Abstract
Background
Various surgical interventions including esthetic surgery, salivary gland excision, and open reduction of fracture have been performed in the area around the mandibular angle and condyle. This study aimed to comprehensively review the anatomy of the neurovascular structures on the angle and condyle with recent anatomic and clinical research.
Methods and results
We provide detailed information about the branching and distributing patterns of the neurovascular structures at the mandibular angle and condyle, with reported data of measurements and proportions from previous anatomical and clinical research. Our report should serve to help practitioners gain a better understanding of the area in order or reduce potential complications during local procedures. Reckless manipulation during mandibular angle reduction could mutilate arterial branches, not only from the facial artery, but also from the external carotid artery. The transverse facial artery and superficial temporal artery could be damaged during approach and incision in the condylar area. The marginal mandibular branch of the facial nerve can be easily damaged during submandibular gland excision or facial rejuvenation treatment. The main trunk of the facial nerve and its upper and lower distinct divisions have been damaged during parotidectomy, rhytidectomy, and open reductions of condylar fractures.
Conclusion
By revisiting the information in the present study, surgeons will be able to more accurately prevent procedure-related complications, such as iatrogenic vascular accidents on the mandibular angle and condyle, complete and partial facial palsy, gustatory sweating (Frey syndrome), and traumatic neuroma after parotidectomy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Arterial tributaries from the external carotid artery (ECA) and nervous branches of the facial (FN), trigeminal, and cervical nerves innervate the area around the mandibular angle and condyle. Esthetic surgery, salivary gland tumor excision, and open reduction of fractures are performed in the mandibular angle and condyle region. Due to the intricate and various distribution patterns of the neurovascular structures in that area, traditional depictions in many textbooks are too simple and inaccurate for surgeons to effectively prevent iatrogenic neurovascular complications during procedures. The present review aims to provide exact anatomical information of the arteries and nerves around the mandibular angle and condyle and to revisit related clinical implications of the anatomical structures.
Literature study
To perform a comprehensive anatomical review, the present study revisited previous anatomical studies about the nerves and arteries around the mandibular angle and condyle. Our review constituted four parts consisting of (1) the arteries around the mandibular ramus, (2) the nerves around the mandibular ramus, (3) the arteries around the mandibular condyle and (4) the nerves around the mandibular condyles. Each part concluded the detailed anatomical information delineated by previous studies with the clinical implication, especially surgical complication.
Angular branches from external carotid artery and facial artery around the mandibular ramus
The facial artery (FA) originates from the ECA inside the mandibular ramus at a level about 8 mm superior to the carotid bifurcation [56, 60]. The artery branches from a common trunk with the lingual artery in approximately one in five cases [39]. The FA turns outward below the antegonial notch of the mandible and it emerges on the face at the point about 2 cm anterior to the gonion, as it ascends toward the nasion with various branching patterns [33]. Inside the mandible, the artery issues the ascending palatine artery (APA) and submental artery (SMA). Additionally, the FA gives off other small branches to the medial pterygoid muscle (MPt) inside the mandibular ramus [34]. After it emerges, the FA provides muscular branches to the masseter muscle (MST) [64]. Not only the FA, but also the ECA, gives off branches inside and outside the ramus to the Mpt and MST.
Arterial branches inside the mandibular ramus
General descriptions have presented that the pterygoid arteries from the maxillary artery (MA) feed the pterygoid muscles [45, 56]. However, the FA or ECA also issue arterial branches distributing the MPt near the mandibular angle. Huang et al. described that the APA consists of glossal, tonsilar, and hamular branches, and these branches supply blood to the area inside the ramus [22]. Kwak et al. determined that the gonial branches from the FA (gonial muscular branch) occur in 20 % of cases, and that the arterial tributaries of the tonsillar branch (anterior muscular branch) occur in 90 % of cases, supplying blood to the MPt and the APA. In their study, the APA was observed in all cases, as originating from the FA (80 %) or ECA (20 %) at the level of the gonion. They reported that the APA seemed to be a dominant artery to the MPt inside the ramus, similar to the study of Huang et al. [22]. The gonial muscular branch branched from the FA before the ramification of the APA, and the anterior muscular branch was ramified from the tonsillar branch after the ramification. In latter cases, the tonsillar branch originated from the FA (72 %) or the SMA (28 %). Other pterygoid branches ramified directly from ECA about 2 cm superior the gonion in 80 % of cases. The area 1.5 cm anterior to the gonion is supposed to be dangerous; where the pterygoid branches from the FA or SMA distribute. Additionally, it is also important that the SMA and tonsillar branch are ramified near the passing area of the FA through the inferior border of the mandible.
Arterial branches outside the mandibular ramus
After passing through the antegonial notch, the FA ascends along the MST toward the nasion, following a tortuous course [67]. Marinho et al. [42] reported that not only the masseteric branch of the MA but also that there are branches from the FA and ECA distribute to the MST. Hwang et al. [28] documented that the masseteric branch directly branches from the ECA, a branch they deemed the middle masseteric artery. The transverse facial artery (TFA) from the superficial temporal artery (STA), a terminal branch of the ECA, coursed forward across the upper part of the MST [56, 66]. Not only the TFA but also other smaller branches (MbECAs), which were directly ramified from the ECA, distributed to the MST, closer to the gonion [64]. Won et al. [64] reported that the MbECA was observed in 56 % of cases, and its average width was 1.0 mm. Thus, vascular accidents involving this artery would result in rather significant postoperative bleeding without a confirmation of arterial intactness.
