Abstract
Purpose
Clinical shoulder science lacks a benchmark against which the early clinical value of new glenoid components can be compared; such a benchmark may be derived from a multicenter study of patients receiving an established, internationally used design of glenoid component.
Methods
We obtained data from 11 centers on 1270 patients having total shoulder arthroplasty using an all-polyethylene component with a fluted central peg. We analyzed individual patient outcomes at 1 and 2 years after surgery. We compared the improvement for each patient to the minimal clinically important difference (MCID) and calculated each patient’s improvement as a percent of maximal possible improvement (MPI).
Results
The preoperative scores improved from SST 3 ± 2, ASES 37 ± 15, Constant score 36 ± 16, and Penn score 30 ± 19 to SST 10 ± 2, ASES 90 ± 12, Constant 76 ± 13, and Penn 80 ± 24 (p < 0.001 for each). A high percentage of patients improved by more than the MCID (SST 96%, ASES 98%, Constant 94%, Penn 93%) and obtained improvement of at least 30% of the MPI (SST 95%, ASES 98%, Constant 91%, Penn 87%). The clinical outcomes realized with this glenoid design were not worse for the 41% of shoulders with preoperative type B glenoids or for the 30% of shoulders with more than 15 degrees of glenoid retroversion.
Conclusions
Individual patients from 11 international practices having total shoulder arthroplasty using a basic glenoid component design obtained highly significant clinical outcomes, providing a benchmark against which the early outcomes of new designs can be compared to determine whether they provide increased clinical value.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Background and rationale
Total shoulder arthroplasty is a widely used surgical treatment for glenohumeral arthritis. Glenoid component failure has been identified as the major mechanical cause of failure of total shoulder arthroplasty [1,2,3,4,5,6,7,8,9,10]. A recent review indicates that this is still the case: glenoid loosening accounted for 38% of all total shoulder complications [11]. In an attempt to address the high rate of glenoid failure, new glenoid components are being submitted and cleared by the U.S. Food and Drug Administration’s 510 (k) process each year (Fig. 1). However, in spite of the introduction of these new designs, a recent analysis failed to show evidence of substantially improving outcomes for total shoulders over the last two decades [12]. It is difficult to know whether the new designs of glenoid components are yielding results that exceed the results of components that have been in widespread international usage for many years.
One of the commonly used glenoid designs is an all-polyethylene component that is fixed to bone with cemented peripheral pegs and an uncemented fluted central peg. The outcomes for patients receiving this glenoid component have been the subject of recent reports by surgeons from different countries [13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31]; however, the patients in these articles have not been analyzed together as a cohort of individuals. We contacted the authors of these publications requesting their most recent data on each patient having a total shoulder using this glenoid design so that we could perform a “by patient” analysis in which the clinical outcome for each patient was weighted individually.
We hypothesized that a great majority of patients with glenohumeral arthritis from 11 independent centers using this design of glenoid component would achieve clinically significant improvement following total shoulder arthroplasty assessed by generally accepted outcome instruments.
Methods
This is a multicenter retrospective observational study approved by our Institutional Review Board (HSD# STUDY00001714).
Study design and participants
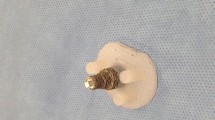
A literature search was performed to identify institutions that had clinical outcome data for total shoulder arthroplasties that used one of two very similar designs of glenoid component: a DePuy Anchor Peg (DePuy, Warsaw, IN, USA) (Fig. 2) or a Wright Medical Perform Cortiloc (Wright Medical, Memphis, TN, USA) fluted central peg glenoid (Fig. 3). The corresponding authors were contacted and invited to participate by submitting de-identified data on each patient to this study.
Importantly, this investigation represented the variety of practice preferences of the participating surgeons using these glenoid components. There was no attempt to standardize patient evaluation and management, except for the design of glenoid component used. Each surgeon applied his own approach to preoperative radiographic evaluation (plain films, MRI or CT scan) and each applied his own indications and technique for total shoulder arthroplasty using this glenoid component design. Each participating surgeon completed a standardized data sheet including age at surgery, sex, year of surgery, diagnosis, preoperative glenoid type [32,33,34], glenoid retroversion, prior surgery, humeral component type, glenoid component, and humeral and glenoid component articular surface diameters of curvature. Each center used one or more of the following validated outcome scores to evaluate the clinical results of the arthroplasty: Simple Shoulder Test (SST), American Shoulder and Elbow Score (ASES), Constant Score (CS), or Penn Score.
