non-catalytic, enzymatic), chemical composition, additives (acidic, monomers, drugs, basic, solvents,), device dimensions (shape, size, surface-to-volume ratio), morphology (amorphous, crystalline), porosity, molecular weight and molecular weight distribution, glass transition temperature (glassy, rubbery), physicochemical factors (ion exchange, ionic strength, pH), sterilization, and site of implantation are features that can modulate the hydrolytic degradation manners of PLGA copolymer [55].
Many techniques are employed to study the degradation process of polyesters, mainly for PLGA. These techniques include gravimetry, viscosimetry, X-ray diffraction, dry differential scanning calorimetry, scanning electron microscopy, size-exclusion chromatography, and H-NMR. However, these techniques are not readily applicable to in vitro erosion studies or lack the accuracy and specificity. In order to overcome these drawbacks, a new HPLC method is proposed for direct simultaneous determination of the monomer(s): d- and l-LA and d- and l-GA.
Figure 2 demonstrates that there is a relation among the pH, PTX release, and amount of released monomers. The degradation phenomenon is the lowest in the initial and leg phase, while it is the highest in the third phase. The released amounts of GA and LA monomers were increased by degradation, which leads to the diminishing of pH and consequently releasing the PTX. The main degradation mechanism in ISFIs is the autocatalytic hydrolysis of ester bonds. In PLGA, the monomers are connected to each other by ester bonds; hence, by penetration of water into the polymer bulk, the ester bonds are randomly cleaved via hydrolytic chain scission or hydrolysis [16, 51]. One of the obvious factors in the degradation of ISFIs is the pH of solution. By degradation of PLGA, the pH of solution was decreased, which it can be related to the releasing of acidic moieties (LA and GA) via the degradation of polymer. Interestingly, this phenomenon acts as an auto-catalyst for further degradation of PLGA since the ester bonds are more hydrolyzed in acidic medium.
In initial phase, no soluble monomer product and no appreciable weight loss are shown. Hence, in contact with the medium, PTX on the surface of ISFIs is released as a function of solubility and diffusion of water into the matrix of copolymer. In leg phase, the surface erosion of ISFIs results in the surface degradation of implant, which triggered a releasing of monomer as well as releasing of PTX. In third phase, the bulk degradation is occurred via the bulk erosion of PLGA implant. In this phase, a high amount of monomer and also PTX are released through the bulk degradation of ISFIs. This performance agrees with previous work of PLGA degradation [56,57,58].
As well, in degradation manner of ISFIs, the molecular weight of PLGA plays a significant role. As shown in Fig. 3, in the low molecular weight of PLGA the autocatalytic degradation of polymer chains can accelerate with relatively large numbers of carboxylic end-groups. However, in comparison with low molecular weight the high molecular weight of PLGA would have fewer carboxylic acid end-groups available for autocatalysis. On the other hand, high carboxylic end-groups in PLGA facilitate the degradation of ISFIs.
Conclusion
ISFIs were successfully prepared based on PLGA using the two syringes method. The results of the in vitro PTX release showed the triphasic release profile: the fast-initial burst release during the first hours and the sustained and slower release in the second and third phases over 28 days. The release data for ISFIs were best followed in initial burst release with Higuchi, and in leg and third phase with zero order. The biodegradation study revealed the relation among the pH, PTX release, and the amount of released monomers. Moreover, in the degradation, the low molecular weight accelerates the autocatalytic polymer chain degradation. According to the obtained results, the prepared ISFIs could potentially be used in localized PTX delivery as an implantable system.
