Abstract
Purpose
There is currently no consensus regarding the optimal treatment for stiffness following total knee arthroplasty (TKA). With the increased utilization of value-based models, it is important to determine the most effective treatments that will reduce the need for further intervention and additional expenditure. A systematic review was performed to compare the outcomes of manipulation under anaesthesia (MUA), arthroscopic lysis of adhesions (aLOA), and revision TKA (rTKA) for arthrofibrosis and stiffness following TKA.
Methods
PubMed and MEDLINE databases were reviewed for articles published through October 2020. Studies were included if they reported patient-reported outcome measures (PROMs) following MUA, aLOA, or rTKA. The primary endpoint was PROMs, while secondary outcomes included range of motion and the percentage of patients who pursued further treatment for stiffness.
Results
A total of 40 studies were included: 21 on rTKA, 7 on aLOA, and 14 on MUA. The mean or median post-operative arc ROM was > 90° in 6/20 (30%) rTKA, 5/7 (71%) aLOA, and 7/10 (70%) MUA studies. Post-operative Knee Society (KSS) clinical and functional scores were the greatest in patients who underwent MUA and aLOA. As many as 43% of rTKA patients required further care compared to 25% of aLOA and 17% of MUA patients.
Conclusion
Stiffness following TKA remains a challenging condition to treat. Nonetheless, current evidence suggests that patients who undergo rTKA have poorer clinical outcomes and a greater need for further treatment compared to patients who undergo MUA or aLOA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Arthrofibrosis, one of the most common complications following total knee arthroplasty (TKA), is a debilitating condition that arises due to excessive scar tissue formation in a joint following injury or trauma [1,2,3,4]. With an occurrence of 1.3–19.8% [5, 6], the inconsistency regarding the definition of arthrofibrosis, especially with respect to flexion and/or extension loss, likely explains the wide range in the reported incidence [3, 5, 7,8,9]. In the USA, arthrofibrosis and stiffness account for 28% of 90-day hospital readmissions following TKA and up to 10% of revisions within years [10, 11].
Risk factors for arthrofibrosis and stiffness following TKA include genetics, low pre-operative range of motion (ROM), complexity of surgery, history of prior surgery, immobilization, and poor motivation during the rehabilitation process [12]. In general, treatment for arthrofibrosis and stiffness is initiated with intensive physical therapy, with or without bracing, and complemented with a multimodal pain regimen until 12 weeks post-operatively [12, 13]. If stiffness persists, manipulation under anesthesia (MUA) is performed between eight and 12 weeks post-op, following which, arthroscopic lysis of adhesions (aLOA) is most commonly performed [8, 13]. Failure of these interventions may warrant revision TKA (rTKA), depending on the patients’ functional requirements. Nevertheless, current literature suggests that the improvements in ROM, pain, and function are only favourable for a select few rTKA patients [14,15,16]. The challenges of treating stiffness and arthrofibrosis have spurred investigation into novel therapies and peri-operative protocols such as low-dose irradiation as a supplement to rTKA [17], as well as the use of continuous passive motion following primary TKA [18]. In the current era of value-based healthcare, there is a growing need to elucidate the most effective and cost-efficient treatment that optimizes clinical outcomes for patients.
The purpose of this systematic review was to compare the functional outcomes of MUA, aLOA, and rTKA for the treatment of arthrofibrosis and stiffness after primary TKA.
Materials and methods
Search methodology
Two databases from the US National Library of Medicine, PubMed and Ovid MEDLINE, were queried in accordance with PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) statement guidelines for all articles that were published prior to October 30, 2020. Four different search terms were utilized to screen for articles: ((total knee arthroplasty) AND (stiffness) OR (arthrofibrosis)), (manipulation under anaesthesia) AND (total knee arthroplasty), and (lysis of adhesions) OR (arthrolysis) and (total knee arthroplasty). Reference lists from each study and related citations from each search engine were explored for additional eligible studies to ensure that no studies were missed after the initial database query. Studies were then screened by two independent reviewers (AH, GG) for eligibility based on the title and abstract. The full text of studies that were deemed to meet the inclusion criteria were reviewed, after which only those that were eligible were included in the analysis. Disagreements were resolved by consensus, and by a third reviewer, if needed.
