Abstract
Extracellular vesicles (EVs) are small vesicles ensuring transport of molecules between cells and throughout the body. EVs contain cell type-specific signatures and have been proposed as biomarkers in a variety of diseases. Their small size (<1 μm) and biological and physical functions make them obvious candidates for therapeutic agents in immune therapy, vaccination, regenerative medicine and drug delivery. However, due to the complexity and heterogeneity of their origin and composition, the actual mechanism through which these vesicles exert their functions is still unknown and represents a great biomedical challenge. Moreover, because of their small dimensions, the quantification, size distribution and biophysical characterization of these particles are challenging and still subject to controversy. Here, we address the advantage of atomic force microscopy (AFM), for the characterization of isolated EVs. We review AFM imaging of EVs immobilized on different substrates (mica, glass) to identify the influence of isolation and deposition methods on the size distribution, morphology and mechanical properties of EVs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Extracellular vesicles (EVs) are small phospholipid-based vesicles present in most, if not all, human body fluids. They are naturally released by cells into the surrounding medium and are used as vehicles for cargo molecules such as proteins and genetic material between cells and throughout the body. EVs mediate active communication between cells and regulate the growth and the fate of adjacent and distant cells (Roma-Rodrigues et al. 2014). The two most prominent classes of EVs are nanoscale exosomes (EXOs) with dimensions between 30 and 150 nm originating from the endosomal system, and larger microvesicles (100–1000 nm) created by the budding of the plasma membrane. Recently, EXOs have drawn considerable attention from the scientific community for their potential application to nanomedicine, in particular in the fight against cancer. It has been shown that, in tumour models, both cancer cells and tumour microenvironment (TME) stromal cells release EXOs that promote tumour-induced immune suppression, angiogenesis and metastasis (Bourkoula et al. 2014). Aside from promoting tumour proliferation, studies conducted on EVs extracted from cancer patients have shown that EXOs carry distinct markers for most types of cancerous tumours and could hence be used as an early diagnostic tool, when cancer is more easily treatable (Vella 2014; Skog et al. 2008; Akers et al. 2013; Svensson et al. 2011). The potential goes beyond cancer detection since EXOs could be used as markers for a variety of diseases, but also as therapeutic agents in immune therapy, in regenerative medicine, drug delivery and in vaccination trials (Fais et al. 2016).
The field, however, is still in its infancy and there are important issues that need urgent attention. In fact, there are no accepted standards for the quantification of the chemical and physical properties of EXOs, in particular with respect to their function. To date, most health-related studies involving EXOs focus on their biological/genetic content (Fais et al. 2016; Minciacchi et al. 2015; Tickner et al. 2014) with little attention to their biophysical properties such as surface charge or mechanical properties. The stiffness of EXOs, from tumour cells in particular, has recently been indicated as a malignant-state dependent signature (Whitehead et al. 2015).
EXO characterization is usually carried out following different steps: (1) collection of biofluids or the supernatant of cultured cells; (2) isolation of vesicles; (3) classification by size, size distribution; (4) characterization of membrane receptors (type and distribution); (5) extraction and analysis of their RNA, DNA and protein contents.
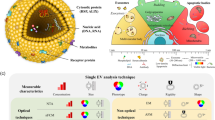
A recent survey (Gardiner et al. 2016) showed that the characterization of EVs is dominated by Western blot analysis (biomarker individuation), single-particle tracking techniques [size distribution evaluation by nanoparticle tracking analysis (Dragovic et al. 2011), resistive pulse sensing (Vogel et al. 2016; Anderson et al. 2015), dynamic light scattering (Van der Pol et al. 2010)] and electron microscopies (morphological and structural characterization; Sharma et al. 2010; Van der Pol et al. 2012). According to the survey, less than 10% of the work carried out with EVs have employed atomic force microscopy (AFM). Compared to the other techniques, AFM can at the same time measure vesicle size distribution, map their mechanical properties with nanometric precision (Whitehead et al. 2015; Calò et al. 2014) and also be used for functional analysis of the protein content of the EXO’s external membrane, via antibody-coated tips (Yuana et al. 2010; Sharma et al. 2011). Moreover, by using specific antibody-coated surfaces (mica and glass), different EXO subpopulations can be captured (Hardij et al. 2013; Jorgensen et al. 2013) and analyzed by AFM. Despite its adaptability, however, the use of AFM for EV characterization is still limited to a few studies, mainly because of the strong effect of immobilization conditions on the measurement of vesicle size. Indeed, there is no consensus yet on the best strategies for a proper AFM characterization of size, morphology and stiffness of exosomes.
