Abstract
Injuries of the cervical spine are uncommon in children. The distribution of injuries, when they do occur, differs according to age. Young children aged less than 8 years usually have upper cervical injuries because of the anatomic and biomechanical properties of their immature spine, whereas older children, whose biomechanics more closely resemble those of adults, are prone to lower cervical injuries. In all cases, the pediatric cervical spine has distinct radiographic features, making the emergency radiological analysis of it difficult. Such features as hypermobility between C2 and C3, pseudospread of the atlas on the axis, pseudosubluxation, the absence of lordosis, anterior wedging of vertebral bodies, pseudowidening of prevertebral soft tissue and incomplete ossification of synchondrosis can be mistaken for traumatic injuries. The interpretation of a plain radiograph of the pediatric cervical spine following trauma must take into account the age of the child, the location of the injury and the mechanism of trauma. Comprehensive knowledge of the specific anatomy and biomechanics of the childhood spine is essential for the diagnosis of suspected cervical spine injury. With it, the physician can, on one hand, differentiate normal physes or synchondroses from pathological fractures or ligamentous disruptions and, on the other, identify any possible congenital anomalies that may also be mistaken for injury. Thus, in the present work, we discuss normal radiological features of the pediatric cervical spine, variants that may be encountered and pitfalls that must be avoided when interpreting plain radiographs taken in an emergency setting following trauma.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The analysis of the pediatric cervical spine in emergency can be challenging because of the wide range of normal anatomic variants and synchondroses that can be mistaken for traumatic injuries. Initial radiographs are almost always technically imperfect because of pain-induced contracture. An understanding of the unique anatomic, radiographic and biomechanical characteristics of the pediatric cervical spine is essential. The cervical spine reaches adult proportions at around 8 to 10 years of age [1]. Spine injuries usually occur in the upper cervical region (C1–C3) in children aged less than 8 years. Beyond 8 years, lesions are most seen in the lower cervical region (C3–C7). Normal variants of the pediatric cervical spine include pseudospread of the atlas on the axis, pseudosubluxation, absence of lordosis, anterior wedging of vertebral bodies, pseudowidening of prevertebral soft tissue and incomplete ossification of synchondrosis.
Development and normal anatomy
An understanding of the developmental anatomy and biomechanical properties of the pediatric cervical spine facilitates the interpretation of its imaging. The childhood cervical spine presents many particularities such as epiphyseal variations, a unique vertebral architecture, incomplete ossification of synchondroses and apophyses, and hypermobility due to ligamentous laxity, especially between C2 and C3. Confronting these particularities, the radiologist may feel uncertain when interpreting the radiographs of children admitted for head or neck trauma.
Atlas (C1)
The atlas has many features (Fig. 1). It is composed of three primary ossification centers: an anterior arch and two posterior neural arches separated by synchondroses. At birth, the neural arches are ossified but the anterior arch, which replaces the absent vertebral body, most frequently is not (only 20 % of cases) (Fig. 2). The neural arches fuse posteriorly by 3 to 4 years of age, and the anterior arch fuses with the neural arches by 7 years of age [2, 3].
Anatomy of the first cervical vertebra (atlas). Drawing (a) and anteroposterior radiograph (b) illustrating the three primary ossification centers of the atlas: two posterior neural arches, ossified at birth (yellow), and one anterior arch, ossified at birth in only 20 % of cases (red). The ossification centers are separated by neurocentral (arrows) and posterior synchondroses (double arrow)
A 4-day-old child admitted to the emergency unit for a high-energy traumatism. On the lateral radiograph (a), the anterior arch of C1 is not ossified. (1) Dens of C2; (2) body of C2; (3) subdental synchondrosis; (4) neural arch of C1; (5) neural arch of C2. Axial CT with 3D reconstruction of C1 vertebra (b, c) shows the neural arches (arrows) and the intraneural “posterior” synchondrosis (double arrow). The anterior arch of C1 is absent; 3D reconstruction (d) permits the visualization of the symmetric and central position of C1 (red) in relation to other vertebrae, especially C2
Axis (C2)
The axis has a unique development. It is derived from four ossification centers: one for the dens, one for each neural arch and one for the body (Figs. 3 and 4). The C2 body fuses to the dens between 3 and 6 years of age. The resulting fusion line may be seen until the age of 11 and sometimes throughout life (in a third of the population). The C2 posterior arches fuse at their midline by 2 to 3 years and to the body by 3 to 6 years. The dens is formed in utero from two separate ossification centers that fuse in the midline by the 7th gestational month. A secondary ossification center at the apex of the dens appears between 6 and 8 years of age and fuses with the dens around 12 years of age (Fig. 5). Failure of fusion at this location results in ossiculum terminale, a condition that is usually benign but sometimes associated with atlantoaxial instability [4–7].
