Abstract
Purpose
To compare the obtained deformity correction and clinical/functional outcomes between patients who underwent total ankle replacement (TAR) with or without a concurrent supramalleolar osteotomy (SMO) to address a varus and/or recurvatum deformity of the distal tibia.
Methods
Data of 23 patients treated with an additional SMO to correct a varus and/or recurvatum deformity of the distal tibia at the time of TAR were prospectively collected. Twenty-three matched patients who underwent TAR only served as controls.
Results
The American Orthopaedic Foot and Ankle Society (AOFAS)-hindfoot scale and pain assessed on a Visual Analogue Scale (VAS) did not significantly differ between the two groups at the final follow-up (AOFAS-hindfoot scale SMO/TAR group = 82 ± 10; TAR group = 82 ± 12; VAS pain SMO/TAR group = 1 (range, 0–4); TAR group = 1 (range, 0–5)). Ankle range of motion (ROM) did not improve in the SMO/TAR group (pre-operative = 27 ± 13 degrees, last follow-up = 30 ± 9 degrees; P = .294), but did improve in the TAR group (pre-operative = 31 ± 14 degrees, last follow-up = 39 ± 14 degrees; P = .049). Two patients who underwent SMO/TAR showed non-union of the tibial osteotomy, and two patients who underwent TAR only suffered from an intra-operative medial malleolar fracture.
Conclusion
An additional SMO during TAR in patients with a varus and/or recurvatum deformity of the distal tibia is not beneficial in most cases and should only be considered in pronounced multiplanar deformities.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In the last two decades, total ankle replacement (TAR) has become a well-accepted treatment option for end-stage ankle osteoarthritis [1,2,3,4,5,6,7]. Recent studies highlighted the impact of appropriate balancing of the ankle joint on radiographic and clinical outcomes following TAR [8,9,10]. In case of malalignment of the prosthesis components, periarticular soft tissue structures can be overused, leading to pain and gait impairment [8,9,10]. To avoid inferior outcomes and early failure after TAR, hindfoot deformities should be properly addressed during prosthesis implantation [8,9,10,11,12].
The role of an additional supramalleolar osteotomy (SMO) to realign deformities at the level of the distal tibia during TAR is poorly understood [12,13,14,15]. Although meticulous addressing of all causes inducing a hindfoot varus has been shown to be necessary in patients with a severe varus deformity, only a few articles reported on the outcome of performing a SMO before TAR to realign the hindfoot [11,12,13,14,15]. To the authors knowledge, there is no data available investigating the outcome in patients suffering of ankle osteoarthritis with a varus and/or recurvatum deformitiy at the level of the ankle joint who underwent SMO and TAR as a one-stage procedure. Possible reasons for the restrained enthusiasm towards performing both procedures in the same operative session could be increased peri-operative risks due to the higher complexity of the operation, increased soft tissue stress, longer operation time, and the risk of delayed or non-union of the osteotomy [14, 15]. In addition, it is unknown whether a combined approach (SMO/TAR) is more effective than TAR only to balance the hindfoot. We hypothesized that patients who underwent SMO/TAR as a one-stage procedure show a better deformity correction on radiographic assessment, a higher increase on the American Orthopaedic Foot and Ankle (AFOAS)-hindfoot scale, better pain relief, and a higher satisfaction score compared with that of patients who underwent TAR only.
The present study aimed to show the advantages as well as disadvantages of performing SMO/TAR as a one-stage procedure. For this, radiographic assessment and clinical/functional outcome measures (AOFAS-hindfoot scale, pain level, satisfaction score, ankle range of motion (ROM)) in patients with a varus and/or a recurvatum deformity of the distal tibia who underwent SMO/TAR were compared with patients suffering of a similar deformity who underwent TAR only.
Materials and methods
Study characteristics and patient demographics
This case-control study was approved by the local ethics committee and conducted according to the Declaration of Helsinki and the Guidelines for Good Clinical Practice. All participants provided informed written consent prior to surgery and participation in the study. Only patients with history of an ankle fracture were considered. Patients with history of a talonavicular and/or subtalar joint fusion were excluded. Also, active smokers or patients with diabetes were not considered. Data of 23 patients (male 12, female 11; mean age 59.9 years, standard deviation (SD) 13.7, range 22.2–72.2) treated with an additional SMO to correct a varus and/or recurvatum deformity of the distal tibia at the time of TAR were prospectively collected. The final cohort included six patients with a varus deformity and five patients with a recurvatum deformity. Twelve patients had a combination of both. The mean follow-up time after surgery was 3.8 (range, 1.8–8.5) years. Twenty-three patients matched using propensity scores estimated by logistic regression (male 16, female 7; mean age 58.2 years; SD 11.9, range 35.3–78.9) out of a consecutive cohort of 1023 patients who underwent TAR between 2002 and 2014 served as controls. The final control cohort included five patients with a varus deformity and two patients with a recurvatum deformity. Sixteen patients had a combination of both. The mean follow-up time after surgery was 3.1 (range 1.9–6.2) years. Baseline characteristics are available in Table 1.
