Abstract
Brugada syndrome (BrS) is a rare channelopathy associated with sudden cardiac death (SCD). Although outcome data of adult cohorts are well known, information on children are lacking. The aim of the present study was to analyze the clinical profile, treatment approach and long-term outcome of children affected with BrS. After a systematic review of the literature compiled from a thorough database search (PubMed, Web of Science, Cochrane Libary, Cinahl), data from a total of 4 studies which included 262 BrS patients were identified. The mean age of patients was 12.1 ± 5.5, 53.8% males and 19.8% spontaneous BrS type I. 80.2% of patients presented BrS ECG I after receiving sodium channel blockers. 76% of these patients were asymptomatic while only 17.9% suffered from recurrent syncope. Around 1.5% of the patients were admitted due to aborted SCD, and 3% suffered from atrial arrhythmias. Electrophysiological work-up was performed in 132 patients. Induction of ventricular tachycardia/ventricular fibrillation using programmed ventricular stimulation was inducible in 16 patients. 56 children received an ICD. 11 patients received quinidine. An electrical storm was documented in 1 patient. Appropriate shocks occured in 16% of the patients over a median follow-up period of 62.2 (54–64). ICD-related complications were observed in 11 patients (19.6%) with a predominance of inappropriate shocks and lead failure and/or fracture. Although BrS in the childhood is rare, diagnosis and management continues to be challenging. ICD therapy is an effective therapy in high-risk children with BrS, however, with relevant ICD-related complications.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Brugada syndrome (BrS) is an inherited channelopathy associated with a substantial risk of sudden cardiac death (SCD) [1]. BrS is a rare disease with a low prevalence. The diagnosis of could be manifested using sodium channel blocking drugs e.g. ajmaline and/or flecainide. Additionally, fever could increase the risk of ventricular tachyarrhythmias [2]. Therefore the European Society of Cardiology guidelines on diagnostic and management of ventricular tachycardia recommended avoiding fever in BrS patients. ICD implantation is recommended in high-risk BrS patients [3]. However, ICD is not always feasible or adequate for every patient. Although a bevy of data have been reported in children with BrS, informations on clinical profile and long-term outcome remain lacking. Subsequent studies reported that prevalence of BrS in the pediatric population is extremely low (0.0098%) compared with the adult population (0.14% to 0.7%).
ICD implantation is recommended for secondary prevention of SCD in some cases for primary prevention [4]. However, no generally accepted or evidence-based guidelines are available for the specific therapeutic management of BrS in children.
The aim of the present study is to present the clinical demographic, treatment and long-term outcome of BrS in children gathered over the last 20 years based on a systematic literature review.
Methods
Systematic Literature Review
In this pooled analysis, we included all reports on BrS patients at age ≤ 18. A total of 262 BrS patients described in four research papers, were included for our analysis [5,6,7,8]. In these reports, patients were younger than 18 years of age and presented between 1992 and 2018.
BrS was diagnosed according current guidelines for diagnostic, management and treatment of BrS [9,10,11]. This article presents a review of all published cases and/or cohort and a pooled data analysis of the identified patients. Publication dates up to December 2017 were included. A literature search (PubMed, Web of Science, Cochrane Library, Cinahl) was performed by a librarian with limits including publication dates (up to December 2017) and eligibility criteria such as English language and human subjects. 3700 titles/abstracts were screened (GR) considering the clinical profile of patients. 23 articles were identified through a second search (Fig. 1). 19 studies were excluded due to double incidence, outcome of not of interest and only an abstract is behind publications. We used the PICO strategy to identify significant literature by using controlled search items [(Brugada Syndrome) AND (Children) or (Pediatric)] related to our clinical question [12].
