Abstract
Background
Breast reduction with the free nipple-areolar graft (FNG) technique has disadvantages such as loss of nipple projection, loss of nipple sensation, and depigmentation of the nipple-areolar complex. In this study, patients in whom a purse-string (PS) suture was used in the center of the de-epithelialized area to prevent loss of nipple projection were compared with patients who underwent the conventional method.
Methods
A retrospective analysis of the patients who underwent breast reduction with the FNG was conducted in our department. Patients were divided into two groups according to the FNG placement. In the PS suture method group, a 1-cm-diameter circumferential suture was placed with a 5-0 Monocryl® (poliglecaprone 25) suture to gain a 6-mm-nipple projection. In the conventional method group, the FNG was placed directly over the de-epithelized area. Graft viability was evaluated after 3 weeks postoperatively. The final nipple projection and depigmentation were evaluated after 6 months postoperatively. The results were evaluated with statistical tests.
Results
The number of patients with the conventional method was 10, and the PS suture method was 12. There was no statistically significant difference between two groups regarding graft loss and depigmentation (p > 0.05). Nipple projection was significantly higher in the PS method group (p < 0.05).
Conclusion
We observed that PS circumferential suture made an acceptable nipple projection compared to the conventional method in breast reduction with the FNG technique. Since the method is easy to apply and has relatively low risk, it would contribute to clinical practice.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bilateral breast hypertrophy may occur in women at any period starting from adolescence. In addition to physical symptoms, it may lead to psychological problems from an esthetic perspective in patients [1]. Breast size can be variable in each patient. Breast reduction surgery reduces breast size and reshapes the breast, which helps to relieve these symptoms and problems [2].
Creating a projected breast and nipple-areolar complex (NAC) that looks cosmetically natural should be considered when reducing breast volume and weight during breast reduction surgeries. NAC does not harvest as a graft in pedicled breast reduction surgeries. It is easier to accomplish the desired projection during pedicled breast reduction surgeries. However, due to the risk of the pedicle and NAC necrosis, it is not possible to perform pedicled breast reduction techniques for all patients. Breast reduction techniques performed with the free nipple-areolar graft (FNG) are preferred in these situations [3].
Breast reduction with the FNG technique is more commonly performed in patients with gigantomastia, in elderly patients with systemic diseases, also in patients who have undergone previous breast surgery [4]. The FNG technique releases the NAC from its vascular pedicle’s dependence. This technique has disadvantages such as loss of FNG, depigmentation in the NAC, loss of nipple sensation, and loss of nipple projection. At the same time, there may be difficulties in creating a natural conical breast shape due to excessive resection. Techniques to increase the projection of the breast itself and to increase graft survival have been described in the literature [5,6,7,8]. There is still a need in the FNG technique for an efficient and straightforward method to prevent the loss of nipple projection.
In this study, purse-string (PS) suture was used at the center of the de-epithelialized area to prevent the loss of nipple projection during breast reduction with the FNG. The results of this method are compared with the results of the conventional method.
Materials and Methods
Between February 2019 and August 2022, a retrospective analysis of the patients who underwent breast reduction with the FNG was conducted in our department. The study was performed after approval by the Ethics Committee of Ankara City Hospital (E.Board-E1-23-3330). According to the type of placement of the FNG, patients were divided into two groups: the FNG placed by conventional method and the FNG placed after a PS suture. In all cases, breast reduction surgery was performed using the Wise pattern skin incisions with the FNG technique. All procedures were performed by the senior author (M.S.).