Anatomy of the second cervical vertebra (axis). Drawing (a) and anteroposterior radiograph centered on C1–C2 (b, c) illustrating the four primary ossification centers of the axis: one for each neural arch (red), one for the body (green) and one for the dens (blue). A secondary ossification center called ossiculum terminale (purple) appears at the apex of the dens (curved arrow). A subdental synchondrosis (arrowheads) is located between the body of C2 and the dens. The neural arches fuse with the body and dens through synchondroses (arrows)
Development of ossiculum terminale of C2. An open-mouth radiograph centered on C1–C2 (a) illustrating the four primary ossification centers of C2: one for each neural arch (red), one for the body (green) and one for the dens (blue). Ossiculum terminale (arrow) appears at the apex of C2 (b, c) and the two longitudinal secondary ossification centers of the dens can be seen (arrowheads) (b)
Lower cervical spine (C3–C7)
The third through seventh cervical vertebrae share a similar ossification pattern comprising a single ossification center for the vertebral body and an ossification center for each neural arch (Fig. 6). The neural arches fuse posteriorly between 2 and 3 years, and the neurocentral synchondroses, located between the neural arches and the vertebral body, fuse by 3 to 6 years of age. There are five secondary ossification centers that may remain open as late as 25 to 30 years of age [8]. These include one each for the spinous processes, transverse processes and the ring apophyses about the vertebral endplates. Partially ossified ring apophyses are observed at multiple levels and at different ages along the anteroinferior corners of vertebral bodies. Their complete ossification occurs belatedly, and they should not be confused with fractures [6, 9]. Posterior synchondroses may appear as a radiolucent thin line crossing the vertebral bodies and thus may be confused with a longitudinal fracture. Their visibility is variable, depending on the orientation of the x-ray beam.
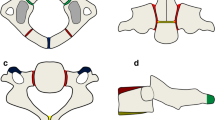
Anatomy of the third to seventh cervical vertebrae. Drawing (a) and axial CT at the level of C3 (b, c), illustrating the vertebra body (yellow), neural arches (red) and synchondroses: neurocentral (arrowheads) and posterior (arrow). On anteroposterior radiographs (d), posterior synchondroses may appear as radiolucent thin lines crossing the vertebral bodies (arrows)
Radiographic views and characteristics
Radiographic findings vary widely in children, and therefore care must be taken when analyzing the images and correlating radiographic information with the patient’s history and clinical findings.
Beyond the age of 16 years, patients should undergo CT, since their spines and the injuries they incur resemble those of adults. MR imaging remains especially helpful in the identification and evaluation of spinal cord, soft tissue and ligamentous injuries.
Furthermore, the Appropriateness Criteria of the American College of Radiology (ACR) [10] indicate radiography as the imaging method of choice for children aged less than 16 years. Anteroposterior, lateral and open-mouth views are the only views needed for diagnosis.
Lateral radiograph
The lateral view is the most important for potential cervical injuries in children (Fig. 7). It must include the entire cervical spine and the C7–T1 disc space.
Criteria for a successful lateral radiograph include the superposition of the mandibular angle and articular processes, an absence of duplication of the posterior wall and visibility of vertebrae, intervertebral discs and the posterior articular interline from the skull base to T1.