Here we review the results of different immobilization strategies on the visualization of exosomes via AFM, evidencing hurdles and precautions to be taken into account when analysing EXO size distribution and mechanical properties with this technique. At the same time, we propose physical explanations for the artefacts both deriving from sample preparation procedures and intrinsic to the measurements, showing how to obtain reliable vesicle size distributions with AFM.
Results and discussion
In Fig. 1, we report the typical experimental workflow for the AFM analysis of EVs. Isolation of the vesicles from biofluids or from the extracellular medium of cultured cells is usually carried out by size exclusion chromatography, ultracentrifuge, particle precipitation, cross flow and diafiltration. Several reports on the different methods for EV isolation and their relative throughput/purification level have been published (Paolini et al. 2016; Khatun et al. 2016; Gholizadeh et al. 2017; Caponnetto et al. 2017; Woo et al. 2016; Iwai et al. 2016). Here, we focus our attention on the steps following vesicle isolation, namely surface immobilization and subsequent AFM analysis.
Schematic of the workflow for EXOs analysis. Biosamples are collected and/or cells are cultured on Petri dishes. Exosomes are subsequently extracted and isolated from the extracellular medium collected after confluence of cells or directly from the biofluid of interest (blood, saliva, urine). EXOs are then deposited on the substrate (mica, glass) and analyzed with AFM
AFM imaging requires a sample immobilized on a surface. To image biological samples (DNA, proteins, fibrils, vesicles), the surface has preferentially to be very flat (roughness <0.5 nm), to inherently have some residual charge for electrostatic interaction, and in some cases, to be transparent (especially when AFM is coupled with fluorescence optical imaging). In Fig. 2 and in Table 1, we summarize the principal immobilization methods reported so far for EV visualization. Among the available substrates, muscovite mica is easily cleavable, leaving a negatively charged, atomically flat surface and represents the most common substrate for single molecule imaging of DNA and proteins. It has been the first choice also for the AFM imaging of EXOs (Fig. 2a). In fact, the electrostatic interaction between the bare surface of mica and the vesicles is sufficient to keep them attached to the surface, also after washing with pure water or buffer and drying with nitrogen for imaging in air (Palanisamy et al. 2010; Sharma et al. 2010, 2014; Woo et al. 2016; DiNoto et al. 2016; Tian et al. 2010; Paolini et al. 2016; Caponnetto et al. 2017). Increasing the incubation time renders vesicle imaging possible even in liquid without functionalization of the mica surface, as reported by several groups (Whitehead et al. 2015; Regev-Rudzki et al. 2013; Danielson et al. 2016). However, to improve the stability of immobilization in liquid and/or the selectivity of vesicle binding with respect to potential contaminants, the surface of mica can be functionalized with either charged polymers (Sebaihi et al. 2017; Woo et al. 2016) or antibodies (Sebaihi et al. 2017; Hardij et al. 2013; Yuana et al. 2010; Fig. 2b, c). Similar results have been also obtained with glass slides and silicon surfaces where an oxygen plasma can create electrostatic conditions for a sufficiently strong binding to the surface (Calò et al. 2014) or the presence of antibodies can facilitate the immobilization of the desired vesicles (Gajos et al. 2017). Great care should be taken in the optimization of the functionalization protocols to avoid an excessive increase in surface roughness. In fact, as will be discussed in more detail in the next few paragraphs, EXO height in AFM is reported to be in some cases as low as a few nanometers (Palanisamy et al. 2010), while sometimes the roughness of antibody coated surfaces can be of the same order of magnitude (roughness values of 2.3 and 2.6 nm have been reported in Yuana et al. 2010), potentially hindering proper vesicle visualization.