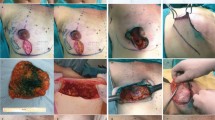
In preoperative planning, new nipple positions were planned between 21 and 24 cm from the presternal notch. At the beginning of surgery, NAC was harvested as a full-thickness skin graft in all patients after being marked with a 40-mm-diameter cookie cutter. All harvested skin grafts were defatted and trimmed. The grafts are kept in saline-soaked gauze for later use. The medial and lateral pillar flaps were left at an appropriate thickness to keep the breast projection. In the conventional method, the FNG was directly placed in its planned new location by paying attention to graft adaptation techniques. In the PS suture group, a hook was placed at the top point of the junction of the lateral and medial flaps in the de-epithelialized area before placing the FNG. A circumferential suture was placed with 5-0 Monocryl® (poliglecaprone 25) along a 1-cm-diameter circle, and dermal projection was ensured to be 6 mm (Fig. 1) (Supplementary File 1). Care was taken to ensure the circumferential suture did not affect dermal vascular supply. In order to ensure the dermal vascular supply of dermal tubercle, the dermal bleeding pattern was evaluated after the circumferential suture was placed. Then, the defatted and trimmed graft was placed on this elevated dermal area while the nipple was positioned to the center (Fig. 2). All placed grafts underwent tie-over dressing.
Standard photography was performed with the patients supine after 3 weeks postoperatively to evaluate graft viability. The percentage of graft loss areas was calculated using Image J software package (ver.13.0.6). After 6 months postoperatively, the presence of depigmentation of NAC was evaluated by standard photography, and nipple projections were measured with a paper ruler and results were documented.
Graft loss percentages and nipple projection values were analyzed statistically by taking the averages of right and left values. Mann–Whitney U Test was used to compare differences between the two groups. The presence of depigmentation was analyzed separately, and the Chi-square test was used to compare differences between the two groups (IBM SPSS ver.25).
Results
Between the specified dates, 22 patients underwent breast reduction surgery with the FNG in our department. The FNG was placed in its new location with the conventional method in ten patients, and the placing of the FNG was after using the PS suture in 12 patients. The mean age of the patients was 57 years (range between 45 and 62). Patients had no previous history of breast surgery.
Graft loss at NAC was measured after 3 weeks postoperatively, and Table 1 shows percentages. Graft loss in the conventional method averaged 4.5% per breast (minimum 0%, maximum 10%). On average, graft loss in the PS suture was 5.9% per breast (minimum 0%, maximum 18%). There was no statistically significant difference between the two groups regarding graft loss at NAC (p > 0.05).
NAC with graft loss were followed up with a non-adhesive dressing. These sites were left to secondary healing and healed without complications. There was no need for any secondary surgical interventions.
Nipple projection values after 6 months postoperatively are summarized in Table 2. In the conventional method, nipple projection per breast was 0.75 mm on average (minimum 0 mm, maximum 2 mm). In the PS suture, projection per breast was 2.38 mm on average (minimum 1 mm, maximum 4 mm). Comparing the two methods found that nipple projection was statistically significantly higher in the group with PS suture (p < 0.05).
Patients with depigmentation of the NAC are shown in Table 3. It was observed that the number of patients with pigment loss was higher in the PS suture group (Figs. 3a–f, 4a–f). There was no statistically significant difference between the two groups regarding the depigmentation of the NAC (p > 0.05).
Patient 5 purse-string method. a preoperative frontal view b preoperative left lateral view c preoperative right lateral view d postoperative frontal view at sixth month e depigmentation of the nipple-areolar complex postoperative left lateral view at sixth month f pigmentation of the nipple-areolar complex postoperative right lateral view at sixth month
Discussion
Breast reduction with the free nipple technique was first described by Thorek in 1922 [9]. The main disadvantages of the technique include loss of sensation and nipple projection, loss of pigment due to partial de-epithelialization, loss of lactation, and loss of nipple skin to varying degrees. Loss of nipple projection and pigmentation is a severe cosmetic deformity [10]. The healing of the FNG could also negatively affect the shape and texture of the new NAC. These problems can be solved by applying dermabrasion of the NAC described by Basaran et al. [11]. However, there were no such complaints from our patients.