Statistics
Data are presented as mean ± SD for continuous variables with a normal distribution, median (interquartile range) for continuous variables with a non-normal distribution, and as frequency (%) for categorical variables. The Kolmogorov–Smirnov test was used to assess normal distribution. Student’s t test and the Mann–Whitney U-test were used to compare continuous variables with normal and non-normal distributions, respectively. The χ2 test or Fisher’s exact test was used to compare categorical variables.
Results
Demographics
The median age of patients was 15.7 (8–18) with a predominance of male patients (55%), Table 1. 80.1% of patients demonstrated BrS type I after use of sodium channel blockers. 76% of the patients were asymptomatic. 17.9% were admitted to the hospital due to recurrent syncope and 1.5% were admitted due to aborted sudden cardiac death (SCD). 3% of patients presented atrial arrhythmias at the time point of diagnosis, Fig. S1a, b. 44.3% of patients have had a family history of SCD.
Syncope was predominantly presented at rest (32.9%). However, 1.1% of patients have suffered from syncope during exercise, Fig. S1c. Using sodium channel blocker none of patients suffered from sustained and/or non-sustained VT.
Electrophysiology Study and Treatment Approach
An electrophysiological study (EP) and PVS was performed in 132 patients. Ventricular tachycardia/ventricular fibrillation was documented in 16 patients (12.1% of cases), Table 2. 72 patients received an ICD and 5 patients were started on hydroquinidine (HQ). Whereas appropriate shocks were documented in 9 patients, 4 patients suffered from inappropriate shocks during a follow-up of 62.2 (54–64) months.
ICD-Related Complications and Management
ICD-related complications were documented in 7 patients. The rate of appropriate ICD shocks (16%) was higher as compared to inappropriate shocks (7.4%) over a follow-up interval of 62.2 (54–64) months, Table 2. Complications are listed as follows: lead failure and fracture (7%), endocarditis (3.6%), hemothorax (2%), and inappropriate shocks (7%), Table 3.
Discussion
Based on the current literature review of BrS in children we found the following:
- (i)
the majority (76%) of patients have no symptoms, however, SCD is the leading cause for admission in 1.5%.
- (ii)
The need to use sodium channel blockers in children might be high to unmask BrS, with no safety concerns
- (iii)
Using EP work-up ventricular tachyarrhythmias are inducible in at least 10% of patients.
- (iv)
The rate of appropriate ICD shocks (16%) was higher as compared to inappropriate shocks (7.4%) over a follow-up interval of 62.2 (54–64) months.
It has been reported that the risk of SCD might be estimated 1.3 to 4.3 per year per 1,00,000 inhabitants. BrS is considered mainly a disease of the young male adult, with a reported mean age at SCD of 40 years.
Recently, published data have presented that BrS is responsible for at least 5% of SCD in patients without structural heart disease [13]. To data, the prevalence of BrS in the childhood remains lacking. It is rarely diagnosed in children and the majority of patients are asymptomatic. Additionally, in addition to the high heterogeneity of BrS the disease penetrance in SCN5A mutation carriers is lower in children with 17% as compared to 100% in adults [14]. Moreover, age-dependent expression of BrS also in response to sodium channel blockers have been reported [15] with an appearance after 5 years of age [16]. All these data might associate with hormone effects and epigenetic confounders [17]. These findings might explain the high percent of asymptomatic. However, these findings are required to be studied using novel experimental studies. Recently, published data showed that human cardiomyocytes from induced-pluripotent stem cells might be a useful model for studying the pathophysiology of inheritable cardiac channelopathies [18, 19] and for drug screening.
The present data show that 3% of patients have suffered from atrial arrhythmias. These finding are not surprising and comparable to data in adult patients, however, with a lower prevalence. This might be explained by the penetrance of BrS in children and not the complete phenotype, which is developing over the years until 30 years of age. Follow-up 12-lead ECG might be helpful to document BrS I ECG and/or symptoms also in asymptomatic patient without BrS I ECG at baseline, since patients may develop BrS I ECG after puberty due to changes of hormone status.
