Abstract
Background
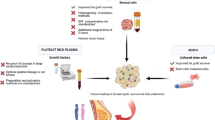
Adipose-derived stem cell (ADSCs)-assisted and platelet-rich plasma (PRP)-assisted lipofilling aim to enhance angiogenesis and cell proliferation and are promising techniques for lipofilling. This study aimed to compare the outcomes of ADSCs-assisted and PRP-assisted lipofilling.
Methods
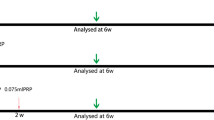
Adipose tissue and human venous blood were obtained from women with early breast cancer. Human ADSCs were isolated and amplified in vitro. PRP was extracted through double centrifugation. The effect of PRP on ADSCs proliferation was evaluated. In the in vivo study, 1 ml of adipose tissue with saline (control group), PRP (PRP group), or ADSCs (ADSCs group) was injected subcutaneously into the dorsum of nude mice. At 2, 4, 8, and 12 weeks after injection, tissues were assessed for volume retention and ultrasound abnormality. For histological assessment, hematoxylin and eosin staining were performed.
Results
Cytokines in PRP and blood were comparable. Regarding the in vitro assay, PRP significantly improved ADSCs proliferation, and the effect was dose-dependent. Concerning the in vivo study, for each time point, ADSCs-assisted lipofilling showed superior volume maintenance. Similarly, the PRP group showed improved angiogenesis and fat survival, as compared with the control group. The angiogenic effect of PRP was inferior to that of ADSCs at most time points. No significant difference was observed at 12 weeks after lipofilling. Complication rates were comparable between the PRP group and ADSCs group.
Conclusions
PRP-assisted and ADSCs-assisted lipofilling can significantly improve the cosmetic results of grafted fat. PRP-assisted lipofilling, which is considered convenient and clinically available, is a promising technique to improve neovascularization and fat survival.
No Level Assigned
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lipofilling has been widely used in plastic and reconstructive surgeries. Adipose tissue is an ideal soft tissue filler owing to its extensive sources and natural texture and the absence of foreign body reactions. However, as it is an energy storing tissue, its survival depends on sufficient oxygen supply. During aspiration and injection, adipose tissue or adipocytes cannot cope well with hypoxia and ischemia. Its pathological characteristics can result in an unpredictable postoperative volume, with a reported maintenance rate ranging from 10 to 80% [1, 2]. To improve the survival of tissue in lipofilling, many techniques aimed at improving neovascularization and fat tissue ischemia have been proposed. Studies have reported the use of supplements, including stromal vascular fractions, adipose-derived stem cells (ADSCs), chemical-resistant cell activating factors (insulin, erythropoietin, etc.), and multiple growth factors [3,4,5,6,7], and some of these studies have noted good outcomes. Among all techniques, cell-assisted lipofilling is considered one of the most impressive approaches. Experimental and clinical studies have demonstrated that in vitro-amplified ADSCs can significantly increase vascularization and ensure volume maintenance of the grafted fat [8, 9]. However, the oncological safety of ADSCs in breast cancer survivors remains unclear [10, 11].
Ischemia and hypoxia are the main obstacles of lipofilling. The addition of angiogenic growth factors has been shown to be a feasible strategy. Previous studies showed that the addition of vascular endothelial growth factor (VEGF) and fibroblast growth factor significantly improved fat survival. However, the high cost of purified cytokines has limited their wide use in clinical practice. Platelet-rich plasma (PRP) is a biomatrix component containing high concentrations of platelets and various growth factors, such as VEGF, platelet-derived growth factor, and transforming growth factor β. It has been shown that PRP-assisted lipofilling improves lipofilling outcomes and is a promising substitute for ADSCs-assisted lipofilling [12, 13]. The present study aimed to compare the adipose tissue survival and vascularization of PRP-assisted and ADSCs-assisted lipofilling.
Materials and Methods
Adipose Tissue Harvesting and Isolation of ADSCs
Adipose tissue was obtained from the mastectomy sample of women with early breast cancer (n = 9) at our institution. Adipose tissue was used for ADSCs isolation and fat grafting in nude mice. ADSCs were digested using 1 mg/ml of collagenase type I according to our previously study [14]. ADSCs from the third passage were used for lipofilling.
This study was approved by the ethics committee of our institution, and written informed consent was obtained from all tissue donors.
