Abstract
Post-traumatic cortical cystic lesions are rare radiolucent lesions that appear as a complication of low-severity fractures in children. Their relevance lies in the fact that few cases of these lesions have been described to date, so they are little known among clinicians caring for children. Three case reports of well-circumscribed cortical lytic lesions detected at 2–4 months during the follow-up of non-displaced distal radius fractures in children aged 9, 7, and 2 years are presented. The consistent clinical history and typical radiological features allowed the accurate diagnosis of post-traumatic cortical cystic lesion, without the need for advanced imaging tests or biopsy. At 12-, 8- and 11-month follow-ups, respectively, the lesions either disappeared or decreased in size. This benign and self-limited lesion should be correctly recognized to avoid confusion with other diagnoses, advanced imaging tests or biopsies, and unnecessary parental concerns.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Post-traumatic cortical cystic lesions or cyst-like cortical defects are subtle radiolucent lesions appearing adjacent to fracture sites in children [1]. These may be incidentally discovered during routine follow-up radiographs after a fracture or in the evaluation of new re-injuries following minor trauma [2]. Despite their benign nature, there is a notable lack of awareness among healthcare providers, leading to possible misdiagnosis. This misidentification might prompt unnecessary, advanced diagnostic procedures, such as advance imaging, blood tests, and even invasive techniques in asymptomatic children, adding stress for both children and their families [3, 4].
Early descriptions trace back to Pfister-Goedeke and Braune, attributing these lesions to “resorption cysts within an excessive periosteal reaction, related to the subperiosteal hematoma” [1]; a theory also substantiated by Dürr based on MR images [5]. Phillips and Keats believed that they were caused by intraosseous hematoma [6]. Later studies relying on CT and MRI supported the theory of transcortical leakage of medullary fat into the subperiosteal hematoma during the fracture event [3, 7,8,9,10,11]. The trapped fat may become visible later as the subperiosteal hematoma becomes calcified [7, 8] (Fig. 1).
Pathogenic hypothesis. A fracture that leads to a rupture of the cortex, leaving the periosteum of the concave side elevated but intact, allows the entry of intramedullary fat into the subperiosteal hematoma. When the subperiosteal hematoma ossifies, cyst-like cortical defects become evident on radiographs [3, 7,8,9,10]
Typically asymptomatic [1, 5, 7], these post-traumatic cortical defects manifest several weeks after the fracture, just proximal to the fracture line within the newly formed subperiosteal bone. Characteristically measuring less than 10 mm in diameter, their appearance ranges from rounded to slightly oval-shaped. Generally solitary, albeit occasionally multiple, these defects do not impede the initial fracture healing process [4, 7], are non-enlarging and non-progressive [1], and usually stabilize, diminish, or resolve spontaneously over time as the periosteal bone matures [1, 7, 9]. The differential diagnosis of this lesion should be made with conditions with more significant clinical implications, like osteomyelitis (Brodie abscess), Langerhans cell histiocytosis, simple or solitary bone cyst, non-ossifying fibroma, aneurysmal bone cyst, and, in some instances, osteoid osteoma, all which can be expanding processes, usually painful, and require a different approach [1, 2, 7, 9, 12].
This report aims to shed light on post-traumatic cortical cystic lesions through the description of three cases and a comprehensive literature review. Our goal is to raise awareness about this uncommon yet benign complication of low-severity pediatric fractures, encouraging accurate diagnosis and management among primary care doctors, orthopedic surgeons, pediatricians, and radiologists specializing in pediatric care.
Case report
Case 1
A nine-year-old boy experienced a Salter-Harris type II fracture (Fig. 2A) in his right hand after a fall, treated with a forearm splint for 4 weeks (Fig. 2B). Three months post-injury, the patient was asymptomatic and had resumed sports activities. On examination, he had no swelling or pain on palpation and demonstrated full mobility. Follow-up radiographs revealed a healed fracture and a well-defined rounded lucent lesion, in the posteromedial cortex of the distal radius metaphysis (Fig. 2C). Considering the characteristics of the lesion in an asymptomatic patient, a post-traumatic cortical cystic lesion was diagnosed, and the decision was to follow up the patient without further tests. After a year, radiographs showed the disappearance of the lesion and the patient was discharged (Fig. 2D).
