Abstract
Background
Ileocolic intussusception occurs when the terminal ileum “telescopes” into the colon. We observed that ileocolic intussusception lengths are similar regardless of location in the colon.
Objective
To examine the uniformity of ileocolic intussusception length and its relationship to colon location, symptom duration and reducibility.
Materials and methods
We retrospectively reviewed ultrasound-diagnosed pediatric ileocolic intussusceptions initially treated with pneumatic reduction at the Mayo Clinic or Texas Children’s Hospital. We recorded demographic, imaging and surgical findings including age, gender, symptom duration, location of the ileocolic intussusception, reducibility with air enema and, if fluoroscopically irreducible, surgical findings.
Results
We identified 119 ileocolic intussusceptions (64% boys), with 81% in the right colon. There was no significant relationship between ileocolic intussusception length and colon location (P=0.15), nor ileocolic intussusception length and symptom duration (P=0.36). Ileocolic intussusceptions were more distal with increasing symptom duration (P=0.016). Successful reductions were unrelated to symptom duration (P=0.84) but were more likely with proximal versus distal locations (P=0.02).
Conclusion
Ileocolic intussusception lengths are relatively uniform regardless of location along the course of the colon where they present. Our findings suggest that most of the apparent distal propagation of ileocolic intussusceptions is not caused by increasing telescoping of small bowel across the ileocecal valve but rather by foreshortening of the right colon. This implies poor cecal fixation and confirms fluoroscopic and surgical observations of cecal displacement from the right lower quadrant with ileocolic intussusceptions. The movement of the leading edge of the ileocolic intussusception during reduction is first due to “relocating” the cecum into the right lower quadrant after which the reduction of small bowel back across the ileocecal valve then occurs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
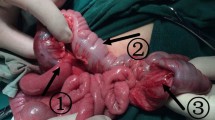
Ileocolic intussusceptions are common pediatric abdominal emergencies with a defining role for pediatric radiologists. The ability to safely and effectively reduce ileocolic intussusceptions with a therapeutic enema is an essential feature of pediatric radiology training and practice. Enema success and perforation rates are frequently monitored and widely reported [1,2,3]. This condition is often described as a telescoping of variable lengths of the distal ileum (intussusceptum) through the ileocecal valve and into the colon (intussuscipiens), and the farther the intussusceptum extends into the colon, the more telescoping of the distal ileum is thought to have occurred. This idea of telescoping as the mechanism of intussusception fits well with what pediatric radiologists observe during fluoroscopic ileocolic intussusception reductions. The leading edge of ileocolic intussusception could be encountered anywhere in the abdomen and could be seen to move from distal to proximal along the expected course of the colon during reductions. However there are reasons to suggest that telescoping does not fully explain what is happening. In 1984, Gilsanz [4] identified cecal and appendiceal displacement out of the right lower quadrant with ileocolic intussusceptions on radiography. This displacement results in an empty right lower quadrant and has been termed Dance sign. For this sign to be present, the cecum and ascending colon must be mobile [5, 6]. In 1911 Waugh [7] first associated incomplete fixation of the right colon with intussusception. Brereton et al. [8] later stated that “mal-fixation of the ileocecal mesentery is a leading factor in allowing the terminal ileum to pass into the cecum.” Moreover, cecal displacement out of the right lower quadrant in ileocolic intussusception is a consistent surgical [9] and imaging finding (Fig. 1).
With the use of US for the pre-enema diagnosis of ileocolic intussusceptions, pediatric radiologists have the opportunity to confirm the findings of cecal and ascending colon displacement in ileocolic intussusceptions and refine our understanding of this disorder. If the traditional dogma for ileocolic intussusception is true, then more distal ileocolic intussusceptions should imply increasing lengths of telescoping small bowel into the colon and should result in longer ileocolic intussusception measurements compared to proximal ileocolic intussusceptions. However we have observed the relative uniform length of ileocolic intussusceptions with ultrasound (US) regardless of their abdominal location. The objective of this study was to confirm this observation and explore its implications.
