Abstract
Vaccines are promising strategies for controlling COVID-19; however, COVID-19 vaccine side effects play a central role in public confidence in the vaccine and its uptake process. This study aimed to provide evidence on the post-vaccination early side effects of the BBIBP-CorV (Sinopharm) vaccine. This cross-sectional survey-based study was conducted between November 2021 and January 2022 among recipients of the BBIBP-CorV vaccine, using a questionnaire-based survey. Our final sample consisted of 657 participants, including 392 women. Among the study cases, only 103 (15.7%) participants received one dose of vaccine, and the rest received both doses (N = 554, 84.3%). Systemic symptoms (first dose: N = 187, both doses: N = 128) were the most commonly reported events after vaccination, and among them, injection site pain (first dose: 19.3%, both doses: 12.9%) was the most prevalent adverse effect. All reporting events were mild and resolved in less than 3 days without hospitalization. Among the participants, females and young people aged 35–65 were more prone to manifest side effects (N = 169, 53.3%) after the vaccine injection. Furthermore, our results revealed that the recipients who were suffering from underlying diseases, including diabetes, renal disorder, and respiratory illness, reported fewer adverse responses after vaccination in comparison with healthy individuals. Vaccination against SARS-CoV-2 may lead to some adverse reactions in recipients. However, the frequency of post-vaccination early side effects differed in people, but all responses were slight and temporary.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In December 2019, COVID-19 emerged as a cluster of pneumonia with an unknown origin in Wuhan, China. On January 30, 2020, the WHO classified this outbreak as a public health emergency due to the rapid increase in confirmed cases [1]. On February 19, 2020, the first cases were officially recognized in Qom city, Iran [2]. The lack of medications or vaccines, and COVID-19 transmission by asymptomatic carriers, made specific public health interventions ineffective [1]. Hand sanitation, social distancing, and quarantine, at the price of less economic activity, were recommended to prevent COVID-19 transmission in the early days of the pandemic [3]. Compared with other viral respiratory infections, SARS-CoV-2 appeared as a highly transmissible disease with an astronomical fatality rate [4]. On the other hand, natural immunity to SARS-CoV-2 from infection with Corona viruses is insufficient and wanes rapidly [5]. Hence, a vaccine was urgently required to control and prevent COVID-19. The primary purpose of an effective vaccine is to prevent virus-mediated disease through developing immunity in vaccinated persons, or indirectly by reducing transmission among the population. In late 2020 and early 2021, COVID-19 vaccines were licensed for widespread use in countries all around the globe [6].
Various SARS-CoV-2 vaccine types were developed, such as DNA- and RNA-based vaccines, recombinant, adenovirus-based vectors, and purified inactivated viruses. Inactivated vaccines, because of their high speed of development, safety, and effectiveness in previous administrations for the prevention of viral infections such as influenza and polio [7, 8], became a promising strategy for COVID-19 vaccine development.
Iran's vaccination program against COVID-19 was launched on February 11, 2021. BBIBP-CorV or Sinopharm BIBP COVID-19 vaccine was one of the first vaccines approved for the general Iranian population [9].
It was first approved for use in people over 18 by China's National Medical Products Administration on December 31, 2020, and around 45 other countries [10]. BBIBP-CorV was developed by the Beijing Institute of Biological Products (Beijing, China) with strain 19nCoV-CDC-Tan-HB02 (HB02). After the pre-clinical studies, the clinical trials phase1/2 on humans was conducted, and safety and efficiency were evaluated [11]. This inactivated SARS-CoV-2 vaccine was safe and immunogenic, in healthy adults, with clinical effectiveness of 79%. Significant humoral responses against SARS-CoV-2 were seen as early as day four following the initial injection, and all participants had shown seroconversion by day 42 [12].
Even though the vaccinations have been approved and are being administered to millions of people throughout the globe, the vaccines manufactured at a faster pace than usual face a risk of causing side effects [9]. There needs to be more information on the potential side effects of vaccines and what participants in vaccination programs may undergo. So, the current study aims to evaluate complications experienced by individuals receiving the BBIBP-CorV vaccine and epidemiological correlations.
Materials and Methods
Study Design
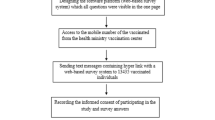
This cross-sectional survey-based study was conducted between November 2021 and January 2022 to estimate the prevalence of COVID-19 vaccine early side effects among recipients of the BBIBP-CorV vaccine in Ardabil province, Iran. A validated questionnaire comprising multiple-choice questions that had been created using Google Forms (Google Inc. Mountain View, California, USA) was utilized in the investigation.
Participants
Data were collected using a questionnaire-based survey, and before answering the questionnaire, all the participants were informed about voluntary participation and anonymity, then their consent was required. No monetary or other motivations were provided for participation in this study. The list of vaccinated individuals from all the vaccination centers in Ardabil province was used as the sampling frame. Samples were randomly selected from this sampling frame and were subjected to questioning. The inclusion criteria for this study were: age over 18 years, having received the first dose of the BBIBP-CorV vaccine no more than 2 weeks prior to questioning, and meeting all other eligibility criteria. If a sample did not meet the inclusion criteria, it was replaced with another qualified sample." In the second phase of the study, these subjects were grouped into two groups receiving only the first dose and who received both doses.
