Abstract
Ulcerative colitis (UC), a kind of inflammatory bowel disease, is generally characterized by chronic, persistent, relapsing, and nonspecific ulceration of the bowel, which is widespread in the world. Although the pathogenesis of UC is multifactorial, growing evidence has demonstrated that gut microbiota and its metabolites are closely related to the development of UC. Lizhong decoction (LZD), a well-known classical Chinese herbal prescription, has been used to clinically treat UC for long time, but its mechanism is not clear. In this study, 16S rRNA gene sequencing combining with untargeted metabolomics profiling was used to investigate how LZD worked. Results indicated that LZD could shape the gut microbiota structure and modify metabolic profiles. The abundance of opportunistic pathogens such as Clostridium sensu stricto 1, Enterobacter, and Escherichia-Shigella correlated with intestinal inflammation markedly decreased, while the levels of beneficial bacteria including Blautia, Muribaculaceae_norank, Prevotellaceae UCG-001, and Ruminiclostridium 9 elevated in various degrees. Additionally, fecal metabolite profiles reflecting microbial activities showed that adenosine, lysoPC(18:0), glycocholic acid, and deoxycholic acid notably decreased, while cholic acid, α-linolenic acid, stearidonic acid, and l-tryptophan significantly increased after LZD treatment. Hence, based on the systematic analysis of 16S rRNA gene sequencing and metabolomics of gut flora, the results provided a novel insight that microbiota and its metabolites might be potential targets for revealing the mechanism of LZD on amelioration of UC.
Key Points
• The potential mechanism of LZD on the amelioration of UC was firstly investigated.
• LZD could significantly shape the structure of gut microbiota.
• LZD could notably modulate the fecal metabolic profiling of UC mice.

Graphical abstract
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ulcerative colitis (UC) is a type of inflammatory intestinal disease, which can result in abdominal pain, chronic diarrhea, bloody stool, and weight loss (Adams and Bornemann 2013). It is characterized by chronic, persistent, recurrent, and nonspecific intestinal ulcer, starting in the rectum and extending to proximal segments of the colon continuously (Ungaro et al. 2017). UC is a common clinical digestive system disease, which is more common in young and middle-aged people aged 17–40 years (Li et al. 2017). Collectively, the serious complications of UC, such as thrombosis, perforation, toxic megacolon, and colorectal cancer, greatly affect patients’ normal life (Marineaţă et al. 2017; Kume et al. 2014; Bianchi et al. 2018; Yuza et al. 2018). Studies have reported that prevalence of UC is higher in developed Western countries like North America and Europe (Ng et al. 2018; Magro et al. 2017). Also, the incidence and prevalence of UC are rising worldwide at the turn of the twenty-first century. With the westernization of lifestyle and dietary changes in the structure, the morbidity of UC has been increasing in developing countries such as Asia, the Middle East, and South America (Ng et al. 2013; da Silva et al. 2014; Vegh et al. 2017). Thus, treatment of UC has drawn more extensive research interests in recent years.
Currently, aminosalicylates (5-ASA), steroids, immunosuppressants, and biologic therapies have been commonly applied to cure UC (Panés and Alfaro 2017). However, these therapeutically drugs are associated with serious side effects, including infection, allergic reaction, intolerance, toxic effects, and high disease recurrence rate (Troncone and Monteleone 2017). Therefore, it is urgent that novel drugs are needed to be explored for the therapy of UC. Inspiringly, traditional Chinese medicines (TCMs), owing to their obvious curative efficacy and few side effects, have been recognized as the important drugs to clinically treat chronic diseases such as UC (Zhang et al. 2013). Lizhong decoction (LZD), which is derived from Zhang Zhongjing’s Treatise on Exogenous Febrile Diseases, is a well-known classical prescription used in treating UC for thousands of years. It is composed of four ingredients: Zingiber officinale Rosc. (Zingiberis Rhizoma), Panax ginseng C. A. Mey. (Ginseng Radix Rhizoma), Atractylodes macrocephala Koidz. (Atractylodis Macrocephalae), and Glycyrrhiza uralensis Fisch. (Glycyrrhizae Radix Et Rhizoma) (Shen et al. 2019). Modern chemical, pharmacological, and clinical studies have illustrated that the four herbs contained many bioactive compounds which showed anti-inflammatory and antioxidant activities. The major compounds in Zingiberis Rhizoma were a series of homologous phenolic ketones known as gingerols, which could inhibit inflammation via negatively affecting macrophage and neutrophils activation as well as monocyte and leukocyte migration (Ezzat et al. 2018). Ginsenosides, the major ingredients in Ginseng Radix Rhizoma, had the capability to block the transcriptional activity of tumor necrosis factor-α-mediated NF-κB (Ma et al. 2017; Lam et al. 2016). It has been reported that Atractylodis Macrocephalae, mainly containing atractylone, orange linoleum, elemene, and isoeugenol, played an important role in modulating the function of the gastrointestinal tract and was commonly used to cure digestive tract diseases (Gu et al. 2019). Glycyrrhizae Radix Et Rhizoma with the major components including glycyrrhetic acid, β-sitosterol, flavonoids, and hydroxycoumarins could inhibit the inflammatory response by regulating the MAPK pathway and pro-inflammatory interleukins (Thiyagarajan et al. 2011). Furthermore, our previous study also indicated that LZD could markedly improve the pathological symptoms of UC, while its mechanism was not clear.
Recently, accumulating evidence has verified that the gastrointestinal tract is colonized by different microbial organisms, including bacteria, viruses, and fungi, which are referred to as the gut microbiota, with more than 1000 microbial species (Basso et al. 2019). Not surprisingly, gut microbiota and its metabolites played key roles in modulating some biological functions of the host, relating to the nutrient processing, host defense, maintenance of energy homeostasis, and development of the immunologic system (Nicholson et al. 2012; Gonçalves et al. 2018). Deviation in the composition of gut flora was involved in UC patients when compared with healthy subjects (Garg et al. 2018). Studies have reported that bacteria with anti-inflammatory capacities decreased while ones related to pro-inflammation increased in UC. And some common changes of gut microbiota were observed, including a decrease of Firmicutes and an increase in Proteobacteria and Bacteroidetes (Nishida et al. 2018). Besides, metabolites produced by gut microbiota also have special responsibility for the integrity of intestinal barrier function. Gut microbiota could ferment indigestible carbohydrates to yield some important metabolites such as short-chain fatty acids (SCFAs) and vitamins that were beneficial for the host (Zhang et al. 2017). Furthermore, phenolic compounds, branched-chain fatty acids, and amine substances were produced under the degradation of proteins, which could reflect the homeostasis of the intestinal tract (Canfora et al. 2019). Hence, many investigators have recognized that the interconnection between gut microbiota and host was complex and gut microbiota could be the possible therapeutic targets of UC (Skelly et al. 2019). However, the mechanism of LZD on the amelioration of UC via modifying gut microbiota structure and its metabolites has not been reported.
In this study, UC mice were successfully induced by dextran sulfate sodium (DSS). The change of gut microbiota composition in UC mice was firstly investigated by using 16S rRNA gene sequencing after LZD treatment. Then, an untargeted metabolomics was applied to analyze the metabolite profiles derived from gut microbiota. Thus, these results provided a new perspective for further understanding the mechanism of LZD in treating UC and the scientific basis for its clinical application.