Radiographic and clinical assessment
Radiographic analysis was performed on weight-bearing mortise, lateral, and hindfoot views. Coronal and sagittal alignment of the distal tibia was assessed using the tibial articular surface angle (TAS, normal value 89 ± 3 degrees; Fig. 1a) and lateral distal tibial surface angle (TLS, normal value 83 ± 3 degrees; Fig. 1b) [16]. The hindfoot moment arm (HMA, normal value 10 ± 0 mm; Fig. 1c) was additionally measured to assess the calcaneal deviation from the tibial axis [16]. A varus deformity of the distal tibia was defined as a TAS < 86 degrees, and a recurvatum deformity as a TLS < 80 degrees. Measurements were performed by an orthopaedic surgeon not involved in patient treatment. Previous studies showed satisfactory reliability for measurements used in this study [17,18,19]. Clinical/functional outcomes were assessed by research associates who were not involved in any clinical duties and included the AOFAS-hindfoot scale, Visual Analogue Scale (VAS) for pain (0 points for no pain and 10 points for maximum pain), and ankle range of motion (ROM) measured using a goniometer applied along the lateral border of the leg and foot [20, 21]. In addition, patients were asked about their satisfaction with the obtained result using a 4-point Likert scale (very satisfied, somewhat satisfied, neither satisfied nor dissatisfied, somewhat dissatisfied) according to previously published protocol used for total joint arthroplasty [22].
Assessment of the coronal, sagittal, and hindfoot alignment. a Weight-bearing mortise view of the ankle showing how the medial distal tibial articular surface angle (TAS) was measured. The tibial axis was drawn by bisecting two pairs of points along the tibial shaft cortex, drawn eight and 13 cm proximal to the distal tibial articular surface (before total ankle replacement (TAR))/tibial component (after TAR). b Weight-bearing lateral view. A line connecting the anterior and posterior margin of the distal tibia was drawn. Then, the axis of the tibia was drawn by bisecting two pairs of points along the tibial shaft cortex, drawn eight and 13 cm proximal to the centre of the ankle joint (before TAR)/tibial component (after TAR). The lateral distal tibial surface angle (TLS) was measured. c Weight-bearing hindfoot alignment view showing measurement of the hindfoot moment arm (HMA), which was defined as a horizontal line connecting the lowest point of the calcaneus and the tibial axis
Surgical technique and rehabilitation protocol
The osteotomy was performed at the centre of rotation and angulation (CORA), which was determined on pre-operative weight-bearing radiographs (mortise and lateral view). In case of an intra-articular deformity, the osteotomy was performed slightly above the CORA. Coronal plane correction was achieved by a medial opening wedge osteotomy, which aimed for a TAS of 90 degrees. Sagittal plane correction was achieved by an anterior opening wedge osteotomy, which aimed for a TLS of 85 degrees. SMO was performed using a standard technique according to previously published protocols [16, 23]. After graft insertion (Tutoplast®, Tutogen Medical GmbH, Neunkirchen am Brand, Germany; human tissue processed with Tutoplast® tissue sterilization process), one or two angular stable plates (TIBIAXYS™, Integra LifeSciences, Plainsboro, New Jersey, USA) were used for fixation (Figs. 2 and 3). An additional fibula osteotomy was performed if proper opening of the tibial osteotomy was not possible, or if the fibular length was not appropriate under fluoroscopic control after fixation of the tibia [16, 23]. TAR was performed using a standard technique as described in earlier reports [12]. The HINTEGRA total ankle system (Integra LifeSciences, Plainsboro, New Jersey, USA) was implanted in all patients. During TAR, the lateral and medial gutters were debrided to allow free positioning of the talus within the ankle mortise. Additional surgical steps necessary to balance the ankle (e.g. calcaneal osteotomy) were performed during the same operation (Table 2).