The online questioning method was used to collect data, and only if it was not possible to provide the data in this way because of low literacy or other technical reasons, the questioning was done through a phone call. The participants who received the first dose and were included in the first phase of the study, were contacted again up to 2 weeks after the specified time according to the national vaccination protocol, provided that no more than 2 weeks had passed since their vaccination. The participants were questioned again and asked about whether or not they received a second dose, and in the case of a second dose vaccination, the information related to the early side effects experienced was collected with the same initial questionnaire.
The experience or lack of experience of complications in patients was evaluated. During a maximum period of 3 days, the symptoms subsided in the vaccinated people. The intensity of the symptoms was such that none of the vaccinated people needed emergency intervention.
Instrument
Twenty-seven multiple-choice items created the self-completed questionnaire for this study, which asked participants about their demographics, medical histories, anthropometric measurements, employment status, anamneses related to COVID-19, and general, oral, and skin-related side effects. The content validity of the questionnaire was examined through a panel of a medical immunologist and an infectious diseases specialist. The reliability of the questionnaire was checked before launching it to a large group of participants by testing and retesting the questionnaire randomly on 30 vaccinated people and calculating Cronbach's alpha. The overall reliability was 0.76, representing that the questionnaire tool was reliable.
Ethical Considerations
The study was evaluated and approved by the Research Ethics Committee of Ardabil University of Medical Sciences on 4 October 2021. Before participation, each subject has given their informed agreement to participate online. No data were kept until the participant submitted their responses, and the participants were free to leave the study at any time without citing a reason.
Statistical Analysis
Data analyses were conducted using SPSS V.21 software. Descriptive statistics were used to present the findings, analysis of variance was used to compare quantitative data, and McNemar's test and chi-squared test were used to compare complications in two vaccination phases. Regression analysis was conducted to shows the relationship between investigated variables. A P-value of 0.05 or less was regarded as significant.
Results
Demographic Characteristics of Participants
657 participants, including 265 (40.3%) men and 392 (59.7%) women, were enrolled in this study. The participants were divided into age groups of 18–35 (N = 263, 40.03%), 35–65 (N = 360, 54.79%), and ≥ 65 (N = 34, 5.18%) and according to their marital status, 484 people (73.7%) were married, and 173 people (26.3%) were singles. All participants had received the Sinopharm BBIBP-CorV vaccine; only 103 (15.7%) participants received one dose of the vaccine, and the rest received both doses (N = 554, 84.3%). According to body mass index (BMI), all the participants were in 4 groups, including Underweight (N = 18, 2.7%), Normal (N = 217, 33.0%), Overweight (N = 243, 37.0%), and Obese (N = 179, 27.3%). Detailed demographic information is shown in Table 1. The medical history of underlying diseases in participants was shown in Fig. 1 and categorized into eight groups, including Cardiac (N = 54, 8.2%), respiratory (N = 24, 3.7%), diabetes (N = 51, 7.8%), Blood pressure (N = 90, 13.7%), hepatic (N = 34, 5.2%), renal (N = 22, 3.3%), cancer (N = 24, 3.7%), others (N = 92, 14%).
Frequency of the most common underlying medical conditions in the participants. Among our study population, 394 people had underlying diseases, in which hypertension-related diseases were the most common and accounted for 90 (13.5%) of the total cases and followed by cardiac diseases 55(8.2%), diabetes 51 (7.6%), hepatic 35 (5.2%), respiratory diseases 24 (3.6%), cancer 24 (3.6%), renal 22 (3.3%), and others 93 (13.9%), respectively (Color figure online)
Reported Early Adverse Effects After Vaccine Receive
Based on our findings, all the reported early side effects after receiving the first dose occurred in less than 48 h (1.81 ± 0.98 days) after vaccination and were prolonged about 60 h (2.49 ± 2.24 days). Likewise, the adverse symptoms related to both doses were launched after 48 h (2.22 ± 1.59 days) and disappeared after less than 60 h (2.40 ± 1.82 days). According to the reported adverse effects, systematic symptoms that consist of the most various signature, including body pain, fever, shivering, fainting, nasal drip, sore throat, and muscular spasm, was found as the most reported side effect (N = 187 after the first dose, N = 128 after both doses). In the following cases, local symptoms (N = 151, N = 98 after the first and both doses, respectively), neurological symptoms (N = 126, N = 110), gastrointestinal symptoms (N = 39, N = 15), and respiratory symptoms (N = 24, N = 15) were the most common reporting post-vaccination adverse effects respectively. Furthermore, the number of mentioned adverse events reported after the first dose injection was more than both doses. In this regard, the number of systematic symptoms, local manifestation, and gastrointestinal symptoms were statistically significant with a P-value of < 0.001, < 0.001, and < 0.001, respectively (Fig. 2).