References
Bode C, Kranz H, Siepmann F, Siepmann J (2018) In-situ forming PLGA implants for intraocular dexamethasone delivery. Int J Pharm 548(1):337–348
Kamali H, Khodaverdi E, Hadizadeh F, Yazdian-Robati R, Haghbin A, Zohuri G (2018) An in situ forming implant formulation of naltrexone with minimum initial burst release using mixture of PLGA copolymers and ethyl heptanoate as an additive: in-vitro, ex vivo, and in vivo release evaluation. J Drug Deliv Sci Technol 47:95–105
Kamali H, Khodaverdi E, Hadizadeh F, Mohajeri SA (2019) In-vitro, ex vivo, and in vivo evaluation of buprenorphine HCl release from an in situ forming gel of PLGA-PEG-PLGA using N-methyl-2-pyrrolidone as solvent. Mater Sci Eng C 96:561–575
Samy WM, Ghoneim AI, Elgindy NA (2014) Novel microstructured sildenafil dosage forms as wound healing promoters. Expert Opin Drug Deliv 11(10):1525–1536
Kempe S, Mäder K (2012) In situ forming implants—an attractive formulation principle for parenteral depot formulations. J Control Release 161(2):668–679
Packhaeuser C, Schnieders J, Oster C, Kissel T (2004) In situ forming parenteral drug delivery systems: an overview. Eur J Pharm Biopharm 58(2):445–455
Luo H, Zhang Y, Gan D, Yang Z, Ao H, Zhang Q, Yao F, Wan Y (2019) Incorporation of hydroxyapatite into nanofibrous PLGA scaffold towards improved breast cancer cell behavior. Mater Chem Phys 226:177–183
Thevar J-TK, Malek NANN, Kadir MRA (2019) In vitro degradation of triple layered poly(lactic-co-glycolic acid) composite membrane composed of nanoapatite and lauric acid for guided bone regeneration applications. Mater Chem Phys 221:501–514
Boimvaser S, Mariano RN, Turino LN, Vega JR (2016) In vitro bulk/surface erosion pattern of PLGA implant in physiological conditions: a study based on auxiliary microsphere systems. Polym Bull 73(1):209–227
Sahoo SK, Panyam J, Prabha S, Labhasetwar V (2002) Residual polyvinyl alcohol associated with poly(d,l-lactide-co-glycolide) nanoparticles affects their physical properties and cellular uptake. J Control Release 82(1):105–114
Winzenburg G, Schmidt C, Fuchs S, Kissel T (2004) Biodegradable polymers and their potential use in parenteral veterinary drug delivery systems. Adv Drug Deliv Rev 56(10):1453–1466
Liu D, Tomasko DL (2007) Carbon dioxide sorption and dilation of poly (lactide-co-glycolide). J Supercrit Fluids 39(3):416–425
Khodaverdi E, Hadizadeh F, Tekie FSM, Jalali A, Mohajeri SA, Ganji F (2012) Preparation and analysis of a sustained drug delivery system by PLGA–PEG–PLGA triblock copolymers. Polym Bull 69(4):429–438
Ranganath SH, Fu Y, Arifin DY, Kee I, Zheng L, Lee H-S, Chow PK-H, Wang C-H (2010) The use of submicron/nanoscale PLGA implants to deliver paclitaxel with enhanced pharmacokinetics and therapeutic efficacy in intracranial glioblastoma in mice. Biomaterials 31(19):5199–5207
Ghalanbor Z, Körber M, Bodmeier R (2013) Interdependency of protein-release completeness and polymer degradation in PLGA-based implants. Eur J Pharm Biopharm 85(3):624–630
Kefayat A, Vaezifar S (2019) Biodegradable PLGA implants containing doxorubicin-loaded chitosan nanoparticles for treatment of breast tumor-bearing mice. Int J Biol Macromol 136:48–56
MaJ Dorta, Santoveña A, Ma Llabrés, Fariña JB (2002) Potential applications of PLGA film-implants in modulating in vitro drugs release. Int J Pharm 248(1–2):149–156
Yasukawa T, Ogura Y, Sakurai E, Tabata Y, Kimura H (2005) Intraocular sustained drug delivery using implantable polymeric devices. Adv Drug Deliv Rev 57(14):2033–2046
Weinberg BD, Patel RB, Wu H, Blanco E, Barnett CC, Exner AA, Saidel GM, Gao J (2008) Model simulation and experimental validation of intratumoral chemotherapy using multiple polymer implants. Med Biol Eng Comput 46(10):1039–1049
