Abstract
Objective
Objectives were to study the MRI appearance of the repaired distal biceps tendon (DBT), anatomically reinserted, and to search for a correlation between tendon measurements and functional results.
Materials and methods
Twenty-five patients (mean age, 49 ± 4.9 years old) who benefited from 3-T MRI follow-up of the elbow after surgical reinsertion of the DBT were retrospectively included and compared to a control group (n = 25; mean age, 48 ± 10 years old). MRI was performed during the month of clinical follow-up and on average 22 months after surgery. Delayed complications (secondary avulsion, new rupture), intratendinous osteoma, tendinous signal on T1-weighted (T1w) and fat-suppressed proton density-weighted (FS-PDw) images as well as DBT measurements were recorded. The maximum isometric elbow flexion strength (MEFS) and range of motion of the elbow were assessed.
Results
Repaired DBT demonstrated a heterogeneous but normally fibrillar structure. Its low T1w signal was less pronounced than that of normal tendons, and the FS-PDW image signal was similar to that of T1w images. MRI detected seven osteomas (Se = 53 % vs. plain radiography), one textiloma and one secondary avulsion. Repaired DBT measurements were significantly correlated with MEFS (dominant arm R2: 0.38; nondominant arm R2: 0.54); this correlation involved the insertion surface (Δ = −75.7 mm2, p = 0.046), transverse diameter (Δ = −2.6 mm, p = 0.018), anteroposterior diameter at the level of the radial head (Δ = −3.9 mm, p = 0.001) and DBT cross-sectional area (Δ = −50.2 mm2, p = 0.003).
Conclusion
The quality of functional outcome after anatomical elbow rehabilitation of DBT correlates with the extent of tendinous hypertrophy during the healing process.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The incidence of distal biceps tendon (DBT) rupture is low, estimated at 1.2 cases per 100,000 patients per year in the USA [1]. It represents only 3 % of the ruptures involving this muscle, which mainly concern the tendon of its long head or, more rarely, its muscular body [2, 3]. DBT rupture occurs in the dominant arm (80 % of cases) of middle-aged males (40–50 years old) engaged in heavy physical activity [1], although some cases have been described in females [4]. Tobacco intoxication and use of anabolic steroids or statins are associated with an increased risk of rupture [5, 6]. The injury appears as a result of a concentric contraction against resistance on a 90° flexed and supinated forearm (lifting force) or by a sudden eccentric contraction (forced extension), creating an avulsion of its enthesis from the radial tuberosity [7, 8]. More rarely, myotendinous strain and disinsertions may occur spontaneously or secondary to minor trauma on preexisting tendinosis [2].
Conservative treatment is associated with significant functional impairment [9, 10], so that except for patients with severe comorbidities [11], surgery is the treatment of choice in almost all cases. The formerly nonanatomical surgical fixation by tenodesis of the DBT is no longer performed except in the case of chronic ruptures or among older patients [12]. It has been superseded by the so-called anatomical fixation, which allows the DBT to be fixed on the radial tuberosity through transosseous reinsertion [13], suture anchors [14, 15] or intraosseous endobuttons [16]. These anatomical techniques provide better functional outcomes in supination and flexion strength [12, 17, 18].
While many studies have focused on clinical outcomes [3, 19, 20] or the complication rates of various surgical techniques [21], few have explored the 1.5-T magnetic resonance imaging (MRI) appearance of reinserted DBT [22, 23]. Three-Tesla MRI now offers a better signal-to-noise ratio than 1.5-T equipment and a better interobserver reproducibility than ultrasound exploration, especially in this postoperative context [24, 25]. Although CT scans provide a good view of osseous structures, they fail to reveal myotendinous structures distinctly. However, this semiology may be useful when exploring a painful elbow after reconstructive surgery. Our work retrospectively investigated the 3-T MRI appearance of anatomically reinserted DBT with an anterior single incision and a suture anchor. The objectives were twofold:
-
to describe the MRI appearance of the DBT reinserted in anatomical position
-
and to search for a correlation between MRI semiology and the quality of functional results.