Several important points should be verified in this view, including the vertebral lines (anterior, posterior and spinolaminar), the posterior cervical line, the atlantodens interval, prevertebral soft tissues and Harris’ ring.
Vertebral lines
The vertebral lines should be aligned and parallel. The anterior, posterior and spinolaminar vertebral lines follow respectively the anterior faces of the vertebral bodies, the posterior faces of the vertebral bodies and the anterior aspects of the spinous processes [11]. The posterior cervical line (described by Swischuk) is actually the upper end of the spinolaminar line. It is drawn between the anterior aspects of the C1 and C3 spinous processes (Fig. 8). This line intersects, touches or comes close to the anterior cortex of the spinous tip of C2 on both flexion and extension radiographs [12].
Static and dynamic lateral radiographs of different children. On static views (a, b), the posterior cervical line does not change with age. On dynamic views on flexion and extension (c, d), the alignment of this line does not change even in this 10-year-old child with fused vertebral bodies and posterior articular masses of C2 and C3 (yellow) and C4 and C5 (red) in the setting of a malformation syndrome
Atlantodens interval
The atlantodens interval is defined as the distance between the anterior aspect of the dens and the posterior aspect of the anterior ring of the atlas. In children, this distance should not exceed 5 mm before 1 year, 4 mm before 8 years or 3 mm after 8 years, when the cervical spine reaches adult proportions [13]. Exceeding these thresholds indicates instability and suggests ligamentous disruption [14–16].
Prevertebral soft tissues
A prevertebral space of less than 7 mm at the C3 level is considered normal in children. Below C4, this space should not exceed 14 mm [17]. Crying is the most common cause of widening.
Harris’ ring
This ring-like structure is a confluence of shadows from the superior articular facet (upper arc), posterior vertebral body (posterior arc), inferior margin of the transverse foramen (inferior arc) and anterior body (anterior arc) of the C2 [18]. Harris’ ring should remain unbroken.
Anteroposterior radiograph
Criteria for a successful anteroposterior radiograph include good visibility of the articular interlines from C3 to T1, the trachea positioned on the midline, the spinous processes aligned on the midline and symmetric mandibles.
This view is used to verify that the transverse process lines (two), uncinate lines (two) and spinous line (one) are parallel and equidistant, that the lateral margins are intact and undulate smoothly, that the spinous processes align and lie in the midline with approximately even spacing and that the height of the vertebral bodies should be approximately equal (Fig. 9).
Landmarks on anteroposterior radiograph. Transverse process lines (2, blue), uncinate lines (2, yellow) and spinous line (1, red) are all parallel and equidistant. Lateral margins should be intact and smoothly undulating. Height of the vertebral bodies should be approximately equal. The interspinous distance of two adjacent segments must not differ by more than 2 mm
Open-mouth radiograph (odontoid view)
This view is used to verify that the lateral masses of C1 do not overhang the articular masses of C2, that the lateral masses of C1 and articular masses of C2 are symmetrical, that the lateral masses of C1 are equidistant from the dens, and that the dens and the spinous process of C2 lie along the same vertical line (Fig. 10).
Special studies may supplement plain radiographs of the cervical spine in children. Oblique radiographs are useful in showing detail of the facet joints and pedicles. Dynamic views should be done when osseous lesions are absent from the static views (anteroposterior, lateral, open mouth). Furthermore, dynamic views are particularly useful to study C2–C3 and to avoid over- or underestimating pseudosubluxation.
Normal radiographic variants and pitfalls
Pseudosubluxation C2–C3
Pseudosubluxation is a physiologic misalignment caused by ligamentous laxity and a more horizontal orientation of the facet joints in children compared to adults [19, 20]. Frequently observed in children less than 8 years old, it usually occurs at the C2–C3 level and less commonly at the C3–C4 level. In normal circumstances, this anterior displacement manifests on the neutral and flexion lateral views and should reduce on extension [21] (Fig. 11). The reduction when the neck is in extension helps to differentiate pseudosubluxation from more serious disorders. If the posterior cervical line misses the anterior cortex of C2 by more than 1.5 mm, a hangman’s fracture should be suspected. Otherwise, the finding should be considered as pseudosubluxation [22].
