Abstract
Monogenic autoinflammatory diseases are defined as a group of conditions with a clinical and biological inflammatory syndrome but little or no evidence of autoimmunity. Over 17 years have passed since the discovery of the first autoinflammatory gene, MEFV, responsible for familial Mediterranean fever. Substantive progress has been made since then, highlighting the key role of the inflammasome in the maintenance of the cell homeostasis but also unravelling new pathophysiological pathways involved in these diseases. The history of autoinflammatory gene discovery demonstrates the powerfulness of next-generation sequencing approaches in linking inflammatory disorders with various overlapping phenotypes. It can be easily anticipated that new genes will be exponentially identified in the coming years. Integrating these new concepts should help to promote personalized patient care through novel therapeutic opportunities.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The autoinflammatory diseases: a fashion with blurred boundaries!
The world of autoinflammatory diseases is in perpetual motion. Its content has expanded dramatically since the discovery of the first gene (MEFV responsible for familial Mediterranean fever, FMF, MIM#249100) in 1997, thanks to new high-throughput sequencing approaches (Fig. 1).
Schematic representation of the autoinflammatory genes discovery over years and the related technical approaches used. Diseases names are in bold letters, and gene names are in italics and in parentheses. AIFEC autoinflammation with infantile enterocolitis, ALDD autoinflammation, lipodystrophy, and dermatosis syndrome, AP1S3 adaptor-related protein complex 1, sigma-3 subunit, APLAID autoinflammation, antibody deficiency, and immune dysregulation, PLCG2-associated, CAPS cryopyrin-associated periodic syndrome, CARD14 caspase recruitment domain-containing protein 14, CECR1 cat eye syndrome chromosome region, candidate 1, DADA2 deficiency of adenosine deaminase 2, DIRA deficiency of interleukin 1 receptor antagonist, DITRA deficiency of interleukin 36 receptor antagonist, FCAS2 familial cold autoinflammatory syndrome 2, FMF familial mediterranean fever, HOIL-1D HOIL1 deficiency, HYDM1 hydatidiform mole, recurrent, 1, IL10 interleukin 10, IL10D interleukine 10 deficiency, IL10R1D interleukin 10 receptor A deficiency, IL10R2D interleukin 10 receptor B deficiency, IL10RA interleukin 10 receptor, alpha, IL10RB interleukin 10 receptor, beta, IL1RN interleukin 1 receptor antagonist, IL36RN interleukin 36 receptor antagonist, LPIN2 LIPIN 2, MEFV Mediterranean fever, MVK mevalonate kinase, MKD mevalonate kinase deficiency, NLRC4 NLR family, caspase recruitment domain-containing 4, NLRP3 NLR pyrin domain-containing protein 3, NLRP7 NLR pyrin domain-containing protein 7, NLRP12 NLR pyrin domain-containing protein 12, NOD2 nucleotide-binding oligomerization domain 2, PAPA pyogenic sterile arthritis, pyoderma gangernosum and acne, PLCG2 phospholipase C, gamma-2, PRP pityriasis rubra pilaris, PSMB8 proteasome subunit, beta-type, 8, PSTPIP1 proline-serine-threonine phosphatase-interacting protein 1, RBCK1 Ranbp-type and C3HC4-type inc finger-containing 1, SAVI sting-associated vasculopathy, infantile-onset, TMEM173 transmembrane protein 173, TNFRSF1A tumour necrosis factor receptor super family 1A, TNFRSF11A tumour necrosis factor receptor super family, member 11A, TRAPS TNF receptor-associated periodic syndrome
A review of PubMed shows that in fact the term “autoinflammatory” appeared in 1988 [1]. The second occurrence was by McDermott in 1999 [2] when the gene responsible for TNF receptor-associated syndrome (TRAPS, MIM#142680) was discovered. He defined a new group of systemic disorders characterized by “apparently unprovoked inflammation in the lack of high-titer autoantibodies or antigen-specific T cells”. At least 25 conditions have been classified in this group so far, including 5 in 2014 (Fig. 1). The corresponding mutations have been recorded in a dedicated and regularly updated online database named infevers (http://fmf.igh.cnrs.fr/ISSAID/infevers/) [3–5].
