Abstract
Objective
To investigate whether the fracture morphology of quadrilateral plate (QP) fragments is associated with the anterior and posterior columns in associated both-column (ABC) fractures.
Materials and methods
Three-dimensional computed tomography data of 100 ABC fractures treated at our hospital from August 2016 to August 2019 were retrospectively analyzed using Mimics and 3-matic software. The distribution of fracture lines was described using the fracture mapping technique.
Results
One fragment presented on the QP was confirmed in 88% of the patients. The QP fragments’ fracture lines were divided into the anterior oblique (AO), superior posterior oblique (SPO), and mid-posterior oblique (MPO) lines, occurring in 100, 86, and 8 cases, respectively. AO lines were distributed along the arcuate line. SPO lines were continuations of the AO lines, which were distributed to the posterior column from the greater sciatic notch to the lesser sciatic notch. MPO lines were involved in the QP’s central area. A simple fracture was found at the proximal AO and SPO lines in 80% and 86% of all displaced fractures, respectively. AO lines distal to the superior rim of the acetabula were confirmed to be comminuted fractures in 32% of all cases.
Conclusions
In ABC fractures, there was only one QP fragment in nearly 90% of all cases. The QP fractures were mainly present in the QP’s peripheral area. More than 80% of the fracture patterns on the cephalic side of the QP were simple. The reduction and internal fixation of QP fractures in ABC fractures should be in the cephalic region.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Associated both-column (ABC) acetabular fractures are the second most common type of acetabular injury, accounting for 22% of all acetabular fractures [1]. This injury is usually caused by forces that drive the femoral head into the acetabulum. As a result, the acetabulum breaks into several parts, usually including an anterior column fragment and a quadrilateral plate (QP) fragment, with or without posterior wall (PW) fragments [2]. According to Letournel et al., acetabular fractures were classified into 5 elemental (posterior wall, posterior column, anterior wall, anterior column, and transverse) and 5 associated (posterior wall plus posterior column, posterior wall with transverse, anterior plus posterior hemitransverse, T-shaped, and both columns) patterns, among which ABC fracture is the most complex one [3]. This fracture is classified as type C according to OTA/AO classification system in which the fractures are classified as elementary( type A), partial articular (type B), and both column fractures (type C) [4]. Most of these fractures require surgical treatment. However, controversies remain regarding the surgical approach choice and internal fixation, especially for QP fragments [5, 6], since both anterior and posterior columns were involved by the fragments, and they contained the posterior portion of the acetabular fossa.
An understanding of three-dimensional (3D) morphological changes serves the purpose of elucidating these complex fractures. To date, Yang et al. [7] have reported the morphological characteristics of the anterior column and PW fragments; they have also reported general morphological changes of QP fragments in acetabular fractures [8, 9]. ElNahal et al. [10] have proposed a novel classification method for QP fractures. However, there is still a lack of relevant research considering the morphological characteristics of the QP in ABC acetabular fractures.
The purpose of this study was to conduct a retrospective analysis of the morphological characteristics of ABC acetabular fractures and provide recommendations for approaches and fixation options for the surgical treatment of such fractures. Specifically, we aimed to investigate whether the fracture morphology of QP fragments is associated with the anterior and posterior columns in ABC fractures.
Methods
Study design and population
All data were collected from the picture archiving and communication system and medical record system of our hospital from August 2016 to August 2019. This study was conducted in accordance with the principles of the Declaration of Helsinki. Ethical approval was granted by the review board of our institution, and informed consent was waived by the ethics review board.
The inclusion criteria were as follows: (1) patients with ABC acetabular fractures, according to the Letournel-Judet classification system [3] and OTA/AO classification [4]; and (2) the availability of complete radiographic data, including plain radiography and computed tomography (CT) scans for the patient. The exclusion criteria were as follows: (1) patients less than 18 years of age; or (2) patients with open or pathological fractures. To ensure the correct classification of the fractures, all radiographic images were reviewed by two senior orthopedic trauma surgeons with over 15 years of experience in treating these fractures. In case of disagreement, a third senior orthopedic trauma surgeon was consulted to generate a uniform decision.
During this time, 490 cases of acetabular fractures were surgically treated, and 100 patients (81 males, 19 females), with a mean age of 52 (18 − 81) years, met the inclusion criteria of this study. Age distribution among our patient cohort as shown in Fig. 1. The Injury Severity Score (ISS) was used to evaluate the injury severity of our cohort. An ISS of 1–8 points is considered minor, 9–15 moderate, 16–24 severe, and 25 points and higher very severe.
