Abstract
Purpose
In multiple sclerosis (MS), how brain functional changes relate to clinical conditions is still a matter of debate. The aim of this study was to investigate how functional connectivity (FC) reorganization at three different scales, ranging from local to whole brain, is related to tissue damage and disability.
Methods
One-hundred-nineteen patients with MS were clinically evaluated with the Expanded Disability Status Scale and the Multiple Sclerosis Functional Composite. Patients and 42 healthy controls underwent a multimodal 3 T MRI, including resting-state functional MRI.
Results
We identified 16 resting-state networks via independent component analysis and measured within-network, between-network, and whole-brain (global efficiency and degree centrality) FC. Within-network FC was higher in patients than in controls in default mode, frontoparietal, and executive-control networks, and corresponded to low clinical impairment (default mode network versus Expanded Disability Status Scale r = − 0.31, p < 0.01; right frontoparietal network versus Paced Auditory Serial Addition Test r = 0.33, p < 0.01). All measures of between-network and whole-brain FC, except default mode network global efficiency, were lower in patients than in controls, and corresponded to high disability (i.e., basal ganglia global efficiency versus Timed 25-Foot Walk r = − 0.25, p < 0.03; default mode global efficiency versus Expanded Disability Status Scale r = − 0.44, p < 0.001). Altered measures of within-network, between-network, and whole-brain FC were combined in functional indices that were linearly related to disease duration, Paced Auditory Serial Addition Test and lesion load and non-linearly related to Expanded Disability Status Scale.
Conclusion
We suggest that the combined evaluation of functional alterations occurring at different levels, from local to whole brain, could exhaustively describe neuroplastic changes in MS, while increased within-network FC likely represents adaptive compensatory processes, decreased between-network and whole-brain FC likely represent loss of functional network integration consequent to structural disruption.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Multiple sclerosis (MS) is a chronic disease of the central nervous system characterized by demyelination, progressive oligodendrocyte and neuronal loss, and axonal degeneration that determine functional and structural disconnection and neuroplastic changes at different scales. Adaptive mechanisms of neuroplasticity, scaling from synaptic transmission and gene expression to structural and functional reorganization of large-scale connectivity, may limit the clinical effects of brain damage, in terms of disability [1].
Large-scale changes in brain function can be investigated by functional magnetic resonance imaging (fMRI) and may partially represent neuroplasticity processes. Several fMRI studies have interpreted functional changes in MS so far, i.e., the increased activation and/or increased connectivity in the initial phases of the disease, as a compensatory neuroplasticity mechanism [2,3,4]. However, non-univocal results have been reported in the literature, i.e., resting state functional connectivity (FC) showed distributed pattern of abnormalities even within the same group of patients (e.g., [5]), suggesting that changes in functional brain connectivity represent mechanisms of either adaptive or maladaptive plasticity [6,7,8] and contribute to a wide spectrum of clinical manifestations [5]. Indeed, increased FC was found to correlate negatively with lesion burden in pediatric patients [9], as in a compensatory attempt. Conversely, in adult patients, decreased FC was found to negatively correlate with lesion load and disability, as well as to positively correlate with neurophsycological measures [5], suggesting a FC exhaustion related to MS. Also, an association between worst cognitive performance and increment of thalamocortical FC was observed in MS patients suggesting a maladaptive mechanism [8].Moreover, cognitive impaired patients showed increased FC negatively correlating with cognitive performances and volumes, while positively correlating with disability [10,11,12].
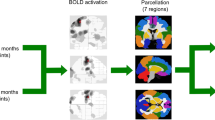
Differences in patients’ selection and methodology may have contributed to results’ discrepancy. Heterogeneous approaches have been developed to analyze resting state (rs) fMRI time series, with a priori assumptions, data-driven or graph theory methods, to characterize FC at different scales of resting state networks (RSNs) [13]. Resting state FC within each RSN, as identified by the independent component analysis (ICA), may represent a first level (single-network scale), the communication between pairs of RSNs may represent a second level (network-pairs scale), and, lastly, brain topological properties, as evaluated by graph theory, may represent a higher level of global organization of FC (whole-brain scale).
Previous studies investigated one single FC scale at a time and fail in drawing a complete picture of the phenomenon, since different scales may represent different aspects of brain connectivity that may occur all at the same time.
We hypothesized that changes of FC may simultaneously occur in the brain of MS patients at every level and that FC changes that occur at single-network, between-network, and whole-brain scales are variously related to tissue damage, cognitive impairment, and disability in MS. We further hypothesized that brain reorganization in MS may be represented by a combined multiscale FC measure that could be not linearly related to disability.
In this study, we investigated FC at these three different scales in a clinically defined sample of MS patients and a group of healthy control subjects (HS) to obtain a comprehensive multiscale description of functional organization and to determine the relationship between the combined FC changes and disability.
Methods
Sample selection
Patients attending the MS center of S. Andrea Hospital (Rome, Italy) were recruited from May 2011 to June 2015. Inclusion criteria were the following: age between 18 and 65 years; righthandedness according to Edinburgh test; diagnosis of MS according to revised McDonald criteria [14]; clinical history on medical record; ability to sign written informed consent. Exclusion criteria were use of steroids and introduction/modification of any medication in the previous month; beginning of disease-modifying or symptomatic treatments 3 months prior to enrollment; any relevant concomitant diseases; contraindications to MRI.