Materials and methods
Chemicals and reagents
DSS was bought from MP Biomedicals (Santa Ana, CA, USA). Acetonitrile (HPLC grade) was supplied by TEDIA (Fairfield, OH, USA). Formic acid and methanol were obtained from Merck (Darmstadt, Germany). Ginseng Radix Rhizoma (voucher specimens NO.180901) was purchased from Anhui Huilong Medicinal Herbs Factory Co., Ltd. (Anhui, China) and quality was controlled. Zingiberis Rhizoma (voucher specimens no. 180821), Atractylodis Macrocephalae (voucher specimens no. 180904), and Glycyrrhizae Radix Et Rhizoma (voucher specimens no. 180815) were all purchased from Bozhou Yonggang Medicinal Herbs Factory Co., Ltd. (Bozhou, China) and quality was controlled.
Preparation of LZD extracts
Ginseng Radix Rhizoma, Zingiberis Rhizoma, Atractylodis Macrocephalae, and Glycyrrhizae Radix Et Rhizoma were mixed at a ratio of 1:1:1:1 and soaked with distilled water (1:6, w/v) for 20 min. The mixture was decocted for 30 min. Then, the filtrate was collected through gauze while the residue was decocted in water (1:4, w/v) for 20 min. Finally, the two filtrates were merged and concentrated to 1.0 g/mL at 60 °C. HPLC chromatogram of LZD extracts was listed in Supplementary Text S1 and Supplemental Fig. S1.
Animals
Male C57BL/6 mice (18–22 g) were purchased from Vital River Laboratory Animal Technology Co., Ltd. (Beijing, China) and maintained in a clean room at 23 ± 2 °C with 55 ± 10% relative humidity, keeping a 12-h light/dark cycle. All animals were handled in accordance with experimental protocols outlined by Guide for the Care and Use of Laboratory Animals (US National Research Council, 1996) and approved by the Research Ethical Committee of Nanjing University of Chinese Medicine (Nanjing, China).
Induction of UC and animal grouping
Colitis model in mice was induced by DSS, which was prepared into 2% and 2.5% (w/w) DSS aqueous solution. UC was induced by administrating mice with 2% DSS aqueous solution in the first 3 days and then 2.5% DSS aqueous solution in the following 4 days instead of drinking water.
All mice were raised according to the specific pathogen free (SPF) standard, acclimatizing to the laboratory environment for 1 week. Thereafter, mice in the normal group (normal, N) were received normal drinking water all the time and the other mice were received DSS aqueous solution for 7 days to obtain colitis. Experimental mice with UC were randomly divided into different groups: model group (DSS, M); LZD low-, middle-, and high-dose treatment group (LL, LM, LH), receiving LZD 1.365 g/kg (DSS + LL), 4.095 g/kg (DSS + LM), and 12.285 g/kg (DSS + LH), respectively. Mice were treated for 14 days by gastric gavage once daily. Normal and model mice were received the same dose of normal saline.
Sample collection and preparation
Fresh stool samples were collected into frozen pipes after the treatment on the 14th day. All the mice were sacrificed and colon samples were taken immediately after anatomy. All the biological samples had been preserved at − 80 °C until the assays were performed.
DNA extraction, polymerase chain reaction amplification, sequencing, and data analysis
Total bacterial DNA was extracted from fresh stool samples by the E.Z.N.A.® Soil DNA Kit (Omega Bio-tek, Norcross, GA, USA). The DNA in stools was quantified through agarose gel electrophoresis. The extracted DNA from each sample was used as template to amplify V3–V4 variable regions of the 16S ribosomal RNA gene with specific primers (341F: 5′-CCTAYGGGRBGCASCAG-3′; 806R: 5′-GGACTACNNGGGTATCTAAT-3′). Specific operational procedures were carried out referring to the previously described method (Wei et al. 2018a). The details were listed in Supplementary materials (Text S2).
Metabolic profiling using UPLC-Q-TOF/MS
Fecal samples were pretreated with methanol and analyzed by using UPLC-Q-TOF/MS. EZinfo 2.0 software (Zhu et al. 2018) was used to obtain principal component analysis (PCA), supervised partial least squares discrimination analysis (PLS-DA), and orthogonal partial least squares discriminant analysis (OPLS-DA) via analyzing each ion. The differential metabolites were selected while meeting the requirements of variable importance in the projection (VIP ˃ 1) and statistically significant difference (P < 0.05). Specific operational procedures were carried out according to the previously described method (Wei et al. 2018b). The details are listed in Supplementary materials (Text S3).
Statistical analysis
All data were analyzed by the analysis of variance (ANOVA). The results were expressed as the mean ± standard deviation (mean ± SD). Statistical comparisons were considered to be statistically significant if P values were less than 0.05 (P < 0.05) by using the SPSS 19.0 software (IBM, Armonk, USA).
Nucleotide sequence accession number
The 16S rRNA sequences obtained in this study were deposited into the NCBI Sequence Read Archive (SRA) database with accession number PRJNA602801.
Results
Amelioration of LZD on DSS-induced colitis
In this study, a UC mouse model was successfully induced by DSS. Pathological symptoms of UC mice were notably ameliorated after LZD treatment, as shown by increased body weight, markedly prolonged colon length, and improved colon lesions of UC mice, as well as significantly decreased DAI and histological scores. The details are listed in Supplementary materials (Text S4, Table S1, and Fig. S2).
Intervention of LZD on gut microbiota in UC mice
16S rRNA phylogenetic approach by sequencing V3–V4 regions was used to investigate the changes in gut microbiota populations of the control, DSS-treated, and LZD-administrated mice. A total of 1,112,941 qualified sequences were generated from 25 samples with an average of 44,518 ± 9540 reads per sample, representing a total of 8969 operational taxonomic units (OTUs). According to the tendency of individual Rarefaction curves and Shannon-Wiener curves (Fig. 1a, b), it was revealed that sequencing data were reasonable and could reflect microbial information in all samples
The community richness and diversity among different groups. a Rarefaction curves in different groups. b Shannon Wiener curves of samples. c, d The Chao1 and Shannon index in different groups were used to estimate the richness and diversity of the gut microbiota. ###P < 0.001 vs normal group; *P < 0.05 vs model group
The alpha diversity indices, including Chao 1 index and Shannon index, are usually used for evaluating the community richness and community diversity. In this study, DSS-induced mice significantly reduced the Chao 1 index (P < 0.05) when compared with the normal group, suggesting less microbial community richness, while LL, LM, and LH groups showed increased abundance. Besides, the level of Shannon index was lower in the M group (P < 0.05) which indicated the fewer diverse microbial communities. In contrast, the microbial diversity in DSS-treated mice was increased after LZD treatment (Fig. 1c, d). Briefly, compared with the DSS-treated group, LZD treatment could notably reverse the reduced abundance of intestinal flora but had little influence on the community diversity. Additionally, PCA and principal coordinate analysis (PCoA) of Bray-Curtis distance matrices were used to evaluate the variance of diversity among different groups. As shown in Fig. 2, evident separation of gut microbiota was observed on the two-dimensional PCA and PCoA plots among different groups. Moreover, compared with DSS-treated mice, different dose groups of LZD showed high similarities in bacterial members with the normal group, which indicated that amelioration of LZD on UC might be due to its modulation on the structure of gut microbiota destroyed by DSS.