The premasseteric artery (PMA) ramifies from the FA and it ascends upward along the anterior border of the MST, after its emergence on the face [40]. The PMA gives off branches (MbPMA) to the anterior portion of the MST, especially its superficial layer [64]. Several tiny branches from the FA (MbFA) entered the anteroinferior portion of the MST. There is a gonial branch from the FA, which directly distributes to the MST. Observation of the intramuscular vascularization of the MST using muscle clearing has shown that the MbECA mostly supplies the angular area superior to the gonion, and that the MbFA supplies the area anterior to the gonion in the superficial layer of the MST. The MbTFA distributes to the angular area around the gonion in the deep layer [64]. Knowledge of the intramuscular distribution of respective arteries is crucial to ligate vessels during hemostatic procedures, including mandibular angle reduction with an excision of the MST.
The arterial branches inside and outside the mandibular angle can be summarized in Table 1 and Fig. 1.
The arteries giving off branches to the mandibular angle area. ECA external carotid artery, FA facial artery, SMA submental artery, PMA premasseteric artery. The masseter muscle is presented. The arteries indicated by MbTFA, MbECA, MbFA and MbPMA with red Figs. (1–4) are located outside the mandibular angle and the arteries indicated by dPtbr, Gobr, APA and aMusbr with blue alphabet letters (a–d) are located inside the mandibular angle. The abbreviations of these arteries are noted in Table 1 (color figure online)
Innervation on the mandibular angle area
The mandibular nerve (V3) branch of the trigeminal nerve gathers sensation of the lower face and the buccal, while the marginal mandibular branches (Mbr) of the FN distribute to the facial expression muscles of the lower face [65, 69]. In the case of the sensory nerve, the mandibular angle area is known to be innervated by the great auricular nerve (GAN) from the superior cervical plexus as well as the trigeminal nerve [15, 30]. The Mbr, motor nerve bundle, proceeds along the inferior border of the mandible, through the areas around the gonion and the FA emergence point on the face.
Marginal mandibular branch of facial nerve: motor fibers on the angle
The FN exits the stylomastoid foramen and proceeds forward about 1–2 cm as a single trunk (or with another minor trunk) within the petrotympanic fissure [21, 35, 52]. The FN then mostly bifurcates into the upper (temporofacial division) and lower trunks (cervicofacial division). The lower division divides into the Mbr and cervical branch (Cbr). It has been reported that the cervicofacial trunk and its branches lie above or at the level of the mandibular angle in 40 % of cases [17]. In particular, the Mbr has been known to run very close to the gonion (Fig. 2) [17, 23, 31]. Saylam et al. reported that the Mbr proceeds superior to the inferior border of the mandible in 74 % of cases, and Woltmann et al. reported that the Mbr passes upward through the inferior border of the mandible in 57.7 % of cases [53, 63].
Marginal mandibular branch in close distance to the gonion of the mandibular angle. Red arrows indicate marginal mandibular branch of facial nerve. Go gonion, DAO depressor anguli oris muscle, Pt platysma muscle, MST masseter muscle, SMG submandibular gland, FA facial artery, FV facial vein, FM intersection point of FA on inferior border of mandible (color figure online)
The distance between the gonion and the Mbr seems to be less than 1 cm. Kim et al. and Hwang et al. reported the distance between the gonion to the Mbr averages 3.4 and 3.5 mm, respectively [25, 31]. The neck’s position may alter the location of the Mbr during surgery [1]. Hwang et al. [25] reported that the distance between the inferior border of the mandible and the MBr at the one-fourth point from the gonion to the menton increased during contralateral rotation of the head in fresh cadavers. The distance between the nerve and border was 6.0 mm after the increase by rotation. In that instance, the Mbr could be more than 1 cm superior to the gonion. Kim et al. suggested that the area 19.8 mm superior and 7.4 mm inferior to the gonion in males and 15.4 mm superior and 8.1 mm inferior in females is the dangerous zone for the Mbr injury in surgery [31].
The intersection point (MF point) of the inferior border of the mandible and the FA has been regarded as an important landmark for the indication of the MBr. It has been reported that the distance between the MF point and the Mbr was about 4–5 mm [25, 31].
The number of Mbr twigs has been known to be between 1 and 4, and the most common number of twigs is 2 [3, 17, 31, 61]. Farahvash et al. reported that they observed multiple twigs of Mbr in only 2 of the 42 specimens and they suggested that the branches, which are regarded as the Mbr in the research reporting multiple twigs of the Mbr would be the buccal branch (Bbr) of the FN [17]. Actually, however, there is a report of two branches of Mbr, one of which crossed the FA deeply and the other crossed it superficially at close proximity [31]. Regardless whether a branch is Mbr or Bbr, termination and course of the FN branches are really important. An injury on the FN branch on the MF point or the gonion might result in palsy of lower facial muscles, and thus careful manipulation should be performed on the inferior border of the mandible near the gonion.