Prevalence of general side effects after the Sinopharm COVID-19 vaccination. Based on the analysis of data, among the reported adverse effects, systematic symptoms were found as the most reported side effect (N = 336, N = 218 after the first and both doses, respectively). In the following cases, local symptoms (N = 185, N = 117), neurological symptoms (N = 148, N = 88), gastrointestinal symptoms (N = 55, N = 19), and respiratory symptoms (N = 24, N = 18) were the most frequent reporting post-vaccination adverse effects, respectively. The frequency of systematic symptoms, local manifestation, and gastrointestinal symptoms was more among subjects who received only the first dose compared with those who received both doses (P-value < 0.001, < 0.001, and < 0.001, respectively)
Our result revealed that the most common adverse effect among the recipients after shooting first and both doses was injection site pain as a local manifestation (first dose: N = 127, 19.3%, both doses: N = 85, 12.9%). Among the participants who had received the first dose, headaches (N = 108, 16.4%) and fainting (N = 102, 15.5%), were among the most frequent side effects. Also, recipients of both doses suffered from headaches (N = 69, 10.5%) and fainting (N = 69, 10.5%) after vaccination. Reported adverse effects of the Sinopharm BBIBP-CorV vaccine are comprehensively presented in Table 2.
Demographic Characteristics and Early Side Effects After Receiving the First Dose
The frequency of post-vaccination symptoms after receiving the first dose and demographic characteristics of recipients were evaluated. Our findings revealed that recipients in the age group of 35–65 (N = 169, 53.3%) with a P-value of 0.024 and overweight persons (N = 119, 38.0%) with a P-value of 0.01 reported the most adverse effects significantly after the first dose. In addition, females (N = 216, 68.1%) showed significantly more side-effects than males (N = 101, 31.8%) (P-value < 0.0001). Furthermore, side effects after the first dose vaccination were seen commonly in an individual without a history of COVID-19 infection (N = 210, 66.2%) (P-value = 0.022). The details of the results are presented in Table 3. The analysis of the reported symptoms after the first dose showed that systemic manifestations were significantly more relevant in females (N = 133, 71.1%) than in males (N = 54, 28.9%) (P-value < 0.0001). Furthermore, the incidence of local symptoms was considerably higher in females (N = 110, 72.8%) in comparison to males (N = 41, 27.1%) (P-value 0.0001). As well, females showed respiratory manifestations (N = 19, 79.2%) more than males (N = 5, 20.8%) (P-value = 0.049). No significant reaction was observed between gender and other side effects, including neurological and gastrointestinal. In addition, according to our findings, the first-dose vaccine recipients who were in the age group 35–65 showed Neurological symptoms (N = 73, 57.9%), Systematic symptoms (N = 99, 51.1%), Gastrointestinal manifestations (N = 23, 59.0%), and Respiratory symptoms (N = 14, 58.3%) with the highest frequency. The systematic ones were statistically significant, with a P-value of 0.046. However, local manifestation was found to be the most common adverse effect in recipients aged 18–35 (P-value = 0.020). Our analysis showed no significant relationship between blood group type and smoke in participants with adverse effects after receiving the first dose. The results are mentioned in more detail in Supplementary Table 1.
Demographic Characteristics and Early Side Effects After Receiving Both Doses
The evaluation of demographic characteristics and side effects after receiving both doses revealed that both dose-related effects showed the same-gender manner with a high frequency in females (N = 149, 73.4%) in comparison to males (N = 54, 26.2%) (P-value = < 0.0001). Our analysis demonstrated that the incidence of systemic symptoms in females (N = 94, 73.4%) was higher in comparison to males (N = 34, 26.6%) (P-value = < 0.0001). Neurological symptoms also were more frequent in females (N = 85, 77.3%) than in males (N = 25, 22.7%) (P-value = < 0.0001). In addition, local manifestations were significantly higher in females (N = 75, 77.5%) in comparison to males (N = 23, 23.5%) (P-value = < 0.0001). Also, all of the adverse effects had the most prevalence in 35–65 years old persons, but this was not significant statistically. Accordingly, other demographic features such as blood type, BMI, smoking, and previous history of COVID-19 represented no considerable relation with side effects after receiving both doses. Detailed information is listed in Supplementary Table 2.
Association Between BMI and Adverse Effects After Receiving the Vaccine
BMI of the participants who reported post-vaccination reactions, including neurological, systematic, gastrointestinal, respiratory, and local effects after receiving the first and both doses, was evaluated. Our results showed that the presence of side effects after vaccination was not influenced significantly by the BMI of the participants. The details of the results are presented in Supplementary Table 3.
Association Between Underlying Diseases and Early Adverse Effects After the First Dose Receive
The existence of chronic diseases in participants who showed side effects after receiving the first dose of the vaccine was evaluated. According to our results, 145 recipients (96.0%) who reported local symptoms had no history of diabetes, and individuals with diabetes presented significantly fewer local side effects (N = 6, 4.0%) after the first dose injection in compared to non-diabetic persons (P-value = 0.048). In addition, only 8 (6.3%) recipients who presented neurological symptoms after the first dose had renal disorders. Therefore, recipients with renal diseases reported a lower incidence of neurological manifestations than those without renal disorders. (P-value = 0.037). However, the history of other conditions, including cancer, blood pressure, cardiac, respiratory, and hepatic, had no significant role in the incidence of side effects after receiving the first dose of the Sinopharm BBIBP-CorV vaccine. Detailed information is listed in Supplementary Table 4.
