Abstract
Background
Mechanical thrombectomy (MT) is an efficient treatment of acute stroke caused by large-vessel occlusion. We evaluated the factors predicting poor clinical outcome (3-month modified Rankin Scale, mRS >2) although MT performed with modern stent retrievers.
Methods
We prospectively collected the clinical and imaging data of 105 consecutive anterior circulation stroke patients who underwent MT after multimodal CT imaging. Patients with occlusion of the internal carotid artery and/or middle cerebral artery up to the M2 segment were included. We recorded baseline clinical, procedural and imaging variables, technical outcome, 24-h imaging outcome and the clinical outcome. Differences between the groups were studied with appropriate statistical tests and binary logistic regression analysis.
Results
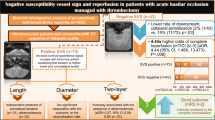
Low cerebral blood volume Alberta stroke program early CT score (CBV-ASPECTS) was associated with poor clinical outcome (median 7 vs. 9, p = 0.01). Lower collateral score (CS) significantly predicted poor outcome in regression modelling with CS = 0 increasing the odds of poor outcome 4.4-fold compared to CS = 3 (95% CI 1.27–15.5, p = 0.02). Lower CBV-ASPECTS significantly predicted poor clinical outcome among those with moderate or severe stroke (OR 0.82, 95% CI 0.68–1, p = 0.05) or poor collateral circulation (CS 0–1, OR 0.66, 95% CI 0.48–0.90, p = 0.009) but not among those with mild strokes or good collaterals.
Conclusions
CBV-ASPECTS estimating infarct core is a significant predictor of poor clinical outcome among anterior circulation stroke patients treated with MT, especially in the setting of poor collateral circulation and/or moderate or severe stroke.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Mechanical thrombectomy (MT) is an efficient treatment of acute stroke caused by large-vessel occlusion in patients presenting with favourable results in imaging evaluation [1–7]. Good clinical outcome, as signified by 3-month modified Rankin score (mRS) ≤2, has been reported in roughly half of patients treated with MT despite high rates of successful reperfusion achieved with newer generation stent retrievers [3–7]. Thus, identification of patients with poor prognosis despite reperfusion is of central importance in improving the effectiveness of MT.
Fast and effective recanalization of the occluded vessel with restoration of normal antegrade circulation has a crucial effect on the clinical outcome of acute stroke. However, it is not the only important factor [8, 9]. Multiple studies have mapped both clinical and imaging variables that predict favourable clinical outcome while those that directly address predictors of poor outcome in different settings are far fewer in number [9–13].
The objective of this investigation was to clarify which clinical and imaging variables predict poor clinical outcome (mRS >2) in patients with anterior circulation stroke who underwent MT.
Methods
Participants and Variables
The study was approved by the institutional review board. We prospectively collected and analysed the clinical and imaging data of 130 consecutive patients presenting with stroke symptoms admitted between January 2013 and December 2014 to Tampere University Hospital. They underwent clinical and imaging evaluation and proceeded to digital subtraction angiography (DSA) with an intention to perform MT. The inclusion criteria for this study were occlusion of the internal carotid artery (ICA) and/or middle cerebral artery (MCA) up to the M2 segment, and MT with stent retriever. 105 Patients met these criteria and 25 patients were excluded: eight patients had posterior circulation stroke; one patient had an occlusion of the A3 segment of the anterior cerebral artery and another of the M3 segment. In 15 cases thrombectomy with a stent retriever device was not performed because the clot had dissolved, there was no access to the thrombus or only aspiration thrombectomy was done. The baseline clinical characteristics included age, sex, clinical risk factors for ischemic stroke (hypertension, diabetes, coronary heart disease, atrial fibrillation) and time from symptom onset to imaging and to initiation of IVT. These data were collected from the patient records. National Institutes of Health Stroke Scale (NIHSS) score at the presentation, time from symptom onset to imaging and to recanalization of the occluded vessel, the duration of the procedure, TICI (Thrombolysis in Cerebral Ischemia) grading evaluated with DSA at the end of the procedure, and procedural complications had been prospectively stored. A follow-up NCCT was performed 24 h after MT. Haemorrhagic complications and post-infarct oedema were classified according to SITS-MOST criteria [14]. The clinical outcome measure was the modified Rankin Scale (mRS) and evaluated three months after the stroke based on a follow-up visit to neurologist or a phone interview by neurologist. One patient could not be reached for this control.
