Abstract
Percutaneous nephrolithotomy (PCNL) is the regular surgery for treating large or complex renal stones. Since its first inception, many variations have come in the approach including the modifications of patient position. The prone position is traditionally used, and subsequently, variations in prone and supine technique have been proposed and assessed over time. In an attempt to provide comprehensive information about the strategy applications of patient’s position, the present review describes the position-related general basis, and provides a literature review of the pros and cons of various positions from a surgical and anaesthetic point of view. Latest evidence has shown the major advantages of supine PCNL compared with standard prone PCNL to be as follows: optimal cardiovascular and airway control; shorter operation time due to lack of the need for repositioning; opportunity for a combined retrograde approach. However, the prone position provides a broader surface area for percutaneous access; a wider space for manipulating the nephroscope and lithotripters; and opportunity for bilateral simultaneous PCNL. To overcome their respective limitations, various positioning modifications have been proposed. However, most reports are based on case series and/or have not obtained their results in a randomized controlled fashion and/or have not been analysed according to stone complexity and particular body status (e.g. obesity, etc.), thereby limiting the ability to make strong recommendations. One important caveat is that endourology training of supine PCNL would increase supine popularization, and the prone ureteroscopic technique would overcome the difficulty of endoscopic combined intrarenal surgery in the prone position. Thereby, adequate training in the different techniques for PCNL is important for optimizing the indications and treatment outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Percutaneous nephrolithotomy (PCNL) is the reference standard treatment for complex and/or large stone burden. Since its first inception in 1976, the progress of PCNL takes place throughout each step of the whole operation including miniaturized instrumentation and access tracts, methods of access puncture guidance, tract dilation, stone disintegration, stone removal, post-operative nephrostomy tube management, and patient position modifications [1]. Although the prone position is traditionally used to perform PCNL, anaesthetic concerns, especially in the morbidly obese or other high-risk patients and the need to reposition the patient during the procedure, were the reasons that initially provoked urologists to explore alternative positions. Second, the advancement of flexible ureteroscopy makes it possible to remove kidney stones in a combined antegrade and retrograde approach, which also prompts the urologist to modify the surgical positions. Since the supine position was initially introduced by Valdivia et al. [2], variations in the prone and supine positions have been proposed and assessed over time [3]. To provide comprehensive information about the strategy of the patient’s position, the present review describes the position-related general basis, and provides a literature review of the pros and cons of various positions from a surgical and anaesthetic point of view. The evidence acquisition was based on the non-systematic literature search in PubMed. We identified original or review articles focused on PCNL position and restricted to those in the English language.
Prone position
Traditionally, retrograde ureteral catheter placement is usually performed in the dorsal lithotomy position, and then the patient is turned to a classic prone position to perform PCNL (Fig. 1a). Rolled saddle is placed under the rib cage/upper abdomen or a Montreal mattress is used (Fig. 1b), to push the kidneys more posteriorly, to obtain more space for accessing the kidney, to minimize the risk of pressure injury and pulmonary compromitation and to facilitate ventilation [4, 5]. Pressure points (knees, feet, forehead, eyes, elbows, fingers) are well padded; the shoulders are abducted to 90°, and the elbows are flexed to 90° and lie on an arm board to prevent brachial plexus injury. To support the head and keep the neck neutrally aligned in the prone PCNL, the head is usually turned to the side on a pillow, or supported by a protective helmet system (Fig. 1b) [5].
The prone position provides a broader surface area for percutaneous access, allows a favourable posterior lower calyx puncture or multiple access tracts, provides a wider space for manipulating the nephroscope and lithotripters, and a good collecting system distension for better vision, and a lower risk of perirenal visceral injury [3, 6, 7]. Particularly in patients with multiple calyx stones or with branched calculi extending into the calyces, endoscope mobility is essential. The prone position also facilitates the upper pole puncture because the postero-medial location of the upper pole is closer to the posterior abdominal wall [8]. With the patient in the prone position, the percutaneous tract to the kidney can be established under fluoroscopy or ultrasound guidance. Furthermore, bilateral simultaneous PCNL has been demonstrated to be safe and effective and this can be done in the prone position [9]. For many years the prone position was the only position used. However, performing PCNL in a prone position also has several disadvantages, such as a relatively longer overall operation time owing to repositioning, possible lesions of the cervical spine or peripheral nerves, ocular injuries, ventilatory compromise, and reduction in cardiac index [1, 6, 7]. Rolling the patient into the prone position must be undertaken with great care as risks include the potential for cervical spine injury, corneal abrasion and increased per orbital pressure, which can result in decreased perfusion to the optic nerve and rarely result in vision loss, as well as brachial plexus compression if the arms are not positioned correctly.
