Abstract
Background
The management of acetabular fractures, which are severe injuries and often complex, is difficult and costly especially for poor and developing African countries.
Aim
To analyze and evaluate the functional and the radiological outcome of patients with acetabular fracture treated with open reduction and internal fixation.
Materials and methods
It is a retrospective study on 24 patients treated with ORIF and followed up in the Trauma Orthopedic Surgery Department of the Military Hospital of Moulay Ismail of Meknès (MHMIM) between January 2014 and December 2019. The average follow-up duration was 35 months (range: 9–81 months). The functional and radiographic outcomes and complication were considered as the main facts in this study.
Results
Twenty-four patients (male: 18, female: 6) with average age 38 years (range: 16 to 65 years) were operated for acetabular fracture. With Matta criteria use for assessing the radiological outcomes, the anatomical and good reduction was achieved in 79.1% of the patients. The functional results based on the modified Merle d’Aubigne and Postel criteria were judged excellent in 70.83%. Postoperative complications of acetabular fracture such as heterotopic ossification were found in 16%, post-traumatic arthritis in 20%, and avascular necrosis in 12.5% of patients.
Conclusion
As there is a strong correlation between anatomic reduction and clinical outcome, the ORIF constitutes an effective method for treatment of displaced acetabular fracture in young aged patients who are considered as the most vulnerable categories in our continent.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acetabular fractures (AFs) are considered as among the most complex injuries treated by orthopaedic surgeons. These fractures scarcely occurred with an approximate incidence 3/100,000 persons/year [1].
These injuries affect heterogeneous patient groups with different aetiological mechanisms [2]; AFs usually come about in high-energy injuries such as traffic accidents involving young active population who are mostly vulnerable to this form of fractures [2, 3].
The management difficulty of AFs lies within the complicated anatomy of the acetabular region. Thanks to the valuable work of Judet and Letournel that these fractures’ therapy has recently known a substantial evolution with successful results. These pioneers have provided us with a clear understanding of acetabular anatomy with two columns concept, radiology, surgical approaches, reduction techniques, complications, and results [4, 5].
It is worth to note that before the 1964 study, most acetabular fractures were addressed conservatively, but the unsatisfactory results, mainly brought on by displaced fractures especially in young people, have given rise to the increased interest in surgical treatment [4]. Nowadays, the use of the open reduction and internal fixation (ORIF) technique in acetabular fracture ensures the obtaining of a stable, mobile, and painless hip joint.
The purpose of our study is to describe our series, highlight in our context the surgical management of these AFs with ORIF, and finally provide an evaluation of the functional and the radiological outcomes by comparing them with the results of the literature.
Materials and methods
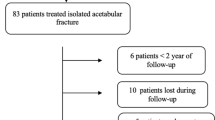
It is about a monocentric retrospective study of 24 patients with acetabular fractures (out of a total of 48 patients) treated with open reduction and osteosynthesis (ORIF ) for various types of acetabular fractures and followed up in the trauma orthopaedic surgery department of the Moulay Ismail Meknès Military Hospital (MIMMH) between January 2014 and December 2019. The average follow-up duration was 35 months (range: 9–81 months). The exclusion criteria were periprosthetic fracture and acetabular fractures treated either orthopaedically or with total hip arthroplasty in first line. Before the operation, an informed consent was obtained from all the patients or from their relatives.
Patients initially were stabilized if required, then pre-operatively evaluated with the physical exam, AP pelvis radiograph, and Judet radiographs of the hip (obturator oblique view and iliac oblique view). A CT scan with thin cuts and 3D reconstructions are also included in the standard protocol for these injuries (Fig. 1) and we adopted the Judet-Letournel classification.
The indications for ORIF were highlighted by the following data:
-
Displaced fracture >2 mm;
-
Unstable fracture dislocation of hip, fracture involving >25% surface of posterior wall;
-
Fracture involving weight bearing area;
-
Retained intra articular fragments;
-
Lack of secondary congruence or loss of congruence of joint on any view.