HS, with no history of neurological of psychiatric diseases, were selected to constitute the control group.
All subjects provided their written informed consent in accordance with the Declaration of Helsinki and approved by the institutional ethic committee (Policlinico Umberto I, Sapienza University of Rome, Italy).
All subjects had an MRI examination with a 3.0 T scanner (12-channel head coil for parallel imaging, Verio, Siemens AG). Around the time of the MRI scan (less than a month), patients were evaluated by means of the Expanded Disability Status Scale (EDSS, [15]) and the MS Functional Composite (MSFC, [16]), including the Paced Auditory Serial Addition Test (PASAT) at both 3- and 2-s interval, the 9 Hole Peg Test (9HPT) with both dominant and non-dominant hand, and the Timed 25-Foot Walk (T25-FW) test. The two outcomes yielded by PASAT and 9HPT were then averaged to obtain single scores.
MRI protocol
MRI protocol included the following sequences for all subjects: (a) High-resolution 3D T1-weighted (T13D) MPRAGE with 176 sagittal slices, 1-mm-thick slice, no gap (TR = 1900 ms, TE = 2.93 ms, TI = 900 ms, flip angle = 9°, matrix = 256 × 256, FOV = 260 mm2); (b) dual-echo proton density (PD) and T2-weighted (T2) images (TR = 3320 ms, TE = 10/103 ms, FOV = 220 mm2, 384 × 384 matrix, 25 4-mm-thick slices, 30% gap); (c) diffusion-based images acquired with a single-shot echo-planar spin-echo sequence with 30 directions (TR = 12,200 ms; TE = 94 ms; FOV = 192 mm2; matrix = 96 × 96; b = 0 and 1000 s/mm2; 72 axial contiguous 2-mm-thick slices); (d) blood-oxygenation-level-dependent single-shot echo-planar images (TR = 3000 ms, TE = 30 ms, flip angle = 89°, 64 × 64 matrix, 50 contiguous slices, 140 volumes, acquisition time = 7 min). Patients and controls were instructed to close their eyes and stay awake during the rsfMRI acquisitions.
Data analysis
Images were pre-processed as described previously [17], using FSL version 5.0.9 (FMRIB’s Software Library http://fsl.fmrib.ox.ac.uk/fsl) and homemade scripts (Bash and Matlab R2017b, https://it.mathworks.com).
Structural imaging
Lesion load (T2LL) in patients was calculated on PD-weighted images (Jim 5.0, Xinapse System, Leicester, UK; http://www.xinapse.com).
Brain volumes were measured using Sienax on lesion-filled head images [18, 19].
Diffusion-weighted imaging
Diffusion-weighted images were corrected for eddy-current distortion-induced distortions and head motions [20].
In each subject, fractional anisotropy (FA) and mean diffusivity (MD) were calculated as the average FA or MD of the skeletonized brain obtained through Tract-Based Spatial Statistics (TBSS) [21].
Functional imaging
Single-subject preprocessing of rsfMRI was carried out using FEAT 6.00 (FMRI Expert Analysis Tool). First three volumes were excluded to grant steady state, then images underwent motion correction (MCFLIRT [22]), spatial smoothing at 5 mm full width at half maximum Gaussian kernel, registration onto standard 2 mm MNI space (FLIRT, FNIRT).
Motion-related features and artifacts were removed via ICA-AROMA [23], band-pass filtering at 0.01–0.09 Hz, regression of white matter, and cerebrospinal fluid signals.
RSNs were identified via FSL Multivariate Exploratory Linear Optimized Decomposition into Independent Components (MELODIC, [24]) concatenating rsfMRI time series of all HS and patients.
Subject-specific time series of spatial maps were obtained using FSL dual regression [25].
In order to measure FC at each of the above-described three scales of brain network description, we assumed within-network FC as a measure of FC at the single-network scale, between any two networks FC as a measure of network-pairs scale, graph metrics as measures of whole-brain FC.
Single-network scale FC
Subject-specific spatial maps of each RSN were obtained from the dual-regression analysis. Voxel-wise differences in within-network FC maps between patients and HS were calculated non-parametrically via FSL Randomise (5000 permutations). Moreover, to quantify within-network FC in individual subjects, we calculated mean Z scores as the average z-Fisher transformation of Pearson correlation coefficient (Z) between voxels included in each RSN.
Network-pairs scale FC
To calculate between-network FC, Z was calculated between time series belonging to every possible pair of RSNs and generated an RSN-correlation matrix for each subject.
Whole-brain FC
To obtain measures of whole-brain FC, we performed graph theory analysis via GRETNA 2.0.0 toolbox (https://www.nitrc.org/projects/gretna/). Based on the between-network FC matrix, we calculated two topological organization parameters, namely the global efficiency, i.e., the average of the inverse shortest path length between RSNs, and degree centrality, i.e., the number of connections that each RSNs exhibits to the others. Graph theory analysis was performed on binary matrices that were created by thresholding between-network FC matrices at incremental values of absolute Z. Global efficiency and degree centrality were calculated at incremental Z and then integrated to obtain a single value for the entire interval of selected Z.
Correlation analysis
Clinical scores and structural features were separately correlated, via multiple correlation analyses, with altered within-network, between-network, and whole-brain FC, in those RSNs showing differences between patients and controls. Thus, we obtained a Spearman correlation coefficient (r) to express the relation between FC at each scale and clinical/ structural features adjusted for the other features.
