Abstract
Background
Metabolic information obtained through 18F-flurodeoxyglucose positron emission tomography/computed tomography (18F-FDG PET/CT) is used to evaluate malignancy by calculating the glucose uptake rate, and these parameters play important roles in determining the prognosis of non-small cell lung cancer (NSCLC). The expression of immune-related markers in tumor tissue reflects the immune status in the tumor microenvironment. However, there is lack of reports on the association between metabolic variables and intra-tumor immune markers. Herein, we investigate the correlation between metabolic status on 18F-FDG PET/CT and intra-tumor immunomarkers’ expression in NSCLC patients.
Methods
From April 2008 to August 2014, 763 patients were enrolled in the analysis to investigate the role of maximum standardized uptake value (SUVmax) in lung cancer. One hundred twenty-two tumor specimens were analyzed by immunohistochemistry (IHC) to intra-tumor immune cells and programmed death protein ligand 1(PD-L1) expression on tumor cells. The correlation between metabolic variables and the expression of tissue immune markers were analyzed.
Results
SUVmax values have significant variations in different epidermal growth factor receptor (EGFR) statuses (wild type vs mutant type), high/low neutrophil-to-lymphocyte ratio (NLR) groups, and high/low platelets-to-lymphocyte ratio (PLR) groups (p < 0.001, p < 0.001, p = 0.003, respectively). SUVmax was an independent prognostic factor in lung cancer patients (p = 0.013). IHC demonstrated a statistically significant correlation between SUVmax and the expression of CD8 tumor-infiltrating lymphocytes (p = 0.015), CD163 tumor-associated macrophages (TAMs) (p = 0.003), and Foxp3-regulatory T cells (Tregs) (p = 0.004), as well as PD-1 and PD-L1 (p = 0.003 and p = 0.012, respectively). With respect to patient outcomes, disease stage, BMI, SUVmax, metabolic tumor volume (MTV), TLG (tumor lesion glycolysis), CD163-TAMs, CD11c-dendritic cells (DCs), PD-L1, and Tregs showed a statistically significant correlation with progression-free survival (PFS) (p < 0.001, 0.023, < 0.001, 0.007, 0.005, 0.004, 0.008, 0.048, and 0.014, respectively), and disease stage, SUVmax, MTV, TLG, CD163-TAMs, CD11c-DCs, and PD-L1 showed a statistically significant correlation with overall survival (OS) (p < 0.001, < 0.001, 0.014, 0.012, < 0.001, 0.001, and < 0.001, respectively).
Conclusion
This study revealed an association between metabolic variable and immune cell expression in the tumor microenvironment and suggests that SUVmax on 18F-FDG PET/CT could be a potential predictor for selecting candidates for immunotherapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lung cancer is the leading cause of cancer-related death worldwide. Non-small cell lung cancer (NSCLC) accounts for 85% of lung cancer cases. Surgery is the main treatment for patients with lung cancer, combined with chemotherapy and radiotherapy. However, the overall 5-year survival rate remains poor [1]. 18F-flurodeoxyglucose positron emission tomography/computed tomography (18F-FDG PET/CT) is one of the most extensive diagnostic regimens for lung cancer. 18F-FDG PET/CT can provide morphological and functional information for cancer management and plays an important role in the diagnosis, staging, treatment planning, therapy response, and recurrence monitoring in lung cancer [2,3,4]. Tumor tissue usually presents a high metabolism and glucose uptake rate, and FDG is actively entrapped in neoplastic tissue and tumor-related activated immune cells [5–6].
Tumor microenvironment usually consists of various cell types, including neoplastic cells, tumor-infiltrating lymphocytes (TILs), tumor-associated macrophages (TAMs), regulatory T cells (Tregs), and dendritic cells (DCs) [7–8], which is an important component for lung cancer understanding. Increasing evidence has established an important contribution by tumor-infiltrating immune cells in the progression and prognosis of cancers and in the tumor response to therapy [9–10]. Tumor-infiltrating immune cells display heterogeneous properties according to disease origin. The immune checkpoints expressed in tumor cells and/or immune cells have also attracted substantial attention for investigations into the tumor microenvironment. Programmed death protein 1 (PD-1), expressed in the majority of TILs, is a membrane protein that is involved in the negative modulation of the immune system by inhibiting T cell activation. This occurs through the engagement of two tumor-expressing ligands, programmed death protein ligand 1 (PD-L1) and PD-L2. Immunotherapy has been the most promising treatment strategy for cancer, and novel immunotherapeutic strategies targeting PD-1-PD-L1 have shown promising results in advanced NSCLC patients [11,12,13]. However, we still lack simple and accurate parameters to predict immune treatment responses.