Fracture mapping
A fracture map was generated as previously described by Xie et al. [11]. The pelvic DICOM data for each case were imported into Mimics software (Version 17.0, Materialize, Leuven, Belgium) for segmentation. Segmented images of all fragments were then imported into 3-matic software (Version 10.2, Materialize). A simulated surgical reduction was performed by moving and rotating each fragment to restore the original anatomical structure. All cases with a left-side fracture were undergone a mirror transformation to establish a right-side fracture model. Subsequently, adjustments to the restored acetabulum were made to best match a pre-created standard 3D acetabulum model. The template surface was then marked and divided into small independent surfaces, the borders of which coincided with the fracture lines of the quadrilateral fragments (Fig. 2). All templates were subsequently superimposed to build a frequency diagram. The frequency of the fractures was represented by the density of borderlines of templates.
Methods of the mapping technique: The 3D model of whole pelvis (a from anterior view) was reconstructed and the innominatum containing fractured acetabulum was separated and isolated into different units according to fragments (b) (left, from inside views). Simulating reduction of each fragment was completed to restore the original anatomical structure (c). A mirror image was created (d). The fracture lines were drawn on a standard model (e) (right innominatum)
The QP is the medial face of the acetabulum, which is bordered by the arcuate line (iliopectineal line) anterosuperiorly, the posterior edge of posterior column and greater sciatic notch posterosuperiorly, the superior edge of obturator foramen anteroinferiorly, and the anterior edge of ischial tuberosity inferoposteriorly [10]. According to Yang et al. [9], QP fracture lines are divided into the anterior oblique (AO) line, the superior posterior oblique (SPO) line, and the mid-posterior oblique (MPO) line.
The AO line originates from the anteroinferior rim of the acetabulum and extends proximally along the arcuate line. The SPO line continues the AO line, bends superoposteriorly distal to the sacroiliac joint, and reaches the posterior column. The MPO line starts from the arcuate line, passes through the central area of the QP, and moves to the posterior column (Fig. 3).
We assumed that the fracture started from the anteroinferior rim of the acetabulum, although the injury mechanism of ABC acetabular fracture is still unclear. Thus, the distribution of the AO, SPO, and MPO lines was analyzed based on the fracture map.
The relations of QP fragments to the anterior and posterior column fragments
A QP fragment was defined as a fragment occurred within the QP area and separated from both anterior and posterior column [10]. In some cases, more than one fragment, which displaced ≥ 2 mm and needed to be reduced, appeared in the area. In ABC acetabular fractures, fracture lines would extend to the inferior pubic ramus and ischial tuberosity. The fragments were observed on axial, sagittal, and coronal images and 3D models in each case. The number of QP fragments, distribution of the AO line, and its connection with the anterior column were reviewed. The distribution of the SPO and MPO lines and their connections with the posterior column were recorded.
Statistics
SPSS software (version 20.0, IBM Corporation, Armonk, NY, USA) was used to perform all statistical analyses. Demographic data and fracture characteristics were analyzed using descriptive statistics. Fracture data are presented as mean and standard deviation. Statistical significance was set at P < 0.05. Interobserver reliability was assessed by Cohen’s Kappa Index. A kappa value from 0.61 to 0.80 suggests substantial agreement, and 0.8 to 1 suggests excellent agreement.
Results
General results
There were 75 cases of type C1, 9 of type C2, and 16 of type C3 according to OTA/AO classification (Table 1). The mean ISS was 9.37 (4 − 27) points. The ISS was less than 16 points in 66 cases and more than 16 points in 34 cases. There were 32 cases only suffered the acetabular fractures. Concomitant injuries including extremity fractures and other organ injuries were found in the rest 68 cases.
Number of QP fragments
The detached QP fragment presented as one in 88 (88%) cases, two in 11 (11%) cases, and four in one (1%) case.
Distribution of fracture lines of QP fragments
AO lines almost started near the area where the superior pubic ramus was connected to the anteroinferior rim of the acetabulum and spread along the arcuate line. The dense area was located on and slightly posteroinferior to the arcuate line. SPO lines were concentrated on the posterosuperior region of the QP. All the lines passed through the posterior edge of the posterior column, from the greater sciatic notch to the lesser sciatic notch. MPO lines involved the central QP and reached to the posterior column. The area of the rare line distribution was the posteroinferior region of the QP, the area between the SPO line and the sacroiliac joint (Fig. 4).
