Abstract
Background
Twenty percent of the patients with AAA have an aneurysm involving the common iliac arteries. Large common iliac diameter can be treated with an iliac branched device or extension of the stent graft to the external iliac artery with occlusion of the ipsilateral internal iliac artery (IIA) to prevent type 2 endoleaks. This study describes and evaluates a embolization technique using Onyx in conjunction with EVAR in aneurysms with poor landing zones in the common iliac arteries.
Methods
Patients with Onyx IIA embolization during EVAR, identified from the hospital operating code database, constitute the study population. Onyx embolization was performed by injection at the IIA origin. Peri- and postoperative complications were collected from the medical records. Thin-sliced CT scan was performed 1 month and 1 year after the procedure.
Results
Thirty-six patients with complex iliac anatomy and insufficient landing zones (without sealing possibility for standard stent grafts) were identified out of 243 consecutive EVAR treatments during a 13-year period. In seventeen patients (7%), the IIA was embolized with Onyx. Technical success was obtained in all 17 patients, without adverse event or procedural complication. No complication related to the embolization procedure was noted during follow-up.
Conclusions
During EVAR treatment of patients with aneurysm involving the common iliac artery, Onyx embolization of IIA is a feasible option without need of selective catheterization of the IIA orifice, potentially preserving important branches of the IIA and simplifying emergency procedures.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Endovascular aneurysm repair (EVAR) of abdominal aortic aneurysms (AAA) is widely accepted and has become the method of choice in many centers. EVAR reduces the peri- and postoperative mortality and morbidity as well as length of stay in hospital and improves short-term survival [1, 2]. Twenty percent of the patients with AAA have an aneurysm involving the common iliac arteries which makes the repair technically more challenging [3]. Large common iliac diameter may increase the risk of inadequate distal seal [4]. In these cases, it is possible to use bell-bottom stent grafts but long-term results involve frequent type 1b endoleaks with insufficient sealing [5, 6]. The use of an iliac branched device (IBD) is alternative when preserved IIA flow is desired [7]. Another widely accepted method to reach adequate distal seal is to extend the landing zone to the external iliac artery (EIA) with occlusion of the ipsilateral internal iliac artery (IIA) to prevent type 2 endoleaks [7, 8]. Occlusion of the IIA can be achieved with coils or plugs [8]. This requires selective catheterization and is often time-consuming and particularly coils may interfere with pelvic circulation. A previous study demonstrated less buttock claudication with proximal occlusion of the hypogastric artery using proximal plugs compared to peripheral coiling [9]. An alternative to occlude the IIA orifice during EVAR is the use of liquid embolic agents. Onyx, an ethylene vinyl alcohol copolymer (6%), is a commercially available liquid embolic agent. When dissolved in anhydrous dimethyl sulfoxide (DMSO) and mixed with tantalum powder, it offers effective targeted embolization with good radiopaque properties [10]. The experience of Onyx has in the past mainly been from neuroradiology treating cerebral arteriovenous malformations [11], but the use of Onyx in peripheral vascular intervention is increasing [12].
The aim of this study was to describe and evaluate a new embolization technique using Onyx in conjunction with EVAR in aneurysms with poor landing zones (without sealing possibility for standard stent grafts) in the common iliac arteries.
Materials and Methods
Population
The clinical records and X-ray examinations, identified from the hospital operating code database, of all consecutive patients who underwent endovascular treatment for AAA at Helsingborg University hospital, Sweden, between January 2003 and March 2015 were reviewed. The patients’ medical records were analyzed for preoperative demographics, indications for treatment, perioperative complications and follow-up information. Preoperative CT scans were studied for diameter measures and collateral vascular patency (ipsilateral profunda femoral artery (PFA) and contralateral IIA). All procedures were planned by 3D-centerline reconstructions. Perioperative angiograms were analyzed for side of approach, level of IIA embolization, amount of used Onyx and technical success. Technical success was defined as successful occlusion of IIA and absence of endoleak on completion angiogram. Method of vascular access and closure were recorded. Perioperative complications, defined as complications associated with the procedure or after the procedure until discharge from hospital, were collected from the medical records. Postoperative complications within 1 month were registered from medical records. Postoperative CT scans after 1 month and 1 year were reviewed for endoleaks and distal embolization in the treated IIA.