Inclusion and exclusion criteria
Articles were included if they involved the treatment of arthrofibrosis and/or stiffness following primary TKA and included patient-reported outcome measures (PROMs), ROM values, and the prevalence of treatment success/failure. The rate of treatment success/failure corresponded to the percentage of patients who experienced an increase/decrease in ROM that exceeded a threshold defined in each individual study, as well as the percentage of patients who pursued further treatment for arthrofibrosis. rTKA was defined to include the removal of at least one component from the index procedure (e.g., isolated polyethylene tibial insert exchange (IPTIE)). Only the most recent publication was included if a study published several interim results. Studies were excluded if they did not report the abovementioned outcome measures or clearly define the group the outcomes belonged to. Case reports, reviews, commentary pieces, and studies that were not available in English were also excluded.
Data extraction
All information and outcomes of interest, including author, date of publication, study design, number of patients, treatment modalities, length of follow-up, and PROMs, were recorded on a study-specific data extraction sheet. The primary outcome was PROMs after surgery with secondary outcomes including improvement in ROM and prevalence of treatment success as defined by the article.
Quality assessment
The level of evidence was determined using the Oxford Center for Evidence-Based Medicine Levels of Evidence. Assessment of quality for the included studies was performed by two of the authors (AH, GG) and scored in accordance with the methodological index for non-randomized studies (MINORS) instrument, a valid and reliable tool for study quality assessment [19]. The MINORS instrument is made of 8 and 12 items for non-comparative studies and comparative studies, respectively, with item scores of 0 (not reported), 1 (reported but inadequate), and 2 (reported and adequate). Non-comparative studies and comparative studies can achieve maximum scores of 16 and 24, respectively.
Results
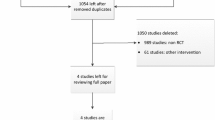
In total, 2,035 articles were initially identified in the database review, and an additional 220 articles were found in relevant systematic reviews and meta-analyses (Fig. 1). Forty articles were included in this study after screening full texts, 16 with a level of evidence (LOE) of III and 24 with a LOE of IV. No level I or II studies were found in the literature. Two of the 40 studies were considered to be of moderate quality, while the 38 other studies were considered to be of poor quality (Table 1).
Revision total knee arthroplasty
In the 21 studies, the mean time to surgery was 1.81 (95% CI (1.29–2.34)) years, and the average follow-up was 3.86 (95% CI (3.41–4.32)) years. Between 15 and 73% of patients underwent some form of treatment before rTKA, although this was only reported in seven studies [3, 15, 16, 31, 40, 48, 49]. Demographics, definitions of stiffness used, and indication of treatment are summarized in Table 2.
rTKA improved arc ROM in all the included studies, with average ROM increasing from 54.60° (95% CI (46.85–62.34°)) to 82.92° (95% CI (78.21–87.62°))—an increase of 28.32°. However, the mean or median post-op arc ROM remained below 90° in 14 of 20 studies [3, 16, 20, 24, 27, 30, 36, 39, 47,48,49,50,51, 54]. Three of the four studies that reported pre-operative and post-operative Knee Society [56] Pain (KSSP) scores showed improvement after surgery [16, 39, 49]. All studies that reported KSS clinical scores (KSSC) or KSS functional scores (KSSF) showed improvement over time but only one reported excellent KSSF, defined as a score > 70 [56].
Two publications compared the outcomes of IPTIE to full rTKA [20, 47] (Table 3). Patients who underwent IPTIE had greater post-operative ROM, flexion, and clinical outcomes than those who underwent complete revision [47]. Another study found that in patients with idiopathic arthrofibrosis, IPTIE leads to greater improvement in ROM and flexion with lower revision rates compared to complete revision. Idiopathic arthrofibrosis was defined as a painful limitation in knee ROM without an underlying etiology. For patients with non-idiopathic arthrofibrosis, complete revision was a better option as patients had lower pain but equivalent values of post-operative ROM compared to those who underwent IPTIE. However, no other studies distinguished between rTKA performed for idiopathic and non-idiopathic causes of stiffness.
Two studies [26, 27] compared the outcomes of patients who underwent rTKA using either a rotating-hinge (RH) device or a traditional constrained condylar device (CC) (Table 4). rTKA patients with a RH device experienced a greater increase in arc ROM. While one study [27] showed that patients with a RH rTKA fared better than those with non-RH TKA in terms of KSS, the report by Bingham et al. [26] contrasted these findings, suggesting that non-RH patients fared better in all outcome measures.
In the twelve rTKA studies that reported the percentage of patients who experienced an improvement in ROM, four studies [15, 26, 50, 54] found that more than 10% of patients did not experience an improvement in ROM, while eight studies reported that 0–6.5% of patients did not experience improvement (Supplementary Table 1) [5, 31, 36, 39, 40, 48, 49, 51]. Furthermore, 14 of 18 studies reporting the percentage of patients who pursued further treatment for stiffness showed that at least 10% of patients required additional treatment.