Subjects were included in our analysis if they were between ages 18–99, had a shoulder arthroplasty procedure performed for arthritis with an all-polyethylene fluted central peg glenoid component between 2000 and 2016, and had functional outcome scores preoperatively and at 1 or 2 years after surgery.
The clinical significance of the preoperative to postoperative improvement in each clinical score was assessed in two ways. First, the published value for the minimal clinically important difference (MCID) for each outcome scale was obtained from the literature: the Simple Shoulder Test (1.5), the American Shoulder Elbow Surgeons Score (13.6), the Constant Score (5.7), and the Penn Score (11.4) [35,36,37]. Each patient’s scores were examined to determine if the improvement exceeded the MCID. Second, the maximal possible improvement for each patient was determined as the difference between the maximal possible value for the outcome scale and the patient’s preoperative score. The amount of improvement achieved by each patient was then divided by the maximal possible improvement to obtain the percent of maximal possible improvement (%MPI)—clinically significant improvement has been defined as improvement of at least 30% of the maximal possible improvement [12, 27, 38,39,40,41,42].
One- and 2-year outcomes were characterized as the amount of improvement on each scale in comparison to the MCID and as the percentage of maximum possible improvement (%MPI). To enable comparison among the different scales, the 12-point Simple Shoulder Test was rescaled to a 0–100 scale [36]. Associations between risk factors and outcomes were estimated using multiple linear regression of the outcomes on each risk factor, adjusting for the practice site and the baseline value of the outcome score.
All calculations were carried out by an experienced statistician in R version 3.4.3 (Vienna, Austria) [42].
Results
In all, 1270 individual patients from 11 centers met the criteria for inclusion (Table 1). The typical patient had osteoarthritis, was 66 years of age at the time of surgery, and had surgery in 2011. The glenoid types reported by the surgeons were A1 (28.5%), A2 (29.2%), B1 (15.3%), and B2 (26.1%). Preoperative glenoid version averaged 12 ± 9°; 30% had retroversion greater than 15°. Seventy percent of the humeral components were standard stems, 18% short stems, and 12% stemless. The Anchor Peg glenoid was used in 65% and the Cortiloc glenoid in 35%. The average diameter of curvature of the humeral component was 49 ± 4 mm and that of the glenoid was 51 ± 6 mm. Preoperative and postoperative function was assessed by the Simple Shoulder Test in 654, the ASES score in 757, the Constant score in 446, and the PENN score in 16 (note that some patients were assessed by multiple scores).
Twenty-five shoulders (2%) were reported to have had a second surgical procedure following their initial total shoulder arthroplasty. The types of second surgery were not further detailed in this study of clinical outcomes. With the exception of patient age, no preoperative patient or shoulder characteristics were significantly associated with the need for a second surgery. The odds ratio for revision by age at surgery (per 10 years) was 0.62 (95% CI 0.44–0.90, p = 0.014).
The great majority of these patients improved by more than the minimal clinically important difference and improved by more than 30% of the maximal possible improvement (MPI) (Table 2). The mean ± SD preoperative scores improved from SST 3 ± 2, ASES 37 ± 15, Constant score 36 ± 16, and Penn score 30 ± 19 to SST 10 ± 2, ASES 90 ± 12, Constant 76 ± 13, and Penn 80 ± 24 (p < 0.001 for each). For patients assessed with the SST, over 90% exceeded the MCID of 1.5 and improved by 30% of the MPI. For patients assessed with the ASES score, over 95% exceeded the MCID of 13.6 and improved by over 30% of the MPI. For patients assessed with the Constant score, over 90% exceeded the MCID of 5.7 and improved by over 30% of the MPI. Finally, for patients assessed with the Penn score, over 85% exceeded the MCID of 11.4 and improved by over 30% of the MPI.