Imaging Protocol, Clinical Decision Making and Image Analysis
The initial imaging evaluation consisted of non-contrast-enhanced computed tomography (NCCT), CT angiography (CTA) and CT perfusion (CTP). The selection of patients as candidates for MT was based on the absence of extensive irreversible ischemic changes (frank hypodensity more than 1/3 of the MCA territory) and haemorrhage in NCCT, and evaluation of the amount of salvageable tissue in CTP imaging and proximal clot position in CTA. The decision to proceed to MT was multidisciplinary (stroke neurologist and neurointerventional radiologist). Patients referred to our institution from other hospitals were re-evaluated with at least NCCT and CTA upon arrival before proceeding to the angiographic suite to rule out bleeding and extensive irreversible ischemic lesion. In the case of wake-up strokes, CTP was performed if no large infarct was seen in NCCT. NCCT, CTA and CTP examinations were reviewed using dedicated medical imaging workstations. Parametric Perfusion maps—mean transit time (MTT), cerebral blood flow (CBF) and cerebral blood volume (CBV)—were generated with the CT Perfusion 4 software that uses a delay insensitive deconvolution-based algorithm (GE Healthcare). CTA images were reviewed by examining both the raw data and maximum intensity projection images. The Alberta stroke program early CT score (ASPECTS) was assessed from admission and follow-up 24-h NCCT images, and from MTT and CBV maps as described in our previous article [15]. CTA was used to evaluate the occlusion site, the clot burden score (CBS) and the collateral score (CS) as described in our previous report [16] and Table 1. The location of the clot was recorded based on the most proximal position of the occlusion. The examinations were reviewed in the order NCCT, CTA and finally CTP, paralleling that of the clinical work flow. Two radiologists assigned ASPECTS, CBS and CS. In cases the scoring or the assignment differed, a consensus opinion was agreed on. The reviewers were blinded to the clinical data apart from the side and nature of the acute symptoms. One radiologist measured the final infarct volumes on the 24-h NCCT. The boundaries of the affected areas were determined visually. Volume was calculated by multiplying the measured area with the slice thickness. Validation of the measurements including intraclass correlation coefficients (ICC) and Cohen’s kappa values can be found in the above-mentioned previous publications.
Recanalization Therapies
MT was performed with different stent retrievers and sometimes with multiple devices based on the judgment of the operator. We used a bi-axial system consisting of an 8F or 9F guiding catheter with a tip balloon and coaxially a 0.021″ micro-catheter or a tri-axial system consisting of an 8F guiding catheter, a distal access catheter trough which a micro-catheter was inserted with the aid of a 0.014″ micro-guidewire. The micro-catheter was navigated through the occluded segment of the artery, and a suitable stent retriever device was positioned trough the micro-catheter to the site of the thrombus and deployed. The stent was left in place for 4 min and then retrieved, and at the same time, the guiding catheter or the intermediate catheter was aspirated forcefully. The same procedure was repeated until satisfactory circulation was restored. Different stent retriever devices were used based on the preference and judgment of the operator with size of the vessel and tortuosity of the vasculature as main selection criteria. The TREVO® device (Stryker Neurovascular/Concentric Medical, Mountain View, CA, USA) was used in 40% of cases, CAPTURE LP™ (eV3/ COVIDIEN/Medtronic, Santa Rosa, CA, USA) in 40%, ERIC® (MicroVention, Tustin, CA, USA) in 9%, Aperio® (Acandis, Pforzheim, Germany) and REVIVE® (Codman & Shurtleff, Raynham, MA, USA) in 1%, respectively, and in 10% of cases multiple device types were used. Intravenous thrombolysis (Actilyse® 0.9 mg/kg, Boehringer-Ingelheim, Ingelheim, Germany) was administered as bridging therapy to patients with no contraindications. The Actilyse® bolus was given on the CT table. If the delay from the symptom onset to groin puncture was expected to be minimal, i.e. in the case of an inpatient during office hours, IVT was not necessarily given. Patients coming from an outside hospital received IVT according to drip-and-ship protocol. Actilyse® drip was continued until groin puncture.
Imaging Parameters
Please see online supplementary material.