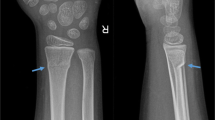
9-year-old male with trauma to the left wrist. A Anteroposterior and lateral radiographs show a Salter-Harris type 2 fracture of the distal radius. B First radiological control with splint immobilization showing no bone lesion. C Radiological control at 3 months showing a 5 × 6 mm lytic lesion in the metaphyseal area of the distal radius affecting the dorsomedial cortex. D Radiographs showing the disappearance of the lesion at one year
Case 2
A 7-year-old girl suffered a Salter-Harris type II distal radius fracture following a fall from a swing (Fig. 3A). She was immobilized with a short cast for 4 weeks (Fig. 3B), with good recovery. Four months later, radiographs incidentally revealed a lytic lesion on the distal radius’s posterior cortex (Fig. 3C). As she was symptom-free and active in sports, she was diagnosed with a post-traumatic cortical cystic lesion. The lesion decreased in size by the eight-month follow-up (Fig. 3D), so no further monitoring was undertaken.
7-year-old girl with right wrist trauma. A Anteroposterior and lateral radiographs show a Salter-Harris type 2 fracture of the distal radius. B Radiological control with closed cast without evidence of bone lesion. C Radiographs at 4 months showing a well-defined lytic bone lesion of 2.5 × 2.5 mm affecting the posterior cortex of the distal radius metaphysis. D Radiographs at 8 months show a decrease in lesion size
Case 3
A 2-year-old was seen at our clinic for a follow-up on an incomplete fracture (also referred to as greenstick fracture) of the radius and ulna, initially treated at another institution two months prior. The child, pain-free and with full motion range, displayed a radiolucent cystic lesion on the radius’s posteromedial diaphyseal cortex in the radiographic assessment (Fig. 4A). Consistent with prior cases, a monitoring approach was instituted (Fig. 4B, C). At the 11-month follow-up, a slight reduction in lesion size was noted, coupled with discernible separation from the growth plate due to longitudinal bone growth (Fig. 4D). This progress led to discharge.
2-year-old male with metaphyseal ulna and radius fracture. A Anteroposterior and lateral radiographs at the first visit to our center, two months after the fracture, showed fracture healing with the presence of callus and the finding of a 3 × 3 mm rounded lytic lesion in the posteromedial cortical metaphyseal area. B, C Radiographs at follow-up at 5 and 8 months, showing remodeling of the fracture and location of the lytic lesion in the dorsomedial bone callus. D Radiographs showing the decrease in size and separation from the physis of the cystic lesion at 11 months
Literature review
Methods
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines were followed when preparing this systematic literature review [13]. The search was performed using 3 electronic databases from inception until August 20, 2023 (Fig. 5). Supplemental bibliographic cross-reference searches were also conducted to identify any additional relevant studies, imposing no limits on language or publication date. Updated searches were performed on September 10 and October 1, 2023. Three reviewers independently evaluated studies for inclusion (M.G.O, P.M.A, and C.M.G), with decisions made through consensus after a detailed review of full texts against our predetermined eligibility criteria (Table 1). The JBI critical appraisal checklist for case reports was used [14].
Search flow diagram performed in PubMed, Embase, and Cochrane databases according to the terms (“Post-traumatic” OR “posttraumatic” OR “post-fracture” OR “following fracture*”) AND (“cystic” OR “Cyst lesion” OR “cyst-like lesion*” OR “Cortical Defect*” OR “osseous cyst” OR “lipid inclusion cyst”) AND (radius OR radial OR tibia OR tibial OR femur OR femoral OR ulna OR ulnar OR humerus OR humeral OR forearm)
Results
The initial database search yielded 90 studies, from which 23 duplicates were removed. After screening, 67 studies were considered for inclusion, leading to 28 articles that met our criteria (Fig. 5). These articles described 49 cases, in addition to the three cases presented in this study. The individual characteristics of the cases described in the included studies are displayed in Supplementary Table 1, while the overall characteristics of the study group are described in Table 2. Notably, the mean age of patients was 7.4 years, predominantly male, with the distal radius being the most frequent fracture site and the greenstick fracture being the most common fracture type. Diagnosis of the post-traumatic cortical cystic lesion was made at a mean of 5.4 months post-injury. Most lesions were solitary, with an average size of 7.1 mm, primarily located on the posterior cortex. No further investigations were performed in 24 cases (46.2%), while 1 advanced test (MRI, CT, blood test, bone scan, bone scan, ultrasound, or biopsy) was performed in 15 cases (28.8%), 2 in 10 cases (19.2%), and 3 advanced tests were performed in 3 cases (5.8%). Follow-up was only reported in 35 cases (67.13%), among which 17 (32.7%) had resolved, 11 remained the same (21.2%), and 7 had decreased in size (13.5%), while none had progressed. In addition, no pathological fractures were described in relation to these cysts.