In RSNs displaying altered FC at every scale, r was used to assess association between abnormalities in within-network, between-network, and whole-brain FC.
Functional Index
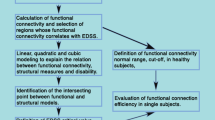
To obtain a combined measure suggestive of functional reorganization in response to MS-related damage, we computed principal component analysis (PCA) on measures of within-network FC (mean Z score), between-network FC (Z score) and whole-brain FC (global efficiency and degree centrality) in those RSNs whose parameters significantly correlated with one clinical or structural features, e.g. disease duration, EDSS, PASAT, 9HPT, T25-FT, T2LL, mean FA and mean MD. First principal component, explaining the highest variance within the data, was selected as functional index (fI) of that specific clinical or structural feature. To investigate the relation between each clinical and structural feature and fI, both a linear and a second order models were applied to data via ordinary least square fit. The best estimating model was identified by an F test for nested models, alpha = 0.05.
Statistical analysis
Age and sex difference between patients and controls were investigated by using two-tailed two-sample t test (alpha = 0.05) and chi-square statistics respectively.
A one sample t test (alpha = 0.05) was performed for both patients and controls to identify any multiscale FC measure, i.e., within-network FC, between-network FC, whole-brain FC, that were significantly different from 0. Group differences of within-network FC (mean Z score), between-network FC (Z), whole-brain FC (global efficiency and degree centrality), and fI were estimated via a two-sample t test (alpha = 0.05, two-tailed, unequal variance). Significance was reached if p < 0.05 after false discovery rate correction (FDR, [26]). In both group-comparison and correlation analysis, age and gray and white matter volumes were included as covariates of no interest.
Since differences in disease form may influence FC, we also included phenotype as covariate of no interest in the correlation analysis. Furthermore, we performed two-sample t test (alpha = 0.05, two-tailed, unequal variance) of the multiscale FC measures, that were altered in MS, between relapsing remitting and secondary progressive patients.
Results
One hundred and nineteen patients (28 males), aged 38.8 ± 10.1 years (mean ± standard deviation), and 42 age- and sex-matched controls (13 males), aged 35.6 ± 11.3 years, were enrolled. Patients’ phenotype was relapsing remitting in 91 cases and secondary progressives in 28, while their median EDSS was 2 (range 0.0–7.5). Forty-seven patients were not under treatment (30 relapsing remitting and 17 secondary progressive), 36 patients were under first-line treatment (32 relapsing remitting and 4 secondary progressive) and 36 patients were under second-line therapy (30 relapsing remitting and 6 secondary progressive). We found, as expected, a significant correlation between PASAT at 2 s and PASAT at 3 s (correlation coefficient 0.79 and p < 0.001), as well as between performance of 9HPT with dominant and non-dominant hands (correlation coefficient 0.70 and p < 0.001). To reduce the number of covariates and avoid co-linearity, we averaged the performances of respectively PASAT at 2 and 3 s, and 9HPT with dominant and non-dominant hands in further analysis. Patients’ demographic and clinical data are reported in Table 1.
Structural damage
The subjects’ lesion load was estimated to be 6.15 ± 6.42 mL. Both gray matter and white matter volumes were lower in patients than in controls, respectively t = − 3.44, p < 0.001 and t = − 2.00, p < 0.05 (see Table 1).
Mean FA was significantly lower in patients than controls (t = − 5.60, p < 0.001, Table 1), which corresponded to mean MD being higher in patients than controls (t = 5.10, p < 0.001, Table 1).
RSNs
We recognized 16 well-known RSNs out of the 35 components identified by MELODIC: default mode network (DMN), left and right frontoparietal networks (lFP, rFP), executive control network (ECN), dorsal and ventral attention networks (DAN, VAN), salience network (SaN), sensorimotor network (SMN), anterior and posterior cerebellar networks (aCb, pCb), basal ganglia network (including thalamus, BGN), medial and lateral visual networks (mVN, lVN), auditory network (AuN), and frontal and orbitofrontal networks (FrN, OFN).
Single-network scale
If compared with controls, patients had higher voxel-wise within-network FC in four RSNs: the DMN, ECN, lFP, and rFP (Fig. 1). In each of those 4 RSNs, mean Z scores were significantly different from zero, in both HS and patients, and differed between groups (patients versus controls t = 5.99, 4.90, 4.23, 4.05, respectively; all FDR corrected p < 0.001, Fig. 1).
Within-network functional connectivity. On the left, maps of Z score differences between patients and controls within, from top to bottom, default mode (DMN), executive control network (ECN), right and left frontoparietal networks (rFN, lFN). Significance was calculated via two-sample t test, alpha = 0.05, FDR corrected p < 0.05. Three-slice axial view is displayed according to radiological convention (RL). Red spots represent areas of significant between-group differences and yellow areas the maps of the four RSNs. On the right, barplots show the mean Z score and relative standard error of the mean (s.e.m.) calculated for both controls (purple bars) and patients with MS (yellow bars), within DMN, ECN, rFN, and lFN. Significance was calculated via two-sample t test, alpha = 0.05, FDR corrected p < 0.05
Between-network scale
We calculated FC between every pair of RSNs and built average between-network FC matrices for both controls and patients (Fig. 2). Between-network FC between aCb and ECN and between aCb and SaN was lower in patients than controls (respectively t = − 4.21, t = − 4.02; all FDR corrected p < 0.02, Fig. 3). Between-network FC of these pairs of RSNs was significantly higher than 0 in controls (respectively t = 7.59, p < 0.001, and t = 6.68, p < 0.001, one-sample t test, FDR correction), and was not different from 0 in patients, indicating disease-driven loss of functional connections that are present in controls.