Association Between Underlying Diseases and Adverse Effects After Both Doses Receive
The relationship between the side effects after receiving both the dose and the clinical backgrounds of the participants was analyzed. Based on our findings, recipients with a history of respiratory disease reported significantly fewer vaccine-related side effects, including systematic symptoms (N = 11, 8.6%, P-value = 0.001), gastrointestinal reactions (N = 2, 13.3% P-value = 0.04) and respiratory symptoms (N = 2, 13.3%, P-value = 0.043). Moreover, the participants with renal disorder showed fewer systematic symptoms (N = 9, 7.0%, P-value = 0.01) and gastrointestinal reactions (N = 2, 13.3%, P-value = 0.027) than percipients without renal diseases. After receiving both doses, there was no significant relationship between other underlying conditions and adverse side effects. Detailed information is listed in Supplementary Table 5.
Association Between Demographic Characters and the Probability of Adverse Effects Occurrence
The relationship between the demographic characteristics of recipients and the probability of the incidence of post-vaccination adverse events was evaluated. For this purpose, the logistic regression analysis was performed. According to the results, increasing age leads to a decrease in the incidence of adverse effects after receiving both the first doses (P-value < 0.001) and both dose (P-value < 0.05). As regards the age of the vaccine recipients may be a predictive factor in the occurrence of post-vaccination reactions. The first and both doses' complementary information are listed in Supplementary Tables 6 and 7, respectively.
Discussion
In the current study, we aimed to assess the side effects experienced by the recipients of the Sinopharm BBIBP-CorV vaccine in Ardebil province, Iran, and evaluate demographic factors associated with post-vaccination reactions. Based on participants’ reports in this study, injection site pain was the most reported adverse effect after receiving both the first and both doses. However, many vaccine recipients suffered from headaches and fainted after injection. In the study about phases 1 and 2 of the clinical trials for the Sinopharm COVID- 19 vaccine, injection site pain, and fever were the most frequent side effects in recipients after vaccination. However, our finding about injection site pain was consistent with his, but about fever was in contrast [13]. According to WHO assessments, arm/injection site pain and headache were the most common side effect of the Sinopharm BBIBP-CorV vaccine [14]. In the study of Mahmood et al., injection site pain and headache after shooting the first and both vaccine doses were reported as the most frequent side effects [15]. In a survey, half (51.4%) of participants who received the Sinopharm vaccine reported injection site pain [16]. The studies on the other vaccines, including CoronaVac (Sinovac), ChAdOx1 (AstraZeneca), and mRNA-1273 (Moderna), showed that pain in the injection site and headache were predominant side effects [17,18,19]. However, among the vaccines, localized pain and headache were frequently reported after injection of the adenoviral vector type vaccine (53.6%), followed by mRNA COVID-19 vaccines (48%) and then the inactivated type (34.8%), according to Rehab Magdy’s study [20]. Excitingly, many participants in our study suffered from faints after receiving the vaccine. However, there were not similar findings in other studies. Still, the significant associations between vaccine injection-related fears and indecision in COVID-19 vaccination and the frequencies and severity of all the post-vaccination side effects were documented [21]. Also, the study by Hatmal, M.M. revealed that nearly half of the vaccine recipients were scared of the COVID-19 vaccine before receiving it [22]. Hence, fainting might be considered a mental reaction to vaccination that results from injection phobia. Furthermore, the current study showed that the incidence of adverse reactions was more in first-dose recipients in comparison to both dose ones. Similarly, several studies documented that the frequency of side effects after injection of the first dose of the Sinopharm COVID-19 vaccine was higher than both doses [15, 23, 24]. In the study of Al-Zidan, an increasing number of reported side effects after the first dose compared to the second dose was described [25]. Also, according to Centers for Disease Control and Prevention reports, adverse effects are higher in first-dose recipients than in both doses [26]. The basis of immune system response by secretion of various inflammatory cytokines after receiving a vaccine may prompt these reactions (12). According to the survey of participants, the adverse effects related to the injection of the first dose and both doses appeared after 24 h, and all the symptoms were not continued above 72 h. These findings was agreed with Al-Zidan’s study that showed post-vaccination adverse events launched after 1 day of the first dose in the majority of recipients [25]. While some studies report that the side effects developed during the 24 h after the vaccine injection and remained for up to 3 days in most recipients [21]. This discrepancy may relate to the demographic characteristics of vaccine recipients and sample size. Altogether, most post-vaccination side effects may be temporary, self-limiting reactions and usually resolved within 1–3 days [27].