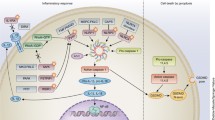
No authoritative classification has emerged in 2015, most likely because of the growing identification of phenotype overlaps and genetic heterogeneity. Originally developed to distinguish diseases of the innate immunity from those related to acquired immunity (autoimmunity), the concept of “autoinflammatory” becomes too restrictive with the emergence of syndromes with mixed autoinflammatory and autoimmune features such as autoinflammation, antibody deficiency, and immune dysregulation, PLCG2-associated (APLAID, MIM#614878) [6, 7]. McGonagle was the first to suggest an integrated classification using the autoimmune versus autoinflammatory ratio involved in each condition as a means to rank it within the continuum of immunological diseases [8]. Clinical and biological criteria are also quite vague when observing the extreme phenotypic differences between the first genetically characterized entity (FMF a hereditary recurrent fever, see S Ozen in this issue) and the latest one autoinflammation with infantile enterocolitis (AIFEC, MIM#616050). AIFEC is characterized by macrophage activation syndrome and pronounced inflammation of the gastrointestinal tract associated with mutation in the NLRC4 (NLR family, caspase recruitment domain-containing 4) gene (see R Goldbach-Manski in this issue) [9, 10]. From a pathophysiological point of view, several signalling pathways have been involved, although a defect of the inflammasome regulation is thought to be the key mechanism underlying most autoinflammatory diseases (see I Aksentijevich in this issue). The inflammasome is a molecular platform triggering activation of inflammatory caspases and processing of proIL-1-beta after a proinflammatory event [11]. Intensive work performed since the discovery of the NLRP3 (NOD-like receptor family, pyrin domain-containing protein 3) gene [12, 13] responsible for cryopyrin-associated periodic syndromes (CAPS) unravelled the pivotal role and functioning of this multimolecular complex, which became the target for the development of new dramatically effective IL-1 blocking agents [14]. To what extent the various inflammasomes dysfunction in either of the autoinflammatory disorders is being progressively elucidated.
FMF is the prototype of the prototypic autoinflammatory group, i.e. hereditary recurrent fevers (HRFs). HRFs are characterized by acute bouts of fever, arthritis, cutaneous eruption and polyserositis, starting in infancy [15]. FMF major specific feature is its almost exclusive confinement to Mediterranean populations, as the most prevalent mutations stemmed from a founder effect. FMF is basically a recessive disease; however, literature data supporting a possible gene dose effect are accumulating [16]. Carriers for MEFV mutations display elevated acute protein reactants and sometimes clinical criteria of the disease, although generally less severe [17]. These observations suggest that one MEFV mutation may confer a heightened inflammation. Colchicine is the mainstay treatment in 95 % of the patients, and IL-1 blockades may become a good option in refractory cases [18]. In the related chapter on FMF, Pr Ozen discusses the myths surrounding FMF since the discovery of MEFV, and how they have evolved and found (or not) answers in the past 15 years.
The hyperimmunoglobulinaemia D and periodic fever syndrome (HIDS) is the milder arm in the mevalonate kinase deficiency (MKD) spectrum [19]. It owes its name to increased (though not specific) serum IgD concentrations observed in these patients prior to the discovery of the gene. Recurrent fever episodes, typically ranging from 3 to 7 days, are sometimes triggered by stress, vaccination or infections. Clinical signs that may help differentiate MKD from other HRF include early onset, diarrhoea, vomiting, lymphadenopathy and aphthous lesions. MVK mutations result in decreased mevalonate kinase activity in the isoprenoid pathway. Although IL-1β is considered a major cytokine in its pathogenesis, IL-1 blockade is not successful in a subset of patients. Interestingly, MVK mutations have recently been pinpointed as responsible for some forms of retinitis pigmentosa [20] and disseminated superficial actinic porokeratosis [21] by means of whole exome sequencing.
