Abstract
Background
Umbilicoplasty is an important surgical procedure in abdominoplasty, regardless of the technique used. An unaesthetic umbilicus often irreversibly affects surgical outcomes. This study describes the experience of our team with the subdermal neo-umbilicoplasty technique and assesses patient satisfaction with the appearance of the new umbilicus.
Methods
Fifty-eight patients with abdominal deformity underwent abdominoplasty with subdermal neo-umbilicoplasty. Patients were followed up for at least 1 year with photographic documentation, assessment of patient satisfaction, and evaluation of eventual postoperative complications.
Results
Postoperative complications included one case of shallow umbilicus, four cases of superficial necrosis, and one case of midline deviation. No patient required surgical revision. There was a high level of patient satisfaction with the natural-looking umbilicus.
Conclusions
Subdermal neo-umbilicoplasty resulted in low postoperative complications and provided a new, natural-looking umbilicus without external scars.
Level of evidence: Level IV, therapeutic study
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Traditional abdominoplasty is a multi-stage procedure, and umbilicoplasty is one of the most challenging tasks. The umbilicus is the only natural scar on the body and an important anatomical and esthetic feature of the abdominal wall. It usually lies at the intersection of the xiphoid-pubic line and the line joining the anterior iliac crests. Slight variations in height and laterality of the umbilicus are normal and depend on the biotype [1,2,3]. The umbilicus is a small anatomical landmark with vertical orientation that may undergo changes associated with aging, weight gain, and pregnancy, which may contribute to a widened appearance with a transverse orientation [4].
Several surgical techniques have been used for umbilical reconstruction, especially the traditional umbilical transposition, in which the umbilicus is reattached to the dermal-fat flap [2,3,4,5,6,7,8,9,10,11,12]. The high rate of unesthetic results obtained with the traditional technique of umbilical transposition is related to alterations in the healing process. Hypertrophic scars, wide scars, partial or total necrosis, and umbilical stenosis are common postoperative complications that may affect the esthetic outcome of a well-executed abdominoplasty [3].
The aim of this study was to describe the experience of our team with the subdermal neo-umbilicoplasty technique, in which the new umbilicus is created by applying a subdermal tension to the abdominal flap to form an esthetic depression. Patient satisfaction with the appearance of the new umbilicus was also assessed.
Patients and methods
This study was performed in accordance with the Resolution 196/96 of the Brazilian National Health Council (CNS) on research involving human beings and with the ethical standards of the 1964 Declaration of Helsinki and its subsequent amendments. Written informed consent was obtained from all individual participants prior to their inclusion in the study; anonymity was assured.
Fifty-eight consecutive patients with abdominal deformity seeking abdominoplasty were selected from private and institutional practice between July 2008 and May 2014 to participate in the study.
According to the classification of Nahas, abdominal wall deformities can be categorized based on excessive subcutaneous tissue and skin as type 0, excess of subcutaneous with little or no excess skin; type I, mild excess skin and high umbilical scar; type II, mild/moderate excess of skin and a high or well-positioned umbilical scar; and type III, severe excess of skin [13]. All patients had type III abdominal deformity for which conventional abdominoplasty is indicated [13].
Nahas [14] classified myoaponeurotic deformities as type A, presence of diastasis recti secondary to pregnancy; type B, laxicity of the lateral and inferior abdominal wall after approximation of the anterior rectus sheaths; type C, congenital lateral insertion of the rectus abdominis muscles; and type D, diastasis recti and poor waistline definition. All patients had type A abdominal deformity, for which plication of the rectus abdominis sheath was indicated [14].
Smokers and patients with comorbidities were not included in the study. All patients were operated on by the same surgeon.
Surgical procedure
The umbilical reconstruction technique used in this study was based on procedures described by Amud [11] and Nogueira [12]. The essence of this technique is to create a skin depression by attaching a small subdermal area on the abdominal flap corresponding to the location of the new umbilicus to the aponeurosis, mimicking the original umbilicus, without the need for incisions in the abdominal flap.
All surgeries were conducted on patients under general anesthesia.
First, the abdominal dermal fat flap was raised toward the rib cage, extending to the xiphoid process. The umbilical pedicle was dissected from its origin (Fig. 1).
All patients had diastasis recti. The remaining orifice of the umbilical stalk was closed with 3-0 nylon suture (Mononylon, Ethicon Inc., Summerville, NJ, USA). Plication of the anterior rectus sheath was performed using double 2-0 polypropylene sutures (Fig. 2).
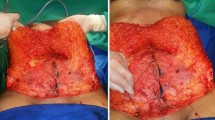
The margin of the abdominal flap was temporarily sutured to the midline of the pubic area to help define the position of the new umbilicus (Fig. 3). A needle was used to inject methylene blue to mark the central point of the new umbilicus in the dermis, adipose tissue, and underlying aponeurosis (Figs. 4 and 5).