Mean correlation matrix. bFC was calculated between each pair of RSNs for both controls (upper left triangle) and patients with MS (lower right triangle). Values on the diagonal are NaNs. Black dots show pair of RSNs significantly correlated in either controls or patients, after FDR correction, sample size correlation analysis with alpha = 0.05 and beta = 0.20, p < 0.05
Between-network functional connectivity. Barplot shows the average between-network FC and relative s.e.m. calculated for both controls (purple bars) and patients with MS (yellow bars). Results are reported only for those pairs of RSNs whose between-network FC significantly varied in patients in respect to controls, i.e., between-network FC reduction between anterior cerebellar network (aCb) and control networks (executive control network, ECN; salience network, SaN). Significance was stated via two-sample t test, alpha = 0.05, FDR corrected p < 0.05
Whole-brain scale
Graph theory analysis was performed on between-network FC matrices, that were previously thresholded at Z ranged (0.24, 0.84) with incremental step 0.05, and then integrated.
Global efficiency of mVN and BGN was lower in patients than in controls (respectively t = − 3.89 p < 0.004, t = − 3.12 p < 0.01 FDR corrected), while global efficiency of DMN was higher in patients than in controls (t = 2.85, p < 0.01 FDR corrected, Fig. 4a). Degree centrality of multiple RSNs, namely ECN, VAN, mVN, and SaN, was lower in patients than controls (respectively t = − 2.46, p < 0.02; t = − 3.11, p < 0.004; t = − 2.93, p < 0.02; t = − 3.09, p < 0.01 FDR corrected, Fig. 4b).
Graph theory parameters. Barplots show average whole-brain FC parameters and relative s.e.m., namely global efficiency (GE) on top of the figure and degree centrality (DC) at the bottom of the figure. Global efficiency and degree centrality were calculated for both controls (purple bars) and patients with MS (yellow bars). Results are reported only for those RSNs whose whole-brain FC significantly varied in patients in respect to controls, i.e., both global efficiency and degree centrality decrease in patients’ RSNs, with the sole exception of DMN global efficiency. Significance calculated via two-sample t test, alpha = 0.05, if FDR corrected p < 0.05
Correlation analysis
In patients, FC measures showed significant correlations with clinical features. Mean Z scores, quantifying within-network FC, in the DMN correlated with EDSS, in the ECN with T2LL, and in the rFP with PASAT (Table 2). These findings indicate that the higher the within-network FC, the better the cognitive performance and the lower the disability and structural damage.
aCb-ECN between-network FC significantly correlated with disease duration, while aCb-SaN between-network FC significantly correlated with disease duration, EDSS, T2LL, and diffusion-based parameters (Table 2), indicating that the lower the between-network FC, the longer the disease duration, and the higher the disability and structural damage.
Global efficiency of mVN significantly correlated with PASAT, while global efficiency of DMN significantly correlated with EDSS and PASAT, indicating that the lower the whole-brain FC, the higher the disability and the worse the cognitive performance. Similarly, degree centrality of the ECN significantly correlated with EDSS and T2LL, degree centrality of VAN significantly correlated with PASAT, and degree centrality of SaN significantly correlated with T2LL, indicating that the lower the whole-brain FC, the worse the cognitive performance, the higher the disability and the structural damage. Values and significance are listed in Table 2.
Among all RSNs, only DMN and ECN displayed alteration in all FC scales. However, these two RSNs did not show any significant correlations between measures of within-network FC and either between-network FC or whole-brain FC.
Functional index
As shown in Table 2, EDSS inversely correlated with five FC measures, i.e., within-network FC in DMN, FC between aCb and ECN and between aCb and SaN, and global efficiency of DMN and degree centrality of ECN. Via PCA, we combined those five FC measures and the first component resulted to explain the 88% of the variance. We selected this first component as the fIEDSS, which negatively correlated with EDSS (r = − 0.52, p < 0.001). fIEDSS was significantly higher in whole patient group than in controls (t = 2.66, p < 0.01). The relationship between EDSS and fIEDSS was best approximated via a non-linear, second order model (F = 7.25, p < 0.001), with the peak between EDSS values 0–3.5 (see Fig. 5a).
Functional index. The graph displays a the non-linear model between EDSS and fIEDSS, and the linear model best approximating b disease duration (DD) vs fI_DD, c PASAT vs fI_PASAT, d T2LL vs fI_T2LL. As explained in the text, fI are the functional indices related to the clinical/structural measure cleared in the proper subscript. Mean and standard deviation of fI values are displayed respectively by the blue line and light blue shade; models are displayed by black solid lines
Disease duration inversely correlated with within-network FC of DMN, FC between aCb and both ECN and SaN, and degree centrality of ECN and mVN. PCA on the latter functional parameters resulted in a first component, thus fIDD, explaining the 83% of the variance, being not different in patients and controls (t = 1.22, p > 0.05) and correlating with disease duration (r = − 0.34, p < 0.001, Fig. 5b).