Onyx Embolization Procedure
An additional puncture was performed in the ipsilateral CFA in close conjunction with the main introducer for the EVAR system. A 4-Fr sheath was used, and a 4-Fr Onyx compatible catheter was subsequently placed in the aneurysm sac or in the proximal common iliac artery. The EVAR procedure was performed with Zenith Flex® AAA Endovascular Graft Bifurcated Main Body Graft (COOK MEDICAL LLC P.O. Box 4195 Bloomington, IN 47402-4195, USA) with extension and deployment of the ipsilateral limb to the EIA for adequate seal. The 4-Fr catheter was, after stentgraft delivery, pulled down into the CIA aneurysm and placed with its tip just cranial to the IIA origin, without need to intubate the ostium of the IIA. The catheter was primed with an amount of DMSO corresponding to the dead space of the catheter. Onyx was slowly injected at the IIA origin until the main IIA branch was occluded. Slow and controlled injection of Onyx is important to prevent distal embolization to peripheral IIA branches. Delivery of a self-expanding nitinol stent from the distal part of the leg extension to the EIA was performed to create a smooth transition from the stent graft. Finally, a completion angiogram was performed to ensure that occlusion is achieved before withdrawing the catheter (Fig. 1A–D).
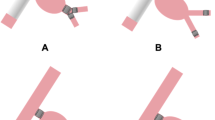
EVAR procedure with IIA Onyx embolization. A Aneurysm involving common iliac artery. B Contrast cast in Onyx compatible catheter (black arrow) outside stent graft at internal iliac artery origin during EVAR, stentgraft limb is extended to external iliac artery. C Onyx cast (broad white arrow) in internal iliac artery origin. D Completion angiogram
Statistics
Categorical variables are indicated by frequency and percentage. Continuous results are shown by means and standard deviations (SD) or median and range. Calculations were performed using SPSS18.0 (SPSS Inc., Chicago, IL, USA).
Ethics
The study was performed in accordance with the spirit of the Declaration of Helsinki and in agreement with the guidelines for conducting a clinical investigation as outlined in the ISO 14-155. Informed consent was obtained from all patients. The study was approved by the Swedish Ethical Review Authority 2019-00452.
Results
A total of 243 patients underwent endovascular repair of AAA during the study period. Complex iliac anatomy with insufficient landing zones in the distal CIA was present in 36 patients (15%). Twelve patients (5%) were treated with IBD (Zenith® Branch—COOK MEDICAL LLC P.O. Box 4195 Bloomington, IN 47402-4195, USA). Seven (3%) patients were treated with coil embolization of IIA.
In seventeen patients (7%), the IIA was embolized with Onyx. Indications for EVAR treatment with Onyx embolization were aortoiliac aneurysm in 12 cases, AAA and short CIA (< 20 mm) in 1 case, ruptured CIA during standard EVAR for AAA in 1 case, bilateral isolated IIA aneurysms treated with EVAR and Onyx embolization of aneurysm side branches in 1 case and isolated CIA aneurysm in 2 cases. Preoperative patient characteristics are shown in Table 1. Preoperative CT scans were reviewed. Mean AAA diameter was 66 mm (53–90), ipsilateral CIA diameter 34 mm (21–76) and ipsilateral IIA diameter 14 mm (6–38). The ipsilateral PFA was patent in all patients, and contralateral IIA patency was 12 (92%). The patient with bilateral IIA aneurysms measured 60 mm diameter bilaterally in the IIA and had patent PFA bilaterally. Perioperative data were recorded in all 17 cases. Ultrasound-guided percutaneous access was achieved in all patients as well as ipsilateral approach for IIA embolization. The level of IIA embolization was the main IIA trunk in all cases. A 3.0–4.5 mL of Onyx was used to embolize the orifice of the hypogastric artery at the procedures. In 1 patient, the first IIA branches were occluded (Fig. 2); however, this was asymptomatic. Technical success was achieved in all 17 patients (100%). Fascial closure technique (a suturing technique for closure of the femoral artery with a purse string suture through fascia lata during EVAR) [13] was successfully used in 18 femoral access sites; femoral cut-down was used in 9 femoral access sites and closure devices in 7 femoral arteries.
EVAR procedure with suboptimal IIA Onyx embolization. A Aneurysm involving common iliac artery. B Contrast cast in Onyx compatible catheter (black arrow) outside stent graft at internal iliac artery origin during EVAR, stentgraft limb is extended to external iliac artery. C Onyx cast (broad white arrow) in internal iliac artery origin. D Completion angiogram
No procedure-related serious complication (colitis, paraplegia or gluteal necrosis) occurred. Perioperative complications as defined were urinary tract infection (n = 2), hip fracture after fall in the vascular ward (n = 1), groin hematoma (n = 1), ruptured CIA when balloon dilatation of the endograft (n = 1), partial coverage of renal artery requiring additional renal stenting (n = 1) and rupture of proximal aortic neck when balloon dilatation of the endograft requiring an additional stentgraft cuff and a Palmaz stent, resulting in loss of one renal artery (n = 1). Postoperative complications were groin infection requiring debridement and VAC treatment (n = 1) and urosepsis (n = 1). Out of 17 patients, 16 had 1-month clinical follow-up without reports of buttock claudication or erectile dysfunction.
