Abstract
Purpose
To retrospectively evaluate the ability of computed tomographic (CT) findings to discriminate nutcracker syndrome (NCS) from asymptomatic nutcracker phenomenon (NCP) and to investigate the diagnostic value of CT findings in diagnosis of NCS.
Methods
From January 2014 to April 2015, 216 patients who underwent initial urographic CT were included. Initially, 216 patients were categorized as “nutcracker” or “normal,” based on the following CT criteria: (1) the presence of beak sign and (2) hilar-aortomesenteric left renal vein diameter ratio >4. Patients who satisfied both of these criteria were diagnosed with nutcracker. The nutcracker was then divided into “NCS” and “asymptomatic NCP” based on the presence of characteristic symptoms. CT findings in sagittal and axial scans of corticomedullary phase were evaluated. Multivariate analysis was used to identify significant factors among 30 NCS, 51 asymptomatic NCP, and 135 normal patients. Diagnostic performance and threshold using receiver operating characteristic (ROC) curve were calculated.
Results
A total of 131 males and 85 females, with mean age of 38.6 years (range 18–89 years), were included. Multivariate analysis demonstrated superior mesenteric artery (SMA)-aortic angle (p < 0.001) and visualization of a dilated collateral vein with reflux (p = 0.001) were independent factors for distinguishing NCS from asymptomatic NCP. The combination of SMA-aortic angle <25° and visualization of a dilated collateral vein with reflux provided the greatest diagnostic accuracy (area under the ROC curve, 0.841).
Conclusions
The combination of SMA-aortic angle and visualization of a dilated collateral vein with reflux in multidetector CT can be useful to differentiate NCS from asymptomatic NCP.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Renal nutcracker syndrome (NCS), also referred to as left renal vein (LRV) entrapment syndrome, indicates compression of the LRV between the superior mesenteric artery (SMA) and the aorta, with characteristic clinical symptoms [1]. This condition is also known as “anterior nutcracker syndrome.” If the LRV is compressed between the aorta and a vertebral body, it is referred to as “posterior nutcracker syndrome” [2]. This compression leads to increased pressure in the LRV with subsequent development of venous varicosities surrounding the renal pelvis, ureter, and the gonadal vein [3]. Hematuria is the most commonly reported symptom and is attributed to rupture of thin-walled varices into the collecting system due to elevated venous pressure. NCS affects young women more frequently; however, the incidence of NCS is unknown [1].
Nutcracker phenomenon (NCP) indicates entrapment of the LRV between the SMA and the aorta, with or without characteristic clinical symptoms [3]. Symptomatic NCP is referred to as NCS [4]. However, NCP is not always associated with clinical symptoms, in which case it is also called asymptomatic NCP, and is regarded as a finding of a normal variant [5, 6]. NCP also affects young women more frequently; however, its exact prevalence is unknown due to an absence of consensus with respect to diagnostic criteria of NCP [1]. The estimated incidences of NCP using multidetector computed tomography (MDCT) have been reported as 10.9% and 27.3% in two previous studies [4, 7].
The most common etiology of renal vein entrapment is compression of the LRV, resulting from an acute SMA-aortic angle (<35°), leading to venous congestion of the left kidney [8]. Other etiologies, such as an abnormal origin [9] or abnormal branching of the SMA from the aorta [10], ptosis of the left kidney [11], preaortic fibrous tissue [12], and duodenal interposition [13], have also been described. Recently, Yun et al. [14] reported that the presence of the liver and pancreas at the LRV level was an independent factor for discriminating NCS from normal patients.
At present, differentiation between NCS and asymptomatic NCP is made based upon clinical diagnosis and is made only when hematuria is present. Based on our experience, LRV entrapment is often detected on urographic CT scanning in patients with non-specific symptoms of NCS, such as abdominal pain. It is unclear whether this symptom is caused by NCS or is unassociated with NCS. However, there has been no investigation on differences between NCS and asymptomatic NCP in imaging findings in urographic CT. Accordingly, the purpose of this study was to identify relevant CT findings able to discriminate NCS from asymptomatic NCP and to investigate the diagnostic values of these relevant CT findings in the diagnosis of NCS.