Pseudospread of the atlas on the axis (pseudo-Jefferson fracture)
Pseudospread of the atlas on the axis is uncommon in children. The ossification of the lateral masses of C1 may precede that of the body of C2, causing an apparent lateral displacement of the masses in relation to C2 (Fig. 12). Pseudospread of the atlas is present in 90 % of children under 2 years of age [23]. Up to 6 mm of combined lateral offset of the lateral masses relative to the dens is common in patients up to 4 years old and may be seen in patients up to 7 years old [24, 25]. When lateral offset exceeds 6 mm, a Jefferson fracture should be suspected. In this setting, the interest of open-mouth radiograph remains debatable because Jefferson fractures are rare in children under 10 years, and when they do occur, severe trauma is usually involved, which necessitates CT imaging instead of plain radiography.
Open-mouth radiograph in a 3-year-old and in a 10-year-old child. In young children, the ossification of the lateral masses of C1 may precede that of the body of C2, giving an impression of a lateral displacement of the former in relation to the latter (a). Beyond 6 years of age (b), the lateral masses of C1 and the articular masses of C2 should be perfectly symmetrical
Anterior wedging of vertebral bodies
In children, anterior wedging is merely a radiographic phenomenon due to the pattern of vertebral ossification; it is not morphological. In babies and infants, vertebral bodies appear oval on radiography. As children grow, their vertebral bodies become increasingly rectangular [26] (Fig. 13). In younger children and particularly at the C3–C4 level, there may be a difference in height of up to 3 mm between the anterior and middle aspects of the vertebral bodies, which should not be mistaken for a compression fracture [24, 27]. This finding is secondary to hypermobility of the spine and because C3–C4 is the flexing point of the cervical spine at this age. As the child matures the flexing point slides to C5–C6 and the wedging deformity resolves.
Absence of lordosis
An absence of normal lordosis on a lateral view of an adult cervical spine suggests the possibility of a ligamentous injury. However, this finding is frequent in children, especially those aged less than 16 years and x-rayed in a neutral position [19, 28]. Absence of normal lordosis normally disappears in extension, whereas kyphosis resulting from an injury does not.
Pseudowidening of prevertebral soft tissue
Prevertebral soft tissue swelling in adults can indicate a cervical spine injury. In pediatric patients, widening of the prevertebral soft tissues may simply be due to expiration (especially if a child is crying), swallowing or particular degrees of flexion or obliquity. Prevertebral space of less than 7 mm at the C3 level is considered normal in children and it should not exceed 14 mm below C4 [29]. When widening of prevertebral soft tissue is observed, a lateral radiograph fluoroscopy should be performed in mild extension and in inspiration (Fig. 14) to determine the nature of the prevertebral soft tissue swelling [17]: if this swelling is pathological, the increased space will persist.
Pseudowidening of prevertebral soft tissue in a 10-month-old child. Lateral radiograph (a) shows an “abnormal” thickening of prevertebral soft tissue (•) with a suspicion of C2 on C3 subluxation in a trauma context. Under real-time fluoroscopy in expiration (b) and in inspiration (c), the important pseudowidening observed in expiration (arrows) disappears in mild extension and in inspiration (arrowheads)
Secondary ossification centers
Variants of the atlas (C1)
There are several ossification and fusion variants of the atlas. The anterior arch usually develops from a single ossification center, but uncommonly it may develop from four small ones [30]. Unfused ossification centers in the atlas is a normal finding in young children. However, in some cases, fusion never occurs, resulting in a cleft that persists into adulthood. Such a cleft shows smooth corticated margins, which help to distinguish it from a fracture. Clefts in the atlas most commonly occur at the posterior synchondrosis [31]. Variants and malformations in the posterior arch of the atlas include failure of posterior synchondrosis fusion, unilateral and bilateral paramedian clefts, and variable absence of the posterior arches [32–34].