Materials and methods
Inclusion criteria
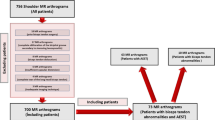
Patients were retrospectively and consecutively recruited between May 2006 and August 2012 for this unicentric case-control study. The case group included 25 patients who benefited from a clinical follow-up at least 6 months after anatomical reinsertion of the DBT on the radial tuberosity and a postoperative MRI control within the month. Patients whose postoperative MRI evaluation was incomplete (no axial or sagittal images) or of insufficient quality were excluded. Local institutional review board approval was obtained as well as informed consent from case group patients.
The control group was made up of 25 consecutive patients over 18 years of age who benefited from a magnetic elbow exploration and who had no injured DBT: retroolecranal infectious bursitis, lateral epicondylitis, rupture of the triceps tendon, ulnar tunnel syndrome, foreign body in soft tissues, capillary-venous angioma or intraosseous synovial cyst. Exclusion criteria were pathology involving the biceps muscle or its immediate environment and examinations where MRI was incomplete (no axial or sagittal images) or of insufficient quality. The control group was needed to allow quantitative comparison between safe and repaired DBT. Informed consent was waived for patients from the control group.
Patient follow-up
-
1.
Every patient from the case group was clinically followed up by the same orthopedic referent surgeon for at least 6 months after surgery. Besides the detection of a possible delayed postoperative complication, this allowed the assessment of two objective parameters:
-
the active elbow range of motion in flexion, extension, supination and pronation, expressed as a deficit in degrees to normal ranges of motion for age [26];
-
the maximum isometric elbow flexion strength (MEFS), expressed as a percentage of the contralateral side. MEFS was registered using a hand-held dynamometer. The arm was immobilized to prevent shoulder movement, and the elbow was flexed to 90° and fully supinated against the resistance of a fixed horizontal plane. The peak force during isometric flexion was measured three times to calculate a mean for each arm and deduce the ratio. MEFS was considered satisfactory when equal to 100 % for the dominant arm or equal to 88 % for the nondominant arm.
-
2.
Three-Tesla MRI (3-Tesla Signa Excite, GE Medical Systems, Milwaukee, WI, USA) was performed during the month of clinical follow-up and on average 22 (range: 6–55) months after surgery. Patients were placed in the prone position, their arm in complete anteversion and supination, and the elbow centered in a general-purpose multichannel receive-only flex coil. Thus, the DBT was placed in the same sagittal section as its insertion on the radial tuberosity. The MRI protocol included sagittal T1-weighted (T1w) and fat-suppressed proton density-weighted (FS-PDw) images in the DBT plane (Fig. 1) and T1w or FS-PDw axial images positioned perpendicular to the DBT.
-
MRI interpretation was retrospectively performed on PACS stations (Kodak Carestream PACS System, Carestream Health, Rochester, NY, USA), by consensus reading between a senior radiologist specialized in musculoskeletal imaging and a junior radiologist.
In addition to seeking delayed postoperative complications (new rupture, secondary avulsion), intratendinous osteoma and analyzing tendinous signals on T1w and FS-PDw images, the following were examined (Fig. 2, 3, 4 and 5):
-
extramuscular length of the tendon (expressed in mm);
-
anteroposterior/transverse diameters and cross-sectional area of the DBT at the radial head (expressed in mm);
-
anteroposterior/transverse diameters and cross-sectional area of the DBT at its distal insertion on the radial tuberosity (expressed in mm2).
The anteroposterior diameters were measured on the sagittal images so as to avoid overestimation on strict axial images.
-
3.
A plain radiograph of the reinserted DBT was systematically performed the day of the MRI to detect the presence of an intratendinous osteoma and to study the sensitivity of postoperative MRI in detecting it.
Statistical analyses
Statistical analysis was performed using Systat 12 Software (Systat Software v12, Chicago, IL, USA). Continuous variables were expressed as the mean, standard deviation (SD) and 95 % confidence interval (CI). An overall p-value or less than 0.05 was considered statistically significant. We performed linear regressions to search for a statistical correlation between the DBT measurements and the following variables: postoperative time of assessment, supination range of motion, MEFS of the dominant arm, MEFS of the nondominant arm and the extramuscular length of the DBT.
When this correlation was significant, we used a Mann-Whitney U test to determine whether there was a significant difference between the case and control group.