The distributions of all the fracture lines of QP fragments (right, from inside view). AO lines were concentrated on the area inferoposterior to arcuate line (red dashed box), SPO line distributed mainly on the superoposterior peripheral region of QP (yellow dashed box), while MPO lines (very few) involved the middle part of QP (blue dashed box). Dashed boxes enclose typical locations of AO, SPO, and MPO lines
Fractures along AO lines
AO lines were present in all 100 patients. AO lines originated from the area where the superior pubic ramus was connected to the anteroinferior rim of the acetabulum in 82 cases (82%), the acetabular notch in 10 cases (10%), the anterior rim in seven cases (7%), and the superior pubic ramus and acetabular notch simultaneously in one case (Fig. 5).
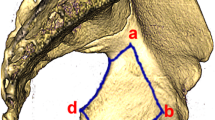
The origination (red area) of AO line: most of them (82%) from the area where the superior pubic ramus connects with the inferoanteior rim of the acetabulum (a), the acetabular notch (10%) (b), the anterior rim (7%) (c), and in one (1%) from the superior pubic ramus and the acetabular notch simultaneously (d) (right, from inside view)
The relationship of AO lines to arcuate lines
AO lines were located inferior to the arcuate line in 56 cases (56%), on the arcuate line in 35 cases (35%), lateral to the arcuate line in three cases (3%), intersected with the arcuate line in two cases (2%), and in the central part of the QP in four cases (4%). AO lines in the central part of the QP were also inferior to the arcuate line; however, their unique character occurred through the mid portion of the QP and oriented anterior oblique, making them an individual group (Fig. 6).
The distribution of the AO line (azure area) along the arcuate line (white bar). AO lines located inferior to the arcuate line (56%) (a), on the arcuate line (35%) (b), lateral to the arcuate line (3%) (c), intersect with the arcuate line (2%) (d), and in the central part of the QP (4%) (e) (right, from inside view)
The relation of the AO lines to anterior column fragments
Considering the relationship between the AO lines and the anterior column, we identified three fracture patterns: (1) simple fractures: one AO line extending between the anterior column fragment and the QP fragment in 68 cases (68%), with the AO lines originating from the anterior column in six cases and from the QP fragment in one case (Fig. 7); (2) hybrid fractures in which a triangular free fragment (six cases) or a bony spike connecting with the superior pubic ramus (six cases) existed between the anterior column fragment and the QP fragment in 12 cases (12%). These fragments were distal to the dome of the acetabulum but were proximal to the iliopubic eminence, leading to a comminuted fracture in the distal part and a simple fracture in the proximal part (Fig. 8). (3) Comminuted fractures in which more than two free fragments existed between the anterior column fragment and the QP fragment, resulting in no direct contact between the two main fragments in 20 cases (20%) (Fig. 9). In hybrid fractures, there was still direct contact between the anterior column fragment and the QP fragment in the proximal arcuate line, which is the main difference between the comminuted fractures as identified above.
A typical fracture model (a), its template (red line) (b) manifesting the simple fracture between the AO lines and the anterior column, with direct contact between the anterior column fragment and QP fragment. Colored fragments in (a) were anterior column fragment (red), and QP fragment (yellow). Fracture map (c) showing simple fractures (red dashed box) in 68% cases (right, from inside view)
A typical fracture model (a), its template (red line) (b) manifesting the hybrid fracture between the AO lines and the anterior column, with fragments presented only distal to the arcuate line. Colored fragments in (a) were anterior column fragment (red), QP fragment (yellow), and comminuted fragment distal to the arcuate line (green). Fracture map (c) showing hybrid fractures (red dashed box) in 12% cases (right, from inside view)
A typical fracture model (a), its template (red line) (b) manifesting the comminuted fractures between the AO lines and the anterior column, with fragments presented along the arcuate line. Colored fragments in (a) were anterior column fragment (red), QP fragment (yellow), and comminuted fragments on the arcuate line (green). Fracture map (c) showing comminuted fractures (red dashed box) in 20% cases (right, from inside view)
Fractures along SPO lines
SPO lines were complete in 86 cases (86%); however, they failed to reach the posterior edge of the posterior column in seven cases (7%) and were nonexistent in seven cases (7%).
In cases with complete SPO lines, a simple fracture was observed in 74 cases (86%) (Fig. 10). A comminuted fracture with free fragments existed between the SPO line and the sacroiliac joint was presented in 10 cases (11.6%) (Fig. 11); SPO lines involved the sacroiliac joint were present in three cases (3.4%) (Fig. 12).