Materials and methods
Study population
This retrospective study was approved by our hospital’s institutional review board. Patients’ informed consent was waived for medical record review. Collection of data and information was performed by one independent radiologist (J.M.L.) based on PACS (Piview Star, Infinitt Healthcare, Seoul, Korea) and electronic medical records. The inclusion criteria were (1) adult patients (≥18 years) and (2) initial urographic CT for the evaluation of possible urologic problems between January 2014 and April 2015. Pediatric patients (<18 years) were not included, because pediatric patients with urologic problems underwent ultrasound initially or 2 weeks later after conservative treatment, rather than urographic CT, in accordance with our institute’s routine protocol as of April 2009. Ultimately, a total of 419 patients were found eligible to participate.
The sole exclusion criterion was other definite urologic conditions, such as trauma, stone, or neoplasm. Of the 419 total patients, 198 were excluded for definite urologic conditions, including trauma (n = 12), stones in urinary systems (n = 69), acute pyelonephritis (n = 40), cystitis (n = 18), renal cell carcinoma (n = 16), transitional cell carcinoma (n = 14), renal tuberculosis (n = 7), idiopathic ureteropelvic junction obstruction (n = 5), and congenital anomalies (n = 17). Five patients were also excluded because the arterial phase of the CT images was not obtained. The remaining 216 patients [mean age 38.6 ± 14.6 (standard deviation) years; range 18–89 years] enrolled in this study included 131 male (mean age 36.8 ± 13.4 years; range 18–85 years) and 85 female patients (mean age 40.2 ± 15.4 years; range 18–89 years).
Image acquisition
All MDCT examinations were performed using 16- or 64-slice MDCT scanner (Brilliance 16 or 64; Philips Medical Systems, Cleveland, OH, USA). All patients underwent craniocaudal scanning in the supine position during a single-held breath. For the 16-slice MDCT scanner, CT parameters were as follows: 120 kVp, 200 mAs, 1.188 pitch, 0.75 s per rotation, and 5 mm slice thickness. For the 64-slice MDCT scanner, the parameters were as follows: 120 kVp, 150 mAs, 0.891 pitch, 0.75 s per rotation time, and 5 mm slice thickness. In the corticomedullary phase, sagittal images were additionally reconstructed with a thickness of 3 mm in 3 mm increments.
Precontrast, corticomedullary, nephrographic, and excretory MDCT images were obtained using a 2 mL/kg dose of iopamidol (Pamiray 370; Dongkuk Pharm, Seoul, Korea) which was administered intravenously followed by a flush of 40 mL saline. For corticomedullary phase scanning, a delay of 15 s was fixed after aorta attenuation reached 200 Hounsfield units according to bolus tracking. For nephrographic phase scanning, a delay of 55 s was fixed after corticomedullary scanning. For excretory phase scanning, a delay of 5 min was fixed after infusion of the contrast media.
Reference standard of final diagnosis
The final diagnosis was determined using urographic CT and electronic medical records. Initially, two board-certificated radiologists, each with 14 (D.H.N.) or 12 (J.K.R.) years of experience, interpreted the urographic CT data using PACS and categorized the patients as “nutcracker” or “normal” by consensus with reference to previously published CT findings for NCS [13, 15]. The diagnostic criteria for the nutcracker group were as follows: (1) ratio of hilar-aortomesenteric LRV diameter >4.0 and (2) the presence of beak sign in all phases. Patients who satisfied both criteria were diagnosed with nutcracker syndrome. In axial images of the corticomedullary phase, the LRV diameter was measured at both the renal hilum and aortomesenteric space (AMS) (Fig. 1a). To ensure objectivity, reviewers used ~×2-magnified CT images and carefully located points on vessel walls. Beak sign was defined as an acute angle formed by the anterior and posterior walls of the narrowing segment of the LRV at the AMS [15]. Thereafter, one physician (S.H.L.), who was not involved in the data collection or image interpretation, divided the nutcracker group into NCS or asymptomatic NCP patients based on the presence of common characteristic symptoms (hematuria, left flank/pelvic pain, or proteinuria) [1] as listed in electronic medical records. Hematuria was considered present if macroscopic, or, if microscopic, with ≥3 red blood cells per high-powered field [16]. Proteinuria was defined as 30 mg/dL or more (≥1+) for scoring purposes [17]. Ultimately, a total of 216 patients were included and divided into three groups: NCS, asymptomatic NCP, and normal.