The metabolic state in the tumor microenvironment, especially glucose consumption, can influence the activity of immune cells and tumor progression [14]. However, the exact correlation between the metabolic state and immune factors is less known. Therefore, determining the network between metabolic variables and immune markers in the tumor microenvironment could lead to the identification of novel tumor progression mechanisms and could aid in seeking potential predictors of immunotherapy response.
18F-FDG PET/CT has been used to accurately show the metabolic status of the tumor microenvironment, thereby contributing to clarifying the interaction between metabolic and immune pathways [15]. Herein, we test the main parameters of 18F-FDG PET/CT (maximum standardized uptake value (SUVmax), metabolic tumor volume (MTV), TLG (tumor lesion glycolysis)) and tumor-infiltrating immune cells (PD-1, PD-L1, CD8-TILs, and CD68-TAMs, as well as others) in a cohort of patients with NSCLC. We also investigated the potential correlation between immune variables and clinical parameters and then analyzed the prognostic roles of these variables in NSCLC patients.
Materials and methods
Patients and study design
We designed a retrospective analysis of patients referred to our institution (Tianjin Cancer Hospital and Institute). Inclusion criteria included patients older than 18 years, pathology-confirmed NSCLC by at least two pathologists, and staging 18F-FDG PET/CT performed at our institution. This retrospective study was conducted with the approval of the Ethical Committee of TMUCIH.
From April 2008 to August 2014, 763 patients were enrolled in the analysis. One hundred twenty-two tumor specimens were analyzed for immunohistochemistry test. Baseline epidemiologic and clinical characteristics of the study population are shown in Table 1. This study’s use of human subjects complies with the Declaration of Helsinki.
Imaging protocol and tumor delineation
Patient image data were acquired using a DiscoveryST4 PET/CT scanner (GE, USA). The PH value of 18F-FDG was 5–7, and the radiochemical purity of the isotonic solution was ≥ 95%. Before the examination, the patient underwent fasting for 6 h, and the blood glucose of each patient was less than 6.8 mmol/L. The developing agent (3.7–4.81 MBq/kg) was injected from the anterior elbow vein. After 60 min of resting, whole body images were obtained from the base of the skull to the mid-thigh by means of an integrated PET/CT tomograph. Finally, two experienced nuclear medicine physicians calculated the area SUVmax, MTV, and TLG by using line attenuation correction and iterative reconstruction of the image in the manually constructed radionuclide focal volume of interest (VOI). SUVmax was defined as the highest pixel value.
Immunohistochemistry
For IHC analyses, 2–3-μm-thick tissue slides from paraffin-embedded tumor sections were processed. The slides were stained with primary antibodies raised against CD11c (Abcam), CD163 (Thermo Fisher), CD68 (Thermo Fisher), CD3 (Thermo Fisher), CD8 (Jinqiao Bio), Foxp3 (Abcam), PD-1 (Proteintech), and PD-L1 (Proteintech). Tissue sections were digitalized using DP Controller (Olympus Corporation) after staining. Two independent pathologists blinded to clinical data selected five non-overlapping and non-contiguous areas for each slide. The cell numbers of CD11c-DC, CD68-TAMs, CD163-TAMs, CD3-TILs, CD8-TILs, Foxp3-Tregs, and PD-1 TILs were quantified at × 400 (0.0484 mm2). The mean value obtained from the five different fields of one slide was calculated for each immune variable and subsequently used for statistical purposes. We determined the median value as the cutoff point for each immune cell. PD-L1 positivity was defined per specimen by a 5% expression threshold (PD-L1+ tumor cells/ total tumor cells) in case more than 5% were considered PD-L1-positive.
Statistical analysis
All parameters correlated with each other and to disease outcome. They were expressed in terms of progression-free survival (PFS) and overall survival (OS) over a median follow-up of 34 months. Hazard ratios with 95% confidence intervals were calculated with the Cox proportional hazards regression model in the multivariate analyses and log-rank test with Kaplan–Meier analysis. For continuous data, differences between groups were compared using the t test or the Wilcoxon test. For rank correlation, we used Spearman’s correlation coefficient (rho) and the linear regression test. Differences between groups were compared by analysis of variance (ANOVA). Statistical significance was set at p < 0.05 for each evaluation. Study analyses were performed on SPSS21.0 (IBM.US).
Results
The role of SUVmax in lung cancer
From April 2008 to August 2014, 763 NSCLC patients were enrolled in the analysis. Of them, 181 had squamous cell carcinoma (SCC), 508 had adenocarcinoma (ADC), and 74 had other subtypes. The baseline epidemiologic and clinical characteristics of the study population are shown in Table 1.