A typical fracture model (a) showing the simple fractures of SPO lines, with direct contact between the posterior ilium and the QP fragment. Colored fragments in (a) were QP fragment (yellow), and posterior iliac fragment (cyan). Fracture map (b) showing simple fractures (red dashed box) in 86% cases (right, from inside view)
A typical fracture model (a) showing the comminuted fractures of SPO lines, with free fragments presented between the posterior ilium and the QP fragment. Colored fragments in (a) were QP fragment (yellow), posterior iliac fragment (cyan), and free fragment (green). Fracture map (b) showing comminuted fractures (red dashed box) in 11.6% cases (right, from inside view)
A typical fracture model (a) showing fractures of SPO lines involving the sacroiliac joint. Colored fragments in (a) were QP fragment (yellow), and posterior iliac fragment (cyan). Fracture map (b) showing SPO lines involving the sacroiliac joint (red dashed box) in 3.4% cases (right, from inside view)
Distribution of SPO lines on the posterior edge of the posterior column
The SPO lines are distributed on the posterior edge of the posterior column from the greater sciatic notch to the lesser sciatic notch. The dense area was distributed proximally (Fig. 4).
MPO lines
The MPO line was present in eight cases, including six complete fractures and two incomplete fractures. In cases with complete MPO lines, fractures involved the central QP and reached posteriorly to the posterior column around the ischial spine in five cases and the middle edge in one case (Fig. 13).
Interobserver reliability
The Kappa value of the OTA/AO classification was 0.873, in identifying the AO lines was 1.000, in identifying the SPO lines was 0.928, and in identifying the MPO lines was 0.847. The Kappa value in assessing the AO line origination was 0.744, in assessing the relationship of AO lines to arcuate lines was 0.783, in assessing the relation of the AO lines to anterior column fragments was 0.773, in assessing the fractures along SPO lines was 0.811.
Discussion
A key point in treating ABC acetabular fractures is to reduce the anterior column and the QP fragments to the ilia connected with the sacrum and to restore the anatomic relations between the two fragments [6]. As for the QP fragments, the optimal selection of approaches and internal fixations remains to be resolved. The approaches reported to be used to expose the QP fragments are the modified ilioinguinal approach [12], the modified Stoppa approach [13], and the pararectus approach [14]. To date, no criteria have been established regarding the selection of approach.
In this study, the morphological changes of the QP fragment in 100 cases of ABC acetabular fractures were evaluated using a fracture mapping technique. The authors found that 88% of all cases had only one fragment presented on the QP. The fracture lines could be divided into the AO, SPO, and MPO lines according to the location of the fractures. The MPO lines distributed on the central area of the QP were found only in eight cases, while the AO lines were present in all cases and were mainly located on or posterior to the arcuate line. The SPO line, present in 86% of all cases, was located in the superoposterior aspect of the QP, just distal to the sacroiliac joints. These results indicate that, in ABC acetabular fractures, most of the QP fractures were simple and occurred on the peripheral sides of the plate; the arcuate line was the most involved region, and the superior posterior area was the second. The central area was rarely involved. Our results support the opinion that a pararectus approach is recommended to expose these fractures, especially for fractures around the arcuate line.
It is very important to find an accurate strategy to reduce the QP fragment during the surgical treatment of fractures. As for its connections with the anterior column fragments, there were three fracture patterns identified: no comminuted fragment between two main fragments, presented in 68%; comminuted fragments only in the distal part of the fracture line, presented in 12%, comminuted fragments appearing in both the distal and proximal parts of the fracture line, presented in 20%. These findings show that nearly 80% of AO lines proximal to the dome of the acetabulum were simple fractures.
Regarding connections to the posterior column, a displaced fracture, presented with the SPO line was confirmed in 86% of all cases; among these, comminuted fractures were ascertained in 10 cases (11.6%), sacroiliac joints were involved in three cases, and the remaining were simple fractures (86%). These outcomes demonstrated that the superoposterior part, defined by the proximal AO and SPO lines, was the appropriate location to be initially considered in the reduction of QP fragments.