Preparation and Characteristics of PRP
Fresh venous blood was donated from the same fat tissue donors. PRP was prepared as previously described by Landesberg et al. [15]. Briefly, fresh venous blood was centrifuged at 200g for 10 min. The upper and middle layers were extracted and further centrifuged at 200g for 10 min. The bottom layer was extracted, and 10% calcium chloride was added as an activator. After the blood clots contracted, samples were centrifuged at 60g for 5 min, and the upper layer was considered as activated PRP.
VEGF-1, VEGF-2, and epidermal growth factor (EGF) levels in PRP and blood samples were measured using the Affymetrix® Elisa Kit (Thermo Fisher Scientific, Waltham, MA, USA). The effect of ADSCs proliferation associated with PRP was tested using a Cell Counting Kit (CCK8, Dojindo, Kumamoto, Japan). All procedures were performed according to the manufacturers’ instructions.
In Vivo Analysis of ADSCs-Assisted and PRP-Assisted Lipofilling in Mice
Adipose tissue was diced into a granular form using ophthalmic scissors. After washing with saline thrice, the tissue was centrifuged at 200g for 5 min. The middle layer was used for grafting.
One hundred healthy male nude mice (20 for each group, 4–6 weeks old) weighing 18–22 g were purchased from Sichuan Dashuo Laboratory Animal Center (Sichuan, China). All animal experiments were approved by the institution animal care and use committee. For the experiment, 1 ml of adipose tissue with or without supplement was injected subcutaneously into the dorsum of nude mice. In the control group, 0.3 ml of saline was added to 1 ml of adipose tissue, while in the PRP group, 0.3, 0.2 and 0.1 ml of PRP was added to 1 ml of adipose tissue to form 30, 20, and 10% PRP-enhanced fat grafts, respectively. In the ADSCs group, 0.3 ml cell suspension (6.67 × 106 cell/ml) was added to 1 ml of adipose tissue.
At 2, 4, 8, and 12 weeks after injection, an ultrasound examination was performed to assess for complications. Images were captured using the Philips IU22 color Doppler ultrasound imaging system (Philips Healthcare, Bothell, WA) equipped with a 5–12-MHz probe. Grafts were harvested, and graft volumes were measured with the Archimedes drainage method. Grafts were further assessed using hematoxylin–eosin staining. The vascular density was semi-quantitatively analyzed.
Statistical Analysis
Data for grafted fat volume and vascular vessel count were analyzed, and differences among independent group averages were tested using the Chi-square test. All data analyses were performed using SPSS software for Windows, version 17.0 (SPSS, Inc., Chicago, IL, USA). Significance was considered at a P value < 0.05.
Results
PRP is Rich in Angiogenic Cytokines
During PRP preparation, nearly 1 ml of PRP was obtained from a 10-ml blood sample. The concentrations of angiogenic cytokines in blood and PRP are shown in Table 1. VEGF-1 and VEGF-2 concentrations were twofold higher in the PRP group than in the control group; however, the differences were not significant. The EGF level was 1.13-fold higher in the PRP group than in the control group.
PRP Improves the Proliferation of Human ADSCs In Vitro
As shown in Fig. 1, PRP can significantly increase ADSCs proliferation, and the effect tends to be dose-dependent (P = 0.017). In particular, ADSCs cultured using a medium supplemented with 30% PRP showed a 25% increase in proliferation at day 5 (P = 0.012).
PRP and ADSCs Improve Adipose Tissue Survival After Lipofilling In Vivo
At 12 weeks after lipofilling, the grafts had a soft texture in all groups, with smooth surfaces and clear boundaries. No chromatosis, rupture, or edema was found.
The maintained volume decreased with time in the control and PRP groups (Fig. 2a). No significant difference was observed for mice that received ADSCs-assisted lipofilling at different time points (P = 0.21). At 12 weeks after lipofilling, the volume of grafts decreased to 43.60% in the control group. The addition of PRP and ADSCs significantly increased the survival of grafted fat. At 12 weeks after lipofilling, the mean volumes of grafts were 0.56, 0.67, and 0.77 ml in the control, PRP, and ADSC groups, respectively. The survival volumes were 19.15 and 36.17% higher in the PRP and ADSCs groups, respectively, when compared to the volume in the control group. In particular, the volume of grafts in the ADSC group was the highest at all time points.
