Abstract
Background
“Gynecomastia” is an enlargement of the male breast. Our study aims to assess patient satisfaction as well as evaluate differences in recurrence rates in lipomatous and glandular gynecomastia 10–19 years postoperatively.
Methods
Forty-one gynecomastia patients undergoing surgical treatment from 1997 to 2005 were invited for a follow-up examination 10–19 years postoperatively. Of these, 16 patients presented for a clinical examination. Patient satisfaction was measured with a validated questionnaire [consultation satisfaction questionnaire (CSQ)-9]. Furthermore, photo-material and patient charts were evaluated concerning preoperative macroscopical type of gynecomastia, BMI, and operative technique.
Results
Mean follow-up time was 13.8 years (range: 10.5–19 years). Eight patients (50%) had presented with lipomatous and eight patients (50%) with glandular gynecomastia prior to surgery. One of the patients with glandular gynecomastia (12.5%) presented with recurrence at the time of follow-up, while five of the eight patients showing lipomatous gynecomastia (62.5%) presented with recurrence. Interestingly, younger patient groups tend to be more satisfied with the operative treatment of gynecomastia than older patient groups, especially regarding the improvement of self-esteem.
Conclusions
Long-term follow-up results showed that recurrence rates are significantly higher in patients with lipomatous gynecomastia than in patients with glandular gynecomastia, with BMI increase in patients with glandular and lipomatous gynecomastia showing no statistically significant differences. Furthermore, general patient satisfaction and improvement of self-esteem was higher in younger patient groups than older patient groups.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Clinical Trial Registration Number: DRKS00009630.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
“Gynecomastia,” an enlargement of the male breast, mainly occurs in three phases of life, corresponding to the times of hormonal changes [1]: during the neonatal period, during puberty, and among adults between the age of 50 and 80 years [2,3,4,5,6,7].
According to Webster, gynecomastia can histologically be divided into three classes: (I) periductal connective tissue hypertrophy tissue change, (II) increase in the amount of both of these, and (III) adipose tissue hypertrophy alone [8]. Although being mostly idiopathic, gynecomastia can be associated with medication, drug abuse, and the exposition of chemical substances such as phenothrin [9], liver function disorders, and endocrine or malign disorders.
Especially in adolescent males, gynecomastia is associated with an increased risk of psychological disorders such as depression, anxiety, and social phobia [10, 11]. Thus, even though spontaneous remission of gynecomastia occurs in up to 75% of cases [2, 12], gynecomastia needs to be treated in case of psychological distress. Pharmacological treatment and prophylaxis of gynecomastia with selective estrogen receptor modulators such as tamoxifen or testosterone derivatives like danazol have proven to be successful, with tamoxifen showing stronger effects but higher relapse rates than danazol [13,14,15,16,17]. Surgical treatment consists of liposuction with or without resection of glandular tissue (Fig. 1) depending on the type and grade of gynecomastia present [18,19,20,21,22,23,24]. To date, apart from studies evaluating the outcome of different operative techniques, no studies have been performed analyzing the risk factors for recurrence of gynecomastia.
Our study aims to evaluate differences in recurrence rates in lipomatous and glandular gynecomastia and its association with BMI increase 10–19 years postoperatively, furthermore assessing patient satisfaction.
Patients and Methods
Forty-one gynecomastia patients undergoing surgical treatment from 1997 to 2005 were invited for a follow-up examination 10–19 years postoperatively. Of these, 16 patients presented for a clinical examination. The treatment modality was chosen according to the preoperative clinical finding: Liposuction combined with direct excision was performed in patients with partially fibrous or dense glandular breast tissue. If a good result was obtained with just liposuction, excision was not performed. Photo-material and patient charts were evaluated concerning preoperative macroscopical type of gynecomastia, BMI, and operative technique. When classified as Simon Grade I [25] or higher, reappearance of gynecomastia after surgery was considered as recurrence.
Patient satisfaction was measured with a validated questionnaire, whose format was adopted from the consultation satisfaction questionnaire 9 (CSQ-9). The CSQ-9 is easily scored and consists of ten items. Each item of the CSQ-9 shows a score of 1–4. Final scoring is carried out by adding the individual item scores to yield a range of 10–40, with higher scores representing greater satisfaction. Patients were informed that participation in the study is voluntary and that answers would be anonymous and would not influence subsequent therapy in our department.