Arthroscopic lysis of adhesions
Seven studies that evaluated aLOA for the treatment of stiffness and arthrofibrosis following TKA were included (Table 5). Patients were treated at an average of 1.03 (95% CI (0.77–1.30)) years after primary TKA and were evaluated at an average of 2.26 (95% CI (1.57–2.95)) years after aLOA. The percentage of patients who had failed prior treatment for stiffness was reported in six studies, ranging from 27.3 to 100%, in three studies [38, 45, 55]. All studies reported an increase in arc ROM from an average pre-operative value of 61.97° (95% CI (57.32–66.61°)) to a post-operative average of 101.78° (95% CI (86.97–116.58°)). Only one study reported Oxford Knee Scores [42]. Of the studies that reported pre-operative and post-operative KSS, all demonstrated improvements from baseline [38, 45, 46, 52].
Six studies reported values for the percentage of patients who did not improve with respect to ROM (Supplementary Table 2) [5, 38, 42, 46, 52, 55]. Four of 6 studies reported that all patients had an increase from their pre-operative arc ROM [5, 38, 52, 55]. Two studies reported that 4.5% and 5.6% of patients did not have an improvement in arc ROM [42, 46]. Four studies analyzed the percentage of patients who pursued further treatment for stiffness, with three of those reporting 0% and one reporting 25% (2 of 8 patients) [5, 40, 47, 54].
Manipulation under anaesthesia
Fourteen studies evaluated the outcomes of MUA. The average time to surgery was 0.24 (95% CI (0.14–0.33)) years with an average follow-up of 4.70 (95% CI (3.12–6.28)) years. The average pre-operative ROM was 78.69° (95% CI (64.14–89.23°)), and this increased to an average of 99.65° (95% CI (91.79–107.50°))—an increase of 20.97°. In six of the ten studies that reported post-operative ROM, the average value was greater than 100° [5, 22, 25, 34, 35, 43], and all studies that recorded the post-operative arc ROM showed means or medians of at least 80° (Table 6). Three studies reported both pre-operative and post-operative KSSP, of which, all three showed improvement [25, 37, 44]. In addition, all studies that reported pre-operative and post-operative KSSC and KSSF showed improvement at final follow-up [22, 25, 35, 37].
Only one study compared patients who underwent MUA with or without a glucocorticoid adjunct (Table 7) [43]. Sub-analysis showed that patients who received this adjunct better retained the gains in ROM at 2-year follow-up despite achieving equivalent ROM during MUA.
Four studies reported the percentage of patients who did not experience an improvement in arc ROM (Supplementary Table 3) [5, 21, 34, 43], three [21, 34, 43] of which reported values less than 10%, with one study [5] reporting 15.2%. Five of seven studies found that less than 10% of patients needed to seek additional treatment for stiffness [33, 35, 37, 43, 44], with two studies reporting that at least 15% of patients had to undergo further treatment [21, 25].
Discussion
Stiffness following TKA is a challenging complication to treat. Multiple definitions of stiffness have been proposed, and the indications for treatment are not uniform [12]. This problem is further compounded by patients who perceive a limitation in knee ROM and are dissatisfied with their knee replacement but who nonetheless do not fit the established criteria for stiffness.
Our findings suggest that rTKA for stiffness and arthrofibrosis, even in the absence of component malposition, leads to inferior clinical outcomes and range of motion compared to MUA and aLOA. A greater percentage of patients who underwent rTKA needed to undergo further treatment for stiffness and arthrofibrosis, with figures reaching up to 42.9% [50]. While the need for additional treatment was greatest for rTKA patients, three of 4 aLOA studies reported a 0% incidence of patients requiring further treatment, while another reported an incidence of 25% [38]. The need for further treatment was also lower in MUA, with most studies reporting values less than 10% [25, 33, 35, 37, 43, 44]. Nonetheless, the reduced incidence of secondary surgery after MUA or aLOA may not indicate treatment success. It could instead possibly suggest a sense of realistic futility by the patient and/or the care team with the prospects of rTKA.