The SUVmax was significantly higher in males than females (p < 0.001). Additionally, older patients, larger tumor sizes, advanced stage, and smokers had higher SUVmax values (p = 0.02, p < 0.001, p = 0.003, and p < 0.001, respectively). We also compared the SUVmax between different epidermal growth factor receptor (EGFR) statuses (wild type vs mutant type); the wild type had a higher SUVmax than mutants (p < 0.001; Table 2). In addition, two promising factors, neutrophil-to-lymphocyte ratio (NLR) and platelets-to-lymphocyte ratio (PLR), were also included in our analysis. Higher NLR and PLR showed elevated SUVmax value (p < 0.001 and p = 0.003). Significant differences were also found between various histotypes (ADC, SCC, large cell lung cancer, adenosquamous carcinoma, and others; p < 0.001). SUVmax in ADC was remarkably lower than that in other histotypes (Suppl Fig. 1).
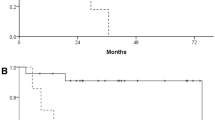
With respect to the outcome, using median values as cutoff points, disease stage (p < 0.001), body mass index (BMI) (p = 0.036), SUVmax (p < 0.001), after treatment (p < 0.001), NLR (p = 0.01), and PLR (p = 0.038) were significantly associated with PFS as analyzed using Kaplan–Meier curves and the log-rank test. Prognostic factors for OS included disease stage (p < 0.001), histotypes (p = 0.017), SUVmax (p < 0.001), smoking history (p = 0.037), after treatment (p = 0.004), and NLR (p = 0.002) (Fig. 1; Suppl Fig. 2). The multivariate analysis showed an independent prognostic role for SUVmax, disease stage, BMI, and after treatment in PFS (p = 0.013, p < 0.001, p = 0.033 and p < 0.001) and disease stage for OS (p < 0.001). SUVmax had marginal significance for OS (p = 0.074) (Suppl Table 1; Suppl Table 2).
Metabolic status and tumor-infiltrating immune cells in NSCLC patients
One hundred and twenty-two tumor specimens were analyzed with IHC for immune factors. Eighty-five ADCs, 31 SCCs, and 6 other NSCLC histotypes were analyzed (Table 3). All investigated tumors were positive at FDG-PET: the median SUVmax was 9.4 (range 2.3–29).
To investigate the relationship between immune variables and other clinical parameters, we calculated the median number of CD68+, CD163+, CD3+, CD8+, CD11c+, Foxp3+, and PD-1+ immune populations in tissue specimens from NSCLC patients in five areas in the same slides (Fig. 2). Considering the overall cohort, CD68-TAMs were present in all tumors, with a median number of 45.5, ranging from 4 to 150; CD163-TAMs were present in all tumors, with a median number of 31 (2–88); CD11c-DCs had a median number of 15 (0–40.5); CD3-TILs were present in all tumors with a median number of 138.75 (4–350); and CD8-TILs were present in all tumors with a median number of 78.25 (18–182). Additionally, PD-1-TILs were present with a median number of 23.5 (0–200), while 64 patient specimens were PD-L1-negative (≤ 5%) and 58 were PD-L1-positive (> 5%).
Immune variables in lung cancer specimens. a Histological sections of human NSCLC, stained for CD3-T cells, CD8-TILs, CD68-TAMs, CD163-TAMs, CD11c-DCs, and Foxp3-Tregs infiltrating cells. The density of immune variables is heterogeneous among specimens, with some scarcely infiltrated cases (upper) and some highly infiltrated cases (lower). b Similar for PD-1-TILs and PD-L1 expression in NSCLC cells
The distribution of immune variables did not differ significantly in SCC compared with ADC, except for Foxp3-Tregs and CD8-TILs: CD68-TAMs (p = 0.181), CD163-TAMs (p = 0.133), CD11c-DCs (p = 0.106), CD3-TILs (p = 0.233), CD8-TILs (p = 0.005), Foxp3-Tregs (p = 0.014), PD-1-TILs (p = 0.254), PD-L1 (p = 0.001) (Suppl Fig. 3).
We found a statistically significant correlation between SUVmax with the expression of CD163-TAMs (rho = 0.267; p = 0.003), CD8-TILs (rho = 0.219; p = 0.015), Foxp3-Tregs (rho = 0.262; p = 0.004), PD-1-TILs (rho = 0.376; p < 0.001), and PD-L1 (rho = 0.227; p = 0.012). In contrast, there was no correlation between SUVmax and CD68-TAMs (rho = − 0.1; p = 0.275), CD11c-DCs (rho < 0.001; p = 0.997), or CD3-TILs (rho = 0.111; p = 0.224) (Fig. 3). The association between MTV, TLG, and immune markers was also analyzed. The significant correlation was found between MTV and CD163-TAMs (rho = 0.202; p = 0.026), CD3-T cells (rho = 0.189; p = 0.037), Foxp3-Tregs (rho = 0.278; p = 0.002); TLG and CD163-TAMs (rho = 0.229; p = 0.011), Foxp3-Tregs (rho = 0.284; p = 0.002), and PD-1-TILs (rho = 0.243; p = 0.007).(Suppl Figs. 4 and 5).
