Abstract
Background
The composition of navicular joint complex is crucial to perform surgical interventions for multiple pathological foot aetiologies. The data on human navicular bone and its facets from Indian population remain scarce in literature.
Aims and objectives
To evaluate the morphometry and morphology of navicular bone.
Methodology
A total of 77 (right: 40; left: 37) dried human navicular bones were used. The collected data were entered and analysed in SPSS software.
Results
The anteroposterior diameter of navicular bone on right side was 15.19 mm (13.92, 16.77) and on left side was 15.87 mm (13.83, 17.27). The transverse diameter on right and left sides were 34.21 mm (31.74, 36.6) and 33.59 mm (30.23, 35.43), respectively. The vertical diameter measured on the right was 22.31 mm (21.19, 23.94) and on left 22.53 mm (20.8, 24.24). Morphometric evaluation showed no significant difference between right and left navicular bones. The commonest shape for posterior facet was quadrilateral, on the right (62.5%) and left (40.5%). The most common shape of anterior facet for medial cuneiform is quadrilateral, on the right (85%) and left (89.1%). For intermediate cuneiform, triangular facet was common on the right side (72.5%) and on the left (59.5%). The lateral cuneiform facet was bean shaped on right side (72.5%) and quadrilateral on the left side (32.5%). There was a significant difference in shape distribution between right and left (P < 0.05). The median length of the groove for tibialis posterior tendon was 18.01 mm and 16.19 mm on right and left side, respectively. Cuboid facet was observed in 28 (70%) and 26 (65.9%) navicular bones on right and left sides, respectively.
Conclusion
There is no significant difference between right and left bones with regards to morphometric parameters. Morphological evaluation revealed significant difference in the distribution of shape between right and left bones.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The navicular bone, one of the tarsal bones, is located on the medial side of the foot. Its resemblance to boat shape is due to the prominent concavity of the proximal surface. Morphologically, it has four surfaces anterior or distal surface, posterior or proximal surface, dorsal or superior surface and plantar surface with two ends medial and lateral. Proximally, it articulates with the head of talus bone and distally with three cuneiform bones [4]. Occasionally, it has an extra facet for articulation with the cuboid bone on the lateral aspect [12]. Both the plantar and dorsal surfaces are roughened for attachment of different ligaments [8]. The medial surface is also rough and contains a prominent tuberosity, the navicular tuberosity. The plantar surface has an osseous prominence extending downwards which presents as a navicular beak lending a quadrangular appearance to the navicular bone [7].
Even though considered as a small bone, it cannot be overlooked due to the exasperating problems which arises because of its multiple pathologies [4]. Also this bone plays a very critical role in maintaining the medial longitudinal arches of the foot [5]. The tibialis posterior tendon serves as the primary dynamic stabiliser of the rearfoot by persevering the medial longitudinal arch and also has a tendinous insertion to the bone [14]. Several ligaments attached to the bone also performs a significant function in human bipedal biomechanics. There are few reports which have focussed on the morphological aspects of navicular such as the shape of various facets and diameters of the facets present for three cuneiform bones [11]. Finer details of morphological aspects of the bone such as concavity of posterior facet, shapes of all the facets and navicular tuberosity has been studied very infrequently in the literature [11]. A study has evaluated the presence of cuboid facet in the population and its role in biomechanics of gait. It also demonstrated its relation with the size of the talar facet and the position of the talonavicular joint [2]. Hence variants of navicular bone still need to be studied in detail to fill the lacunae in the available literature.
Studies show the role of altered morphology of navicular bone in pathological entities like navicular stress fractures and flat feet deformity [9]. Nowadays navicular fractures are common in young athletes where they present with foot pain and disability in movements [3]. A wide array of pathologies like accessory ossicles, coalition, Kohler’s disease, osteonecrosis, osteochondral lesions, arthropathies [1, 15]. Muller Weiss disease and tumours are associated with the navicular bone [6, 10, 13]. To overcome the surgical difficulties faced by the surgeons and improve treatment options finer anatomical details ought to be evaluated. The data on human navicular bone and its facets from Indian population remain scarce in literature. The present study aims to measure the morphometry data like dimensions of the various aspects of navicular bone and shapes of facets and tuberosities. The purpose of this study is to provide general and additional aspects on the morphology and morphometry of the navicular bone which will help us understand its pathologies better and plan appropriately for foot surgeries.