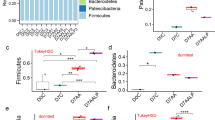
Additionally, the most abundant phyla, which included Bacteroidetes, Firmicutes, Proteobacteria, Verrucomicrobia, Actinobacteria, and Deferribacteres, were detected in the fecal microbiota through 16S rRNA sequencing analysis, and details are displayed in Fig. 3a. Bacteroidetes was the most abundant phyla in all samples. Compared with the normal group, the relative abundance of Proteobacteria in the model group significantly increased, while Bacteroidetes markedly decreased. After the oral administration of LZD, this change was remarkably reversed. Results showed that the relative abundance of Bacteroidetes in the different LZD groups was significantly higher than that in the normal and model groups, and a reduction in the ratio of Firmicutes to Bacteroidetes was observed after the therapy as well.
The structure of gut microbiota among different groups. a Microbial community barplotat phylum level of all samples. b Relative abundance of the main genera of the intestinal microbiota in all samples. c Composition of microbiota genera in normal, model, LL, LM, and LH groups. White up-pointing triangle indicates significant change of M vs N (###P < 0.001; ##P < 0.01); Asterisk symbol indicates significant change of different treatment groups vs M (**P < 0.01; *P < 0.05). N, normal group; M, UC group; LL, 1.365 g/kg LZD group; LM, 4.095 g/kg LZD group; LH, 12.285 g/kg LZD group
To identify the specific bacterial flora associated with colitis and LZD treatment, the linear discriminant analysis effect size (LEfSe) analysis was applied to compare the changing bacterial flora from phylum to genus in the different treated mice (Zhang et al. 2019). The composition of intestinal flora was significantly different among the groups, and more details are listed in Supplementary materials (Fig. S3). Results revealed that Bacteroidetes and Firmicutes were the most microbiota in the N group. Nevertheless, many opportunistic pathogens in the Proteobacteria phylum such as Proteobacteria, Gammaproteobacteria, and Escherichia_ Shigella were the main different bacteria in the M group. After LZD intervention, the relative abundance of opportunistic bacteria decreased, and main genera from Bacteroidetes and Firmicutes were restored in LL, LM, and LH groups.
The genus level distribution for five groups is illustrated in Fig. 3b. After comparing the relative abundance of the intestinal flora in N and M groups, 61 intestinal bacteria exhibited significant difference. The results are listed in Supplemental Table S2. Additionally, seven of them were markedly shifted after LZD intervention (Fig. 3c). Notably, gut microbiota such as Blautia, Muribaculaceae_norank, Prevotellaceae UCG-001, and Ruminiclostridium 9 decreased in the M group, and increased in LL, LM, and LH groups, while Clostridium sensu stricto 1, Enterobacter, and Escherichia-Shigella possessed the absolutely opposite alteration in the different treated groups. Above results showed that LZD had an effective influence on the treatment of UC by regulating the dysbiosis of intestinal flora.
Effects of LZD on fecal metabolic profiling of UC mice
A highly sensitive and specific analytical method, ultra performance liquid chromatography/quadrupole time-of-flight mass spectrometry (UPLC-Q-TOF/MS) with an automated data analysis system (Metabolynx™) (Leonart et al. 2017), was established and successfully applied to identify the metabolic profiling of feces samples collected from different mice in negative and positive ESI modes, respectively. Typical total ion chromatograms (TICs) are shown in Supplementary materials (Fig. S4). To evaluate differences among groups, PLS-DA technique was performed. As shown in Fig. 4a, the N group was significantly separated from the M group, suggesting that the metabolic profiles in DSS-induced mice were changed when compared with the normal group. Additionally, as shown in Fig. 4b, three dosages of LZD-treated groups were also significantly separated from the M group and were closer to the N group in the varied degree, suggesting LZD affected these metabolites. Besides, the OPLS-DA method was applied to maximize the class discrimination and determine potential metabolites. The variables analyzed by the OPLS-DA method were screened for potential biomarkers based on VIP values (VIP ˃ 1) and statistically significant difference (P < 0.05). Potential metabolites were preliminarily identified according to the HMDB database (https://www.hmdb.ca) and the KEGG database (https://www.kegg.jp). The metabolites are listed in Table 1. Compared with the N group, the notably increased metabolites in the M group included adenosine, glycocholic acid, lysoPC(18:0), cholic acid, and deoxycholic acid, along with the markedly decreased levels of α-linolenic acid, stearidonic acid, and l-tryptophan, and the trend of these biomarkers was significantly reversed after LZD treatment. Then, identified potential biomarkers related to UC were imported into the MetPA databases (https://www.metaboanalyst.ca) and the KEGG databases to establish the metabolic pathways, which included purine metabolism, primary bile acid biosynthesis, biosynthesis of unsaturated fatty acids, α-linolenic acid metabolism, secondary bile acid biosynthesis, tryptophan metabolism, and glycerophospholipid metabolism (Fig. 5). The above results indicated that LZD could regulate the disorder of metabolites and their related metabolic pathways which contributed to the development of colitis.
PCA scores plot and S-plots of OPLS-DA models resulting from UPLC/Q-TOF-MS spectra. a PCA scores plot between different groups. b The results of PCA score plots and S-plots of OPLS-DA models. N, normal group; M, UC group; LL, 1.365 g/kg LZD group; LM, 4.095 g/kg LZD group; LH, 12.285 g/kg LZD group. ESI+, positive ion mode; ESI−, negative ion mode
Correlation among gut microbiota, metabolites, and UC-related indexes
To better understand the functional correlation between gut microbiota alterations and metabolic changes, the Pearson correlation analysis was carried out between the altered microbiota and perturbed metabolites, which showed clear correlations eventually. As shown in Fig. 6a, Ruminiclostridium 9, Prevotellaceae UCG-001, Muribaculaceae_norank, and Blautia were positively correlated with α-linolenic acid, stearidonic acid, and cholic acid, which were obviously enriched in the N group, while Escherichia-Shigella, Enterobacter, and Clostridium sensu stricto 1 were dominant in the M group and positively correlated with adenosine and lysoPC(18:0). Besides, the correlation between altered microbiota and UC-related indexes (IL-1β, IL-6, IFN-γ, IL-8, TNF-α, IL-10, IL-4, marrow peroxidase (MPO), superoxide dismutase (SOD), nitric oxide (NO)) is shown in Fig. 6b and the details of UC-related indexes are listed in Supplementary materials (Text S4 and Fig. S5). At the genus level, Ruminiclostridium 9, Prevotellaceae UCG-001, Muribaculaceae_norank, and Blautia were positively correlated with IL-10, IL-4, and SOD as well as negatively related with IL-1, IL-6, IFN-γ, IL-8, and TNF-α. Nevertheless, Escherichia-Shigella, Enterobacter, and Clostridium sensu stricto 1 were absolutely opposite.
