Abstract
Background
Microdialysis is a technique for continuous measurement of extracellular substances. It may be used to monitor tissue viability. The clinical implications of using microdialysis as a tool in gastrointestinal surgery have yet to be defined. The aim of the present study was to evaluate the clinical significance of microdialysis with special attention to different markers measured to predict the clinical outcome of surgical patients.
Methods
Embase, MEDLINE, and the Cochrane Library were searched systematically for human studies written in English. Study selection, data extraction, and quality assessment were performed independently by two authors. We included studies in which the microdialysis technique was used for postoperative monitoring of patients undergoing gastrointestinal surgery. To be eligible, studies had to compare patients with and without postoperative complications.
Results
Twenty-six studies were included in this review. MINORS score ranged from 3 to 12 (median 10.5). Most studies showed that levels of biomarkers obtained by microdialysis correlated with the postoperative clinical course. Lactate, pyruvate, glucose, and glycerol were the most frequently measured biomarkers. Several studies found that changes in biomarkers in complicated patients preceded symptoms of complications and/or changes in conventional paraclinical methods of postoperative monitoring.
Conclusions
Studies show that microdialysis may have the potential to become a tool in postoperative surveillance of surgical patients. Larger randomized studies are needed to define the clinical implications of microdialysis.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Microdialysis is a well-established method to measure and survey metabolism and viability in a given tissue compartment. In brief, the microdialysis system consists of a double-lumen catheter, a pump for fluid infusion, and a vial for fluid collection (Fig. 1). The thin microdialysis catheter contains a semipermeable microdialysis membrane often located at the tip of the catheter and may be inserted into any organ of interest. Molecules diffuse passively from the interstitial fluid (ISF) across the microdialysis membrane and into the perfusion fluid such that the microdialysis catheter mimics a capillary. The returning fluid, the dialysate, is collected in the vial for subsequent analysis. Thus, the microdialysis technique provides a dynamic view of changes in the concentrations of specific substances of interest within the extracellular space. Microdialysis may be used for measurements of both endogenous and exogenous substances. Levels of endogenous substances measured within tissue reflect the condition of the tissue of interest. Microdialysis may therefore be used for monitoring of tissue viability, e.g., following surgery.
Equipment for bedside analysis of biomarkers (including lactate, pyruvate, glucose, and glycerol) is commercially available. A review of the methodological principles in the microdialysis technique has been published previously [1].
In surgical patients, timely intervention toward postoperative complications increases postoperative survival. Thus, it is desirable to evaluate new methods for postoperative monitoring of surgical patients. The microdialysis technique for postoperative surveillance of patients undergoing abdominal surgery was introduced more than 20 years ago [2, 3]. The objective of the present systematic review was to evaluate the clinical significance of the method with special attention to different markers measured to predict the clinical outcome of an uncomplicated versus a complicated postoperative course.
Method
This systematic review was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [4].
Study registration
The protocol of this systematic review was registered in the International Prospective Register of Systematic reviews (PROSPERO), registration number CRD42016051638.
Search strategy
We conducted a primary systematic literature search of studies in which the microdialysis technique was used for postoperative monitoring of patients undergoing surgery of the gastrointestinal tract. The PICO model [5] was used to define the clinical question addressed in this review. Population: patients undergoing surgery on the gastrointestinal tract including esophageal, ventricular, small bowel, large bowel, rectal, hepatic, or pancreatic surgery. Intervention: insertion of microdialysis catheters within the abdominal cavity or the mediastinum including insertion of catheters within the peritoneal cavity, esophagus, ventricle, small bowel, large bowel, rectum, liver, or pancreas. Comparison: uncomplicated versus complicated surgical patients (any postoperative complications). Outcome: any postoperative biomarker levels measured by microdialysis.
We searched the following databases: Embase, MEDLINE, and the Cochrane Library. The literature search ended on September 20, 2016. We included human studies written in English. Animal studies were excluded. We did not apply restrictions with regard to date of publication. In MEDLINE, we also searched for unpublished studies. An updated literature search was conducted on October 9, 2018.