Materials and methodology
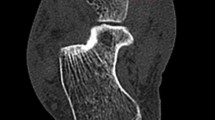
The study was performed in the Department of Anatomy on dried human navicular bones. A total of 77 navicular bones, including 40 right and 37 left, of unknown age and gender were included for analysis. Navicular bone was subjected to morphometric measurements using a digital vernier calliper. (Mitutoyo make, Kawasaki, Japan). Adequate attention was provided to ensure consistent uniformity in the method of measurement whilst using the calliper. Measurements were taken in proximal, distal, dorsal and plantar surfaces and medial and lateral ends of the navicular bone. The following diameters were measured: vertical, transverse and antero-posterior for the entire bone as well as both anterior and posterior facets (Fig. 1a, b).
Morphometric measurements of navicular bone. a Transverse and vertical diameters of the navicular bone. b Transverse and vertical diameters of the posterior facet. c Arrow (red) showing the plantar tubercle or beak. d Double arrow (red) showing the groove length of the tibialis posterior tendon (color figure online)
The presence of plantar tubercle on the plantar surface was noted (Fig. 1c). Navicular tuberosity was identified on the medial surface as a blunt bony prominence directed downwards and medially. The anteroposterior, vertical and transverse diameters of navicular tuberosity were measured. The presence of cuboid facet, its vertical and transverse diameters and its area were recorded. The median length of the groove on the plantar surface for tibialis posterior tendon was noted (Fig. 1d). The shapes of proximal surface, distal surface, navicular tuberosity and cuboid facet were observed. The collected data was entered and analysed in SPSS software 26.0 version (IBM corp. Armonk, NY, 2019) and results were represented in median with range in millimetre. Student T test was used to study the association between categorical and continuous variable. Chi-Square test was used to study the association between 2 categorical variables. Spearman correlation test was performed to assess the correlation between measurements of cuboid facet and posterior facet.
Results
The medial cuneiform, intermediate cuneiform and lateral cuneiform part of anterior facet had a mean vertical and transverse diameter (in mm) of 13.52 ± 1.93 & 10.1 ± 1.5, 16.37 ± 1.83 & 12.96 ± 1.62 and 15.15 ± 1.78 & 14.26 ± 1.75, respectively. The vertical and transverse diameters of posterior facet were (in mm) 19.96 ± 2.09 and 24.20 ± 2.11, respectively. The mean length, breadth and area of cuboid facet were 4.3 ± 2.27 mm, 7.19 ± 2.68 mm and 32.44 ± 1.08 mm2, respectively. The measurement of anterior and posterior facets and navicular tuberosity are given in Tables 1 and 2. There difference in the dimensions of left and right sides were not significant.
The detailed result of the morphological evaluation of navicular bone was presented in Tables 3 and 4. Proximal surface was quadrilateral in shape in 52% bones and the shapes for the rest of the bones were square, rectangle and oval (Fig. 2). Almost three-fourth (73%) of the bones were deeply concave. The most common shape of medial, intermediate and lateral cuneiform was quadrilateral (87.1%), triangle (68.8%) and bean shaped (52%), respectively.
We observed six navicular bones of the left side to have an extra facet on the anterior surface near the medial cuneiform facet. Cuboid facet was observed only in 23 (58.9%) and 13 (34.2%) on the navicular bone in right and left sides, respectively. The various shapes of cuboid facet like square, oval, quadrilateral, rectangle and triangle were observed (Fig. 3).
Plantar tubercle was absent in seven bones on both sides at a rate of 17.9–18.6%, respectively. The plantar surface was observed to have a grove for tibialis posterior tendon and the groove was of the length 13.08 and 13.5 mm in the right and left side, respectively (Table 1). When comparing the proportion of bones between right and left side with regards to the shape of facet for intermediate and lateral cuneiforms there was significant difference (P < 0.05). Similarly, there was significant difference between the bones of right and left limb with regards to the profile of the tuberosity on the medial surface.