Variants of the axis (C2)
There are three entities that may result in an ossific density adjacent to the cranial aspect of the dens: persistent ossiculum terminale, os odontoideum and dens fracture. Ossiculum terminale is a normal secondary ossification center that appears by 3 to 6 years of age and usually fuses to the dens by 12 years of age [35]. However, an unfused ossiculum terminale may persist into adulthood. It presents as a well-corticated ossicle that abuts the dens tip. An os odontoideum is larger than a persistent ossiculum terminale. It is a smooth, well-corticated ossicle located superior to a small dens. It can be located in the expected anatomic position posterior to the anterior arch of C1 (orthotopic os odontoideum) or be located in some other position (dystopic os odontoideum) [36, 37]. A feature that helps distinguish an os odontoideum from a type 2 dens fracture (the third entity) is the distance between the intact dens and the ossific fragment. In a fracture, there is usually only a narrow zone of separation between the bone fragments, and the overall size and shape of the dens will be maintained. An os odontoideum usually results in a larger gap between the os and the dens, and it usually does not exhibit the expected contour of the upper dens [38].
Persistence of subdental synchondrosis of C2
The centrum and odontoid ossification centers fuse across the subdental synchondrosis (Fig. 15), usually between ages 3 to 6. A vestige of the synchondrosis may remain visible up to 11 years of age [21].
It appears as a sclerotic line surrounded by lucency (Fig. 16) and may be erroneously interpreted as an undisplaced fracture or even a non-union of an old fracture [39].
Subdental synchondroses. On lateral radiographs taken in a 7-year-old (a) and in a 9-year-old (b) girl in the setting of trauma, a persistent radiolucent line is visible between the dens (arrowheads) and the body of C2 (curved arrow). This line is surrounded by a thin and regular sclerotic margin (double arrows), corresponding to a remnant of the cartilaginous subdental synchondrosis
Ring apophyses
Ring apophyses are normal and common findings in the growing child. They appear as thin wedge-like structures along the anterior inferior and superior borders of the developing vertebral bodies on a lateral radiograph.
This cartilaginous structure, usually seen at multiple levels, begins to ossify at age 10 and to fuse at age 17 (Fig. 17). Complete fusion with the vertebral body occurs between 18 and 25 years of age [40, 41]. An unfused inferior ring apophysis can be mistaken for an avulsion but normal physeal plates should be recognizable by their smooth, regular structures with subchondral sclerotic lines.
Non-symmetric closure of neurocentral synchondrosis from C3 through C7
The neurocentral synchondroses are the joining elements between the neural arches and the vertebral body. The neural arches fuse with the body between 3 and 6 years of age.
Neurocentral synchondrosis closure proceeds craniocaudally and must be symmetric to maintain normal spine alignment. Occasionally, closure may not occur or occur non-symmetrically. Persistence of these synchondroses may be confused with fractures, especially at 6 to 7 years of age. On anteroposterior radiographs, neurocentral synchondroses may appear as a smooth, regular, radiolucent line with a sclerotic border crossing the vertebral bodies (Fig. 18). Acute fractures are irregular and non-sclerotic.
Unfused synchondroses. Anteroposterior cervical radiographs in a 2-year-old and in a 7-year-old child illustrating neurocentral synchondroses (thin arrows) between vertebral bodies (yellow) and still-cartilaginous neural arches (red). Note their non-symmetric closure (a). Osteosclerosis (double arrow) distinguishes them from real fracture, especially in post-trauma (b)
Miscellaneous pitfalls
Other anatomical elements of the head may appear as radiolucent lines and can sometimes be mistaken for a fracture (Fig. 19). Particularly, on an open-mouth view, centered on C1–C2, the interdental space between the two central incisors can resemble a fracture, but identifying the outline of the incisors will prevent an error in interpretation. Also, the laryngotracheal airways can mimic posterior synchondroses or fractures. A CT scan can eliminate any confusion.