The flap was everted and a cross-shaped incision was made in the adipose tissue to expose a circular portion of the deep dermis, about 1 cm in diameter, by blunt undermining of the skin flap (Fig. 6). Six peripheral points were marked on the deep dermis around the central point, representing the corners of a hexagon, with its long axis (defined by two opposing points) aligned with the midline in the vertical direction (Fig. 6). The points were used as references to attach the deep dermis to the midline of the abdominal wall. At this moment, it is necessary to verify the actual position of the midline on the abdominal wall, which may not correspond to the plication line. The six peripheral points and the central point were mirrored to the abdominal wall and the new umbilicus was secured to the aponeurosis with simple 3-0 polypropylene sutures (Fig. 7). Three 2-0 polyglactin quilting sutures were placed around the new umbilicus, concentrically attaching adipose tissue to the created depression [12]. This procedure results in a skin depression firmly secured to the midline of the abdominal wall (Fig. 8). The abdominal flap was sutured to the aponeurosis with 10 to 15 quilting sutures, depending on the size of the undermined area, which was drained with a 4.8-mm silicone drain for 5 days. The wound was closed in layers using 2-0, 3-0, or 4-0 polyglactin sutures in the subcutaneous tissue and 4-0 poliglecaprone 25 sutures in the subdermal and intradermal planes.
All patients were observed in the hospital for 24 h, and a light-compression abdominal binder was used for 30 days. Care should be taken not to over-compress the abdominal region, as an excessive compression may lead to the formation of a cicatricial retraction in the midline supraumbilical region. Patients were instructed to walk with the trunk semi-flexed for a week, after which they were allowed to walk with the trunk in a straight-up position. Patients were also instructed to avoid abdominal exertion and vigorous rotation of the trunk for 30 days.
The patients were followed up in outpatient facilities for at least 12 months. Photographs were taken preoperatively and at 3, 6, and 12 months postoperatively.
Patient satisfaction following abdominoplasty combined with subdermal umbilicoplasty was assessed at the 12-month follow-up using a 5-point Likert-type scale [15], ranging from extremely dissatisfied (1) to extremely satisfied (5), as shown in Fig. 9.
Results
Fifty-six of the 58 patients were women, the mean age was 42.98 ± 10.38 years (median, 44; range, 21–64), and the mean body mass index (BMI) was 27.06 ± 4.25 kg/m2 (median, 26.5; range, 19.71–41.52) (Table 1).
Typical examples of the results obtained after abdominoplasty with umbilical reconstruction using the subdermal technique are shown in Figs. 10, 11, and 12.
Postoperative complications occurred in six patients and included one case of shallow umbilicus (Fig. 13), two cases of superficial necrosis of the distal end of the umbilicus, two cases of superficial linear necrosis caused by skin stretching (Fig. 14), and one case of midline deviation (Fig. 15). No patient required surgical revision (Table 2).
All 58 patients responded to the satisfaction survey 1 year or more after surgery. The mean satisfaction scores were 4.55 for abdominoplasty outcome and 4.59 for the umbilical scar, showing a high level of satisfaction with both the new umbilicus and abdominoplasty results (Table 3).
Discussion
Although the umbilicus represents only a small portion of the abdominal flap, it plays an essential role in the abdominoplasty outcome and should not be considered a feature of minor importance. An unesthetic umbilicus may jeopardize the outcome of a well-executed abdominoplasty, creating sequelae difficult to solve, and sometimes irreversible results.
Subdermal neo-umbilicoplasty is a simple, easily reproducible technique that can be part of most abdominoplasty procedures where the original umbilicus is lost, including traditional abdominoplasty, post-bariatric surgeries, and repair procedures following laparotomy.
The new umbilicus is placed at the intersection of the xiphoid-pubic line and the line joining the anterior iliac crests [1]. However, because the original umbilicus is excised in this technique, it is possible to vary the position of the new umbilicus according to the characteristics of each patient biotype.
After the abdominal flap is everted, the adipose tissue is incised, avoiding as much as possible its resection around the exposed dermis. The resection of adipose tissue may reduce the depth of the created umbilical depression, leaving the new umbilicus with a shallow appearance (Fig. 13). The attachment of adipose tissue around the umbilical depression also increases its depth, preventing a shallow umbilicus. These sutures also create a circular-shaped halo, contributing to the protection and stability of the skin depression and reducing flap displacement in the early postoperative period. This is particularly important in underweight patients with a thin layer of subcutaneous adipose tissue. A shallow umbilicus may require surgical revision to be corrected with fat grafting.
