Abstract
Purpose
The physical examination and pelvic imaging with MRI are often used in the pre-operative evaluation of pelvic organ prolapse. The objective of this study was to compare grading of prolapse on defecography phase of dynamic magnetic resonance imaging (dMRI) with physical examination (PE) grading using both the Pelvic Organ Prolapse Quantification (POP-Q) staging and Baden–Walker (BW) grading systems in the evaluation of pelvic organ prolapse (POP).
Methods
We retrospectively reviewed the charts of 170 patients who underwent dMRI at our institution. BW grading and POP-Q staging were collected for anterior, apical, and posterior compartments, along with absolute dMRI values and overall grading of dMRI. For the overall grading/staging from dMRI, BW, and POP-Q, Spearman rho (ρ) was used to assess the correlation. The correlations between dMRI grading and POP-Q staging were compared to the correlations between dMRI grading and BW grading using Fisher’s Z transformation.
Results
A total of 54 patients were included. dMRI grading was not significantly correlated with BW grading for anterior, apical, and posterior compartment prolapse (p > 0.15). However, overall dMRI grading demonstrated a significant (p = 0.025) and positive correlation (ρ = 0.305) with the POP-Q staging system. dMRI grading for anterior compartment prolapse also demonstrated a positive correlation (p = 0.001, ρ = 0.436) with the POP-Q staging derived from measurement locations Aa and Ba. The overall dMRI grade is better correlated with POP-Q stage than with BW grade (p = 0.024).
Conclusion
Overall and anterior compartment grading from dMRI demonstrated a significant and positive correlation with the overall POP-Q staging and anterior compartment POP-Q staging, respectively. The overall dMRI grade is better correlated with POP-Q staging than with BW grading.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Pelvic floor disorders (PFD), such as urinary incontinence, voiding dysfunction, and pelvic organ prolapse, are prevalent in US women, with up to 25% of women reporting some symptoms of the disease [1] and up to 75% of women with PFD reporting that their symptoms negatively affected their quality of life [2]. The severity of pelvic organ prolapse is typically evaluated with physical exam (PE). However, an accurate physical exam can be limited by patient-related factors and can be subjective, with the quality of an exam depending on the physician performing it [3]. Additionally, clinical examination alone may not reliably differentiate between rectocele and enterocele and may misdiagnose (likely underdiagnosing) the severity of the prolapse [4, 5].
Introduced in 1996, the Pelvic Organ Prolapse Quantification system (POP-Q) is a physical exam technique developed to provide an objective, site-specific protocol for describing, quantifying, and staging pelvic support [6]. The system has been found to be reproducible and also provides a precise method of communicating physical exam findings of pelvic organ prolapse [6, 7]. The POP-Q staging system has since been formally adopted as the standard for describing prolapse by the International Continence Society, the American Urogynecologic Society, and the Society of Gynecologic Surgeons [8]. The Baden–Walker (BW) halfway grading system, another physical exam system commonly used to classify prolapse disease, grades prolapse on a scale of 0 to 4 based on the relationship of the prolapsed anatomic structure to the hymen [3]. However, POP-Q remains the gold standard for physical exam by multiple gynecological societies [8].
Dynamic pelvic MRI (dMRI) is an objective radiologic method used to evaluate the pelvic floor, particularly as part of the pre-operative assessment [3]. It is a multiphase imaging protocol with imaging acquired at rest, during straining/Valsalva, and defecography after instillation of vaginal and rectal gel. The defecography or evacuation phase involves expulsion of rectal contrast, which simulates physiologic conditions contributing to the pelvic organ prolapse and may visualize prolapse that is not apparent when the external sphincter is closed and the pelvic floor is contracted. A previous study at this institution, which compared the dMRI defecography phase of the pelvic floor to physical exam using the BW classification system for evaluation of pelvic organ prolapse, found that dMRI was well correlated to physical exam (using the BW grading system) for anatomically significant prolapse in the anterior and posterior compartment [3]. The objective of this current study was to expand on that work by including a patient cohort containing both BW and POP-Q data, allowing the comparison of dMRI with PE using both the BW and POP-Q classifications systems.