Narayanan et al. described a “nerve-free window” between Bbr and Mbr of the FN at the anterior edge of the parotid gland [49]. Since the two branch groups tended to divide there, the anteroparotid approach may be recommended to treat condylar fractures. However, Kwak et al. reported that the Bbr and Mbr are anastomosed in 34.6 % of cases [35]. Consequently, we cannot guarantee the area between Bbr and Mbr at the angular area of the mandible is truly “nerve-free”.
Submandibular gland excision and facial nerve injury
Submandibular gland (SMG) excision has been performed broadly in cases of benign and malignant salivary gland tumors. The Mbr is the most frequently damaged nerve during SMG excision. Smith et al. reported that temporary and permanent Mbr injury during submandibular SMG surgery occurred in 36 and 12 % of cases, respectively, while lingual nerve injury and hypoglossal nerve injury occurred in 2–5 % [55]. Mbr injury can cause facial muscle palsy around the corner of the mouth and asymmetry of the lower face [8]. Thus, Shaheen suggested three methods to prevent the nerve damage: (1) a lower incision at the level of the hyoid bone, (2) a clear identification and retraction of the Mbr at the level of parotid tail, and (3) a division and traction of the facial vessels and identification of the Mbr [20]. The location and course of the Mbr in the vicinity of the antegonial notch could be identified by its relationship with the FA.
Great auricular nerve: a sensory nerve on the angle
The GAN is the largest nerve of the four major cutaneous nerves from the superior cervical plexus. The GAN emerges on the anterior border of the sternocleidomastoid muscle (SCM) and ascends superoanteriorly toward the mandibular ramus and auricular area (Fig. 3). Ella et al. documented that the GAN distributes to the mandibular angle area in 97 % of cases. Thus, it is a vulnerable nerve during surgical manipulation on the mandibular angle. Amputation of the GAN could result in dysesthesia, otalgia, or traumatic neuroma [2, 7, 44, 72].
Great auricular nerve distributing retromandibular area after ascending anteriorly passing over the sternocleidomastoid muscle. GAN great auricular nerve, MST masseter muscle, SCM sternocleidomastoid muscle, EJV external jugular vein. Red arrowheads indicate twigs of the GAN that locates retromandibular area (color figure online)
Lefkowitz et al. documented that the GAN mostly coursed over the upper one-third of the SCM, and Ozturk et al. also reported that the GAN crossed the upper one-third of the muscle in more than half of the cases (53.9 %) [38, 50]. It was reported that the GAN was located about 1 cm posterior to the external jugular vein and 5 cm anterior to the external auditory meatus at the anterior border of the SCM [47, 50]. Hence, it is quite possible that the GAN lies between the mandibular angle and the upper one-third of the SCM.
Additionally, the GAN communicates with the V3 branches of the facial nerve branches. Whereas little has been revealed about functional feature of nervous connection between them, the close embryologic and phylogenic relationship between the pharyngeal apparatus and superior cervical segment in the mammals might be associated with anastomosis and overlap between the cranial and spinal nervous components [15].
Sometimes an injury or amputation of the GAN is inevitable during parotidectomy, and it has been regarded as an insignificant problem, whereas the FN injury has been known to cause more catastrophic complications, including permanent facial palsy [72]. However, Ozturk et al. reported that GAN injury can cause severe pain, although the probability is low, around 0–2.6 % of cases [50]. Amputation of the GAN during parotidectomy has been reported to occur as a traumatic neuroma in 6 % of patients undergoing parotid gland surgery [46]. Additionally, GAN injuries are known to occur at a rate of 6 % during rhytidectomy procedures, and minimally invasive techniques can increase the incidence of injury [2]. Thus, the GAN should be meticulously preserved during surgical intervention, if possible.
Arteries around the condylar process of the mandible
The ECA divides into the STA and the MA below the temporomandibular joint (TMJ). The STA ascends as it crosses the TMJ and the zygomatic arch. The STA issues the TFA that proceeds forward about 1 cm below the zygomatic arch. The STA and TFA can be easily palpated in most cases. The MA passes deep to the condylar neck of the mandible. The MA issues the deep auricular artery, anterior tympanic artery, and middle meningeal artery near the condylar neck. These arteries supply blood to the retrodiscal tissue for nutrient supply for the TMJ structure. Not only the MA, but also the ECA, STA, and TFA give off branches to the TMJ [11].
Transverse facial artery proceeding over the masseter
Yang et al. reported that the TFA ramified posterior to the ramus of the mandible as a single branch in 70.5 % of cases, and it divided into superior and inferior trunks after proceeding another 1 cm [66]. In more than half of the cases, the upper trunk of the TFA is located at the same or above the level of the temporofacial trunk of the FN. The researchers also reported that the perforator branch of TFA upper trunk perforated the anterior third of the MST in most cases. Won et al. described that the branch from the deep temporal branch of the MA supplies the anterior portion of the MST [34]. That is, the TFA and MA, which are passing superficial and deep to the condylar process of mandible, respectively, could anastomose at the anterior portion of the MST. Additionally, the branch from the FA may be connected with the TFA [66]. Thus, from an anatomical perspective, an oozing of blood near the condyle after injury might persist despite the ligation of the TFA, since a distal segment can be supplied from the MA of the FA after the anastomosis.