Intra-operative situs of a patient treated with a supramalleolar osteotomy (SMO) followed by total ankle replacement (TAR). a An anterior and medial open wedge osteotomy was performed and secured with two angular stable plates. b Intraoperative situs after the resection cuts of the distal tibia and talus have been performed. c Insertion of the prosthesis
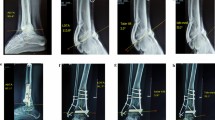
Radiographic assessment of a patient treated with a supramalleolar osteotomy (SMO) followed by total ankle replacement (TAR). a Mortise view before surgery. b Lateral view before surgery. c Mortise view 3 months following surgery. d Lateral view 3 months following surgery. e Mortise view 6 years following surgery. f Lateral view 6 years following surgery. The prosthesis is well-balanced, and the patient satisfied with the obtained result
The post-operative protocol included a short leg splint with the foot in neutral position for the first two to four post-operative days. A stabilizing boot (VACOped, OPED AG, Steinhausen, Switzerland) was used for protection for 8 weeks permitting touch ground weight-bearing (foot can be placed on the ground without weight application) in patients treated with SMO and TAR simultaneously, and full weight-bearing in patients treated with TAR only. The rehabilitation programme (including strengthening and stretching exercises) was initiated once bone healing at the osteotomy site was confirmed radiographically (typically after 8 weeks). Post-operative radiographs were obtained at eight weeks, three months, one year, and annually thereafter. An additional computed tomography (CT) scan was only performed if delayed union of the osteotomy was suspected at the three month follow-up visit.
Statistical analysis
Statistical significance level was set as P lower than .05. Assumption of normality in samples was tested using the Shapiro-Wilk test. If normality was confirmed, variance homogeneity was assessed using the Levene’s test (car package in R), and either an independent Student’s t test (given variance homoscedasticity) or Welch t test (given variance heteroscedasticity) was applied to assess differences between continuous variables [24]. If the assumption of normality was violated, a Kruskal-Wallis test was carried out. Similarity in continuous variables across strata was tested using analysis of variance (ANOVA). The results were reported as mean and standard deviation (SD). Differences between proportions were tested using Fisher’s exact test. The statistical data analysis was performed in R (version 3.4.3) using R Studio (version 1.1.42) [25].
Results
Radiographic and clinical outcomes
Neither the TAS nor the TLS differed significantly between the SMO/TAR and the TAR group pre-operatively or at the last follow-up (Fig. 4a, b). In both groups, the TAS and TLS improved from pre-operative to the last follow-up (either P < 0.001; Fig. 4a, b). HMA did not differ significantly between both groups pre- and post-operatively, and did not significantly improve at the last follow-up (Fig. 4c). No significant difference was evident pre-operatively and at the last follow-up between the SMO/TAR and TAR group for the AOFAS-hindfoot scale (Fig. 5a), and for the VAS for pain (Fig. 5b). While ROM did not significantly increase in the SMO/TAR group, it increased in the TAR group (P = .049; Fig. 5c). In the SMO/TAR group, 19 patients were very satisfied with the obtained results, and three patients were somewhat satisfied. In the TAR group, 20 patients were very satisfied, and two patients somewhat satisfied. Overall, two patients were dissatisfied. One patient underwent revision surgery due to delayed union of the osteotomy (SMO/TAR group). The other patient reported persistent pain in the area of the medial malleolus following an intra-articular malleolar fracture (TAR group). Patient satisfaction did not differ between the SMO/TAR and TAR group (P = .465).
Radiographic outcome measures pre-operative (PreOP) and at the last follow-up (Last FU) of patients who underwent total ankle replacement (TAR) and patients who underwent a supramalleolar osteotomy (SMO) followed by TAR. a Medial distal tibial articular surface angle (TAS). b Lateral distal tibial surface angle (TLS). c Hindfoot moment arm (HMA)
Clinical outcome measures pre-operative (PreOP) and at the last follow-up (Last FU) of patients who underwent total ankle replacement (TAR) and patients who underwent a supramalleolar osteotomy (SMO) followed by TAR. a The American Orthopaedic Foot and Ankle Society (AOFAS)-hindfoot scale. b Pain measured using the Visual Analogue Scale (VAS) did not differ significantly between the two groups. c Range of motion (ROM) at the last follow-up differed significantly between patients treated with TAR and patients treated with SMO followed by TAR
Complications and revision surgery
Intra-operative fracture of the medial malleolus occurred in two patients who underwent TAR only (Table 3). Both fractures were fixed intra-operatively and healed within eight weeks. In total, four patients evidenced delayed wound healing. No revision surgery was necessary for those patients. Cyst formation was evident in three patients of the SMO/TAR group and in five patients of the TAR group. All eight patients were revised either by bone grafting of the cysts (four patients), or component exchange (four patients, Table 3). Arthrofibrosis/impingement occurred more frequently in the SMO/TAR group. Non-union of the supramalleolar osteotomy was found in two patients (Fig. 6); healing occurred in both patients after revision and bone grafting. Hardware removal in the SMO/TAR group was necessary in 13 patients. The reason was local discomfort in all patients.