Females in our study are more prone than males to manifest adverse symptoms. After the first dose injection, systemic manifestations, local symptoms, and respiratory manifestations, and after both doses, systemic signs, neurological symptoms, and local expressions were more common in females than males. According to similar studies, among the participants who received the BBIBP-CorV (Sinopharm) vaccine, females reported more adverse reactions than males after both doses [15, 21, 28]. Also, A survey of CoronaVac, an inactivated virus vaccine, and other types of vaccines, such as RNA-based COVID-19 vaccines, documented that females showed more side effects after vaccination than males [18, 29,30,31]. Furthermore, Gender-dependent side effects after receiving other inactivated virus vaccines such as influenza, measles-mumps-rubella combination vaccine, attenuated Japanese encephalitis, and attenuated Dengue vaccines were reported. The exact cause is unclear, but a more robust immune system and more cytokine and antibody responses in females were suggested [32]. Our findings show that young individuals between 35 and 65 presented the most adverse effects after receiving the first dose. Xia et al., in the phase 1/2 clinical trial of the BBIBP-CorV vaccine, reported that the 18–59 years-old group was prone to present adverse reactions after the first injection compared to others [12]. Furthermore, Saeed et al., demonstrated that the younger adults (≤ 49 years) showed the highest frequency of vaccine-related side effects (injection site pain, fatigue, and headache) in comparison to older age groups (> 49 years) [28]. Studies on different populations confirmed that the side effects of other types of COVID-19 vaccines were significantly more dominant in younger individuals than in the elderly [33, 34]. It was noted that the adverse effects in the young age group are mild to moderate, and serious events are rare [35]. Since younger people with age under 50 have a robust immune system to develop a rapid and extended immune response to vaccines which may lead to more adverse effects in contrast to elderly persons with a decreased immune system and reactogenicity [15].
Our results showed that participants with BMI in the overweight range after the first dose injection reported more symptoms than others. In the current study, a significant association between BMI and the incidence of post-vaccination side effects was not found. However, according to the study of Mahmood et al., individuals with a BMI in the underweight range were prone to present adverse effects after receiving Covid-19 vaccines compared to others [15]. In a study in Saudi Arabia, COVID-19 vaccine recipients with normal BMI reported more side effects [36]. This controversial result seems to be related to sample size, demographic characterizations, and types of vaccines, so more studies are needed.
The evaluation of the correlation between underlying diseases and post-vaccination adverse effects after the first dose showed that local symptoms were significantly lower in diabetic participants than in non-diabetics. There are controversial findings about post-vaccination side effects in diabetic people. However, the study of Vasilev G on COVID-19 vaccination noted that diabetes was not a predisposing factor for the post-vaccination side effects incidence [37]. Nevertheless, in another study, diabetes mellitus type-2 was considered a risk factor for injection site pain after receiving the Pfizer–BioNTech COVID-19 vaccine [29]. Additionally, studies revealed that the vaccine seroconversion rate in diabetic recipients was scarce. Zhou’s study noted that inactivated COVID-19 vaccines like the Sinopharm lead to a weak immune response and low antibody levels in diabetes patients [38, 39], which may describe the moderated post-vaccination adverse reactions. At the same time, the study on influenza vaccine showed that the local adverse events in diabetic recipients were less frequently compared to the non-diabetics control group [40]. Accordingly, neuropathy and sensory impairment in diabetic individuals might influence local sensitivity [40]. In the current study, the recipients who had renal disorders showed fewer symptoms of neurological reactions after the first dose injection and systematic and gastrointestinal responses after receiving both doses compared to healthy recipients. In the study of Holt, the evaluation of the Sinopharm COVID-19 vaccine in dialysis patients in the United Arab Emirates revealed that the vaccine effectiveness and post-vaccination adverse events were less in people with renal disease than in healthy recipients [41]. Besides, seroconversion after vaccination was lower in the dialysis patients compared the general population [42]. According to the study on the mRNA-1273 COVID-19 vaccine (Moderna Biotech Spain, S.L.), recipients who suffer from renal disorder and dialysis patients experienced fewer post-vaccination adverse events [43]. Also, BioNTech/Pfizer mRNA vaccine recipients with renal disorders showed fewer systemic symptoms and local manifestations after vaccine injection than the control group. Moreover, the assessment of the antibody response to vaccination showed that dialysis patients had a lower titer in comparison to the health group [44]. Several studies noted that, in dialysis patients, impaired renal function leads to the accumulation of uraemic toxins and nitrogenous substances, which might influence immune system functions, and, consequently, moderate immune response following vaccination [45, 46]. In addition, systematic and gastrointestinal presence is low in recipients with respiratory disease after both dose injections. There was evidence of immune system weakness in patients with chronic respiratory disease that results from increasing exhausted T cells, T regulatory cells, and myeloid-derived suppressor cells [47, 48]. Hence, diminished response to the COVID-19 vaccine might decrease post-vaccination side effects in the recipients with respiratory disease. Altogether, studies showed that weakened immune responsiveness, which results from chronic diseases, was supported to develop reduced side effects following vaccines [49].
Conclusion
The BBIBP-CorV (Sinopharm) is an inactivated vaccine that is one of the most used vaccines in Iran. Despite the vaccine's critical role in protecting people against SARS-CoV-2, it causes some side effects after injection, such as local symptoms and systemic manifestation. However, these reactions are not severe and will wane in 3 days, but some people may be more prone to show post-vaccination adverse events, including females and young people. In addition, based on documents, vaccine injections in individuals with underlying diseases, such as renal disorders, diabetes, and respiratory illness, are tolerable and safe.
Data Availability
The authors declare that data supporting the findings of this study are available within the article.