Commonly used fixations to stabilize the QP fragments are buttress plating [15], infrapectineal plating [16,17,18], extrapelvic plating with periarticular screws [19], calcaneal plating [20], novel anatomic plating [21, 22], and a combination of these techniques [15, 23]. The optimal indications for choice of fixation remain unclear. We found that, in 88% of all cases, the number of QP fragments was only one and that the fracture line of the fragment was peripherally distributed. Meanwhile, 80% and 86% of the displaced fractures at the proximal AO and SPO lines, respectively, were simple. There was an intact area inferoanterior to the sacroiliac joint in all cases except for three cases in which the sacroiliac joint was intruded on by SPO lines. According to these results, most QP fragments could be fixed with intrapelvic buttress plating or infrapectineal plating, as recommended by Peter et al. [15,16,17,18]. Compression and reduction are produced by the screws inserted into the intact area inferoanterior to the sacroiliac joint through a contoured or anatomic plate [24]. An intrapelvic buttress plate was useful when the AO lines were positioned on or lateral to the arcuate line, and the size of the intact bone just inferoanterior to the sacroiliac joint was large enough to accommodate two screws [25]. We previously recommended an extrapelvic plate combined with periarticular screw fixation [19] to fix the QP fragment with a simple fracture pattern on the proximal AO lines. A novel anatomic plate [22] was proposed to fix the QP fragment when comminuted fragments were identified along all AO lines. Since nearly 32% of comminuted fractures were found at the junction between the superior pubic rim and the inferoanterior wall of the acetabulum, and because the QP fragment close to the acetabular notch is thin, it is not optimal to fix fractures at this site using periarticular screws.
Accompanied by the substantial/excellent interobserver variabilities, the features of variable fracture lines and comminuted fragments were fairly cognizable in this study. However, potential challenges still exist in the categorization in routine clinical practice, especially in those fractures with extremely severe and nontypical fracture patterns. To some extent, the fracture identification in this study could be verified by using delicate 3D models with unrestricted angular adjustment in the mapping software. However, in clinical practices where fracture mapping software may not be available, it may be hard to obtain a confident categorization. Thus, interobserver variability studies are requisite in assessing fracture patterns of the ABC acetabular fractures with a larger sample size.
This study has a few limitations. Firstly, this study was based on the hypothesis that the ABC acetabular fractures originate from the inferoanterior rim, despite the fact that the mechanism of the fracture is unclear. Secondly, according to the OTA/AO classification, ABC acetabular fractures are divided into types C1, C2, and C3. In this study, the possible effects of these classifications were not considered.
In conclusion, we found that the number of QP fragments in ABC acetabular fractures was one in a majority of cases and that the arcuate line and the site posterior to the line and superoposterior to the QP were mostly involved. The major fracture patterns in the proximal AO and SPO lines were simple. The key position of reduction and internal fixation of QP fragments was the superoposterior region of the fragments. These results may provide references for the surgical approach choice and internal fixation.
References
Giannoudis PV, Grotz MR, Papakostidis C, Dinopoulos H. Operative treatment of displaced fractures of the acetabulum. A meta-analysis. J Bone Joint Surg Br. 2005;87(1):2–9.
Chotai N, Arshad H, Bates P. Radiographic anatomy and imaging of the acetabulum. Orthop Trauma. 2018;32:102–9.
Judet R, Judet J, Letournel E. Fractures of the acetabulum: classification and surgical approaches for open reduction. Preliminary Report. J Bone Joint Surg Am. 1964;46:1615–46.
Meinberg EG, Agel J, Roberts CS, Karam MD, Kellam JF. Fracture and dislocation classification compendium-2018. J Orthop Trauma. 2018;32(Suppl 1):S1–170.
Isaacson MJ, Taylor BC, French BG, Poka A. Treatment of acetabulum fractures through the modified Stoppa approach: strategies and outcomes. Clin Orthop Relat Res. 2014;472(11):3345–52.
Pierannunzii L, Fischer F, Tagliabue L, Calori GM, d’Imporzano M. Acetabular both-column fractures: essentials of operative management. Injury. 2010;41(11):1145–9.
Yang Y, Zou C, Fang Y. Mapping of both column acetabular fractures with three-dimensional computed tomography and implications on surgical management. BMC Musculoskelet Disord. 2019;20(1):255.
Yang Y, Yi M, Zou C, Yan ZK, Yan XA, Fang Y. Mapping of 238 quadrilateral plate fractures with three-dimensional computed tomography. Injury. 2018;49(7):1307–12.
Yang Y, Zou C, Fang Y. A study on fracture lines of the quadrilateral plate based on fracture mapping. J Orthop Surg Res. 2019;14(1):310.