Discussion
UC is a chronic disease characterized by inflammatory gastrointestinal tract and longstanding colitis has a high risk associated with colon cancer (Sairenji et al. 2017; Han et al. 2017). The mechanisms that contribute to UC pathogenesis are multifactorial, and strong evidence shows that genetic predisposition, environmental factors, microbial dysbiosis, and immune responses dysregulation appear to be responsible for initiating UC (Cheon 2013; Shouval and Rufo 2017; Maloy and Powrie 2011; Rosen et al. 2017). Considering the critical roles of the gut microbiota in human health, in the present study, the experiment primarily focused on the dysregulation of gut microbiota combining with the alteration of metabolic profiles in vivo during UC progression to investigate the underlying mechanism of LZD on alleviation of UC.
A disruption in the composition and diversity of microbiota is closely associated with the gastrointestinal disease, following the pathogenic bacteria proliferating and enterotoxins secreting, thereby resulting in abnormal intestinal immunity. Therefore, the disorder of intestinal microflora is a known feature of UC. In this study, the 16S rRNA phylogenetic approach was used to reveal the changes in the composition of gut microbiota. Results showed a significant difference in microbial alpha diversity and beta diversity between the DSS-induced colitis and normal groups, indicating the number of microbiota in UC was less and the distribution of species was more uneven. Compared with the DSS model group, LZD treatment could increase the richness of the gut microbiota community based on a higher Chao1 index but had little significant difference on community diversity based on the Shannon index, suggesting the remission of richness and evenness of the gut microbiota community in DSS-induced colitis after LZD therapy. Interestingly, obvious differences existed between each group in PCA and PCoA analyses, with a shorter distance between the normal and LZD groups, indicating that experimentally induced colitis disrupted the overall structure of intestinal community and LZD partially mitigated it. According to previous researches, from the level at phylum, one of the features of the microbial dysbiosis in UC was the increase in the ratio of Firmicutes/Bacteroidetes (Peng et al. 2019). That shift in microbiota was also observed in our results and LZD changed the ratio trend to decline based on the decreased abundance in Firmicutes and increased abundance in Bacteroidetes. Furthermore, the relative abundance of Proteobacteria in the model group appeared an increasing state, indicating the pathogenic bacteria increased. Additionally, in the level at genus, Enterobacter, Escherichia-Shigella, and Clostridium sensu stricto 1 increased in the DSS-induced group, which was associated with intestinal inflammation (Chen et al. 2014). Enterobacter, belonged to the normal intestinal flora, is a kind of opportunistic pathogens that lives with the host in coexistence, which could initiate opportunistic infections when the host immunity system disorders occur or bacteria migrate outward the intestinal tract due to the increased intestinal permeability (Gaston 1988; Scarpellini et al. 2015). It has been reported that pathogenic bacteria such as Escherichia-Shigella were significantly elevated in UC, which was consistent with the variation in our study (Xu et al. 2018). Escherichia-Shigella that adhered to the mucosal epithelial cells of the colon was positively correlated with pro-inflammatory cytokines and promoted 7-alpha-dehydroxylation on primary bile acids to produce secondary bile acids, which in turn activated the P38 pathway, further leading to high expression of inflammatory cytokines to destroy the integrity of the intestinal barrier (Sasaki and Klapproth 2012; Autenrieth and Baumgart 2012; Jia et al. 2018). Besides, Clostridium sensu stricto 1 which was deemed to harmful bacteria also had adverse effects on the intestinal tract (Lin et al. 2018; Zhou et al. 2015). Hence, restoration of Enterobacter, Escherichia-Shigella, and Clostridium sensu stricto 1 contributed to the re-establishment of intestinal equilibrium after LZD treatment. In contrast, beneficial bacteria such as Blautia, Muribaculaceae_norank, Prevotellaceae UCG-001, and Ruminiclostridium 9 species, as the probable keystone taxa in UC, widely decreased in the DSS-induced group, while dramatically increased in the LZD therapy groups, demonstrating that LZD had therapeutic effects on UC through modulating the homeostasis of intestinal microbiota (Yilmaz et al. 2019; Schirmer et al. 2019; Lagkouvardos et al. 2019). Blautia could produce SCFAs, such as acetate, which could bind the G protein-coupled receptor 43 to affect the inflammatory responses, leading to the relief of intestinal inflammation (Durand et al. 2017; Maslowski et al. 2009); Muribaculaceae_norank might play an important role in mucosal layer degradation of the colon (Lee et al. 2019); similarly, Prevotellaceae UCG-001, a gram-negative and obligate anaerobic bacillus, had the capability to ferment carbohydrates and generate SCFAs including acetate and butyrate, thereby exerting an anti-inflammatory effect on immune cells and inhibiting the growth of potentially invading pathogenic bacteria (Downes et al. 2013; Rivera-Chávez et al. 2016); moreover, Ruminiclostridium 9 could degrade polysaccharides to produce acetate and butyrate, and then promote the development of the immune system (Wang et al. 2017). Some constituents from traditional Chinese medicines can be metabolized by gut microbes, and herb components can also affect the health homeostasis of the host through initiating changes in the composition and function of the microbial community. The phytochemical composition of LZD is extraordinarily complex, including liquirtin, isoliquirtin, glycyrrhizin, gensenoside, gingerol, atracylenolide, as well as substantial amounts of polysaccharides. Ginseng, a general tonic and adaptogen for the maintenance of host homeostasis, has been reported to exert “prebiotic-like” effects towards gut microbial community composition, along with the decreased harmful bacteria, such as Enterobacter (Eom et al. 2017). Atractylodes was capable of reducing intestinal pH value and fostering the normal gut microbiota (Wang et al. 2019a). Studies have demonstrated that the combination of ginseng and atractylodes significantly inhibited the growth of potential pathogens like Clostridiumm (Wang et al. 2019b). Interaction of gut microbiota with licorice also seemed to have potential effects on gut microbiota. Supplementation with isoliquiritin reduced the levels of opportunistic pathogens like Escherichia and increased the abundance of potentially beneficial genera, including Prevotellaceae and SCFA-producing Ruminococcus (Wu et al. 2016). Similarly, rhizoma zingiberis also possessed anti-inflammatory activities and the ability to regulate bacteria (Hong et al. 2018). Apart from effective small molecule compounds, amounts of polysaccharides were rich in LZD, which could be metabolized by gut microbes to generate SCFAs (Holscher 2017), and in turn selectively upregulate the beneficial intestinal microbiota such as acetate-producing Blautia (Guo and Li 2019). Interestingly, in UC, changes in the number and proportion of the microbiota destroyed the original micro-ecological balance, accompanied with the increase of pathogenic bacteria and decrease of beneficial bacteria, damaging intestinal mucosa and initiating chronic intestinal inflammatory response (Kong et al. 2017). Based on the above results, it indicated that LZD markedly shaped the microbiota to maintain its homeostasis and function, which had implications in the pathogenesis of DSS-induced colitis.
