Abstract
Background
Since the beginning of the last century, when the aesthetic rejuvenating surgery was first described, there have been great changes in tactics and methods for solving the problems of age-related facial changes. Since the first description of the superficial muscular aponeurotic system (SMAS), there have been two main approaches to influencing this structure. These are various types of SMAS plications and different in-depth and technique sub-SMAS liftings. Each of these approaches has its advantages and disadvantages.
Methods
We have developed and applied a face-lift technique that combines the advantages of both approaches. We call it the triple-S lift, which is based on three basic principles:
-
1.
A short scar technique;
-
2.
The safety SMAS (limited sub-SMAS dissection to anterior border of the masseter muscle);
-
3.
The support system (a complex of ligatures in the sub-SMAS layer, which allows lifting and plication of the medial part of the SMAS simultaneously)
According to this method, there were 93 operations performed on 8 men and 85 women aged 38 to 72 years.
Results
The first clinical applications produced good results. The patients noted a high degree of satisfaction, and the level of complications was quite low. Since the technique has been performed for a short period of time, we demonstrate results of the 2-year period.
Conclusion
The described technique requires further study, but the first results suggest that this type of a surgical intervention is safe, easy to execute, and may be an option to choose for surgical correction of facial aging changes.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The demand for anti-aging procedures increases year after year. This is influenced not only by a change in trends, the promotion of a healthy lifestyle, the influence of the media, or a change in attitude toward plastic surgery, but also a competitive environment in business and social life. The fact that a younger-looking person has more opportunities and perspectives is undeniable.
More than a century of experience in the use of anti-aging face surgeries has not led surgeons to the choice of a single optimal and unified method of operation. A confirmation of this fact is the continuing search for new techniques and methods for optimizing results. On the one hand, we can see this with the emergence of new technologies and the introduction of more radical interventions on the soft face tissues, and on the other hand, the obvious return of surgeons to more conservative and safe techniques [1, 2].
At the same time, the conceptual view of the anatomical structures of the face, the description of the retaining ligaments of the face, sliding spaces, facial tissues, and skeleton aging have changed over the last period of time [3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19,20,21].
Today, the requirements for efficiency and stability of the result with faster recovery, as well as for a less traumatic impact on the tissue, are increased by using short scar technique.
Analyzing and taking into account these trends, we have conceptually developed and put into practice the SMAS SUPPORT SYSTEM LIFT (triple-S lift) technique of face-lifting.
Materials and Methods
The technique is based on the following principles:
-
1.
A short scar technique;
-
2.
Safety SMAS (limited sub-SMAS dissection up to anterior border of masseter muscle);
-
3.
The support system (a complex of ligatures in the sub-SMAS layer, which allows lifting and plication of the medial part of the SMAS simultaneously).
The operation has been performed on 93 patients of Slavic appearance from the end of 2016 to 2018. Among them were 85 women (91%) and 8 men (9%) with the age range from 38 to 72 years. The average age was 49 years.
The main goal of our research was to develop a minimally invasive effective face-lift surgery with the use of the short scar technique. Requirements for the method are to minimize the risks of damage to the nerves and salivary duct, reduce the number of complications, shorten the recovery period, and achieve long-lasting results.
Surgical Technique
Preoperative marking includes determining the type and length of incision. Depending on the preference of the patient, the pretragal or retrotragal approach is chosen. In the case of 1–2 types of ptosis (according to Baker DC), the incision goes from the earlobe to the temporal area, and then it makes the arch in the temporal region at the hairline or goes vertically to the scalp 1.5–2 cm above the helical rim [22]. In severe ptosis of cervical and jowl soft tissues, the incision line is also marked in the postauricular region, upwards to the posterior auricular muscle and 2–2.5 cm to the hairy part of the head (Fig. 1a). The following areas are marked: skin undermining zone (3.5–4 cm anteriorly from the ear), anterior edge of m. masseter, lateral margin of m. orbicularis oculi and malar eminence, and platysmal bands (Fig. 1b). The location of the lines of the ligature support system corresponding to the vector of lifting SMAS and soft tissues is also marked.
The operation is performed under general anesthesia with the use of Sevorane gas, which keeps hypotension at the level of 80–90/50–60 mmHg. for the optimal work of the surgeon. A limited use of muscle relaxant agents is recommended for better control of mimic muscle movements when the monopolar electrode reaches the motor nerve branches.