PASAT score correlated with within-network FC of rFP, global efficiency of DMN and mVN, and degree centrality of VAN. First principal component of the latter features, thus fIPASAT, explained the 89% of the variance of such features, was higher in patients than in controls (t = 2.79, p < 0.01) and positively correlated with PASAT (r = 0.40, p < 0.02, Fig. 5c).
T2LL significantly correlated with FC within ECN, with FC between aCb and ECN, FC between aCb and SaN, with global efficiency of mVN and with degree centrality of ECN and SaN. The first principal component of such features, fIT2LL, explained the 83% of their variance. fIT2LL was lower in patients than controls (t = − 2.24, p < 0.03) and negatively correlated with T2LL (r = − 0.34, p < 0.001, Fig. 5d).
The relation between fIDD, fIPASAT, and fIT2LL and the relative clinical or structural parameter, e.g., disease duration, PASAT score, and T2LL were best approximated by a linear, first-order model (F < 0.6, p > 0.05).
Phenotype analysis
Patients with relapsing remitting form had higher multiscale functional connectivity parameters than patients with secondary progressive form, as in the following: within-network FC of DMN (t = 2.85, p < 0.01) and ECN (t = 4.09, p < 0.001), FC between aCb and SaN (t = 3.39, p < 0.001), global efficiency of BGN (t = 2.49, p < 0.02), degree centrality of ECN (t = 3.36, p < 0.001) and VAN (2.92, p < 0.01).
Similarly, in comparison to progressive patients, patients with relapsing remitting form had higher fIEDSS (5.14, p < 0.001), fIDD (3.97, p < 0.001), fIPASAT (3.34, p < 0.01), and fIT2LL (2.93, p < 0.01).
Discussion
We performed a multilevel network reorganization analysis and provide a complete picture of functional brain reorganization following MS-related damage. We showed that the disease affects brain network organization at the single-network scale, network-pairs scale and whole-brain scale.
Functional connectivity as segregation and integration estimate
Brain functional organization is based on two fundamental properties, i.e., segregation and integration, which must be considered complementary and essential for brain activities [27]. FC within RSNs may be assumed as a measure of functional segregation, that is a neuronal processing distributed among specialized brain regions, which have synchronous spontaneous fluctuations and are functionally specialized [28]. How pairs of RSNs communicate with each other and how RSNs globally arrange their functional interactions may be considered measures of functional integration that represents how networks cooperate in brain function processing through the convergent and joint elaboration of information derived from diverse sources [29].
In this framework, our results suggest that increased segregation, i.e., within-network FC, of cortical networks may be related to cognitive functions and may be ascribed to adaptive neuroplasticity mechanisms, while decreased integration, i.e., disconnection between cortical and cerebellar areas, together with the reduced global efficiency and degree centrality of basal ganglia, attentive and control networks, may result from structural disconnection and the exhaustion of compensatory mechanisms.
Functional connectivity changes as compensation for MS-related damage
The analysis of single-network scale FC revealed increase network segregation in some cortical areas, in particular are those involved in cognitive processes. Within-network FC in DMN increased in patients but was lower in secondary progressive MS in respect to relapsing remitting MS, and was directly correlated with a better cognitive performance and inversely related with disease duration. These results suggest that, at least in this network, the increase of segregation may represent a compensatory mechanism that runs out with disease progression, in keeping with previous reports showing DMN activity reduction in progressive forms and in presence of fatigue [5, 30] and reporting correlation between DMN FC and either disability or cognitive rehabilitation [31, 32]. Furthermore, we found that also integration of DMN, namely the global efficiency, increased in patients and positively correlated with clinical performances. Indeed, the ability of DMN to functionally adapt upon cognitive demands has been recently observed by studying the role of DMN dynamic FC in maintaining the information processing speed in patients with MS [33].
Similarly, our results suggest a compensatory effect corroborating that MS led to enhanced within-network FC in the bilateral frontoparietal networks and ECN [32], which are reported to be relevant for cognitive processing and structural damage also in Alzheimer disease [34, 35]. Our data are apparently in contrast to those of other authors, who reported a negative correlation between FC of rFP and PASAT [31]. This discrepancy may, however, be due to differences in the definition and size of the samples studied.
Functional connectivity exhaustion related to MS
As regards the between-network and whole-brain FC, we observed a cerebellar functional disconnection from control RSNs, such as ECN and SaN in patients [36], as well as a widespread decrement of integration that were negatively correlated with disease duration, disability, and structural damage and positively correlated with cognitive score. Our results confirmed that in MS-related damage compensation a central role is played by the cerebellum, whose functional changes are triggered by pathological structural damage [37] and whose functional disconnection accompanies the exhaustion of compensative mechanisms [17].
Besides, FC exhaustion due to MS was shown by studies on dynamic functional connectivity, which reported lower permanence in high-connectivity states and less dynamic functional configurations in cognitive impaired patients in respect to cognitive preserved patients [38].Moreover, compared to controls, patients demonstrated loss of dynamic connectivity, which was positively correlated with cognitive performances [39].