Analysis of KSSP showed that the three different procedures provided similar levels of pain relief following treatment, despite lower overall post-operative KSSC and KSSF after rTKA compared to both MUA and aLOA. While the majority of rTKA studies reported KSSC less than 70, the lowest reported KSSC was 70.7 for MUA and 77 for aLOA. This finding could be attributed to the nature of the procedures—MUA and aLOA preserve the index arthroplasty and bone stock, while rTKA is associated with bone loss during implant removal, precluding optimal fixation of implants [57]. Furthermore, during rTKA for stiffness, constrained condylar (CC) prostheses are often used due to the difficulty in achieving soft tissue balance [58]. As multiple studies having shown that the outcomes of rTKA are inferior to those of primary TKA [59,60,61,62,63], these factors could explain, in part, the more limited knee functionality among patients who undergo rTKA. Nonetheless, the poorer outcomes after rTKA could be indicative of a higher incidence of component malposition or failure of prior procedures such as MUA and aLOA. In other words, it is unclear how many patients in the rTKA had failed prior interventions and thus represented a more intrinsically complicated group.
Patients who underwent aLOA had greater improvement in total arc ROM from baseline compared to patients who underwent rTKA. With the exception of Campbell et al. [55], all the included studies on aLOA reported an increase of least 29° in ROM, whereas patients who underwent MUA had an increase in mean ROM of 21°. While rTKA significantly increased ROM by at least 40° in some studies [5, 27, 40, 49, 51], others reported only a modest increase of 4° at follow-up [24]. Improvement in mean ROM across all rTKA studies was 28°, and a subgroup analysis of 5 studies [20, 27, 39, 50, 51] that specified the indication for revision showed an increase in mean ROM of 27° in rTKAs performed for idiopathic arthrofibrosis alone. It is important to note that despite the higher pre-operative ROM in MUA compared to rTKA patients (79° vs. 55°), MUA patients had a similar, albeit slightly smaller increase in mean ROM (21°) compared to patients who underwent rTKA for idiopathic arthrofibrosis (27°) [20, 27, 39, 50, 51] (Table 8).
It has been reported that idiopathic stiffness rTKA patients have worse outcomes than non-idiopathic stiffness rTKA patients [22]. Although the distinction between idiopathic and non-idiopathic stiffness was not made in most studies, one study by Xiong et al. suggested that IPTIE may be more efficacious for these patients compared to complete rTKA, as IPTIE patients reported greater improvement in ROM and flexion with lower rates of revision [22]. However, approximately 17% of IPTIE patients with idiopathic arthrofibrosis still required further treatment, higher than reported figures for MUA and aLOA.
In rTKA, implant choice may also influence treatment outcomes. RH prostheses do not rely on ligamentous or soft tissue balancing for stability, allowing for the release of collateral ligaments and posterior capsule as well as elevation of the joint-line [26]. Patients who undergo rTKA with a RH prosthesis may experience less pain, better knee function, and greater improvement in extension and flexion compared to those who underwent rTKA with CC prostheses [26, 27]. Despite these benefits, patients who undergo rTKA with a RH device are at greater risk of implant failure and re-revision; hence, the trade-offs between ROM and implant durability should be evaluated and tailored to the needs of the patient [26].
Few of the included studies investigated the impact of timing from the index TKA on the outcomes of rTKA or aLOA. Mont et al. reported that patients who underwent aLOA at less than one year post-op had higher gains in ROM than those who underwent aLOA at greater than 1 year post-op [46]. One study found no difference in flexion, extension, and KSS gains in patients who underwent rTKA before (n=22) or after two years post-op (n=24) [33]. In contrast, Donaldson et al. reported that patients who underwent rTKA before two years post-op had superior improvement in ROM, and outcomes were reported [3]. However, the authors suggested that these results be interpreted with caution due to the small sample size and heterogeneity of the study population [3]. Nonetheless, further studies evaluating the effect of timing on the outcomes of rTKA for stiffness are warranted.
The timing of MUA is another important consideration that has been shown to influence the outcome of treatment. MUAs performed later in the post-operative period need to overcome a greater degree of fibrotic [5]. Several studies have shown improved function and ROM in MUAs performed before 12 weeks post-op compared to those performed after 12 weeks post-op [32, 64]. Further, of the included studies in this systematic review, only one compared the outcomes of MUA with and without a glucocorticoid adjunct. Despite achieving similar ROM during manipulation, MUA patients who received a glucocorticoid adjunct better retained the gains in ROM and had higher final ROM at two years (111° vs. 92°) [43]. Further studies are needed to confirm these clinical benefits in a larger cohort and explore the mechanisms behind the synergistic effect of steroid treatment.