Superficial temporal artery ascends through the condylar area
The STA ascends 2–5 cm after ramification from the ECA and it splits into the frontal and parietal branches; the former proceeds forward and upward toward the frontal belly of the occipitofrontalis [37]. Kwak et al. reported that a muscular branch of the MST from the STA above the ramification of the TFA occurs in 36 % of cases [64]. It seems to be ramified from the TFA from the STA in front of the mandibular neck, while other masseteric branches from the TFA originate as it traverses the parotid gland between the zygomatic arch and parotid duct.
Clinically, iatrogenic or traumatic injury can cause an aneurysm or pseudoaneurysm of the head vessels. Conner et al. reported that 85 % of traumatic pseudoaneurysms of the face and temple occur in the STA [10]. The development of an aneurysm can be delayed weeks to years after the traumatic injury. Arterial expansion after post-traumatic development can lead to rupture of the artery [11].
Nerve distribution around the condylar process of the mandible
The axons of the FN innervate to the facial expression muscles and the main trunk of the FN transverses the ECA and it divides into 4–5 main divisions within the vicinity of the condyle of the mandible (Figs. 4, 5) [1, 51, 52]. The auriculotemporal nerve (ATN) is a sensory branch of the mandibular nerve and the nerve passes over the neck of the mandible and zygomatic arch (Fig. 6).
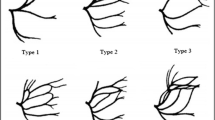
Facial nerve trunk and its five branch groups. Tbr temporal branch of the facial nerve (FN), Zbr zygomatic branch of the FN, Bbr buccal branch of the FN, Mbr marginal mandibular branch of the FN, Cbr cervical branch of the FN, TFT temporofacial trunk (or upper trunk) of the FN, CFT cervicofacial trunk (or lower trunk) of the FN, UC upper branch from the TFT forming the Bbr, LC lower branch from the cervicofacial trunk (or lower trunk) of the FN forming the Bbr, C mandibular condyle, Go gonion, PD parotid duct, STA superficial temporal artery
Nervous plexus of facial nerve trunks and divisions at the condylar area. Tbr temporal branch of the FN, Zbr zygomatic branch of the FN, Bbr buccal branch of the FN, TFT temporofacial trunk (or upper trunk) of the FN, UC upper branch from the TFT forming the Bbr, LC, lower branch from the cervicofacial trunk (or lower trunk) of the FN forming the Bbr, Tg tragus
Facial nerve trunk and its major branches at the condylar area
Mostly, the FN bifurcates into upper temporofacial and lower cervicofacial divisions [35]. Within the parotid gland, the FN divisions issue numerous twigs of four or five groups as they lie superficial to the TFA branches (Fig. 4) [66]. The FN constitutes a complicated plexus, and they anastomose with twigs from other cranial nerves, and as a result, it is very difficult to provide a nerve-free safe zone within the condylar area for the prevention of FN branch injury (Fig. 5) [1, 6, 12, 13, 24, 26, 35, 68, 70, 71]. Laurentjoye et al. recommended that three cutaneous reference lines from the tragus could serve as safe nerve-free area for dissection; the tragus-lateral canthus line for Tbr, the tragus-ala nasi line for Zbr and the tragus-lip corner line for Bbr [36]. However, Yang and Yoo reported that the FN branches formed a loop or plexiform on the condylar area in 52 % of patients, and thus, superficial landmarks cannot be provided for the FN branches within the condylar area [71]. In the case of the Tbr, which crosses the condyle and zygomatic arch, de Bonnecaze et al. found that there is no actual safe area in the temporal region [6]. The Bbr generally proceeds forwards below the orbit as it distributes to the midface musculature of the upper lip, cheek, and nose area. While the Bbr rarely branches from the main trunk of the FN, it almost forms a Y shape from the branches of the upper and lower trunks. Numerous studies have reported that the Bbr reconnects with the Zbr in about 87–100 % of cases [5, 35, 62].