Measurement of the ratio of hilar-aortomesenteric left renal vein (LRV) diameter, D AMS, AMA, D APW, D AW, and LRV ptosis. A The ratio of hilar-aortomesenteric LRV diameter is measured using the largest diameter of the LRV (line) at the renal hilum (circle) and the smallest diameter of the LRV (dotted line) at the aortomesenteric space (box). To calculate the ratio of hilar-aortomesenteric LRV, the largest diameter of hilar LRV is divided by the smallest diameter of aortomesenteric LRV. B D AMS is defined as the shortest distance between the aorta and the superior mesenteric artery (SMA) at the LRV level (line A). D APW is defined as the largest spanned height of the abdomen (line B). D AW is defined as the shortest distance between the outer margin of the anterior abdominal wall and the anterior wall of the aorta (line C). D APW and D AW are perpendicular to the outer margin of the posterior abdominal wall. C AMA is defined as the angle between the straight midline of the aorta, which is perpendicular to the outer margin of the posterior abdominal wall, and the straight midline of the aorta-SMA at the LRV level (angle D). LRV ptosis is defined as the angle between the straight midline of the aorta and the straight midline of the LRV at the left renal hilar level (angle E)
Imaging analysis
All CT scans of the corticomedullary phase were evaluated retrospectively by one independent radiologist (S.J.Y.) who were not involved in image evaluation. The reviewers were unaware of any patient information, including final diagnoses. The reviewer performed the evaluations in a random order, irrespective of CT study date, using PACS. All measurements were obtained using electronic calipers in PACS. All measurements were obtained three times in ~×2-magnified CT images and average values were calculated.
The SMA-aortic angle was evaluated in sagittal scan. Based on a previous study [18], the SMA-aortic angle was defined as the angle between vertex, the SMA ray, and the aorta ray; the vertex refers to the SMA origin. SMA ray is a line drawn between the vertex and a 1 cm distance point from the vertex along the posterior wall of SMA. Aorta ray is between the vertex and a 1 cm distance point from vertex along the anterior wall of aorta. If the SMA-aortic angle did not lie on the true sagittal scan, the angle was measured using oblique sagittal reconstructed images in a workstation in order to provide an accurate angle measurement between the SMA and aorta (Fig. 2).
Measurement of superior mesenteric artery (SMA)—aortic angle on a corticomedullary phase oblique sagittal reconstructed image in a workstation. The angle (angle A) was measured by defining the origin of the SMA and two points, a distance of 1 cm after its origin along the posterior wall of the SMA (line B), and a distance of 1 cm after its origin along the anterior wall of the abdominal aorta (line C)
In axial scans, the following were noted: (1) whether or not the liver or pancreas was visualized; (2) the shortest distance of the AMS (D AMS); (3) the aortomesenteric angle (AMA); (4) the shortest distance from the anterior abdominal wall to the posterior abdominal wall (D APW); (5) the shortest distance from the aorta to the anterior abdominal wall (D AW); (6) whether or not a dilated gonadal (>5 mm) or lumbar vein (>3 mm) with reflux was visualized; and (7) LRV ptosis (Fig. 1B, C). Evaluation of D APW and D AW was performed instead of BMI because BMI was not routinely checked for outpatients. The reviewers stratified patients into the following four CT groups according to the presence of liver and/or pancreas at the LRV level by a modification of a previously published measurement method [14]: group LP, group L, group P, and group O. Based on published standards in the literature [19, 20], a gonadal vein was considered dilated if its maximal diameter was greater than 5 mm. A lumbar vein communicating with the LRV was considered dilated if the maximum diameter measured was greater than 3 mm [21]. Reflux of the gonadal (ovarian or testicular) or lumbar vein was defined as early opacification of the gonadal or lumbar vein in the corticomedullary phase [22].