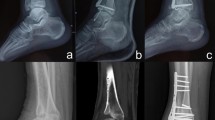
Radiographic assessment of a patient treated with a supramalleolar osteotomy (SMO) followed by total ankle replacement (TAR) who underwent revision surgery due to non-union of the tibial osteotomy. a Mortise view before surgery. b Lateral view before surgery. c Mortise view 6 months following surgery. d Lateral view 6 months following surgery shows secondary dislocation due to non-union of the osteotomy. e Mortise view 2 years following revision surgery. f Lateral view 2 years following revision surgery. The tibial osteotomy healed and the prosthesis is well-balanced
Discussion
The aim of this study was to show the advantages as well as disadvantages of performing SMO and TAR simultaneously in patients with a varus and/or recurvatum deformity of the distal tibia. Radiographic assessment and functional/clinical outcomes were compared with patients with a similar pre-operative deformity who underwent TAR only. The four most relevant findings are (1) radiographic measures did not differ significantly at the last follow-up between the two groups; (2) the ankle ROM did significantly increase in the TAR, but remained similar in the SMO/TAR group; (3) additional soft tissue procedures were more frequently performed in patients who underwent TAR only; and (4) complication and revision rate was similar between the SMO/TAR and the TAR group.
Controversy still exists regarding the indications for TAR in patients with a varus and/or recurvatum deformity. Obviously, the available bone stock of the distal tibia limits adjustments of the tibial cuts during TAR to compensate for coronal and/or sagittal plane deformities [12]. Performing a SMO before TAR aims to transfer the ankle joint under the weight-bearing axis of the tibia, to normalize the direction of the force vector of the triceps, and therefore to restore ankle biomechanics [12, 26]. Restoration of ankle biomechanics prior to TAR possibly reduces the extent of distal tibial resection in a varus and/or recurvatum deformity. This is especially important with regard to the reported 12% rate of metal component revision after 4.3 ± 3 years after TAR in the literature [3]. Revision surgery in TAR likely is even more difficult if the available bone stock is limited. In addition, high tibial resection, which is typically necessary during TAR in severe coronal and/or sagittal plane deformities, may weaken the medial malleolus, possibly leading to medial malleolar fracture.
A lower ankle ROM was evident at the last follow-up in patients treated with SMO/TAR compared with that of patients treated with TAR only. Extensive soft tissue surgery above the ankle may result in a greater amount of scarring of peri-articular structures (e.g. tendons, ligaments). Furthermore, open wedge osteotomies may additionally increase the tension on periarticular soft tissue structures, which can negatively impact on ROM. This may also explain the higher rate of arthrofibrosis and impingement in patients treated with SMO/TAR. Consequently, if SMO/TAR is performed simultaneously, patients should be informed that the ROM likely will not improve post-operatively.
The complication and revision rates were comparable in patients who underwent SMO/TAR and patients treated with TAR only. Although a combined procedure SMO/TAR does extend the operation time, there was no increase in complications. It is important to mention that no deep infection (e.g. infected total ankle) occurred in either group. Furthermore, no component revision was necessary due to osteonecrosis of the distal tibia. One may argue that an additional SMO at time of TAR might compromise the vascularity of distal tibia and thus provoke avascular necrosis which, in turn, may result in delayed or missing osteointegration of tibial component. However, this was not the case in the present study. Of note, two patients had a non-union of the tibia osteotomy, a significant complication needing revision surgery. In contrast, two patients who underwent TAR only suffered from an intra-operative malleolar fracture. It is important to mention that SMO/TAR can also be performed in two separate operations. However, patients must undergo twice a rehabilitation protocol, possibly lengthening the overall rehabilitation time. Nevertheless, performing SMO/TAR as a one-stage procedure is technically demanding and should be reserved for experienced surgeons to avoid inferior results due to severe complications.