The advent of value-based models has increased the pressure on healthcare systems to provide high-quality and cost-efficient care. As of 2018, the inpatient National Average Medicare CMS payment for performing rTKA was $17,115.36, while the average outpatient costs for MUA and aLOA were $1209 and $2041, respectively. Future cost-effectiveness studies should be performed to directly compare the three options.
There were several limitations of our study. This systematic review only contained studies with a LOE of III and IV, likely resulting in cohorts that were unmatched in terms of demographics, aetiologies, indications, and other confounding variables such as time from TKA, prior surgeries, procedural techniques, and peri-operative protocols. Furthermore, patients in the three cohorts varied with respect to pre-operative KSSF and KSSC (Table 9). We also could not include studies that evaluated the efficacy of physical therapy as none of these studies analyzed PROMs, which was our primary endpoint. Finally, it is unclear whether patients in the rTKA group were similar to those in the other cohorts, as patients who underwent rTKA presented with significantly lower pre-operative ROM and at a significantly longer time following the index surgery. The extent of component malalignment, inaccurate implant sizing, or instability is poorly reported in the literature, and thus, their incidence in each group also remains unknown. Hence, it is uncertain how these factors could have influenced the results of each treatment modality. Furthermore, given the vagueries in the literature, our study could not elucidate potential differences for either MUA or rTKA done for idiopathic arthrofibrosis alone or with implant malposition. Nevertheless, we believe that the findings of this study still provide a valuable synthesis of the literature to guide clinical practice.
Conclusion
Manipulation under anesthesia (MUA) and arthroscopic lysis of adhesions (aLOA) patients had superior clinical outcomes, knee functionality, and range of motion after intervention compared to patients who underwent revision total knee arthroplasty (rTKA). As this was a systematic review of studies with LOE III and IV, additional prospective randomized studies are warranted to elucidate any differences among these treatment modalities. Future studies should also compare the cost-effectiveness of these treatment options, especially given the greater cost and unpredictable results of rTKA.
Data availability
N/A
References
Sanders TL, Kremers HM, Bryan AJ, Kremers WK, Stuart MJ, Krych AJ (2017) Procedural intervention for arthrofibrosis after ACL reconstruction: trends over two decades. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-015-3799-x
Parvataneni HK, Shah VP, Howard H, Cole N, Ranawat AS, Ranawat CS (2007) Controlling pain after total hip and knee arthroplasty using a multimodal protocol with local periarticular injections. A prospective randomized study. J Arthroplasty. https://doi.org/10.1016/j.arth.2007.03.034
Donaldson JR, Tudor F, Gollish J (2016) Revision surgery for the stiff total knee arthroplasty. Bone Joint J. https://doi.org/10.1302/0301-620X.98B5.35969
Vezeridis PS, Goel DP, Shah AA, Sung SY, Warner JJP (2010) Postarthroscopic arthrofibrosis of the shoulder. Sports Med Arthrosc Rev. https://doi.org/10.1097/JSA.0b013e3181ec84a5
Yercan HS, Sugun TS, Bussiere C, Ait Si Selmi T, Davies A, Neyret P (2006) Stiffness after total knee arthroplasty: Prevalence, management and outcomes. Knee. https://doi.org/10.1016/j.knee.2005.10.001
Malahias MA, Birch GA, Zhong H et al (2020) Postoperative serum cytokine levels are associated with early stiffness after total knee arthroplasty: a prospective cohort study. J Arthroplasty. https://doi.org/10.1016/j.arth.2020.02.046
Manrique J, Gomez MM, Parvizi J (2015) Stiffness after total knee arthroplasty. J Knee Surg. https://doi.org/10.1055/s-0034-1396079
Kalson NS, Borthwick LA, Mann DA, Deehan DJ (2016) International consensus on the definition and classification of fibrosis of the knee joint. Bone Joint J. https://doi.org/10.1302/0301-620X.98B10.37957