Aseptic preparation of the surgical area should be done with Octenisept solution or 0.5% chlorhexidine (CHX) aqua solution. This procedure begins with the infiltration of buffered local anesthesia utilizing both 1% lidocaine and epinephrine. After the skin incision, the subcutaneous tissue is tunneled with a 3-mm blunt liposuction cannula, and then the remaining vertical bands are transected with the scissors. This method of detachment is the safest and creates a smooth SMAS surface. The skin flap is separated medially on the cheek and neck for 3–5 cm. Creating a SMAS flap begins with a horizontal incision along the zygomatic arch with the Colorado electrode, 1 cm from the tragus, 3.5–4 cm long. Then, the incision is extended vertically up and stops at the edge of the orbicular oculi muscle. The preauricular vertical incision of the SMAS is performed 1 cm medial to the skin incision and is directed from the zygomatic arch down to the angle of the mandible. Then, the incision follows along the platysmal fibers 3 cm lower.
The corner of the SMAS flap is elevated with forceps, and the dissection proceeds anteriorly in the sub-SMAS layer with the monopolar coagulator while applying traction.
In the middle portion, the flap is mobilized to the anterior edge of the masseter and into the lower “sliding” space (according to Bryan Mendelson). The upper sliding space (prezygomatic) and McGregor’s ligaments are mobilized with a blunt tip cannula or closed scissors in the supraperiosteal layer. After the SMAS flap is completed, the support system is applied to provide the main lifting effect (Fig. 2).
The support system is placed in two planes: in the subcutaneous and sub-SMAS layers. It allows for performing medial SMAS plication and fixing the soft tissues to the anchor points on the temporal fascia, platysma-auricular ligament, and the fascia m. sternocleidomastoideus.
The support system is created with five hanging nonabsorbable braided sutures Ethibond 2-0 (Ethicon). The first suture goes through the mobile SMAS portion in the area of the malar fat and is sutured to the anterior edge of the temporal fascia.
The second, third, and fourth sutures are placed in three-ray direction.
These sutures are anchored in the area of the mobile SMAS portion 1.5–2 cm back to the nasolabial fold and then fixed to platysma-auricular ligament.
The fifth thread is anchored to the platysma 0.5–1 cm distal of the subcutaneous dissection, and then it is fixed to the fascia of m. sternocleidomastoideus.
The principle of passing the sutures
The thread penetrates the anchoring zone. Then, it goes through the sub-SMAS layer in the direction of the dissection end and comes out through the SMAS into the subcutaneous layer, and then it goes medially to the subcutaneous dissection end and again through the SMAS in the area of the transitional fold. After that, the thread goes back by the same route to the starting anchoring point. After knotting threads, the SMAS is elevated in the upper lateral direction with simultaneous plication of its medial part. The tension is transferred from the SMAS to the fixed anchor points [23]. The distal SMAS flap edge becomes tensionless. Then, the SMAS is divided into two flaps in the projection of the lower mandibular arch [13, 24]. The superior medial flap is replaced vertically upward and is fixed with interrupted stitches to the deep temporal fascia, covering the first–fourth sutures of the support system. The inferior lateral flap is moved to the retroauricular region in the form of a strap and fixed to the periosteum of the mastoid process without tension, covering the fifth suture (Fig. 3).
The described suture system significantly reduces the tension on the distal flap and improves the stability of the SMAS fixation. Lifting degree does not depend on the thickness and strength of the distal flap portion and even the quality of SMAS edge fixation when the support system is applied. Furthermore, SMAS tissue redistribution in the distal portion can be used for volumetric correction of the temporal and supra-zygomatic region.
The skin is redistributed without tension in the upper lateral direction. Excessive skin is removed in the retroauricular and temporal regions with lateral rotation of excessive tissues and minimal tension outwards from the auricle.
The use of arcuate incisions reduces the dog-ear formation in the distal section of the incision and shortens the incision by almost two times compared to the classical approach, which uses linear incisions located along the hairline in the occipital region that are visible as a kind of sign (surgery’s signs) of the operation, especially when assembling a ponytail hair. When using rotary flaps in the future, there remains a short and inconspicuous scar in the hair that does not require special masking [25].
After the operation, active 2–3 mm drainages are inserted which are removed on the second–fourth day. An aseptic compressive bandage is used for 7–10 days. The stitches in the hairy part of the head are taken out at the 10–14th day. Absorbable Monocryl 4-0 intracutaneous suture is commonly used in the preauricular area.