Considering the Sihler’s staining study of Yang et al., the distribution of the FN would be thought to form a non-linear branching pattern over a two-dimensional area [68]. There were many studies that provided the intersection points of the FN with superficial landmarks regarding the complexity of FN ramification (Table 2) [6, 17, 23, 58, 71]. Tayfur et al. delineated that there were an average of 3.7 branches of TBr which crossed the level of the zygomatic arch [58]. de Bonnecaze et al. reported that the area 22.6–26.1 mm anterior to the tragus at the level of the superior part of the zygomatic arch and 27.5–30.4 mm anterior to the tragus at the level of the inferior part of the arch are dangerous areas, where the FN branch existed in the case of more than 85 % of patients [6]. Hwang et al. described that the Tbr is located 21.5–35.4 mm anterior to the root of the helix at the zygomatic arch [27]. Farahvash et al. reported that the first intersecting Tbr branch on the zygomatic arch is located about 20 mm anterior to the tragus, the second one is located about 27–28 mm anterior to the tragus, and the third is located about 39–36 mm anterior to the tragus [17]. They also reported that the bifurcation of upper and lower division of the FN is located about 1.5–1.6 mm anterior to a line through the tragus and gonion. Yang and Yoo reported that the FN passed over a vertical line anterior 2 cm to the tragus, on one point in 24 %, two points in 48 %, and three points in 28 %. The FN nerves crossed this vertical line 0.5–2 cm inferior to the tragus [71]. They also documented that the FN branches proceed between the tragus and lowermost point of earlobe and that several twigs of the Tbr and Zbr cross the tragus-ala nasi line 24–38 mm anterior to the tragus. Considering these studies, there is a high probability of encountering FN branches in the area 2–4 cm anterior to the tragus at the vicinity of the condyle.
Complicated ramification and abundant anastomosis of the FN branch could serve as fibers deliver motor control information bypassing via plexiform network, in the cases of nerve injury [14, 36, 43, 59, 68]. Thus, the injury of nerve twigs on these nervous plexiform area might result in minimal loss of function [49]. However, the proximal part of FN lies on the condylar area as a small number of thick divisions. An injury of the main trunk or large divisions of the FN on the condylar area would result in irreversible serious palsy on broad area of the face.
Clinical implications of the facial nerve at the condylar area
The FN can be damaged during rhytidectomy, parotidectomy, and reduction of a condylar fracture. In the cases of condylar fracture, many surgeons prefer an open reduction for the fracture with various surgical approaches. There are many reports about facial nerve damage after a preauricular or retromandibular incision for the reduction of condylar fractures [16, 41, 57]. The FN and ATN lie within or deep to the temporoparietal fascia, which is one of the SMAS (superficial musculoaponeurotic system) structures [56]. The parotid sheath is connected to the platysma muscle and it lies beneath the SMAS. The initial surgical approach should be performed as to avoid injury of the Tbr and Zbr, heeding this layered relationship [49].
Additionally, the FN branches near the condyle should be preserved during removal of parenchyma of parotid gland. Musani et al. reported that temporary FN dysfunction occurred in 26.3 % of 235 patients after parotidectomy and permanent FN dysfunction occurred in 1.7 % [48]. In particular, the removal of a tumor at the anterior and superior portion of the deep lobe of parotid gland presents a higher risk of temporary or permanent FN dysfunction [29]. The risk is closely related to the Tbr and Zbr within the vicinity of the mandibular condyle. The Tbr has been regarded as the most vulnerable branch of the FN during the parotidectomy [9]. Finding the main trunk of the FN before removing parotid gland tissue, and tracing its divisions and twigs meticulously would be the safest method to prevent FN injury during parotidectomy procedures. Hence, it is important to discover the course and location of the nerve near the condyle, regardless of the branching pattern of the FN within the parotid gland.
Auriculotemporal nerve at the condylar area and Frey syndrome
Schmidt et al. described that the ATN passes in direct contact with the medial aspect of the mandibular neck at a level of about 7 mm (range 0–13 mm) inferior to the superior condyle [54]. Fernandes et al. also reported that the ATN proceeded 10–13 mm inferior and 1–2 mm posterior to the superior surface of the mandibular condyle [18]. The nerve distributes to the skin of auricle, external acoustic meatus, and temporal region. It also delivers postganglionic parasympathetic fibers, which synapse with preganglionic fibers of the lesser petrosal nerve of glossopharyngeal nerve at the otic ganglion. The parasympathetic component via the ATN plays a role in the secretion of the parotid gland [56].
Sometimes, the parasympathetic fibers within the ATN reconnect with not only parotid gland, but also with sweat glands after parotidectomy or open reduction of a condylar fracture. This causes gustatory sweating (sweating while eating foods) and it has been known as auriculotemporal syndrome or Frey syndrome. Although the condylar fracture is very frequent in mandibular fractures, the Frey syndrome occurs very rarely [19]. It has been recommended to approach the condylar area via a retroauricular or intraoral incision to prevent ATN or FN injury during the reduction of a condylar fracture or correction of TMJ ankylosis [4, 32].
Conclusion
The ECA and FA issue various branches into the internal and external aspects of the mandibular ramus at the angular area. The Mbr proceeds forward through area within 10 mm around the gonion, the posteroinferior point of the mandibular angle. The GAN distributes to the angular and parotid regions. The ECA, STA, TFA, and MA give off various branches passing medial and lateral to the mandibular neck and condyle. The FN trunk and ATN proceed near the condyle. The neurovascular structures of the mandibular angle and condyle area are vulnerable during esthetic surgeries, such as mandibular angle reduction and rhytidectomy; removal of tumors, such as parotidectomy and submandibular gland excision; and the TMJ approach for reduction of condylar fractures and correction of TMJ ankylosis. Comprehensive anatomical information in the present study could help surgeons prevent injury to the described neurovascular structures during procedures.