Materials and methods
Human subjects
This study was conducted in adherence to a HIPAA compliant, IRB reviewed protocol. 170 patients with pelvic organ prolapse who were evaluated in our pelvic floor clinic from 2015 to 2019 were identified. These patients were evaluated by one of two attending surgeons performing female pelvic medicine and reconstructive surgical (CT or JF) procedures, with the majority of patients being evaluated by one attending (CT). A retrospective chart review was performed evaluating for physical exam findings, dMRI measurements, and other clinical data. We excluded patients who did not have a complete PE using the POP-Q system, did not have a complete PE using the BW system, or did not have a dMRI performed. 65 patients were eligible for inclusion. Of these 65 patients, 11/65 (16.9%) patients were excluded because the dMRI interpretation recorded only the presence or absence of cystocele, rectocele or vaginal vault prolapse, but not the absolute value or overall grade. Ultimately, data from 54 patients were analyzed. All data were stored in a HIPPA compliant database.
Clinical symptoms
Clinical data collected included age, hysterectomy status, parity, prior prolapse repair surgery, and the presence of obstructive or irritative voiding symptoms, as well as the presence of incontinence. Also evaluated was in-office urinalysis results and post void residual volume.
Patient preparation for dynamic pelvic MRI
Our institutional protocol for dynamic pelvic MRI was used to image all 54 patients included in the study. Women were requested not to evacuate their bladder for at least one hour prior to imaging to achieve adequate bladder distention. Detailed instructions related patient participation in the different phases of dynamic MRI were explained to the patients, including defecography phase (expulsion of rectal gel). Patients were put in left lateral decubitus position on the MR scanner table and Ultrasound (US) gel was inserted into rectum and vagina. A vaginal gel was used because vaginal prolapse is better demonstrated with this gel, which is water-based intraluminal contrast. Approximately 200–300 cc of (US) gel was put in the rectum using plastic enema bottles (Medi-Dose EPS, Ivyland, Pennsylvania), and a smaller amount (≫ 10–20 cc) of gel was instilled into the vagina via a 20 cc plastic syringe. Every patient was also given an adult diaper to contain the rectal gel following expulsion during the defecography phase [3]. Patients were scanned in supine position.
MR image acquisition
MR defecography exams were performed on 1.5 T or 3.0 T system (Magnetom Aera/Skyra, Siemens Healthineers, Erlangen, Germany), with 18 channel body phased array anterior coil and a 32-channel table-integrated posterior coil for signal reception. Scanners were equipped with 45 mT/m gradients operating at a slew rate of 200 T/m/s. Evaluation of the dynamic pelvic floor motion was done on balanced steady state free precession sequences in the mid-sagittal plane (FOV 400 × 375, 256 matrix, 7 mm slice thickness, TR/TE/flip angle 3.6 ms/1.8 ms/60°, PAT factor = 2), with cine acquisitions acquired over a 30-s time period during defecation (Table 1) [3].
MR image analysis
Dynamic MR examinations were reviewed in consensus by two body MRI fellowship trained attending radiologists specifically for this study. The studies were anonymized on a workstation with image review software (Intellispace version 4.4, Philips Healthcare, Andover, MA). Quantification of pelvic floor prolapse was done using HMO grading system (H-line, M-line, organ prolapse grading system) at rest and defecation [9]. All images were evaluated for adequate evacuation of rectal gel.
Using mid-sagittal plane in steady state free precession sequence, the pubococcygeal line (PCL) was marked from the inferior margin of the symphysis pubis to the junction between the first and second coccygeal vertebrae. Following the PCL, the H-line, M-line and O-line were drawn on the images to evaluate organ prolapse. The H-line (the puborectal line), measures the distance between the inferior margin of the symphysis pubis and the posterior aspect of the puborectalis muscle sling along the long axis of the puborectalis muscle. The M-line is the shortest perpendicular between the PCL and H-lines depicting posterior pelvic floor motion in form of ano-rectal junction prolapse. Descent of more than 2.5 cm below the PCL, corresponding to the M-line is considered abnormal [10,11,12] (Table 2; Fig. 1).
Additionally, vaginal vault prolapse, cystocele and rectocele were also looked for during dynamic imaging. Organ prolapse (O line) was used to identify and categorize cystocele, when a portion of the bladder prolapsed below the PCL (Fig. 2). Utero-vaginal prolapse or vaginal vault prolapse (apical prolapse) was also measured with respect to PCL (Table 2). Rectocele was defined as anterior bulging (> 1 cm) of the anterior wall of the rectum compared to static imaging. Both ano-rectal junction decent and rectocele were assessed in the posterior compartment [10,11,12]. Enterocele, sigmoidocele, and peritoneocele were evaluated in every case on MRI.