Results
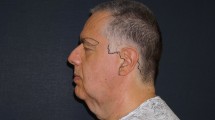
There were 93 procedures performed by using the triple-S lift technique during the period from the end of 2016 to 2018. The level of satisfaction with the achieved results reached 90% (Figs. 4, 5, 6). Neither necrosis nor nerve damage was registered. In one case, the female patient with previous long-term intake of anticoagulants experienced retroauricular hematoma, which was successfully drained with uneventful recovery and no wound revision was required.
Discussion
Anti-aging facial surgery is a little over 100 years old, originating from techniques that involve only the excision of excess skin folds. Gradually, it has become a more profound and delicate intervention. Since the description of the superficial muscular aponeurotic system (SMAS), new techniques have appeared including SMAS plication and resection [6, 22, 26]. More detailed study of facial ligaments, influence of mimic musculature, study of age-related changes in soft tissues of the face, and description of “sliding” spaces—all these factors had a great impact on the general tendency in the development of face surgery [8, 14].
From all the available literature about face-lift and interaction with the SMAS flap, we see that the predominant techniques are those, in which the surgeon either mobilizes the SMAS flap and fixes its distal part in different directions, or performs various types of intact SMAS plication with purse-string sutures.
An impactful trend has been noted in facial surgery lately. If at the beginning of the 1990s there was a significant enthusiasm of surgeons for endoscopic techniques and deep plane surgery and a noticeable decrease in the number of surgeries using SMAS plication, then since 2000 there have been more and more publications about returning to less traumatic techniques, shot scar incisions, and more limited sub-SMAS lifting [18, 27,28,29,30]. A striking example is the appearance of articles of a comparative nature between the efficiency of SMAS plication and deep sub-SMAS lifting [15, 17, 31, 32]. The frequency of complications and the duration of the achieved result are compared [33,34,35].
Special mention should be made of research that demonstrates that sub-SMAS face-lift complication rates were not statistically different compared to those of subcutaneous face-lift with or without SMAS plication. These data suggest that sub-SMAS dissection can be performed with similar safety compared to the traditional subcutaneous face-lift, with the potential additional advantage of the SMAS flap elevation [36].
Increasing demand among patients and surgeons for less traumatic and minimally invasive operative techniques is an undeniable fact nowadays. Hence, the emergence of short scar lift and MACS lift techniques with their intensive usage has become a vivid example of those processes. The authors of those methods suggest avoiding sub-SMAS dissection and suspending the non-undermined SMAS with purse-string sutures [19, 37, 38]. The description of the anterior SMAS lifting procedure has been presented as well, suggesting the beginning of SMAS flap formation in the medial portion of the SMAS, on the borderline between the fixed and mobile portions [16, 39,40,41,42].
The articles describing the elements of SMAS plication and lateral SMASectomy with simultaneous suture suspension of the malar fat are of great interest. The suture passes from the subcutaneous position where it is fixed to the malar fat pad, through the SMAS, and over the periosteum of the zygoma, and is fixed to the deep temporal fascia. Plication of the SMAS over the suture, combined with lateral SMASectomy, provides three vectors of elevation beneath the skin in midface rhytidectomy [43].
Each of those methods has its pros and cons. Because of this, we decided to invent a new method of face-lifting that combines the advantages of SMAS plication and the sub-SMAS lift. To achieve a stable soft tissue lift effect, we introduced the support system of nonabsorbable sutures [20].
The originality of our idea is based on the simultaneous detachment of the SMAS flap and the achievement of its lifting by a series of nonabsorbable ligatures (support system) in the sub-SMAS layer. The support system provides lifting of the medial portion of the SMAS flap and its plication simultaneously, while to some extent it simulates and compensates for age-related changes in the face retaining ligaments. This technique allows us to treat more medial SMAS portions with a smaller area of detachment. Dissection of the SMAS flap is usually limited to the anterior border of the m. masseter, unlike the many techniques of deep sub-SMAS face-lift. In this case, the support system reduces the impact on the distal part of the SMAS flap, which is fixed without tension and can be used to fill the volume in the temporal region. Sub-SMAS localization of ligatures reduces their exposure to the touch (tactile sensation) and allows for closing the “dead space” effectively. On the other hand, in contrast to the techniques of applying purse-string sutures and SMAS plications (MACS lift and S lift), our technique also has a more pronounced effect of lifting the medial portion of the SMAS, since the SMAS flap has greater mobility after detachment.