The baseline characteristics include age, gender, mechanism of injury, fracture pattern, site of fracture, associated injuries, surgical approach, and delay from admission to time of surgery. Moreover, intra-operative complications were extracted from medical records.
Patients were subsequently followed up by radiological and functional assessments in six weeks, 12 weeks, three months, six months, one year, or whenever necessary. In each follow-up session, each patient was clinically and radiographically evaluated. The radiological results were assigned in conformity with the criteria described by Matta whereas the functional evaluation was performed with control forms based on Matta’s modified Merle d’Aubigne and Postel criteria at final check-ups.
Result
The study included six (25%) female patients and 18 (75%) male patients. The average age of the patients was 38 years, ranging from 16 to 55 years. The major causes of acetabular fractures were mainly linked to in-vehicle traffic accidents in 20 (84%) patients, to falls from high places in three (12%), but sport related injury was associated in one patient.
The hip dislocation was present in 11 patients which was reduced at the emergency department, and the skeletal traction was applied with wire passed through the supracondylar region until the effective surgery. However, sciatic nerve symptoms were not present in any patients at the time of presentation. Associated injuries were seen in 20 of the patients (83.33%). Lower extremities injury (70%) was the most common associated injuries (Fig. 2), followed by upper extremities (10%), head injury (10%), and thoracic injury (10%).
Fifteen (62.5%) fractures were simple type, and nine (37.5%) were complex type. Eleven (46%) simple fractures were posterior wall, and four (16.5%) were transverse. Four (16.5%) complex fractures involved transverse posterior wall fractures, two (8%) were T-shaped fractures, one (4.16%) was fractures of both columns, posterior column/posterior wall in one (4.16%), and one (4.16%) was anterior column posterior hemitransverse fractures.
The average period between trauma and surgery was nine (6–15) days. Twenty-two patients were operated through Kocher-Langenbeck approach (Fig. 3), and two patients through the ilioinguinal approach. Fixation was performed with plates in 17 cases (Figs. 2 and 4), screw fixation in four cases, and both of plates and screw in three patients (Table 1).
Post-operative AP pelvis radiograph of case 23 with fixation of posterior wall fracture with contoured 3.5–mm pelvic reconstruction plate. Note associated femoral shaft fracture in contralateral side fixed with locked intramedullary nail
Concerning the immediate complications, a superficial (ilioinguinal) infection developed in one (4.1%) of the 24 patients, and this was treated with dressing and antibiotic therapy. Otherwise, no haemorrhagic, nor nerve injuries, nor deep vein thrombosis were observed in any case.
With the average 35 months as follow-up (range 9–81 months), detailed radiological and functional results are given in Table 2. In 19 (79.1%) cases, excellent-good reduction in five (20.9%) cases, fair-poor reduction was achieved.
Functionally evaluation revealed excellent-good outcomes in 17 (70.8%) patients, moderate outcomes in five (20.83%), and poor outcomes in two (8.3%). The heterotopic ossification was determined in four (16.6%) of the 24 patients (Fig. 5), the avascular necrosis (AVN) was observed in two patients (8.3%) and the post-traumatic arthritis was determined in five (20.83%) hips (Fig. 5 and Table 2).
Complication. a Case 8 with posterior wall fracture fixed with screws and complicated in the final follow-up by heterotopic ossification (Brooker 2) and post-traumatic arthritis. b Case 5 with both column fracture fixed with two plates and complicated in the final follow-up by post-traumatic arthritis
Discussion
In 1964, Robert Judet, Jean Judet, and Émile Letournel published a landmark article allowing a better anatomical understanding of acetabular fracture and thus laying down the principles of surgical treatment [4, 6]. Due to these pioneers and to the development of imaging and the surgical techniques, the results of these fractures have clearly improved [6]. Nowadays ORIF is an outstanding standard broadly used for the displaced AFs.