Interestingly, we also found a correlation between intra-tumor immune markers; Tregs were negatively correlated with CD68-TAMs (rho = − 0.227; p = 0.012) but had positive correlation with CD163-TAMs (rho = 0.22; p = 0.015). Tregs were also positively correlated with CD3-TILs (rho = 0.506; p < 0.001) and CD8-TILs (rho = 0.166; p = 0.068). In addition, CD11c-DCs were correlated with CD8-TILs (rho = 0.196; p = 0.03). No significance was found for correlation with other markers.
Next, the roles of metabolic parameters and immune factors in determining the prognosis of the 122 lung cancer patients were also analyzed. Disease stage (p < 0.001), BMI (p = 0.023), SUVmax (p < 0.001), MTV (p = 0.007), TLG (p = 0.005), CD163-TAMs (p = 0.006), CD11c-DCs (p = 0.008), PD-L1 (p = 0.048), and Tregs (p = 0.014) were prognostic factors with PFS as documented on Kaplan–Meier curves by the log-rank test (Suppl Fig. 6). For OS, disease stage (p < 0.001), SUVmax (p < 0.001), MTV (p = 0.014), TLG (p = 0.012), CD163-TAMs (p < 0.001), CD11c-DCs (p = 0.001), and PD-L1 (p < 0.001) were significantly associated with OS.
Discussion
In this study, we performed a retrospective analysis on the roles of metabolic parameters in NSCLC patients and found a remarkable correlation between metabolic variables and immune-related markers in the tumor microenvironment. Our analysis suggests a network of 18F-FDG PET/CT metabolic information with intra-tumor immune features.
The role of SUVmax in lung cancer
Many tumors have high rates of glycolysis and an elevated metabolism rate. Tumor cells require catabolites to maintain the reduction–oxidation balance and produce biomass. As the most abundant nutrient, glucose is a metabolic substrate commonly used by tumor cells. 18F-FDG PET/CT imaging of the metabolic activity in tissues is on the basis of hexokinase inhibited by 2-deoxyglucose. SUVmax, a semi-quantitative factor of radioactivity for 18F-FDG PET/CT, is the most widely used parameter in clinical practice. Consistent with previous reports, we found that high SUVmax was negatively correlated with lung cancer prognosis [16,17,18].
We also calculated the correlation between SUVmax and NLR as well as PLR, two promising inflammation-related prognostic factors for lung cancer. We found that higher NLR and PLR were positively correlated with SUVmax and negative prognostic factors for PFS and OS. Increasing evidence has shown that systemic inflammatory responses were important prognostic factors [19]. As inflammatory response indicators, NLR and PLR were found to be negative prognostic factors in several solid tumors, including NSCLC [20,21,22]. Inflammation is the hallmark of cancer, and tumor occurrence is closely associated with inflammation in many tumor types [23]. Inflammatory mediators, produced by the tumor or innate response, can exert immunomodulatory effects by suppressing specific antitumor immune mechanisms [24–25].
Targeted agents have ushered NSCLC therapy into an era of precision medicine. The most extensive investigated target is EGFR. With advances in molecular research, the wide usage of molecular-targeted agents such as EGFR tyrosine kinase inhibitors (TKIs) has markedly improved the prognosis and decreased the inverse effect produced by chemotherapy. Various studies have been conducted to establish the association between 18F-FDG PET uptake and EGFR mutation, but the results have been conflicting and thus the correlation has not been well established. We detected the EGFR gene status in lung cancer patients in this analysis. NSCLC with EGFR mutations (including exons 19, 20, and 21) has shown a decreased metabolic rate compared with the wild type, which was consistent with Mak et al.’s and Na et al.’s results [26–27]. We also detected variations between the three mutation exons (exons 19, 20, and 21), but no significance was found (data not shown). Although no concurrent results, gene polymorphism could affect the metabolic state, which opened an additional window for innovation to detect gene mutation by molecular imaging.
In addition, we also detected the correlations between SUVmax and histotypes. We found that ADCs have significantly lower SUVmax than other types. Moreover, Higashi et al. found that the SUV value was significantly lower in bronchioloalveolar carcinomas than that in non-bronchioloalveolar adenocarcinomas [28]. Although the reason for these results requires further investigation, this outcome shows us that the complex molecular structure in various pathological types may influence tumor metabolism. Furthermore, SUVmax has a potential predictive value for the identification of histotypes.