CAPS are also rare HRFs. They owe their name to the cryopyrin protein that is encoded by the culprit gene NLRP3 [12, 13]. As does MKD, CAPS encompass a continuum of phenotypes including the mildest familial cold autoinflammatory syndrome (FCAS, MIM#120100), Muckle–Wells syndrome (MWS, MIM191900), and the more severe chronic infantile neurologic, cutaneous and articular (CINCA)/neonatal-onset multisystem inflammatory disease (NOMID) syndrome (MIM#607115). Specific clinical features to search for are urticarial non-pruritic rash, headache or fatigue, ocular involvement, progressive sensorineural hearing loss and central nervous system symptoms (CINCA only). More recently, de Koning et al. suggested that Schnitzler syndrome might be considered also as belonging to CAPS, since somatic mosaicism for NLRP3 mutations was found in some of these patients [22]. After the discovery that cryopyrin was the key inflammasome component, therapeutic trials have shown that IL-1 inhibitors are now safe and effective treatments for almost all patients CAPS [14].
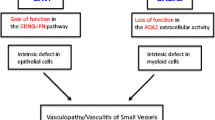
The recent unmasking of numerous novel autoinflammatory genes underscores the power of next-generation sequencing in deciphering the pathophysiology of the associated disorders at an unprecedented speed [23]. The initial demonstration of the role of the NLRP3 inflammasome in HRFs is being completed by outstanding demonstration of unexpected cellular and molecular mechanisms underlying autoinflammation among which, protein misfolding, endoplasmic reticulum-stress response and autophagy. Studying autoinflammatory patients has also recently revealed genetic defects resulting in chronic type I interferon (IFN) signalling (see Goldback-Mansky in this issue). For example gain-of-function mutations in the transmembrane protein 173 (TMEM173) gene induce constitutive stimulator of interferon genes (STING) activation leading to constitutive IFN-β transcription responsible for the sting-associated vasculopathy, infantile-onset (SAVI, MIM# 615934) syndrome [24].
In conclusion, description of new autoinflammatory phenotypes associated with genetic and experimental research fuelled our understanding of immune pathways and of mechanisms of inflammation in general over the last 17 years. These insights allowed the discovery of the inflammasomes and the subsequent opportunities for novel therapeutic developments. There is no doubt that an expanding number of new monogenic and multifactorial disorders and their underlying molecular mechanisms will be highlighted in the coming years.
References
Klein I, Naor D (1988) Autoinflammatory response to self-antigens of lymphoblasts. Isr J Med Sci 24:373–375
McDermott MF, Aksentijevich I, Galon J et al (1999) Germline mutations in the extracellular domains of the 55 kDa TNF receptor, TNFR1, define a family of dominantly inherited autoinflammatory syndromes. Cell 97:133–144
Milhavet F, Cuisset L, Hoffman HM et al (2008) The infevers autoinflammatory mutation online registry: update with new genes and functions. Hum Mutat 29:803–808
Sarrauste de Menthiere C, Terriere S, Pugnere D, Ruiz M, Demaille J, Touitou I (2003) INFEVERS: the registry for FMF and hereditary inflammatory disorders mutations. Nucleic Acids Res 31:282–285
Touitou I, Lesage S, McDermott M et al (2004) Infevers: an evolving mutation database for auto-inflammatory syndromes. Hum Mutat 24:194–198
Ombrello MJ, Remmers EF, Sun G et al (2012) Cold urticaria, immunodeficiency, and autoimmunity related to PLCG2 deletions. N Engl J Med 366:330–338
Zhou Q, Lee GS, Brady J et al (2012) A hypermorphic missense mutation in PLCG2, encoding phospholipase Cgamma2, causes a dominantly inherited autoinflammatory disease with immunodeficiency. Am J Hum Genet 91:713–720