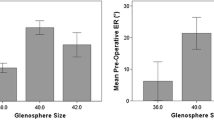
For patients with data at both 1 and 2 years after surgery, there was little clinical improvement in outcome scores between year 1 and 2, even though some of the differences were statistically significant (Fig. 4).
Average SST, ASES, and Constant scores before and at 1 and 2 years after surgery for patients receiving a standard all-polyethylene glenoid component with a fluted central peg. Vertical axis indicates the percentage of a perfect score. Data for the Penn Score are not shown because of the small number of patients assessed with this score
These outcomes for the standard, non-augmented glenoid component were realized in cases with a range of patient and shoulder characteristics (Table 1), including the 41% of cases that had type B glenoids and the 30% of cases that had more than 15° of glenoid retroversion. The outcomes for shoulders with retroverted or type B glenoids were not inferior to those with neutral version or type A glenoids, respectively (Appendix Tables 4 and 5). The clinical outcomes were not consistently associated with the degree of mismatch between the humeral and glenoid diameters of curvature [43, 44].
A comparison of the percent of maximal possible improvement for the SST, ASES, and Constant scores for ten different sites is shown in Table 3. Each scale at each site showed values for the average percent of maximal possible improvement that easily exceeded the threshold of 30%.
Discussion
This study design is unique in that it analyzes the early total shoulder clinical outcomes at the discrete time points of 1 and 2 years for 1270 individual patients from 11 independent international centers using a standard design all-polyethylene glenoid component with a fluted central peg and three cemented peripheral pegs.
As assessed by generally accepted outcome instruments, the average improvement in comfort and function achieved by these individual patients easily exceeded the published values for the minimal clinically important difference and provided well over 30% of the maximum possible improvement.
For patients having results at both the year 1 and year 2 time points, the improvement after the first year was small: 0.2 ± 1.5 for the SST, 0.8 ± 8.9 for the ASES score, and 0.5 ± 8.0 for the Constant score. This observation suggests that most of the clinical improvement after a total shoulder arthroplasty occurs within the first year; therefore, year 1 data may be sufficient for characterizing the early outcomes for total shoulder arthroplasty with different glenoid component designs [36].
An interesting finding in this analysis was that with this basic glenoid component design, type B glenoids and glenoids with more than 15° of retroversion did not have outcomes that were inferior to those with less severe glenoid pathoanatomy. While special glenoid components have been designed for the type B retroverted glenoid [26, 45, 46], our study and other recent publications [27, 39, 47, 48] point out that the role for these special components has yet to be clarified.
The clinical outcomes reported were qualitatively similar among the different scoring systems used by the different centers. The application of published values for the MCID and the use of the percent of maximal possible improvement offer the possibility of comparing outcomes obtained with different outcome instruments.
The results of this study should be considered in light of certain limitations. First, this study focused only on the improvement in standard, validated, widely used, and universally available clinical outcome scales—Simple Shoulder Test, American Shoulder and Elbow score, Constant Score, and Penn Score—each of which has a defined MCID. Range of motion estimates and radiographic interpretations by the surgeons were not included in this analysis. Second, this study focused on the clinical improvement at discrete time points: 1 and 2 years after surgery, rather than mixing outcomes recorded over a range of years. While both 1 and 2-year follow-up data were not available for all patients, the results available at both of the two time points were quite similar [36]. Third, while most of the variables we assessed did not have a consistent, statistically significant effect on the outcome, some of these effects may have become significant if the number of patients was larger. Fourth, there was no attempt on our part to standardize the indications for surgery, the preoperative clinical or radiographic evaluation, the choice of humeral component, the surgical technique, or the postoperative rehabilitation program; instead, the surgeons treated each of their patients according to their personal practice guidelines. The consistency of the outcomes among these varied practices indicates the general utility of this design of glenoid component. Fifth, this study did not investigate component revision and survivorship, which require follow-up of 5 years or longer to obtain meaningful data [9, 22, 49, 50]. Finally, the surgeons whose patients were included in this analysis each had substantial experience in shoulder arthroplasty; the outcomes reported here might not be generalizable to the practices of surgeons with less experience [47, 51,52,53,54,55,56].