References
Sun J, He W-T, Wang L, Lai A, Ji X, Zhai X et al (2020) COVID-19: epidemiology, evolution, and cross-disciplinary perspectives. Trends Mol Med 26(5):483–495
Raoofi A, Takian A, Haghighi H, Rajizadeh A, Rezaei Z, Radmerikhi S et al (2021) COVID-19 and comparative health policy learning; the experience of 10 countries. Arch Iran Med 24(3):260–272. https://doi.org/10.34172/aim.2021.37
Güner HR, Hasanoğlu İ, Aktaş F (2020) COVID-19: prevention and control measures in community. Turk J Med Sci 50(9):571–577. https://doi.org/10.3906/sag-2004-146
Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y et al (2020) Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. The Lancet 395(10223):507–513. https://doi.org/10.1016/S0140-6736(20)30211-7
Huang AT, Garcia-Carreras B, Hitchings MD, Yang B, Katzelnick LC, Rattigan SM et al (2020) A systematic review of antibody mediated immunity to coronaviruses: antibody kinetics, correlates of protection, and association of antibody responses with severity of disease. MedRxiv. https://doi.org/10.1101/2020.04.14.20065771
Biswas N, Mustapha T, Khubchandani J, Price JH (2021) The nature and extent of COVID-19 vaccination hesitancy in healthcare workers. J Community Health 46(6):1244–1251. https://doi.org/10.1007/s10900-021-00984-3
Murdin AD, Barreto L, Plotkin S (1996) Inactivated poliovirus vaccine: past and present experience. Vaccine 14(8):735–746. https://doi.org/10.1016/0264-410x(95)00211-i
Vellozzi C, Burwen DR, Dobardzic A, Ball R, Walton K, Haber P (2009) Safety of trivalent inactivated influenza vaccines in adults: background for pandemic influenza vaccine safety monitoring. Vaccine 27(15):2114–2120. https://doi.org/10.1016/j.vaccine.2009.01.125
Houshmand B, Keyhan SO, Fallahi HR, Ramezanzade S, Sadeghi E, Yousefi P (2022) Vaccine-associated complications: a comparative multicenter evaluation among dental practitioners and dental students—which candidate vaccine is more safe in SARS COV II, Gam-COVID-Vac (Sputnik V), ChAdOx1 nCoV-19 (AstraZeneca), BBV152 (Covaxin), or BBIBP-CorV (Sinopharm)? Maxillofac Plast Reconstr Surg 44(1):1–11. https://doi.org/10.1186/s40902-021-00330-6
Sahraian MA, Ghadiri F, Azimi A, Moghadasi AN (2021) Adverse events reported by Iranian patients with multiple sclerosis after the first dose of Sinopharm BBIBP-CorV. Vaccine 39(43):6347–6350. https://doi.org/10.1016/j.vaccine.2021.09.030
Wang H, Zhang Y, Huang B, Deng W, Quan Y, Wang W et al (2020) Development of an inactivated vaccine candidate, BBIBP-CorV, with potent protection against SARS-CoV-2. Cell 182(3):713-721.e9. https://doi.org/10.1016/j.cell.2020.06.008
Xia S, Zhang Y, Wang Y, Wang H, Yang Y, Gao GF et al (2021) Safety and immunogenicity of an inactivated SARS-CoV-2 vaccine, BBIBP-CorV: a randomised, double-blind, placebo-controlled, phase 1/2 trial. Lancet Infect Dis 21(1):39–51. https://doi.org/10.1016/S1473-3099(20)30831-8
Xia S, Duan K, Zhang Y, Zhao D, Zhang H, Xie Z et al (2020) Effect of an inactivated vaccine against SARS-CoV-2 on safety and immunogenicity outcomes: interim analysis of 2 randomized clinical trials. JAMA 324(10):951–960. https://doi.org/10.1001/jama.2020.15543
https://cdn.who.int/media/docs/default-source/immunization/sage/2021/april/2_sage29apr2021_critical-evidence_sinopharm.pdf. Accessed Apr 2021
Mahmood A, Shujaat SA, Hayat M, Ijaz F, Habib S, Sadaqat W et al (2022) Acute adverse effects of vaccines against SARS-COV-2. Cureus. https://doi.org/10.7759/cureus.27379
Thonginnetra S, Tawinprai K, Niemsorn K, Promsena P, Tandhansakul M, Kasemlawan N et al (2022) Safety after BBIBP-CorV (Sinopharm) COVID-19 vaccine in adolescents aged 10–17 years in Thailand. Vaccines 10(10):1765. https://doi.org/10.3390/vaccines10101765
Moll MEC, Martínez AMS, Cisneros BT, Onofre JIG, Floriano GN, de León MB (2022) Extension and severity of self-reported side effects of seven COVID-19 vaccines in mexican population. Front Public Health. https://doi.org/10.3389/fpubh.2022.834744
Menni C, Klaser K, May A, Polidori L, Capdevila J, Louca P et al (2021) Vaccine side-effects and SARS-CoV-2 infection after vaccination in users of the COVID symptom study app in the UK: a prospective observational study. Lancet Infect Dis 21(7):939–949. https://doi.org/10.1016/S1473-3099(21)00224-3
Attash HM, Al-Obaidy LM, Al-Qazaz HK (2022) Which type of the promising COVID-19 vaccines produces minimal adverse effects? A retrospective cross-sectional study. Vaccines 10(2):186. https://doi.org/10.3390/vaccines10020186