Other pitfalls on anteroposterior and open-mouth radiographs in children. On anteroposterior radiographs (a), laryngotracheal airway features (arrowheads) can mimic posterior synchondroses or fractures. In open-mouth views, centered on C1–C2 (b), the interdental space between the two central incisors (thick arrows) can resemble a fracture, but identifying the outline of the incisors (dotted line) will clarify the situation. In another open-mouth view from a different child (c), the interdental space is visible (thin arrows). The presence of that space should not divert attention away from a real lesion (curved arrow)
Conclusion
Sound knowledge of the pediatric cervical spine is essential to accurately diagnose suspected traumatisms while avoiding errors and pitfalls. The anatomy of the pediatric cervical spine evolves continuously with growth, and it presents several normal variants. Thus, interpreting post-trauma plain radiographs of the pediatric spine can be difficult. Good interpretation must be based on the age of the child, the anatomical location of the injury and the mechanism of injury.
References
Bailey DK. The normal cervical spine in infants and children. Radiology. 1952;59:712–9.
Fesmire FM, Luten RC. The pediatric cervical spine: developmental anatomy and clinical aspects. J Emerg Med. 1989;7:133–42.
Ogden JA. Skeletal injury in the child. Spine. 2nd ed. Philadelphia: Saunders; 1990.
Herman MJ, Pizzutillo PD. Cervical spine disorders in children. Orthop Clin N Am. 1999;30:457–66.
Harris Jr JH, Mirvis SE. The radiology of acute cervical spine trauma. 3rd ed. Baltimore: Williams & Wilkins; 1996. p. 1–73.
Swischuk LE. Emergency imaging of the acutely ill or injured child. The spine and the spinal cord. 4th ed. Philadelphia: Lippincott Williams & Wilkins; 2000. p. 532–87.
Ogden JA. Radiology of postnatal skeletal development. XII. The second cervical vertebra. Skelet Radiol. 1984;12:169–77.
Lawson JP, Ogden JA, Bucholz RW, Hughes SA. Physeal injuries of the cervical spine. J Pediatr Orthop. 1987;7:428–35.
Dwek JR, Chung JB. Radiography of cervical spine injury in children: are flexion-extension radiographs useful for acute trauma? Am J Roentgenol. 2000;174:1617–9.
Daffner RH, Hackney DB. ACR Appropriateness Criteria® on suspected spine trauma. J Am Coll Radiol. 2007;4(11):762–75.
Williams CF, Bernstein TW, Jelenko 3rd C. Essentiality of the lateral cervical spine radiograph. Ann Emerg Med. 1981;10:198–204.
Swischuk LE. Anterior displacement of C2 in children: physiologic or pathologic? Radiology. 1977;122:759–63.
Steel HH. Anatomical and mechanical considerations of the atlanto-axial articulation. J Bone Joint Surg Am. 1968;50:1481–8.
Wang JC, Nuccion SL, Feighan JE, Cohen B, Dorey FJ, Scoles PV. Growth and development of the pediatric cervical spine documented radiographically. J Bone Joint Surg Am. 2001;83-A:1212–8.
Locke GR, Gardner JI, Van Epps EF. Atlas-dens interval (ADI) in children: a survey based on 200 normal cervical spines. Am J Roentgenol Radium Therapy Nucl Med. 1966;97:135–40.
Roche C, Carty H. Spinal trauma in children. Pediatr Radiol. 2001;31:677–700.
Warner WC. Rockwood and Wilkins’ fractures in children. Cervical spine injuries in children. Baltimore: Lippincott Williams & Wilkins; 2001. p. 809–46.
Harris Jr JH, Burke JT, Ray RD, Nichols-Hostetter S, Lester RG. Low (type III) odontoid fracture: a new radiologic sign. Radiology. 1984;153:353–6.
Hall DE, Boydston W. Pediatric neck injuries. Pediatr Rev. 1999;20:13–9.
Shaw M, Burnett H, Wilson A, Chan O. Pseudosubluxation of C2 on C3 in polytraumatized children: prevalence and significance. Clin Radiol. 1999;54:377–80.