A 42-year-old female, post hysterectomy with pelvic pain and urinary symptoms. Balanced steady state free precession MR images acquired in static (a) and defecography phase (b) reveals global tricompartment prolapse. At rest, pubo-coccegeal line (PCL, red-line) is a reference line drawn from the inferior margin of the symphysis pubis to the junction between the first and second coccygeal vertebrae. The H-line (the puborectal line, green color), measures the distance between the inferior margin of the symphysis pubis and the posterior aspect of the puborectalis muscle sling along the long axis of the puborectalis muscle (not shown in mid-sagittal plane). The M-line (blue line) is the shortest perpendicular between the PCL and H-lines depicting posterior pelvic floor motion in form of ano-rectal junction prolapse, which is normal here measuring 2 am. In comparison to rest, on defecography phase (Fig. 1b) pelvic floor organs decent inferiorly below pubo-coccegeal line (PCL, red-line). A large cystocele (6 cm, arrow) with urethral hypermobility is seen (dashed arrow). Vagina descents below the PCL (arrowhead) from its position at rest (above the PCL). Severe ano-rectal junction prolapse is also demonstrated with M-line measuring 7.3 cm. Physical examination revealed grade 3 anterior compartment prolapse, grade 2 apical (vaginal vault) prolapse, and grade 1 posterior compartment prolapse using the BW grading system. Using the POP-Q staging system, this patient exhibited overall Stage II prolapse
Baden–Walker halfway grading system
The BW halfway grading system is commonly used to grade pelvic organ prolapse [13]. The extent of prolapse is recorded by using a grade from the number 0 to 4, using the hymen as a fixed anatomic reference point [14]. Cystocele, vaginal vault prolapse, rectocele, and enterocele can all be scored using the BW grading system (Table 3) [3].
POP-Q staging
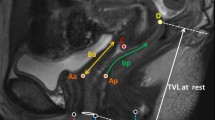
Pelvic Organ Prolapse has been defined by the International Urogynecological Association/International Continence Society (IUGA/ICS) as a departure from normal sensation, structure, or function, experienced by the woman in reference to her pelvic organs [15]. The POP-Q system provides an objective, site-specific system for describing, quantifying, and staging pelvis support in women using six defined points in the vagina measured during maximal Valsalva or cough in relation to the hymen [8]. Additionally, it provides a standardized tool for documenting, comparing, and communicating clinical findings with proven inter-observer and intra-observer reliability [7, 14] (Fig. 3).
A 76-year-old female with stress incontinence. Balanced steady state free precession MR images acquired in static (a) and defecography phase (b) show global pelvic floor prolapse during the dynamic phase. Moderate cystocele (5.5 cm) is seen with bladder prolapse below the PCL, in addition to urethral hypermobility. Moderate cervical decent (4.8 cm) is also seen (arrow). Posterior compartment prolapse in form of small rectocele (curved arrow) and ano-rectal junction prolapse (8 cm) is also demonstrated. Physical examination revealed grade 3 anterior compartment prolapse, grade 2 apical (vaginal vault) prolapse, and no posterior compartment prolapse using the BW grading system. Using the POP-Q staging system, this patient exhibited overall Stage I prolapse
Using the POP-Q staging system, prolapse of each compartment is staged based on its relationship to the hymen (Table 4) [16]. For this paper, anterior compartment prolapse was staged as the maximum of the stage determined for locations Aa and Ba. Similarly, posterior compartment prolapse was staged using locations Ap and Bp, and apical prolapse was staged using locations C and D (if present) (Fig. 1). Overall stage was determined using the prolapse stage of the leading edge, then confirmed using an interactive online tool provided by the American Urogynecologic Society (https://www.augs.org/patient-services/pop-q-tool-interactive).
Statistical methods
All continuous variables were tested for normal distribution (Shapiro–Wilk’s test) and appropriate summary statistics were obtained. Categorical and ordinal variables were numerically coded. For the ordinal grading/staging from dMRI, BW and POP-Q, Spearman rho (ρ) was used to assess the correlation. The correlation coefficients were tested to determine if they significantly differed from zero. The correlations between dMRI grading and POP-Q staging were compared to the correlations between dMRI grading and BW grading using Fisher’s Z transformation. Effects associated with p < 0.05 were considered statistically significant. All analyses were performed using statistical software (SAS® version 9.4, SAS Institute Inc., Cary, NC).