Statistics
The data were analysed with SPSS version 23 (SPSS Inc., Chicago, IL, USA). Group comparisons were performed by using the Student t test, the Chi-squared test, the Fisher exact test and the Mann–Whitney U test according to the type and distribution properties of the variable studied. Univariable and multivariable binary logistic regression analyses using poor clinical outcome as dependent variable were performed and odds ratio (OR) with 95% confidence interval (CI) were calculated for each covariate. Patients with collateral score from 2 to 4 were regarded as having good collateral vessel filling. Patients who had 3-month mRS >2 were considered to have experienced poor clinical outcome. A TICI score >2a was considered as a good recanalization result. A p value <0.05 was considered statistically significant.
Results
Baseline Characteristics
The inclusion criteria were met by 105 patients with 37 patients (35%) presenting with an occlusion of the ICA, 46 patients (44%) had an M1 segment occlusion, and 22 patients (21%) had an M2 segment occlusion. The main baseline and admission imaging characteristics are summarized in Table 2. Poor clinical outcome was seen in 47 of 105 patients (45%). Ninety-two patients (88%) had TICI >2a, which was considered the threshold of good technical result of MT. In this group, 38 patients (41%) experienced poor clinical outcome despite the successful recanalization. In two cases, NIHSS could not be scored reliably because the paramedic crew had sedated the patient during transportation. In eight cases, the time of the onset of the symptoms was unknown (i.e. they were wake-up strokes). CTP was successfully obtained from 72 patients (69%).
Predictors of Poor 3-Month Clinical Outcome
There were no significant differences between patients with poor and good clinical outcome in age, sex or other established stroke risk factors. Likewise, there were no statistically significant differences in the onset-to-imaging and recanalization times. The duration of the intervention was significantly longer in the mRS >2 group compared to the mRS ≤2 group (37 versus 23 min, p < 0.001, Table 3). The clot burden score (CBS) was similar in the two groups (Table 2). Patients with more severe strokes according to NIHSS at admission showed a trend towards worse 3-month clinical outcome (p = 0.08, Table 2). The administration of intravenous thrombolysis (IVT) was more common in the good outcome group even though the difference was not statistically significant (p = 0.08, Table 2). Fifteen (32%) patients in the poor outcome group succumbed to their illness.
The size of the infarct core as estimated from CBV parametric maps and quantified with ASPECTS was significantly larger in the poor outcome group (median CBV-ASPECTS 7 vs. 9, p = 0.01, Table 2). In univariable regression analysis, incrementing one ASPECTS point decreased the odds of poor outcome by a factor of 0.79 (95% CI 0.64–0.94, p = 0.01, Table 4). The result was similar when only patients with a favourable reperfusion result (TICI >2a) were considered (Table 4).
Extremely poor collateral circulation (CS = 0) was significantly associated with poor outcome with 73% of patients having no visible collateral circulation experiencing poor clinical outcome at three months (p = 0.03, Table 2). Correspondingly, in univariable regression analysis including all patients, CS significantly predicted poor clinical outcome and having CS = 0 increased the odds of poor outcome 4.4-fold (95% CI 1.27–15.5, p = 0.02, Table 4) compared to having optimal collateral filling (CS = 3). This association was even stronger if only those with successful reperfusion were considered (OR 6.5, 95% CI 1.6–26.4, p = 0.009, Table 4).
When patients with moderate or severe stroke were evaluated (NIHSS 8 or more), lower CBV-ASPECTS significantly predicted poor clinical outcome (OR 0.82, 95% CI 0.68–1, p = 0.05), whereas no significant difference was found among those with mild strokes. Similarly, when restricting the analysis to patients with poor collateral circulation (CS 0–1), incrementing one CBV-ASPECTS point significantly decreased the odds of poor prognosis (OR 0.66, 95% CI 0.48–0.90, p = 0.009), whereas no significant difference was found among those with good collaterals. Patients with reperfusion result TICI = 2a or worse showed a trend to poorer outcome (OR 3.14, 95% CI 0.9–11, p = 0.07, Table 4).
Finally, a binary logistic multivariable model using backwards likelihood method was devised with poor 3-month clinical outcome as the dependent variable and variables with p < 0.1 in the univariable analysis included as covariates. Lower CBV-ASPECTS (OR 0.77, 95% CI 0.63–0.95, p = 0.01) and not receiving IVT (OR 3.2, 95% CI 1.1–9.4, p = 0.04) emerged as the only statistically significant predictors of poor outcome in the final model.