Cattell HS, Filtzer DL. Pseudosubluxation and other normal variations in the cervical spine in children. J Bone Joint Surg Am. 1965;47:1295–309.
Swischuk LE. Imaging of the cervical spine in children. New York: Springer; 2013. p. 11–28.
Kriss VM, Kriss TC. Imaging of the cervical spine in infants. Pediatr Emerg Care. 1997;13:44–9.
Lustrin ES, Karakas SP, Ortiz AO, Cinnamon J, Castillo M, Vaheesan K, et al. Pediatric cervical spine: normal anatomy, variants, and trauma. Radiographics. 2003;23:539–60.
Suss RA, Zimmerman RD, Leeds NE. Pseudospread of the atlas: false sign of Jefferson fracture in young children. Am J Roentgenol. 1983;140:1079–82.
Swischuk LE, Swischuk PN, John SD. Wedging of C3 in infants and children: usually a normal finding and not a fracture. Radiology. 1993;188:523–6.
Bonadio WA. Cervical spine trauma in children. I. General concepts, normal anatomy, radiographic evaluation. Am J Emerg Med. 1993;11:158–65.
Loder RT. The cervical spine. 4th ed. Philadelphia: Lippincott-Raven; 1996. p. 739–79.
Grabb PA, Hadley MN. Spinal column trauma in children. New York: Thieme; 1999. p. 935–53.
Junewick JJ, Chin MS, Meesa IR, Ghori S, Boynton SJ, Luttenton CR. Ossification patterns of the atlas vertebra. Am J Roentgenol. 2011;197:1229–34.
Glasser SA, Glasser ES. Rare congenital anomalies simulating upper cervical spine fractures. J Emerg Med. 1991;9:331–5.
Haakonsen M, Gudmundsen TE, Histol O. Midline anterior and posterior atlas clefts may simulate a Jefferson fracture. Acta Orthop Scand. 1995;66:369–71.
Sharma A, Gaikwad SB, Deol PS, Mishra NK, Kale SS. Partial aplasia of the posterior arch of the atlas with isolated posterior arch remnant: findings in three cases. Am J Neuroradiol. 2000;21:1167–71.
Currarino G, Rollins N, Diehl JT. Congenital defects of the posterior arch of the atlas: a report of 7 cases including an affected mother and son. Am J Neuroradiol. 1994;15:249–54.
Ogden JA. Radiology of postnatal skeletal development. XI. The first cervical vertebra. Skelet Radiol. 1984;12:12–20.
Macalister A. Notes on the development and variations of the atlas. J Anat Physiol. 1893;27:519–42.
Patel JC, Tepas 3rd JJ, Mollitt DL, Pieper P. Pediatric cervical spine injuries: defining the disease. J Pediatr Surg. 2001;36:373–6.
Platzer P, Jaindl M, Thalhammer G, Dittrich S, Kutscha-Lissberg F, Vecsei V, et al. Cervical spine injuries in pediatric patients. J Trauma. 2007;62:389–96.
Carr RB, Fink KR, Gross JA. Imaging of trauma: part 1, pseudotrauma of the spine-osseous variants that may simulate injury. Am J Roentgenol. 2012;199:1200–6.
Köhler A, Zimmer EA. Borderlands of the normal and early pathologic in skeletal roentgenology. 3rd ed. New York: Grune and Stratton; 1968.
Bick EM, Copel JW. The apophysis of the human vertebra. J Bone Joint Surg Am. 1951;33:783–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that they have no conflicts of interest.
This article involved no studies with human participants or animals performed by any of the authors.
This article does not contain patient data.
Additional information
None of the authors received any financial support during the creation of this work
Rights and permissions
About this article
Cite this article
Adib, O., Berthier, E., Loisel, D. et al. Pediatric cervical spine in emergency: radiographic features of normal anatomy, variants and pitfalls. Skeletal Radiol 45, 1607–1617 (2016). https://doi.org/10.1007/s00256-016-2481-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-016-2481-9