Statistical analysis
To assess differences among NCS, asymptomatic NCP, and normal patients with regard to demographic characteristics and measured values, one-way analysis of variance with post hoc Tukey’s honest significant differences test was performed for continuous variables, and Chi-square test or Fisher’s exact test for non-continuous variables. To determine independent factors for the differential diagnosis between NCS and asymptomatic NCP, multivariate logistic regression analysis was applied. Multivariate logistic regression analysis was conducted on those variables that were found to be statistically significant on univariate analysis. Adjusted odds ratios (ORs) and 95% confidence intervals (CIs) were generated from multivariate analyses. Thereafter, to determine the diagnostic performance of significant variables for differentiation between NCS and asymptomatic NCP, a receiver operating characteristic (ROC) curve analysis was performed. Cut-off values of variables were determined for optimal area under the ROC curve (AUC), sensitivity, and specificity. p < 0.05 was considered statistically significant. Statistical analyses were conducted with SPSS 18.0 (SPSS Inc., Chicago, IL, USA).
Results
Patient characteristics
Of 216 patients, there were 30 NCS (13.9%), 51 asymptomatic NCP (23.6%), and 135 normal patients (62.5%). The mean age was 36.3 ± 12.4 years for NCS, 38.8 ± 12.2 years for asymptomatic NCP, and 40.3 ± 12.5 years for normal. Among NCS patients, 15 were male and 15 were female; for those with asymptomatic NCP, 25 were male and 26 were females; and for normal, 91 were male and 44 were females. In terms of age, NCS patients were significantly younger than asymptomatic NCP (p = 0.020) or normal (p < 0.001) ones. There was no significant difference between NCS and asymptomatic NCP patients (p = 0.932), or between NCS and normal (p = 0.072) patients in terms of gender distribution.
Of the 216 patients, all 30 NCS (100%) and 96 of 135 normal (71.1%) showed characteristic symptoms. Among 30 NCS, 16 (53.3%) microscopic hematuria with left flank pain/pelvic, 7 (23.3%) isolated macroscopic hematuria, and 7 (23.3%) isolated microscopic hematuria were seen. Proteinuria was not seen in NCS. Among 135 normal, 53 (39.3%) isolated left flank/pelvic pain, 34 (25.2%) isolated microscopic hematuria, 5 (3.7%) microscopic hematuria with left flank/pelvic pain, 2 (1.5%) microscopic hematuria with proteinuria, and 2 (1.5%) macroscopic hematuria were seen. All 126 patients with characteristic symptoms received conservative treatment at the time of the first follow-up after undergoing urographic CT. None of 51 asymptomatic NCP showed characteristic symptoms. The patients with asymptomatic NCP performed CT for the evaluation of right flank pain (n = 39) and the cause of secondary hypertension such as renal artery stenosis (n = 12).
Measured values among NCS, asymptomatic NCP, and normal patients
The measured values of NCS, asymptomatic NCP, and normal patients are described in Table 1. SMA-aortic angle (p = 0.002), D AMS (p = 0.006), D APW (p = 0.043), D AW (p = 0.023), and visualization of a dilated collateral vein with reflux (p < 0.001) were significantly different between NCS and asymptomatic NCP patients. However, the CT group was not significantly different (p = 0.180). Between NCS and normal patients, SMA-aortic angle (p < 0.001), CT group (p < 0.001), D AMS (p < 0.001), AMA (p = 0.012), D APW (p < 0.001), D AW (p < 0.001), and visualization of a dilated collateral vein with reflux (p < 0.001) were significantly different. Between asymptomatic NCP and normal patients, SMA-aortic angle (p < 0.001), CT group (p < 0.001), D AMS (p < 0.001), AMA (p = 0.018), D APW (p < 0.001), D AW (p < 0.001), and visualization of a dilated collateral vein with reflux (p < 0.001) were significantly different, as was the case between NCS and normal patients (Table 2).