Results
Population
Included patients were only males from 36 to 60 years of age (mean age: 49 ± 4.9). All were active at the time of rupture, and 68 % were manual workers (n = 17). The trauma was reported as a workplace accident in 52 % of cases (n = 13). The dominant arm was injured in 56 % of cases (n = 14). The injury was caused by a lifting force (n = 8), a forced extension (n = 8), a flexion against resistance (n = 7) or occurred spontaneously (n = 2). The average time interval between the injury and surgery was 9 days (range: 0–50). Every patient had an anterior single incision surgery with two metallic suture anchors. No endobuttons were used.
In the control group, the mean patient age was 48 ± 10 years, comparable to that of the study group.
Clinical evaluation
The active ranges of motion in flexion and extension were respectively normal in 92 % (n = 23/25) and 96 % (n = 24/25) of patients. Two patients had a flexural deficit <10° and one patient had an extension deficit <5°. The range of motion in supination was normal in 72 % of cases (n = 18/25), but six patients had a supination deficit <20° and one patient <10°.
The mean postoperative MEFS was 91 (CI 66–121) %:
-
when the dominant arm was involved, the mean MEFS was 92 (CI 66–121) %;
-
when the nondominant arm was involved, the mean MEFS was 87 (CI 66–105) %.
Immediate minor postoperative complications involved about 40 % of patients (n = 10) and were mainly peripheral neurological disorders:
-
paresthesia in the territory of the lateral cutaneous nerve of the forearm (n = 4);
-
paresthesia in the radial nerve territory (n = 3);
-
reflex sympathetic dystrophy syndrome (n = 2);
-
radial nerve paresis (n = 1).
They all regressed spontaneously or under correct symptomatic treatment.
Qualitative MRI evaluation
All reinserted DBTs appeared heterogeneous but kept the characteristic fibrillar rearrangements (Fig. 6). In 24 % of cases (n = 6), the repaired DBT had multinodular rearrangements associated with metal artifacts (Fig. 7).
The caliber of the myotendinous junction was similar to the opposite side, while the DBT gradually widened and had a flared appearance at its distal insertion.
The normal intratendinous homogeneous low signal was altered. On T1w images, the low signal was less pronounced than that of normal tendons. On FS-PDw images, the signal was more variable, mostly similar to that observed on T1w images, but sometimes in mild high signal (Fig. 8). One asymptomatic patient presented a strong intratendinous high signal on FS-PDw images (Fig. 9). This rearrangement was all the more unusual since in this case the ranges of motion and MEFS were preserved.
Osteomas corresponded to the intratendinous foci of ossification seen in 13 patients on plain radiographs. Of these 13 cases, 7 were detected on T1w images and appeared as high signal intratendinous foci, surrounded by a low signal border (Fig. 10). In all cases of osteoma, the MEFS was conserved.
MRI made it possible to diagnose two delayed complications:
-
one textiloma, confirmed on plain radiographs, which showed the metal surgical equipment within the soft tissues (Fig. 11). On MRI, it appeared as multiple concentric rings of variable signals within an oblong mass syndrome facing the deep portion of the DBT. The patient was asymptomatic and there was no functional deficit.
-
one secondary disinsertion of the DBT in a patient whose MEFS was unsatisfactory at 88 %. The suture anchor was identified at a distance from the radial tuberosity (Fig. 12).
Secondary disinsertion of the DBT: The myotendinous junction is not seen on the upper axial section (a). The tendon is retracted and is seen on the highest axial section (1) and medially displaced via the safe lacertus fibrosus (black arrowheads) (b). No tendon was seen on the radial tuberosity in axial section (c) or sagittal section (d). Suture anchor holes were seen on the sagittal section (white arrows)
Quantitative MRI results
In the control group, tendon measurements (extramuscular length, cross-sectional area at the distal insertion of the DBT and cross-sectional area at the radial tuberosity) were not significantly correlated with age (R2 = 0.068, 0.047 and 0.039, respectively). This allowed us to compare the groups even independently from the mean ages. Operated DBTs were significantly longer and thicker and had a larger insertion area than normal DBTs (Table 1).