In MEDLINE, the following Mesh terms and subheadings were used: microdialysis [MeSH], abdomen [MeSH], abdominal wall [MeSH], peritoneum [MeSH], peritoneal cavity [MeSH], intestines [MeSH], mediastinum [MeSH], gastroenterology [MeSH], gastrointestinal tract [MeSH], esophagus [MeSH], liver [MeSH], pancreas [MeSH], stomach [MeSH], colon [MeSH], rectum [MeSH], omentum [MeSH], jejunum [MeSH], duodenum [MeSH], ileum [MeSH], biliary tract [MeSH], gallbladder [MeSH], bile ducts [MeSH], surgery [Subh], and digestive system surgical procedures [MeSH]. In MEDLINE, the following free text words were used: microdialysis, micro-dialysis, microdialyses, micro-dialyses, abdomen, abdominal, peritoneum, peritoneal, intraabdominal, intra-abdominal, intraperitoneal, intra-peritoneal, intestine, intestinal, gut, bowel, mediastinum, mediastinal, intramediastinal, intra-mediastinal, esophagus, oesophagus, esophageal, oesophageal, stomach, liver, hepatic, hepar, pancreas, pancreatic, colon, colorectal, rectum, rectal, duodenum, duodenal, jejunum, jejunal, ileum, omentum, omental, gastroenterol, gastric, gastrointestin, hepatol, hepatobiliary, bile duct, biliary, gallbladder, gall bladder, surgery, surgical, operative, postoperative, and post-operative.
The full search strategy is available online at http://www.crd.york.ac.uk/prospero/.
Study selection
Two investigators independently (JES and MBE) screened and excluded studies in two phases. During the first phase, every study retrieved was screened on the basis of title and abstract. During the second phase, the remaining studies (studies that could not be excluded based on title and abstract) were evaluated on the basis of full-text assessment. Disagreements over study selection were resolved by consensus.
Data extraction
Two investigators (JES and MBE) independently extracted data from the included studies. We extracted the following information from each study included in this review: publication year, surgical intervention used on the study population, molecular weight cutoff value (MWCO) of microdialysis catheters used in the study, anatomical location of microdialysis catheters, maximum duration of postoperative microdialysis, and microdialysis results including comparison of complicated and uncomplicated patients.
Quality assessment
The methodological index for non-randomized studies (MINORS) [6] was used to assess the quality and risk of bias of the included studies. This scoring system includes eight items for non-randomized studies and four additional items for comparative studies. Each item is scored between 0 and 2, and the maximum attainable score is 16 and 24 for non-randomized studies and comparative studies, respectively. Two investigators scored each study independently. Detailed scoring of each included study is available at https://www.crd.york.ac.uk/prospero/.
Results
Study selection
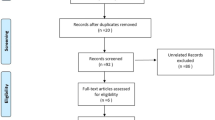
A primary search of the three databases resulted in 276 potentially eligible studies (Fig. 2). Ninety-five studies were duplicates, and 138 studies were excluded on the basis of the titles or abstracts. The full texts of 43 studies were screened, after which 11 studies were excluded due to wrong study design and 7 studies were excluded due to wrong outcomes. Twenty-five studies were included in the present review following the primary literature search. One study [7] was included following an updated literature search. In total, 26 studies were included in the present review.
Study characteristics
Characteristics of the included studies are presented in Table 1. All studies were prospective cohort studies. The included studies comprised 12 studies on upper gastrointestinal tract surgery including liver and pancreatic surgery [8,9,10,11,12,13,14,15,16,17,18,19], 5 studies on bowel surgery [21,22,23,24,25], 3 studies on pediatric surgery [26,27,28], 3 studies on acute surgery and/or admission to the intensive care unit (ICU) [7, 29, 30], and 3 studies on a mixed study population [31,32,33]. The number of patients included in the studies ranged from 7 to 91. The duration of microdialysis varied between 45 h and 28 days.
Risk of bias within studies
All studies included in this systematic review were non-randomized. The MINORS score ranged from 3 to 12 (median 10.5). All studies received the highest score on the item Prospective collection of data. No study performed an unbiased assessment of the study endpoint or prospective calculation of the study size.
Risk of bias across studies
In eight of the included studies, there was a discrepancy between outcomes listed in the method section and the result section and/or an unclear definition of outcomes in the study [13, 15, 20, 25, 27, 30,31,32].