Materials and methods
We conducted a retrospective review of the medical records and imaging findings of children younger than 18 years diagnosed with ileocolic intussusception at the Mayo Clinic from 2008 to 2016 and at Texas Children’s Hospital from December 2016 to October 2017. Our institutional review boards approved this study, which complied with the Health Insurance Portability and Accountability Act. We recorded demographic, clinical and imaging data including age, gender, symptom duration, and location of the ileocolic intussusception based on the US findings.
The US studies were performed using a combination of curved and linear transducers to optimize intra-abdominal visualization and were performed by dedicated pediatric sonographers at both institutions. The studies consisted of transverse and longitudinal imaging of all four quadrants and in the midline with static images and cine clips documenting full coverage. If an ileocolic intussusception was encountered, multiple images and cine clips in orthogonal planes would be obtained.
We included all children who underwent US for the diagnosis of ileocolic intussusception at the two institutions; specifically, none was excluded because of difficulty obtaining ileocolic intussusception measurements. The length of each ileocolic intussusception was retrospectively measured separately by four pediatric radiologists at the Mayo Clinic (L.A.B., with 25 years’ experience, A.B.K., with 5 years’ experience, N.C.H., with 1 year of experience, and P.G.T., with 7 years’ experience) and two pediatric radiologists at Texas Children’s Hospital (R.C.O., with 9 years’ experience, and N.F.M., with 7 years’ experience), who reviewed all US images and clip stores. These measurements included the bowel wall as well as the invaginated mesentery. The measurements were taken from the single image or cine frame demonstrating the greatest length. If the ileocolic intussusception was curvilinear, several line segments were drawn approximating the arc of the ileocolic intussusception and the separate lengths were added together (Fig. 2). We used the average length measurement for statistical analysis.
Based on the location of the transducer on the abdominal wall indicated by the sonographer, the ileocolic intussusception location was recorded within one of five colonic segments as follows: 1 = right lower quadrant–cecum/proximal ascending colon, 2 = right upper quadrant–hepatic flexure, 3 = right upper quadrant/left upper quadrant–transverse colon, 4 = left upper quadrant–splenic flexure, and 5 = left lower quadrant–descending/sigmoid colon. Group statistics were expressed as mean ± standard deviation (SD) for continuous variables and n (%) for categorical variables. Group comparisons were made using a Student’s t-test for continuous variables and chi square/Fisher exact test for categorical variables. Relationships between length and other variables were assessed using a general linear model. Significance level was set at P≤0.05. Statistical analyses were performed using SAS (SAS Institute, Cary, NC).
Results
We identified a total of 119 ileocolic intussusceptions, 64 at the Mayo Clinic and 55 at Texas Children’s Hospital in 57 and 53 unique children, respectively. Sixty-four percent of ileocolic intussusceptions occurred in boys. The mean age of the children at the Mayo Clinic was 21.8 months (±16.9 months), whereas at Texas Children’s Hospital the mean age was 15.6 months (±13.5 months), P=0.03. Ninety-six (81%) ileocolic intussusceptions were encountered in the proximal colon, locations 1 or 2. Ileocolic intussusception measured longer for children at Texas Children’s Hospital, with a mean length of 5.2 cm, whereas at the Mayo Clinic the mean length was 4.6 cm (P=0.002), and intussusceptions were smaller as the age of the patients increased (P=0.002). Excluding two cases where there was spontaneous reduction before the air enema, the colon location of the ileocolic intussusception at fluoroscopy was within one colon segment, as was indicated with US in 91% of the ileocolic intussusceptions. In the remaining cases, there was progression or regression of two colonic locations. Table 1 lists the intussusceptions according to location and the mean and range lengths by colon segments. Because of the low numbers of cases in segments 4 and 5, we combined these two locations for statistical analysis. The duration of symptoms averaged 33 h for both groups. Inter-observer agreement for measurement of ileocolic intussusception lengths was excellent for both groups of children (kappa=0.88 at both sites).
There was no statistically significant relationship between ileocolic intussusception length and colon location for the entire study group (P=0.15), nor for children 3 years or younger (P=0.17; Fig. 3), nor was there a statistically significant relationship between ileocolic intussusception length and symptom duration (P=0.36; Fig. 4). Ileocolic intussusceptions were encountered more distally along the course of the colon with increasing symptom duration (P=0.002; Fig. 5).