The presence or absence of cuboid facet was not significantly associated with vertical and transverse diameter of posterior facet with P value of 0.64 and 0.77, respectively. The dimensions of cuboid facet and posterior facet was correlated. There was a positive correlation between length, breadth, and area of cuboid facet with transverse diameter of posterior facet with a correlation coefficient of 0.043, 0.036 and 0.040, respectively. Similarly, there was a positive correlation between length, breadth and area of cuboid facet with vertical diameter of posterior facet with a correlation coefficient of 0.313, 0.144 and 0.293, respectively. The correlation between the length and area of cuboid facet and vertical diameter of posterior facet was nearing significance with a p value of 0.066 and 0.087, respectively (Fig. 4).
Discussion
In general, the navicular bone has an oval or quadrilateral and some specimens has boat shaped configurations. DiGiovanni et al. had mentioned about the ovoid or saucer shaped nature of the navicular bone. [2]. It has a round or convex base situated dorso-laterally. Its apex is blunted pointing plantar medially and adapting itself to anatomical position with other foot ossicle (Head of talus).
Proximal surface articulates with the head of talus. The surface presents with concavity or sometimes deeply concave. The posterior surface was observed to be of quadrilateral, oval, triangular or rectangular in shape. Most of the specimens were observed to have quadrilateral shape (62.5% in right and 40.5% in left). According to Pfitzn.er et al. (as cited in Manners-Smith et al.) [7] in his article described the facet to have either egg shaped or quadrilateral in shape. Whereas Smith et al. represented the shape to be of quadrilateral (5.8%) or pear (76.7%) or triangular (0.7%) or oval (5.8) or egg shaped (15.1%) based on the presence of plantar point. They also pointed out the nature and depth of the concave articulating surface. Smith et al. observed increase in the concavity along the longest diameter in 238 bones (63.4%), along the shortest diameters in 55 bones (14.6%) and in both diameters in 82 bones (21.8%). Thus, the concavity was examined to be deep in the longest diameters in humans compared to other species like Simiidae [14]. Tuthill et al. had described the proximal articulating surface as strongly concave and thus giving a boat shape nature to the bone. This surface plays a key role in bearing the mechanical load during walking and also helps in maintaining longitudinal arch of the foot [16]. DiGiovanni et al. had observed that the concave nature of this proximal surface is responsible for majority of the hindfoot motion (80%) and thereby making up most of the talonavicular articulation of the foot [4]. The study by Peeters et al. highlighted the morphological changes of talar and navicular bones in flatfeet. The main changes include more proximal facing articular surfaces of the talus and navicular, a deeper navicular cup, an increased articular surface width for the talus, a less protruding talar head compared to the navicular cup, and a higher navicular articular surface relative to the articulating talar head height. All these changes can be related to medial arch collapse and add to previously observed changes inducing forefoot abduction, two major characteristics of flatfoot deformity [9].
Distal surface is convex with two crests dividing the articular surface into three facets in most of examined specimens. Cunningham et al., Morris et al. and Quain et al. (as cited in Manners-Smith et al.) [7] in their studies have discussed the presence of two faint ridges dividing the anterior surface into three facets. Out of 77 specimens, 16 specimens (20.7%) had three crests and two specimens (2.5%) had four crests dividing articular surface into four. All articular surfaces were oriented in different directions articulating with three cuneiform bones. The three articular surfaces converge on the plantar aspect for maintenance of transverse tarsal arch of foot. In majority of 77 specimens, the facet for lateral cuneiform was measured to be the largest in transverse diameter (14.18 mm in right and 14.36 mm in left). The facet for middle cuneiform was the largest in the vertical diameter (15.75 mm in right, 16.88 mm in left). On the contrary Smith et al. in his study had described the facet for medial articular surface to be the largest in both dimensions [7]. The most common shape of articular surface for medial cuneiform was observed to be quadrilateral (87.1%) and middle cuneiform was triangular shape (68.8%). The facet for lateral cuneiform was found to have typically bean-shaped (72.5%) in right side and rectangular (32.5%) in right side. Manners-Smith et al. has observed the shape of all three facets mostly to be of wedge shaped and in middle cuneiform one specimen was triangular with its apex pointing towards the plantar surface. The facet for lateral cuneiform was similar in size to the cohort observed by Renner et al. in the transverse diameter. The diameter (both vertical and transverse) of the facet for medial and intermediate cuneiform and the vertical diameter of facet for lateral cuneiform was smaller in size in comparison to the cohort observed by Renner et al. [11]. This could largely be because of the racial difference between the studies.