The measured EXO height values ranged from a few nanometers to several tens of nanometers, depending on imaging conditions and immobilization method employed. Usually, when measurements are performed in air in amplitude modulation mode, the height distribution ranges from 1–2 to 15–20 nm, while the diameter spans from 30 to 200 nm (Palanisamy et al. 2010; Sharma et al. 2010, 2011, 2014; Sharma and Gimzewski 2012; Woo et al. 2016; DiNoto et al. 2016; Tian et al. 2010; Paolini et al. 2016; Sebaihi et al. 2017; Hardij et al. 2013). In air, exosomes often appear as roundish vesicles, presenting a typical “cup shape” (Palanisamy et al. 2010; Sharma and Gimzewski 2012). In Fig. 3a, we present an AFM image of SKBR3-derived EXOs deposited on mica, dried with N2 and imaged in air in amplitude modulation AFM (NT-MDT Solver Pro, spring constant 2 N/m, resonance frequency ≈70 kHz, amplitude ≈50 nm). This “cup shape” effect is clearly distinguishable, with the vesicles presenting a central collapsed area (see arrows in Fig. 3a) that appears almost as dark as the mica surface around it. This effect has been shown to be more pronounced when increasing the applied force during AFM measurements (Sharma et al. 2010) and can be avoided working in very soft amplitude modulation conditions or in peak force mode (Hardij et al. 2013; Sebaihi et al. 2017; DiNoto et al. 2016; Paolini et al. 2016; Caponnetto et al. 2017). The central collapse of the vesicles is, therefore, mainly imputed to the mechanical perturbation exerted by the AFM tip to the vesicle in air: the vesicle central area is softer than its surroundings, and responds to the force applied by the tip with a more pronounced indentation (Sharma et al. 2010).
Representative AFM topographic images (amplitude modulation) of EXO samples obtained following different preparation methods. a EXOs spotted on mica, dried with N2 and imaged in air. b EXOs spotted on mica, fixed with PFA, dried with N2 and imaged in air. c EXOs spotted on plasma-cleaned glass, and imaged in PBS
Few attempts have been made to preserve the shape of vesicles while imaging them in air by using fixation protocols, like the ones adopted in electron microscopy. However, fixation with glutaraldehyde or paraformaldehyde has been reported for the analysis of EVs (Nguyen et al. 2016; Rauti et al. 2016). After fixation, the vesicles appear more spherical with respect to the non-fixated ones: during the fixation process, in fact, aldehydes stabilize the nucleic acid-protein shell interacting with free amino groups, with a cross-linking effect that stabilizes the membrane, preserving the natural structures of the molecules (lipids, proteins) and hence the vesicle shape (Chao and Zhang 2011). In Fig. 3b, we report an image taken in our group of SKBR3-derived EXOs, fixed in 4% paraformaldehyde, deposited on mica, dried with N2 and imaged in air in amplitude modulation AFM (NT-MDT Solver Pro, spring constant 2 N/m, resonance frequency ≈70 kHz, amplitude ≈50 nm).
When vesicles are imaged in a liquid environment, their spherical shape is preserved during AFM imaging, and heights in the range of 10–100 nm are routinely measured, regardless of the imaging conditions [amplitude modulation AFM in the case of Regev-Rudzki et al. (2013), Sebaihi et al. (2017), and Calò et al. (2014) and peak force AFM with Hardij et al. (2013), and Whitehead et al. (2015)]. As an example of AFM measurements in liquid, in Fig. 3c, we report an image of SKBR3-derived EXOs, deposited on a plasma-cleaned glass slide [following protocols reported in Calò et al. (2014)], imaged in PBS in amplitude modulation AFM (MFP-3D Asylum Research, spring constant 0.1 N/m, resonance frequency ≈32 kHz, amplitude ≈30 nm).
The specific drying process used before measurements in air might also affect AFM morphological measurements. Hardji et al. (2013) observed a shrinking of the particle size from liquid to air measurements, and attributed this effect to the loss of water during the drying process. On the contrary, Sebaihi et al. (2017) observed no differences between diameter and height distributions of the same EVs measured in liquid and in air. Sebaihi et al. justified the contrasting results with the different mechanical response of the two distinct families of EVs used in his work and in the one of Hardji et al. However, in Hardij et al. (2013), as in many other reports, EVs were dried by means of a gentle stream of nitrogen, while in Sebaihi et al. (2017) the water drop covering EVs was left to naturally evaporate. This last method keeps the vesicles hydrated during in air measurements, better preserving their shape. A similar observation has been reported by Chernishev et al. (2015): by means of electron microscopy measurements, dynamic light scattering and nanoparticle tracking they observed that an isotropic desiccation in aerosol is more prone to preserve the spherical shape of the exosomes, than a direct drying on a surface.