References
Baker DC, Conley J (1979) Avoiding facial nerve injuries in rhytidectomy. Anatomical variations and pitfalls. Plast Reconstr Surg 64(6):781–795
Barbour JR, Iorio ML, Halpern DE (2013) Surgical decompression of the great auricular nerve: a therapeutic option for neurapraxia following rhytidectomy. Plast Reconstr Surg 133(2):255–260
Basar R, Sargon MF, Tekdemir Y, Elhan A (1997) The marginal mandibular branch of the facial nerve. Surg Radiol Anat 19(5):311–314
Benech A, Arcuri F, Baragiotta N, Nicolotti M, Brucoli M (2011) Retroauricular transmeatal approach to manage mandibular condylar head fractures. J Craniofac Surg 22(2):641–647
Bernstein L, Nelson RH (1984) Surgical anatomy of the extraparotid distribution of the facial nerve. Arch Otolaryngol 110(3):177–183
de Bonnecaze G, Chaput B, Filleron T, Al Hawat A, Vergez S, Chaynes P (2014) The frontal branch of the facial nerve: can we define a safety zone? Surg Radiol Anat. doi:10.1007/s00276-014-1386-3. [Epub ahead of print]
de Chalain T, Nahai F (1995) Amputation neuromas of the great auricular nerve after rhytidectomy. Ann Plast Surg 35(3):297–299
Chang YN, Kao CH, Lin YS, Lee JC (2013) Comparison of the intraoral and transcervical approach in submandibular gland excision. Eur Arch Otorhinolaryngol 270(2):669–674
Clayman G, Cohen J (2011) Atlas of Head & Neck Surgery, 1st edn. Elsevier Saunders, Philadelphia, pp 227–241
Conner WC, Rohrich RJ, Pollock RA (1998) Traumatic aneurysms of the face and temple: a patient report and literature review, 1644 to 1998. Ann Plast Surg 41(3):321–326
Cuccia AM, Caradonna C, Caradonna D, Anastasi G, Milardi D, Favaloro A, De Pietro A, Angileri TM, Caradonna L, Cutroneo G (2013) The arterial blood supply of the temporomandibular joint: an anatomical study and clinical implications. Imaging Sci Dent 43(1):37–44
Dargent M, Corales G, Estigarribia A (1970) Value of total parotidectomy preserving the facial nerve in malignant tumors of the parotid gland. Ann Chir 24(11):617–626
Davis RA, Anson BJ, Budinger JM, Kurth LR (1956) Surgical anatomy of the facial nerve and parotid gland based upon a study of 350 cervicofacial halves. Surg Gynecol Obstet 102(4):385–412
Diamond M, Wartmann CT, Tubbs RS, Shoja MM, Cohen-Gadol AA, Loukas M (2011) Peripheral facial nerve communications and their clinical implications. Clin Anat 24(1):10–18
Ella B, Langbour N, Caix P, Midy D, Deliac P, Burbaud P (2014) Transverse cervical and great auricular nerve distribution in the mandibular area: a study in human cadavers. Clin Anat 28(1):109–117
Ellis E 3rd (1998) Complications of mandibular condyle fractures. Int J Oral Maxillofac Surg 27(4):255–257
Farahvash MR, Yaghoobi A, Farahvash B, Farahvash Y, Hadadi Abiyaneh S (2013) The extratemporal facial nerve and its branches: analysis of 42 hemifacial dissections in fresh Persian (Iranian) cadavers. Aesthetic Plast Surg 33(2):201–208
Fernandes PRB, de Vasconsellos HA, Okeson JP, Bastos RL, Maia MLT (2003) The anatomical relationship between the position of the auriculotemporal nerve and mandibular condyle. Cranio J Craniomandib Pract 21(3):165–171
Güleç AT, Seçkin D, Bulut Ş, Sarfakoğlu E (2001) Cutaneous sinus tract of dental origin. Int J Dermatol 40(10):650–652
Hernando M, Echarri RM, Taha M, Martin-Fragueiro L, Hernando A, Mayor GP (2012) Surgical complications of submandibular gland excision. Acta Otorrinolaringológica Esp 63(1):42–46
Holt JJ (1996) The stylomastoid area: anatomic-histologic study and surgical approach. Laryngoscope 106(4):396–400
Huang MH, Lee ST, Rajendran K (1998) Clinical implications of the velopharyngeal blood supply: a fresh cadaveric study. Plast Reconstr Surg 102(3):655–667
Hwang K (2014) Surgical anatomy of the facial nerve relating to facial rejuvenation surgery. J Craniofac Surg 25(4):1476–1481
Hwang K, Han JY, Battuvshin D, Kim DJ, Chung IH (2004) Communication of infraorbital nerve and facial nerve: anatomic and histologic study. J Craniofac Surg 15(1):88–91
Hwang K, Huan F, Ki SH, Nam YS, Han SH (2012) Location of the mandibular branch of the facial nerve according to the neck position. J Craniofac Surg 23(5):1488–1490
Hwang K, Hwang JH, Cho HJ, Kim DJ, Chung IH (2005) Horizontal branch of the supraorbital nerve and temporal branch of the facial nerve. J Craniofac Surg 16(4):647–649