Of the 119 ileocolic intussusceptions, 90 were pneumatically reduced (76%), two reduced spontaneously prior to pneumatic reduction, and 27 could not be reduced pneumatically and required surgery. Of the surgical cases, 11 were irreducible, with a total of 8 lead points (5 Meckel diverticula, 1 perforated appendicitis, 1 small bowel polyp and 1 case of lymphoma). The three remaining cases that were irreducible did not have lead points but required resection because of necrotic bowel. There were no perforations related to pneumatic reduction. The reduction rates were similar for both the Mayo Clinic and Texas Children’s Hospital, 77% and 76%, respectively (P=0.54). Neither symptom duration nor ileocolic intussusception length had an effect on pneumatic reduction success (P=0.84 and P=0.63, respectively), but successful reductions were more likely with proximal ileocolic intussusception (colon locations 1 and 2) versus distal locations (colon locations 3–5; odds ratio [OR]=3.9 [1.5, 10.4]; P=0.02).
Discussion
The observation that ileocolic intussusception length is relatively constant and is independent of the location where it is encountered along the course of the colon has several implications that dispute traditional teaching. Given this relatively constant length of ileocolic intussusceptions, it is likely that most displacement of the ileocolic intussusception from the right lower quadrant is not from increased small-bowel telescoping in to the colon. Our data suggest that after the initial telescoping of a relatively short length of ileum in ileocolic intussusception, the apparent propagation of the intussusception distally is caused by the colon shortening upon itself like an accordion, or invagination of the proximal colon into the more distal colon, like a sock being turned inside out by the toe (Fig. 6). This explanation better matches what is encountered during surgical [10] and fluoroscopic ileocolic intussusception reductions. Initially, there is frequently rapid movement of the ileocolic intussusception proximally toward the right lower quadrant, often in discrete “jumps” as if the colon is elongating haustra by haustra. This rapid movement of the ileocolic intussusception is likely caused by unfolding and elongation of the colon rather than retrograde movement of the telescoped ileum through the ileocecal valve. When the colon has fully lengthened and the cecum has been replaced to the right lower quadrant, the actual reduction of the ileum through the ileocecal valve occurs, and is often more difficult, requiring higher intraluminal pressures. It is likely that the foreshortening and invagination of the colon does not result in sufficient bowel wall thickening to be noticeable with US because we have not observed this on pre-enema ultrasound studies. If it were, the overall length of the ileocolic intussusception would increase the further along the course of the colon the ileocolic intussusception was encountered, but this has not been the case.
Schematic demonstration of Dance sign. a Initial position of ileocolic intussusception in the right lower quadrant with early invagination of the colon. b Further propagation of the leading edge of the ileocolic intussusception to the splenic flexure with increasing invagination and shortening of right colon behind the ileocolic intussusception. (Used with permission of © [2018] Mayo Foundation for Medical Education and Research. All Rights Reserved)
Our data do not support the classic teaching that ileocolic intussusceptions become more distal the longer the child is symptomatic. We found no significant relationship between symptom duration and colonic location. However we did find that distal ileocolic intussusceptions, locations 3–5, were more difficult to reduce than proximal ones, locations 1 and 2. The relationship between symptom duration and the likelihood for successful pneumatic reductions is unclear. Lampl et al. [11] found that radiologic reductions were less successful and surgical intervention more likely with increasing symptom duration. However we are in agreement with Tareen et al. [12] and Flaum et al. [13], who found that increasing symptom duration did not correlate with irreducibility. With this observation, we agree with previous authors [14, 15] that in clinically stable children whose initial pneumatic reduction attempts failed, it is safe to repeat the enema after a brief waiting period. The lack of a relationship between irreducibility and symptom duration leads us to speculate that ileocolic intussusceptions do not become irreducible with increasing symptom duration but might be either reducible or irreducible from their onset or shortly thereafter.