Nkenke E, Stelzle F (2009) Clinical outcomes of sinus floor augmentation for implant placement using autogenous bone or bone substitutes: a systematic review. Clin Oral Implant Res 20:124–133
Hussien NA, Işıklan N, Türk M (2018) Aptamer-functionalized magnetic graphene oxide nanocarrier for targeted drug delivery of paclitaxel. Mater Chem Phys 211:479–488
Marupudi NI, Han JE, Li KW, Renard VM, Tyler BM, Brem H (2007) Paclitaxel: a review of adverse toxicities and novel delivery strategies. Expert Opin Drug Saf 6(5):609–621
Wang L, Chaw C-S, Yang Y-Y, Moochhala SM, Zhao B, Ng S, Heller J (2004) Preparation, characterization, and in vitro evaluation of physostigmine-loaded poly (ortho ester) and poly (ortho ester)/poly(d,l-lactide-co-glycolide) blend microspheres fabricated by spray drying. Biomaterials 25(16):3275–3282
Li KW, Dang W, Tyler BM, Troiano G, Tihan T, Brem H, Walter KA (2003) Polilactofate microspheres for Paclitaxel delivery to central nervous system malignancies. Clin Cancer Res 9(9):3441–3447
Ong BY, Ranganath SH, Lee LY, Lu F, Lee H-S, Sahinidis NV, Wang C-H (2009) Paclitaxel delivery from PLGA foams for controlled release in post-surgical chemotherapy against glioblastoma multiforme. Biomaterials 30(18):3189–3196
von Eckardstein KL, Patt S, Kratzel C, Kiwit JC, Reszka R (2005) Local chemotherapy of F98 rat glioblastoma with paclitaxel and carboplatin embedded in liquid crystalline cubic phases. J Neurooncol 72(3):209–215
Elkharraz K, Faisant N, Guse C, Siepmann F, Arica-Yegin B, Oger J, Gust R, Goepferich A, Benoit J, Siepmann J (2006) Paclitaxel-loaded microparticles and implants for the treatment of brain cancer: preparation and physicochemical characterization. Int J Pharm 314(2):127–136
Amini-Fazl MS, Mobedi H, Barzin J (2014) Incorporation of HSA microparticles within the taxol-loaded in situ forming PLGA microspheres: synthesis, characterization, and drug release. Int J Polym Mater Polym Biomater 63(12):632–640
Amini-Fazl MS, Mobedi H, Barzin J (2014) Investigation of aqueous stability of taxol in different release media. Drug Dev Ind Pharm 40(4):519–526
Amini-Fazl MS, Mohammadi R, Kheiri K (2019) 5-Fluorouracil loaded chitosan/polyacrylic acid/Fe3O4 magnetic nanocomposite hydrogel as a potential anticancer drug delivery system. Int J Biol Macromol 132:506–513
Karimzadeh Z, Javanbakht S, Namazi H (2018) Carboxymethylcellulose/MOF-5/Graphene oxide bio-nanocomposite as antibacterial drug nanocarrier agent. BioImpacts 9(1):5–13
Dash S, Murthy PN, Nath L, Chowdhury P (2010) Kinetic modeling on drug release from controlled drug delivery systems. Acta Pol Pharm 67(3):217–223
Langenbucher F (1972) Linearization of dissolution rate curves by the Weibull distribution. J Pharm Pharmacol 24:979–981
Shah S, Cha Y, Pitt C (1992) Poly(glycolic acid-co-dl-lactic acid): diffusion or degradation controlled drug delivery? J Control Release 18(3):261–270
Bhardwaj R, Blanchard J (1997) In vitro evaluation of poly(d,l-lactide-co-glycolide) polymer-based implants containing the α-melanocyte stimulating hormone analog, Melanotan-I. J Control Release 45(1):49–55
Desai NP, Trieu V, Hwang LY, Wu R, Soon-Shiong P, Gradishar WJ (2008) Improved effectiveness of nanoparticle albumin-bound (nab) paclitaxel versus polysorbate-based docetaxel in multiple xenografts as a function of HER2 and SPARC status. Anticancer Drugs 19(9):899–909
Fu Y, Kao WJ (2010) Drug release kinetics and transport mechanisms of non-degradable and degradable polymeric delivery systems. Expert Opin Drug Deliv 7(4):429–444
Mu L, Feng SS (2001) Fabrication, characterization and in vitro release of Paclitaxel (Taxol®) loaded poly (lactic-co-glycolic acid) microspheres prepared by spray drying technique with lipid/cholesterol emulsifiers. J Control Release 76:239–254
Hiremath JG, Devi VK (2010) Preparation and in vitro characterization of paclitaxel-loaded injectable microspheres. Asian J Pharm 4:205–211