It is well known that BrS is inherited with a presence of a mutation in 20–30% of patients causing a loss of function of sodium channel current predominated by the SCN5A gene. Since the peak sodium current is influencing the conduction, it is not a surprising finding that BrS may present with sinus node dysfunction [20]. These phenomena have been reported in adult BrS patients with a need for pacemaker implantation [21]. In this children cohort, 1.9% of patients received a pacemaker implantation regarding to sinus node dysfunction and or atrioventricular block, which might be higher than reports in adults [21].
Sodium channel blockers are indicated to manifest the diagnosis of BrS triggering type I ECG in suspected patients [22]. It is recommended to infuse ajmaline. However, this is not available in all countries. For this reason alternative drugs may be required such as flecainide or procainamide. Recently published data have shown a lower sensitivity as compared to ajmaline [22]. The value of ajmaline in adults have studied well and presented a positive response in 20–40% of cases with a very low complication rate including ventricular arrhythmias in 0.1–1.5% of tested patients [23]. In our present analysis, we show that the response to ajmaline is up to 80% with no concerns of safety. This large difference in the response rate might be explained by a heterogeneity of the populations. Children included in these studies are selected regarding either a high risk of SCD in their family and/or BrS of their parents. The short half-life of ajmaline and its rate-dependent sodium channel blocking might be an advantage as compared to other sodium channel blockers.
One important data point in BrS is the use of risk stratification strategies. Recently published data have confirmed that EP study with PVS might be a useful approach to identify high-risk BrS patients. However, current guidelines neither discourage nor encourage EP with PVS in BrS patients especially in asymptomatic patients. It has been reported that ventricular tachyarrhythmias were inducible in 50–70% of adult patients. Our present study shows that ventricular tachyarrhythmias with 10% are less induced in children. This could be explained by the low clinical penetrance and not completely developed phenotype in children as compared to adults.
In addition to SCN5A gene different genes have been associated with BrS in the last decade and all together may be responsible for 2% to 5% of diagnosed cases. Despite our understanding of genetic basis of BrS only 20–30% of patients have an affected gene with predominance of SCN5A. In the present cohort of children SCN5A mutations have been found in nearly 71% of patients. This is explained by recruiting these children due to cascade family/genetic screening. Up to date, until now the association of mutations of SCN5A with BrS is studied well. However, appropriate cellular models to understand the pathophysiology of BrS patients with other affected genes remain lacking. Human cardiomyocytes from induced pluripotent stem cells (hiPSC-CM) might be a promising model in the future.
Overall, there is great variation in the reported rate of appropriate ICD therapy in adult BrS patients approximately 5–22%. One of the most significant differences between these studies is the incidence of appropriate therapies in previously asymptomatic individuals. Although several authors report no therapy in this group, during an average follow-up of 2.3 to 7.3 years, other studies report an overall rate of 4% to 13% after an average follow-up of 3.2 to 9.3 years [24,25,26]. A difference in the study population is the most likely explanation for this observation. Our data on appropriate ICD therapy in children (16%) might be consistent with reports on long-term outcome in adults.
Although data on ICD-related complications e.g. inappropriate shocks show a little higher rate as compared to appropriate shocks in adults, our finding in children might be consistent with reported data in adults. We present ICD-related complication rate of at least 19.6% with a predominance of inappropriate shocks and lead fracture.
Based on these data, the diagnosis and management of children with BrS continues to be challenging. Patient’s age, family history, and clinical history should be taken into consideration in an individualized algorithm especially in asymptomatic children. This is recommended due to high rate of ICD-related complications. Children with BrS should be treated in special cardiogenetic centers. Sinus node dysfunction and high degree atrioventricular block might be more presented in children as compared with adults. Therefore, regular ECG follow-ups are also recommended.