Interplay among functional scales to react to disease
The balance between functional segregation of specialized areas and their functional integration is essential for the operation of distributed networks underlying cognitive function [40], although, as observed previously in basal ganglia and cerebellar long-range and local connectivity [41], changes in network segregation and integration in our study did not occur concomitantly within and between the same RSNs and could be dissociated.
Previous studies that investigated functional segregation and integration have yielded discordant results (e.g., [41,42,43,44]) probably due to the different technique used. To merge the information from the three scale analyses, we created and investigated a unique index for each clinical/structural measure correlating with FC at more than one scale. The identified indices can explain a large amount of variance of the related clinical/structural measure underlining the relevance of functional integrity for clinical performances. As already proposed [17], in relation to EDSS, our results showed an initial increment of functional connectivity followed by the decrement when functional compensatory mechanisms fail confirming the functional reorganization model explained by Schoonheim et al. 2015 [45].
The analysis of the other parameters showed a monotonic behavior with a linear correlation between the indices and the related measures. These results combine the linear correlations that have already been cleared between FC and disease duration (e.g., [46]), lesion load (e.g., [9, 47]) and PASAT (e.g., [47]).
Limitations
We found correlation coefficients that were about 0.3, it may be due to a not very large sample size and/or a high variance of the measures within the group. One limitation of this study is that the evaluation of cognitive function included PASAT test alone. However, the PASAT is acknowledged to be a difficult and demanding cognitive test that is sufficiently sensitive to detect early cognitive abnormalities in patients. Furthermore, the only network parameters in the graph theory analysis we addressed were global efficiency and degree centrality, because they were assumed to be those that would most accurately explain the whole-brain integration process. Another limit of the study was that, due to study design, we did not analyze the relationship between FC at different scales and damage of specific white matter tracts; future research combining diffusion-based metrics and FC could investigate those issues. Lastly, our population did not include patients at the very beginning of the disease. Therefore, it is impossible to speculate whether FC alterations occur soon after a first demyelinating event rather than as a consequence of a time-dependent reorganization.
Conclusion
Our results suggest that increased functional segregation compensates for structural damage so as to maintain cognitive and motor abilities; conversely, disrupted functional integration likely results from structural disconnection and is linked to clinical severity. Our results also suggest that 1. disease duration correlates mainly with cerebello-cortical functional diaschisis; 2. structural damage mainly corrupts pathways that are related to control networks; 3. cognition is preserved if both frontoparietal segregation and integration of DMN, visual and attentive networks are enhanced; 4. disability is compensated for by increased DMN segregation and residual integration of cerebellar, control, and basal ganglia networks.
References
Zatorre RJ, Fields RD, Johansen-Berg H (2012) Plasticity in gray and white: neuroimaging changes in brain structure during learning. Nat Neurosci 15:528–536. https://doi.org/10.1038/nn.3045
De Giglio L, Tommasin S, Petsas N, Pantano P (2018) The role of fMRI in the assessment of neuroplasticity in MS: a systematic review. In: Neural Plasticity. https://www.hindawi.com/journals/np/2018/3419871/. Accessed 1 Jan 2019
Pantano P, Iannetti GD, Caramia F, Mainero C, di Legge S, Bozzao L, Pozzilli C, Lenzi GL (2002) Cortical motor reorganization after a single clinical attack of multiple sclerosis. Brain 125:1607–1615
Roosendaal SD, Schoonheim MM, Hulst HE, Sanz-Arigita EJ, Smith SM, Geurts JJ, Barkhof F (2010) Resting state networks change in clinically isolated syndrome. Brain 133:1612–1621. https://doi.org/10.1093/brain/awq058
Rocca MA, Valsasina P, Leavitt VM, Rodegher M, Radaelli M, Riccitelli GC, Martinelli V, Martinelli-Boneschi F, Falini A, Comi G, Filippi M (2018) Functional network connectivity abnormalities in multiple sclerosis: correlations with disability and cognitive impairment. Mult Scler 24:459–471. https://doi.org/10.1177/1352458517699875
Penner I-K, Aktas O (2017) Functional reorganization is a maladaptive response to injury - NO. Mult Scler 23:193–194. https://doi.org/10.1177/1352458516679895
Rocca MA, Meani A, Riccitelli GC, Colombo B, Rodegher M, Falini A, Comi G, Filippi M (2016) Abnormal adaptation over time of motor network recruitment in multiple sclerosis patients with fatigue. Mult Scler 22:1144–1153. https://doi.org/10.1177/1352458515614407