Modifications of the prone position
Modifications of the prone position include the reverse lithotomy position, split-leg, and prone-flexed positions. The reverse lithotomy position was introduced as a standard prone modification to allow simultaneous retrograde access to the upper urinary tract during PCNL (Fig. 1c). This position combined with retrograde approach was first reported in female patients in 1988 [10]. According to the initial description, the patient is placed prone and the patient’s thighs and knees are placed in a moulded plastic cradle. The legs are then abducted at the hips; the caudal end of the operating table is lowered as far as possible. The operator approaching from the caudal end of the table could enter the urethra, bladder, and ureter with the ureteroscope while remaining in a comfortable position. However, this position is seldom used by other groups of urologists.
Then, Grasso et al. [11] further modified the prone position into what they called the “prone split-leg position”. This position allows easier simultaneous percutaneous and transurethral access both in female and male patients. Two soft padded rolls are placed under the thorax and upper abdomen to facilitate ventilation. The lower extremities are placed on two padded adapters in the plane of the operating table that allow the extremities to be split as much as 45°. The genitalia are positioned at the bottom of the operating table, making room for retrograde access. This position obviously decreases the operation time and the need for operation staff to carry out multiple patient transfers. However, performing flexible cystoscopy and ureteroscopy is challenging in the prone position. Recently, Hamamoto et al. demonstrated that flexible ureteroscopy in the prone split-leg position is a viable technique (Fig. 1d, e) [12]. It allows easy insertion of the ureteral sheath and access of the ureteroscope to the renal pelvis.
Another modification of the prone position is the prone-flexed position (Fig. 1f) [8]. This position provides a larger surface area and wider working space. After the patient is placed in the prone position and the operating table flexes 30° to 40° to increase the space (about 2.9 cm) between the 12th rib and the posterior iliac crest. This means that this position provides improved access to the upper pole and more mobility for lower pole PCNL. When in this position, the kidneys are displaced inferiorly in the retroperitoneum. Because of this modification, a supra-11th rib access may be converted to a supra-12th rib or a supra-12th to an infracostal access. However, the prone-flexed modification may further increase difficulty in maintaining anaesthesia, particularly in obese patients or those with cardiovascular or respiratory compromise, due to the airway increased pressures and the decreased cardiac index.
Supine position
Although standard and modified prone positions have been successfully performed, they still have drawbacks related to increased cardiopulmonary risks. To overcome these drawbacks, supine PCNL was introduced. Valdivia and associates first described the supine PCNL in 1987 [2, 13] (Fig. 2a). The patient is placed supine with the side of interest on the lateral extreme of the operating table. The affected flank is elevated with a one 3-L bag of fluid placed under the lumbar fossa. The patient is completely stretched out with extension of the ipsilateral leg. The ipsilateral arm is positioned across the thorax and soft pads are applied to pressure points. Several studies have reported favourable outcomes and the technical benefits of this technique. Theoretically and practically, the advantages of supine PCNL compared with standard prone PCNL are as follows: (1) optimal cardiovascular and airway control, (2) better in high-risk patients with heart failure or in obese patients, (3) shorter operation time due to lack of need for repositioning, (4) opportunity for a combined retrograde approach, (5) better stone fragment washout due to the horizontal dorsal sheath angle, and (6) less radiation exposure to the surgeon’ hands. However, supine PCNL also has several limitations, such as (1) limited space for renal puncture and nephroscope mobility; (2) upper pole calyx puncture is more challenging; (3) a greater challenge for puncture and tract dilation due to high kidney mobility; (4) decreased filling of the collecting system, which is constantly collapsed.
Supine position and its prone modifications. a The original Valdivia supine position [2]. b The modified ‘Valdivia’ position [3]. c The Galdakao-modified Valdivia position [14]. d The Barts technique modified supine position [15]. e, f The Barts flank-free supine position [16]. g The supine oblique position [17]. h The semi-supine position [18]. i The lateral/flank position [21]. j The complete supine position [22]. k, l The modified complete supine position [24]
Modifications of supine position
Various modified positions have recently been proposed. The advantage of these positions is mainly focused on the possibility for simultaneous antegrade and retrograde access to the kidney without repositioning, and with more and more space area for puncture and nephroscope manipulation.