Moreover, accumulating studies have shown that colonic microbiota could degrade some non-digestive components such as fiber, resistant starch, and phenolic compounds via fermentation in the colon to produce metabolic substances that could reveal biological perturbations associated with diseases (Monk et al. 2016). In addition to 16S rRNA gene sequencing, untargeted metabolomics profiling based on UPLC-Q-TOF-MS was further applied to analyze fecal metabolite profiles to reflect microbial activities to understand host-microbiota interactions related to UC. Here, our observation showed that the levels of adenosine, lysoPC(18:0), glycocholic acid, and deoxycholic acid were notably increased, while cholic acid, α-linolenic acid, stearidonic acid, and l-tryptophan were markedly decreased in the DSS-induced colitis mice. However, these alterations were remarkably reversed after LZD treatment. Adenosine, an important substrate in mitochondrial adenosine triphosphate (ATP) biosynthesis that regulates energy homeostasis, was significantly increased in the DSS-induced colitis, suggesting that ATP biosynthesis might be associated with the injury of intestinal barrier and the level of inflammation (Li et al. 2019). According to numerous researches, lysoPC(18:0), one kind of the precursor of lysophosphatidic acid, was known as a bioactive glycerophospholipid, which was involved in various pathological processes such as fibrosis, inflammation, and cancer. The modification of LZD on lysoPC(18:0) level might contribute to relieving the inflammation in colitis (Gräler and Goetzl 2002). Additionally, numerous researches have revealed that the change of bile acids was also involved in the pathogenesis of colitis, which could regulate energy homeostasis and mucosal immune homeostasis via intestinal bacteria (Fiorucci and Distrutti 2015). Indeed, current understanding of glycocholic acid showed that it could damage cellular membranes and have cytotoxic effects at high concentrations, bringing about apoptosis of intestinal cells (Chen et al. 2019). Also, deoxycholic acid, as the secondary bile acid, could activate NLRP3 inflammasome through a bile acid receptor sphingosine-1-phosphate receptor 2 (S1PR2) and thus contributed to colonic inflammation (Zhao et al. 2018). Besides, significant reduction in cholic acid was observed in DSS-induced colitis in this study. Cholic acid was a high-affinity agonist of farsenoid X receptor (FXR) and the activation of FXR could promote the expression of antimicrobial peptides to strengthen the epithelial barrier and inhabit Toll-like receptor 4 (TLR4) to limit the expression of pro-inflammatory cytokines, eventually suppressing mucosal inflammation (Gadaleta et al. 2011). Additionally, the downregulation of α-linolenic acid, stearidonic acid, and l-tryptophan in colitis was linked to altered gut microbial metabolism and pathological state. As was reported, α-linolenic acid and stearidonic acid were polyunsaturated fatty acid. Alpha-linolenic acid could downregulate the intestinal inflammatory response by inhibiting colonic mRNA levels of pro-inflammatory genes, for example, IL-6, TNF-α, and cyclooxygenase 2 (Reifen et al. 2015). Stearidonic acid could alleviate inflammation by suppressing iNOS-mediated NO production via inactivation of nuclear factor κB (NF-κB) and mitogen-activated protein kinase (MAPK) signaling pathways (Sung et al. 2017). The upregulated effects of LZD on the decreased levels of α-linolenic acid and stearidonic acid in colitis mice might contribute to exerting the anti-inflammatory effect. Furthermore, in this study, data illustrated that the concentration of l-tryptophan was obviously higher after LZD intervention than in the DSS-treated mice. It is known that l-tryptophan is an essential aromatic amino acid and has a negative correlation with the inflammatory disease activity that might serve as a biomarker for UC, which could alleviate the symptoms of colitis, improve intestinal permeability, and reduce local inflammatory mediators and expression of pro-apoptotic factors, as suggested in some experimental studies (Kim et al. 2010; Sofia et al. 2018). Consistently, as the results showed, the observed differences in fecal metabolite profiles that participated in the pathological process were markedly regulated after LZD treatment.
Taken together, the present study demonstrated that LZD intervention could significantly ameliorate DSS-induced colitis by targeting gut microbiota to restore its diversity and composition and modify its metabolic profiling. After LZD treatment, gut bacteria with anti-inflammation were markedly increased, while pro-inflammatory bacteria were notably decreased by comparison with the DSS group. Meanwhile, potential metabolites and the corresponding metabolic pathways in fecal samples were altered to normal transformation with LZD intervention. This research helped clarify the detailed pharmacological mechanism of LZD on UC.
References
Adams SM, Bornemann PH (2013) Ulcerative colitis. Am Fam Physician 87:699–705. https://doi.org/10.0000/PMID23939448
Autenrieth DM, Baumgart DC (2012) Toxic megacolon. Inflamm Bowel Dis 18:584–591. https://doi.org/10.1002/ibd.21847
Basso PJ, Câmara NOS, Sales-Campos H (2019) Microbial-based therapies in the treatment of inflammatory bowel disease - an overview of human studies. Front Pharmacol 9:1571. https://doi.org/10.3389/fphar.2018.01571
Bianchi L, Gaiani F, Vincenzi F, Kayali S, Di Mario F, Leandro G, De’ Angelis GL, Ruberto C (2018) Hemolytic uremic syndrome: differential diagnosis with the onset of inflammatory bowel diseases. Acta Biomed 89:153–157. https://doi.org/10.23750/abm.v89i9-S.7911
Canfora EE, Meex RCR, Venema K, Blaak EE (2019) Gut microbial metabolites in obesity, NAFLD and T2DM. Nat Rev Endocrinol 15:261–273. https://doi.org/10.1038/s41574-019-0156-z
Chen L, Wang W, Zhou R, Ng SC, Li J, Huang M, Zhou F, Wang X, Shen B, Kamm MA, Wu K, Xia B (2014) Characteristics of fecal and mucosa-associated microbiota in Chinese patients with inflammatory bowel disease. Medicine (Baltimore) 93:e51. https://doi.org/10.1097/MD.0000000000000051
Chen ML, Takeda K, Sundrud MS (2019) Emerging roles of bile acids in mucosal immunity and inflammation. Mucosal Immunol 12:851–861. https://doi.org/10.1038/s41385-019-0162-4