The AFs are infrequent and their epidemiology in the USA and Europe has been well established, showing comparable bimodal age distributions (the first peak representing young patients sustaining high-energy fractures and the second peak older patients sustaining low-energy osteoporotic/fragility fractures) and declining incidence [7]. Epidemiological analysis of acetabular fracture revealed that the incidence of the acetabular fracture is increasing in developing countries and affecting mainly the young male subject [8]. This fact corresponds and adheres to our series in which the average age was 38 years with predominance of the male sex in 75% of cases. In parallel with the previous reports on emerging countries, our study confirmed that most of the fractures were engendered by high-energy trauma with the rate of 84% mainly caused by road traffic accidents in our studies [7–8].
The classification of acetabular fractures by Letournel identified five elementary patterns and five complex ones [5]. The posterior wall (46%) and transverse posterior wall fractures (16.5%) were respectively two most common fractures in elementary and associated patterns in our papulation. This is similar to what was identified by major previous studies about elementary fractures. But for complex fractures, they were mainly represented by both column fracture in these studies [1, 7, 8]. In contrast, anterior fractures (wall or column) had the most frequency in German and French population; this can be explained by the high average age mentioned in these studies [3, 9].
The timing of surgery has been identified as a factor affecting the outcome and it was nine days as average in our study. The ability to achieve an anatomic reduction in a displaced AFs decreases significantly beyond two weeks. Since the reduction correlates with the functional outcome, it is advisable to proceed early with surgery within the first 14 days [6, 10].
There are various surgical approaches for treatment of displaced AFs and their choice depends upon the surgeon familiarity and the fracture configuration. Selecting the appropriate surgical approach is a key factor to achieve a better anatomical reduction of acetabular and a satisfactory post-operative function. In summary, we used Kocher-Langenbeck for posterior fracture family and ilio-inguinal approach for anterior fracture family. Currently, the modified Stoppa approach is widely used for visualization and the osteosynthesis of the anterior column or the quadrilateral surface. The combination of an anterior and posterior approach or extended ilio-femoral approach should be used for those complex fractures which involved two columns [2, 11].
The most common approach used in our centre was that of Kocher-Langenbeck in about 92% of the patients, probably due to higher frequency of posterior family fractures and to greater familiarity with this approach among our surgeons.
The largest studies from ORIF of AFs, of Letournel [12], Tannast/Matta [13], Mears [14], and others, give 80 to 90% of good and excellent (G-E) results.
In emerging countries such as India and Brazil, Gupta RK [8] and Almedia [15] found respectively 74% and 81% G-E results. Whereas in Africa where studies are extremely rare concerning this pathology, Mahdane [16] and EN Eliezer [17] found respectively 77% and 73.5% of G-E results. While DA et al. [18] were able to obtain 85% of G-E results, this very encouraging rate should be treated with caution given the small number of cases operated on which was seven patients (Table 3).
Our results showed about 70.8% G-E clinical outcomes at minimally one year post-operatively.
Various studies demonstrate that there are certain consensus prognostic indicators for outcomes, whose main factors of poor prognosis are represented by [6, 12]:
-
Patient age > 40
-
Poor fracture reduction (> 3 mm)
-
Multi-fragmentary fractures of the posterior/ anterior wall/tectum
-
Cartilage damage to the femoral head and/or acetabulum
-
Delay to surgery > 15 days.
-
Initial fracture displacement > 20 mm.
In summary, it is an accepted fact and has been clearly demonstrated that the functional results of the displaced AFs correlate strongly with the quality of reduction and that open reduction is the best method to achieve congruity [6, 12].
In our series, the infection rate was 4.1% whether one patient with superficial infection which was well checked by debridement and antibiotic therapy. Based on available data, the incidence of infection is approximately 2–5% [6, 18].
Iatrogenic nerve injury included sciatic nerve, femoral nerve, and lateral cutaneous nerve of thigh are possible complications during acetabular surgery with incidence ranging from 2 to 6% [12, 19, 20]. In this study, no cases with nerve palsy were seen despite the greatest risk for sciatic nerve knowing that the posterior surgical approach was mainly used in our series. To avoid these lesions of the sciatic nerve, we highly observe these precautions: the visualization and the protection of the nerve, the hip extension/knee flexion, and the careful placement of retractors with more attention paid to retractor effect on nerve tension.