Hwang K, Kim YJ, Chung IH (2004) Innervation of the corrugator supercilii muscle. Ann Plast Surg 52(2):140–143
Hwang K, Kim YJ, Chung IH, Lee SI (2001) Deep middle masseteric artery (dMMA) attributed to hemorrhage in resection of masseter muscle and mandibular angle. J Craniofac Surg 12(4):381–385
Ikoma R, Ishitoya J, Sakuma Y, Hirama M, Shiono O, Komatsu M, Oridate N (2014) Temporary facial nerve dysfunction after parotidectomy correlates with tumor location. Auris Nasus Larynx 41(5):479–484
Kim HJ, Koh KS, Oh CS, Hu KS, Kang JW, Chung IH (2002) Emerging patterns of the cervical cutaneous nerves in Asians. Int J Oral Maxillofac Surg 31(1):53–56
Kim DI, Nam SH, Nam YS, Lee KS, Chung RH, Han SH (2009) The marginal mandibular branch of the facial nerve in Koreans. Clin Anat 22(2):207–214
Ko EC, Chen MY, Hsu M, Huang E, Lai S (2009) Intraoral approach for arthroplasty for correction of TMJ ankylosis. Int J Oral Maxillofac Surg 38(12):1256–1262
Koh KS, Kim HJ, Oh CS, Chung IH (2003) Branching patterns and symmetry of the course of the facial artery in Koreans. Int J Oral Maxillofac Surg 32(4):414–418
Kwak HH, Hu KS, Hur MS, Won SY, Kim GC, Park BS, Kim HJ (2008) Clinical implications of the topography of the arteries supplying the medial pterygoid muscle. J Craniofac Surg 19(3):795–799
Kwak HH, Park HD, Youn KH, Hu KS, Koh KS, Han SH, Kim HJ (2004) Branching patterns of the facial nerve and its communication with the auriculotemporal nerve. Surg Radiol Anat 26(6):494–500
Laurentjoye M, Veyret A, Ella B, Uzel AP, Majoufre-Lefebvre C, Caix P, Ricard AS (2014) Surgical anatomy of the preauricular anteroparotid approach for mandibular condyle surgery. Surg Radiol Anat 36(9):883–888
Lee JG, Yang HM, Hu KS, Lee YI, Lee HJ, Choi YJ, Kim HJ (2015) Frontal branch of the superficial temporal artery: anatomical study and clinical implications regarding injectable treatments. Surg Radiol Anat 37(1):61–68
Lefkowitz T, Hazani R, Chowdhry S, Elston J, Yaremchuk MJ, Wilhelmi BJ (2013) Anatomical landmarks to avoid injury to the great auricular nerve during rhytidectomy. Aesthetic Plast Surg 33(1):19–23
Lucev N, Bobinac D, Maric I, Drescik I (2000) Variations of the great arteries in the carotid triangle. Otolaryngol Head Neck Surg 122(4):590–591
Magden O, Edizer M, Tayfur V, Atabey A (2004) Anatomic study of the vasculature of the submental artery flap. Plast Reconstr Surg 114(7):1719–1723
Manisali M, Amin M, Aghabeigi B, Newman L (2003) Retromandibular approach to the mandibular condyle: a clinical and cadaveric study. Int J Oral Maxillofac Surg 32(3):253–256
Marinho LH, Shanahan DA, Langdon JD, Sinnatamby CS (1991) The inferiorly based masseter muscle flap: anatomical basis for its use in head and neck reconstructive surgery. Int J Oral Maxillofac Surg 20(2):100–105
Martin H, Helsper JT (1957) Spontaneous return of function following surgical section or excision of the seventh cranial nerve in the surgery of parotid tumors. Ann Surg 146(5):715–727
McKinney P, Katrana DJ (1980) Prevention of injury to the great auricular nerve during rhytidectomy. Plast Reconstr Surg 66(5):675–679
Moore KL, Dalley AF (2005) Clinically Oriented Anatomy, 5th edn. Lippincott Williams & Wilkins, Baltimore, pp 978–982
Moss CE, Johnston CJ, Whear NM (2000) Amputation neuroma of the great auricular nerve after operations on the parotid gland. Br J Oral Maxillofac Surg 38(5):537–538
Murphy R, Dziegielewski P, O’Connell D, Seikaly H, Ansari K (2012) The great auricular nerve: an anatomic and surgical study. J Otolaryngol Head Neck Surg 41:75–77
Musani MA, Zafar A, Suhail Z, Malik S, Mirza D (2014) Facial nerve morbidity following surgery for benign parotid tumours. J Coll Physicians Surg Pak 24(8):569–572
Narayanan V, Ramadorai A, Ravi P, Nirvikalpa N (2012) Transmasseteric anterior parotid approach for condylar fractures: experience of 129 cases. Br J Oral Maxillofac Surg 50(5):420–424
Ozturk CN, Ozturk C, Huettner F, Drake RL, Zins JE (2014) A failsafe method to avoid injury to the great auricular nerve. Aesthetic Plast Surg 34(1):16–21
Park IY, Lee ME (1977) A morphological study of the parotid gland and the peripheral branches of the facial nerve in Koreans. Yonsei Med J 18(1):45–51