Tsai MC (2003) Biodegradable paclitaxel-loaded PLGA microsphere for regional treatment of peritoneal cancers. Ohio State University, Columbus
Shiny J, Ramchander T, Goverdhan P, Habibuddin M, Aukunuru JV (2013) Development and evaluation of a novel biodegradable sustained release microsphere formulation of paclitaxel intended to treat breast cancer. Int J Pharm Investig 3(3):119–125
Azouz SM, Walpole J, Amirifeli S, Taylor KN, Grinstaff MW, Colson YL (2008) Prevention of local tumor growth with paclitaxelloaded microspheres. J Thorac Cardiovasc Surg 135:1014–1021
Radulescu D, Schwade N, Wawro D (2003) Uniform paclitaxel-loaded biodegradable microspheres manufactured by ink-jet technology. Recent Adv Drug Deliv Syst 126
Wang J, Ng CW, Win KY, Shoemakrs P, Lee TKY, Feng SS, Wang CH (2002) Release of paclitaxel from polylactide-co-glycolide (PLGA) microparticles and discs under irradiation. J Microencapsul 20:317–327
Jackson JK, Hung T, Letchford K, Burt HM (2007) The characterization of paclitaxel-loaded microspheres manufactured from blends of poly(lactic-co-glycolic acid) (PLGA) and low molecular weight diblock copolymers. Int J Pharm 342:6–17
Freitas M, Marchetti J (2005) Nimesulide PLA microspheres as a potential sustained release system for the treatment of inflammatory diseases. Int J Pharm 295(1–2):201–211
Grassi M, Grassi G (2005) Mathematical modelling and controlled drug delivery: matrix systems. Curr Drug Deliv 2(1):97–116
Shoaib MH, Tazeen J, Merchant HA, Yousuf RI (2006) Evaluation of drug release kinetics from ibuprofen matrix tablets using HPMC. Pak J Pharm Sci 19(2):119–124
Makwana VA, Larrañaga A, Vilas JL, Lizundia E (2019) Kinetic, thermal, structural and degradation studies on the effect of meta-substituted aromatic-aliphatic polyesters built through ring-opening polymerisation. Polym Degrad Stab 169:108984
Tserki V, Matzinos P, Pavlidou E, Vachliotis D, Panayiotou C (2006) Biodegradable aliphatic polyesters. Part I. Properties and biodegradation of poly(butylene succinate-co-butylene adipate). Polym Degrad Stab 91(2):367–376
Leja K, Lewandowicz G (2010) Polymer biodegradation and biodegradable polymers: a review. Pol J Environ Stud 19(2):255–266
Vert M, Mauduit J, Li S (1994) Biodegradation of PLA/GA polymers: increasing complexity. Biomaterials 15(15):1209–1213
Visscher G, Robison R, Maulding H, Fong J, Pearson J, Argentieri G (1985) Biodegradation of and tissue reaction to 50:50 poly(d,l-lactide-co-glycolide) microcapsules. J Biomed Mater Res 19(3):349–365
Tabata Y, Ikada Y (1988) Macrophage phagocytosis of biodegradable microspheres composed of l-lactic acid/glycolic acid homo-and copolymers. J Biomed Mater Res 22(10):837–858
Anderson JM, Shive MS (1997) Biodegradation and biocompatibility of PLA and PLGA microspheres. Adv Drug Deliv Rev 28(1):5–24
Makadia HK, Siegel SJ (2011) Poly lactic-co-glycolic acid (PLGA) as biodegradable controlled drug delivery carrier. Polymers 3(3):1377–1397
Darestani FT, Entezami A, Mobedi H, Abtahi M (2005) Degradation of poly(d,l-lactide-co-glycolide) 50:50 implant in aqueous medium. Iran Polym J 14(8):753–763
Sundarapandiyan D, Olear A, Exner AA (2015) The effect of additives on the behavior of phase sensitive in situ forming implants. J Pharm Sci 104(10):3471–3480
Acknowledgements
The authors express their sincere gratitude to the University of Tabriz for providing experimental support to this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that they have no conflict of interest in the case of this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Amini-Fazl, M.S. Biodegradation study of PLGA as an injectable in situ depot-forming implant for controlled release of paclitaxel. Polym. Bull. 79, 2763–2776 (2022). https://doi.org/10.1007/s00289-020-03347-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00289-020-03347-5