Results
54 patients were included in the final cohort. The average age was 68.5 years. 57.4% (31/54) of patients had previously undergone a hysterectomy, and 38.5% (20/52) of patients, with data available, had undergone prolapse or incontinence surgery in the past. A wide range of symptoms was noted during evaluation, including stress incontinence in 48.2% (26/54). Bothersome prolapse symptoms were noted in 96.2% (51/53) of patients. Obstructive voiding symptoms were present in 48.1% (25/52) of patients with data available. The patient characteristics, symptoms and clinical presentation are summarized in Table 5.
The H-line and M-line measurements from dMRI satisfied the normality assumption (p > 0.055, Shapiro–Wilk’s test). The mean ± SD were 8.2 ± 1.6 cm and 5.3 ± 1.7 cm for H-line and M-line, respectively. None of the POP-Q measurements satisfied the normality assumption (p < 0.023, Shapiro–Wilk’s test). None of the patients were stage IV using POP-Q. There were 4 patients (4/54; 7.4%) who were grade 0 on dMRI, whereas none were grade/stage 0 on either BW grading or POP-Q staging (Table 6). Summary data for the dMRI grading and clinical staging using POP-Q and BW systems are provided in Table 6. For dMRI anterior compartment prolapse grading of 0 through 3, the median (interquartile range, IQR) of corresponding Aa and Ba from POP-Q were − 2 (− 2.5, 1) cm and 0 (− 2.5, 1) cm for dMRI grade 0; − 2.5 (− 3, − 1.5) cm and 0 (− 0.75, 1.25) cm for dMRI grade 1; 0 (− 1, 1) cm for both Aa and Ba in dMRI grade 2; and, − 0.5 (− 1, 0.75) cm and 2.5 (1.5, 3) cm for dMRI grade 3, respectively. For dMRI apical prolapse grading of 0 through 3, the median (IQR) of corresponding C and D (if reported) from POP-Q were 1 (1, − 4) cm and 1, (1, − 6.625) cm for dMRI grade 0; − 5.25 (− 6.75, − 3.625) cm and − 7.25 (− 9.375, 6.625) cm for dMRI grade 1; − 5 (− 6.125, 3.625) cm and − 6 (− 7, − 5) cm for dMRI grade 2; and, 5.5 (4.75, 6.25) cm and 7 (7, 7) cm for dMRI grade 3, respectively. For dMRI posterior compartment prolapse grading of 0 through 3, the median (IQR) of corresponding Ap and Bp from POP-Q were − 3 (− 3, − 2) cm for both Ap and Bp in dMRI grade 0; − 2.25 (− 2.625, − 1.625) cm and − 2 (− 2.5, − 1.5) cm for dMRI grade 1; − 2.25 (− 2.875, − 1) cm for both Ap and Bp in dMRI grade 2; and, − 3 (− 3, − 2) cm for both Ap and Bp in dMRI grade 3, respectively.
The correlation (Spearman rho) between BW grading and POP-Q staging is summarized in Table 7. The diagonal elements in Table 7 show there is a significant correlation between BW grading and POP-Q staging for anterior, apical and posterior compartments and for overall stage (p ≤ 0.004). The correlation (Spearman rho) between dMRI grading and clinical grading/staging is summarized in Table 8. dMRI grading was not significantly correlated with BW grading for anterior, apical and posterior compartment prolapse (p > 0.15, 2nd column, Table 8) in this cohort. The overall grade from dMRI demonstrated a significant (p = 0.025) and a positive correlation (ρ = 0.305) with the POP-Q stage (3rd column, Table 8). dMRI grading for anterior compartment prolapse also demonstrated a significant and positive correlation (ρ = 0.436, p = 0.001) with the POP-Q stage derived from measurement locations Aa and Ba (3rd column, Table 8). The overall dMRI grade is better correlated with the POP-Q stage than with the BW grade (p = 0.024, 4th column, Table 8).