Study Limitation
This study provides registry data dominated by retrospective studies and, although the authors clinically evaluated all patients, clinical assessment and treatment algorithm was not uniform and consecutively ICD indications were not homogeneous throughout the study. The number of recruited patients in the present analysis is low. Only SCN5A mutations were evaluated in the present analysis; excluding the possibility of mutations in other BrS-related genes. In addition, despite the obvious advantages of our recruited studies, novel therapeutic approaches such as ventricular ablation was not evaluated. Finally, the role of subcutaneous ICD was not evaluated in the present study.
Conclusions
Although BrS in the childhood is rare, diagnosis and management continues to be challenging. ICD therapy is an effective therapy in high-risk children with BrS, however, with relevant ICD-related complications.
References
Amin AS, Verkerk AO, Bhuiyan ZA, Wilde AA, Tan HL (2005) Novel Brugada syndrome-causing mutation in ion-conducting pore of cardiac Na+ channel does not affect ion selectivity properties. Acta Physiol Scand 185:291–301
Casado-Arroyo R, Berne P, Rao JY, Rodriguez-Manero M, Levinstein M, Conte G, Sieira J, Namdar M, Ricciardi D, Chierchia GB, de Asmundis C, Pappaert G, La Meir M, Wellens F, Brugada J, Brugada P (2016) Long-term trends in newly diagnosed brugada syndrome: implications for risk stratification. J Am Coll Cardiol 68:614–623
Priori SG, Blomstrom-Lundqvist C, Mazzanti A, Blom N, Borggrefe M, Camm J, Elliott PM, Fitzsimons D, Hatala R, Hindricks G, Kirchhof P, Kjeldsen K, Kuck KH, Hernandez-Madrid A, Nikolaou N, Norekval TM, Spaulding C, Van Veldhuisen DJ (2015) 2015 ESC Guidelines for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: the task force for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death of the european society of cardiology (ESC). Endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC). Eur Heart J 36:2793–2867
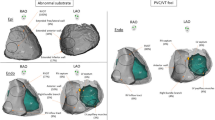
Pappone C, Brugada J, Vicedomini G, Ciconte G, Manguso F, Saviano M, Vitale R, Cuko A, Giannelli L, Calovic Z, Conti M, Pozzi P, Natalizia A, Crisa S, Borrelli V, Brugada R, Sarquella-Brugada G, Guazzi M, Frigiola A, Menicanti L, Santinelli V (2017) Electrical substrate elimination in 135 consecutive patients with Brugada syndrome. Circ Arrhythm Electrophysiol 10:e005053
Andorin A, Behr ER, Denjoy I, Crotti L, Dagradi F, Jesel L, Sacher F, Petit B, Mabo P, Maltret A, Wong LC, Degand B, Bertaux G, Maury P, Dulac Y, Delasalle B, Gourraud JB, Babuty D, Blom NA, Schwartz PJ, Wilde AA, Probst V (2016) Impact of clinical and genetic findings on the management of young patients with Brugada syndrome. Heart Rhythm 13:1274–1282
Sorgente A, Sarkozy A, De Asmundis C, Chierchia GB, Capulzini L, Paparella G, Henkens S, Brugada P (2011) Ajmaline challenge in young individuals with suspected Brugada syndrome. Pacing Clin Electrophysiol 34:736–741
Gonzalez Corcia MC, Sieira J, Sarkozy A, de Asmundis C, Chierchia GB, Hernandez Ojeda J, Pappaert G, Brugada P (2017) Brugada syndrome in the young: an assessment of risk factors predicting future events. Europace 19:1864–1873