Factors associated with the differential diagnosis of NCS and asymptomatic NCP
On multivariate logistic regression analysis, SMA-aortic angle (p < 0.001) and visualization of a dilated collateral vein with reflux (p = 0.001) were significant factors for the differential diagnosis of NCS and asymptomatic NCP patients. For each 1 degree of angle decrease, the risk of NCS increased 1.487-fold. When the collateral vein was seen, the risk of NCS increased 17.227-fold (Table 3).
Diagnostic performance of the significant factors of NCS
The cut-off value for optimal sensitivity and specificity was determined by ROC analysis, and the AUCs of significant factors are summarized in Table 4. When we set the cut-off values at 15° to 30°, SMA-aortic angle <25° showed the optimal AUC, sensitivity, and specificity, statistically (AUC, 0.784; sensitivity, 100%; specificity, 56.9%). Visualization of a dilated collateral vein with reflux had lower AUC (0.782), lower sensitivity (80.0%), and higher specificity (76.5%) than did those of the SMA-aortic angle. When both SMA-aortic angle <25° and visualization of a dilated collateral vein with reflux were combined, the highest AUC (0.841), sensitivity (80%), and specificity (88.2%) were obtained (Figs. 3, 4).
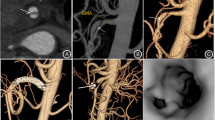
A 31-year-old woman with nutcracker syndrome. A A corticomedullary phase axial image demonstrates beak sign (arrow) and narrowed aortomesenteric left renal vein (LRV). The maximal diameter of aortomesenteric LRV is 1.89 mm (distance between two points of aorta and superior mesenteric artery). B A corticomedullary phase axial image shows dilated hilar LRV at the level of the renal pelvis (arrowhead). The maximal diameter of hilar LRV is 9.8 mm (distance between two points of hilar LRV). The hilar-aortomesenteric LRV diameter ratio was 5.1. C The left lumbar vein was found to be dilated to 5 mm (>3 mm) in diameter and with reflux (arrows). D A corticomedullary phase oblique sagittal reconstructed image shows a superior mesenteric artery (SMA)-aortic angle of 20.8 degrees and entrapped aortomesenteric LRV (asterisk)
A 19-year-old man with asymptomatic nutcracker phenomenon. A A corticomedullary phase axial image shows beak sign (arrow) and mildly narrowed aortomesenteric left renal vein (LRV). The maximal diameter of aortomesenteric LRV is 2.05 mm (distance between two points of aorta and superior mesenteric artery). B A corticomedullary phase axial image shows mildly dilated hilar LRV at the level of the renal pelvis (arrowhead). The maximal diameter of hilar LRV is 8.51 mm (distance between two points of hilar LRV). The hilar-aortomesenteric LRV diameter ratio was 4.2. There is no observation of dilated left testicular/lumbar vein with reflux. C A corticomedullary phase oblique sagittal reconstructed image shows a superior mesenteric artery (SMA)-aortic angle of 29.7 degrees and entrapped aortomesenteric LRV (asterisk)
Discussion
Among the various etiologies of NCS, it is widely accepted that the most common is a shorter D AMS and acute SMA-aortic angle than normal [8, 23]. However, the cited studies [8, 23] performed evaluations between NCS and normal patients, not between NCS and asymptomatic NCP patients. Through the results from our study, we found that there were significant differences in the SMA-aortic angle, D AMS, D APW, D AW, and visualization of a dilated collateral vein with reflux when comparing patients with NCS to asymptomatic NCP patients. Among these significant variables, SMA-aortic angle and visualization of a dilated collateral vein with reflux were detectable anticipatory factors. Notably, when SMA-aortic angle <25° and visualization of a dilated collateral vein with reflux were combined, this resulted in the most accurate diagnosis of NCS.