Salame K, Ouaknine GER, Arensburg B, Rochkind S (2002) Microsurgical anatomy of the facial nerve trunk. Clin Anat 15(2):93–99
Saylam C, Ucerler H, Orhan M, Uckan A, Ozek C (2007) Localization of the marginal mandibular branch of the facial nerve. J Craniofac Surg 18(1):137–142
Schmidt BL, Pogrel MA, Necoechea M, Kearns G (1998) The distribution of the auriculotemporal nerve around the temporomandibular joint. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 86(2):165–168
Smith WP, Peters WJ, Markus AF (1993) Submandibular gland surgery: an audit of clinical findings, pathology and postoperative morbidity. Ann R Coll Surg Engl 75(3):164–167
Standring S (2008) Gray’s Anatomy: The Anatomical Basis of Clinical Practice, 40th edn. Churchill Livingstone, Edinburgh, p 446
Tang W, Gao C, Long J, Lin Y, Wang H, Liu L, Tian W (2009) Application of modified retromandibular approach indirectly from the anterior edge of the parotid gland in the surgical treatment of condylar fracture. J Oral Maxillofac Surg 67(3):552–558
Tayfur V, Edizer M, Magden O (2010) Anatomic bases of superficial temporal artery and temporal branch of facial nerve. J Craniofac Surg 21(6):1945–1947
Tohma A, Mine K, Tamatsu Y, Shimada K (2004) Communication between the buccal nerve (V) and facial nerve (VII) in the human face. Ann Anat 186(2):173–178
Troupis TG, Dimitroulis D, Paraschos A, Michalinos A, Protogerou V, Vlasis K, Troupis G, Skandalakis P (2011) Lingual and facial arteries arising from the external carotid artery in a common trunk. Am Surg 77(2):151–154
Wang TM, Lin CL, Kuo KJ, Shih C (1991) Surgical anatomy of the mandibular ramus of the facial nerve in Chinese adults. Acta Anat 142(2):126–131
Wilson AW, Ethunandan M, Brennan PA (2005) Transmasseteric antero-parotid approach for open reduction and internal fixation of condylar fractures. Br J Oral Maxillofac Surg 43(1):57–60
Woltmann M, de Faveri R, Sgrott EA (2006) Anatomosurgical study of the marginal mandibular branch of the facial nerve for submandibular surgical approach. Braz Dent J 17(1):71–74
Won SY, Choi DY, Kwak HH, Kim ST, Kim HJ, Hu KS (2012) Topography of the arteries supplying the masseter muscle: using dissection and Sihler’s method. Clin Anat 25(3):308–313
Won SY, Yang HM, Woo HS, Chang KY, Youn KH, Kim HJ, Hu KS (2014) Neuroanastomosis and the innervation territory of the mental nerve. Clin Anat 27(4):598–602
Yang HJ, Gil YC, Lee HY (2010) Topographical anatomy of the transverse facial artery. Clin Anat 23(2):168–178
Yang HM, Lee JG, Hu KS, Gil YC, Choi YJ, Lee HK, Kim HJ (2014) New anatomical insights on the course and branching patterns of the facial artery: clinical implications of injectable treatments to the nasolabial fold and nasojugal groove. Plast Reconstr Surg 133(5):1077–1082
Yang HM, Won SY, Kim HJ, Hu KS (2013) Sihler staining study of anastomosis between the facial and trigeminal nerves in the ocular area and its clinical implications. Muscle Nerve 48(4):545–550
Yang HM, Won SY, Lee JG, Han SH, Kim HJ, Hu KS (2011) Sihler-stain study of buccal nerve distribution and its clinical implications. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 113(3):334–339
Yang HM, Won SY, Lee YI, Kim HJ, Hu KS (2014) The Sihler Staining Study of the Infraorbital Nerve and Its Clinical Complication. J Craniofac Surg 25(6):2209–2213
Yang HM and Yoo YB (2014) Anatomy of the Facial Nerve at the Condylar Area: Measurement Study and Clinical Implications. Sci World J e473568
Yang HM, Kim HJ, Hu KS (2015) Anatomic and histological study of great auricular nerve and its clinical implication. J Plast Reconstr Aesthet Surg 68(2):230–236
Acknowledgments
We thank Dr. Youn Kwan-Hyun at Medart and Mr. Lee Hyung-Jin at Yonsei University College of Dentistry for contribution to dissection, photograph and illustration.
Conflict of interest
None of the authors have financial or private relationships with commercial, academic, or political organizations or people that could have improperly influenced this research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yang, HM., Won, SY., Kim, HJ. et al. Neurovascular structures of the mandibular angle and condyle: a comprehensive anatomical review. Surg Radiol Anat 37, 1109–1118 (2015). https://doi.org/10.1007/s00276-015-1482-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-015-1482-z