This study has several limitations. First, the number of patients included is rather small. Nevertheless, according to the authors’ knowledge, this represents the largest cohort currently available in the literature using such an approach to balance the ankle in TAR. Second, multiple additional procedures (e.g. osteotomy of the medial malleolus, fibula osteotomy) were necessary for proper correction of the deformity. It is difficult to discern the degree to which those procedures may confound the observed results. However, given the heterogeneity of the concomitant procedures, it would seem less likely that there is a systematic confounding effect with these procedures. Third, the AOFAS-hindfoot scale is a non-validated outcome score. Nevertheless, it is widely used to assess the clinical outcome following hindfoot surgery [27, 28].
To conclude, most varus and/or recurvatum deformities of the distal tibia can successfully be corrected through adjusted tibial cuts during TAR. An additional SMO during TAR may be only beneficial in case of severe multiplanar (e.g. combined coronal and sagittal) deformities.
References
Schuh R, Hofstaetter J, Krismer M, Bevoni R, Windhager R, Trnka HJ (2012) Total ankle arthroplasty versus ankle arthrodesis. Comparison of sports, recreational activities and functional outcome. Int Orthop 36(6):1207–1214. https://doi.org/10.1007/s00264-011-1455-8
Barg A, Zwicky L, Knupp M, Henninger HB, Hintermann B (2013) HINTEGRA total ankle replacement: survivorship analysis in 684 patients. J Bone Joint Surg Am 95(13):1175–1183. https://doi.org/10.2106/JBJS.L.01234
Daniels TR, Mayich DJ, Penner MJ (2015) Intermediate to long-term outcomes of total ankle replacement with the Scandinavian Total Ankle Replacement (STAR). J Bone Joint Surg Am 97(11):895–903. https://doi.org/10.2106/JBJS.N.01077
Frigg A, Germann U, Huber M, Horisberger M (2017) Survival of the Scandinavian total ankle replacement (STAR): results of ten to nineteen years follow-up. Int Orthop 41(10):2075–2082. https://doi.org/10.1007/s00264-017-3583-2
Kim HJ, Suh DH, Yang JH, Lee JW, Kim HJ, Ahn HS, Han SW, Choi GW (2017) Total ankle arthroplasty versus ankle arthrodesis for the treatment of end-stage ankle arthritis: a meta-analysis of comparative studies. Int Orthop 41(1):101–109. https://doi.org/10.1007/s00264-016-3303-3
Yang HY, Wang SH, Lee KB (2019) The HINTEGRA total ankle arthroplasty: functional outcomes and implant survivorship in 210 osteoarthritic ankles at a mean of 6.4 years. Bone Joint J 101-B(6):695–701. https://doi.org/10.1302/0301-620X.101B6.BJJ-2018-1578.R1
Usuelli FG, Di Silvestri CA, D’Ambrosi R, Orenti A, Randelli F (2019) Total ankle replacement: is pre-operative varus deformity a predictor of poor survival rate and clinical and radiological outcomes? Int Orthop 43(1):243–249. https://doi.org/10.1007/s00264-018-4189-z
Queen RM, Adams SB Jr, Viens NA, Friend JK, Easley ME, Deorio JK, Nunley JA (2013) Differences in outcomes following total ankle replacement in patients with neutral alignment compared with tibiotalar joint malalignment. J Bone Joint Surg Am 95(21):1927–1934. https://doi.org/10.2106/JBJS.L.00404
Yi Y, Cho JH, Kim JB, Kim JY, Park SY, Lee WC (2017) Change in talar translation in the coronal plane after mobile-bearing total ankle replacement and its association with lower-limb and hindfoot alignment. J Bone Joint Surg Am 99(4):e13. https://doi.org/10.2106/JBJS.15.01340
Ruiz R, Susdorf R, Krahenbuhl N, Barg A, Hintermann B (2019) Syndesmotic overload in 3-component total ankle replacement. Foot Ankle Int:1071100719894528. https://doi.org/10.1177/1071100719894528
Trajkovski T, Pinsker E, Cadden A, Daniels T (2013) Outcomes of ankle arthroplasty with preoperative coronal-plane varus deformity of 10 degrees or greater. J Bone Joint Surg Am 95(15):1382–1388. https://doi.org/10.2106/JBJS.L.00797