This report provides a broad-based and well-characterized data set against which the 1- and 2-year clinical outcomes for different glenoid components can be compared using universally available assessment scales (SST, ASES, Constant, Penn). Such comparisons are becoming increasing necessary and timely: new shoulder arthroplasty systems are being introduced annually without evidence that their clinical outcomes are superior to or even equal to those in current use [12]. Thus, a strong case exists for establishing a reference of 1- and 2-year clinical outcomes for standard glenoid components—such as that presented in this report—against which the early performance of new components can be compared. The results of this study suggest a possible benchmark for shoulders having pre and postoperative SST, ASES, Constant, or Penn scores: at 1 and 2 years after total shoulder arthroplasty, 90% of the shoulders are improved by the minimal clinically important difference and are improved by 30% of the maximal possible improvement.
Conclusion
The strength of this study lies in its demonstration that surgeons in 11 independent practices using their individual approaches to patient selection, preoperative evaluation, surgical technique, and outcome evaluation were able to obtain robust early clinical outcomes in an international group of over 1200 individual patients using a basic all-polyethylene glenoid component. These data provide a basis for comparison with newer designs to determine whether these new designs lead to better early clinical outcomes.
References
Australian Government Department of Health Therapeutic Goods Administration (2012) SMR L2 metal back glenoid component (used in shoulder replacements). Product discontinued. Available at: https://www.tga.gov.au/alert/smr-l2-metal-back-glenoid-component-used-shoulder-replacements. Accessed 13 Feb 2018
Australian Orthopaedic Association (2017) Australian Orthopaedic Association National Joint Replacement Registry (AOANJRR). Hip, knee & shoulder arthroplasty. Table ST30. Adelaide: AOA; Available at: https://aoanjrr.sahmri.com/documents/10180/397736/Hip%2C%20Knee%20%26%20Shoulder%20Arthroplasty. Accessed 13 Feb 2018
Bohsali KI, Wirth MA, Rockwood CA Jr (2006) Complications of total shoulder arthroplasty. J Bone Joint Surg Am 88(10):2279–2292. https://doi.org/10.2106/JBJS.F.00125
Buckingham BP, Parsons IM, Campbell B, Titelman RM, Smith KL, Matsen FA 3rd (2005) Patient functional self-assessment in late glenoid component failure at three to eleven years after total shoulder arthroplasty. J Shoulder Elb Surg 14(4):368–374. https://doi.org/10.1016/j.jse.2004.10.008 Blinded for review purposes.
Hsu JE, Hackett DJ Jr, Vo KV, Matsen FA 3rd (2018) What can be learned from an analysis of 215 glenoid component failures? J Shoulder Elb Surg 27(3):478–486. https://doi.org/10.1016/j.jse.2017.09.029 Blinded for review purposes.
Karelse A, Van Tongel A, Van Isacker T, Berghs B, De Wilde L (2016) Parameters influencing glenoid loosening. Expert Rev Med Devices 13(8):773–784. https://doi.org/10.1080/17434440.2016.1205483
Matsen FA 3rd, Clinton J, Lynch J, Bertelsen A, Richardson ML (2008) Glenoid component failure in total shoulder arthroplasty. J Bone Joint Surg Am 90(4):885–896. https://doi.org/10.2106/JBJS.G.01263 Blinded for review purposes.
Papadonikolakis A, Matsen FA 3rd (2014) Metal-backed glenoid components have a higher rate of failure and fail by different modes in comparison with all-polyethylene components: a systematic review. J Bone Joint Surg Am 96(12):1041–1047. https://doi.org/10.2106/JBJS.M.00674 Blinded for review purposes.
Papadonikolakis A, Neradilek MB, Matsen FA 3rd (2013) Failure of the glenoid component in anatomic total shoulder arthroplasty: a systematic review of the English-language literature between 2006 and 2012. J Bone Joint Surg Am 95(24):2205–2212. https://doi.org/10.2106/JBJS.L.00552 Blinded for review purposes.