Desai AS, Karmegam A, Dramis A, Board TN, Raut V (2014) Manipulation for stiffness following total knee arthroplasty: when and how often to do it? Eur J Orthop Surg Traumatol. https://doi.org/10.1007/s00590-013-1387-7
Schairer WW, Vail TP, Bozic KJ (2014) What are the rates and causes of hospital readmission after total knee arthroplasty? Knee. In: Clinical Orthopaedics and Related Research. https://doi.org/10.1007/s11999-013-3030-7
Schroer WC, Berend KR, Lombardi AV et al (2013) Why are total knees failing today? Etiology of total knee revision in 2010 and 2011. J Arthroplasty. https://doi.org/10.1016/j.arth.2013.04.056
Cheuy VA, Foran JRH, Paxton RJ, Bade MJ, Zeni JA, Stevens-Lapsley JE (2017) Arthrofibrosis associated with total knee arthroplasty. J Arthroplasty. https://doi.org/10.1016/j.arth.2017.02.005
Bong MR, Di Cesare PE (2004) Stiffness after total knee arthroplasty. J Am Acad Orthop Surg. https://doi.org/10.5435/00124635-200405000-00004
Cohen JS, Gu A, Lopez NS, Park MS, Fehring KA, Sculco PK (2018) Efficacy of revision surgery for the treatment of stiffness after total knee arthroplasty: a systematic review. J Arthroplasty. https://doi.org/10.1016/j.arth.2018.04.036
Moya-Angeler J, Bas MA, Cooper HJ, Hepinstall MS, Rodriguez JA, Scuderi GR (2017) Revision arthroplasty for the management of stiffness after primary TKA. J Arthroplasty. https://doi.org/10.1016/j.arth.2017.01.010
Kim J, Nelson CL, Lotke PA (2004) Stiffness after total knee arthroplasty: prevalence of the complication and outcomes of revision. J Bone Jt Surg - Ser A. https://doi.org/10.2106/00004623-200407000-00017
Farid YR, Thakral R, Finn HA (2013) Low-dose irradiation and constrained revision for severe, idiopathic, arthrofibrosis following total knee arthroplasty. J Arthroplasty 28(8):1314–1320. https://doi.org/10.1016/j.arth.2012.11.009
Harvey LA, Brosseau L, Herbert RD (2014) Continuous passive motion following total knee arthroplasty in people with arthritis. Cochrane Database Syst Rev 2014(2). https://doi.org/10.1002/14651858.CD004260.pub3
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (Minors): development and validation of a new instrument. ANZ J Surg. https://doi.org/10.1046/j.1445-2197.2003.02748.x
Xiong L, Klemt C, Yin J, Tirumala V, Kwon YM (2021) Outcome of revision surgery for the idiopathic stiff total knee arthroplasty. J Arthroplasty. https://doi.org/10.1016/j.arth.2020.09.005
Randsborg PH, Tajet J, Negård H, Røtterud JH (2020) Manipulation under anesthesia for stiffness of the knee joint after total knee replacement. Arthroplast Today. https://doi.org/10.1016/j.artd.2020.05.019
Boo HC, Yeo SJ, Chong HC (2020) Manipulation under anaesthesia for patient reported stiffness after total knee arthroplasty in an Asian population. Malays Orthop J. https://doi.org/10.5704/MOJ.2003.009
Yao D, Bruns F, Ettinger et al (2020) Manipulation under anesthesia as a therapy option for postoperative knee stiffness: a retrospective matched-pair analysis. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-020-03381-y
van Rensch PJH, Hannink G, Heesterbeek PJC, Wymenga AB, van Hellemondt GG (2020) Long-term outcome following revision total knee arthroplasty is associated with indication for revision. J Arthroplasty. https://doi.org/10.1016/j.arth.2020.01.053
Crawford DA, Adams JB, Morris MJ, Berend KR, Lombardi AV (2021) Manipulation under anesthesia after knee arthroplasty is associated with worse long-term clinical outcomes and survivorship. J Knee Surg. https://doi.org/10.1055/s-0039-1700569
Bingham JS, Bukowski BR, Wyles CC, Pareek A, Berry DJ, Abdel MP (2019) Rotating-hinge revision total knee arthroplasty for treatment of severe arthrofibrosis. J Arthroplasty. https://doi.org/10.1016/j.arth.2019.01.072
Hermans K, Vandenneucker H, Truijen J, Oosterbosch J, Bellemans J (2019) Hinged versus CCK revision arthroplasty for the stiff total knee. Knee. https://doi.org/10.1016/j.knee.2018.10.012
van Rensch PJH, Heesterbeek PJC, Hannink G, van Hellemondt GG, Wymenga AB (2019) Improved clinical outcomes after revision arthroplasty with a hinged implant for severely stiff total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-018-5235-5