Metabolic variables and immune factors
To compare the association between immune variables and 18F-FDG PET/CT parameters, specimens from the 122 lung cancer patients were tested by IHC for tumor-infiltrating immune cells, such as Tregs, TAMs, DCs, and TILs.
Tregs are a type of specific immune regulatory cells that can promote tumor progression by secreting inhibitory cytokines such as TGF-β and IL-10 or expressing negative regulatory factors such as CTLA-4, TIM-3, and PD-L1 to inhibit T cell activation [29,30,31,32]. Evidence has shown that Tregs infiltrating the tumor microenvironment could accelerate the invasion and metastasis of lung cancer and could be a negative prognostic immune factor in lung cancer [33, 34]. Foxp3 is a common biomarker for Tregs. In our analysis, more Foxp3-Tregs reveal shorter PFS in lung cancer patients, which is consistent with previous studies. Moreover, we found that Foxp3-Tregs are positively associated with SUVmax, MTV, and TLG.
Macrophages contribute to immune responses by possessing phenotypic plasticity. M2-polarized macrophages exhibit increased transcription of genes and possess tumor promotion functions. TAMs in the tumor microenvironment usually exhibit M2 polarization. M2 has higher basal mitochondrial oxygen consumption rates than either resting macrophages or M1 macrophages. CD163 is the common marker for M2-polarized macrophages. In our analysis, CD163-TAMs showed positive correlation with metabolic parameters. Additionally, more CD163+ macrophages had shorter PFS and OS; these results were consistent with previous conclusions.
Studies have recently reviewed the effect of T cells on the clinical outcome of a variety of solid cancers and found that a strong infiltration of TILs was associated with a positive clinical outcome in several cancers, including lung cancer. More specifically, the most consistent positive prognostic impacts were demonstrated for T cells, especially cytotoxic T cells. However, CD8-TIL was not a prognostic factor in our analysis, partly because of the small sample size. Positive correlation between CD8-TIL and SUVmax was found in our data. This outcome was similar with Lopci’s results [35]. Although Lopci did not explain the seemingly contradictory outcome, we think it is attributed to two points: first, more CD8-TILs still reveal the severity of tumor and tumor-related inflammation, and both could increase the FDG uptake; second, T cells have the ability to extensively and rapidly proliferate upon activation, which sets them apart from other immune cells. Additionally, CD8-TILs themselves engage Warburg metabolism when proliferating [36,37,38], which is due to the high glucose uptake and higher SUVmax value.
PD-L1 is expressed on a wide variety of tumors, including NSCLC. In general, PD-1 and PD-L1 have been demonstrated to indicate poor prognosis [39]. The PD-1-PD-L1 pathway plays a critical role in immunity inhibition, which could induce the exhaustion of lymphocytes and immune tolerance through suppressing lymphocyte proliferation and cytokine production [40, 41]. Recent studies with checkpoint inhibitors targeting the PD-1/PD-L1 axis showed promising patient outcomes. Two anti-PD-1 agents, nivolumab and pembrolizumab, have been approved by the US Food and Drug Administration with notable efficacy and a favorable toxicity profile in histologically or biologically selected NSCLC populations [11,12,13]. Although studies with PD-1/PD-L1-targeted therapies showed encouraging results, not all patients responded to this type of treatment and there is an urgent need for predictive biomarkers.
Our analysis showed a potential predictive value of metabolic imaging for immunotherapy response. Research has shown that PD-L1 could directly affect the glucose metabolism in vitro [14]. PD-L1 increased glycolysis-related enzymes by affecting the Akt/mTOR signaling pathway, leading to glycolysis rate acceleration [42]. As the immune regulation protein, PD-L1 can inhibit T cell activation by binding with PD-1 but can also enhance the glycolysis rate and exhaustion of glucose, thus making the immune cells “hungry” [43]. Our results confirmed this conclusion: SUVmax was positively correlated with PD-L1+ tumor cells, which demonstrated that SUVmax may be a valuable indicator for PD-L1 expression and the use of checkpoint inhibitors.
Our analysis has some shortcomings: first, a limited sample size in each stage influenced our further research on SUVmax and immune variables in different stages. Second, more FDG-PET parameters need to be included in our test for more comprehensive results.
In conclusion, our preliminary findings showed a statistically significant association between metabolic parameters on 18F-FDG PET/CT and the intra-tumor expression of immune-related markers, providing a rationale to further explore the role of 18F-FDG PET/CT as a predictor of tumor microenvironment patterns and checkpoint inhibitor activity.