There are two major limitations of our study. First, we retrospectively measured ileocolic intussusception length from the US images. Because of this, the length could have been underestimated, especially for ileocolic intussusceptions that were longer than a single US frame. However, this is unlikely because sonographers at both institutions were instructed to fully document the ileocolic intussusception with clips stores in both the transverse and longitudinal planes and this allowed for retrospective measurements. Second, the length of time children have an intussusception cannot be precisely known. Thus symptom duration is an estimation based on the clinical notes stating, at times imprecisely, the start of the child’s symptoms that led to the emergency department visit.
Conclusion
The traditional understanding of ileocolic intussusception as telescoping of a variable length of ileum into the colon was based on fluoroscopic observations. The US findings of ileocolic intussusceptions indicate that the amount of ileum that crosses through the ileocecal valve is relatively constant and independent of the location where the ileocolic intussusception is encountered in the abdomen. Most displacement of the ileocolic intussusception is not caused by telescoping but by shortening and invagination of the mobile right colon. Our findings dispute the traditional teaching that ileocolic intussusceptions become less likely to be reducible the longer the child has been symptomatic. Although speculative, our findings imply that ileocolic intussusceptions do not become irreducible with time but are either reducible or irreducible at or shortly after their onset.
Change history
25 January 2019
In this article, the fourth author’s name is misspelled. The correct spelling, as shown above, should be “Nadia F. Mahmood.”
References
Katz ME, Kolm P (1992) Intussusception reduction 1991: an international survey of pediatric radiologists. Pediatr Radiol 22:318–322
Hannon E, Williams R, Allan R, Okoye B (2014) UK intussusception audit: a national survey of practice and audit of reduction rates. Clin Radiol 69:344–349
Edwards EA, Pigg N, Courtier J et al (2017) Intussusception: past, present and future. Pediatr Radiol 47:1101–1108
Gilsanz V (1984) Displacement of the appendix in intussusception. AJR Am J Roentgenol 142:407–408
Berdon WE (1995) The diagnosis of malrotation and volvulus in the older child and adult: a trap for radiologists. Pediatr Radiol 25:101–103
O’Neil J (2003) Chapter 54: intussusception. In: O’Neil J, Grosfeld J, Fonkalsrud E (eds) Principles of pediatric surgery. Mosby, St. Louis, pp 527–528
Waugh GE (1911) Referred penile pain in intussusception, with notes of three cases. Lancet 177:1492–1494
Brereton RJ, Taylor B, Hall CM (1986) Intussusception and intestinal malrotation in infants: Waugh's syndrome. Br J Surg 73:55–57
Cera SM (2008) Intestinal intussusception. Clin Colon Rectal Surg 21:106–113
Columbini PM, Scholz S (2012) Chapter 85: intussusception in pediatric surgery. In: Coran AG, Adzick NS, Krummel TM et al (eds) Pediatric surgery e-book. Elsevier, Philadelphia, pp 1093–1110
Lampl BS, Glaab J, Ayyala RS et al (2017) Is intussusception a middle-of-the-night emergency? Pediatr Emerg Care. https://doi.org/10.1097/PEC.0000000000001246
Tareen F, Ryan S, Avanzini S et al (2011) Does the length of the history influence the outcome of pneumatic reduction of intussusception in children? Pediatr Surg Int 27:587–589
Flaum V, Schneider A, Gomes Ferreira C et al (2016) Twenty years' experience for reduction of ileocolic intussusceptions by saline enema under sonography control. J Pediatr Surg 51:179–182
Saxton V, Katz M, Phelan E, Beasley SW (1994) Intussusception: a repeat delayed gas enema increases the nonoperative reduction rate. J Pediatr Surg 29:588–589
Sandler A, Ein S, Connolly B et al (1999) Unsuccessful air-enema reduction of intussusception: is a second attempt worthwhile? Pediatr Surg Int 15:214–216
Acknowledgments
The authors acknowledge the manuscript preparation assistance of Sonia Watson, PhD.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Binkovitz, L.A., Kolbe, A.B., Orth, R.C. et al. Pediatric ileocolic intussusception: new observations and unexpected implications. Pediatr Radiol 49, 76–81 (2019). https://doi.org/10.1007/s00247-018-4259-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-4259-9