Medial surface is convex with blunt bony prominence (navicular tuberosity) directed downwards and medially. Smith et al. described the tuberosity as projecting from the line drawn round the tibio-plantar angle to the apex of the facet for internal cuneiform. The size of the tuberosity was compared with the size of the corpus and the traction exerted by the tibialis posterior muscle on it. They classified some cases to have extremely larger tuberosity and some cases had insignificant tuberosity. The tuberosity in our study were extremely large (59.7%), in some others it was ill-defined. About 13 specimens shows similarity with type III accessory navicular bone (os tibiale externum) according to Geist classification. Manners-Smith et al. described the shape as prismatic and elongated based on the morphological elements [7]. Shape of tuberosity in our study in most of the specimens were pyriform shaped (67.5%). In some specimens, tuberosity was curved medially giving resemblance of boat shaped. DiGiovanni et al. had mentioned in his study that most of the navicular fractures occur through the medial tuberosity due to their morphological nature [2].
Lateral surface was slightly convex and was directed outwards and laterally. A groove was present near lateral border of proximal concave surface for lateral calcaneo-navicular ligament (bifurcate ligament). Numerous pinhole sized vascular foramina (5–10 in number) were present over the groove. It looks rough in its appearance and the chief point of interest in this surface was the presence of cuboid facet and facet for os calcis occasionally as described by Manners-Smith et al. [7].
The cuboid facet (CF) was located at the junction between the lateral surface and anterior surfaces. As described by Pfitzner et al. and Gruber et al. (as cited in Manners-Smith et al.) [7] CF was not present in all the specimens. CF was present in 46.71% of specimens, right side being more than the left. The cuboid facets had variable shapes. In most specimens they were rectangular (69.6% in right and 85% in left). Few specimens showed square-shaped, triangle, quadrilateral or bean shape. There was no significant difference between right and left sided bones in the area measured. (P value 0.94) Data regarding the size of the facet have been lacking in the existing literatures and needs to be studied further. Saldias et al. in his study stated that cuboid facet was present in 52.7% of the population. He further stated that sagittal length (21.61 ± 2.15 mm) of the talar facet was increased when cuboid facet was present thereby relating the size of talar facet with cuboid facet as observed in our study. These data still need to be studied further which remain a knowledge gap in the existing literature [12]. The positive correlation between dimensions of cuboid facet and posterior facet suggest that the dimension of cuboid facet increases as the dimension of posterior facet increases. The length and area of cuboid facet was nearing significant correlation with vertical diameter of posterior facet which needs to be studied in future observations.
Dorsal surface was slightly convex or broad and continuous with medial surface. This surface had two grooves which were present in 63 specimens (81.8%). The depth and prominence of the groove was variable amongst the observed specimens. First groove near upper margin of distal articular surface (dorsal cubo navicular ligament). Second groove (tarsal branch of dorsalis pedis artery) obliquely crossing the dorsal surface and reached up to upper margin of proximal articular surface. In 25.9% specimen, second groove was present along its midportion of dorsal surface. Dorsal surface possesses numerous pin hole sized vascular foramina along the grooves. Manners-Smith et al. had described three grooves in his study, one running obliquely forwards and inwards for the attachment of dorsal cubo-navicular ligament and the second groove for the dorsalis pedis artery and the third groove for the attachment of external calcaneo navicular ligament in humans [7].
Plantar surface was irregular and continuous with medial surface. It presents with a bony prominence called Navicular beak/Plantar point (represents fused os cuboides secundarium) which is responsible for quadrangular morphology of posterior articular surface. Around 62 specimens (80.8%) showed well defined plantar beak. Numerous pin hole sized vascular foramina present on its distal surface continuous with distal articular surface of the bone. The mean groove length was 17.84 mm in right side and 16.19 mm on left side. Smith et al. described the plantar point to be rounded or spur like in some specimens and well developed or absent in few specimens. Pfitzner et al. view (as cited in Manners-Smith et al.) [7] regarding the plantar point as a separate tarsal element is considered too meagre to accept. The point has purely mechanical function in maintaining the arch of the foot and its development is based on the traction outgrowth as viewed by Manners-Smith et al.