Cheon JH (2013) Genetics of inflammatory bowel diseases: a comparison between western and eastern perspectives. J Gastroenterol Hepatol 28:220–226. https://doi.org/10.1111/jgh.12053
Downes J, Dewhirst FE, Tanner AC, Wade WG (2013) Description of Alloprevotella rava gen. nov., sp. nov., isolated from the human oral cavity, and reclassification of Prevotella tannerae Moore et al. 1994 as Alloprevotella tannerae gen. nov., comb. nov. Int J Syst Evol Microbiol 63:1214–1218. https://doi.org/10.1099/ijs.0.041376-0
Durand GA, Pham T, Ndongo S, Traore SI, Dubourg G, Lagier JC, Michelle C, Armstrong N, Fournier PE, Raoult D, Million M (2017) Blautia massiliensis sp. nov. isolated from a fresh human fecal sample and emended description of the genus Blautia. Anaerobe 43:47–55. https://doi.org/10.1016/j.anaerobe.2016.12.001
Eom SJ, Hwang JE, Kim KT, Paik HD (2017) Antibacterial effects against various foodborne pathogens and sensory properties of yogurt supplemented with Panax ginseng Marc extract. Korean J Food Sci Anim Resour 37:787–791. https://doi.org/10.5851/kosfa.2017.37.5.787
Ezzat SM, Ezzat MI, Okba MM, Menze ET, Abdel-Naim AB (2018) The hidden mechanism beyond ginger ( Zingiber officinale, Rosc.) potent, in vivo, and, in vitro, anti-inflammatory activity. J Ethnopharmacol 214:113–123. https://doi.org/10.1016/j.jep.2017.12.019
Fiorucci S, Distrutti E (2015) Bile acid-activated receptors, intestinal microbiota, and the treatment of metabolic disorders. Trends Mol Med 21:702–714. https://doi.org/10.1016/j.molmed.2015.09.001
Gadaleta RM, van Erpecum KJ, Oldenburg B, Willemsen EC, Renooij W, Murzilli S, Klomp LW, Siersema PD, Schipper ME, Danese S, Penna G, Laverny G, Adorini L, Moschetta A, van Mil SW (2011) Farnesoid X receptor activation inhibits inflammation and preserves the intestinal barrier in inflammatory bowel disease. Gut 60:463–472. https://doi.org/10.1136/gut.2010.212159
Garg M, Hendy P, Ding JN, Shaw S, Hold G, Hart A (2018) The effect of vitamin D on intestinal inflammation and faecal microbiota in patients with ulcerative colitis. J Crohns Colitis 12:963–972. https://doi.org/10.1093/ecco-jcc/jjy052
Gaston MA (1988) Enterobacter: an emerging nosocomial pathogen. J Hosp Infect 11:197–208. https://doi.org/10.1016/0195-6701(88)90098-9
Gonçalves P, Araújo JR, Di Santo JP (2018) A cross-talk between microbiota-derived short-chain fatty acids and the host mucosal immune system regulates intestinal homeostasis and inflammatory bowel disease. Inflamm Bowel Dis 24:558–572. https://doi.org/10.1093/ibd/izx029
Gräler MH, Goetzl EJ (2002) Lysophospholipids and their G protein-coupled receptors in inflammation and immunity. Biochim Biophys Acta 1582:168–174. https://doi.org/10.1016/s1388-1981(02)00152-x
Gu S, Li L, Huang H, Wang B, Zhang T (2019) Antitumor, antiviral, and anti-inflammatory efficacy of essential oils from Atractylodes macrocephala Koidz. produced with different processing methods. Molecules 24. https://doi.org/10.3390/molecules24162956
Guo M, Li Z (2019) Polysaccharides isolated from Nostoc commune Vaucher inhibit colitis-associated colon tumorigenesis in mice and modulate gut microbiota. Food Funct 10:6873–6881. https://doi.org/10.1039/c9fo00296k
Han YD, Al Bandar MH, Dulskas A, Cho MS, Hur H, Min BS, Lee KY, Kim NK (2017) Prognosis of ulcerative colitis colorectal cancer vs. sporadic colorectal cancer: propensity score matching analysis. BMC Surg 17:28. https://doi.org/10.1186/s12893-017-0224-z
Holscher HD (2017) Dietary fiber and prebiotics and the gastrointestinal microbiota. Gut Microbes 8:172–184. https://doi.org/10.1080/19490976.2017.1290756
Hong H, Lee JH, Kim SK (2018) Phytochemicals and antioxidant capacity of some tropical edible plants. Asian-Australas J Anim Sci 31:1677–1684. https://doi.org/10.5713/ajas.17.0903
Jia W, Xie G, Jia W (2018) Bile acid–microbiota crosstalk in gastrointestinal inflammation and carcinogenesis. Nat Rev Gastroenterol Hepatol 15:111–128. https://doi.org/10.1038/nrgastro.2017
Kim CJ, Kovacs-Nolan JA, Yang C, Archbold T, Fan MZ, Mine Y (2010) L-Tryptophan exhibits therapeutic function in a porcine model of dextran sodium sulfate (DSS)-induced colitis. J Nutr Biochem 21:468–475. https://doi.org/10.1016/j.jnutbio.2009.01.019
Kong W, Huang C, Tang Y, Zhang D, Wu Z, Chen X (2017) Effect of Bacillus subtilis on Aeromonas hydrophila -induced intestinal mucosal barrier function damage and inflammation in grass carp ( Ctenopharyngodon Idella ). Sci Rep 7(1):1588. https://doi.org/10.1038/s41598-017-01336-9
Kume K, Watanabe T, Oshima J, Yoshikawa I, Harada M (2014) Rectal perforation caused by mesalazine enema in a patient with ulcerative colitis. Endoscopy 46(Suppl 1 UCTN):E190. https://doi.org/10.1055/s-0034-1365148
Lagkouvardos I, Lesker TR, Hitch TCA, Gálvez EJC, Smit N, Neuhaus K, Wang J, Baines JF, Abt B, Stecher B, Overmann J, Strowig T, Clavel T (2019) Sequence and cultivation study of Muribaculaceae reveals novel species, host preference, and functional potential of this yet undescribed family. Microbiome 7:28. https://doi.org/10.1186/s40168-019-0637-2
Lam P, Cheung F, Tan HY, Wang N, Yuen MF, Feng Y (2016) Hepatoprotective effects of Chinese medicinal herbs: a focus on anti-inflammatory and anti-oxidative activities. Int J Mol Sci 17:465. https://doi.org/10.3390/ijms17040465
Lee KS, Palatinszky M, Pereira FC, Nguyen J, Fernandez VI, Mueller AJ, Menolascina F, Daims H, Berry D, Wagner M, Stocker R (2019) An automated Raman-based platform for the sorting of live cells by functional properties. Nat Microbiol 4:1035–1048. https://doi.org/10.1038/s41564-019-0394-9
Leonart LP, Gasparetto JC, Pontes FLD, Cerqueira LB, de Francisco TMG, Pontarolo R (2017) New metabolites of coumarin detected in human urine using ultra performance liquid chromatography/quadrupole-time-of-flight tandem mass spectrometry. Molecules 22:2031. https://doi.org/10.3390/molecules22112031
Li X, Song P, Li J, Tao Y, Li G, Li X, Yu Z (2017) The disease burden and clinical characteristics of inflammatory bowel disease in the Chinese population: a systematic review and meta-analysis. Int J Environ Res Public Health 14. https://doi.org/10.3390/ijerph14030238