Discussion
Accurate diagnosis of abnormalities of the pelvic floor is imperative in planning reconstructive procedures in order to minimize the risk of recurrence and re-operation [17]. One study found that women who undergo surgery for POP disease are subjected to a re-operation rate of 13%, which further emphasizes the importance of an accurate initial diagnosis [18]. While physical exam is the primary modality used by physicians to evaluate the severity of pelvic organ prolapse, it is not without its limitations. To start, it can be difficult to determine which structure is located behind the vaginal epithelium, especially in the posterior compartment [17]. Additionally in the setting of significant vaginal prolapse, it can be difficult to differentiate among cystocele, enterocele, and rectocele by physical exam alone [9].
Dynamic pelvic MRI has been previously shown to be an important additional tool in the evaluation of pelvic organ prolapse prior to surgical intervention [19]. A dMRI however is not without its limitations, among them that it is expensive, not universally available, not physiologic (defecation in supine position), which can be burdensome and embarrassing. However, vaginal speculum exam in lithotomy position is also arguably non-physiologic and embarrassing. A previous study at this institution found that dMRI demonstrated good correlation to PE using the BW classification system for anatomically significant prolapse in anterior and posterior compartments [3]. The results of that study indicated that physical exam using the BW halfway grading system, particularly in the anterior compartment, provided similar information to that obtained by dMRI. The current study aimed to expand on that study and evaluate the correlation, if any, between dMRI and PE using both the POP-Q and BW classification systems, since the POP-Q system is currently the gold standard for evaluation worldwide [8].
Anterior compartment analysis demonstrated positive correlation between dMRI grading and POP-Q staging (ρ = 0.436, p = 0.001). However, there was no significant correlation seen between dMRI grading and BW grading for the anterior compartment, which is inconsistent with our previous findings that did find a significant correlation [3]. This is likely an effect of sample size and the greater power of our prior study (178 patients versus 54 patients) leading to incongruent results. Overall, this study and our previous study suggest that dMRI and physical exam correlate well in the anterior compartment. Additionally, the current study found that the BW grading and POP-Q staging systems are well correlated with each other, likely providing similar subjective information.
While no statistically significant difference was seen when analyzing the correlation between dMRI grade, BW grade, and POP-Q stage in the apical and posterior compartments, overall dMRI grade was found to be better correlated to POP-Q stage than BW grade (p = 0.024). The results of this study suggest that both physical exam and dMRI may provide different information to the surgeon, and therefore each has a potential role in the pre-operative evaluation. Providers performing BW grading as their primary physical exam technique may have the most to gain from dMRI, as the results show that the two are not correlated, particularly in the apical and posterior compartments [3], and therefore additional anatomic information or identification of additional prolapse may be provided by imaging. The correlation between dMRI grading and overall POP-Q staging suggests that POP-Q may be the more objective and more accurate physical exam system at classifying vaginal prolapse when compared to BW grading. Additionally, the lack of statistically significant correlation between dMRI grading and POP-Q staging in the apical and posterior compartments alone suggests that dMRI may provide additional anatomic information within these vaginal compartments.
The strengths of this study are the standardized dMRI protocol, and the inclusion of both BW and POP-Q data in the dataset. Also, nearly all POP-Q exams were performed by a single urologic surgeon which decreases the possibility that results were skewed by inexperience or inter-observer variability. Finally, the POP-Q exam is considered the gold standard by multiple gynecologic and incontinence societies, and its addition to this study is an important distinction from the previous study performed at this institution.
This study is not without its limitations. This study sample size was relatively small with 54 patients. Post-hoc power analysis indicated that the sample size of 54 subjects was sufficient to achieve a statistical power of at least 80%, provided the correlation coefficient was 0.38 or higher (Fisher’s Z test, two-sided, α = 0.05). Thus, the sample size was adequate to determine even a weak correlation, which generally corresponds to a correlation coefficient range of 0.3 to 0.5. The sample size was sufficient to detect significant correlations between BW and POP-Q. Additionally, none of the patients in the study demonstrated Stage IV prolapse using the POP-Q staging system, however some did have grade 4 prolapse using the BW grading system and were re-classified after the POP-Q staging exam was performed. Although prolapse bother was assessed, more specifics with regards to most bothersome symptomatology, such as fecal incontinence, stool trapping, dyspareunia, etc., were not included.