U.S. Food and Drug Administration (2016) Zimmer Biomet recalls comprehensive reverse shoulder due to high fracture rate. Silver Spring; Available at: https://www.fda.gov/MedicalDevices/Safety/ListofRecalls/ucm541862.htm. Accessed 4 Mar 2018
Bohsali KI, Bois AJ, Wirth MA (2017) Complications of shoulder arthroplasty. J Bone Joint Surg Am 99(3):256–269. https://doi.org/10.2106/JBJS.16.00935
Somerson JS, Neradilek MB, Hsu JE, Service BC, Gee AO, Matsen FA 3rd (2017) Is there evidence that the outcomes of primary anatomic and reverse shoulder arthroplasty are getting better? Int Orthop 41(6):1235–1244. https://doi.org/10.1007/s00264-017-3443-0 Blinded for review purposes.
Arnold RM, High RR, Grosshans KT, Walker CW, Fehringer EV (2011) Bone presence between the central peg’s radial fins of a partially cemented pegged all poly glenoid component suggest few radiolucencies. J Shoulder Elb Surg 20(2):315–321. https://doi.org/10.1016/j.jse.2010.05.025
Churchill RS, Zellmer C, Zimmers HJ, Ruggero R (2010) Clinical and radiographic analysis of a partially cemented glenoid implant: five-year minimum follow-up. J Shoulder Elb Surg 19(7):1091–1097. https://doi.org/10.1016/j.jse.2009.12.022
De Wilde L, Dayerizadeh N, De Neve F, Basamania C, Van Tongel A (2013) Fully uncemented glenoid component in total shoulder arthroplasty. J Shoulder Elb Surg 22(10):e1–e7. https://doi.org/10.1016/j.jse.2013.01.036
Edwards TB, Labriola JE, Stanley RJ, O'Connor DP, Elkousy HA, Gartsman GM (2010) Radiographic comparison of pegged and keeled glenoid components using modern cementing techniques: a prospective randomized study. J Shoulder Elb Surg 19(2):251–257. https://doi.org/10.1016/j.jse.2009.10.013
Groh GI (2010) Survival and radiographic analysis of a glenoid component with a cementless fluted central peg. J Shoulder Elb Surg 19(8):1265–1268. https://doi.org/10.1016/j.jse.2010.03.012
Ho JC, Sabesan VJ, Iannotti JP (2013) Glenoid component retroversion is associated with osteolysis. J Bone Joint Surg Am 95(12):e82. https://doi.org/10.2106/JBJS.L.00336
Hsu JE, Namdari S, Baron M, Kuntz AF, Abboud JA, Huffman GR, Williams GR, Glaser DL (2014) Glenoid perforation with pegged components during total shoulder arthroplasty. Orthopedics 37(6):e587–e591. https://doi.org/10.3928/01477447-20140528-61
Iannotti JP, Greeson C, Downing D, Sabesan V, Bryan JA (2012) Effect of glenoid deformity on glenoid component placement in primary shoulder arthroplasty. J Shoulder Elb Surg 21(1):48–55. https://doi.org/10.1016/j.jse.2011.02.011
Kilian CM, Morris BJ, Sochacki KR, Gombera MM, Haigler RE, O'Connor DP, Edwards TB (2018) Radiographic comparison of finned, cementless central pegged glenoid component and conventional cemented pegged glenoid component in total shoulder arthroplasty: a prospective randomized study. J Shoulder Elb Surg 27(6S):S10–S16. https://doi.org/10.1016/j.jse.2017.09.014
Kilian CM, Press CM, Smith KM, O'Connor DP, Morris BJ, Elkousy HA, Gartsman GM, Edwards TB (2017) Radiographic and clinical comparison of pegged and keeled glenoid components using modern cementing techniques: midterm results of a prospective randomized study. J Shoulder Elb Surg 26(12):2078–2085. https://doi.org/10.1016/j.jse.2017.07.016
Merolla G, Ciaramella G, Fabbri E, Walch G, Paladini P, Porcellini G (2016) Total shoulder replacement using a bone ingrowth central peg polyethylene glenoid component: a prospective clinical and computed tomography study with short- to mid-term follow-up. Int Orthop 40(11):2355–2363. https://doi.org/10.1007/s00264-016-3255-7
Noyes MP, Meccia B, Spencer EE Jr (2015) Five- to ten-year follow-up with a partially cemented all-polyethylene bone-ingrowth glenoid component. J Shoulder Elb Surg 24(9):1458–1462. https://doi.org/10.1016/j.jse.2015.02.018
Parks DL, Casagrande DJ, Schrumpf MA, Harmsen SM, Norris TR, Kelly JD 2nd (2016) Radiographic and clinical outcomes of total shoulder arthroplasty with an all-polyethylene pegged bone ingrowth glenoid component: prospective short- to medium-term follow-up. J Shoulder Elb Surg 25(2):246–255. https://doi.org/10.1016/j.jse.2015.07.008
Sabesan V, Callanan M, Sharma V, Iannotti JP (2014) Correction of acquired glenoid bone loss in osteoarthritis with a standard versus an augmented glenoid component. J Shoulder Elb Surg 23(7):964–973. https://doi.org/10.1016/j.jse.2013.09.019
Service BC, Hsu JE, Somerson JS, Russ SM, Matsen FA 3rd (2017) Does postoperative glenoid retroversion affect the 2-year clinical and radiographic outcomes for total shoulder arthroplasty? Clin Orthop Relat Res 475(11):2726–2739. https://doi.org/10.1007/s11999-017-5433-3 Blinded for review purposes.