Magdy R, Khedr D, Yacoub O, Attia A, Abdelrahman MA, Mekkawy D (2022) Epidemiological aspects of headache after different types of COVID-19 vaccines: an online survey. Headache: J Head Face Pain 62(8):1046–1052. https://doi.org/10.1111/head.14374
Hatmal MM, Al-Hatamleh MA, Olaimat AN, Mohamud R, Fawaz M, Kateeb ET et al (2022) Reported adverse effects and attitudes among Arab populations following COVID-19 vaccination: a large-scale multinational study implementing machine learning tools in predicting post-vaccination adverse effects based on predisposing factors. Vaccines 10(3):366. https://doi.org/10.3390/vaccines10030366
Hatmal MM, Al-Hatamleh MA, Olaimat AN, Hatmal M, Alhaj-Qasem DM, Olaimat TM et al (2021) Side effects and perceptions following COVID-19 vaccination in Jordan: a randomized, cross-sectional study implementing machine learning for predicting severity of side effects. Vaccines 9(6):556. https://doi.org/10.3390/vaccines9060556
Boshra MS, Hussein RR, Mohsen M, Elberry AA, Altyar AE, Tammam M et al (2022) A battle against COVID-19: vaccine hesitancy and awareness with a comparative study between Sinopharm and AstraZeneca. Vaccines 10(2):292. https://doi.org/10.3390/vaccines10020292
Abu-Hammad O, Alduraidi H, Abu-Hammad S, Alnazzawi A, Babkair H, Abu-Hammad A et al (2021) Side effects reported by Jordanian healthcare workers who received COVID-19 vaccines. Vaccines 9(6):577. https://doi.org/10.3390/vaccines9060577
Al-Zidan R, Darweesh O, Salah M, Bebane P, Ahmed H, Abdulrazzaq G et al (2023) Are some COVID-19 vaccines better than others regarding the short-term side effects? Ceska a Slovenska Farmacie: Casopis Ceske Farmaceuticke Spolecnosti a Slovenske Farmaceuticke Spolecnosti 72(1):45–54
Possible side effects after getting a COVID-19 vaccine (2021). https://www.cdc.gov/coronavirus/2019-ncov/vaccines/expect/after.html. Accessed 29 Sept 2023
Al Khames Aga QA, Alkhaffaf WH, Hatem TH, Nassir KF, Batineh Y, Dahham AT et al (2021) Safety of COVID-19 vaccines. J Med Virol 93(12):6588–6594. https://doi.org/10.1002/jmv.27214
Saeed BQ, Al-Shahrabi R, Alhaj SS, Alkokhardi ZM, Adrees AO (2021) Side effects and perceptions following Sinopharm COVID-19 vaccination. Int J Infect Dis 111:219–226. https://doi.org/10.1016/j.ijid.2021.08.013
Riad A, Pokorná A, Attia S, Klugarová J, Koščík M, Klugar M (2021) Prevalence of COVID-19 vaccine side effects among healthcare workers in the Czech Republic. J Clin Med 10(7):1428. https://doi.org/10.3390/jcm10071428
Almufty HB, Mohammed SA, Abdullah AM, Merza MA (2021) Potential adverse effects of COVID19 vaccines among Iraqi population; a comparison between the three available vaccines in Iraq; a retrospective cross-sectional study. Diabetes Metab Syndr: Clin Res Rev 15(5):102207. https://doi.org/10.1016/j.dsx.2021.102207
Riad A, Sağıroğlu D, Üstün B, Pokorná A, Klugarová J, Attia S et al (2021) Prevalence and risk factors of CoronaVac side effects: an independent cross-sectional study among healthcare workers in Turkey. J Clin Med 10(12):2629. https://doi.org/10.3390/jcm10122629
Klein SL, Jedlicka A, Pekosz A (2010) The Xs and Y of immune responses to viral vaccines. Lancet Infect Dis 10(5):338–349. https://doi.org/10.1016/S1473-3099(10)70049-9
Babamahmoodi F, Saeedi M, Alizadeh-Navaei R, Hedayatizadeh-Omran A, Mousavi SA, Ovaise G et al (2021) Side effects and Immunogenicity following administration of the Sputnik V COVID-19 vaccine in health care workers in Iran. Sci Rep 11(1):1–8. https://doi.org/10.1038/s41598-021-00963-7
Iguacel I, Maldonado AL, Ruiz-Cabello AL, Casaus M, Moreno LA, Martínez-Jarreta B (2021) Association between COVID-19 vaccine side effects and body mass index in Spain. Vaccines 9(11):1321. https://doi.org/10.3390/vaccines9111321
Evidence Assessment (2021) Sinopharm/BBIBP COVID-19 vaccine. World Health Organization, Geneva
Amer FHI, Alzayyat R, Alzayyat N, Alomran S, Wafai S, Alabssi H et al (2022) Side effects of COVID-19 vaccines (Pfizer, AstraZeneca) in Saudi Arabia, Eastern Province. Cureus. https://doi.org/10.7759/cureus.27297
Vasilev G, Kabakchieva P, Miteva D, Batselova H, Velikova T (2022) Effectiveness and safety of COVID-19 vaccines in patients with diabetes as a factor for vaccine hesitancy. World J Diabetes 13(9):738–751. https://doi.org/10.4239/wjd.v13.i9.738