Techniques such as e-flap, round block dermal suturing technique, and star flap applications on dermoglandular flap have been previously described to prevent projection loss [12, 13]. Creating a dog ear in the new nipple area while reshaping the breast is an option for the projection of the nipple. Casas et al. described this technique but did not perform any projection measurement; they focused primarily on breast projection [14].
Karabagli et al. described the e-flap technique in which the flap elevated on the superior aspect of the junction of the pillar flaps, measured the nipple projection as 0.9 cm after 6 months, and stated that nipple sensation was present. However, they did not perform any specific test for sensitivity. They reported pigment loss in the reconstructed nipple because the flaps were harvested from the pillar flaps’ skin. They observed that the nipple projection was 1.2 cm on average in the early postoperative period. The average was 0.9 cm after 6 months. It showed a 25% decrease [12]. The maximum nipple projection obtained in our study with PS suture was 4 mm after 6 months. However, this projection was less than the study of Karabagli et al. [12]. Our results were more cosmetically acceptable because it was obtained on a nipple graft.
In another study, Bektas et al. [13] performed nipple reconstruction with the star flap technique on the medial dermoglandular pedicle. They reported that the loss of nipple projection after 12 months postoperatively was 70%, higher than the literature rate of 40%. Our study observed that the projection of the PS suture after 6 months was well preserved. In our study, it was thought that the better preservation of the nipple projection was since there was no flap elevation.
Nipple reconstruction after breast reconstruction is a different case because there is no NAC to use. Bitik et al. [15] discarded the original NAC in the FNG and described the nipple-areola reconstructing (NAR) reduction mammaplasty technique to create a new NAC. Even if there is no measurement of nipple projection in their study, patients’ satisfaction rates were high. Various autologous and synthetic biomaterials also have been used to enhance nipple projection, especially for nipple reconstruction after breast reconstructions [16]. Fujisawa et al. [17] performed nipple reconstruction with dermal bridge flap and cartilage graft in patients who underwent breast reconstruction after mastectomy and achieved an average projection of 4.4 mm after an average follow-up of 25.7 months. As understood from this, the projections they obtained in their studies were higher than ours. Sisti et al. [18] compared the nipple-areolar complex reconstruction methods performed between 1946 and 2015. Their study stated that conchal cartilage, biological collagen, and rib cartilage were used as autologous biomaterials, and Artecoll (polymethyl methacrylate), AlloDerm (acellular dermal matrix), Calcium hydroxyapatite were used as biomaterials. Improving the nipple projection, some authors used hyaluronic acid filler following breast reconstruction and nipple retractor for inverted nipples [19, 20].
In our study, the circumferential suture’s tightness is crucial for maintaining dermal blood supply. Since this tightness will determine the projection of the nipple, it was applied to all patients by the same surgeon and with a standard 1-cm-diameter circular suture. The higher rate of pigment loss in PS sutures was thought to be caused by the fact that not all patients had the same dermal quality, despite using the standard suturing technique. Patients who experienced pigmentation loss after surgery had no complaints in this regard. At the same time, enlarging the diameter of the circle of circumferential suture may produce better results if the dermal blood supply is not impaired.
The patients expected to see a nipple image that could be distinguished from the areola following surgery when using the FNG technique. Although there were also projection losses in the PS suture method, a more prominent nipple was obtained compared to the conventional method. It was thought that the preservation of nipple projection was because of dermal suture-related changes. Longer-term studies in a larger patient population would be beneficial for the technique to be widely used. Since only FNGs applied to female patients were used in this study, no predictions can be made about the FNGs applied to male patients. Another limitation was that some patients were lost to follow-up after the 6 months postoperatively.
Conclusions
We observed that providing nipple projection with purse-string circumferential suture made a significant difference in projection in patients undergoing breast reduction surgery with the free nipple-areolar graft technique. Since the method is easy to apply and relatively low risk, it would contribute to clinical practice.