The early modified Valdivia position (Fig. 2b) was described by Valdivia et al. to allow the use of simultaneous retrograde and percutaneous access to the urinary tract, and to preserve all the surgical and anaesthesiological advantages of the previous Valdivia position. The difference is that the legs are flexed in supports, with the ipsilateral leg more elevated and the contralateral more descended, to facilitate the use of a ureteroscope.
The Galdakao-modified Valdivia position (Fig. 2c) renewed the attention of the urological community to supine PCNL, which was described by Ibarluzea et al. [14]. It is a supine decubitus with a lithotomic arrangement of the legs. The supine Valdivia position is the same, the patient lies supine with a 3-L saline bag under the flank or by two separate jelly pillows placed under the thorax and the hip, but the leg of the operated side is extended, while the contralateral one is well abducted, achieving a modified lithotomy position. The ipsilateral arm is bent over the thorax. Advantages for the Galdakao-modified Valdivia position include greater versatility of stone manipulation along the whole upper urinary tract, given the increasing use of combined or subsequent retrograde and percutaneous access to the urinary tract with both rigid and flexible instruments.
The Barts-modified Valdivia position (Fig. 2d) offers a large surface area for access with easy manipulation of the nephroscope, as the trunk is placed at 90° to the operating table [15]. The patient is placed in the lithotomy position with the ipsilateral hemi-pelvis tilted by 45°, supported by a foam wedge. The ipsilateral lower limb is slightly flexed in a ventral direction and follows the lateral rotation of the trunk, while the contralateral lower limb remains fully abducted. However, this position cannot be used for every patient as it requires musculoskeletal mobility and flexibility of the spine. The position results in rotation of the kidney such that the calyces are viewed end on and also the spine lies in the field of the collecting system. Therefore, puncture is difficult to achieve under fluoroscopy alone and often requires ultrasound guidance. Simultaneous retrograde intrarenal surgery is possible but from a position of relative unfamiliarity due to the rotated position. In this position, the kidney is hypermobile. There is therefore the risk that puncture and guidewire manipulation is more difficult.
The Barts flank-free-modified supine position (Fig. 2e, f) was introduced with good exposure of the flank, and also incorporated a lithotomy position, but with less rotation of the torso [16]. The patient is supine with a 15° tilt of the ipsilateral flank made using a saline bag under the rib cage and a gel pad under the pelvis. The ipsilateral arm lies across the chest. The legs are placed in the lithotomy position with the ipsilateral leg relatively extended and the contralateral leg abducted and slightly elevated. This modification increases the distance between the last rib and iliac crest, and moving the cushion from under the flank (as in the original Valdivia position) to under the rib cage provides ample free-flank space for the puncture, dilatation and manipulation of the stone. This manoeuvre allows easy access to the posterior calyx. The kidney is also less mobile and puncture and dilatation are consequently easier. Hence, there is a smaller operating field because the tract is fairly horizontal and on occasion makes the scope more difficult to manoeuvre.
Other various modified positions
In addition, other various modified positions have also been proposed. The supine oblique position (Fig. 2g) [17] is a position without a cushion and consists of placing the patient in the lateral position while the patient leans with his/her back in a 45° angle with the operating table to perform PCNL. No cushion is placed on the side but two 25-cm-length rolls of sheets are padded, one at hip level, the other one at scapula level so that the patient can lean on them. After that, the patient is fixed at trochanter and thorax level with surgical tape, and if necessary, a slight angulation to the table is adjusted to facilitate the approach. The authors commented that this position facilitates the action of the anaesthetist in cases with severe patients, if necessary, and the replacement of the patient to a supine position in a few seconds.