Tona F, Petsas N, Sbardella E et al (2014) Multiple sclerosis: altered thalamic resting-state functional connectivity and its effect on cognitive function. Radiology:131688. https://doi.org/10.1148/radiol.14131688
Rocca MA, Valsasina P, Absinta M et al (2014) Intranetwork and internetwork functional connectivity abnormalities in pediatric multiple sclerosis. Hum Brain Mapp 35:4180–4192. https://doi.org/10.1002/hbm.22469
Eijlers AJC, Meijer KA, Wassenaar TM, Steenwijk MD, Uitdehaag BM, Barkhof F, Wink AM, Geurts JJ, Schoonheim MM (2017) Increased default-mode network centrality in cognitively impaired multiple sclerosis patients. Neurology 88:952–960. https://doi.org/10.1212/WNL.0000000000003689
Meijer KA, Eijlers AJC, Douw L, Uitdehaag BMJ, Barkhof F, Geurts JJG, Schoonheim MM (2017) Increased connectivity of hub networks and cognitive impairment in multiple sclerosis. Neurology 88:2107–2114. https://doi.org/10.1212/WNL.0000000000003982
Meijer KA, Eijlers AJC, Geurts JJG, Schoonheim MM (2018) Staging of cortical and deep grey matter functional connectivity changes in multiple sclerosis. J Neurol Neurosurg Psychiatry 89:205–210. https://doi.org/10.1136/jnnp-2017-316329
van den Heuvel MP, Hulshoff Pol HE (2010) Exploring the brain network: a review on resting-state fMRI functional connectivity. Eur Neuropsychopharmacol 20:519–534. https://doi.org/10.1016/j.euroneuro.2010.03.008
Polman CH, Reingold SC, Banwell B, Clanet M, Cohen JA, Filippi M, Fujihara K, Havrdova E, Hutchinson M, Kappos L, Lublin FD, Montalban X, O'Connor P, Sandberg-Wollheim M, Thompson AJ, Waubant E, Weinshenker B, Wolinsky JS (2011) Diagnostic criteria for multiple sclerosis: 2010 revisions to the McDonald criteria. Ann Neurol 69:292–302. https://doi.org/10.1002/ana.22366
Kurtzke JF (1983) Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS). Neurology 33:1444–1452. https://doi.org/10.1212/wnl.33.11.1444
Fischer JS, Rudick RA, Cutter GR, Reingold SC (1999) The multiple sclerosis functional composite measure (MSFC): an integrated approach to MS clinical outcome assessment. National MS Society clinical outcomes assessment task force. Mult Scler 5:244–250. https://doi.org/10.1177/135245859900500409
Tommasin S, De Giglio L, Ruggieri S et al (2018) Relation between functional connectivity and disability in multiple sclerosis: a non-linear model. J Neurol 265:2881–2892. https://doi.org/10.1007/s00415-018-9075-5
Smith SM (2002) Fast robust automated brain extraction. Hum Brain Mapp 17:143–155. https://doi.org/10.1002/hbm.10062
Smith SM, De Stefano N, Jenkinson M, Matthews PM (2001) Normalized accurate measurement of longitudinal brain change. J Comput Assist Tomogr 25:466–475
Andersson JLR, Sotiropoulos SN (2016) An integrated approach to correction for off-resonance effects and subject movement in diffusion MR imaging. Neuroimage 125:1063–1078. https://doi.org/10.1016/j.neuroimage.2015.10.019
Smith SM, Jenkinson M, Johansen-Berg H, Rueckert D, Nichols TE, Mackay CE, Watkins KE, Ciccarelli O, Cader MZ, Matthews PM, Behrens TE (2006) Tract-based spatial statistics: voxelwise analysis of multi-subject diffusion data. Neuroimage 31:1487–1505. https://doi.org/10.1016/j.neuroimage.2006.02.024
Jenkinson M, Bannister P, Brady M, Smith S (2002) Improved optimization for the robust and accurate linear registration and motion correction of brain images. Neuroimage 17:825–841
Pruim RHR, Mennes M, van Rooij D et al (2015) ICA-AROMA: a robust ICA-based strategy for removing motion artifacts from fMRI data. Neuroimage 112:267–277. https://doi.org/10.1016/j.neuroimage.2015.02.064
Beckmann CF, DeLuca M, Devlin JT, Smith SM (2005) Investigations into resting-state connectivity using independent component analysis. Philos Trans R Soc B Biol Sci 360:1001–1013. https://doi.org/10.1098/rstb.2005.1634
Beckmann C, Mackay C, Filippini N, Smith S (2009) Group comparison of resting-state FMRI data using multi-subject ICA and dual regression. NeuroImage 47:S148. https://doi.org/10.1016/S1053-8119(09)71511-3
Benjamini Y, Hochberg Y (1995) Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc Ser B Methodol 57:289–300
Sporns O (2013) Network attributes for segregation and integration in the human brain. Curr Opin Neurobiol 23:162–171. https://doi.org/10.1016/j.conb.2012.11.015
Tononi G, Sporns O, Edelman GM (1994) A measure for brain complexity: relating functional segregation and integration in the nervous system. Proc Natl Acad Sci U S A 91:5033–5037
Friston K (2002) Functional integration and inference in the brain. Prog Neurobiol 68:113–143
Bisecco A, Nardo FD, Docimo R et al (2017) Fatigue in multiple sclerosis: the contribution of resting-state functional connectivity reorganization. Mult Scler J 135245851773093. https://doi.org/10.1177/1352458517730932
Faivre A, Rico A, Zaaraoui W, Crespy L, Reuter F, Wybrecht D, Soulier E, Malikova I, Confort-Gouny S, Cozzone PJ, Pelletier J, Ranjeva JP, Audoin B (2012) Assessing brain connectivity at rest is clinically relevant in early multiple sclerosis. Mult Scler 18:1251–1258. https://doi.org/10.1177/1352458511435930