Such an approach minimizes the number of complications and achieves the desired vector of SMAS lifting. Merging all created spaces (subcutaneous and sub-SMAS) excludes the development of seromas and hematomas. Using this method allows for decreased tension from the created SMAS flap, so the lifting effect has minimal dependence on SMAS thickness and strength. All those aspects make it possible to use a short scar technique and reduce rehabilitation time.
For correction of aging changes of 1–2 type according to Baker (more precisely, the absence of objective and subjective changes in the neck), we use a short preauricular approach. The lower ligature in the neck is not used, the SMAS is redistributed upwards, and the retroauricular SMAS flap remains unengaged.
When correcting aging changes of 3–4 type, the lower ligature of the support system is aimed at improving the neck contouring and provides lifting of the platysma in the upper lateral direction due to lifting of the previously mobilized SMAS flap and forming platysma plication in the upper part of the neck. Applying the support system allowed for a vivid lifting effect at the neck and malar area.
Conclusion
The triple-S lift technique provides both lifting of the medial portion of the SMAS flap and its plication simultaneously. The special support ligatures in the sub-SMAS layer allow us to lift the medial SMAS portions with a smaller area of detachment and to fix the lateral part of the SMAS flap without tension.
Through minimal skin access, we have good result stability, safety, and shortened recovery time. Using limited detachment minimizes the probability of nerve trauma.
This technique is a latter-day one. It requires further study, but the present results are encouraging. All this allows us to recommend this technique as an option in anti-aging facial surgery.
References
Lassus C (1997) Cervicofacial rhytidectomy: the superficial plane. Aesth Plast Surg 21:25–31
Min-Hee Ryu, Moon VA, Yin W (2018) The inclusion of orbicularis oculi muscle in the SMAS flap in Asian facelift: anatomical consideration of orbicularis muscle and zygomaticus major muscle. Aesth Plast Surg 42:471–478
Gosain AK, Amarante MT, Hyde JS, Yousif NJ (1996) A dynamic analysis of changes in the nasolabial fold using magnetic resonance imaging: implications for facial rejuvenation and facial animation surgery. Plast Reconstr Surg 98:622–636
Hamra ST (2000) Prevention and correction of the “facelifted” appearance. Facial Plast Surg 16:215–229
Hamra ST (1990) The deep-plane rhytidectomy. Plast Reconstr Surg 861:53–616
Hamra ST (1992) Composite rhytidectomy. Plast Reconstr Surg 90:1–13
Hamra ST (2001) Correcting the unfavorable outcomes following face-lift surgery. Clin Plast Surg 28:621–638
Mendelson BC (2009) Facelift anatomy, SMAS, retaining ligaments, and facial spaces. In: Aston SJ, Steinbrech DS, Walden JL (eds) Aesthetic plastic surgery. Elsevier, London, pp 53–72
Owsley JQ (1993) Lifting the malar fat pad for correction of prominent nasolabial folds. Plast Reconstr Surg 91:463–474 (discussion 475–466)
Owsley JQ (1995) Elevation of the malar fat pad superficial to the orbicularis oculi muscle for correction of prominent nasolabial folds. Clin Plast Surg 22:279–293
Owsley JQ (1997) Face lift. Plast Reconstr Surg 100:514–519
Owsley JQ, Zweifler M (2002) Midface lift of the malar fat pad: technical advances. Plast Reconstr Surg 110(2):674–685 (discussion 686–687)
Panfilov DE (2003) MIDI face-lift and tricuspidal SMAS-flap. Aesth Plast Surg 27:27–37
Paul MD (2017) The anterior SMAS approach for facelifting and for buccal fat pad removal. Aesth Plast Surg. https://doi.org/10.1007//s00266-017-0921-0
Prado A, Andrades P, Danilla S, Castillo P, Leniz P (2006) A clinical retrospective study comparing two short-scar face lifts: minimal access cranial suspension versus lateral SMASectomy. Plast Reconstr Surg 117:1413–1425 (discussion 1426–1427)
Robbins LB, Brothers DB, Marshall DM (1995) Anterior SMAS application for the treatment of prominent nasomandibular folds and restoration of normal cheek contour. Plast Reconstr Surg 96:1279–1287
Sundine MJ, Kretsis V, Connell BF (2010) Longevity of SMAS facial rejuvenation and support. Plast Reconstr Surg 126:229–237