Imaging Outcome
ASPECTS was markedly lower in the 24 h-follow-up NCCT of patients with a mRS >2 (7 vs. 9, p < 0.001, Table 3). Correspondingly, the total infarct volume was larger among those with poor outcome (64 vs. 11 ccm, p < 0.001, Table 3). Furthermore, the number of haemorrhagic complications and the extent of post-infarct oedema were significantly larger among these patients: the proportion of those with a haemorrhagic complication at 24 h 14 versus 6% (p = 0.01, Table 3), major space-occupying haemorrhage type PH2 or PHr2 5 versus 2% (p = 0.05) and post-infarct oedema grade COED 2 or 3 18 versus 2% (p < 0.001).
Discussion
Rapid and effective recanalization of the occluded vessel is a crucial predictor of good clinical outcome in the treatment of acute anterior circulation ischemic stroke [9, 12]. It is still unclear which patients with a large-vessel occlusion should be denied of MT because of poor prognosis regardless of the type of reperfusion therapy. A number of studies have focused on evaluating the factors predicting good outcome, whereas fewer studies have primarily addressed the factors related to poor clinical outcome at 3 months [11, 17–21]. The setup of the majority of these studies has been the evaluation of factors associated with poor clinical outcome despite successful recanalization. In contrast, we studied all consecutive patients presenting with anterior circulation stroke who underwent MT with a goal to understand which factors that are known at the time of the clinical decision making to perform MT predict poor outcome. However, a subgroup analysis including only patients with successful recanalization revealed that these factors are essentially the same as in the entire study population. This finding was somewhat expected because of the high recanalization rate (88%).
Higher NIHSS score at admission signifying more severe stroke, proximal site of occlusion and absence of IVT treatment are closely associated with a poor 3-month outcome among patients undergoing MT [17, 19, 20]. In our study, we saw similar trends but these findings were borderline statistically non-significant apart from the last. Interestingly, according to a meta-analysis of the five recent randomized studies that established MT as the treatment of choice in large-vessel occlusions, MT increased the odds of good clinical outcome regardless of IVT [2]. In our study also, the location of the occlusion was not a significant predictor of outcome which can in part be due to worse recanalization outcomes among those with an M2 occlusion compared to those with more proximal occlusions [22]. Moreover, patients with an M2 occlusion had more severe strokes (median NIHSS 14) than expected from the literature [23] and somewhat higher average age (69.8 vs. 64.8 and 65.3 years among patients with ICA and M1 occlusions, respectively). On the other hand, age was not significantly related to a poor outcome in our study. This may be because only a small number of patients in our study were 80 years of age or older, which has been demonstrated to be related to a poorer outcome. [17, 19]
There was no significant difference in NCCT-ASPECTS scores at admission between those with good and poor outcome. This needs to be interpreted in the context of relatively short-average onset-to-imaging times. However, where NCCT-ASPECTS lacks sensitivity, CBV-ASPECTS emerged as an important imaging parameter with lower scores predicting poor outcome (Table 2; Fig. 1). This is compatible with previous results regarding both IVT and MT [4, 21, 24–29]. As demonstrated in previous studies on IVT, a CBV-ASPECTS threshold of 7 or 8 best differentiates good and poor outcome [15, 30]. In our study, the median CBV-ASPECTS in the poor outcome group was 7.
A 82-year-old male with type 2 diabetes mellitus and chronic hypertension was brought to the emergency department because of right-sided hemiparesis. NCCT revealed minor ischemic changes (ASPECTS = 9, only one level shown, A). There was an occlusion of the left distal M1 segment in CTA (B). CBV-ASPECTS was scored 7 and MTT-ASPECTS 5 (D, E White arrows indicate the boundaries of the lesion). Revascularization was achieved with MT (TICI = 2b, C). In the 24-h control NCCT, ASPECTS was 7. The 3-month mRS was 3 (F)
The status of the collateral circulation as measured with collateral score has been shown to be an important predictor of clinical outcome [31–33]. In our study, having no visible collateral circulation at all (CS = 0) was specifically related to poor outcome.
CBV-ASPECTS did not significantly predict poor clinical outcome among patients with mild strokes (NIHSS <8) or good collateral circulation (CS 2–4), whereas low CBV-ASPECTS was significantly associated with poor outcome among those suffering from moderate or severe stroke and/or having poor collateral circulation. A mild stroke entails less extensive and severe ischemia which considering the mean onset-to-imaging time of less than 3-h translates into a small infarct core especially if an aggregating quantification method like ASPECTS is used. Similarly, good collateral circulation is related to smaller infarct core in this short timeframe. In a recent meta-analysis, MT did not significantly improve the clinical outcome of patients with NIHSS <10 compared to IVT [2]. These findings imply that perfusion imaging in the context of MT may be targeted to specific subgroups if not performed routinely to all patients presenting with stroke symptoms. This would also reduce the total radiation dose incurred in diagnostic imaging.