As a general effect on the measured size distribution in both liquid and air measurements, tip convolution effects should be taken into account in the vesicles’ lateral size assessment: the finite dimensions of the tip cause an extension of the interacting surface area, that is reflected in a broadening of the surface features (Canet-Ferrer et al. 2014). Usually, in the evaluation of particle dimensions, tip convolution effects are minimized by taking into account the diameter measured at mid-height of the vesicles. Nonetheless, as proven by Sebaihi et al. in their recent report (Sebaihi et al. 2017), by deconvoluting tip effects, the distribution of diameters shifted towards lower values, from an average value of 76.2 ± 19.9 nm before correction to 64.1 ± 19 nm after correction. An accurate analysis of the tip size after imaging should be carried out on reference samples [polysterene beads, as suggested in Sebaihi et al. (2017) or commercially available kits (Yacoot and Koenders 2008)]. This effect has, therefore, to be considered when comparative analyses between EXOs of different origin are performed. In fact, size distributions can be different in healthy or tumour-derived vesicles, as already observed by Sharma et al. (2011): in oral cancer patients saliva-isolated exosomes have a broader distribution and an average size significantly higher than the ones of healthy donor-derived exosomes.
The change in size distribution is not the only effect observed on analysing tumour and healthy vesicles. Indeed, Whitehead and coworkers demonstrated that the mechanical properties (stiffness and adhesion) of vesicles derived from malignant cells are, on average, one order of magnitude lower compared with non-malignant cell EXOs (Whitehead et al. 2015). In their report, by using dynamic nanomechanical mapping (DNM) in liquid (Zhang et al. 2014), they acquired fast force curves for each recorded image pixel, and simultaneously visualized, with standard topographic images, adhesion and stiffness maps. This kind of nanomechanical analysis should be further implemented for clinical purposes.
Beside force mapping as implemented in DNM, a bunch of single force-indentation curves can be measured on isolated vesicles with a standard AFM setup. In Fig. 4, we report a schematic and a typical force-indentation curve on a vesicle. We can clearly observe the onset of interaction force between the AFM tip and the EV surface starting at around 20 nm (black arrow in Fig. 4) from the surface of the supporting glass (δ = 0). This force-distance curve is in agreement with typical indentation curves for lipid vesicles on hard surfaces (Liang et al. 2004; Roos et al. 2010; Park 2010; Li et al. 2011; Vorselen et al. 2017). Such curves can be then be analyzed by modelling the nanovesicles as elastic shells with a defined thickness as reported by Calò et al. (2014). They extracted the elastic modulus of EVs derived from Saccharomyces cerevisiae, using the thin shell formula of Hernando-Perez et al. (2012), finding values comparable with vesicles of other origin reported in the literature.
Remaining with nanomechanics, recently, Voorselen et al. presented an AFM nanoindentation-based approach for quantification of the mechanics of nanovesicles. They used liposomes of mixed compositions and analyzed their nanomechanical behaviour by developing a theoretical model, which includes fluidity effects on the membrane. They were able to show the importance of internal osmotic pressure due to surface adhesion in the analysis of liposomes in liquid conditions. Their findings might then be exported to study natural vesicles and compared with the data already present in the literature (Calò et al. 2014; Palanisamy et al. 2010; Sharma et al. 2010).
Finally, additional information on vesicle composition can be obtained from force-distance curves with AFM tips functionalized with antibodies directed to proteins present in the membrane of vesicles, as demonstrated by Gimzewsky’s group (Sharma et al. 2010). Their analysis of the distribution of rupture events showed that the specific interaction between the antibody (anti-CD63) and the protein (CD63) on the membrane of the exosomes ranged from 30 to 200 pN, evidencing strong adhesive events, easily distinguishable with respect to nonspecific interactions (Sharma et al. 2010). The molecular recognition mapping based in this approach could allow the visualization of EVs by their biomolecular load and their specific interaction, allowing distinguishing of different EXO subpopulations.