Maintained volume of grafted fat in different groups. a The maintained volume of grafted fat in the control, adipose-derived stem cells (ADSCs), and platelet-rich plasma (PRP) groups. ADSCs and PRP significantly increase the maintained volume of grafted fat. b The maintained volume of grafted fat in different volume fractions of PRP. The 20 and 30% PRP show similar outcomes. *P < 0.05, **P < 0.01
The effect of additional PRP on fat survival was observed from the fourth week. PRP-assisted lipofilling showed a dose-dependent relationship (Fig. 2b). At all time points, no significant difference was observed between the 10% PRP group and the control group. However, with 20% PRP, increased fat survival was observed from the fourth week (P = 0.015). In addition, no significant difference was observed between the 20 and 30% PRP groups at all time points. These data suggested that 20% PRP might be the most suitable concentration for fat grafting.
Results of the Ultrasound Examinations
Ultrasound images of grafted fat in all groups were similar across all time points (Fig. 3a). A capsule was noted in all groups 4 weeks after lipofilling. Fat necrosis was noted in all groups, with an average rate of 47% (Fig. 3b, c). Specifically, the rates of fat necrosis in the control, PRP, and ADSCs groups were 45, 55, and 45%, respectively.
PRP and ADSCs Can Improve Neovascularization
In histological images, fibrous connective tissue was observed in all groups (Fig. 4). No significant difference was observed among the groups, and the median fibrous connective tissue area was 9.47%.
Neovascularization is the key factor for adipose tissue survival. Angiogenesis was semi-quantified, and the results are shown in Fig. 5. The vascular density in all groups increased with time. At all time points, vascular density was the lowest in the control group and the highest in the ADSCs group. For the PRP and ADSCs groups, no significant difference in neovascularization was noted, except at the eighth week.
Vessel density of the platelet-rich plasma (PRP)-assisted and adipose-derived stem cell (ADSCs)-assisted lipofilling. a The vessel density of the PRP-assisted and ADSCs-assisted lipofilling at different time points. ADSCs-assisted lipofilling can significantly increases the angiogenesis of lipogenesis. No difference is observed between the PRP-assisted and ADSCs-assisted lipofilling at the 2, 4, and 12 weeks. b The vascularization of lipofilling under a different volume fraction of PRP. The 20 and 30% PRP have a similar angiogenic effect. *P < 0.05, **P < 0.01
The dose-dependent effect of PRP is shown in Fig. 5b. 10% PRP can significantly improve neovascularization at long-term observation. 20 and 30% PRP can significantly improve neovascularization at the fourth week after injection. Similar to the findings for fat survival, no significant difference was observed between 20 and 30% PRP at all time points.
Conclusions
PRP-assisted and ADSCs-assisted lipofilling can improve the volume maintenance and angiogenesis of grafted fat significantly at 2–12 weeks after lipofilling. We believe that 20% PRP is a preferable concentration for lipofilling, as 20% PRP had similar vascularization when compared to that with ADSCs enhancement. Considering clinical accessibility and safety, 20% PRP-assisted lipofilling is a preferable approach for soft tissue augmentation.
Discussions
Insufficient neovascularization was the main limitation for fat survival. To improve neovascularization, many techniques have been reported. Among all the approaches, ADSCs-assisted lipofilling has shown promising results. The multi-potential differentiation of ADSCs allows differentiation into adipocytes and endothelial cells to increase fat survival and vascularization of grafted fat [16, 17]. ADSCs can also secret angiogenic and antiapoptotic factors to improve cell survival and reduce post-injury fibrogenesis [18, 19]. Kølle et al. have shown that the residual volume of ADSCs-assisted lipofilling was 80.9% at 121 days after injection, while that of conventional fat grafting was 16.3% (P < 0.0001) [9]. In our study, after 3 months of lipofilling, the residual volume of ADSCs-assisted lipofilling was 76.8% and that of control lipofilling was 56.4%. The residual volume was approximately 10% higher in the ADSCs group than in the control group at 2 weeks after injection and approximately 20% higher in the ADSCs group than in the control group at 12 weeks after injection. Vascular density was also greater in the ADSCs group than in the other groups at 4–8 weeks after injection, which indicates that ADSCs effectively improved volume maintenance and vascularization of grafted fat.