In the case group, multivariable linear regressions identified a statistically significant relationship between the tendon measurements and the MEFS, whether for the dominant (R2 = 0.38) or the nondominant (R2 = 0.54) arm. The Mann-Whitney U test indicated that the correlation concerned more specifically the cross-sectional area at the distal insertion, anteroposterior diameter, transverse diameter and cross-sectional area at the radial tuberosity (Table 2). Further analysis was done in subgroups with satisfactory MEFS and also in those with an unsatisfactory MEFS (Fig. 13). There was a statistically significant difference between these two subgroups regarding the anteroposterior diameter (p = 0.01), transverse diameter (p = 0.003) and cross-sectional area at the distal insertion (p = 0.046). These measures were significantly higher in patients with a satisfactory MEFS. On the other hand, there was no significant correlation between the extramuscular length of the DBT and MEFS (p = 0.934).
Discussion
Except for a case reported by Sötje in 1993 [27] and a retrospective study by Schmidt in 2012 [22], ours is the first study describing the 3-T MRI appearance of the repaired DBT. The analysis is both qualitative, defining MRI aspects, including atypia, and quantitative, with precise measurements of the DBT. Our results are in agreement with the studies respectively conducted by Roger and Mafulli on the calcaneal tendon and the patellar tendon, which described an increased tendon caliber and signal alterations after reconstructive surgery [28, 29].
This is the first study showing the existence of a statistical correlation between the measurements of the repaired DBT and functional outcomes: larger cross-sectional areas at the radial tuberosity and at the distal insertion resulted in a better postoperative MEFS. The healthy DBT is thinner and has a much more limited insertion than the repaired one. This suggests that a satisfactory healing process occurs through a tendinous thickening and enlargement of the insertion area. By comparing the MRI signal of the repaired tendon (low signal on T1w images and variable signal on FS-PDw images) to histological studies [30], this thickening seems to be primarily of a fibrous nature. Given patients’ improved functional outcomes, the neoformation of tendon fibers is most likely to be associated with those patients who have thicker tendons. However, DBT measurements, especially the cross-sectional area at its distal insertion, should be interpreted with caution, taking into consideration surgical techniques that would be different from those performed in our institution.
Metallic anchors artifacted the very close area of the radial insertion, but measurements of the insertion itself were always possible because this zone was enlarged and we used spin-echo MR sequences.
The case of strong intratendinous high signal on FS-PDw images (Fig. 9) was seen 14 months after the operation. It has to be considered as pathological, as suggested by Fantino, who described postoperative intratendinous signal abnormalities of the calcaneal tendon occupying more than 50 % of its cross-sectional area [31]. We diagnosed tendinosis, a term commonly used in tendon pathology, as opposed to tendinitis, which refers to the transient state of early inflammation. The absence of functional deficit in this case shows the lack of correlation between an intratendinous signal alteration, detected long after surgery, and clinical outcome. This did not allow us in this case to determine whether the tendinosis was the cause or the consequence of the rupture.
We identified the presence of osteoma on 3-T MRI, with a sensitivity of 53 % as compared to plain radiographs. This rate is slightly higher than that of the literature data (0–50 %) and could be explained by the use of a 3-T magnetic field. Analysis of the osteoma signals (central high signal surrounded by a border of low signal on T1w images) reflects a genuine intratendinous ossification, consisting of a central medulla (fatty signal) surrounded by cortical bone. As is the case in the literature, we did not find any significant association between the presence of an osteoma and postoperative functional outcomes [18, 32–34].
In the absence of consensus regarding the evaluation of the functional outcome of the operated elbow [35], we chose to measure the MEFS, which is a simple, reproducible and discriminating way to assess the effectiveness of the treatment without using any specialized equipment. The thresholds between satisfactory and unsatisfactory MEFS were deduced from the work of Morrey and Askew [36, 37]. They found a physiological difference of 6 % in the MEFS between the two arms. Regarding the dominant arm, the normal MEFS ratio would be 106 % of the opposite side. On the contrary, the normal MEFS ratio for the nondominant arm would be 94 % of the opposite side. We arbitrarily set the 6 % deficit as a unsatisfactory postoperative MEFS so that cutoff for unsatisfactory postoperative MEFS was 100 % for the dominant arm (106–6 %). As a consequence, the threshold for the nondominant arm was 88 % (94–6 %). Nothing in the literature indicates which quantitative MEFS values should be considered satisfactory. Such a correction of dominance was challenged by Wittstein [38] although previously validated by Sotereanos [39]. The lack of evaluation of the isokinetic flexion strength of the elbow was not detrimental because different studies in this area are inconsistent and could not serve as a reference [20, 38, 40, 41].