Abbreviations
- NSCLC:
-
Non-small cell lung cancer
- 18F-FDG PET/CT:
-
18F-Flurodeoxyglucose positron emission tomography/computed tomography
- TILs:
-
Tumor-infiltrating lymphocytes
- TAMs:
-
Tumor-associated macrophages
- Tregs:
-
Regulatory T cells
- DCs:
-
Dendritic cells
- PD-1:
-
Programmed death protein 1
- IHC:
-
Immunohistochemistry
- SUV:
-
Standardized uptake value
- PFS:
-
Progression-free survival
- OS:
-
Overall survival
- SCC:
-
Squamous cell carcinoma
- ADC:
-
Adenocarcinoma
- NLR:
-
Neutrophil-to-lymphocyte ratio
- PLR:
-
Platelets-to-lymphocyte ratio
- BMI:
-
Body mass index
References
Saintigny P, Burger JA. Recent advances in non-small cell lung cancer biology and clinical management. Discov Med. 2012;13:287–97.
Ashamalla H, Rafla S, Parikh K, Mokhtar B, Goswami G, Kambam S, et al. The contribution of integrated PET/CT to the evolving definition of treatment volumes in radiation treatment planning in lung cancer. Int J Radiat Oncol Biol Phys. 2005;63:1016–23. https://doi.org/10.1016/j.ijrobp.2005.04.021.
Mac MM, Hicks RJ. The role of positron emission tomography/computed tomography in radiation therapy planning for patients with lung cancer. Semin Nucl Med. 2012;42:308–19. https://doi.org/10.1053/j.semnuclmed.2012.04.003.
Opoka L, Szolkowska M, Podgajny Z, Kunikowska J, Baranska I, Blasinska-Przerwa K, et al. Assessment of recurrence of non-small cell lung cancer after therapy using CT and Integrated PET/CT. Pneumonol Alergol Pol. 2013;81:214–20.
Palsson-McDermott EM, O’Neill LA. The Warburg effect then and now: from cancer to inflammatory diseases. Bioessays. 2013;35:965–73. https://doi.org/10.1002/bies.201300084.
Appelberg R, Moreira D, Barreira-Silva P, Borges M, Silva L, Dinis-Oliveira RJ, et al. The Warburg effect in mycobacterial granulomas is dependent on the recruitment and activation of macrophages by interferon-gamma. Immunology. 2015;145:498–507. https://doi.org/10.1111/imm.12464.
Gajewski TF, Schreiber H, Fu YX. Innate and adaptive immune cells in the tumor microenvironment. Nat Immunol. 2013;14:1014–22. https://doi.org/10.1038/ni.2703.
Hanahan D, Coussens LM. Accessories to the crime: functions of cells recruited to the tumor microenvironment. Cancer Cell. 2012;21:309–22. https://doi.org/10.1016/j.ccr.2012.02.022.
Fridman WH, Pages F, Sautes-Fridman C, Galon J. The immune contexture in human tumours: impact on clinical outcome. Nat Rev Cancer. 2012;12:298–306. https://doi.org/10.1038/nrc3245.
Dunn GP, Old LJ, Schreiber RD. The three Es of cancer immunoediting. Annu Rev Immunol. 2004;22:329–60. https://doi.org/10.1146/annurev.immunol.22.012703.104803.
Borghaei H, Paz-Ares L, Horn L, Spigel DR, Steins M, Ready NE, et al. Nivolumab versus docetaxel in advanced nonsquamous non-small-cell lung cancer. N Engl J Med. 2015;373:1627–39. https://doi.org/10.1056/NEJMoa1507643.
Herbst RS, Baas P, Kim DW, Felip E, Perez-Gracia JL, Han JY, et al. Pembrolizumab versus docetaxel for previously treated, PD-L1-positive, advanced non-small-cell lung cancer (KEYNOTE-010): a randomised controlled trial. Lancet. 2016;387:1540–50. https://doi.org/10.1016/S0140-6736(15)01281-7.
Fehrenbacher L, Spira A, Ballinger M, Kowanetz M, Vansteenkiste J, Mazieres J, et al. Atezolizumab versus docetaxel for patients with previously treated non-small-cell lung cancer (POPLAR): a multicentre, open-label, phase 2 randomised controlled trial. Lancet. 2016;387:1837–46. https://doi.org/10.1016/S0140-6736(16)00587-0.
Chang CH, Qiu J, O’Sullivan D, Buck MD, Noguchi T, Curtis JD, et al. Metabolic competition in the tumor microenvironment is a driver of cancer progression. Cell. 2015;162:1229–41. https://doi.org/10.1016/j.cell.2015.08.016.
Pearce EL, Pearce EJ. Metabolic pathways in immune cell activation and quiescence. Immunity. 2013;38:633–43. https://doi.org/10.1016/j.immuni.2013.04.005.