The local Ethics Committee approved the study. The study has been registered in the German Clinical Trials Register (DRKS) (clinical trial registration number: DRKS00009630) which meets the requirements of the International Committee of Medical Journal Editors (ICMJE). The design and performance of the study is in accordance with the Declaration of Helsinki. Statistical analysis was performed using GraphPad Prism 5 (GraphPad Software, San Diego, CA, USA). Comparison of normally distributed, continuous data between different groups was performed with unpaired Student’s t-test and categorical data with Chi-square test.
Results
Mean follow-up time was 13.8 years (range: 10.5–19 years). Mean age of patients at the time of surgery was 32.4 years; mean age at the time of follow-up was 46.2 years (range: 25–71 years). Eight patients (50%) had presented with lipomatous and eight patients (50%) with glandular gynecomastia prior to surgery. In each five of the patients (62.5%) who presented with glandular and lipomatous gynecomastia, liposuction and resection of glandular tissue was carried out, while in each three (37.5%) patients, only liposuction was performed (Table 1). One patient with glandular and one patient with lipomatous gynecomastia had surgery twice due to gynecomastia recurrence within 1 year after the primary surgery. In two patients with glandular gynecomastia undergoing both liposuction and resection of glandular tissue, scar correction was carried out following primary surgery, whereas in one patient, periareolar mastopexy was performed due to postoperative periareolar skin excess. Of the patients presenting with recurrence in the first postoperative year (n = 2), one was primarily treated with liposuction, whereas the other one was treated with liposuction and resection of glandular tissue. Of the patients presenting with recurrence (n = 6), three (50%) were primarily treated with liposuction, whereas three (50%) were treated with liposuction and resection of glandular tissue. Three patients (18.8%) presented with dysesthesia at the time of follow-up.
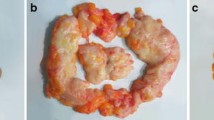
One of the patients with glandular gynecomastia (Fig. 2) presented with recurrence at the time of follow-up, whereas five of the eight patients showing lipomatous gynecomastia (Fig. 3) presented with recurrence (12.5 vs. 62.5%, respectively; p = 0.0389; Fig. 4). The mean increase in BMI from the time of surgery until the time of follow-up was 1.7 kg/m2 (range: 0–6.7 kg/m2) in patients with preoperative glandular gynecomastia and 3.8 kg/m2 (range: 1.5–10.0 kg/m2) in patients with preoperative lipomatous gynecomastia (Table 1); however, BMI increase was not significantly different between the two groups (p = 0.1405).
Patient satisfaction was good with a mean score of 33.8 of 40 possible points (84.5%; Table 1).
We did not find statistically significant differences in CSQ-9 scores in patients with lipomatous gynecomastia compared to patients with glandular gynecomastia [34.6 (n = 8) and 32.9 points (n = 8), respectively; p = 0.4410], patients with and without recurrence of gynecomastia [35.2 (n = 6) and 32.9 points (n = 10), respectively; p = 0.3308], patients with and without dysesthesia of the nipple areolar complex at the time of follow-up [30.3 (n = 3) and 34.5 (n = 13) points, respectively, p = 0.1366], and patients with and without follow-up surgery due to skin retraction or skin excess [35.0 (n = 3) and 33.5 (n = 13), respectively, p = 0.5991; data not shown].
However, we found that younger patient groups tend to be more satisfied with the operative treatment than older patient groups, irrespective of the rate of the complication and recurrence rate. Thus, the mean score of 13–17-year (n = 3) and 18–30-year-old patients (n = 4) was 37.0 and 34.8 points, respectively, whereas in patients aged 31–49 years (n = 6) and 50–60 years (n = 3) was 33 and 30.7 points, respectively (Fig. 5). However, these differences were not statistically significant (p = 0.4060; p = 0.4981, and p = 0.5181, respectively). Of interest, younger patient groups showed better improvement of self-esteem after operative treatment of gynecomastia than older patient groups (Fig. 6; p = 0.1608)
.
Discussion
Throughout this study, we showed that patients with lipomatous gynecomastia show significantly higher rates of recurrence than patients with glandular gynecomastia. Although one might argue that this is mainly due to the higher increase in body weight/BMI units in patients with lipomatous gynecomastia, one has to consider that only one of eight (12.5%) patients with glandular gynecomastia showed recurrence, whereas five of eight patients with lipomatous gynecomastia (62.5%) presented with recurrence at follow-up, with the difference of BMI increase in patients with lipomatous and glandular not being statistically significant. Of interest, even patients with glandular gynecomastia showing a BMI increase of up to 6.7 BMI units (kg/m2) from the time of surgery until the follow-up examination did not show gynecomastia recurrence. However, one has to take into account that all our data were analyzed in a retrospective manner. Thus, to validate our results, further studies are warranted.