One limitation of our study is the absence of measurement of the supination strength of the elbow. Unlike the flexion movement, which has compensatory mechanisms via the lacertus fibrosus, supination is profoundly altered in case of DBT rupture [19, 35, 42]. Despite a particularly pronounced difference in the preoperative deficit, the literature review shows a relatively similar recovery of the MEFS and the supination strength after anatomical reinsertion of the DBT. Thus, the MEFS appears then to be as good as the supination strength in the postoperative evaluation of the repaired DBT [18, 33–35, 42–44].
Although patient height would have been a relevant parameter, it was not specifically studied in our series. Another limitation was the absence of evaluation of other muscles of the elbow that interact with the biceps brachii (brachialis muscle, brachioradialis muscle).
The MRI examinations lasted on average 15 min. Patient cooperation was essential to align the DBT and radial tuberosity on the same sagittal section. The correlation between the tendon measurements and the functional outcome was detected using a strict methodology, emphasizing on the use of sagittal section to estimate the anteroposterior diameter (avoiding the strict axial section that would overestimate measurement).
We only used 2D MRI sequences because during the period of the study 3D acquisitions were not available. These recent sequences should be evaluated in further studies in order to determine whether or not they are able to improve measurement precision. However, 3D acquisitions may not be relevant for a proper evaluation of the DBT because:
-
the DBT is a small structure and we needed a good signal-to-noise ratio, which is better in traditional 2D sequences;
-
the 3D gradient echo sequences are very sensitive to metal artifacts.
The discovery of delayed complications confirmed the interest of postoperative radiological follow-up. Unlike the secondary avulsion of the DBT, which we had suspected because of a sudden drop in MEFS, textiloma was not clinically expected because it was asymptomatic. The secondary rupture involved a patient who was operated on later in our series, 55 months after the rupture. Tendon retraction was probably more pronounced with an exaggerated traction force due to the suture anchor system. Conservative rehabilitation should probably have been preferred in this case [45].
Conclusion
Obtaining a better MEFS after anatomical reinsertion of a ruptured DBT depends on increased cross-sectional areas of the DBT at the radial tuberosity and at its distal insertion. Therefore, the tendon-healing process occurs when new functional tendon fibers are formed, associated with the production of fibrous scar tissue. Furthermore, intratendinous postoperative signal alterations and the occurrence of osteomas are not correlated with the functional outcome.
References
Safran MR, Graham SM. Distal biceps tendon ruptures: incidence, demographics, and the effect of smoking. Clin Orthop Rel Res. 2002(404):275-283
Morrey BF. Injury of the flexors of the elbow: biceps tendon injury. The elbow and its disorders. 4th ed. Philadelphia: Saunders; 2008:518-535.
Mazzocca AD, Spang JT, Arciero RA. Distal biceps rupture. Orthop Clin N Am. 2008;39(2):237–49. vii.
Vidal AF, Drakos MC, Allen AA. Biceps tendon and triceps tendon injuries. Clin Sports Med. 2004;23(4):707–22.
Schneider A, Bennett JM, O’Connor DP, Mehlhoff T, Bennett JB, Savvidou C. Bilateral ruptures of the distal biceps brachii tendon Spontaneous distal biceps tendon ruptures: are they related to statin administration. J Should Elb Surg Am Should Elb Surg. 2009;18(5):804–7.
Savvidou C, Moreno R. Spontaneous distal biceps tendon ruptures: are they related to statin administration? Hand surgery: An international journal devoted to hand and upper limb surgery and related research. J Asia Pac Fed Soc Surg Hand. 2012;17(2):167–71.
Rineer CA, Ruch DS. Elbow tendinopathy and tendon ruptures: epicondylitis, biceps and triceps ruptures. J Hand Surg. 2009;34(3):566–76.
Bernstein AD, Breslow MJ, Jazrawi LM. Distal biceps tendon ruptures: a historical perspective and current concepts. Am J Orthop (Belle Mead NJ). 2001;30(3):193–200.
Chillemi C, Marinelli M, De Cupis V. Rupture of the distal biceps brachii tendon: Conservative treatment versus anatomic reinsertion—clinical and radiological evaluation after 2 years. Arch Orthop Trauma Surg. 2007;8:705–8.