One patient died due to hepatic failure after 5 months. One type 1b endoleak from the contralateral side and 2 cases of type 2 endoleak from IMA or lumbar arteries, not related to the embolized IIA, were noted at 1-year follow-up.
No reintervention related to Onyx embolization was needed during follow-up. Two reinterventions were performed during 12-month follow-up: extension to EIA in the one patient with type 1b endoleak on the contralateral side, and percutaneous angioplasty (PTA) of the common femoral artery (CFA) due to stenosis of the artery after fascial closure in the other patient.
Discussion
This paper describes successful results from occlusion of IIA using Onyx deposition outside of the stent graft at the level of the orifice of the IIA, without serious major complications.
Aneurysmal extension into the CIA if performing EVAR is challenging and adds complexity to endovascular repair. Various options are available for treating aortoiliac aneurysms. Dilatation of the common iliac artery (CIA) leaves a limited or even a completely absent distal landing zone for commercially available stent grafts, which have a maximum diameter of 28 mm. Lack of an adequate landing zone in the CIA is a common reason for late type 1b endoleaks [14].
Limb extension to EIA is frequently needed to achieve adequate distal seal. To prevent type 2 endoleak in such cases, the IIA must be occluded or treated with an IBD. Distal relocation of the iliac bifurcation with external-to-internal bypass is a hybrid EVAR alternative to preserve the pelvic circulation [15]. IIA occlusion is not performed without complications. Buttock claudication (BC) and impotence have been reported in up to 50% after IIA occlusion [16]. BC tends to be reversible in many cases [17]. IBD is flow preserving thus preventing pelvic ischemic symptom, but not all patients are anatomically suitable for IBD. Different techniques for IIA occlusion have been investigated, and some key features have been pointed out such as proximal main branch occlusion, staged occlusion when bilateral, importance of collateral vessel blood supply and risk groups for BC, e.g., low age and/or left ventricular dysfunction [17]. Previous reported techniques include coils, plugs and plain IIA coverage with stentgraft limb without prior embolization (in selected cases) or the use of bell-bottom-shaped iliac limb grafts for IIA preservation in unsuitable common iliac landing site [5,6,7, 11]. This paper describes a technique of IIA occlusion with Onyx [10]. The technique used in the present study can be performed without need of selective catheterization of the IIA orifice, potentially simplifying emergency procedures.
Embolization with particles and liquid embolic agents inherit a risk of non-target embolization. The presented technique focuses on embolization of the main IIA trunk. As shown in Fig. 2, it is possible for the Onyx cast to extend into proximal IIA branches without any symptoms for the patient. The main issue is to prevent embolization to distal IIA branches. No case of buttock claudication was reported; this is probably due to the fact that no distal branches of the IIA were obliterated which allows for collateralization.
Proximal main IIA branch occlusion was achieved in all 17 cases. There were no reported serious complications associated with the embolization procedure (colitis, paraplegia, gluteal necrosis). Buttock claudication and/or erectile dysfunction was not reported. On 1-month follow-up CT scan, there were no IIA-related type 2 endoleaks. In 1 patient, the first IIA branches were occluded; however, this was asymptomatic. On 1-year follow-up, we found 2 patients with type 2 endoleaks, but none were related to the embolized IIA.
Study limitations: This is a small retrospective study with limited, 12-month follow-up time. Although cost is an issue with Onyx, in our experience 3–4.5 mL of Onyx was needed for adequate occlusion of the IIA adding a cost of aproximally 1600–2100 Euro to the procedure; no direct comparison to coil- or plug occlusion was performed.
Conclusion
In EVAR treatment of patients with aneurysm involving the common iliac artery, Onyx embolization of IIA is a feasible option without need of selective catheterization of the IIA orifice, potentially preserving important branches of the IIA and simplifying emergency procedures.
References
Patel R, Sweeting MJ, Powell JT, Greenhalgh RM, EVAR Trial Investigators. Endovascular versus open repair of abdominal aortic aneurysm in 15-years’ follow-up of the UK endovascular aneurysm repair trial 1 (EVAR trial 1): a randomised controlled trial. Lancet. 2016;388(10058):2366–74.
Powell JT, Sweeting MJ, Ulug P, Blankensteijn JD, Lederle FA, Becquemin JP et al. EVAR-1, DREAM, OVER and ACE Trialists. Meta-analysis of individual-patient data from EVAR-1, DREAM, OVER and ACE trials comparing outcomes of endovascular or open repair for abdominal aortic aneurysm over 5 years. Br J Surg. 2017;104:166–78.
Armon MP, Wenham PW, Whitaker SC, Gregson RH, Hopkinson BR. Common iliac artery aneurysms in patients with abdominal aortic aneurysms. Eur J Vasc Endovasc Surg. 1998;15(3):255–7.