Discussion
The 3 cases presented, along with this systematic review of the literature totaling 52 cases, confirm that post-traumatic cortical cysts are a benign, self-limited complication of minimally displaced fractures in children. The information derived from this systematic review in terms of age at presentation, affected bone, type of preceding fracture, time to onset of the lesion, radiological characteristics, and natural history allows us to be confident in managing these injuries without the need for further investigations.
Despite these lesions being unusual, we believe they are underreported in the literature. A possible explanation for the underdiagnosis and unknown exact incidence is that many distal radius fractures in children are monitored only by clinical signs [4, 7, 15] or radiographically within the first month, when the lesion may not be yet visible [8]. At the stage when the lesion may manifest, radiological examinations are not typically conducted for minimally displaced fractures in children [2, 8]. On the other hand, its rarity can be explained by specific conditions for their formation—a combination of cortical disruption allowing the extrusion of the crushed bone marrow [7, 8] and intact periosteum, only detached from the bone [3, 7, 8]. Emphasis is placed on highlighting that the presence of these lesions is a post-traumatic phenomenon rather than a pre-existing condition.
These injuries predominantly manifest in children due to their enhanced bone elasticity, predisposing them to distinctive fracture patterns, primarily in the metaphyseal region, such as torus or greenstick fractures [2, 16]. The robust periosteum in children often remains intact, ensuring that complete metaphyseal fractures are minimally displaced. The high percentage of distal radius involvement compared to other locations may be associated with the higher percentage of fractures occurring in this location in children, many of which are minimally displaced. In addition, the more frequent location in the posterior cortex is related to the higher frequency of dorsally displaced distal radius fractures by having the periosteum intact on the concave side [3, 11, 16], allowing the accumulation of trapped intramedullary fat, and leading to the appearance of a dorsally located intracortical lesion within the ossified layers of the subperiosteal hematoma [7].
Many of the reports and case series included in this systematic review routinely use advanced imaging techniques and blood tests without further altering management. Therefore, there is sufficient evidence to support that they appear unnecessary for the diagnosis of these lesions in the context of a consistent clinical history and a typical radiographic appearance (Table 3) [5, 11, 17], as shown in our cases. Careful review of the radiographs can often rule out the possibility of an unrecognized pre-existing lesion and pathological fracture [3]. Furthermore, biopsy is clearly unjustified in these benign, self-limiting lesions [5], unless progression is observed on follow-up radiographs, or there are initial different or aggressive features [3, 11, 18]. A monitoring based on clinical and radiological follow-up showing the absence of progression, with a decrease in size or disappearance, is sufficient and reduces the stress on patients and their families [3]. Moreover, since no pathological fractures have been described in relation to these cystic lesions [3], we consider that preventive protection with an orthosis is not necessary, let alone prophylactic surgical treatment.
Conclusions
In conclusion, post-traumatic cortical cystic lesions are recognized as benign, self-limiting sequelae to low-severity fractures in pediatric patients and are likely underreported. Their etiology, though elusive, is primarily theorized to involve a transcortical migration of intramedullary fat during fracture events, entrapped by periosteum, and becomes visible several weeks post-trauma as subperiosteal hematomas calcify. Accurate identification should be facilitated by the presence of an asymptomatic, healthy child along with characteristic radiographic findings, thereby avoiding misdiagnoses and the routine pursuit of unnecessary further examinations, reducing undue parental anxiety. Follow-up observations generally reveal a trajectory of stabilization, diminution in size, or complete resolution of these lesions.
References
Pfister-Goedeke L, Braune M. Cyst-like defects following fractures in children. Pediatr Radiol. 1981;11(2):83–6. https://doi.org/10.1007/BF00971785.
Papadimitriou NG, Christophorides J, Beslikas TA, Doulianaki EG, Papadimitriou AG. Post-traumatic cystic lesion following fracture of the radius. Skeletal Radiol. 2005;34(7):411–4. https://doi.org/10.1007/s00256-004-0877-4.