SMA originates from the abdominal aorta, then runs straight for 0.6–2.6 cm, and curves in a downward 90° angle [10, 24]. However, mean abnormal SMA-aortic angles vary from 8° to 39.3° [25–28]. In the recent study conducted by Arthurs et al. [18], they made the innovation of setting 25° in pediatric patients as the cut-off values between normal and abnormal SMA-aortic angle. In our study, a cut-off value of the SMA-aortic angle of less than 25° also provided optimal diagnostic performance NCP in adult patients for discriminating NCS from asymptomatic. However, an SMA-aortic angle <25° provided relatively low specificity, which means that, in many cases, asymptomatic NCP could not be excluded.
NCS is a spectrum of diseases, reflecting degrees of LRV compression [29]. As the compression of the LRV increases, the pressure in the LRV increases, leading collateral veins to decompress the renal vein occlusion [29]. Symptoms can resolve according to the state of collateral vein development [1]. According two previous reports [29, 30], reflux in gonadal or other collateral veins on CT or US were indirect findings of NCS. Our study yielded similar results that detected dilated collateral veins with reflux in 80.0% of NCS patients. However, visualization of dilated collateral veins without reflux by itself is of no use in diagnosing NCS, because dilation of the left gonadal or lumbar vein alone is present in 16% and 24% of asymptomatic patients, respectively [7]. Moreover, previous studies have reported that the left ovarian vein was dilated in 5% to 47% of asymptomatic women [22, 31].
In our study, dilated collateral vein with reflux was not seen in six (20%) NCS patients. It was thought that these patients might be in the early stage of NCS. According to a previous study [29], collateral veins cannot develop in the early stage of NCS, so they cannot reduce renocaval pressure, resulting in gross hematuria. However, if a dilated collateral vein with reflux were to be well developed even in the presence of LRV entrapment, it would present as partial or compensatory NCS without symptoms. The renocaval pressure gradient depends on the degree of compensatory collateral vein formation. If collateral veins are sufficient (compensatory NCS), symptoms such as hematuria can be relieved [1]. In our study, dilated collateral vein with reflux was seen in 12 (23.6%) patients with asymptomatic NCP, which may represent compensatory NCS. Thus, compensatory NCS may be included among the asymptomatic NCP patients in our study. Regretfully, radiological differentiation between asymptomatic NCP and compensatory NCS remains unreliable [29]. However, because compensatory NCS is the late stage of NCS, it could be differentiated by patients’ histories of previous symptoms.
It was noted for the first time in the study of Yun et al. [14] that CT results including the liver and pancreas were important in distinguishing between NCS and normal patients, as the liver and pancreas were frequently found in front of the LRV in NCS. This agrees with the findings of our study that 76.7% of NCS patients were assigned to group LP, while only 16.3% were normal. However, the frequency of assignment of NCS patients to group LP was slightly higher than that of asymptomatic NCP of NCS patients. The CT group had no significant difference between NCS and asymptomatic NCP rates, and thus CT group was not helpful in discriminating NCS from asymptomatic NCP.
We speculated that the finding of SMA-aortic angle <25° might be an appropriate initial evaluation factor for discrimination between NCS and asymptomatic NCP because it has the highest sensitivity in excluding normal patients from NCS patients. But as previously mentioned, it has low specificity in discriminating between NCS and asymptomatic NCP, and thus visualization of a dilated collateral vein with reflux may be needed as a secondary evaluation. If NCS is suspected rather than asymptomatic NCP in MDCT, it would be necessary for physicians to perform a detailed history-taking or urine analysis.