Baker BE, Bierwagen D. Rupture of the distal tendon of the biceps brachii. Operative versus non-operative treatment. J Bone Joint Surg Am. 1985;67(3):414–7.
Geaney LE, Mazzocca AD. Biceps brachii tendon ruptures: a review of diagnosis and treatment of proximal and distal biceps tendon ruptures. Physician Sports Med. 2010;38(2):117–25.
Catonne Y, Delattre O, Pascal-Mousselard H, d’Istria FC, Busson J, Rouvillain JL. Rupture of the distal tendon of the biceps brachialis: apropos of 43 cases. Rev Chir Orthop Reparatrice Appar Mot. 1995;81(2):163–72.
Boyd HB, Anderson LD. A method for reinsertion of the distal biceps brachii tendon. J Bone Joint Surg Am. 1961;43(7):1041–3.
Lintner S, Fischer T. Repair of the distal biceps tendon using suture anchors and an anterior approach. Clin Orthop Relat Res. 1996;322:116–9.
Barnes SJ, Coleman SG, Gilpin D. Repair of avulsed insertion of biceps. A new technique in four cases. J Bone Joint Surg Br. 1993;75(6):938–9.
Bain GI, Prem H, Heptinstall RJ, Verhellen R, Paix D. Repair of distal biceps tendon rupture: A new technique using the Endobutton. J Should Elb Surg Am Should Elb Surg. 2000;9(2):120–6.
Morrey BF, Askew LJ, An KN, Dobyns JH. Rupture of the distal tendon of the biceps brachii. A biomechanical study. J Bone Joint Surg Am. 1985;67(3):418–21.
Bell RH, Wiley WB, Noble JS, Kuczynski DJ. Repair of distal biceps brachii tendon ruptures. J Should Elb Surg Am Should Elb Surg. 2000;9(3):223–6.
Nesterenko S, Domire ZJ, Morrey BF, Sanchez-Sotelo J. Elbow strength and endurance in patients with a ruptured distal biceps tendon. J Should Elb Surg Am Should Elb Surg. 2010;19(2):184–9.
Balabaud L, Ruiz C, Nonnenmacher J, Seynaeve P, Kehr P, Rapp E. Repair of distal biceps tendon ruptures using a suture anchor and an anterior approach Repair of distal biceps tendon ruptures in athletes. J Hand Surg (Edinb Scotl). 2004;29(2):178–82.
Cain RA, Nydick JA, Stein MI, Williams BD, Polikandriotis JA, Hess AV. Complications following distal biceps repair. J Hand Surg. 2012;37(10):2112–7.
Schmidt CC, Diaz VA, Weir DM, Latona CR, Miller MC. Repaired distal biceps magnetic resonance imaging anatomy compared with outcome. J Should Elb Surg Am Should Elb Surg. 2012;21(12):1623–31.
Marnitz T, Spiegel D, Hug K, Huper M, Gerhardt C, Steffen IG. MR imaging findings in flexed abducted supinated (FABS) position and clinical presentation following refixation of distal biceps tendon rupture using bioabsorbable suture anchors. RoFo: Fortschr auf dem Geb Rontgenstrahlen und Nuklearmedizin. 2012;184(5):432–6.
Ramnath RR. 3T MR imaging of the musculoskeletal system (Part I): Considerations, coils, and challenges. Mag Reson Imaging Clin N Am. 2006;14(1):27–40.
Brasseur JL. The biceps tendons: From the top and from the bottom. J Ultrasound. 2012;15(1):29–38.
Soucie JM, Wang C, Forsyth A, Funk S, Denny M, Roach KE. Range of motion measurements: Reference values and a database for comparison studies. Haemophilia. Off J World Fed Hemophilia. 2011;17(3):500–7.
Sotje G, Besch L. Distal rupture of the biceps tendon—a magnetic resonance tomography follow-up. Aktuelle Traumatol. 1993;23(2):105–7.
Roger B, Saillant G. Imagerie par résonance magnétique du tendon patellaire opéré Getroa Opus XXX: Sauramps Medical; 2003:389-394.
Maffulli N, Thorpe AP, Smith EW. Magnetic resonance imaging after operative repair of Achilles tendon rupture. Scand J Med Sci Sports. 2001;11(3):156.