Boroumand AB, Forouhi M, Karimi F, Soltani Moghadam A, Ghanbari Naeini L, Kokabian P et al (2022) Immunogenicity of COVID-19 vaccines in patients with diabetes mellitus: a systematic review. Front Immunol. https://doi.org/10.3389/fimmu.2022.940357
Zhou X, Lu H, Sang M, Qiu S, Yuan Y, Wu T et al (2023) Impaired antibody response to inactivated COVID-19 vaccines in hospitalized patients with type 2 diabetes. Hum Vaccines Immunother. https://doi.org/10.1080/21645515.2023.2184754
Seo YB, Baek JH, Lee J, Song JY, Lee JS, Cheong HJ et al (2015) Long-term immunogenicity and safety of a conventional influenza vaccine in patients with type 2 diabetes. Clin Vaccine Immunol 22(11):1160–1165. https://doi.org/10.1128/CVI.00288-15
Holt SG, Mahmoud S, Ahmed W, Acuna JM, Al Madani AK, Eltantawy I et al (2022) An analysis of antibody responses and clinical sequalae of the Sinopharm HB02 COVID19 vaccine in dialysis patients in the United Arab Emirates. Nephrology 27(3):260–268. https://doi.org/10.1111/nep.13980
Alirezaei A, Fazeli SA, Shafiei M, Miladipour A (2022) Efficacy of Sinopharm® COVID-19 vaccine in hemodialysis patients: a preliminary report. Iran J Kidney Dis 16(4):259
Sanders J-SF, Bemelman FJ, Messchendorp AL, Baan CC, van Baarle D, van Binnendijk R et al (2022) The RECOVAC immune-response study: the immunogenicity, tolerability, and safety of COVID-19 vaccination in patients with chronic kidney disease, on dialysis, or living with a kidney transplant. Transplantation 106(4):821–834. https://doi.org/10.1097/TP.0000000000003983
Simon B, Rubey H, Treipl A, Gromann M, Hemedi B, Zehetmayer S et al (2021) Haemodialysis patients show a highly diminished antibody response after COVID-19 mRNA vaccination compared with healthy controls. Nephrol Dial Transpl 36(9):1709–1716. https://doi.org/10.1093/ndt/gfab179
Babel N, Hugo C, Westhoff TH (2022) Vaccination in patients with kidney failure: lessons from COVID-19. Nat Rev Nephrol. https://doi.org/10.1038/s41581-022-00617-5
Rincon-Arevalo H, Choi M, Stefanski A-L, Halleck F, Weber U, Szelinski F et al (2021) Impaired humoral immunity to SARS-CoV-2 BNT162b2 vaccine in kidney transplant recipients and dialysis patients. Sci Immunol 6(61):eabj1031. https://doi.org/10.1126/sciimmunol.abj1031
Bhat TA, Panzica L, Kalathil SG, Thanavala Y (2015) Immune dysfunction in patients with chronic obstructive pulmonary disease. Ann Am Thorac Soc 12(Supplement 2):S169–S175. https://doi.org/10.1513/AnnalsATS.201503-126AW
Kalathil SG, Lugade AA, Pradhan V, Miller A, Parameswaran GI, Sethi S et al (2014) T-regulatory cells and programmed death 1+ T cells contribute to effector T-cell dysfunction in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 190(1):40–50. https://doi.org/10.1164/rccm.201312-2293OC
Berbudi A, Rahmadika N, Tjahjadi AI, Ruslami R (2020) Type 2 diabetes and its impact on the immune system. Curr Diabetes Rev 16(5):442. https://doi.org/10.2174/1573399815666191024085838
Acknowledgements
This study supported by Students Research Committee, Ardabil University of Medical Sciences. The authors thank the patients and healthy individuals for participating in this study. The authors also wish to acknowledge the assistance of the staff of Imam Khomeini Hospital, Ardabil, Iran.
Funding
This study was supported in part by Ardabil University of Medical Sciences (finance code 400000331).
Author information
Authors and Affiliations
Contributions
AM, ME, and ES conceived and planned the study; AM, ME and KK carried out the experiment and collected available literature; ME, MG, RP, NF and ES prepared the manuscript, analyzed the statistical data and verified the accuracy of the tests.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Consent to Participate
All patients signed informed consent before any study-related procedures were performed.
Consent for Publication
The patients were informed of the purpose of this study and an informed written consent has been obtained from the patients to publish this paper.
Ethical Approval
This study was approved by the approved by the Ethics Committee of Ardabil University of Medical Sciences, Ardabil, Iran (IR.ARUMS.REC.1400.212).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mohebbi, A., Eterafi, M., Fouladi, N. et al. Adverse Effects Reported and Insights Following Sinopharm COVID-19 Vaccination. Curr Microbiol 80, 377 (2023). https://doi.org/10.1007/s00284-023-03432-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00284-023-03432-8