Cartwright-Terry M, Cohen DR, Polydoros F, Davidson JS, Santini AJA (2018) Manipulation under anaesthetic following total knee arthroplasty: Predicting stiffness and outcome. J Orthop Surg. https://doi.org/10.1177/2309499018802971
Hug KT, Amanatullah DF, Huddleston JI, Maloney WJ, Goodman SB (2018) Protocol-driven revision for stiffness after total knee arthroplasty improves motion and clinical outcomes. J Arthroplasty. https://doi.org/10.1016/j.arth.2018.05.013
Rutherford RW, Jennings JM, Levy DL, Parisi TJ, Martin JR, Dennis DA (2018) Revision total knee arthroplasty for arthrofibrosis. J Arthroplasty. https://doi.org/10.1016/j.arth.2018.03.037
Filho PGT de S, Chisté YL, e Albuquerque RSP, Cobra HA de AB, Barretto JM, Cavanellas NT (2017) Late evaluation of patients undergoing manipulation of the knee after total arthroplasty. Acta Ortop Bras. https://doi.org/10.1590/1413-785220172506165770
Pierce TP, Issa K, Festa A, Scillia AJ, McInerney VK, Mont MA (2017) Does manipulation under anesthesia increase the risk of revision total knee arthroplasty? A matched case control study. J Knee Surg. https://doi.org/10.1055/s-0037-1598040
Yoo JH, Oh JC, Oh HC, Park SH (2015) Manipulation under anesthesia for stiffness after total knee arthroplasty. Knee Surg Relat Res. https://doi.org/10.5792/ksrr.2015.27.4.233
Dzaja I, Vasarhelyi EM, Lanting BA et al (2015) Knee manipulation under anaesthetic following total knee arthroplasty: a matched cohort design. Bone Jt J. https://doi.org/10.1302/0301-620X.97B12.35767
Heesterbeek PJC, Goosen JHM, Schimmel JJP, Defoort KC, van Hellemondt GG, Wymenga AB (2016) Moderate clinical improvement after revision arthroplasty of the severely stiff knee. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-015-3712-7
Issa K, Kapadia BH, Kester M, Khanuja HS, Delanois RE, Mont MA (2014) Clinical, objective, and functional outcomes of manipulation under anesthesia to treat knee stiffness following total knee arthroplasty. J Arthroplasty. https://doi.org/10.1016/j.arth.2013.07.046
Hegazy AM, Elsoufy MA (2011) Outcome of arthroscopic arthrolysis of arthrofibrosis after total knee replacement. Univ Pa Orthop J
Kim GK, Mortazavi SMJ, Parvizi J, Purtill JJ (2012) Revision for stiffness following TKA: a predictable procedure? Knee. https://doi.org/10.1016/j.knee.2011.06.016
Hartman CW, Ting NT, Moric M, Berger RA, Rosenberg AG, Della Valle CJ (2010) Revision total knee arthroplasty for stiffness. J Arthroplasty. https://doi.org/10.1016/j.arth.2010.04.013
Patil N, Lee K, Huddleston JI, Harris AHS, Goodman SB (2010) Aseptic versus septic revision total knee arthroplasty: patient satisfaction, outcome and quality of life improvement. Knee. https://doi.org/10.1016/j.knee.2009.09.001
Arbuthnot JE, Brink RB (2010) Arthroscopic arthrolysis for the treatment of stiffness after total knee replacement gives moderate improvements in range of motion and functional knee scores. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-009-0878-x
Sharma V, Maheshwari A, Tsailas P, Ranawat A, Ranawat C (2008) The results of knee manipulation for stiffness after total knee arthroplasty with or without an intra-articular steroid injection. Indian J Orthop. https://doi.org/10.4103/0019-5413.41855
Keating EM, Ritter MA, Harty LD et al (2007) Manipulation after total knee arthroplasty. J Bone Jt Surg - Ser A. https://doi.org/10.2106/JBJS.E.00205
Jerosch J, Aldawoudy AM (2007) Arthroscopic treatment of patients with moderate arthrofibrosis after total knee replacement. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-006-0099-5
Mont MA, Seyler TM, Marulanda GA, Delanois RE, Bhave A (2006) Surgical treatment and customized rehabilitation for stiff knee arthroplasties. Clin Orthop Relat Res. https://doi.org/10.1097/01.blo.0000214419.36959.8c
Keeney JA, Clohisy JC, Curry M, Maloney WJ (2005) Revision total knee arthroplasty for restricted motion. Clin Orthop Relat Res. https://doi.org/10.1097/01.blo.0000185312.43955.c8
Haidukewych GJ, Jacofsky DJ, Pagnano MW, Trousdale RT (2005) Functional results after revision of well-fixed components for stiffness after primary total knee arthroplasty. J Arthroplasty. https://doi.org/10.1016/j.arth.2004.09.057
Christensen CP, Crawford JJ, Olin MD, Vail TP (2002) Revision of the stiff total knee arthroplasty. J Arthroplasty. https://doi.org/10.1054/arth.2002.32105