Gonzalez Corcia MC, Sieira J, Pappaert G, de Asmundis C, Chierchia GB, La Meir M, Sarkozy A, Brugada P (2018) Implantable cardioverter-defibrillators in children and adolescents With Brugada Syndrome. J Am Coll Cardiol 71:148–157
Antzelevitch C, Brugada P, Borggrefe M, Brugada J, Brugada R, Corrado D, Gussak I, LeMarec H, Nademanee K, Perez Riera AR, Shimizu W, Schulze-Bahr E, Tan H, Wilde A (2005) Brugada syndrome: report of the second consensus conference: endorsed by the Heart Rhythm Society and the European Heart Rhythm Association. Circulation 111:659–670
Antzelevitch C, Yan GX, Ackerman MJ, Borggrefe M, Corrado D, Guo J, Gussak I, Hasdemir C, Horie M, Huikuri H, Ma C, Morita H, Nam GB, Sacher F, Shimizu W, Viskin S, Wilde AAM (2017) J-Wave syndromes expert consensus conference report: Emerging concepts and gaps in knowledge. Europace 19:665–694
Priori SG, Blomstrom-Lundqvist C, Mazzanti A, Blom N, Borggrefe M, Camm J, Elliott PM, Fitzsimons D, Hatala R, Hindricks G, Kirchhof P, Kjeldsen K, Kuck KH, Hernandez-Madrid A, Nikolaou N, Norekval TM, Spaulding C, Van Veldhuisen DJ, Group ESCSD (2015) 2015 ESC Guidelines for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: the task force for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death of the european society of cardiology (ESC). Endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC). Eur Heart J 36:2793–2867
da Costa Santos CM, de Mattos Pimenta CA, Nobre MR (2007) The PICO strategy for the research question construction and evidence search. Rev Lat Am Enfermagem 15:508–511
Papadakis M, Papatheodorou E, Mellor G, Raju H, Bastiaenen R, Wijeyeratne Y, Wasim S, Ensam B, Finocchiaro G, Gray B, Malhotra A, D'Silva A, Edwards N, Cole D, Attard V, Batchvarov VN, Tome-Esteban M, Homfray T, Sheppard MN, Sharma S, Behr ER (2018) The diagnostic yield of brugada syndrome after sudden death with normal autopsy. J Am Coll Cardiol 71:1204–1214
Schulze-Bahr E, Eckardt L, Breithardt G, Seidl K, Wichter T, Wolpert C, Borggrefe M, Haverkamp W (2003) Sodium channel gene (SCN5A) mutations in 44 index patients with Brugada syndrome: different incidences in familial and sporadic disease. Hum Mutat 21:651–652
Makita N, Sumitomo N, Watanabe I, Tsutsui H (2007) Novel SCN5A mutation (Q55X) associated with age-dependent expression of Brugada syndrome presenting as neurally mediated syncope. Heart Rhythm 4:516–519
Beaufort-Krol GC, van den Berg MP, Wilde AA, van Tintelen JP, Viersma JW, Bezzina CR, Bink-Boelkens MT (2005) Developmental aspects of long QT syndrome type 3 and Brugada syndrome on the basis of a single SCN5A mutation in childhood. J Am Coll Cardiol 46:331–337
Matsuo K, Akahoshi M, Seto S, Yano K (2003) Disappearance of the Brugada-type electrocardiogram after surgical castration: a role for testosterone and an explanation for the male preponderance. Pacing Clin Electrophysiol 26:1551–1553
Battrawy I, Lan H, Cyganek L, Zhao Z, Li X, Buljubasic F, Lang S, Yucel G, Sattler K, Zimmermann WH, Utikal J, Wieland T, Ravens U, Borggrefe M, Zhou XB, Akin I (2018) Modeling short QT syndrome using human-induced pluripotent stem cell-derived cardiomyocytes. J Am Heart Assoc 7:e007394
El-Battrawy I, Albers S, Cyganek L, Zhao Z, Lan H, Li X, Xu Q, Kleinsorge M, Huang M, Liao Z, Zhong R, Rudic B, Muller J, Dinkel H, Lang S, Diecke S, Zimmermann WH, Utikal J, Wieland T, Borggrefe M, Zhou X, Akin I (2019) A cellular model of Brugada syndrome with SCN10A variants using human-induced pluripotent stem cell-derived cardiomyocytes. Europace 21:1410–1421