Conclusions
We presented here an overview of the AFM characterization of EVs. We reviewed different conditions of immobilization and imaging of the vesicles, evidencing the importance of operating in liquid to better preserve the physical properties of the vesicles. Imaging in air is definitely useful to rapidly check the presence of vesicles and the quality of the sample; however, to obtain meaningful size distributions, and carefully derive mechanical properties, AFM in liquid is the optimal choice. Establishing immobilization and visualization protocols is the starting point for the collection of an “ID card” (size distribution, morphology, mechanical properties, biomolecular load) of exosomes derived from specific subpopulations of cells. This ID card could be an effective tool for discrimination between exosomes deriving from cancer and healthy cells and will be crucial in the development of protocols for the separation and analysis of plasma-derived exosomes whose origin is unknown.
References
Akers JC, Ramakrishnan V, Kim R, Skog J, Nakano I, Pingle S, Kalinina J, Hua W, Hesari S, Mao Y, Breakefield XO, Hochberg FH, Van Meir EG, Carter BS, Chen CC (2013) MiR-21 in the extracellular vesicles (EVs) of cerebrospinal fluid (CSF): a platform for glioblastoma biomarker development. PLoS ONE 8:e78115. doi:10.1371/journal.pone.0078115
Anderson W, Lane R, Korbie D, Trau M (2015) Observations of tunable resistive pulse sensing for exosome analysis: improving system sensitivity and stability. Langmuir 31:6577–6587. doi:10.1021/acs.langmuir.5b01402
Ashcroft BA, de Sonneville J, Yuana Y, Osanto S, Bertina R, Kuil ME, Oosterkamp TH (2012) Determination of the size distribution of blood microparticles directly in plasma using atomic force microscopy and microfluidics. Biomed Microdevice 14:641. doi:10.1007/s10544-012-9642-y
Bourkoula E, Mangoni D, Ius T, Pucer A, Isola M, Musiello D, Marzinotto S, Toffoletto B, Sorrentino M, Palma A, Caponnetto F, Gregoraci G, Vindigni M, Pizzolitto S, Falconieri G, De Maglio G, Pecile V, Gruaro M, Gri G, Parisse P, Casalis L, Scoles G, Skrap M, Beltrami CA, Beltrami AP, Cesselli D (2014) Glioma-associated stem cells: a novel class of tumor-supporting cells able to predict prognisis of human low-grade gliomas. Stem Cells 32:1239–1253. doi:10.1002/stem.1605
Calò A, Reguera D, Oncincs G, Persuy MA, Sanz G, Lobasso S, Corcelli A, Pajot-Augy E, Gomila G (2014) Force measurements on natural membrane nanovesicles reveal a composition-independent, high Young’s modulus. Nanoscale 21:2275–2285. doi:10.1039/c3nr05107b
Canet-Ferrer J, Coronado E, Forment-Aliaga A, Pinilla-Cienfuegos E (2014) Correction of the tip convolution effects in the imaging of nanostructures studied through scanning force microscopy. Nanotechnology 25:395703. doi:10.1088/0957-4484/25/39/395703
Caponnetto F, Manini I, Skrap M, Palmai-Pallaga T, Loreto C, Beltrami AP, Cesselli D, Ferrari E (2017) Size-dependent cellular uptake of exosomes. Nanomed NMB 13:1011. doi:10.1016/j.nano.2016.12.009
Chao Y, Zhang T (2011) Optimization of fixation methods for observation of bacterial cell morphology and surface ultrastructures by atomic force microscopy. Appl Microbiol Biotechnol 92:381. doi:10.1007/s00253-011-3551-5
Chernyshev VS, Rachamadugu R, Tseng YH, Belnap DM, Jia Y, Branch KJ, Butterfield AE, Pease LF III, Bernard PS, Skliar M (2015) Size and shape characterization of hydrated and desiccated exosomes. Anal Bioanal Chem 407:3285–3301. doi:10.1007/s00216-015-8535-3