Na F, Wang J, Li C, Deng L, Xue J, Lu Y. Primary tumor standardized uptake value measured on F18-Fluorodeoxyglucose positron emission tomography is of prediction value for survival and local control in non-small-cell lung cancer receiving radiotherapy: meta-analysis. J Thorac Oncol. 2014;9:834–42. https://doi.org/10.1097/JTO.0000000000000185.
Nair VS, Krupitskaya Y, Gould MK. Positron emission tomography 18F-fluorodeoxyglucose uptake and prognosis in patients with surgically treated, stage I non-small cell lung cancer: a systematic review. J Thorac Oncol. 2009;4:1473–9. https://doi.org/10.1097/JTO.0b013e3181bccbc6.
Paesmans M, Berghmans T, Dusart M, Garcia C, Hossein-Foucher C, Lafitte JJ, et al. Primary tumor standardized uptake value measured on fluorodeoxyglucose positron emission tomography is of prognostic value for survival in non-small cell lung cancer: update of a systematic review and meta-analysis by the European Lung Cancer Working Party for the International Association for the Study of Lung Cancer Staging Project. J Thorac Oncol. 2010;5:612–9. https://doi.org/10.1097/JTO.0b013e3181d0a4f5.
Mantovani A, Allavena P, Sica A, Balkwill F. Cancer-related inflammation. Nature. 2008;454:436–44. https://doi.org/10.1038/nature07205.
Templeton AJ, McNamara MG, Seruga B, Vera-Badillo FE, Aneja P, Ocana A, et al. Prognostic role of neutrophil-to-lymphocyte ratio in solid tumors: a systematic review and meta-analysis. J Natl Cancer Inst. 2014;106:u124. https://doi.org/10.1093/jnci/dju124.
Liu H, Wu Y, Wang Z, Yao Y, Chen F, Zhang H, et al. Pretreatment platelet-to-lymphocyte ratio (PLR) as a predictor of response to first-line platinum-based chemotherapy and prognosis for patients with non-small cell lung cancer. J Thorac Dis. 2013;5:783–9. https://doi.org/10.3978/j.issn.2072-1439.2013.12.34.
Kaya V, Yildirim M, Demirpence O, Yildiz M, Yalcin AY. Prognostic significance of basic laboratory methods in non- small-cell-lung cancer. Asian Pac J Cancer Prev. 2013;14:5473–6.
Colotta F, Allavena P, Sica A, Garlanda C, Mantovani A. Cancer-related inflammation, the seventh hallmark of cancer: links to genetic instability. Carcinogenesis. 2009;30:1073–81. https://doi.org/10.1093/carcin/bgp127.
Balkwill F, Mantovani A. Inflammation and cancer: back to Virchow? Lancet. 2001;357:539–45. https://doi.org/10.1016/S0140-6736(00)04046-0.
Elkord E, Alcantar-Orozco EM, Dovedi SJ, Tran DQ, Hawkins RE, Gilham DE. T regulatory cells in cancer: recent advances and therapeutic potential. Expert Opin Biol Ther. 2010;10:1573–86. https://doi.org/10.1517/14712598.2010.529126.
Na II, Byun BH, Kim KM, Cheon GJ, Choe DH, Koh JS, et al. 18F-FDG uptake and EGFR mutations in patients with non-small cell lung cancer: a single-institution retrospective analysis. Lung Cancer. 2010;67:76–80. https://doi.org/10.1016/j.lungcan.2009.03.010.
Mak RH, Digumarthy SR, Muzikansky A, Engelman JA, Shepard JA, Choi NC, et al. Role of 18F-fluorodeoxyglucose positron emission tomography in predicting epidermal growth factor receptor mutations in non-small cell lung cancer. Oncologist. 2011;16:319–26. https://doi.org/10.1634/theoncologist.2010-0300.
Higashi K, Ueda Y, Sakurai A, Mingwang X, Xu L, Murakami M, et al. Correlation of Glut-1 glucose transporter expression with [18F]FDG uptake in non-small cell lung cancer. Eur J Nucl Med. 2000;27(12):1778–85. https://doi.org/10.1007/s002590000367.
Wei T, Zhang J, Qin Y, Wu Y, Zhu L, Lu L, et al. Increased expression of immunosuppressive molecules on intratumoral and circulating regulatory T cells in non-small-cell lung cancer patients. Am J Cancer Res. 2015;5:2190–201.
Jayaraman P, Jacques MK, Zhu C, Steblenko KM, Stowell BL, Madi A, et al. TIM3 mediates t cell exhaustion during Mycobacterium tuberculosis infection. PLoS Pathog. 2016;12:e1005490. https://doi.org/10.1371/journal.ppat.1005490.