Our study has limitations. First, as the formation of the MT cohort was clinically driven and thus non-randomized, there can be selection biases. Further, due to relatively small number of patients, subgroup analyses may be underpowered to detect small differences between the subgroups.
Conclusions
Clinical variables and NCCT at admission are lacking in precision in the detection of patients with poor prognosis regardless of MT. A low CBV-ASPECTS score associated with large infarct core is a significant predictor of poor clinical outcome among these patients especially in the setting of poor collateral circulation and/or moderate or severe stroke. Thus, perfusion imaging should be considered in the evaluation of acute anterior circulation stroke patients who are candidates to undergo MT.
Abbreviations
- ASPECTS:
-
Alberta stroke program early CT score
- CBV:
-
Cerebral blood volume
- COED:
-
Cerebral oedema
- CS:
-
Collateral score
- ICA:
-
Internal carotid artery
- IVT:
-
Intravenous thrombolysis
- MCA:
-
Middle cerebral artery
- MT:
-
Mechanical thrombectomy
- MTT:
-
Mean transit time
- NIHSS:
-
National Institutes of Health Stroke Scale
- TICI:
-
Thrombolysis in cerebral infarction
References
Ding D. Endovascular mechanical thrombectomy for acute ischemic stroke: a new standard of care. J Stroke. 2015;17:123–6.
Goyal M, Menon BK, van Zwam WH, et al. Endovascular thrombectomy after large-vessel ischaemic stroke: a meta-analysis of individual patient data from five randomised trials. Lancet. 2016;387:1723–31.
Berkhemer OA, Fransen PS, Beumer D, et al. A randomized trial of intraarterial treatment for acute ischemic stroke. N Engl J Med. 2015;372:11–20.
Campbell BC, Mitchell PJ, Kleinig TJ, et al. Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med. 2015;372:1009–18.
Goyal M, Demchuk AM, Menon BK, et al. Randomized assessment of rapid endovascular treatment of ischemic stroke. N Engl J Med. 2015;372:1019–30.
Saver JL, Goyal M, Bonafe A, et al. Stent-retriever thrombectomy after intravenous t-PA vs. t-PA alone in stroke. N Engl J Med. 2015;372:2285–95.
Jovin TG, Chamorro A, Cobo E, et al. Thrombectomy within 8 hours after symptom onset in ischemic stroke. N Engl J Med. 2015;372:2296–306.
Zangerle A, Kiechl S, Spiegel M, et al. Recanalization after thrombolysis in stroke patients: predictors and prognostic implications. Neurology. 2007;68:39–44.
Rha JH, Saver JL. The impact of recanalization on ischemic stroke outcome: a meta-analysis. Stroke. 2007;38:967–73.
Nogueira RG, Liebeskind DS, Sung G, et al. Predictors of good clinical outcomes, mortality, and successful revascularization in patients with acute ischemic stroke undergoing thrombectomy: pooled analysis of the Mechanical Embolus Removal in Cerebral Ischemia (MERCI) and Multi MERCI Trials. Stroke. 2009;40:3777–83.
Soize S, Barbe C, Kadziolka K, et al. Predictive factors of outcome and hemorrhage after acute ischemic stroke treated by mechanical thrombectomy with a stent-retriever. Neuroradiology. 2013;55:977–87.
Fields JD, Lutsep HL, Smith WS, et al. Higher degrees of recanalization after mechanical thrombectomy for acute stroke are associated with improved outcome and decreased mortality: pooled analysis of the MERCI and Multi MERCI trials. AJNR Am J Neuroradiol. 2011;32:2170–4.
Zaidat OO, Castonguay AC, Gupta R, et al. North American Solitaire Stent Retriever Acute Stroke registry: post-marketing revascularization and clinical outcome results. J. Neurointerv Surg. 2014;6:584–8.
Toni D, Lorenzano S, Puca E, et al. The SITS-MOST registry. Neurol. Sci. 2006;27(Suppl 3):S260–2.
Sillanpaa N, Saarinen JT, Rusanen H, et al. CT perfusion ASPECTS in the evaluation of acute ischemic stroke: thrombolytic therapy perspective. Cerebrovasc Dis. Extra. 2011;1:6–16.