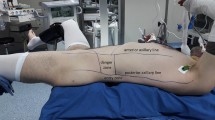
Recently, Xu et al. [18] further modified the semi-supine PCNL (Fig. 2h), and three methods were introduced to set the patients in a 45° semi-supine position. They reported a single centre experience of 542 patients using this technique. They showed a high stone-free rate for either single calculi (92.2%) or for staghorn calculi (72.9%). They also could obtain tracts from the upper (12.1%), middle (63%) and lower calix (24.9%). The authors commented that the semi-supine position could avoid the inconvenience caused by a prone or supine position. The patient is able to remain more comfortable during the procedure, and anaesthesia monitoring is comparable to that of the supine position. In addition, there is enough space (from the anterior axillary line to the subscapular angle line) to set up the PCNL tract as is performed in the prone position. This position also facilitates the ability to achieve an adequate sterile field. However, there is also no readily available retrograde access to the urinary tract and hence combined procedures are not possible.
Kerbl et al. [19] proposed a lateral decubitus position for performing PCNL. Initially, this position is performed in patients who are unable to tolerate anaesthesia in the prone position. Gofrit et al. [20] reported on PCNL in patients in the lateral decubitus flank position in three morbidly obese and kyphotic patients. The lateral position is very familiar to urologists, and may minimize the hemodynamic and respiratory risks and allow for increased patient comfort and safety; however, the lateral position is inconvenient for PCNL guided by a C-arm (Fig. 2i) [21], and the working tract is nearly vertical to the operating table, which limits the evacuation of stone fragments.
Falahatkar et al. [22] reported a complete supine PCNL (Fig. 2j) with no rolled towel under the flank and no change in leg position, and they reported that this technique was safe and feasible in all patients [23]. However, there were drawbacks with supine PCNL noted as well. Due to the restricted exposure of the surgical field, the surface for renal puncture would be quite narrow, thus resulting in obvious restriction in access and angle of entry. Fabio et al. [24] reported a modified complete supine position (Fig. 2k, l). It needed no pads under the flank, and the patient remained in the supine position with the posterior axillary line located just outside the border of the surgical table, and the flank was extended to increase the space between the last rib and the iliac crest. The ipsilateral arm was positioned over the thorax, and the legs were kept straight and positioned slightly apart. It provided a broader area for renal puncture and surgical instrumentation. However, both positions limit the use of a combined approach to remove the kidney stone.
Discussion
Positioning the patient for a surgical procedure is a shared responsibility between the surgeon, the anaesthesiologist, and the nurses in the operating room. The optimal position may require a compromise between the best position for surgical access and the position that the patient can tolerate. The chosen position may result in physiological changes and can result in soft tissue injury (e.g., nerve damage, pressure-induced injury or ulceration, or compartment syndrome).
All positions used for surgery can cause cardiovascular and pulmonary changes. Most commonly, with level prone positioning, there is a reduction in cardiac index, which has been attributed to reduction in venous return to the heart and reduced left ventricular compliance as a result of increased intrathoracic pressure. Abdominal compression in the prone position can cause vena cava compression, reduction in venous return resulting in hypotension, venous stasis, and increased pressure in the epidural venous plexus. It also can cause cephalic displacement of the diaphragm, reduced pulmonary compliance, and increased peak airway pressure [25]. There are minimal horizontal gradients in the vascular system in the supine position. Heart rate (HR) and peripheral vascular resistance are generally lower in the supine position compared with those in the prone positions. There is easy and rapid access to the airway in the supine position. Al-Dessoukey et al. [26] compared the haemodynamic alterations when changing body position from upright to oblique supine position and prone position, and they found significant differences in anaesthesiological parameters (the mean heart rate changed by − 0.82 and + 13.28 beat/minute, the peak air way pressure changed by + 1.08 cm H2O and + 7.56 cm H2O and the mean dropped blood pressure by 2.0 and 14 mmHg in supine and prone positions, respectively). In addition, some particular concerns with the prone position were required including turning prone, torso support, neck position, and protecting the face. However, in the absence of abdominal compression, the prone position may result in beneficial effects on pulmonary function. In healthy volunteers breathing spontaneously, functional residual capacity increases in this position [27].
PCNL is the major method of treating complex renal stones, and is traditionally performed in the prone position [1, 28]. Recent systematic reviews demonstrated that prone positioning is widely applied because it is believed to avoid abdominal visceral injuries, and it allows a wide field for renal puncture and simple execution of multiple access tracts, and imposes no limits on instrument manipulation [3, 6, 7, 28]. However, patients with severe kyphosis, morbidly obese patients, and patients with marginal lung and heart function do not tolerate the prone position well [29].