Khan KM, Cook JL, Bonar F, Harcourt P, Astrom M. istopathology of common tendinopathies. Update and implications for clinical management. Sports Med (Auckland NZ). 1999;27(6):393–408.
Fantino O, Besse J, Moyen B, Tran Minh V. Imagerie du tendon calcanéen opéré: Echographie et IRM. Getroa Opus XXX: Sauramps Medical; 2003. p. 395–408.
Greenberg JA, Fernandez JJ, Wang T, Turner C. EndoButton-assisted repair of distal biceps tendon ruptures. J Should Elb Surg Am Should Elb Surg. 2003;12(5):484–90.
Klonz A, Loitz D, Wohler P, Reilmann H. Rupture of the distal biceps brachii tendon: isokinetic power analysis and complications after anatomic reinsertion compared with fixation to the brachialis muscle. J Should Elb Surg Am Should Elb Surg. 2003;12(6):607–11.
Behounek J, Hrubina M, Skotak M, Krumpl O, Zahalka M, Dvorak J. Evaluation of surgical repair of distal biceps tendon ruptures. Acta Chir Orthop Traumatol Cechoslovaca. 2009;76(1):47–53.
Freeman CR, McCormick KR, Mahoney D, Baratz M, Lubahn JD, Nesterenko S. Nonoperative treatment of distal biceps tendon ruptures compared with a historical control group. Elbow strength and endurance in patients with a ruptured distal biceps tendon. J Bone Joint Surg Am. 2009;91(10):2329–34.
Morrey BF, Chao EY, Hui FC. Biomechanical study of the elbow following excision of the radial head. J Bone Joint Surg Am. 1979;61(1):63–8.
Askew LJ, An KN, Morrey BF, Chao EY, Morrey BF, Chao EY. Isometric elbow strength in normal individuals. Biomechanical study of the elbow following excision of the radial head. Clin Orthop Relat Res. 1987;61(222):261–6.
Wittstein J, Queen R, Abbey A, Moorman CT. 3rd. Isokinetic testing of biceps strength and endurance in dominant versus nondominant upper extremities. J Should Elb Surg Am Should Elb eons. 2010;19(6):874–7.
Sotereanos DG, Pierce TD, Varitimidis SE. A simplified method for repair of distal biceps tendon ruptures. J Should Elb Surg Am Should Elb Surg. 2000;9(3):227–33.
Leighton MM, Bush-Joseph CA, Bach Jr BR, Wittstein J, Queen R, Abbey A. Distal biceps brachii repair. Results in dominant and nondominant extremities Isokinetic testing of biceps strength and endurance in dominant versus nondominant upper extremities. Clin Orthop Relat Res. 1995;19(317):114–21.
D’Alessandro DF, Shields Jr CL, Tibone JE, Chandler RW, Wittstein J, Queen R. Repair of distal biceps tendon ruptures in athletes Isokinetic testing of biceps strength and endurance in dominant versus nondominant upper extremities. Am J Sports Med. 1993;21(1):114–9.
Hetsroni I, Pilz-Burstein R, Nyska M, Back Z, Barchilon V, Mann G. Avulsion of the distal biceps brachii tendon in middle-aged population: is surgical repair advisable? A comparative study of 22 patients treated with either nonoperative management or early anatomical repair. Injury. 2008;39(7):753–60.
Silva J, Eskander MS, Lareau C, DeAngelis NA. Treatment of distal biceps tendon ruptures using a single-incision technique and a Bio-Tenodesis screw. edics. 2010;33(7):477.
Frazier MS, Boardman MJ, Westland M, Imbriglia JE. Surgical treatment of partial distal biceps tendon ruptures. J Hand ery. 2010;35(7):1111–4.
Berlet GC, Johnson JA, Milne AD, Patterson SD, King GJ. Distal biceps brachii tendon repair. An in vitro biomechanical study of tendon reattachment. Am J Sports Med. 1998;26(3):428–32.
Author disclosure statement
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Alemann, G., Dietsch, E., Gallinet, D. et al. Repair of distal biceps brachii tendon assessed with 3-T magnetic resonance imaging and correlation with functional outcome. Skeletal Radiol 44, 629–639 (2015). https://doi.org/10.1007/s00256-014-2079-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-014-2079-z