In the ADSCs group, we added 2 × 106 cells for 1 ml of fat, which is approximately 200 times the physiological concentration [20, 21]. However, in clinical practice, the in vitro amplification of ADSCs requires approval from the state Food and Drug Administration, and no standard practice for stem cell amplification is currently available. Additionally, in clinical practice, the in vitro amplification of ADSCs needs a high tissue source content and a waiting period of 10–15 days. Furthermore, studies on the oncological safety of ADSCs remain controversial [22]. In basic studies, the promotion of proliferation and metastasis and the inhibiting effect of tumor growth were both observed [23, 24]. Meanwhile, multiple prospective and retrospective studies have also reported increased and non-increased locoregional recurrence [25, 26]. The oncological safety of ADSCs-assisted lipofilling remains the main obstacle for clinical use, especially in women with breast cancer.
Autologous ADSCs and PRP are both promising biological supplements for fat grafting. Our study also demonstrated that ADSCs-assisted lipofilling is superior to PRP-assisted lipofilling in terms of improved fat survival and neovascularization. However, concerns about the oncological safety of ADSCs have limited its clinical usage. Therefore, PRP is a promising alternative to ADSCs.
The effects of PRP for improving angiogenesis and supporting proliferation of ADSCs have been reported in some studies [27,28,29,30]. Autologous PRP is also proposed as a biological supplement for skin wound healing, bone defects, and soft tissue augmentation [28, 29]. Previous studies have demonstrated that PRP can interact with ADSCs and have a synergistic effect on vascularization [30]. Our study showed that PRP is rich in angiogenic growth factors, and the levels were comparable to those in blood. These angiogenic and proliferation-promoting effects are important for fat graft survival. In addition, PRP is also thought to provide elementary nutrients and inhibit the apoptosis of adipocytes and preadipocytes [31]. However, the effect of PRP on ADSCs differentiation was debatable. The improved and decreased differentiation ability of ADSCs were both reported in studies [32,33,34]. Thus, more studies are needed to clarify the effect of PRP on ADSCs differentiation.
The optimal dose of PRP for lipofilling is under debate. In our study, volume maintenance and vascularization of grafted fat increased with an increase in the dose of PRP, exhibiting a dose-dependent effect. However, the volume maintenance and neovascularization of 20% PRP and 30% PRP were similar, suggesting that a higher concentration did not increase vascularization and fat survival. Our study’s finding was similar to that of Li et al.’s study that also reported no significant difference between the 20 and 30% PRP-assisted lipofilling [33]. Results of in vitro assays have also indicated the greatest proliferative effect of 20% PRP when compared with 10 and 30% PRP [34, 35]. Based on our data, for 100-ml lipofilling, 20-ml PRP or 200-ml fresh blood is needed to achieve improved aesthetic outcomes, which can be easily acquired from the patient. Apart from clinical availability, when compared with other cell supplements or growth factors, PRP has many advantages, including easy preparation, no waiting time, and low cost. In our study, we used a single-dose strategy for adding PRP. Further studies are required to assess whether sustained growth factor release could provide better outcomes.
To increase neovascularization, multi-channel and multi-direction injections are needed in clinical practice to ensure an increased surface-volume ratio [36]. However, the structure of subcutaneous tissue in mice is different from that in humans. We used a single channel injection, which is likely to result in a low surface-volume ratio and high fat necrosis. The injection method may contribute to the high fat necrosis rate in an animal study.