Stuzin JM, Baker TJ, Gordon HL, Baker TM (1995) Extended SMAS dissection as an approach to midface rejuvenation. Clin Plast Surg 22:295–311
Tonnard P, Verpaele A, Monstrey S, Van Landuyt K, Blondeel P, Hamdi M, Matton GA (2002) Minimal access cranial suspension lift: a modified S-lift. Plast Reconstr Surg 1096:2074–2086
Yousif N, Gosain A, Matloub H et al (1994) The nasolabial fold: an anatomic and histologic reappraisal. Plast Reconstr Surg 93:60
Yousif N, Mendelson BC (1995) Anatomy of the midface. Clin Plast Surg 22:227–240
Baker DC (1997) Lateral SMASectomy. Plast Reconstr Surg 100(2):509–513
Basile FV, Basile AR, Basile VV (2012) Triple-anchoring sub-SMAS face-lift. Aesthet Plast Surg 36:526–533
Connell BF, Semlacher RA (1997) Contemporary deep layer facial rejuvenation. Plast Reconstr Surg 100:1513
Guyuron B (2005) Modified temporal incision for facial rhytidectomy: an 18-year experience. Plast Reconstr Surg 115:609
Mitz V, Peyronie M (1976) The superficial aponeurotic system (SMAS) in the parotid and cheek area. Plast Reconstr Surg 58:80–88
Berry MG, Daivies D (2010) Platysma-SMAS placation facelift. J Plast Reconstr Aesthet Surg 63(5):793–800
Choucair RJ, Hamra ST (2008) Extended superficial musculo-aponeurotic system dissection and composite rhytidectomy. Clin Plast Surg 35(4):607–622
Jacono AA, Parikh SS (2011) The minimal access deep plane extended vertical facelift. Aesthet Surg J 318:874–890
Marten TJ (2008) High SMAS facelift: combined single flap lifting of the jawline, cheek, and midface. Clin Plast Surg 35:569–603
Chang S, Pusic A, Rohrich RJ (2011) A systematic review of comparison of efficacy and complication rates among face-lift techniques. Plast Reconstr Surg 127(1):423–433
Matarasso A, Elkwood A, Rankin M, Elkowitz M (2000) National plastic surgery survey: facelift techniques and complications. Plast Reconstr Surg 106:1185–1195 (discussion 1196)
Abboushi N, Yezhelyev M, Symbas J, Nahai F (2012) Facelift complications and the risk of venous thromboembolism: a single center’s experience. Aesthet Surg J 32:413–420
Baker TJ, Gordon HL (1967) Complications of rhytidectomy. Plast Reconstr Surg 40:31–39
Grover R, Jones BM, Waterhouse N (2001) The prevention of hematoma following rhytidectomy: a review of 1078 consecutive facelifts. Br J Plast Surg 54:481–486
Rammos CK, Mohan AT, Maricevich MA et al (2015) Is the SMAS flap facelift safe? A comparison of complications between the sub-SMAS approach versus the subcutaneous approach with or without SMAS plication in aesthetic rhytidectomy at an academic institution. Aesthet Plast Surg 39(6):870–876
Baker DC (2001) Minimal incision rhytidectomy (short scar face-lift) with lateral SMASectomy. Aesthet Surg J 21:68–79
Labbe´ D, Franco RG, Nicolas J (2006) Platysma suspension and platysmaplasty during neck lift: anatomical study and analysis of 30 cases. Plast Reconstr Surg 117:2001–2007
Adamson PA, Dahiya R, Litner J (2007) Midface effects of the deep-plane vs. the superficial musculoaponeurotic system plication face-lift. Arch Fac Plast Surg 9(1):9–11
Becker FF, Bassichis BA (2004) Deep-plane face-lift vs superficial musculoaponeurotic system plication face-lift: a comparative study. Arch Facial Plast Surg 6(1):8–13
Jacono AA, Stong BC (2010) Anatomic comparison of the deep plane face-lift and the transtemporal midface-lift. Arch Facial Plast Surg 12(5):339–341
Miller AJ, Graham HD 3rd (1997) Comparison of conventional and deep plane facelift. J La State Med Soc 149(11):406–411
Noon BR (2006) Suture suspension malarplasty with SMAS plication and modified SMASectomy: a simplified approach to midface lifting. Plast Reconstr Surg 117:792
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest in this paper.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent
The patients provided their consent for publication of their photographs.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Belyi, I., Tymofii, O. & Barannik, M. Triple-S Lift for Facial Rejuvenation. Aesth Plast Surg 43, 1204–1211 (2019). https://doi.org/10.1007/s00266-019-01319-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-019-01319-3