Li Z, Li J, Zhang S, Chen G, Chi S, Li X, Guo F, Zhu J, Sun B (2019) Metabolomics analysis of gut barrier dysfunction in a trauma-hemorrhagic shock rat model. Biosci Rep 39:BSR20181215. https://doi.org/10.1042/BSR20181215
Lin C, Wan J, Su Y, Zhu W (2018) Effects of early intervention with maternal fecal microbiota and antibiotics on the gut microbiota and metabolite profiles of piglets. Metabolites 8:89. https://doi.org/10.3390/metabo8040089
Ma B, Kan WL, Zhu H, Li SL, Lin G (2017) Sulfur fumigation reducing systemic exposure of ginsenosides and weakening immunomodulatory activity of ginseng. J Ethnopharmacol 195:222–230. https://doi.org/10.1016/j.jep.2016.11.023
Magro F, Gionchetti P, Eliakim R, Ardizzone S, Armuzzi A, Barreiro-de Acosta M, Burisch J, Gecse KB, Hart AL, Hindryckx P, Langner C, Limdi JK, Pellino G, Zagórowicz E, Raine T, Harbord M, Rieder F (2017) European evidence-based consensus on the diagnosis and management of ulcerative colitis: definitions and diagnosis. J Crohns Colitis 11:649–670. https://doi.org/10.1093/ecco-jcc/jjx008
Maloy KJ, Powrie F (2011) Intestinal homeostasis and its breakdown in inflammatory bowel disease. Nature 474:298–306. https://doi.org/10.1038/nature10208
Marineaţă A, Rezuş E, Mihai C, Prelipcean CC (2017) Extra intestinal manifestations and complications in inflammatory bowel disease. Rev Med Chir Soc Med Nat Iasi 118:279–288. https://doi.org/10.1111/j.1365-2036.2006.03021.x
Maslowski KM, Vieira AT, Ng A, Kranich J, Sierro F, Yu D, Schilter HC, Rolph MS, Mackay F, Artis D, Xavier RJ, Teixeira MM, Mackay CR (2009) Regulation of inflammatory responses by gut microbiota and chemoattractant receptor GPR43. Nature 461:1282–1286. https://doi.org/10.1038/nature08530
Monk JM, Lepp D, Zhang CP, Wu W, Zarepoor L, Lu JT, Pauls KP, Tsao R, Wood GA, Robinson LE, Power KA (2016) Diets enriched with cranberry beans alter the microbiota and mitigate colitis severity and associated inflammation. J Nutr Biochem 28:129–139. https://doi.org/10.1016/j.jnutbio.2015.10.014
Ng SC, Tang W, Ching JY, Wong M, Chow CM, Hui AJ, Wong TC, Leung VK, Tsang SW, Yu HH, Li MF, Ng KK, Kamm MA, Studd C, Bell S, Leong R, de Silva HJ, Kasturiratne A, Mufeena MNF, Ling KL, Ooi CJ, Tan PS, Ong D, Goh KL, Hilmi I, Pisespongsa P, Manatsathit S, Rerknimitr R, Aniwan S, Wang YF, Ouyang Q, Zeng Z, Zhu Z, Chen MH, Hu PJ, Wu K, Wang X, Simadibrata M, Abdullah M, Wu JC, Sung JJY, Chan FKL (2013) Incidence and phenotype of inflammatory bowel disease based on results from the Asia-pacifc Crohn’s and colitis epidemiology study. Gastroenterology 145:158–165.e2. https://doi.org/10.1053/j.gastro.2013.04.007
Ng SC, Shi HY, Hamidi N, Underwood FE, Tang W, Benchimol EI, Panaccione R, Ghosh S, Wu JCY, Chan FKL, Sung JJY, Kaplan GG (2018) Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: a systematic review of population-based studies. Lancet 390:2769–2778. https://doi.org/10.1016/S0140-6736(17)32448-0
Nicholson JK, Holmes E, Kinross J, Burcelin R, Gibson G, Wi J, Pettersson S (2012) Host-gut microbiota metabolic interactions. Science 336:1262–1267. https://doi.org/10.1126/science.1223813
Nishida A, Inoue R, Inatomi O, Bamba S, Naito Y, Andoh A (2018) Gut microbiota in the pathogenesis of inflammatory bowel disease. Clin J Gastroenterol 11:1–10. https://doi.org/10.1007/s12328-017-0813-5
Panés J, Alfaro I (2017) New treatment strategies for ulcerative colitis. Expert Rev Clin Immunol 13:963–973. https://doi.org/10.1080/1744666X.2017.1343668
Peng Y, Yan Y, Wan P, Chen D, Ding Y, Ran L, Mi J, Lu L, Zhang Z, Li X, Zeng X, Cao Y (2019) Gut microbiota modulation and anti-inflammatory properties of anthocyanins from the fruits of Lycium ruthenicum Murray in dextran sodium sulfate-induced colitis in mice. Free Radic Biol Med 136:96–108. https://doi.org/10.1016/j.freeradbiomed.2019.04.005
Reifen R, Karlinsky A, Stark AH, Berkovich Z, Nyska A (2015) α-Linolenic acid (ALA) is an anti-inflammatory agent in inflammatory bowel disease. J Nutr Biochem 26:1632–1640. https://doi.org/10.1016/j.jnutbio.2015.08.006
Rivera-Chávez F, Zhang LF, Faber F, Lopez CA, Byndloss MX, Olsan EE, Xu G, Velazquez EM, Lebrilla CB, Winter SE, Bäumler AJ (2016) Depletion of butyrate-producing Clostridia from the gut microbiota drives an aerobic luminal expansion of Salmonella. Cell Host Microbe 19:443–454. https://doi.org/10.1016/j.chom.2016.03.004
Rosen MJ, Karns R, Vallance JE, Bezold R, Waddell A, Collins MH, Haberman Y, Minar P, Baldassano RN, Hyams JS, Baker SS, Kellermayer R, Noe JD, Griffiths AM, Rosh JR, Crandall WV, Heyman MB, Mack DR, Kappelman MD, Markowitz J, Moulton DE, Leleiko NS, Walters TD, Kugathasan S, Wilson KT, Hogan SP, Denson LA (2017) Mucosal expression of type 2 and type 17 immune response genes distinguishes ulcerative colitis from colon-only Crohn’s disease in treatment-naive pediatric patients. Gastroenterology 152:1345–1357.e7. https://doi.org/10.1053/j.gastro.2017.01.016
Sairenji T, Collins KL, Evans DV (2017) An update on inflammatory bowel disease. Primary Care 44:673–692. https://doi.org/10.1016/j.pop.2017.07.010
Sasaki M, Klapproth JM (2012) The role of bacteria in the pathogenesis of ulcerative colitis. J Signal Transduct 2012:704953–704956. https://doi.org/10.1155/2012/704953
Scarpellini E, Ianiro G, Attili F, Bassanelli C, De Santis A, Gasbarrini A (2015) The human gut microbiota and virome: potential therapeutic implications. Dig Liver Dis 47:1007–1012. https://doi.org/10.1016/j.dld.2015.07.008
Schirmer M, Garner A, Vlamakis H, Xavier RJ (2019) Microbial genes and pathways in inflammatory bowel diseas. Nat Rev Microbiol 17:497–511. https://doi.org/10.1038/s41579-019-0213-6
Shen Y, Cui X, Jiang S, Qian DW, Duan JA (2019) Comparative pharmacokinetics of nine major bioactive components in normal and ulcerative colitis rats after oral administration of Lizhong decoction extracts by UPLC-TQ-MS/MS. Biomed Chromatogr 33:e4521. https://doi.org/10.1002/bmc.4521
Shouval DS, Rufo PA (2017) The role of environmental factors in the pathogenesis of inflammatory bowel diseases: a review. JAMA Pediatr 171:999–1005. https://doi.org/10.1001/jamapediatrics.2017.2571
da Silva BC, Lyra AC, Rocha R, Santana GO (2014) Epidemiology, demographic characteristics and prognostic predictors of ulcerative colitis. World J Gastroenterol 20:9458–9467. https://doi.org/10.3748/wjg.v20.i28.9458