Heterotopic ossification (HO) is a common post-operative complication in the surgery of acetabular fractures with a reported incidence of 25 to 80% [6, 18]. The rate of this complication is mostly increased following posterior or extensile approaches. Moreover, it seems that race is an important factor. According to Slone et al., African American patients are considerably more likely to develop severe HO when compared to Caucasian patients [21]. However, no African study has shown the rate of this complication in this population. HO was seen in only four of our patients, who had Brooker type 1 or 2 ossification. None of them needed excision and the routine prescribed prophylaxis with Indomethacin could be the reason for this low incidence.
A meta-analysis reported an overall incidence of AVN of 5.6% in 2010 patients; this AVN occurs more frequently after fractures associated with posterior dislocation with an incidence of around 9.2% [18]. In our series, two patients (8.3%) evolved with AVN and both of them have sustained a posterior dislocation.
The main complication following a AFs is post-traumatic osteoarthritis and it is proportional to the quality of reduction [6, 22]. The incidence of osteoarthritis in our series was 20.83%, which is comparable with Letournel and Giannoudis who reported respectively 19.7% and 19.1% [12, 18].
The main limitations of our study are mainly linked to its retrospective nature and the restricted number of patients. Therefore, we share the same constraints with the scarce series from our continent. It is worth to mention that in the twenty-first century [23], traffic accidents occured in majority of developping African countries, are assessed to be the highest in the world among the young population because of the increase of motorization, roads infrastructure expansion and especially due to poor or absence of traffic law enforcements. Moreover, due to lack of driving attitudes and law enforcements, road traffic accidents are assessed to be the highest in the world. So, the young population is regularly victim of road traffic crashes with highest mortality rate and thus the risk of AFs [24]. Since, the younger segment of population is more affected, the ORIF is proved to the most suitable treatment for this type of fracture. In the perspective to enhance the treatment rate and achieve the 70 to 80% G-E results of the wide series [6], it is recommended to set up regional reference centers that should be run by specialized surgeons in acetabulum and pelvis trauma surgery so as to boost their experience after operating on a great number of cases which thus enable them to achieve successful outcomes. Moreover, the organization of periodic seminars and master courses, through the current Information and Communications Technology means, has also a significant role in the qualification of regional surgeons during which fruitful experiences can be shared in the management of these complex injuries.
Conclusion
AFs in our continent are roughly due to high velocity injury involving young active adults. Despite the fact that the surgical treatment of these fractures constitutes a challenge for the qualified specialists, the ORIF remains the best treatment for these types of fractures in the attempt to restore the native hip biomechanics with long survivorship. With a view to achieve successful goals in our continent, the efforts should focus on:
-
The upgrading of the orthopaedic surgeon skills and performances;
-
The permanent availability of instruments and implants in the surgery department,
-
And the full accessibility to appropriate post-operative rehabilitation services for acetabular surgery.