Some investigators have begun to explore methods of carrying out PCNL in a more comfortable and safe operating position. The supine decubitus position progressed, displaying its advantages over the prone decubitus position [3, 6, 7, 28]. But when PCNL was performed in a supine position, the flank renal puncture area was limited to between the anterior axillary line and the posterior axillary line. The puncture site and angle might also be restricted. Therefore, suggested ways to overcome the original supine limitation would be either to tilt the table toward the contralateral side or to modify the supine position such as lateral decubitus, Galdakao-modified Valdivia position, Barts flank-free-modified supine position, supine oblique position. These modifications can benefit either the simultaneous RIRS to the kidney without repositioning, or the ability and ease of making and dilating multiple tracts, larger space area for nephroscope manipulation as possible [30]. But it is acknowledged that each supine position has its limitations.
There are numerous data comparing the supine PCNLs with the prone position. At the time of writing, five meta-analyses comparing supine and prone PCNL have been published [31,32,33,34,35]. The early two meta-analyses [33, 35] included two prospective RCTs and two case–control studies and showed that the supine position was associated with a significantly shorter operating time than the prone position with no difference in success rate, complication, transfusion rate, and fever rate. The rates of colonic injury, pelvic perforation and failed access were also comparable between the supine and prone positions. These data favour the supine position as an alternative option for the removal of renal calculi by PCNL. Three years later in 2014, Zhang et al. [32] included more studies in their meta-analysis and found that the supine position was still associated with a significantly shorter operation time but with a lower stone-free rate than that in the prone position. There was no difference in hospital stay and complication rate. Interestingly, Yuan et al. [34] performed this meta-analysis and included 13 studies (six randomized controlled trials and seven retrospective studies). This analysis confirmed that the supine position resulted in a lower stone-free rate and a shorter operation time, but they also showed a lower incidence of blood transfusions in the supine groups and no difference in total complications. However, the most recent meta-analysis updated by Falahatkar et al. [31] concluded that supine PCNL had similar stone-free rates, operation time, and hospital stay relative to prone PCNL. However, the supine position has the advantage of less fever and need for blood transfusion. While familiarity with the procedure performed in the supine or prone position may affect the success and efficiency of the operation, it is important to note that there was a high degree of heterogeneity of the studies in these analyses as the majority of the patients included in this analysis were from the CROES database. Furthermore, there is a paucity of data comparing the modified supine to the prone position [36,37,38], and most reports about position modifications are case series and/or are not analysed according to stone complexity and special body status (obese, age, high-risk patients, etc.) [28, 39,40,41], thereby limiting the ability to make strong recommendations and the current literature has no clear consensus on which position is superior.
Conclusions
Even though various positioning modifications have been proposed over years, neither the American Urological Association nor the European Association of Urology guidelines give recommendations on the best position during PCNL. Each modification has its strengths and weaknesses. Well-designed, randomized, multi-institutional studies are certainly needed to better understand the indications for these modified position techniques before considering which of them is the superior position with the potential for replacing conventional prone PCNL. There is one important caveat. Endourology training of supine PCNL would increase supine popularization, and the prone ureteroscopic technique could overcome the difficulty of endoscopic combined intrarenal surgery in the prone position. Thereby, adequate training in the different techniques for PCNL is important to optimize indications for the right patient and stone burden, and then be benefit for treatment outcomes.