Danielson KM, Estanislau J, Tigges J, Toxavidis V, Camacho V, Felton EJ, Khoory J, Kreimer S, Ivanov AR, Mantel P-Y, Jones J, Akuthota P, Das S, Ghiran I (2016) Diurnal variations of circulating extracellular vesicles measured by nano flow cytometry. PLoS ONE 11:e0144678. doi:10.1371/journal.pone
DiNoto G, Bugatti A, Zendrini A, Mazzoldi EL, Montanelli A, Caimi L, Rusnati M, Ricotta D, Bergese P (2016) Merging colloidal nanoplasmonics and surface plasmon resonance spectroscopy for enhanced profiling of multiple myeloma-derived exosomes. Biosens Bioelectron 77:518. doi:10.1016/j.bios.2015.09.061
Dragovic RA, Gardiner C, Brooks AS, Ds Tannetta, Ferguson DJ, Hole P, Carr B, Redman CW, Harris AL, Dobson PJ, Harrison P, Sargent IL (2011) Sizing and phenotyping of cellular vesicles using nanoparticle tracking analysis. Nanomedicine 7:780. doi:10.1016/j.nano.2011.04.003
Fais S, O’Driscoll L, Borras FE, Buzas E, Camussi G, Cappello F, Carvalho J, Cordeiro da Silva A, Del Portillo H, El Andaloussi S, Ficko Trcek T, Furlan R, Hendrix A, Gursel I, Kralj-Iglic V, Kaeffer B, Kosanovic M, Lekka ME, Lipps G, Logozzi M, Marcilla A, Sammar M, Llorente A, Nazarenko I, Oliveira C, Pocsfalvi G, Rajendran L, Raposo G, Rohde E, Siljander P, van Niel G, Vasconcelos MH, Yanez-Mo M, Yliperttula ML, Zarovni N, Zavec AB, Giebel B (2016) Evidence-based clinical use of nanoscale extracellular vesicles in nanomedicine. ACS Nano 10:3886. doi:10.1021/acsnano.5b08015
Gajos K, Kamińska A, Awsiuk K, Bajor A, Gruszczyński K, Pawlak A, Żądło A, Kowalik A, Budkowski A, Stępień E (2017) Immobilization and detection of platelet-derived extracellular vesicles on functionalized silicon substrate: cytometric and spectrometric approach. Anal Bioanal Chem 409:1109. doi:10.1007/s00216-016-0036-5
Gardiner C, Di Vizio D, Sahoo S, Thery C, Witwer KW, Wauben M, Hill AF (2016) Techniques used for the isolation and characterization of extracellular vesicles: results of a worldwide survey. J Extracell Ves 5:32945. doi:10.3402/jev.v5.32945
Gholizadeh S, Draz M, Zarghooni M, Nezhad AS, Ghavami S, Shafiee H, Akbari M (2017) Microfluidic approaches for isolation, detection, and characterization of extracellular vesicles: current status and future directions. Biosens Bioelectron 91:588. doi:10.1016/j.bios.2016.12.062
Hardij J, Cecchet F, Berquand A, Gheldof D, Chatelain C, Mullier F, Chatelain B, Dogné JM (2013) Characterisation of tissue factor-bearing extracellular vesicles with AFM: comparison of air-tapping-mode AFM and liquid peak force AFM. J Extracell Vesicles 2:21045. doi:10.3402/jev.v2i0.21045
Hernando-Perez M, Miranda R, Aznar M, Carrascosa JL, Schaap IAT, Reguera D, de Pablo PJ (2012) Direct measurement of phage phi29 stiffness provides evidence of internal pressure. Small 8:2366. doi:10.1002/smll.201200664
Iwai K, Minamisawa T, Suga K, Yajima Y, Shiba K (2016) Isolation of human salivary extracellular vesicles by iodixanol density gradient ultracentrifugation and their characterizations. J Extracell Vesicles. doi:10.3402/jev.v5.30829
Jorgensen M, Baek R, Pedersen S, Sondergaarf EKL, Kristensen SR, Varming K (2013) Extracellular vesicle (EV) array: microarray capturing of exosomes and other extracellular vesicles for multiplexed phenotyping. J Extracell Vesicles 2:20920. doi:10.3402/jev.v2i0.20920
Khatun Z, Bhat A, Sharma S, Sharma A (2016) Elucidating diversity of exosomes: biophysical and molecular characterization methods. Nanomedicine 11:2359–2377. doi:10.2217/nnm-2016-0192
Li S, Eghiaian F, Sieben C, Herrmann A, Schaap IAT (2011) Bending and puncturing the influenza lipid envelope. Biophys J 100:637. doi:10.1016/j.bpj.2010.12.3701