Skelly AN, Sato Y, Kearney S, Honda K (2019) Mining the microbiota for microbial and metabolite-based immunotherapies. Nat Rev Immunol 19:305–323. https://doi.org/10.1038/s41577-019-0144-5
Sofia MA, Ciorba MA, Meckel K, Lim CK, Guillemin GJ, Weber CR, Bissonnette M, Pekow JR (2018) Tryptophan metabolism through the kynurenine pathway is associated with endoscopic inflammation in ulcerative colitis. Inflamm Bowel Dis 24:1471–1480. https://doi.org/10.1093/ibd/izy103
Sung J, Jeon H, Kim IH, Jeong HS, Lee J (2017) Anti-inflammatory effects of stearidonic acid mediated by suppression of NF-κB and MAP-kinase pathways in macrophages. Lipids 52:781–787. https://doi.org/10.1007/s11745-017-4278-6
Thiyagarajan P, Chandrasekaran CV, Deepak HB, Agarwal A (2011) Modulation of lipopolysaccharide-induced pro-inflammatory mediators by an extract of Glycyrrhiza glabra and its phytoconstituents. Inflammopharmacology 19:235–241. https://doi.org/10.1007/s10787-011-0080-x
Troncone E, Monteleone G (2017) The safety of non-biological treatments in ulcerative colitis. Expert Opin Drug Saf 16:779–789. https://doi.org/10.1080/14740338.2017.1340936
Ungaro R, Mehandru S, Allen PB, Peyrin-Biroulet L, Colombe JF (2017) Ulcerative colitis. Lancet 389:1756–1770. https://doi.org/10.1016/S0140-6736(16)32126-2
Vegh Z, Kurti Z, Lakatos PL (2017) Epidemiology of inflammatory bowel diseases from west to east. J Dig Dis 18:92–98. https://doi.org/10.1111/1751-2980.12449
Wang Z, Elekwachi C, Jiao J, Wang M, Tang S, Zhou C, Tan Z, Forster RJ (2017) Changes in metabolically active bacterial community during rumen development, and their alteration by rhubarb root powder revealed by 16S rRNA amplicon sequencing. Front Microbiol 8:159. https://doi.org/10.3389/fmicb.2017.00159
Wang J, Feng W, Zhang S, Chen L, Tang F, Sheng YC, Ao H, Peng C (2019a) Ameliorative effect of Atractylodes macrocephala essential oil combined with Panax ginseng total saponins on 5-fluorouracil induced diarrhea is associated with gut microbial modulation. J Ethnopharmacol 238:111887. https://doi.org/10.1016/j.jep.2019.111887
Wang J, Feng W, Zhang S, Chen L, Tang F, Sheng YC, Ao H, Peng C (2019b) Gut microbial modulation in the treatment of chemotherapy-induced diarrhea with Shenzhu capsule. BMC Complement Altern Med 19:126. https://doi.org/10.1186/s12906-019-2548-y
Wei X, Tao J, Xiao S, Jiang S, Shang E, Zhu Z, Qian D, Duan J (2018a) Xiexin Tang improves the symptom of type 2 diabetic rats by modulation of the gut microbiota. Sci Rep 8:3685. https://doi.org/10.1038/s41598-018-22094-2
Wei X, Tao J, Shen Y, Xiao S, Jiang S, Shang E, Zhu Z, Qian D, Duan J (2018b) Sanhuang Xiexin Tang ameliorates type 2 diabetic rats via modulation of the metabolic profiles and NF-κB/PI-3K/Akt signaling pathways. Front Pharmacol 9:955. https://doi.org/10.3389/fphar.2018.00955
Wu M, Wu Y, Deng B, Li JS, Cao HY, Qu Y, Qian XL, Zhong GS (2016) Isoliquiritigenin decreases the incidence of colitis-associated colorectal cancer by modulating the intestinal microbiota. Oncotarget 7:85318–85331. https://doi.org/10.18632/oncotarget.13347
Xu J, Chen N, Wu Z, Song Y, Zhang Y, Wu N, Zhang F, Ren X, Liu Y (2018) 5-Aminosalicylic acid alters the gut bacterial microbiota in patients with ulcerative colitis. Front Microbiol 9:1274. https://doi.org/10.3389/fmicb.2018.01274
Yilmaz B, Juillerat P, Øyås O, Ramon C, Bravo FD, Franc Y, Fournier N, Michetti P, Mueller C, Geuking M, Pittet VEH, Maillard MH, Rogler G, Wiest R, Stelling J, Macpherson AJ (2019) Microbial network disturbances in relapsing refractory Crohn’s disease. Nat Med 25:323–336. https://doi.org/10.1038/s41591-018-0308-z
Yuza K, Nagahashi M, Shimada Y, Nakano M, Tajima Y, Kameyama H, Nakajima M, Takabe K, Wakai T (2018) Upregulation of phosphorylated sphingosine kinase 1 expression in colitis-associated cancer. J Surg Res 231:323–330. https://doi.org/10.1016/j.jss.2018.05.085
Zhang C, Jiang M, Lu A (2013) Considerations of traditional Chinese medicine as adjunct therapy in the management of ulcerative colitis. Clin Rev Allergy Immunol 44:274–283. https://doi.org/10.1007/s12016-012-8328-9
Zhang M, Sun K, Wu Y, Yang Y, Tso P, Wu Z (2017) Interactions between intestinal microbiota and host immune response in inflammatory bowel disease. Front Immunol 8:942. https://doi.org/10.3389/fimmu.2017.00942
Zhang F, Li Y, Wang X, Wang S, Bi D (2019) The impact of Lactobacillus plantarum on the gut microbiota of mice with DSS-induced colitis. Biomed Res Int 2019:3921315–3921310. https://doi.org/10.1155/2019/3921315
Zhao S, Gong Z, Du X (2018) Deoxycholic acid-mediated sphingosine-1-phosphate receptor 2 signaling exacerbates DSS-induced colitis through promoting cathepsin B release. J Immunol Res 2018:2481418–2481419. https://doi.org/10.1155/2018/2481418
Zhou Y, Shan G, Sodergren E, Weinstock G, Walker WA, Gregory KE (2015) Longitudinal analysis of the premature infant intestinal microbiome prior to necrotizing enterocolitis: a case-control study. PLoS One 10:e0118632. https://doi.org/10.1371/journal.pone.0118632
Zhu B, Cao H, Sun L, Li B, Guo LW, Duan JA, Zhu HX, Zhang QC (2018) Metabolomics-based mechanisms exploration of Huang-Lian Jie-Du decoction on cerebral ischemia via UPLC-Q-TOF/MS analysis on rat serum. J Ethnopharmacol 216:147–156. https://doi.org/10.1016/j.jep.2018.01.015
Funding
This work was financially supported by Jiangsu Collaborative Innovation Center of Chinese Medicinal Resources Industrialization (No.ZDXM-1-10).
Author information
Authors and Affiliations
Contributions
J.F.Z. designed the study, performed experiments, analyzed the data, and wrote the manuscript. Y.M.S., M.J.C, Z.M.Z, S.W.X, C.L, Y.W, L.Y., and E.X.S. helped with performed experiments and analyzed data. S.J. helped with design and review of the manuscript. D.W.Q. and J.A.D. contributed analytical tools. All authors read and approved the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PDF 901 kb)
Rights and permissions
About this article
Cite this article
Zou, J., Shen, Y., Chen, M. et al. Lizhong decoction ameliorates ulcerative colitis in mice via modulating gut microbiota and its metabolites. Appl Microbiol Biotechnol 104, 5999–6012 (2020). https://doi.org/10.1007/s00253-020-10665-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00253-020-10665-1