Hintermann B, Ruiz R (2019) Total replacement of varus ankle: three-component prosthesis design. Foot Ankle Clin 24(2):305–324. https://doi.org/10.1016/j.fcl.2019.02.005
Choi WJ, Kim BS, Lee JW (2012) Preoperative planning and surgical technique: how do I balance my ankle? Foot Ankle Int 33(3):244–249. https://doi.org/10.3113/FAI.2012.0244
DeOrio JK (2012) Peritalar symposium: total ankle replacements with malaligned ankles: osteotomies performed simultaneously with TAA. Foot Ankle Int 33(4):344–346. https://doi.org/10.3113/FAI.2012.0344
Gauvain TT, Hames MA, McGarvey WC (2017) Malalignment correction of the lower limb before, during, and after total ankle arthroplasty. Foot Ankle Clin 22(2):311–339. https://doi.org/10.1016/j.fcl.2017.01.003
Krahenbuhl N, Akkaya M, Deforth M, Zwicky L, Barg A, Hintermann B (2019) Extraarticular supramalleolar osteotomy in asymmetric varus ankle osteoarthritis. Foot Ankle Int 40(8):936–947. https://doi.org/10.1177/1071100719845928
Magerkurth O, Knupp M, Ledermann H, Hintermann B (2006) Evaluation of hindfoot dimensions: a radiological study. Foot Ankle Int 27(8):612–616
Stufkens SA, Barg A, Bolliger L, Stucinskas J, Knupp M, Hintermann B (2011) Measurement of the medial distal tibial angle. Foot Ankle Int 32(3):288–293. https://doi.org/10.3113/FAI.2011.0288
Saltzman CL, el-Khoury GY (1995) The hindfoot alignment view. Foot Ankle Int 16(9):572–576. https://doi.org/10.1177/107110079501600911
Lindsjo U, Danckwardt-Lilliestrom G, Sahlstedt B (1985) Measurement of the motion range in the loaded ankle. Clin Orthop Relat Res (199):68–71
Schneider W, Jurenitsch S (2016) Normative data for the American Orthopedic Foot and Ankle Society ankle-hindfoot, midfoot, hallux and lesser toes clinical rating system. Int Orthop 40(2):301–306. https://doi.org/10.1007/s00264-015-3066-2
Goodman SM, Mehta BY, Kahlenberg CA, Krell EC, Nguyen J, Finik J, Figgie MP, Parks ML, Padgett DE, Antao VC, Yates AJ, Springer BD, Lyman SL, Singh JA (2020) Assessment of a satisfaction measure for use after primary total joint arthroplasty. J Arthroplast. https://doi.org/10.1016/j.arth.2020.02.039
Scheidegger P, Horn Lang T, Schweizer C, Zwicky L, Hintermann B (2019) A flexion osteotomy for correction of a distal tibial recurvatum deformity: a retrospective case series. Bone Joint J 101-B(6):682–690. https://doi.org/10.1302/0301-620X.101B6.BJJ-2018-0932.R2
Fox J, Weisber S (2019) An R companion to applied regression, 3rd edn. Sage, Thousand Oaks
R Core Team (2015) R: A language and environment for statistical computing. R Foundation for Statistical Computing 2015; Vienna, Austria. (http://www.R-project.org/)
Krahenbuhl N, Susdorf R, Barg A, Hintermann B (2020) Supramalleolar osteotomy in post-traumatic valgus ankle osteoarthritis. Int Orthop. https://doi.org/10.1007/s00264-019-04476-x
Pena F, Agel J, Coetzee JC (2007) Comparison of the MFA to the AOFAS outcome tool in a population undergoing total ankle replacement. Foot Ankle Int 28(7):788–793. https://doi.org/10.3113/FAI.2006.0788
Naal FD, Impellizzeri FM, Rippstein PF (2010) Which are the most frequently used outcome instruments in studies on total ankle arthroplasty? Clin Orthop Relat Res 468(3):815–826. https://doi.org/10.1007/s11999-009-1036-y
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All royalties that the senior author (Beat Hintermann) received from Integra LifeSciences from 2005 to 2012 were given to the Orthopaedic Research Fund of the Kantonsspital Baselland. Dr. Barg reports personal fees from Medartis (outside the submitted work).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Level of evidence: III, case-control study
Rights and permissions
About this article
Cite this article
Franz, AC., Krähenbühl, N., Ruiz, R. et al. Hindfoot balancing in total ankle replacement: the role of supramalleolar osteotomies. International Orthopaedics (SICOT) 44, 1859–1867 (2020). https://doi.org/10.1007/s00264-020-04681-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-020-04681-z