References
Ghani KR, Andonian S, Bultitude M et al (2016) Percutaneous nephrolithotomy: update, trends, and future directions. Eur Urol 70:382–396. https://doi.org/10.1016/j.eururo.2016.01.047
Valdivia Uría JG, Lachares Santamaría E, Villarroya Rodríguez S et al (1987) [Percutaneous nephrolithectomy: simplified technic (preliminary report)]. Arch Esp Urol 40:177–180
Karaolides T, Moraitis K, Bach C et al (2012) Positions for percutaneous nephrolithotomy: thirty-five years of evolution. Arab J Urol 10:307–316. https://doi.org/10.1016/j.aju.2012.06.005
Turner CD, Anderson J, Gerber GS (2000) Improved patient positioning for percutaneous nephroscopic procedures using a surgical saddle. J Urol 163:199–200
Papatsoris A, Masood J, El-Husseiny T et al (2009) Improving patient positioning to reduce complications in prone percutaneous nephrolithotomy. J Endourol 23:831–832. https://doi.org/10.1089/end.2008.0611
Mak DK-C, Smith Y, Buchholz N, El-Husseiny T (2016) What is better in percutaneous nephrolithotomy—prone or supine? A systematic review. Arab J Urol 14:101–107. https://doi.org/10.1016/j.aju.2016.01.005
Patel RM, Okhunov Z, Clayman RV, Landman J (2017) Prone versus supine percutaneous nephrolithotomy: what is your position? Curr Urol Rep 18:26. https://doi.org/10.1007/s11934-017-0676-9
Ray AA, Chung D-G, Honey RJD (2009) Percutaneous nephrolithotomy in the prone and prone-flexed positions: anatomic considerations. J Endourol 23:1607–1614. https://doi.org/10.1089/end.2009.0294
Desai M, Grover R, Manohar T, Ganpule A (2007) Simultaneous bilateral percutaneous nephrolithotomy: a single-center experience. J Endourol 21:508–514. https://doi.org/10.1089/end.2006.0401
Lehman T, Bagley DH (1988) Reverse lithotomy: modified prone position for simultaneous nephroscopic and ureteroscopic procedures in women. Urology 32:529–531
Grasso M, Nord R, Bagley DH (1993) Prone split leg and flank roll positioning: simultaneous antegrade and retrograde access to the upper urinary tract. J Endourol 7:307–310. https://doi.org/10.1089/end.1993.7.307
Hamamoto S, Yasui T, Okada A et al (2014) Developments in the technique of endoscopic combined intrarenal surgery in the prone split-leg position. Urology 84:565–570. https://doi.org/10.1016/j.urology.2014.04.020
Valdivia Uría JG, Valle Gerhold J, López López JA et al (1998) Technique and complications of percutaneous nephroscopy: experience with 557 patients in the supine position. J Urol 160:1975–1978
Ibarluzea G, Scoffone CM, Cracco CM et al (2007) Supine Valdivia and modified lithotomy position for simultaneous anterograde and retrograde endourological access. BJU Int 100:233–236. https://doi.org/10.1111/j.1464-410X.2007.06960.x
Papatsoris AG, Zaman F, Panah A et al (2008) Simultaneous anterograde and retrograde endourologic access: “the Barts technique”. J Endourol 22:2665–2666. https://doi.org/10.1089/end.2008.0283
Bach C, Goyal A, Kumar P et al (2012) The Barts “flank-free” modified supine position for percutaneous nephrolithotomy. Urol Int 89:365–368. https://doi.org/10.1159/000341430
Arrabal-Polo MA, Arrabal-Martin M, Saz T, Paiz P (2011) Emergency percutaneous nephrostomy in supine-oblique position without cushion. Urol Res 39:521–522. https://doi.org/10.1007/s00240-011-0384-8
Xu K-W, Huang J, Guo Z-H et al (2011) Percutaneous nephrolithotomy in semisupine position: a modified approach for renal calculus. Urol Res 39:467–475. https://doi.org/10.1007/s00240-011-0366-x
Kerbl K, Clayman RV, Chandhoke PS et al (1994) Percutaneous stone removal with the patient in a flank position. J Urol 151:686–688
Gofrit ON, Shapiro A, Donchin Y et al (2002) Lateral decubitus position for percutaneous nephrolithotripsy in the morbidly obese or kyphotic patient. J Endourol 16:383–386. https://doi.org/10.1089/089277902760261437
Basiri A, Ziaee SAM, Nasseh H et al (2008) Totally ultrasonography-guided percutaneous nephrolithotomy in the flank position. J Endourol 22:1453–1457. https://doi.org/10.1089/end.2007.0391
Falahatkar S, Moghaddam AA, Salehi M et al (2008) Complete supine percutaneous nephrolithotripsy comparison with the prone standard technique. J Endourol 22:2513–2517. https://doi.org/10.1089/end.2008.0463