Conclusion
Dynamic pelvic MRI grading demonstrated a significant and positive correlation with the POP-Q staging system and is better correlated with the POP-Q staging system than the BW grading system. Also, dMRI grading for anterior compartment prolapse demonstrated a significant and positive correlation with the POP-Q staging derived from measurement locations Aa and Ba. Providers should continue to perform regular physical exams as part of the pre-operative assessment and may consider imaging with dMRI, as both methods of evaluation may provide different and valuable information.
References
Nygaard, I., et al., Prevalence of symptomatic pelvic floor disorders in US women. JAMA, 2008. 300(11): p. 1311-6.
Mouritsen, L. and J.P. Larsen, Symptoms, bother and POPQ in women referred with pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct, 2003. 14(2): p. 122-7.
Lin, F.C., et al., Dynamic Pelvic Magnetic Resonance Imaging Evaluation of Pelvic Organ Prolapse Compared to Physical Examination Findings. Urology, 2018. 119: p. 49-54.
Arif-Tiwari, H., et al., Improved Detection of Pelvic Organ Prolapse: Comparative Utility of Defecography Phase Sequence to Nondefecography Valsalva Maneuvers in Dynamic Pelvic Floor Magnetic Resonance Imaging. Curr Probl Diagn Radiol, 2019. 48(4): p. 342-347.
Elshazly, W.G., A.l.A. El Nekady, and H. Hassan, Role of dynamic magnetic resonance imaging in management of obstructed defecation case series. Int J Surg, 2010. 8(4): p. 274-82.
Muir, T.W., K.J. Stepp, and M.D. Barber, Adoption of the pelvic organ prolapse quantification system in peer-reviewed literature. Am J Obstet Gynecol, 2003. 189(6): p. 1632-5; discussion 1635-6.
Hall, A.F., et al., Interobserver and intraobserver reliability of the proposed International Continence Society, Society of Gynecologic Surgeons, and American Urogynecologic Society pelvic organ prolapse classification system. Am J Obstet Gynecol, 1996. 175(6): p. 1467-70; discussion 1470-1.
Bump, R.C., et al., The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol, 1996. 175(1): p. 10-7.
Comiter, C.V., et al., Grading pelvic prolapse and pelvic floor relaxation using dynamic magnetic resonance imaging. Urology, 1999. 54(3): p. 454-7.
Yang, A., et al., Pelvic floor descent in women: dynamic evaluation with fast MR imaging and cinematic display. Radiology, 1991. 179(1): p. 25-33.
El Sayed, R.F., et al., Magnetic resonance imaging of pelvic floor dysfunction - joint recommendations of the ESUR and ESGAR Pelvic Floor Working Group. Eur Radiol, 2017. 27(5): p. 2067-2085.
Pannu, H.K., Dynamic MR imaging of female organ prolapse. Radiol Clin North Am, 2003. 41(2): p. 409-23.
Baden WF, W.T., Surgical repair of vaginal defects. 1992, Lippincot: Philadephia. p. 161-174, 1950198, 235-238
Persu, C., et al., Pelvic Organ Prolapse Quantification System (POP-Q) - a new era in pelvic prolapse staging. J Med Life, 2011. 4(1): p. 75-81.
Haylen, B.T., et al., An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic organ prolapse (POP). Int Urogynecol J, 2016. 27(4): p. 655-84.
Madhu, C., et al., How to use the Pelvic Organ Prolapse Quantification (POP-Q) system? Neurourol Urodyn, 2018. 37(S6): p. S39-S43.
Rodríguez, L.V. and S. Raz, Diagnostic imaging of pelvic floor dysfunction. Curr Opin Urol, 2001. 11(4): p. 423-8.
Clark, A.L., et al., Epidemiologic evaluation of reoperation for surgically treated pelvic organ prolapse and urinary incontinence. Am J Obstet Gynecol, 2003. 189(5): p. 1261-7.
Colaiacomo, M.C., et al., Dynamic MR imaging of the pelvic floor: a pictorial review. Radiographics, 2009. 29(3): p. e35.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pollock, G.R., Twiss, C.O., Chartier, S. et al. Comparison of magnetic resonance defecography grading with POP-Q staging and Baden–Walker grading in the evaluation of female pelvic organ prolapse. Abdom Radiol 46, 1373–1380 (2021). https://doi.org/10.1007/s00261-019-02313-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-019-02313-8