Sacco R, Bonavita S, Esposito F et al (2013) The contribution of resting state networks to the study of cortical reorganization in MS. Mult Scler Int 2013. https://doi.org/10.1155/2013/857807
van Geest Q, Douw L, van ‘t Klooster S et al (2018) Information processing speed in multiple sclerosis: relevance of default mode network dynamics. Neuroimage Clin 19:507–515. https://doi.org/10.1016/j.nicl.2018.05.015
Li K, Luo X, Zeng Q, Huang P, Shen Z, Xu X, Xu J, Wang C, Zhou J, Zhang M, Alzheimer’s Disease Neuroimaging Initiative (2019) Gray matter structural covariance networks changes along the Alzheimer’s disease continuum. Neuroimage Clin 23:101828. https://doi.org/10.1016/j.nicl.2019.101828
Zhao Q, Sang X, Metmer H, Swati ZNNK, Lu J, Alzheimer’s Disease NeuroImaging Initiative (2019) Functional segregation of executive control network and frontoparietal network in Alzheimer’s disease. Cortex 120:36–48. https://doi.org/10.1016/j.cortex.2019.04.026
Dosenbach NUF, Visscher KM, Palmer ED, Miezin FM, Wenger KK, Kang HC, Burgund ED, Grimes AL, Schlaggar BL, Petersen SE (2006) A core system for the implementation of task sets. Neuron 50:799–812. https://doi.org/10.1016/j.neuron.2006.04.031
Weier K, Banwell B, Cerasa A, Collins DL, Dogonowski AM, Lassmann H, Quattrone A, Sahraian MA, Siebner HR, Sprenger T (2015) The role of the cerebellum in multiple sclerosis. Cerebellum 14:364–374. https://doi.org/10.1007/s12311-014-0634-8
d’Ambrosio A, Valsasina P, Gallo A et al (2019) Reduced dynamics of functional connectivity and cognitive impairment in multiple sclerosis. Mult Scler:1352458519837707. https://doi.org/10.1177/1352458519837707
Lin S-J, Vavasour I, Kosaka B, Li DKB, Traboulsee A, MacKay A, McKeown M (2018) Education, and the balance between dynamic and stationary functional connectivity jointly support executive functions in relapsing-remitting multiple sclerosis. Hum Brain Mapp 39:5039–5049. https://doi.org/10.1002/hbm.24343
Sporns O (2013) Structure and function of complex brain networks. Dialogues Clin Neurosci 15:247–262
Dogonowski A-M, Andersen KW, Madsen KH, Sørensen PS, Paulson OB, Blinkenberg M, Siebner HR (2014) Multiple sclerosis impairs regional functional connectivity in the cerebellum. Neuroimage Clin 4:130–138. https://doi.org/10.1016/j.nicl.2013.11.005
Louapre C, Perlbarg V, García-Lorenzo D, Urbanski M, Benali H, Assouad R, Galanaud D, Freeman L, Bodini B, Papeix C, Tourbah A, Lubetzki C, Lehéricy S, Stankoff B (2014) Brain networks disconnection in early multiple sclerosis cognitive deficits: an anatomofunctional study: disconnection and cognition in MS. Hum Brain Mapp 35:4706–4717. https://doi.org/10.1002/hbm.22505
Rocca MA, Valsasina P, Meani A, Falini A, Comi G, Filippi M (2016) Impaired functional integration in multiple sclerosis: a graph theory study. Brain Struct Funct 221:115–131. https://doi.org/10.1007/s00429-014-0896-4
Zhou F, Zhuang Y, Gong H, Wang B, Wang X, Chen Q, Wu L, Wan H (2014) Altered inter-subregion connectivity of the default mode network in relapsing remitting multiple sclerosis: a functional and structural connectivity study. PLoS One 9:e101198. https://doi.org/10.1371/journal.pone.0101198
Schoonheim MM, Meijer KA, Geurts JJG (2015) Network collapse and cognitive impairment in multiple sclerosis. Front Neurol 6:82. https://doi.org/10.3389/fneur.2015.00082
Liu Y, Liang P, Duan Y, Huang J, Ren Z, Jia X, Dong H, Ye J, Shi FD, Butzkueven H, Li K (2015) Altered thalamic functional connectivity in multiple sclerosis. Eur J Radiol 84:703–708. https://doi.org/10.1016/j.ejrad.2015.01.001
Sbardella E, Upadhyay N, Tona F et al (2017) Dentate nucleus connectivity in adult patients with multiple sclerosis: functional changes at rest and correlation with clinical features. Mult Scler 23:546–555. https://doi.org/10.1177/1352458516657438
Funding
This study was partially supported by the Italian Foundation of multiple sclerosis (FISM), grant number 2018/S/3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
ST and CG declare no conflict of interest. LDG received speaking honoraria from Genzyme and Novartis; travel grants from Biogen, Merk, and Teva; and consulting fees from Genzyme, Merk, and Novartis. SR received fees as speaking honoraria from Teva, Merck Serono, and Biogen; travel grants from Biogen and Merck Serono; and fees as advisory board consultant from Merck Serono and Novartis. NP received speaker fees from Biogen and mission support from Genzyme and Novartis. CP received consulting and lecture fees and research funding and travel grants from Almirall, Bayer, Biogen, Genzyme, Merck Serono, Novartis, Roche, and Teva. PP received founding for travel from Novartis, Genzyme, Bracco, and Biogen.
Ethical approval
All procedures performed in the studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tommasin, S., De Giglio, L., Ruggieri, S. et al. Multi-scale resting state functional reorganization in response to multiple sclerosis damage. Neuroradiology 62, 693–704 (2020). https://doi.org/10.1007/s00234-020-02393-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-020-02393-0