Results of individual studies
Upper gastrointestinal surgery
Pharyngeal and esophageal resection
In a study by Sorensen [8], microdialysis catheters were placed within the mesentery of the free jejunal flap used for reconstruction after pharyngeal or proximal esophageal resection for cancer. The aim of the study was to investigate whether the results from microdialysis could detect graft ischemia. Microdialysis results were implemented in the decision of whether to reoperate on suspicion of ischemia. Fourteen patients were included in the study. Graft ischemia was suspected in two patients and confirmed at reoperation. The glucose concentration and lactate/glucose (L/G) ratio in the microdialysate predicted ischemia in both patients. Lactate concentration was only correlated with ischemia in one patient. The concentration of the analytes in the remaining 12 patients did not indicate ischemia, and none of these patients experienced graft failure.
Mediastinal microdialysis was performed in two studies on patients undergoing esophageal resection due to malignancy [9, 10]. The first study included seven patients, one of which developed anastomotic leakage. The mediastinal lactate/pyruvate (L/P) ratio and glucose level measured were correlated with the development of the anastomotic leakage, as the L/P ratio increased, and glucose decreased prior to diagnosis. The second study included 60 patients. Seven patients developed anastomotic leakage, and one patient developed an esophagobronchial fistula. No single biomarker (lactate, pyruvate, glycerol, or glucose) was indicative of postoperative anastomotic complications. When values of the L/P ratio, L/G ratio, lactate, pyruvate, and glucose were combined in a logistic regression model, sensitivity and specificity were 100% (confidence intervals (CIs) 44–100% and 91–100%, respectively) for the detection of early anastomotic leakage defined as before day 7 postoperative. Sensitivity and specificity were 86% (95% CI 42–99%) and 96% (95% CI 84–99%), respectively, for detection of any anastomotic complication. In one case, placement of the microdialysis catheter caused a lesion in an intercostal artery with major bleeding. No other complications were related to microdialysis.
Whipple’s pancreaticoduodenectomy
Ansorge et al. [11] examined whether the development of pancreatic fistula (PF) following Whipple’s pancreaticoduodenectomy could be predicted using microdialysis. A total of 48 patients were included in the study, and the microdialysis catheter was placed intraperitoneally near the pancreaticojejunal anastomosis. Biomarkers studied included lactate, pyruvate, glycerol, glucose, and trypsinogen activation peptide (TAP). TAP was measured on postoperative days (PODs) 1 and 2 and the remaining biomarkers on POD 1–5. Seven patients developed clinically significant PF, eight patients developed other intraabdominal postoperative complications, and 33 patients had an uncomplicated postoperative course. The concentration of glycerol and the L/P ratio was found to be significantly higher in patients who developed PF compared with the other two groups of patients. The concentration of TAP was higher in the PF group compared with the other two groups. It was concluded that changes in biomarker concentrations obtained by microdialysis could potentially predict the development of postoperative PF. The clinical consequence was not evaluated.
Liver transplantation
In studies where microdialysis is used for postoperative surveillance of patients receiving hepatic surgery, the primary focus has been patients undergoing liver transplantation [12,13,14, 16, 34]. Intrahepatic insertion of microdialysis catheters has been the preferred method for placement of the probe and has proven to be associated with a low risk of bleeding [12]. In addition to the traditional biomarkers (glucose, lactate, pyruvate, and glycerol), various other biomarkers have been measured. These include interleukin (IL)-6, IL-8, IL-10, γ-aminobutyric acid (GABA), interleukin-1 receptor antagonist (IL-1ra), C-X-C motif chemokine 8 (CXCL-8), CXCL-10 (or inducible protein ((IP)-10)), macrophage inflammatory protein 1β(MIP1β), monocyte chemoattractant protein (MCP)-1, complement activation C5a (C5a), alanine, arginine, citrulline, γ-aminobutyric acid, glutamate, glutamine, glycine, and taurine [13, 15, 34].