Babis GC, Trousdale RT, Pagnano MW, Morrey BF (2001) Poor outcomes of isolated tibial insert exchange and arthrolysis for the management of stiffness following total knee arthroplasty. J Bone Jt Surg - Ser A. https://doi.org/10.2106/00004623-200110000-00012
Ries MD, Badalamente M (2000) Arthrofibrosis after total knee arthroplasty. Clin Orthop. https://doi.org/10.1097/00003086-200011000-00024
Williams RJ, Westrich GH, Siegel J, Windsor RE (1996) Arthroscopic release of the posterior cruciate ligament for stiff total knee arthroplasty. Clin Orthop Relat Res. https://doi.org/10.1097/00003086-199610000-00026
Daluga D, Lombardi AV, Mallory TH, Vaughn BK (1991) Knee manipulation following total knee arthroplasty: Analysis of prognostic variables. J Arthroplasty. https://doi.org/10.1016/S0883-5403(11)80006-9
Nicholls DW, Dorr LD (1990) Revision surgery for stiff total knee arthroplasty. J Arthroplasty. https://doi.org/10.1016/S0883-5403(08)80029-0
Campbell ED (1987) Arthroscopy in total knee replacements. Arthroscopy. https://doi.org/10.1016/S0749-8063(87)80007-5
Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the knee society clinical rating system. Clin Orthop Relat Res. https://doi.org/10.1097/00003086-198911000-00004
Rosso F, Cottino U, Dettoni F, Bruzzone M, Bonasia DE, Rossi R (2019) Revision total knee arthroplasty (TKA): mid-term outcomes and bone loss/quality evaluation and treatment. J Orthop Surg Res. https://doi.org/10.1186/s13018-019-1328-1
Sanz-Ruiz P, Villanueva-Martínez M, Matas-Diez JA, Vaquero-Martín J (2015) Revision TKA with a condylar constrained prosthesis using metaphyseal and surface cementation: a minimum 6-year follow-up analysis. BMC Musculoskelet Disord. https://doi.org/10.1186/s12891-015-0485-6
Greidanus NV, Peterson RC, Masri BA, Garbuz DS (2011) Quality of life outcomes in revision versus primary total knee arthroplasty. J Arthroplasty. https://doi.org/10.1016/j.arth.2010.04.026
Stirling P, Middleton SD, Brenkel PJW IJ (2020) Revision total knee arthroplasty versus primary total knee arthroplasty a matched cohort study. Bone Jt Open. https://doi.org/10.1302/2633-1462.13.BJO-2019-0001.R1
Hardeman F, Londers J, Favril A, Witvrouw E, Bellemans J, Victor J (2012) Predisposing factors which are relevant for the clinical outcome after revision total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-011-1624-8
Kannan A, O’Connell RS, Kalore N, Curtin BM, Hull JR, Jiranek WA (2015) Revision TKA for flexion instability improves patient reported outcomes. J Arthroplasty. https://doi.org/10.1016/j.arth.2014.12.010
Scott CEH, Turnbull GS, Powell-Bowns MFR, MacDonald DJ, Breusch SJ (2018) Activity levels and return to work after revision total hip and knee arthroplasty in patients under 65 years of age. Bone Jt J. https://doi.org/10.1302/0301-620X.100B8.BJJ-2017-1557.R2
Issa K, Banerjee S, Kester MA, Khanuja HS, Delanois RE, Mont MA (2014) The effect of timing of manipulation under anesthesia to improve range of motion and functional outcomes following total knee arthroplasty. J Bone Jt Surg - Am Vol 96(16):1349–1357. https://doi.org/10.2106/JBJS.M.00899
Author information
Authors and Affiliations
Contributions
AH: data collection, analysis, manuscript writing. GSG: data collection, analysis, manuscript writing. YAF: data collection, analysis, manuscript review and editing. MTT: data collection, analysis, manuscript review and editing. JHL: data collection, analysis, manuscript review and editing.
Corresponding author
Ethics declarations
Ethics approval
Review by an institutional review board was not required for this study.
Consent to participate
N/A
Consent for publication
N/A
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This work was performed at Rothman Orthopaedic Institute in Philadelphia, PA.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Haffar, A., Goh, G.S., Fillingham, Y.A. et al. Treatment of arthrofibrosis and stiffness after total knee arthroplasty: an updated review of the literature. International Orthopaedics (SICOT) 46, 1253–1279 (2022). https://doi.org/10.1007/s00264-022-05344-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-022-05344-x