Davids JR, Graner KA, Mubarak SJ. Post-fracture lipid inclusion cyst. A case report. J Bone Joint Surg Am. 1993;75(10):1528–32. https://doi.org/10.2106/00004623-199310000-00014.
Wass AR, Sloan JP. Cortical bone cyst following a greenstick radial fracture. J Accid Emerg Med. 1996;13(1):63–4. https://doi.org/10.1136/emj.13.1.63.
Dürr HR, Lienemann A, Stäbler A, Küehne J, Refior HJ. MRI of posttraumatic cyst-like lesions of bone after a greenstick fracture. Eur Radiol. 1997;7(8):1218–20. https://doi.org/10.1007/s003300050278.
Phillips CD, Keats TE. The development of post-traumatic cyst-like lesions in bone. Skeletal Radiol. 1986;15(8):631–4. https://doi.org/10.1007/BF00349859.
Malghem J, Maldague B. Transient fatty cortical defects following fractures in children. Skeletal Radiol. 1986;15(5):368–71. https://doi.org/10.1007/BF00348864.
Malghem J, Maldague B, Claus D, Clapuyt P. Transient cyst-like cortical defects following fractures in children. Medullary fat within the subperiosteal haematoma. J Bone Joint Surg Br. 1990;72(5):862–5. https://doi.org/10.1302/0301-620X.72B5.2211773.
Ball CM, Dawe CJ. Transient posttraumatic cystlike lesions of bone. J Pediatr Orthop. 2001;21(1):9–13. https://doi.org/10.1097/00004694-200101000-00004.
Roach RT, Cassar-Pullicino V, Summers BN. Paediatric post-traumatic cortical defects of the distal radius. Pediatr Radiol. 2002;32(5):333–9. https://doi.org/10.1007/s00247-001-0608-0.
Lewandowski LR, Murphey MD, Potter BK. Posttraumatic cysts after pediatric fracture. J Pediatr Orthop. 2013;33(3):239–43. https://doi.org/10.1097/BPO.0b013e318280a63f.
García-Alvarez F, Bello ML. Another case of a transient posttraumatic cyst-like lesion in bone. J Pediatr Orthop. 2001;21(6):828–9. https://doi.org/10.1097/00004694-200111000-00032.
Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:71.
Moola S, Munn Z, Tufanaru C, Aromataris E, Sears K, Sfetcu R, Currie M, Qureshi R, Mattis P, Lisy K, Mu P-F. Chapter 7: Systematic reviews of etiology and risk. In: Aromataris E, Munn Z (Editors). JBI manual for evidence synthesis. JBI, 2020. https://synthesismanual.jbi.global. Accessed 10 Sept 2023.
Talawadekar GD, Muller M, Zahn H. Benign self-limiting cystic lesion after lower end radius fracture in a child. Indian J Orthop. 2009;43(1):99–101. https://doi.org/10.4103/0019-5413.45333.
Light TR, Ogden DA, Ogden JA. The anatomy of metaphyseal torus fractures. Clin Orthop Relat Res. 1984;188:103–11.
Allali J, Escalard C, Belloy F, Blouet M. Cyst-like lesions following fracture in a child - sonographic appearances. Pediatr Radiol. 2020;50(4):583–6. https://doi.org/10.1007/s00247-019-04575-2.
Asrian A, Shahabpour M, Tajdar F, de Boeck H. Posttraumatic cyst-like lesions of cortical bone in children. Acta Orthop Belg. 2010;76(2):264–8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and informed consent
Informed written consent was obtained from the patient’s family before submission. This study was conducted in accordance with the principles of the 1964 Helsinki Declaration.
Conflict of interest
The authors declare no competing interests.
Additional information
Reporting guidelines
• The authors have adhered to the recommendations for the accurate reporting of information in case reports that resulted in the CARE (CAse REport) Statement and Checklist.
• This systematic review was performed in accordance with the Cochrane Collaboration and the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) statement and the Cochrane Handbook for Systematic Reviews of Interventions latest methodological guidance.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Galán-Olleros, M., Manzarbeitia-Arroba, P., Miranda-Gorozarri, C. et al. Post-traumatic cortical cystic lesions in children: three case reports and a systematic review of the literature. Skeletal Radiol (2024). https://doi.org/10.1007/s00256-024-04661-z
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00256-024-04661-z