Baum RA, Stavropoulos SW, Fairman RM, Carpenter JP. Endoleaks after endovascular repair of abdominal aortic aneurysms. J Vasc Interv Radiol. 2003;14(9 Pt 1):1111–7.
McDonnel CO, Semmens JB, Allen YB, Jansen SJ, Brooks DM, Lawrence-Brown MM. Large iliac arteries: a high-risk group for endovascular aortic aneurysm repair. J Endovasc Ther. 2007;14(5):625–9.
Torsello G, Schönefeld E, Osada N, Austermann M, Pennekamp C, Donas KP. Endovascular treatment of common iliac artery aneurysms using the bell-bottom technique: long-term results. J Endovasc Ther. 2010;17(4):504–9.
Verzini F, Parlani G, Romano L, De Rango P, Panuccio G, Cao P. Endovascular treatment of iliac aneurysm: concurrent comparison of side branch endograft versus hypogastric exclusion. J Vasc Surg. 2009;49(5):1154–61.
Vieth FJ, Baum RA, Ohki T, Amor M, Adiseshiah M, Blankensteijn JD, et al. Nature and significance of endoleaks and endotension: summary of opinions expressed at an international conference. J Vasc Surg. 2002;35(5):1029–35.
Libicher M, Pavlidis D, Bangard C, Gawenda M. Occlusion of the internal iliac artery prior EVAR: comparison of coils and plugs. Vasc Endovasc Surg. 2012;46(1):34–9.
Vanninen RL, Manninen I. Onyx, a new liquid embolic material for peripheral interventions: preliminary experience in aneurysm, pseudoaneurysm and pulmonary arteriovenous malformation embolization. Cardiovasc Interv Radiol. 2007;30(2):196–200.
Cekirge HS, Saatci I, Ozturk MH, Cil B, Arat A, Mawad M, et al. Late angiographic and clinical follow-up results of 100 consecutive aneurysms treated with Onyx reconstruction: largest single center experience. Neuroradiology. 2006;48(2):113–26.
Bosiers MJ, Deloose K, Peeters P, Torsello G, Zeller T, Scheinert D, et al. Midterm results of the transarterial use of Onyx in the treatment of persisting type II endoleaks after EVAR. J Cardiovasc Surg (Torino). 2013;54(4):469–75.
Harrison GJ, Thavarajan D, Brennan JA, Vallabhaneni SR, McWilliams RG, Fisher RK. Fascial closure following percutaneous endovascular aneurysm repair. Eur J Vasc Endovasc Surg. 2011;41(3):346–9.
Gray D, Shahverdyan R, Reifferscheid V, Gawenda M, Brunkwall JS. EVAR with flared iliac limbs has a high risk of late type 1b endoleak. Eur J Vasc Endovasc Surg. 2017;54(2):170–6.
Mansukhani NA, Havelka GE, Helenowski IB, Rodriguez HE, Hoel AW, Eskandari MK. Hybrid EVAR: preservation of pelvic perfusion with external to internal iliac artery bypass. Ann Vasc Surg. 2017;42:162–8.
Bosanquet DC, Wilcox C, Whitehurst L, Cox A, Williams IM, Twine CP. Systematic review and meta-analysis of the effect of internal iliac artery exclusion for patients undergoing EVAR. Eur J Vasc Endovasc Surg Off J Eur Soc Vasc Surg. 2017;53(4):534–48.
Saengprakai W, van Herwaarden JA, Georgiadis GS, Slisatkorn W, Moll FL. Clinical outcomes of hypogastric artery occlusion for endovascular aortic aneurysm repair. Minim Invasive Ther Allied Technol MITAT Off J Soc Minim Invasive Ther. 2017;26(6):362–71.
Acknowledgements
This study has been possible through the generous support from the Stig and Ragna Gorthon’s foundation for medical research.
Funding
This study has been possible through the generous support from the Stig and Ragna Gorthon’s foundation for medical research, not involved in the design of the study and collection, analysis, and interpretation of data and in writing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
P. Kjellin and H. Pärsson have nothing to disclose. Hans Lindgren has received compensation according to a proctoring and training agreement with ev3 Nordic AB and William Cook Europe ApS. These sponsors had no involvement in any part of the study. The study was conducted without sponsoring from any medical device company.
Consent for Publication
For this type of study consent for publication is not required.
Ethical Approval
The study was performed in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. The study was approved by the Swedish Ethical Review Authority 2019-00452.
Informed Consent
Informed consent was obtained from all patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kjellin, P., Pärsson, H. & Lindgren, H.I.V. Onyx Embolization for Occlusion of the Proximal Internal Iliac Artery During EVAR in Patients with Unsuitable Landing Zones in the Common Iliac Artery. Cardiovasc Intervent Radiol 42, 956–961 (2019). https://doi.org/10.1007/s00270-019-02188-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-019-02188-8