Vidil A, Valenti P, Guichoux F, Barthas JH (2013) CT scan evaluation of glenoid component fixation: a prospective study of 27 minimally cemented shoulder arthroplasties. Eur J Orthop Surg Traumatol 23(5):521–525. https://doi.org/10.1007/s00590-012-1126-5
Wijeratna M, Taylor DM, Lee S, Hoy G, Evans MC (2016) Clinical and radiographic results of an all-polyethylene pegged bone-ingrowth glenoid component. J Bone Joint Surg Am 98(13):1090–1096. https://doi.org/10.2106/JBJS.15.00475
Wirth MA, Korvick DL, Basamania CJ, Toro F, Aufdemorte TB, Rockwood CA Jr (2001) Radiologic, mechanical, and histologic evaluation of 2 glenoid prosthesis designs in a canine model. J Shoulder Elb Surg 10(2):140–148. https://doi.org/10.1067/mse.2001.112021
Wirth MA, Loredo R, Garcia G, Rockwood CA Jr, Southworth C, Iannotti JP (2012) Total shoulder arthroplasty with an all-polyethylene pegged bone-ingrowth glenoid component: a clinical and radiographic outcome study. J Bone Joint Surg Am 94(3):260–267. https://doi.org/10.2106/JBJS.J.01400
Bercik MJ, Kruse K 2nd, Yalizis M, Gauci MO, Chaoui J, Walch G (2016) A modification to the Walch classification of the glenoid in primary glenohumeral osteoarthritis using three-dimensional imaging. J Shoulder Elb Surg 25(10):1601–1606. https://doi.org/10.1016/j.jse.2016.03.010
Walch G, Badet R, Boulahia A, Khoury A (1999) Morphologic study of the glenoid in primary glenohumeral osteoarthritis. J Arthroplast 14(6):756–760
Walch G, Boulahia A, Boileau P, Kempf JF (1998) Primary glenohumeral osteoarthritis: clinical and radiographic classification. The Aequalis Group. Acta Orthop Belg 64(Suppl 2):46–52
Leggin BG, Michener LA, Shaffer MA, Brenneman SK, Iannotti JP, Williams GR Jr (2006) The Penn shoulder score: reliability and validity. J Orthop Sports Phys Ther 36(5):138–151. https://doi.org/10.2519/jospt.2006.36.3.138
Puzzitiello RN, Agarwalla A, Liu JN, Cvetanovich GL, Romeo AA, Forsythe B, Verma NN (2018) Establishing maximal medical improvement after anatomic total shoulder arthroplasty. J Shoulder Elb Surg 27(9):1711–1720. https://doi.org/10.1016/j.jse.2018.03.007
Simovitch R, Flurin PH, Wright T, Zuckerman JD, Roche CP (2017) Quantifying success after total shoulder arthroplasty: the substantial clinical benefit. J Shoulder Elb Surg 27(5):903–911. https://doi.org/10.1016/j.jse.2017.12.014
Gilmer BB, Comstock BA, Jette JL, Warme WJ, Jackins SE, Matsen FA 3rd (2012) The prognosis for improvement in comfort and function after the ream-and-run arthroplasty for glenohumeral arthritis: an analysis of 176 consecutive cases. J Bone Joint Surg 94(14):e102. https://doi.org/10.2106/JBJS.K.00486 Blinded for review purposes.