Impaired hepatic arterial blood flow following liver transplantation has been correlated with increases in intrahepatic levels of lactate, the L/P ratio, C5a, CXCL-8, and IL-6, whereas levels of intrahepatic lactate, pyruvate, C5a, IL-8, and CXCL-10 have been found to increase prior to liver rejection [13,14,15]. Furthermore, microdialysis studies have shown that changes in intrahepatic biomarkers, including lactate, IL-8, C5a, and CXCL-10, may precede changes in biomarker levels in peripheral blood [including lactate, bilirubin, and alanine aminotransferase (ALT)] in patients who experienced postoperative complications [12, 13, 15].
Haugaa et al. [14] compared 9 patients who developed liver ischemia (detected by Doppler ultrasound and/or computed tomography) and 12 patients who developed liver rejection (proven by biopsy) with 39 uneventful cases. In a contingency table model including lactate >3 mM/ml and L/P ratio >20, ischemia was detected with a sensitivity of 100% and a specificity of 72% or greater (range 72%–100%). Specificity varied according to the location of ischemia (right lobe, left lobe, both lobes, or split transplant) and the frequency of consecutive measurements. For liver rejection, the sensitivity was 89% or greater (range 89%–100%), while specificity ranged from 10 to 90% at cutoff values for lactate, pyruvate, and L/P ratio of >2 mM, >170 µM, and <20, respectively. Interestingly, the microdialysis results indicated rejection prior to traditional blood markers (lactate, ALT, and bilirubin). As for the detection of ischemia, the sensitivity and specificity depended on the anatomic placement of the catheter within the liver and the frequency of consecutive microdialysis measurements. Later, Haugaa et al. [15] studied intrahepatic levels of inflammatory biomarkers in 17 uneventful cases, 12 cases of rejection (proven by biopsy), and 4 cases of liver ischemia (proven by ultrasound, computed tomography, or surgical exploration). Increasing levels of CXCL-10 and C5a predicted graft rejection and graft ischemia, respectively. CXCL-10 predicted rejection with an area under the receiver operating characteristic (ROC) curve of 0.81 and differentiated patients with liver rejection from those with liver ischemia with an area under the ROC curve of 1.00. CXCL-10 tended to increase prior to conventional biomarkers (ALT and bilirubin) in patients experiencing liver rejection. C5a predicted ischemia with an area under the curve (AUC) of 0.96 and distinguished patients with liver ischemia from those with liver rejection with an AUC of 0.88.
In a series of three studies [16,17,18] on the same study population comprising 15 patients undergoing liver transplantation, intrahepatic microdialysis was performed during organ harvesting, preparation, and 48 h following implantation. Patients experiencing ischemia/reperfusion injuries (IRI) (defined as postoperative AST > 2000 IU) (complicated group) (n = 6) were compared with those without IRI (uncomplicated group). A significantly higher concentration of aspartate was registered before harvesting in donor livers that were transplanted into the group of patients with complications. The group with complications also showed significantly higher lactate concentrations during the preparation procedure. β-Alanine, GABA, glutamine, and threonine were all found to be significantly higher in liver transplant patients with complications during the back-table procedure. In the postoperative course, lactate decreased at a significantly slower rate in the group with complications than in the complication-free group. However, there was a discrepancy in the published results, as one of the studies [18] claimed that no difference was registered between patients with and without complications regarding amino acid levels, including those of GABA and glutamine.
Perera et al. [19] studied 30 patients undergoing liver transplantation. The microdialysate was sampled during preparation, during implantation, and 48 h postoperatively. A secondary aim of the study was to investigate differences in levels of intrahepatic biomarkers between patients with and without complications. The study revealed that graft failure (n = 4) was associated with higher L/P ratios during cold storage of the graft. The differences were not tested for statistical significance.
Bowel surgery
Several studies have investigated the applicability of microdialysis in postoperative monitoring of patients undergoing colorectal resection [20,21,22,23,24,25]. In a study by Jansson et al. [21], the safety of peritoneal microdialysis in eight patients who had undergone right-sided hemicolectomy with primary anastomosis for colonic neoplasia was investigated. No procedure-related adverse events were observed. In another study by Jansson et al. [22], the importance of catheter placement was investigated in 12 patients undergoing right-sided hemicolectomy. A total of three catheters were placed intraperitoneally, one near the anastomosis, one free floating within the intestinal loops, and one within the omentum. A reference catheter was placed subcutaneously in the right pectoral region. The median L/P ratio varied according to catheter location, with the highest values being recorded adjacent to the anastomosis, and it was concluded that catheters should be near the anastomosis. Four patients had repeatedly high L/P ratios (defined as a ratio >20) measured adjacent to the anastomosis and/or within the small intestinal loops. Two patients experienced postoperative anastomotic leakage (AL).