Liang B, Workman C, Lee J, Chew C, Dale BM, Colonna L, et al. Regulatory T cells inhibit dendritic cells by lymphocyte activation gene-3 engagement of MHC class II. J Immunol. 2008;180:5916–26.
Rabe H, Nordstrom I, Andersson K, Lundell AC, Rudin A. Staphylococcus aureus convert neonatal conventional CD4(+) T cells into FOXP3(+) CD25(+) CD127(low) T cells via the PD-1/PD-L1 axis. Immunology. 2014;141:467–81. https://doi.org/10.1111/imm.12209.
Hasegawa T, Suzuki H, Yamaura T, Muto S, Okabe N, Osugi J, et al. Prognostic value of peripheral and local forkhead box P3+ regulatory T cells in patients with non-small-cell lung cancer. Mol Clin Oncol. 2014;2:685–94. https://doi.org/10.3892/mco.2014.299.
Bille A, Okiror L, Skanjeti A, Errico L, Arena V, Penna D, et al. The prognostic significance of maximum standardized uptake value of primary tumor in surgically treated non-small-cell lung cancer patients: analysis of 413 cases. Clin Lung Cancer. 2013;14:149–56. https://doi.org/10.1016/j.cllc.2012.04.007.
Lopci E, Toschi L, Grizzi F, Rahal D, Olivari L, Castino GF, et al. Correlation of metabolic information on FDG-PET with tissue expression of immune markers in patients with non-small cell lung cancer (NSCLC) who are candidates for upfront surgery. Eur J Nucl Med Mol Imaging. 2016;43:1954–61. https://doi.org/10.1007/s00259-016-3425-2.
Fox CJ, Hammerman PS, Thompson CB. Fuel feeds function: energy metabolism and the T-cell response. Nat Rev Immunol. 2005;5:844–52. https://doi.org/10.1038/nri1710.
Jones RG, Thompson CB. Revving the engine: signal transduction fuels T cell activation. Immunity. 2007;27:173–8. https://doi.org/10.1016/j.immuni.2007.07.008.
van Bruggen R, Koker MY, Jansen M, van Houdt M, Roos D, Kuijpers TW, et al. Human NLRP3 inflammasome activation is Nox1–4 independent. Blood. 2010;115:5398–400. https://doi.org/10.1182/blood-2009-10-250803.
Zou W, Chen L. Inhibitory B7-family molecules in the tumour microenvironment. Nat Rev Immunol. 2008;8:467–77. https://doi.org/10.1038/nri2326.
Curiel TJ, Wei S, Dong H, Alvarez X, Cheng P, Mottram P, et al. Blockade of B7-H1 improves myeloid dendritic cell-mediated antitumor immunity. Nat Med. 2003;9:562–7. https://doi.org/10.1038/nm863.
Freeman GJ, Long AJ, Iwai Y, Bourque K, Chernova T, Nishimura H, et al. Engagement of the PD-1 immunoinhibitory receptor by a novel B7 family member leads to negative regulation of lymphocyte activation. J Exp Med. 2000;192:1027–34.
Laplante M, Sabatini DM. mTOR signaling in growth control and disease. Cell. 2012;149:274–93. https://doi.org/10.1016/j.cell.2012.03.017.
Spranger S, Koblish HK, Horton B, Scherle PA, Newton R, Gajewski TF. Mechanism of tumor rejection with doublets of CTLA-4, PD-1/PD-L1, or IDO blockade involves restored IL-2 production and proliferation of CD8(+) T cells directly within the tumor microenvironment. J Immunother Cancer. 2014;2:3. https://doi.org/10.1186/2051-1426-2-3.
Funding
This work was supported by National Natural Science Funds of China (Nos. 81401887 and 81401888).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent and ethics statement
Informed consent was obtained from all individual participants included in the study. Written informed obtained from each subject complies with the Declaration of Helsinki. The study was approved by the Ethical Committee of TMUCHI.
Confirmation statement
My study’s involvement with human subjects complies with the Declaration of Helsinki.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Oncology – Chest
Electronic supplementary material
Supplementary Figure 1
(PNG 33 kb)
Supplementary Figure 2
(PNG 25 kb)
Supplementary Figure 3
(PNG 84 kb)
Supplementary Figure 4
(PNG 54 kb)
Supplementary Figure 5
(PNG 58 kb)
Supplementary Figure 6
(PNG 74 kb)
ESM 1
(DOC 52 kb)
Rights and permissions
About this article
Cite this article
Wang, Y., Zhao, N., Wu, Z. et al. New insight on the correlation of metabolic status on 18F-FDG PET/CT with immune marker expression in patients with non-small cell lung cancer. Eur J Nucl Med Mol Imaging 47, 1127–1136 (2020). https://doi.org/10.1007/s00259-019-04500-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-019-04500-7