Matsen FA 3rd, Russ SM, Vu PT, Hsu JE, Lucas RM, Comstock BA (2016) What factors are predictive of patient-reported outcomes? A prospective study of 337 shoulder arthroplasties. Clin Orthop Relat Res 474(11):2496–2510. https://doi.org/10.1007/s11999-016-4990-1 Blinded for review purposes.
McElvany MD, McGoldrick E, Gee AO, Neradilek MB, Matsen FA 3rd (2015) Rotator cuff repair: published evidence on factors associated with repair integrity and clinical outcome. Am J Sports Med 43(2):491–500. https://doi.org/10.1177/0363546514529644 Blinded for review purposes.
Somerson JS, Sander P, Bohsali KI, Tibbetts R, Rockwood CA Jr, Wirth MA (2016) What factors are associated with clinically important improvement after shoulder hemiarthroplasty for cuff tear arthropathy? Clin Orthop Relat Res 474(12):2682–2688. https://doi.org/10.1007/s11999-016-5037-3 Blinded for review purposes.
R Core Team (2017) R: a language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing; Available at: https://www.R-project.org/. Accessed 4 Mar 2018
Schoch B, Abboud J, Namdari S, Lazarus M (2017) Glenohumeral mismatch in anatomic total shoulder arthroplasty. JBJS Rev 5(9):e1. https://doi.org/10.2106/JBJS.RVW.17.00014
Walch G, Edwards TB, Boulahia A, Boileau P, Mole D, Adeleine P (2002) The influence of glenohumeral prosthetic mismatch on glenoid radiolucent lines: results of a multicenter study. J Bone Joint Surg Am 84(12):2186–2191
Iannotti JP, Lappin KE, Klotz CL, Reber EW, Swope SW (2013) Liftoff resistance of augmented glenoid components during cyclic fatigue loading in the posterior-superior direction. J Shoulder Elb Surg 22(11):1530–1536. https://doi.org/10.1016/j.jse.2013.01.018
Stephens SP, Spencer EE, Wirth MA (2017) Radiographic results of augmented all-polyethylene glenoids in the presence of posterior glenoid bone loss during total shoulder arthroplasty. J Shoulder Elb Surg 26(5):798–803. https://doi.org/10.1016/j.jse.2016.09.053
Orvets ND, Chamberlain AM, Patterson BM, Chalmers PN, Gosselin M, Salazar D, Aleem AW, Keener JD (2018) Total shoulder arthroplasty in patients with a B2 glenoid addressed with corrective reaming. J Shoulder Elb Surg 27(6S):S58–S64. https://doi.org/10.1016/j.jse.2018.01.003
Ricchetti ET, Jun BJ, Cain RA, Youderian A, Rodriguez EJ, Kusin D, Subhas N, Patterson TE, Iannotti JP (2018) Sequential 3-dimensional computed tomography analysis of implant position following total shoulder arthroplasty. J Shoulder Elb Surg 27(6):973–992. https://doi.org/10.1016/j.jse.2017.12.012
Nelson CG, Brolin TJ, Ford MC, Smith RA, Azar FM, Throckmorton TW (2018) Five-year minimum clinical and radiographic outcomes of total shoulder arthroplasty using a hybrid glenoid component with a central porous titanium post. J Shoulder Elb Surg 27(8):1462–1467. https://doi.org/10.1016/j.jse.2018.01.012
Walch G, Young AA, Boileau P, Loew M, Gazielly D, Mole D (2012) Patterns of loosening of polyethylene keeled glenoid components after shoulder arthroplasty for primary osteoarthritis: results of a multicenter study with more than five years of follow-up. J Bone Joint Surg Am 94(2):145–150. https://doi.org/10.2106/JBJS.J.00699
Hammond JW, Queale WS, Kim TK, McFarland EG (2003) Surgeon experience and clinical and economic outcomes for shoulder arthroplasty. J Bone Joint Surg Am 85(12):2318–2324
Jain N, Pietrobon R, Hocker S, Guller U, Shankar A, Higgins LD (2004) The relationship between surgeon and hospital volume and outcomes for shoulder arthroplasty. J Bone Joint Surg Am 86(3):496–505
Karelse A, Leuridan S, Van Tongel A, Debeer P, Van Der Sloten J, Denis K, De Wilde LF (2015) Consequences of reaming with flat and convex reamers for bone volume and surface area of the glenoid; a basic science study. J Orthop Surg Res 10:181. https://doi.org/10.1186/s13018-015-0312-7