The use of microdialysis to detect postoperative AL has been the primary focus of several studies of patients undergoing colorectal resection [23,24,25]. In a study including 23 patients undergoing low anterior rectal resection, 7 patients experienced AL [23]. Two microdialysis catheters were placed in the abdominal cavity, one in close proximity to the anastomosis and one in the center of the abdominal cavity. Data from catheters placed next to the anastomosis showed no significant difference between the two groups on POD 1–4. On POD 5–6, the L/P ratio increased in the leakage group and was significantly higher than that in the complication-free group. The L/P ratio measured in the catheters placed in the center of the abdomen showed similar trends, although they were not significant. Another important finding was that the increase in L/P ratio occurred prior to the development of clinical symptoms.
Ellebæk et al. [24] studied 45 patients who underwent open low anterior resection due to rectosigmoid cancer. Four patients developed anastomotic leakage, and in all four patients, significant increases in lactate concentration and the L/P ratio were found together with a significant decrease in glucose concentration. In three of the four cases, a late anastomotic leakage occurred (>10 days postoperatively).
In another study [25] on 24 patients undergoing left-sided hemicolectomy, three patients developed anastomotic leakage. Intraperitoneal lactate was significantly higher in patients developing anastomotic leakage. There were no other significant findings.
Pediatric surgery
In a pilot study [26] in 12 neonates operated on for necrotizing enterocolitis (NEC), the intraperitoneal concentrations of lactate, pyruvate, glycerol, and glucose were all found to be significantly different in three of the four neonates with postoperative complications compared with patients who had an uncomplicated course.
Risby et al. [27] conducted a study of 13 neonates operated on for congenital abdominal wall defects (9 with gastroschisis and 4 with omphalocele). A microdialysis catheter was placed intraperitoneally after primary closure or placement of a silo. Intraperitoneal lactate was found to be significantly higher in infants with gastroschisis. No other statistically significant difference was found. Infants receiving secondary closure following silo treatment did not differ from the rest of the study population. Intraperitoneal lactate did not reflect the duration of parenteral nutrition or tube feeding. A noteworthy finding was that intraperitoneal lactate and glucose were not correlated with values of lactate and glucose in peripheral blood.
Haugaa et al. conducted a microdialysis study on pediatric patients undergoing liver transplantation [28], which was a continuation of another study by Haugaa et al. described above [14]. Regarding detection of ischemia by intrahepatic microdialysis, the cutoff values for lactate and the L/P ratio were >3 mM and >20, respectively. Regarding detection of rejection, cutoff values for lactate and the L/P ratio were >2 mM and <20, respectively. Sixteen patients receiving a total of 20 liver grafts were included in the study. Using 2–3 consecutive measurements, ischemia was detected with a sensitivity of 100% and a specificity of 86%. When measurements were interpreted over a period of >6 h, rejection was detected with a sensitivity of 88% and a specificity of 45%. Changes in microdialysis biomarkers preceded changes in blood markers in patients with graft rejection.
Acute surgery and intensive care
Verdant et al. [29] carried out a study including 25 patients admitted to the ICU after urgent laparotomy. A microdialysis catheter was placed intraperitoneally during surgery. Regarding the risk of complications (death, refractory shock related to the abdominal condition, mesenteric ischemia, need for reintervention, secondary peritonitis, intraabdominal collection, and anastomotic leakage or fistula) in the postoperative course, they found that an L/P ratio >22 within 24 h after surgery was associated with a positive predictive value of 64% and a negative predictive value of 79%. Glucose, glycerol, and lactate alone were not found to be significantly predictive of the clinical course.
Konstantinos et al. [30] included 21 patients admitted to the ICU with various abdominal pathological conditions. Each patient had a microdialysis catheter placed in the abdominal cavity. Nine patients died, and microdialysis results showed that survivors tended to have higher concentrations of intraperitoneal glucose and lower concentrations of intraperitoneal glycerol as well as lower intraperitoneal L/P ratios. Regarding the intraperitoneal L/P ratio and survival, the authors proposed a cutoff value of 25.94, above which the likelihood of survival decreases considerably.