References
Lessard L, Papanastasiou C, Fortin M et al (2023) Breast hypertrophy: a real pain in the back. Plast Reconstr Surg 151:498–508
Crittenden TA, Watson DI, Ratcliffe J et al (2023) Long-term outcomes of breast reduction surgery: a prospective cohort study. J Plast Reconstr Aesthet Surg 79:58–67
Lo AY, Yu RP, Raghuram A et al (2020) Patient characteristics associated with free nipple graft reduction mammoplasty. Cureus 12:e9063
Colen SR (2001) Breast reduction with use of the free nipple graft technique. Aesthet Surg J 21:261–271
Firat C, Gurlek A, Erbatur S et al (2012) An autoprosthesis technique for better breast projection in free nipple graft reduction mammaplasty. Aesthet Plast Surg 36:1340–1346
Sterodimas A, Pineda EF, Meirelles V et al (2008) Maximizing nipple graft survival after performing free nipple-areolar complex reduction mammaplasty. J Plast Reconstr Aesthet Surg 61:971–972
Engel R, Greenberg Y, Siddiqui A (2022) Negative pressure wound therapy for improved nipple survival in large volume reduction mammaplasty. Aesthet Plast Surg 46:108–112
Abramson DL (1999) Increasing projection in patients undergoing free nipple graft reduction mammoplasty. Aesthet Plast Surg 23:282–284
Thorek M (1989) Possibilities in the reconstruction of the human form 1922. Aesthet Plast Surg 13:55–58
McGregor JC, Hafeez A (2006) Is there still a place for free nipple areolar grafting in breast reduction surgery? A review of cases over a three year period. J Plast Reconstr Aesthet Surg 59(3):213–218
Basaran K, Basat SO, Mercan ES et al (2015) The use of dermabrasion to achieve natural-looking areolas following breast reduction or mastopexy: a study of 23 patients. Aesthet Plast Surg 39:534–539
Karabagli Y, Kose AA, Mangir S et al (2012) e-Flap nipple reconstruction in amputation mammaplasty. Aesthet Plast Surg 36:1140–1143
Bektas G, Cinpolat A, Bicici P et al (2012) A new application to free-nipple-graft reduction mammaplasty for breast and nipple projection. Eplasty 12:339–341
Casas LA, Byun MY, Depoli PA (2001) Maximizing breast projection after free-nipple-graft reduction mammaplasty. Plast Reconstr Surg 107:955–960
Bitik O, Uzun H, Zins JE (2013) Nipple areola reconstructing reduction mammaplasty. Aesthet Surg J 33:1129–1137
Lee HJ, Ock JJ (2019) How to improve projection in nipple reconstruction: a modified method using acellular dermal matrix disk and fragments. Plast Reconstr Surg 143:698e–706e
Fujisawa D, Asato H, Suzuki Y et al (2018) Quadruped and dermal bridge flap for nipple reconstruction. Plast Reconstr Surg Glob Open 6:e1872
Sisti A, Grimaldi L, Tassinari J et al (2016) Nipple-areola complex reconstruction techniques: a literature review. Eur J Surg Oncol 42:441–465
Sue GR, Seither JG, Nguyen DH (2020) Use of hyaluronic acid filler for enhancement of nipple projection following breast reconstruction: an easy and effective technique. JPRAS Open 23:19–25
Yukun L, Ke G, Jiaming S (2016) Application of nipple retractor for correction of nipple inversion: a 10-year experience. Aesthet Plast Surg 40:707–715
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There is no conflict of interests to disclose.
Ethical Approval
The study was performed after approval by the Ethics Committee of Ankara City Hospital (E.Board-E1-23-3330).
Informed Consent
Informed consent was obtained from all patients in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MPG 1572 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sonmez, M., Saglam, M.E. Preserving the Nipple Projection in Breast Reduction with the Free Nipple-Areolar Graft Technique: Purse-String Suture. Aesth Plast Surg 47, 2255–2260 (2023). https://doi.org/10.1007/s00266-023-03429-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-023-03429-5