ElNahal WA, Abdel Karim M, Khaled SA, Abdelazeem AH, Abdelazeem H. Quadrilateral plate fractures of the acetabulum: proposition for a novel classification system. Injury. 2018;49(2):296–301.
Xie X, Zhan Y, Dong M, He Q, Lucas JF, Zhang Y, et al. Two and three-dimensional CT mapping of Hoffa fractures. J Bone Joint Surg Am. 2017;99(21):1866–74.
Matta JM. Operative treatment of acetabular fractures through the ilioinguinal approach: a 10-year perspective. J Orthop Trauma. 2006;20(1 Suppl):S20-29.
Cole JD, Bolhofner BR. Acetabular fracture fixation via a modified Stoppa limited intrapelvic approach. Description of operative technique and preliminary treatment results. Clin Orthop Relat Res. 1994;305:112–23.
Keel MJ, Ecker TM, Cullmann JL, Bergmann M, Bonel HM, Buchler L, et al. The Pararectus approach for anterior intrapelvic management of acetabular fractures: an anatomical study and clinical evaluation. J Bone Joint Surg Br. 2012;94(3):405–11.
Peter RE. Open reduction and internal fixation of osteoporotic acetabular fractures through the ilio-inguinal approach: use of buttress plates to control medial displacement of the quadrilateral surface. Injury. 2015;46(Suppl 1):S2-7.
Qureshi AA, Archdeacon MT, Jenkins MA, Infante A, DiPasquale T, Bolhofner BR. Infrapectineal plating for acetabular fractures: a technical adjunct to internal fixation. J Orthop Trauma. 2004;18(3):175–8.
Tosounidis TH, Gudipati S, Panteli M, Kanakaris NK, Giannoudis PV. The use of buttress plates in the management of acetabular fractures with quadrilateral plate involvement: is it still a valid option? Int Orthop. 2015;39(11):2219–26.
Zhuang Y, Zhang K, Wang H, Wei X, Liu P, Wang PF, et al. A short buttress plate fixation of posterior column through single ilioinguinal approach for complex acetabular fractures. Int Orthop. 2017;41(1):165–71.
May C, Egloff M, Butscher A, Keel MJB, Aebi T, Siebenrock KA, et al. Comparison of fixation techniques for acetabular fractures involving the anterior column with disruption of the quadrilateral plate: a biomechanical study. J Bone Joint Surg Am. 2018;100(12):1047–54.
Boni G, Pires RE, Sanchez GT, Dos Reis FB, Yoon RS, Liporace FA. Use of a stainless steel locking calcaneal plate for quadrilateral plate buttress in the treatment of acetabular fractures. Eur J Orthop Surg Traumatol. 2019;29(5):1141–5.
Zhang R, Yin Y, Li S, Jin L, Guo J, Hou Z, et al. Fixation of displaced acetabular fractures with an anatomic quadrilateral surface plate through the Stoppa approach. Orthopedics. 2019;42(2):e180–6.
Sen RK, Saini G, Kadam S, Raman N. Anatomical quadrilateral plate for acetabulum fractures involving quadrilateral surface: a review. J Clin Orthop Trauma. 2020;11(6):1072–81.
Wu YD, Cai XH, Liu XM, Zhang HX. Biomechanical analysis of the acetabular buttress-plate: are complex acetabular fractures in the quadrilateral area stable after treatment with anterior construct plate-1/3 tube buttress plate fixation? Clinics (Sao Paulo). 2013;68(7):1028–33.
Nicol G, Sanders E, Liew A, Wilkin G, Gofton WT, Papp S, et al. Does use of a quadrilateral surface plate improve outcome in elderly acetabular fractures? J Clin Orthop Trauma. 2020;11(6):1045–52.
Meena UK, Sharma AK, Behera P, Lamoria RK, Meena RC, Chahar PK. Treatment of acetabular fractures with quadrilateral plate injury - a comparison of two commonly used methods. Orthop Traumatol Surg Res. 2021;108:102951.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This study was conducted in accordance with the principles of the Declaration of Helsinki. Ethical approval was granted by the review board of our institution.
Informed consent
The requirement for obtaining patient informed consent was waived by the ethics review board.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ye, K., Tang, J., Shen, L. et al. Three-dimensional morphological analysis of quadrilateral plate fragments in associated both-column acetabular fractures. Skeletal Radiol 51, 2175–2184 (2022). https://doi.org/10.1007/s00256-022-04068-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-022-04068-8