There are several limitations to our study. First, this study was inherently limited by its retrospective design and the small number of patient populations from a single institution. However, the results of this study might be applicable for the preliminary evaluation of significant factors discriminating NCS from asymptomatic NCP. Second, ultrasound or LRV venography, which are considered the most reliable methods for evaluating NCS, were not performed in our study because of their subjectiveness and invasiveness, respectively. Kim et al. [15] reported that CT provided excellent diagnostic accuracy for symptomatic NCS; they reported the AUC of CT to be 0.903. Third, we did not perform repeated CT scanning with postural change. It was reported that SMA-aortic angle vary between supine and upright positions using Doppler Ultrasound, with more narrowing of the SMA-aortic angle in the upright position, and more pronounced entrapment findings in patients with NCS [32]. It might be possible that we would miss the diagnosis of NCS as the CT scan was only obtained in supine position without additional positions. Fourth, although we could evaluate the initial treatments for all patients, we could not collect clinical and radiological follow-up for all patients to evaluate the efficacy of the treatments and any changes of SMA-aortic angle. The relationship between follow-up clinical and radiological studies after treatments may be necessary in future studies. Finally, consensus interpretation was used in this study, but intra- and inter-observer reliability were not assessed. However, this limitation does not at all undermine the results of our study. Specifically, the use of sliding slab ray-sum techniques on workstation would further support the argument that MDCT is useful for the diagnosis of NCS.
In conclusion, the combination of SMA-aortic angle and visualization of a dilated collateral vein with reflux in MDCT can be useful for discriminating NCS from asymptomatic NCP. It may allow clinicians to identify NCS patients and influence the choice of treatment.
References
Kurklinsky AK, Rooke TW (2010) Nutcracker phenomenon and nutcracker syndrome. Mayo Clin Proc 85:552–559
Fong JK, Poh AC, Tan AG, Taneja R (2014) Imaging findings and clinical features of abdominal vascular compression syndromes. Am J Roentgenol 203:29–36
Butros SR, Liu R, Oliveira GR, Ganguli S, Kalva S (2013) Venous compression syndromes: clinical features, imaging findings and management. Br J Radiol 86:20130284
Poyraz AK, Firdolas F, Onur MR, Kocakoc E (2013) Evaluation of left renal vein entrapment using multidetector computed tomography. Acta Radiol 54:144–148
Zerin JM, Hernandez RJ, Sedman AB, Kelsch RC (1991) “Dilatation” of the left renal vein on computed tomography in children: a normal variant. Pediatr Radiol 21:267–269
Hanna HE, Santella RN, Zawada ET Jr, Masterson TE (1997) Nutcracker syndrome: an underdiagnosed cause for hematuria? S D J Med 50:429–436
Grimm LJ, Engstrom BI, Nelson RC, Kim CY (2013) Incidental detection of nutcracker phenomenonon multidetector CT in an asymptomatic population: prevalence and associated findings. J Comput Assist Tomogr 37:415–418
He Y, Wu Z, Chen S, et al. (2014) Nutcracker syndrome-how well do we know it? Urology 83:12–17
Ahmed K, Sampath R, Khan MS (2006) Current trends in the diagnosis and management of renal nutcracker syndrome: a review. Eur J Vasc Endovasc Surg 31:410–416
Hohenfellner M, Steinbach F, Schultz-Lampel D, et al. (1991) The nutcracker syndrome: new aspects of pathophysiology, diagnosis and treatment. J Urol 146:685–688
Wendel RG, Crawford ED, Hehman KN (1980) The “nutcracker” phenomenon: an unusual cause for renal varicosities with hematuria. J Urol 123:761–763
Ariyoshi A, Nagase K (1990) Renal hematuria caused by “nutcracker” phenomenon: a more logical surgical management. Urology 35:168–170
Buschi AJ, Harrison RB, Norman A, et al. (1980) Distended left renal vein: CT/sonographic normal variant. Am J Roentgenol 135:339–342