In a study of patients treated for secondary peritonitis [7], 10 uncomplicated patients were compared to 5 complicated patients using intraperitoneal microdialysis. No statistical analysis was performed due to a low number of patients included in the study, but a trend indicated that complicated patients had lower levels of intraperitoneal glucose and higher levels of glycerol, L/P ratio, and L/G ratio.
Mixed populations
The first study to perform intraperitoneal microdialysis on human subjects was conducted by Jansson et al. [31]. The authors aimed to assess the safety of microdialysis and to investigate the relationship between the L/P ratio and postoperative recovery in patients undergoing scheduled and acute surgical procedures. A total of 91 patients were included in the study. Three patients experienced major lethal postoperative complications (irreversible ischemia in each case). The intraperitoneal L/P ratio increased prior to any clinical signs of complications or changes in blood parameters.
The relationship between the L/P ratio and the concentration of TNF-α and IL-10 in the peritoneal fluid was studied in 19 patients undergoing abdominal surgery for various reasons [32]. Microdialysis was used to sample lactate and pyruvate, whereas TNF-α and IL-10 were measured in the drain fluid. Sixteen patients experienced no complications. Three patients had a prolonged painful recovery without any other complications, and high L/P ratios were seen in all three patients, whereas TNF-α and IL-10 showed pronounced interindividual variation.
In a study by Horer et al. [33], 60 patients underwent abdominal surgery for various reasons. Intraperitoneal microdialysis catheters were placed for 48 h following surgery. Sixteen patients experienced postoperative complications. The postoperative intraperitoneal L/P ratio was found to be significantly higher among patients with complications than in complication-free patients. In addition, postoperative intraperitoneal glycerol concentration was found to be significantly higher among patients with uncomplicated clinical courses, which is surprising because glycerol is regarded as a biomarker of cell degradation.
Discussion
This systemic review included 25 studies. In general, microdialysis proved to be a safe procedure carrying a low risk of complications when performed on surgical patients. The majority of studies included in this review reported a correlation between biomarkers measured by microdialysis and the postoperative clinical course. In several studies, it was also found that changes in microdialysis biomarkers in complicated patients occurred prior to symptoms of complications and/or prior to changes detected by conventional paraclinical methods for postoperative monitoring (including peripheral blood markers).
Surgical conditions varied between the 25 included studies, making it difficult to compare these studies. However, several studies investigated study populations under the same surgical conditions. These conditions included liver transplantation and bowel resection. In microdialysis studies of patients undergoing liver transplantation, in which microdialysis catheters were placed intrahepatically, results indicated that the microdialysis technique has the potential to become a clinical tool in postoperative monitoring following liver transplantation. Relatively high sensitivity and specificity were obtained when measuring both conventional biomarkers (including lactate and pyruvate) and infrequently measured biomarkers (including IL-8 and CXCL-10). Additionally, studies showed that changes in various biomarkers preceded changes in traditional biomarkers in patients with complications.
In studies of patients receiving anastomosis following bowel resection, postoperative microdialysis appeared to differentiate between patients experiencing AL and complication-free patients. AL is a serious complication, and the rate varies according to the anatomic location of the anastomosis. AL following elective low anterior rectal resection and colonic resection has been reported at 13.68% and 7.5%, respectively, in large cohort studies [35, 36]. AL frequently occurs at a late stage following surgery [37]. A reliable method to detect AL at an early stage before the development of overt symptoms is attractive to minimize the serious complications that often follow AL. In microdialysis studies, it was reported that changes in intraperitoneal biomarker levels in some cases occurred prior to the development of clinical symptoms of anastomotic leakage [23, 24]. These findings may indicate the utility of microdialysis in the clinic.