References
Alexander D, Bucky LP (2011) Breast augmentation using pre-expansion and autologous fat transplantation—a clinical radiological study. Plast Reconstr Surg 127:2451–2452
Spear SL, Pittman T (2014) A prospective study on lipoaugmentation of the breast. Aesthet Surg J 34:400
Yoshimura K, Sato K, Aoi N, Kurita M, Hirohi T, Harii K (2008) Cell-assisted lipotransfer for cosmetic breast augmentation: supportive use of adipose-derived stem/stromal cells. Aesthet Plast Surg 32:48–55
Yoshimura K, Sato K, Aoi N, Kurita M, Inoue K, Suga H, Eto H, Kato H, Hirohi T, Harii K (2008) Cell-assisted lipotransfer for facial lipoatrophy: efficacy of clinical use of adipose-derived stem cells. Dermatol Surg 34:1178–1185
Chung CW, Marra KG, Li H, Leung AS, Ward DH, Tan H, Kelmendi-Doko A, Rubin JP (2012) VEGF microsphere technology to enhance vascularization in fat grafting. Ann Plast Surg 69:213–219
Yuksel E, Weinfeld AB, Cleek R, Wamsley S, Jensen J, Boutros S, Waugh JM, Shenaq SM, Spira M (2000) Increased free fat-graft survival with the long-term, local delivery of insulin, insulin-like growth factor-I, and basic fibroblast growth factor by PLGA/PEG microspheres. Plast Reconstr Surg 105:1712–1720
Hamed S, Egozi D, Kruchevsky D, Teot L, Gilhar A, Ullmann Y (2010) Erythropoietin improves the survival of fat tissue after its transplantation in nude mice. PLoS ONE 5:e13986
Zhu M, Zhou Z, Chen Y, Schreiber R, Ransom JT, Fraser JK, Hedrick MH, Pinkernell K, Kuo HC (2010) Supplementation of fat grafts with adipose-derived regenerative cells improves long-term graft retention. Ann Plast Surg 64:222–228
Kølle SF, Fischer-Nielsen A, Mathiasen AB, Elberg JJ, Oliveri RS, Glovinski PV, Kastrup J, Kirchhoff M, Rasmussen BS, Talman ML, Thomsen C, Dickmeiss E, Drzewiecki KT (2013) Enrichment of autologous fat grafts with ex vivo expanded adipose tissue-derived stem cells for graft survival: a randomised placebo-controlled trial. Lancet 382:1113–1120
Schweizer R, Tsuji W, Gorantla VS, Marra KG, Rubin JP, Plock JA (2015) The role of adipose-derived stem cells in breast cancer progression and metastasis. Stem Cells Int 2015:120949
Wong RSY (2011) Mesenchymal stem cells: angels or demons? Biomed Res Int 2011:459510
Strassburg S, Nienhueser H, Björn SG, Finkenzeller G, Torio-Padron N (2016) Co-culture of adipose-derived stem cells and endothelial cells in fibrin induces angiogenesis and vasculogenesis in a chorioallantoic membrane model. J Tissue Eng Regen Med 10:496–506
Merfeldclauss S, Gollahalli N, March KL, Traktuev DO (2010) Adipose tissue progenitor cells directly interact with endothelial cells to induce vascular network formation. Tissue Eng Part A 16:2953–2966
Tian CX, Fan XJ, Chen XH, Deng L, Qin TW, Luo JC, Li XQ, Lv Q (2012) Preparation and biocompatibility of porcine skeletal muscle acellular matrix for adipose tissue engineering. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi 26:749–754
Landesberg R, Roy M, Glickman RS (2000) Quantification of growth factor levels using a simplified method of platelet-rich plasma gel preparation. J Oral Maxillofac Surg 58:297–300
Matsumoto D, Sato K, Gonda K, Takaki Y, Shigeura T, Sato T, Aiba-Kojima E, Iizuka F, Inoue K, Suga H, Yoshimura K (2006) Cell-assisted lipotransfer: supportive use of human adipose-derived cells for soft tissue augmentation with lipoinjection. Tissue Eng 12:3375–3382
Miranville A, Heeschen C, Sengenès C, Curat CA, Busse R, Bouloumié A (2004) Improvement of postnatal neovascularization by human adipose tissue-derived stem cells. Circulation 110:349–355
Suga H, Eto H, Shigeura T, Inoue K, Aoi N, Kato H, Nishimura S, Manabe I, Gonda K, Yoshimura K (2009) IFATS collection: fibroblast growth factor-2-induced hepatocyte growth factor secretion by adipose-derived stromal cells inhibits postinjury fibrogenesis through a c-Jun N-terminal kinase-dependent mechanism. Stem Cells 27:238–249
Rehman J, Traktuev D, Li J, Merfeld-Clauss S, Temm-Grove CJ, Bovenkerk JE, Pell CL, Johnstone BH, Considine RV, March KL (2004) Secretion of angiogenic and antiapoptotic factors by human adipose stromal cells. Circulation 109:1292–1298
Barret JP, Sarobe N, Grande N, Vila D, Palacin JM (2009) Maximizing results for lipofilling in facial reconstruction. Clin Plast Surg 36:487–492