Yun SJ, Nam DH, Ryu JK, Kim JS (2014) The roles of the liver and pancreas in renal nutcracker syndrome. Eur J Radiol 83:1765–1770
Kim KW, Cho JY, Kim SH, et al. (2011) Diagnostic value of computed tomographic findings of nutcracker syndrome: correlation with renal venography and renocaval pressure gradients. Eur J Radiol 80:648–654
Grossfeld GD, Litwin MS, Wolf JS, et al. (2001) Evaluation of asymptomatic microscopic hematuria in adults: the American Urological Association best practice policy–part I: definition, detection, prevalence, and etiology. Urology 57:599–603
Go AS, Chertow GM, Fan D, McCulloch CE, Hsu CY (2004) Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N Engl J Med 351:1296–1305
Arthurs OJ, Mehta U, Set PA (2012) Nutcracker and SMA syndromes: What is the normal SMA angle in children? Eur J Radiol 81:e854–e861
Karaosmanoglu D, Karcaaltincaba M, Karcaaltincaba D, et al. (2009) MDCT of the ovarian vein: normal anatomy and pathology. Am J Roentgenol 192:295–299
Park SJ, Lim JW, Ko YT, et al. (2004) Diagnosis of pelvic congestion syndrome using transabdominal and transvaginal sonography. Am J Roentgenol 182:683–688
Yao Y, Okada Y, Yamato M, et al. (2003) Communicating vein between the left renal vein and left ascending lumber vein: incidence and significance on abdominal CT. Radiat Med 21:252–257
Hiromura T, Nishioka T, Nishioka S, et al. (2004) Reflux in the left ovarian vein: analysis of MDCT findings in asymptomatic women. Am J Roentgenol 183:1411–1415
Park SJ, Lim JW, Cho BS, Yoon TY, Oh JH (2002) Nutcracker syndrome in children with orthostatic proteinuria: diagnosis on the basis of Doppler sonography. J Ultrasound Med 21:39–45
Ozkurt H, Cenker MM, Bas N, Erturk SM, Basak M (2007) Measurement of the distance and angle between the aorta and superior mesenteric artery: normal values in different BMI categories. Surg Radiol Anat 29:595–599
Unal B, Aktas A, Kemal G, et al. (2005) Superior mesenteric artery syndrome: CT and ultrasonography findings. Diagn Interv Radiol 11:90–95
Fu WJ, Hong BF, Gao JP, et al. (2006) Nutcracker phenomenon: a new diagnostic method of multisclice CT angiography. Int J Urol 13:870–873
Cho BS, Suh JS, Hahn WH, Kim SD, Lim JW (2010) Multidetector CT findings and correlations with proteinuria in nutcracker syndrome. Pediatr Nephrol 25:469–475
Ozbulbul NI, Yurdakul M, Dedeoglu H, Tola M, Olcer T (2009) Evaluation of effect of visceral fat area on the distance and angle between the SMA and aorta. Surg Radiol Anat 31:545–549
Takebayashi S, Ueki T, Ikeda N, Fujikawa A (1999) Diagnosis of the nutcracker syndrome with color Doppler sonography: correlation with flow patterns on retrograde left renal venography. Am J Roentgenol 172:39–43
i Calàbria HC, Gómez SQ, Cerqueda CS, et al. (2005) Nutcracker or left renal vein compression phenomenon: multidetector computed tomography findings and clinical significance. Eur Radiol 15:1745–1751
Rozenblit AM, Ricci ZJ, Tuvia J, et al. (2001) Incompetent and dilated ovarian veins: a common CT finding in asymptomatic parous women. Am J Roentgenol 176:119–122
Fitoz S, Ekim M, Ozcakar ZB, Elhan AH, Yalcinkaya F (2007) Nutcracker syndrome in children: the role of upright position examination and superior mesenteric artery angle measurement in the diagnosis. J Ultrasound Med 26:573–580
Acknowledgments
We acknowledge Yong Sung Park for help with statistics.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required (retrospective study).
Informed consent
Patients’ informed consent was waived by our hospital’s institutional review board.
Rights and permissions
About this article
Cite this article
Yun, S.J., Lee, J.M., Nam, D.H. et al. Discriminating renal nutcracker syndrome from asymptomatic nutcracker phenomenon using multidetector computed tomography. Abdom Radiol 41, 1580–1588 (2016). https://doi.org/10.1007/s00261-016-0717-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-016-0717-8