Saarinen JT, Rusanen H, Sillanpaa N. Collateral score complements clot location in predicting the outcome of intravenous thrombolysis. AJNR Am. J. Neuroradiol. 2014;35:1892–6.
Linfante I, Starosciak AK, Walker GR, et al. Predictors of poor outcome despite recanalization: a multiple regression analysis of the NASA registry. J. Neurointerv Surg. 2016;8:224–9.
Linfante I, Walker GR, Castonguay AC, et al. Predictors of mortality in acute ischemic stroke intervention: analysis of the North American Solitaire Acute Stroke Registry. Stroke. 2015;46:2305–8.
Shi ZS, Liebeskind DS, Xiang B, et al. Predictors of functional dependence despite successful revascularization in large-vessel occlusion strokes. Stroke. 2014;45:1977–84.
Sarraj A, Albright K, Barreto AD, et al. Optimizing prediction scores for poor outcome after intra-arterial therapy in anterior circulation acute ischemic stroke. Stroke. 2013;44:3324–30.
Espinosa de Rueda M, Parrilla G, Manzano-Fernandez S, et al. Combined multimodal computed tomography score correlates with futile recanalization after thrombectomy in patients with acute stroke. Stroke. 2015;46:2517–22.
Protto S, Sillanpaa N, Pienimaki JP, et al. Stent Retriever Thrombectomy in Different Thrombus Locations of Anterior Cerebral Circulation. Cardiovasc. Intervent. Radiol. 2016;39:988–93.
Saarinen JT, Sillanpaa N, Rusanen H, et al. The mid-M1 segment of the middle cerebral artery is a cutoff clot location for good outcome in intravenous thrombolysis. Eur. J. Neurol. 2012;19:1121–7.
van Seeters T, Biessels GJ, Kappelle LJ, et al. The prognostic value of CT angiography and CT perfusion in acute ischemic stroke. Cerebrovasc Dis. 2015;40:258–69.
Turk AS, Nyberg EM, Chaudry MI, et al. Utilization of CT perfusion patient selection for mechanical thrombectomy irrespective of time: a comparison of functional outcomes and complications. J Neurointerv Surg. 2013;5:518–22.
Tsogkas I, Knauth M, Schregel K, et al. Added value of CT perfusion compared to CT angiography in predicting clinical outcomes of stroke patients treated with mechanical thrombectomy. Eur. Radiol. 2016;26:4213–9.
Gasparotti R, Grassi M, Mardighian D, et al. Perfusion CT in patients with acute ischemic stroke treated with intra-arterial thrombolysis: predictive value of infarct core size on clinical outcome. AJNR Am J Neuroradiol. 2009;30:722–7.
Lum C, Ahmed ME, Patro S, et al. Computed tomographic angiography and cerebral blood volume can predict final infarct volume and outcome after recanalization. Stroke. 2014;45:2683–8.
Turk AS, Magarick JA, Frei D, et al. CT perfusion-guided patient selection for endovascular recanalization in acute ischemic stroke: a multicenter study. J Neurointerv Surg. 2013;5:523–7.
Aviv RI, Mandelcorn J, Chakraborty S, et al. Alberta Stroke Program Early CT Scoring of CT perfusion in early stroke visualization and assessment. AJNR Am J Neuroradiol. 2007;28:1975–80.
Pereira VM, Gralla J, Davalos A, et al. Prospective, multicenter, single-arm study of mechanical thrombectomy using Solitaire Flow Restoration in acute ischemic stroke. Stroke. 2013;44:2802–7.
Tan IY, Demchuk AM, Hopyan J, et al. CT angiography clot burden score and collateral score: correlation with clinical and radiologic outcomes in acute middle cerebral artery infarct. AJNR Am J Neuroradiol. 2009;30:525–31.
Beretta S, Cuccione E, Versace A, et al. Cerebral collateral flow defines topography and evolution of molecular penumbra in experimental ischemic stroke. Neurobiol Dis. 2015;74:305–13.
Souza LC, Yoo AJ, Chaudhry ZA, et al. Malignant CTA collateral profile is highly specific for large admission DWI infarct core and poor outcome in acute stroke. AJNR Am J Neuroradiol. 2012;33:1331–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest for all authors.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study, formal consent is not required.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Protto, S., Pienimäki, JP., Seppänen, J. et al. Low Cerebral Blood Volume Identifies Poor Outcome in Stent Retriever Thrombectomy. Cardiovasc Intervent Radiol 40, 502–509 (2017). https://doi.org/10.1007/s00270-016-1532-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-016-1532-x