The most common shape of the posterior facet was observed to be of quadrilateral in shape (52%). The shapes of facets for intermediate and lateral cuneiforms between right and left bones had significant difference. The incidence of cuboid facet was observed to be 46.7% in the specimens, right side being more than the left. Our anatomical description and morphometric measurements of the navicular bone and its joint complex was the first to the best to our knowledge. The results from our present study would aid in better understanding and improved outcomes for the ankle and foot surgeries. The study had some limitations like the gender, age and the cadaveric nature of the samples were unknown. The current study sets a trend towards improved operative management to allow better healing with lower risk of reinjury and provides better understanding about morphology of the navicular bone and its role in maintaining the arches of foot.
Data availability
All data underlying the results are available as part of the article and no additional source data are required.
References
Chan JY, Young JL (2019) Köhler disease. Avascular necrosis in the child. Foot Ankle Clin 24(1):83–88
DiGiovanni CW (2004) Fractures of the navicular. Foot Ankle Clin 9(1):25–63
Gheewala R, Arain A, Rosenbaum AJ. (2023) Tarsal Navicular Fractures. In: Stat Pearls [Internet]. Treasure Island (FL): Stat Pearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK542221/
Golano P, Fariñas O, Sáenz I (2004) The anatomy of the navicular and periarticular structures. Foot Ankle Clin 9(1):1–23
Kaye RA, Jahss MH (1991) Tibialis posterior: a review of anatomy and biomechanics in relation to support of the medial longitudinal arch. Foot Ankle 11(4):244–247
Kitaura Y, Nishimura A, Nakazora S, Fukuda A, Senga Y, Kato K, Sudo A (2019) Spontaneous osteonecrosis of the tarsal navicular: a report of two cases. Case Rep Orthop 30:5952435
Manners-Smith T (1907) A study of the navicular in the human and anthropoid foot. J Anat Physiol 41(Pt 4):255–279
Marshall D, MacFarlane RJ, Molloy A, Mason L (2020) A review of the management and outcomes of tarsal navicular fracture. Foot Ankle Surg 26(5):480–486
Peeters K, Schreuer J, Burg F, Behets C, Van Bouwel S, Dereymaeker G et al (2013) Alterated talar and navicular bone morphology is associated with pes planus deformity: a CT-scan study. J Orthop Res 31(2):282–287
Perisano C, Greco T, Vitiello R, Maccauro G, Liuzza F, Tamburelli FC, Forconi F (2018) Mueller-Weiss disease: review of the literature. J Biol Regul Homeost Agents 32(6 Suppl. 1):157–162
Renner K, McAlister JE, Galli MM, Hyer CF (2017) Anatomic description of the naviculocuneiform articulation. J Foot Ankle Surg 56(1):19–21
Saldías E, Malgosa A, Jordana X, Isidro A (2019) Morphological and biomechanical implications of cuboid facet of the navicular bone in the gait. Int J Morphol 37(4):1397–1403
Samim M, Moukaddam HA, Smitaman E (2016) Imaging of Mueller-Weiss syndrome: a review of clinical presentations and imaging spectrum. AJR Am J Roentgenol 207(2):W8–W18
Smith CF (1999) Anatomy, function, and pathophysiology of the posterior tibial tendon. Clin Podiatr Med Surg 16(3):399–406
Trammell AP, Davis DD, Scott AT. Kohler Disease. (2023). In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan–. PMID: 29939608
Tuthill HL, Finkelstein ER, Sanchez AM, Clifford PD, Subhawong TK, Jose J (2014) Imaging of tarsal navicular disorders: a pictorial review. Foot Ankle Spec 7(3):211–225
Funding
None.
Author information
Authors and Affiliations
Contributions
NR and SS collected the data, reviewed the literature and drafted the manuscript. NR performed the data analysis. SV critically revised the manuscript. All authors contributed to review of literature, drafting of the manuscript and approved the final version of the manuscript. SV shall act as guarantor of the paper.
Corresponding author
Ethics declarations
Conflict of interests
None stated.
Ethics approval
Waiver of consent approval was obtained from Institute ethics committee and the study was performed in accordance to ethical standards laid by declaration of Helsinki 1964.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rajaram, N., Srinivasan, S. & Verma, S. Human navicular bone: a morphometric and morphological evaluation. Surg Radiol Anat 46, 71–79 (2024). https://doi.org/10.1007/s00276-023-03259-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-023-03259-9