Falahatkar S, Farzan A, Allahkhah A (2011) Is complete supine percutaneous nephrolithotripsy feasible in all patients? Urol Res 39:99–104. https://doi.org/10.1007/s00240-010-0287-0
Vicentini FC, Torricelli FCM, Mazzucchi E et al (2013) Modified complete supine percutaneous nephrolithotomy: solving some problems. J Endourol 27:845–849. https://doi.org/10.1089/end.2012.0725
Palmon SC, Kirsch JR, Depper JA, Toung TJ (1998) The effect of the prone position on pulmonary mechanics is frame-dependent. Anesth Analg 87:1175–1180
Al-Dessoukey AA, Moussa AS, Abdelbary AM et al (2014) Percutaneous nephrolithotomy in the oblique supine lithotomy position and prone position: a comparative study. J Endourol 28:1058–1063. https://doi.org/10.1089/end.2014.0078
Lumb AB, Nunn JF (1991) Respiratory function and ribcage contribution to ventilation in body positions commonly used during anesthesia. Anesth Analg 73:422–426
de la Rosette JJMCH., Tsakiris P, Ferrandino MN et al (2008) Beyond prone position in percutaneous nephrolithotomy: a comprehensive review. Eur Urol 54:1262–1269. https://doi.org/10.1016/j.eururo.2008.08.012
Pelosi P, Croci M, Calappi E et al (1995) The prone positioning during general anesthesia minimally affects respiratory mechanics while improving functional residual capacity and increasing oxygen tension. Anesth Analg 80:955–960
Kumar P, Bach C, Kachrilas S et al (2012) Supine percutaneous nephrolithotomy (PCNL): “in vogue” but in which position? BJU Int 110:E1018–E1021. https://doi.org/10.1111/j.1464-410X.2012.11188.x
Falahatkar S, Mokhtari G, Teimoori M (2016) An update on supine versus prone percutaneous nephrolithotomy: a meta-analysis. Urol J 13:2814–2822
Zhang X, Xia L, Xu T et al (2014) Is the supine position superior to the prone position for percutaneous nephrolithotomy (PCNL)? Urolithiasis 42:87–93. https://doi.org/10.1007/s00240-013-0614-3
Wu P, Wang L, Wang K (2011) Supine versus prone position in percutaneous nephrolithotomy for kidney calculi: a meta-analysis. Int Urol Nephrol 43:67–77. https://doi.org/10.1007/s11255-010-9801-0
Yuan D, Liu Y, Rao H et al (2016) Supine versus prone position in percutaneous nephrolithotomy for kidney calculi: a meta-analysis. J Endourol 30:754–763. https://doi.org/10.1089/end.2015.0402
Liu L, Zheng S, Xu Y, Wei Q (2010) Systematic review and meta-analysis of percutaneous nephrolithotomy for patients in the supine versus prone position. J Endourol 24:1941–1946. https://doi.org/10.1089/end.2010.0292
Jones MN, Ranasinghe W, Cetti R et al (2016) Modified supine versus prone percutaneous nephrolithotomy: surgical outcomes from a tertiary teaching hospital. Investig Clin Urol 57:268–273. https://doi.org/10.4111/icu.2016.57.4.268
De Sio M, Autorino R, Quarto G et al (2008) Modified supine versus prone position in percutaneous nephrolithotomy for renal stones treatable with a single percutaneous access: a prospective randomized trial. Eur Urol 54:196–202. https://doi.org/10.1016/j.eururo.2008.01.067
Curry D, Srinivasan R, Kucheria R et al (2017) Supine percutaneous nephrolithotomy in the galdako-modified valdivia position: a high-volume single center experience. J Endourol. https://doi.org/10.1089/end.2017.0064
Okeke Z, Smith AD, Labate G et al (2012) Prospective comparison of outcomes of percutaneous nephrolithotomy in elderly patients versus younger patients. J Endourol 26:996–1001. https://doi.org/10.1089/end.2012.0046
Mazzucchi E, Vicentini FC, Marchini GS et al (2012) Percutaneous nephrolithotomy in obese patients: comparison between the prone and total supine position. J Endourol 26:1437–1442. https://doi.org/10.1089/end.2012.0257
Manohar T, Jain P, Desai M (2007) Supine percutaneous nephrolithotomy: effective approach to high-risk and morbidly obese patients. J Endourol 21:44–49. https://doi.org/10.1089/end.2006.0212
Acknowledgements
We thank Professor William G. Robertson for the helpful comments and careful revise work on the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Zhao, Z., Fan, J., Liu, Y. et al. Percutaneous nephrolithotomy: position, position, position!. Urolithiasis 46, 79–86 (2018). https://doi.org/10.1007/s00240-017-1019-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00240-017-1019-5