Liang X, Mao G, Ng KYS (2004) Mechanical properties and stability measurement of cholesterol-containing liposome on mica by atomic force microscopy. Colloids Surf B 34:41. doi:10.1016/j.jcis.2004.05.042
Minciacchi V, Freeman MR, Di Vizio D (2015) Extracellular vesicles in cancer: exosomes, microvesicles and the emerging role of large oncosomes semin. Cell Develop Biol 40:41–51. doi:10.1016/j.semcdb.2015.02.010
Nguyen DB, Ly TBT, Wesseling MC, Hittinger M, Torge A, Devitt A, Perrie Y, Bernhardt I (2016) Characterization of microvesicles released from human red blood cells. Cell Physiol Biochem 38:1085. doi:10.1159/000443059
Palanisamy V, Sharma S, Deshpande A, Zhou H, Gimzewski J, Wong DT (2010) Nanostructural and transcriptomic analyses of human saliva derived exosomes. PLoS ONE 5:e8577. doi:10.1371/journal.pone.0008577
Paolini L, Zendrini A, Di Noto G, Busatto S, Lottini E, Radeghieri A, Dossi A, Caneschi A, Ricotta D, Bergese P (2016) Residual matrix from different separation techniques impacts exosome biological activity. Sci Rep 6:23550. doi:10.1038/srep23550
Park JW (2010) Sulfatide incorporation effect on mechanical properties of vesicles. Colloids Surf B 80:59. doi:10.1016/j.colsurfb.2010.05.031
Rauti R, Lozano N, Leon V, Scaini D, Musto M, Rago I, Ulloa Severino FP, Fabbro A, Casalis L, Vazquez E, Kostarelos K, Prato M, Ballerini L (2016) Graphene oxide nanosheets reshape synaptic function in cultured brain networks. ACS Nano 10:4459. doi:10.1021/acsnano.6b00130
Regev-Rudzki N, Wilson DW, Carvalho TG, Sisquella X, Coleman BM, Rug M, Bursac D, Angrisano F, Gee M, Hill AF, Baum J, Cowman AF (2013) Cell-cell communication between malaria-infected red blood cells via exosome-like vesicles. Cell 153:1120. doi:10.1016/j.cell.2013.04.029
Roma-Rodrigues C, Fernandes AR, Baptista PV (2014) Exosome in tumour microenvironment: overview of the crosstalk between normal and cancer cells. Biomed Res Int 2014:179486. doi:10.1155/2014/179486
Roos WH, Bruinsma R, Wuite GJL (2010) Physical virology. Nat Phys 6:733. doi:10.1038/nphys1797
Sebaihi N, De Boeck B, Yuana Y, Nieuwland R, Pétry J (2017) Dimensional characterization of extracellular vesicles using atomic force microscopy. Meas Sci Technol 28:034006. doi:10.1088/1361-6501/28/3/034006
Sharma S, Gimzewski JK (2012) The quest for characterizing exosomes: circulating nano-sized vesicles. J Nanomed Nanotechol 3:e115. doi:10.4172/2157-7439.1000e115
Sharma S, Rasooi HI, Palanisamy V, Mathisen C, Schmidt M, Wong DT, Gimzewski (2010) Structural-mechanical characterization of nanoparticle exosomes in human saliva, using correlative AFM, FESEM, and force spectroscopy. ACS Nano 4:1921. doi:10.1021/nn901824n
Sharma S, Gillespie BM, Palanisamy V, Gimzewski J (2011) Quantitative nanostructural and single-molecule force spectroscopy biomolecular analysis of human-saliva-derived exosomes. Langmuir 27:14394. doi:10.1021/la2038763
Sharma S, Das K, Woo J-R, Gimzewski JK (2014) Nanofilaments on glioblastoma exosomes revealed by peak force microscopy. J R Soc Interface 11:20131150. doi:10.1098/rsif.2013.1150
Siedlecki CA, Wang IW, Higashi JM, Kottke-Marchant K, Marchant RE (1999) Platelet-derived microparticles on synthetic surfaces observed by atomic force microscopy and fluorescence microscopy. Biomaterials 20:1521. doi:10.1016/S0142-9612(99)00065-4
Skog J, Wurdinger T, van Rijn S, Meijer DH, Gainche L, Sena-Esteves M, Curry WT, Carter BS, Krichevsky AM, Breakefield XO (2008) Glioblastoma microvesicles transport RNA and proteins that promote tumour growth and provide diagnostic biomarkers. Nat Cell Biol 10:1470. doi:10.1038/ncb1800 (Epub 2008 Nov 16)