The 25 studies included in this systematic review were in general of low scientific quality as indicated by their low MINORS scores. The studies were underpowered and non-randomized. In order to define the clinical implication of microdialysis in postoperative monitoring of surgical patients, future randomized studies with an appropriate sample size are needed. The majority of microdialysis studies included in the present review focused on conventional biomarkers (lactate, pyruvate, glucose, and glycerol). This is presumably due to commercially available equipment for bedside measurement of these substances. Some of the studies described in this review, however, investigated other biomarkers. Particularly, studies of patients undergoing liver transplantation have investigated less commonly measured biomarkers (including amino acids and cytokines). Promising results have been obtained in this context, including the correlation between levels of CXCL-10 and liver rejection as well as levels of C5a and liver ischemia [15]. We recommend that non-conventional biomarkers such as cytokines be investigated further in future studies.
Conclusion
In conclusion, microdialysis is a promising technique for postoperative monitoring of surgical patients. Larger and randomized studies are needed to define the clinical implications of microdialysis.
Change history
03 April 2019
In the original article, most of the reference numbers in the first column in Table 1 are off by one reference. Following is the corrected table.
References
Sabroe JE, Ellebaek MB, Qvist N (2016) Intraabdominal microdialysis—methodological challenges. Scand J Clin Lab Invest 76:671–677
Fellander G, Nordenstrom J, Tjader I et al (1994) Lipolysis during abdominal surgery. J Clin Endocrinol Metab 78:150–155
Fellander G, Nordenstrom J, Ungerstedt U et al (1994) Influence of operation on glucose metabolism and lipolysis in human adipose tissue: a microdialysis study. Eur J Surg 160:87–95
Moher D, Liberati A, Tetzlaff J et al (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA Statement. Open Med 3:e123–e130
Richardson WS, Wilson MC, Nishikawa J et al (1995) The well-built clinical question: a key to evidence-based decisions. ACP J Club 123:A12–A13
Slim K, Nini E, Forestier D et al (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73:712–716
Sabroe JE, Axelsen AR, Ellebaek MB et al (2017) Intraperitoneal lactate/pyruvate ratio and the level of glucose and glycerol concentration differ between patients surgically treated for upper and lower perforations of the gastrointestinal tract: a pilot study. BMC Res Notes 10:302
Sorensen HB (2008) Free jejunal flaps can be monitored by use of microdialysis. J Reconstr Microsurg 24:443–448
Pedersen ME, Mortensen MB, Qvist N et al (2009) Mediastinal microdialysis: early diagnosis of anastomotic leakage after resection for esophageal cancer. Esophagus 6:63–66
Ellebaek M, Qvist N, Fristrup C et al (2014) Mediastinal microdialysis in the diagnosis of early anastomotic leakage after resection for cancer of the esophagus and gastroesophageal junction. Am J Surg 208:397–405
Ansorge C, Regner S, Segersvard R et al (2012) Early intraperitoneal metabolic changes and protease activation as indicators of pancreatic fistula after pancreaticoduodenectomy. Br J Surg 99:104–111
Nowak G, Ungerstedt J, Wernerman J et al (2002) Clinical experience in continuous graft monitoring with microdialysis early after liver transplantation. Br J Surg 89:1169–1175
Waelgaard L, Thorgersen EB, Line PD et al (2008) Microdialysis monitoring of liver grafts by metabolic parameters, cytokine production, and complement activation. Transplantation 86:1096–1103
Haugaa H, Thorgersen EB, Pharo A et al (2012) Early bedside detection of ischemia and rejection in liver transplants by microdialysis. Liver Transpl 18:839–849
Haugaa H, Thorgersen EB, Pharo A et al (2012) Inflammatory markers sampled by microdialysis catheters distinguish rejection from ischemia in liver grafts. Liver Transpl 18:1421–1429
Silva MA, Murphy N, Richards DA et al (2006) Interstitial lactic acidosis in the graft during organ harvest, cold storage, and reperfusion of human liver allografts predicts subsequent ischemia reperfusion injury. Transplantation 82:227–233
Richards DA, Silva MA, Murphy N et al (2007) Extracellular amino acid levels in the human liver during transplantation: a microdialysis study from donor to recipient. Amino Acids 33:429–437