The type of surgery performed was liposuction and resection of glandular tissue in each five of the patients (62.5%) who presented with glandular and lipomatous gynecomastia and liposuction only in each three (37.5%) patients (Table 1). Thus, one of the strengths of our study constitutes the fact that the type of surgery performed does not need to be considered as a confounding factor. Furthermore, of the patients presenting with recurrence (n = 6), three were primarily treated with liposuction, whereas in three patients, liposuction and resection of glandular tissue were performed. Thus, each type of surgery performed was associated with equal recurrence rates.
Nevertheless, the combination of liposuction with resection of glandular tissue has been widely described to provide best results [18, 26]. A further advantage of the resection of glandular tissue is the possibility of a histological examination; however, the incidence of malignancy or abnormal pathology associated with gynecomastia tissue in the adolescent male is extremely low [27].
Regarding patient satisfaction, we found overall good results (84.5% of the maximum score); however, we did not find statistically significant differences in patients with lipomatous gynecomastia compared to patients with glandular gynecomastia, patients with and without recurrence of gynecomastia, patients with and without follow-up surgery due to skin retraction or skin excess, and patients with and without dysesthesia of the nipple areolar complex at the time of follow-up, which indicates that patients were overall content with the operative treatment performed, with minor complications such as skin excess, retracted scars, or even recurrence not altering their level of satisfaction. Of interest, we found that younger patients tend to be more satisfied with the operative treatment than older patient groups, irrespective of the rate of complications or recurrence. This is in contrast to a study conducted by Jaipaul et al., who argue that satisfaction scores of hospital care generally increase until the age of 65–80 and then decline [28].
The fact that throughout our study, adolescents and young adults are generally more content about their surgical treatment and show a better improvement of self-esteem might also be due to the fact that the initial psychological distress caused by the enlargement of their breasts might have been more pronounced when compared to older patients: Gynecomastia has long been known to lead to depression, anxiety, disordered eating, body dissatisfaction, and reduced self-esteem [29]; however, it has only recently been shown that especially in adolescents [1, 10, 11], gynecomastia is an enormous psychological threat to normal self-esteem, social functioning, and sexual identity, with 100% of patients receiving a Diagnostic and Statistical Manual of Mental Disorders-IV diagnosis in a case series of 24 adolescents. Therefore, according to Kinsella et al., future studies examining the postoperative effects on psychological health both with and without psychological treatment might be of great interest [10].
To sum up, we find it important to preoperatively inform the patient about the high recurrence rates after a time period of more than 10 years, especially in lipomatous gynecomastia. However, the second important finding of this study was the fact that the patients’ self-esteem significantly improved throughout the younger patient groups after gynecomastia surgery, which shows that especially adolescents with gynecomastia clearly benefit from operative treatment. Thus, our findings could serve as a helping tool in preoperative patient’s consultation.
Conclusion
Long-term follow-up results showed that recurrence rates are significantly higher in patients with lipomatous gynecomastia than in patients with glandular gynecomastia, with BMI increase in patients with glandular and lipomatous gynecomastia showing no statistically significant differences. Interestingly, we also found that adolescents and young adults tend to present with higher postoperative satisfaction levels than older patients, irrespective of complication and recurrence rates.