Lazarus MD, Jensen KL, Southworth C, Matsen FA 3rd (2002) The radiographic evaluation of keeled and pegged glenoid component insertion. J Bone Joint Surg Am 84(7):1174–1182 Blinded for review purposes
Lyman S, Jones EC, Bach PB, Peterson MG, Marx RG (2005) The association between hospital volume and total shoulder arthroplasty outcomes. Clin Orthop Relat Res (432):132–137
Walch G, Mesiha M, Boileau P, Edwards TB, Lévigne C, Moineau G, Young AA (2013) Three-dimensional assessment of the dimensions of the osteoarthritic glenoid. Bone Joint J 95B(10):1377–1382. https://doi.org/10.1302/0301-620X.95B10.32012
Acknowledgements
We thank Susan DeBartolo, University of Washington, Department of Orthopaedics and Sports Medicine, (blinded for review purposes) for her editorial work on this manuscript.
Funding
There was no extramural funding for this investigation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This was a retrospective cohort study approved by our Institutional Review Board (HSD# STUDY00001714). For this type of study, formal consent is not required.
Informed consent
N/A.
Conflict of interest
Financial remuneration the authors, or any member of their family, may have received directly related to the subject of the article: none.
The following is blinded for review purposes:
Dr. Matsen (first and corresponding author), Dr. De Wilde, Dr. Groh, Dr. Kilian, Dr. Merolla, Mr. Neradilek, Dr. Porcellini, Ms. Russ, Dr. Somerson, and Dr. Vidil have no conflict of interests to report.
The following doctors have conflict of interests outside of the submitted work as noted:
Dr. Iannotti reports personal fees from DePuy Synthes, personal fees from DJO Surgical, personal fees from Wright Tornier, from null, outside the submitted work.
Dr. Churchill reports personal fees from Wright Medical Tornier, Inc., during the conduct of the study; personal fees from Wright Medical Tornier, Inc., outside the submitted work. In addition, Dr. Churchill has a patent Glenoid Anchor Post licensed to Tornier Inc.
Dr. Edwards reports personal fees and non-financial support from Wright Medical Inc., during the conduct of the study; personal fees and non-financial support from Wright Medical Inc., outside the submitted work; and royalties and consulting fees from Wright Medical Inc. & DJO.
Dr. Evans reports other from DePuy-Johnson and Johnson, outside the submitted work.
Dr. Fehringer reports grants from University of Nebraska Medical Center, other from Wright Medical, during the conduct of the study.
Dr. Kelly reports other from Wright Medical, during the conduct of the study; personal fees and other from Wright Medical, outside the submitted work.
Dr. Norris reports personal fees and other from Wright Medical, during the conduct of the study.
Dr. Spencer reports personal fees from Tornier/Wright, outside the submitted work.
Dr. Wirth reports other from DePuy-Johnson and Johnson, other from Wright Medical, other from Elsevier, grants from Arthrex, outside the submitted work. In addition, Dr. Wirth has a patent with royalties paid.
Additional information
Level of Evidence: Level IV Therapeutic
Investigation performed at University of Washington Department of Orthopedics and Sports Medicine, Seattle WA
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Matsen, F.A., Iannotti, J.P., Churchill, R.S. et al. One and two-year clinical outcomes for a polyethylene glenoid with a fluted peg: one thousand two hundred seventy individual patients from eleven centers. International Orthopaedics (SICOT) 43, 367–378 (2019). https://doi.org/10.1007/s00264-018-4213-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-4213-3