Francis MP, Sachs PC, Elmore LW, Holt SE (2010) Isolating adipose-derived mesenchymal stem cells from lipoaspirate blood and saline fraction. Organogenesis 6:11–14
O’Halloran N, Courtney D, Kerin MJ, Lowery AJ (2017) Adipose-derived stem cells in novel approaches to breast reconstruction: their suitability for tissue engineering and oncological safety. Breast Cancer 11:1–18
Ryu H, Oh JE, Rhee KJ, Baik SK, Kim J, Kang SJ, Sohn JH, Choi E, Shin HC, Kim YM, Kim HS, Bae KS, Eom YW (2014) Adipose tissue-derived mesenchymal stem cells cultured at high density express IFN-β and suppress the growth of MCF-7 human breast cancer cells. Cancer Lett 352:220–227
Dirat B, Bochet L, Dabek M, Daviaud D, Dauvillier S, Majed B, Wang YY, Meulle A, Salles B, Le Gomidec S, Garrido I, Escourrou G, Valet P, Muller C (2011) Cancer-associated adipocytes exhibit an activated phenotype and contribute to breast cancer invasion. Cancer Res 71:2455–2465
Tan SS, Loh W (2017) The utility of adipose-derived stem cells and stromal vascular fraction for oncologic soft tissue reconstruction: is it safe? A matter for debate. Surgeon 15:186–189
Petit JY, Maisonneuve P, Rotmensz N, Bertolini F, Clough KB, Sarfati I, Gale KL, Macmillan RD, Rey P, Benyahi D, Rietjens M (2015) Safety of lipofilling in patients with breast cancer. Clin Plast Surg 42:339–344
Choi J, Minn KW, Chang H (2012) The efficacy and safety of platelet-rich plasma and adipose-derived stem cells: an update. Arch Plast Surg 39:585–592
Luiz C, Gontijo-de-Amorim NF, Takiya CM, Radovan B, Donatella B, Paolo B, Andrea S, Gino R (2017) Effect of use of platelet-rich plasma (PRP) in skin with intrinsic aging process. Aesthet Surg J. https://doi.org/10.1093/asj/sjx137
Smith OJ, Kanapathy M, Khajuria A, Prokopenko M, Hachach-Haram N, Mann H, Mosahebi A (2017) Protocol for a systematic review of the efficacy of fat grafting and platelet-rich plasma for wound healing. Syst Rev 6:111
Blanton MW, Hadad I, Johnstone BH, Mund JA, Rogers PI, Eppley BL, March KL (2009) Adipose stromal cells and platelet-rich plasma therapies synergistically increase revascularization during wound healing. Plast Reconstr Surg 123:56S–64S
LiaoHT Marra KG, Rubin JP (2014) Application of platelet-rich plasma and platelet-rich fibrin in fat grafting: basic science and literature review. Tissue Eng Part B Rev 20:267–276
Chignonsicard B, Kouidhi M, Xi Y, Audrey DA, Villageois P, Peraldi P, Ferrari P, Rival Y, Piwnica D, Aubert J, Dani C (2017) Platelet-rich plasma respectively reduces and promotes adipogenic and myofibroblastic differentiation of human adipose-derived stromal cells via the TGFβ signalling pathway. Sci Rep 7:2954
Li F, Guo W, Li K, Yu M, Tang W, Wang H, Tian WD (2015) Improved fat graft survival by different volume fractions of platelet-rich plasma and adipose-derived stem cells. Aesthet Surg J 35:319
Feng L, Huang SB, Zhao S, Deng H (2017) Effects of platelet-rich plasma on proliferation and adipogenic differentiation of adipose-derived stem cells in vitro. J Wenzhou Med Univ 7–13
Felthaus O, Prantl L, Skaff-Schwarze M, Klein S, Anker A, Ranieri M, Kuehlmann B (2017) Effects of different concentrations of platelet-rich plasma and platelet-poor plasma on vitality and differentiation of autologous adipose tissue-derived stem cells. Clin Hemorheol Microcirc 66:1–9
Khouri RK, Rigotti G, Cardoso E, Khouri RK, Biggs TM (2014) Megavolume autologous fat transfer: part I. Theory and principles. Plast Reconstr Surg 133:1369–1377
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration Helsinki and its later amendments or comparable ethical standards. All applicable institutional and/or national guidelines for the care and use of animals were followed.
Informed Consent
Informed consent was obtained from all tissue donors.
Rights and permissions
About this article
Cite this article
Xiong, BJ., Tan, QW., Chen, YJ. et al. The Effects of Platelet-Rich Plasma and Adipose-Derived Stem Cells on Neovascularization and Fat Graft Survival. Aesth Plast Surg 42, 1–8 (2018). https://doi.org/10.1007/s00266-017-1062-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-017-1062-1