Svensson KJ, Kucharzewska P, Christianson HC, Skold S, Lofstedt T, Johansson MC, Morgelin M, Bengzon J, Ruf Belting M (2011) Hypoxia triggers a proangiogenic pathway involving cancer cell microvesicles and PAR-2-mediated heparin-binding EGF signaling in endothelial cells. PNAS 198:13147. doi:10.1073/pnas.1104261108
Tian T, Wang Y, Wang H, Zhu Z, Xiao Z (2010) Visualizing of the cellular uptake and intracellular trafficking of exosomes by live-cell microscopy. J Cell Biochem 111:488. doi:10.1002/jcb.22733
Tickner JA, Urquhart AJ, Stephenson S, Richard DJ, O’Byrne KJ (2014) Functions and therapeutic roles of exosomes in cancer. Front Oncol 4:127. doi:10.3389/fonc.2014.00127.eCollection
Van der Pol E, Hoekstra AG, Sturk A, Otto C, van Leeuwen TG, Nieuwland R (2010) Optical and non-optical methods for detection and characterization of microparticles and exosomes. J Thromb Haemost 8:2596. doi:10.1111/j.1538-7836.2010.04074.x
Van der Pol E, van Gemert MJ, Sturk A, Nieuwland R, van Leeuwen TG (2012) Single vs. swarm detection of microparticles and exosomes by flow cytometry. J Thromb Haemost 10:919 doi: 10.1111/j.1538-7836.2012.04683.x
Vella LJ (2014) The emerging role of exosomes in epithelial-mesenchymal-transition in cancer. Front Oncol 4:361. doi:10.3389/fonc.2014.00361
Vogel R, Coumans FAW, Maltesen RG, Boing AN, Bonnington KE, Broekman ML, Broom MF, Buzas EI, Christiansen G, Hajji N, Kristensen SR, Kuehn MJ, Lund SM, Maas SLN, Nieuwland R, Osteikoetxea X, Schnoor R, Scicluna BJ, Shambrook M, de Vrij J, Mann SI, Hill AF, Pedersen S (2016) A standardized method to determine the concentration of extracellular vesicles using tunable resistive pulse sensing. J Extracell Vesicles 5:31242. doi:10.3402/jev.v5.31242
Vorselen D, MacKintosh FC, Roos WH, Wuite GJL (2017) Competition between bending and internal pressure governs the mechanics of fluid nanovesicles. ACS Nano 11:2628. doi:10.1021/acsnano.6b07302
Whitehead B, Wu L, Hvam ML, Aslan H, Dong M, Dyrskjot L, Ostenfeld MS, Moghimi SM, Howard KA (2015) Tumour exosomes display differential mechanical and complement activation properties dependent on malignant state: implications in endothelial leakiness. J Extracell Ves 4:29685. doi:10.3402/jev.v4.29685
Woo JR, Sharma S, Gimzewski J (2016) The role of isolation methods on a nanoscale surface structure and its effect on the size of exosomes. J Circ Biomark 5:11. doi:10.5772/64148
Yacoot A, Koenders L (2008) Aspects of scanning force microscope probes and their effects on dimensional measurement. J Phys D Appl Phys 41:103001. doi:10.1088/0022-3727/41/10/103001
Yuana Y, Oosterkamp TH, Bahatyrova S, Ashcroft B, Garcia Rodriguez P, Bertina RM, Osanto S (2010) Atomic force microscopy: a novel approach to the detection of nanosized blood microparticles. J Thromb Haemost 8:315. doi:10.1111/j.1538-7836.2009.03654.x
Zhang S, Aslan H, Besenbacher F, Dong M (2014) Quantitative biomolecular imaging by dynamic nanomechanical mapping. Chem Soc Rev 43:7412. doi:10.1039/c4cs00176a
Acknowledgements
The authors acknowledge funding from the Italian Ministry of Education (FIRB grant RBAP11ETKA-005) and European Regional Development Fund Interreg V-A Italia–Austria 2014–2020 (EXOTHERA ITAT1036).
Author information
Authors and Affiliations
Corresponding author
Additional information
Special issue: Regional Biophysics Conference 2016.
Rights and permissions
About this article
Cite this article
Parisse, P., Rago, I., Ulloa Severino, L. et al. Atomic force microscopy analysis of extracellular vesicles. Eur Biophys J 46, 813–820 (2017). https://doi.org/10.1007/s00249-017-1252-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00249-017-1252-4