Preoperative peri-umbilical hernia is frequently present in patients undergoing abdominoplasty. Herniorrhaphy combined with traditional umbilical transposition is associated with increased postoperative umbilical necrosis, especially in patients with diabetes and smoking habit [16]. Subdermal neo-umbilicoplasty provides an additional benefit in these cases [16]. Postoperative superficial necrosis (Fig. 14) can be prevented by reducing the tension on the abdominal flap below the new umbilicus. In cases of superficial necrosis, excessive circular compression should be avoided in the immediate postoperative period and conservative treatment with healing ointments can be used.
In order to prevent midline deviation (Fig. 15), the new umbilicus should be properly positioned along the aponeurosis of the rectus abdominis muscle. It is necessary to verify the actual position of the midline on the abdominal wall before defining the attachment position of the umbilicus to the aponeurosis, because the plication line not always corresponds to the midline due to changes in abdominal wall compliance resulting from previous pregnancy or laparotomy. Cases of midline deviation may require surgical revision.
According to Craig et al. [6], the ideal umbilicus should be small and have a vertical orientation, a small superior hooding, and no visible scar. The subdermal neo-umbilicoplasty technique results in a natural-looking umbilicus. Its main advantage over the traditional umbilical transposition technique is the absence of postoperative scars, allowing the use of bikini bathing suits and eliminating scar revision procedures, which is a major source of postoperative complications [3].
Conclusion
Subdermal neo-umbilicoplasty is an easily reproducible surgical technique that provides a natural-looking umbilicus without a scar and is associated with high reported levels of patient satisfaction.
References
Dobou R, Ousterhout DK (1978) Placement of the umbilicus in an abdominoplasty. Plast Reconstr Surg 64:291–293
Dogan T (2010) Umbilicoplasty in abdominoplasty: a new approach. Ann Plast Surg 64(6):718–721
Bruekers SE, van der Lei B, Tan TL, Luijendijk RW, Stevens HP (2009) “Scarless” umbilicoplasty: a new umbilicoplasty technique and a review of the English language literature. Ann Plast Surg 63(1):15–20
Malic CC, Spyrou GE, Hough M, Fourie L (2007) Patient satisfaction with two different methods of umbilicoplasty. Plast Reconstr Surg 119(1):357–361
Franco T, Franco D (1999) Neoomphaloplasty: an old and new technique. Aesthetic Plast Surg 23(2):151–154
Craig SB, Faller MS, Puckett CL (2000) In search of the ideal female umbilicus. Plast Reconstr Surg 105(1):389–392
Lee MJ, Mustoe TA (2002) Simplified technique for creating a youthful umbilicus in abdominoplasty. Plast Reconstr Surg 109(6):2136–2140
Pardo Mateu L, Chamorro Hernandez JJ (1997) Neo-umbilicoplasty through a purse-string suture of three defatted flaps. Aesthetic Plast Surg 21(5):349–351
Pfulg M, Van de Sijpe K, Blondeel P (2005) A simple new technique for neo-umbilicoplasty. Br J Plast Surg 58(5):688–691
Rozen SM, Redett R (2007) The two-dermal-flap umbilical transposition: a natural and aesthetic umbilicus after abdominoplasty. Plast Reconstr Surg 119(7):2255–2262
Amud RJM (2008) Omphaloplasty without scars. Rev Bras Cir Plast 23:37–40
Nogueira DSC (2008) Routine neoomphaloplasty during abdominoplasties. Rev Bras Cir Plast 23:207–213
Nahas FX (2001) A pragmatic way to treat abdominal deformities based on skin and subcutaneous excess. Aesthetic Plast Surg 125:365–371
Nahas FX (2001) An aesthetic classification of the abdomen based on the myoaponeurotic layer. Plast Reconstr Surg 108(6):1787–1795
Likert R (1932) A technique for the measurement of attitudes. Arch Psychol 140:1–55
McKnight CL, Fowler JL, Cobb WS, Smith DE, Carbonell AM (2012) Concomitant sublay mesh repair of umbilical hernia and abdominoplasty. Can J Plast Surg 20(4):258–260
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
There was no external funding for this study.
Conflict of interest
Alejandro Povedano, Gabriel Salum D’Alessandro, Lauren Klas Iurk Leme dos Santos, Alexandre Mendonça Munhoz, Rolf Gemperli, and João Carlos de Sampaio Góes declare that they have no conflict of interest.
Ethical approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments. However, for this type of retrospective study formal consent from a local ethics committee is not required.
Patient consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Povedano, A., D’Alessandro, G.S., dos Santos, L.K.I.L. et al. Subdermal neo-umbilicoplasty in abdominoplasty. Eur J Plast Surg 41, 335–344 (2018). https://doi.org/10.1007/s00238-017-1374-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-017-1374-z