References
Lemaine V, Cayci C, Simmons PS, Petty P (2013) Gynecomastia in adolescent males. Semin Plast Surg 27(1):56–61
Braunstein GD (1993) Gynecomastia. N Engl J Med 328(7):490–495
Ma NS, Geffner ME (2008) Gynecomastia in prepubertal and pubertal men. Curr Opin Pediatr 20(4):465–470
Bembo SA, Carlson HE (2004) Gynecomastia: its features, and when and how to treat it. Clevel Clin J Med 71(6):511–517
Kumanov P, Deepinder F, Robeva R, Tomova A, Li J, Agarwal A (2007) Relationship of adolescent gynecomastia with varicocele and somatometric parameters: a cross-sectional study in 6200 healthy boys. J Adolesc Health 41(2):126–131
Nuttall FQ (1979) Gynecomastia as a physical finding in normal men. J Clin Endocrinol Metab 48(2):338–340
Niewoehner CB, Nuttal FQ (1984) Gynecomastia in a hospitalized male population. Am J Med 77(4):633–638
Webster JP (1946) Mastectomy for gynecomastia through a semicircular intra-areolar incision. Ann Surg 124:557–575
Brody SA, Loriaux DL (2003) Epidemic of gynecomastia among haitian refugees: exposure to an environmental antiandrogen. Endocr Pract 9(5):370–375
Kinsella C Jr, Landfair A, Rottgers SA et al (2012) The psychological burden of idiopathic adolescent gynecomastia. Plast Reconstr Surg 129(1):1–7
Nuzzi LC, Cerrato FE, Erickson CR et al (2013) Psychosocial impact of adolescent gynecomastia: a prospective case-control study. Plast Reconstr Surg 131(4):890–896
Treves N (1958) Gynecomastia; the origins of mammary swelling in the male: an analysis of 406 patients with breast hypertrophy, 525 with testicular tumors, and 13 with adrenal neoplasms. Cancer 11(6):1083–1102
Jones DJ, Holt SD, Surtees P, Davison DJ, Coptcoat MJ (1990) A comparison of danazol and placebo in the treatment of adult idiopathic gynaecomastia: results of a prospective study in 55 patients. Ann R Coll Surg Engl 72(5):296–298
Ting AC, Chow LW, Leung YF (2000) Comparison of tamoxifen with danazol in the management of idiopathic gynecomastia. Am Surg 66(1):38–40
Fradet Y, Egerdie B, Andersen M et al (2007) Tamoxifen as prophylaxis for prevention of gynaecomastia and breast pain associated with bicalutamide 150 mg monotherapy in patients with prostate cancer: a randomised, placebo-controlled, dose–response study. Eur Urol 52(1):106–114
Perdona S, Autorino R, De Placido S et al (2005) Efficacy of tamoxifen and radiotherapy for prevention and treatment of gynaecomastia and breast pain caused by bicalutamide in prostate cancer: a randomised controlled trial. Lancet Oncol 6(5):295–300
Di Lorenzo G, Perdona S, De Placido S et al (2005) Gynecomastia and breast pain induced by adjuvant therapy with bicalutamide after radical prostatectomy in patients with prostate cancer: the role of tamoxifen and radiotherapy. J Urol 174(6):2197–2203
Voigt M, Walgenbach KJ, Andree C, Bannasch H, Looden Z, Stark GB (2001) Minimally invasive surgical therapy of gynecomastia: liposuction and exeresis technique. Chirurg 72(10):1190–1195
Wong KY, Malata CM (2014) Conventional versus ultrasound-assisted liposuction in gynaecomastia surgery: a 13-year review. J Plast Reconstr Aesthet Surg 67(7):921–926
Bracaglia R, Fortunato R, Gentileschi S, Seccia A, Farallo E (2004) Our experience with the so-called pull-through technique combined with liposuction for management of gynecomastia. Ann Plast Surg 53(1):22–26
Gingrass MK, Kenkel JM (1999) Comparing ultrasound-assisted lipoplasty with suction-assisted lipoplasty. Clin Plast Surg 26(2):283–288
Graf R, Auersvald A, Damasio RC et al (2003) Ultrasound-assisted liposuction: an analysis of 348 cases. Aesthetic Plast Surg 27(2):146–153
Walgenbach KJ, Riabikhin AW, Galla TJ et al (2001) Effect of ultrasonic assisted lipectomy (UAL) on breast tissue: histological findings. Aesthetic Plast Surg 25(2):85–88
Stark GB, Grandel S, Spilker G (1992) Tissue suction of the male and female breast. Aesthetic Plast Surg 16(4):317–324
Simon BE, Hoffman S, Kahn S (1973) Classification and surgical correction of gynecomastia. Plast Reconstr Surg 51(1):48–52
Fischer S, Hirsch T, Hirche C et al (2014) Surgical treatment of primary gynecomastia in children and adolescents. Pediatr Surg Int 30(6):641–647
Koshy JC, Goldberg JS, Wolfswinkel EM, Ge Y, Heller L (2011) Breast cancer incidence in adolescent males undergoing subcutaneous mastectomy for gynecomastia: Is pathologic examination justified? A retrospective and literature review. Plast Reconstr Surg 127(1):1–7
Jaipaul CK, Rosenthal GE (2003) Are older patients more satisfied with hospital care than younger patients? J Gen Intern Med 18(1):23–30
Ordaz DL, Thompson JK (2015) Gynecomastia and psychological functioning: a review of the literature. Body Image 15:141–148
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Fricke, A., Lehner, G.M., Stark, G.B. et al. Long-Term Follow-up of Recurrence and Patient Satisfaction After Surgical Treatment of Gynecomastia. Aesth Plast Surg 41, 491–498 (2017). https://doi.org/10.1007/s00266-017-0827-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-017-0827-x