El-Battrawy I, Lang S, Zhao Z, Akin I, Yucel G, Meister S, Patocskai B, Behnes M, Rudic B, Tulumen E, Liebe V, Tiburcy M, Dworacek J, Zimmermann WH, Utikal J, Wieland T, Borggrefe M, Zhou XB (2016) Hyperthermia influences the effects of sodium channel blocking drugs in human-induced pluripotent stem cell-derived cardiomyocytes. PLoS ONE 11:e0166143
Sumiyoshi M, Nakazato Y, Tokano T, Yasuda M, Mineda Y, Nakata Y, Daida H (2005) Sinus node dysfunction concomitant with Brugada syndrome. Circ J 69:946–950
Wolpert C, Echternach C, Veltmann C, Antzelevitch C, Thomas GP, Spehl S, Streitner F, Kuschyk J, Schimpf R, Haase KK, Borggrefe M (2005) Intravenous drug challenge using flecainide and ajmaline in patients with Brugada syndrome. Heart Rhythm 2:254–260
Veltmann C, Wolpert C, Sacher F, Mabo P, Schimpf R, Streitner F, Brade J, Kyndt F, Kuschyk J, Le Marec H, Borggrefe M, Probst V (2009) Response to intravenous ajmaline: a retrospective analysis of 677 ajmaline challenges. Europace 11:1345–1352
Conte G, Dewals W, Sieira J, de Asmundis C, Ciconte G, Chierchia GB, Di Giovanni G, Baltogiannis G, Saitoh Y, Levinstein M, La Meir M, Wellens F, Pappaert G, Brugada P (2014) Drug-induced brugada syndrome in children: clinical features, device-based management, and long-term follow-up. J Am Coll Cardiol 63:2272–2279
Sacher F, Meregalli P, Veltmann C, Field ME, Solnon A, Bru P, Abbey S, Jais P, Tan HL, Wolpert C, Lande G, Bertault V, Derval N, Babuty D, Lacroix D, Boveda S, Maury P, Hocini M, Clementy J, Mabo P, Lemarec H, Mansourati J, Borggrefe M, Wilde A, Haissaguerre M, Probst V (2008) Are women with severely symptomatic brugada syndrome different from men? J Cardiovasc Electrophysiol 19:1181–1185
Sacher F, Probst V, Maury P, Babuty D, Mansourati J, Komatsu Y, Marquie C, Rosa A, Diallo A, Cassagneau R, Loizeau C, Martins R, Field ME, Derval N, Miyazaki S, Denis A, Nogami A, Ritter P, Gourraud JB, Ploux S, Rollin A, Zemmoura A, Lamaison D, Bordachar P, Pierre B, Jais P, Pasquie JL, Hocini M, Legal F, Defaye P, Boveda S, Iesaka Y, Mabo P, Haissaguerre M (2013) Outcome after implantation of a cardioverter-defibrillator in patients with Brugada syndrome: a multicenter study-part 2. Circulation 128:1739–1747
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Research Involving Human and Animal Participants
This article does not contain any studies with animals performed by any of the authors.
Informed Consent
Informed consent is not required regarding the pooled analysis of data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
246_2019_2254_MOESM1_ESM.tif
Electronic supplementary material 1 Fig. S1: A. Demographic of BrS patients with spontaneous and/or in presence of sodium channel blockers or fever. B. Distribution of symptoms in BrS patients at admission. C. Syncope event of patients taking the activity state into consideration. (TIF 24735 kb)
Rights and permissions
About this article
Cite this article
El-Battrawy, I., Roterberg, G., Schlentrich, K. et al. Clinical Profile and Long-Term Follow-Up of Children with Brugada Syndrome. Pediatr Cardiol 41, 290–296 (2020). https://doi.org/10.1007/s00246-019-02254-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-019-02254-5