Code availability
Not applicable
References
Laird A, Keating JF (2005) Acetabular fractures: a 16-year prospective epidemiological study. J Bone Joint Surg (Br) 87(7):969–973
Theodoros H, Tosounidis, Giannoudis PV (2015) What is new in acetabular fracture fixation? Injury, Int J Care Injured 46:2089–2092
Boudissa M, Franconya F, Kerschbaumer G, Ruatti S, Milaire M, Merloz P, Tonetti J (2017) Epidemiology and treatment of acetabular fractures in a level-1 trauma centre: retrospective study of 414 patients over 10 years. Orthopaedics & Traumatology: Surgery & Research 103:335–339
Judet R, Judet J, Letournel É (1964) Fractures of the acetabulum: classification and surgical approaches for open reduction. Preliminary report. J Bone Joint Surg Am 46:1615–1646
Letournel É (1980) Acetabulum fractures: classification and management. Clin Orthop Relat Res 151:81–106
Ziran N, Soles Gillian LS, Matta JM (2019) Outcomes after surgical treatment of acetabular fractures: a review. Patient Saf Surg 13(16):1–19
Mauffrey C, Hao J, Cuellar DO, Herbert B, Chen X, Liu B, Zhang Y, Smith W (2014) The epidemiology and injury patterns of acetabular fractures: are the USA and China comparable? Clin Orthop Relat Res 472(11):3332–3337
Gupta RK, Singh H, Dev B, Kansay R, Gupta P, Garg S (2009) Results of operative treatment of acetabular fractures from the Third World—how local factors affect the outcome. Int Orthop 33:347–352
Ochs BG, Marintschev I, Hoyer H, Rolauffs B, Culemann U, Pohlemann T, Stuby FM (2010) Changes in the treatment of acetabular fractures over 15 years: analysis of 1266 cases treated by the German Pelvic Multicentre Study Group (DAO/DGU). Injury. 41(8):839–851
Dailey SK, Phillips CT, Radley JM, Archdeacon MT (2016) Achieving anatomic acetabular fracture reduction-when is the best time to operate? J Orthop Trauma 30(8):426–431
Küper MA, Konrads C, Trulson A, Bahrs C, Stöckle U, Stuby FM (2020) Complications of surgical approaches for osteosynthesis treatment of acetabular fractures: analysis of pitfalls and how to avoid them. Injury 51:984–990
Letournel E, Judet R (1993) Fracture of the acetabulum, 2nd edn. Springer-Verlag, Berlin
Tannast MM, Najibi SS, Matta JM (2012) Two to twenty-year survivorship of the hip in 810 patients with operatively treated acetabular fractures. J Bone Joint Surg Am 94(17):1559–1567
Mears DC, Velyvis JH, Chang C-P (2003) Displaced acetabular fractures managed operatively: indicators of outcome. Clin Orthop Relat Res 407:173–186
Almedia AGI, Garrido CA, Amaral LEV, Vargas LFL (2011) Prospective study on seventy-six cases of fractured acetabulum with surgical treatment. Rev Bras Ortop 46(5):520–525
Mahdane H, Elghazi A, Shimi M, Elibrahimi A, Elmrini A (2014) Surgical treatment of acetabular fractures: report of 22 cases. Pan Afr Med J 17:123. https://doi.org/10.11604/pamj.2014.17.123.2572
Eliezer EN, Haonga B, Mrita FS, Liu MB, Wu H (2016) Functional outcome and quality of life after surgical management of displaced acetabular fractures in Tanzania. East African Orthopaedic Journal 10(1):16–20
Giannoudis PV, Grotz MRW, Papakostidis C, Dinopoulos H. (2005) Operative treatment of displaced fractures of the acetabulum. A meta-analysis. J Bone Joint Surg (Br).;87-B:p. 2–9.
Middlebrooks ES, Sims SH, Kellam JF et al (1997) Incidence of sciatic nerve injury in operatively treated acetabular fractures without somatosensory evoked potential monitoring. J Orthop Trauma 11(5):327–329
Briffa N, Pearce R, Hill AM, Bircher M (2011) Outcomes of acetabular fracture fixation with ten years’ follow-up. J Bone Joint Surg (Br) 93(2):229–236
Slone HS, Walton ZJ, Daly CA, Chapin RW, Barfield WR, Leddy LR et al (2015) The impact of race on the development of severe heterotopic ossification following acetabular fracture surgery. Injury 46(6):1069–1073
Matta JM, Anderson LM, Epstein HC, Hendricks P (1986) Fractures of the acetabulum. A retrospective analysis. Clin Orthop Relat Res 205:230–240
Goldstone JA. (2019 ) Africa 2050: demographic truth and consequences, Hoover Institution, Governance In An Emerging New World, no. 119
World Health Organization. Global status report on road safety 2015. Geneva:WHO; 2015.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This study was performed in full compliance with the ethics in force in our institution.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
The authors affirm that patients provided informed consent regarding publishing their data and photographs.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cherrad, T., Ouahidi, M., Bennani, M. et al. Outcomes of surgical management regarding acetabular fractures: cases from African countries. International Orthopaedics (SICOT) 46, 29–35 (2022). https://doi.org/10.1007/s00264-021-05024-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-021-05024-2