McGonagle D, Aziz A, Dickie LJ, McDermott MF (2009) An integrated classification of pediatric inflammatory diseases, based on the concepts of autoinflammation and the immunological disease continuum. Pediatr Res 65:38R–45R
Canna SW, de Jesus AA, Gouni S et al (2014) An activating NLRC4 inflammasome mutation causes autoinflammation with recurrent macrophage activation syndrome. Nat Genet 46:1140–1146
Romberg N, Al Moussawi K, Nelson-Williams C et al (2014) Mutation of NLRC4 causes a syndrome of enterocolitis and autoinflammation. Nat Genet 46:1135–1139
Martinon F, Burns K, Tschopp J (2002) The inflammasome: a molecular platform triggering activation of inflammatory caspases and processing of proIL-beta. Mol Cell 10:417–426
Feldmann J, Prieur AM, Quartier P et al (2002) Chronic infantile neurological cutaneous and articular syndrome is caused by mutations in CIAS1, a gene highly expressed in polymorphonuclear cells and chondrocytes. Am J Hum Genet 71:198–203
Hoffman HM, Mueller JL, Broide DH, Wanderer AA, Kolodner RD (2001) Mutation of a new gene encoding a putative pyrin-like protein causes familial cold autoinflammatory syndrome and Muckle-Wells syndrome. Nat Genet 29:301–305
Lachmann HJ, Kone-Paut I, Kuemmerle-Deschner JB et al (2009) Use of canakinumab in the cryopyrin-associated periodic syndrome. N Engl J Med 360:2416–2425
Simon A, van Deuren M, Tighe PJ, van der Meer JW, Drenth JP (2001) Genetic analysis as a valuable key to diagnosis and treatment of periodic fever. Arch Intern Med 161:2491–2493
Federici S, Calcagno G, Finetti M et al (2012) Clinical impact of MEFV mutations in children with periodic fever in a prevalent western European Caucasian population. Ann Rheum Dis 71:1961–1965
Hentgen V, Grateau G, Stankovic-Stojanovic K, Amselem S, Jeru I (2013) Familial Mediterranean fever in heterozygotes: are we able to accurately diagnose the disease in very young children? Arthritis Rheum 65:1654–1662
Ter Haar N, Lachmann H, Ozen S et al (2012) Treatment of autoinflammatory diseases: results from the Eurofever Registry and a literature review. Ann Rheum Dis 72:678–685
Haas D, Hoffmann GF (2006) Mevalonate kinase deficiencies: from mevalonic aciduria to hyperimmunoglobulinemia D syndrome. Orphanet J Rare Dis 1:13
Siemiatkowska AM, van den Born LI, van Hagen PM et al (2013) Mutations in the mevalonate kinase (MVK) gene cause nonsyndromic retinitis pigmentosa. Ophthalmology 120:2697–2705
Zhang SQ, Jiang T, Li M et al (2012) Exome sequencing identifies MVK mutations in disseminated superficial actinic porokeratosis. Nat Genet 44:1156–1160
de Koning HD, van Gijn ME, Stoffels M et al (2014) Myeloid lineage-restricted somatic mosaicism of NLRP3 mutations in patients with variant Schnitzler syndrome. J Allergy Clin Immunol 135:561–564
Aksentijevich I, Kastner DL (2011) Genetics of monogenic autoinflammatory diseases: past successes, future challenges. Nat Rev Rheumatol 7:469–478
Liu Y, Jesus AA, Marrero B et al (2014) Activated STING in a vascular and pulmonary syndrome. N Engl J Med 371:507–518
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is a contribution to the Special Issue on The Inflammasome and Autoinflammatory Diseases - Guest Editors: Seth L. Masters, Tilmann Kallinich and Seza Ozen
Rights and permissions
About this article
Cite this article
Sarrabay, G., Barat-Houari, M., Annakib, S. et al. The autoinflammatory diseases: a fashion with blurred boundaries!. Semin Immunopathol 37, 359–362 (2015). https://doi.org/10.1007/s00281-015-0495-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00281-015-0495-3