Silva MA, Mirza DF, Buckels JAC et al (2006) Arginine and urea metabolism in the liver graft: a study using microdialysis in human orthotopic liver transplantation. Transplantation 82:1304–1311
Perera MTPR, Richards DA, Silva MA et al (2014) Comparison of energy metabolism in liver grafts from donors after circulatory death and donors after brain death during cold storage and reperfusion. Br J Surg 101:775–783
Jansson M, Strand I, Jansson K (2006) Intraperitoneal microdialysis: postoperative monitoring of splanchnic ischemia by measurements of the lactate pyruvate ratio. Crit Care Med 34:2695–2697
Jansson K, Ungerstedt J, Jonsson T et al (2003) Human intraperitoneal microdialysis: increased lactate/pyruvate ratio suggests early visceral ischaemia. A pilot study. Scand J Gastroenterol 38:1007–1011
Jansson K, Strand I, Redler B et al (2004) Results of intraperitoneal microdialysis depend on the location of the catheter. Scand J Clin Lab Invest 64:63–70
Matthiessen P, Strand I, Jansson K et al (2007) Is early detection of anastomotic leakage possible by intraperitoneal microdialysis and intraperitoneal cytokines after anterior resection of the rectum for cancer? Dis Colon Rectum 50:1918–1927
Ellebaek Pedersen M, Qvist N, Bisgaard C et al (2009) Peritoneal microdialysis. Early diagnosis of anastomotic leakage after low anterior resection for rectosigmoid cancer. Scand J Surg 98:148–154
Daams F, Wu Z, Cakir H et al (2014) Identification of anastomotic leakage after colorectal surgery using microdialysis of the peritoneal cavity. Tech Coloproctol 18:65–71
Pedersen ME, Dahl M, Qvist N (2011) Intraperitoneal microdialysis in the postoperative surveillance after surgery for necrotizing enterocolitis: a preliminary report. J Pediatr Surg 46:352–356
Risby K, Ellebaek MB, Jakobsen MS, et al (2015) Intraperitoneal microdialysis in the postoperative surveillance of infants undergoing surgery for congenital abdominal wall defect: a pilot study. J Pediatr Surg 50:1676–1680
Haugaa H, Almaas R, Thorgersen EB et al (2013) Clinical experience with microdialysis catheters in pediatric liver transplants. Liver Transpl 19:305–314
Verdant CL, Chierego M, De Moor V et al (2006) Prediction of postoperative complications after urgent laparotomy by intraperitoneal microdialysis: a pilot study. Ann Surg 244:994–1002
Konstantinos T, Apostolos K, Georgios P et al (2014) Intraperitoneal microdialysis as a monitoring method in the intensive care unit. Int Surg 99:729–733
Jansson K, Jonsson T, Norgren L (2003) Intraperitoneal microdialysis: a new method to monitor patients after abdominal surgery. Int J Intensive Care 10:8–13
Jansson K, Redler B, Truedsson L et al (2004) Postoperative on-line monitoring with intraperitoneal microdialysis is a sensitive clinical method for measuring increased anaerobic metabolism that correlates to the cytokine response. Scand J Gastroenterol 39:434–439
Horer TM, Norgren L, Jansson K (2011) Intraperitoneal glycerol levels and lactate/pyruvate ratio: early markers of postoperative complications. Scand J Gastroenterol 46:913–919
Silva MA, Richards DA, Bramhall SR et al (2005) A study of the metabolites of ischemia-reperfusion injury and selected amino acids in the liver using microdialysis during transplantation. Transplantation 79:828–835
Kang CY, Halabi WJ, Chaudhry OO et al (2013) Risk factors for anastomotic leakage after anterior resection for rectal cancer. JAMA Surg 148:65–71
Bakker IS, Grossmann I, Henneman D et al (2014) Risk factors for anastomotic leakage and leak-related mortality after colonic cancer surgery in a nationwide audit. Br J Surg 101:424–432; discussion 432
Morks AN, Ploeg RJ, Sijbrand Hofker H et al (2013) Late anastomotic leakage in colorectal surgery: a significant problem. Colorectal Dis 15:e271–e275
Acknowledgements
Thanks to Herdis Foverskov, Librarian, The Medical Research library, The University Library of Southern Denmark, Odense University Hospital, and Svendborg Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Sabroe, J.E., Qvist, N. & Ellebæk, M.B. Microdialysis in Postoperative Monitoring of Gastrointestinal Organ Viability: A Systematic Review. World J Surg 43, 944–954 (2019). https://doi.org/10.1007/s00268-018-4860-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-018-4860-y