Abstract
Pseudoachondroplasia (PSACH) and multiple epiphyseal dysplasia type 1 (MED1) are two rare skeletal disorders caused by cartilage oligomeric matrix protein (COMP) variants. This study aims to analyze the genotype and phenotype of patients with COMP variants. Clinical information for 14 probands was collected; DNA was extracted from blood for COMP variant detection. Clinical manifestations and radiology scoring systems were established to evaluate the severity of each patient’s condition. Serum COMP levels in PSACH patients and healthy subjects were measured. Thirty-nine patients were included, along with 12 PSACH probands and two MED1 probands. Disproportionate short stature, waddling gait, early-onset osteoarthritis and skeletal deformities were the most common features. The height Z-score of PSACH patients correlated negatively with age at evaluation (r = − 0.603, p = 0.01) and the clinical manifestation score (r = − 0.556, p = 0.039). Over 50% of the PSACH patients were overweight/obese. The median serum COMP level in PSACH patients was 16.75 ng/ml, which was significantly lower than that in healthy controls (98.53 ng/ml; p < 0.001). The condition of MED1 patients was better than that of PSACH patients. Four novel variants of COMP were detected: c.874T>C, c.1123_1134del, c.1531G>A, and c.1576G>T. Height Z-scores and serum COMP levels were significantly lower in patients carrying mutations located in calmodulin-like domains 6, 7, and 8. As the two phenotypes overlap to different degrees, PSACH and MED1 are suggested to combine to produce “spondyloepiphyseal dysplasia, COMP type”. Clinical manifestations and radiology scoring systems, serum COMP levels and genotype are important for evaluating patient condition severity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pseudoachondroplasia (PSACH, MIM 177170) and multiple epiphyseal dysplasia type 1 (MED1, MIM 132400) are two relatively common osteochondral disorders caused by mutations in the gene encoding cartilage oligomeric matrix protein (COMP), and both phenotypes are in accordance with an autosomal dominant inheritance pattern [1]. Since the identification of the pathogenic gene in 1995, an increased number of endocrinologists, orthopedists and pediatricians have recognized these two disorders [2,3]. Although the prevalence of PSACH and MED1 worldwide remains unclear, the estimated prevalence of PSACH is 1–9/100,000 (www.orpha.net). The typical manifestations of PSACH include postnatal linear growth retardation, severe short-limbed dwarfism, predominant spinal and pelvic deformities, joint laxity or pain, and short phalanges and metacarpals, among others, although craniofacial development and intelligence are normal [4]. The phenotype of MED1 and PSACH overlap to some extent. However, the severity of MED1 is less than that of PSACH, which is characterized mainly by mild to moderate short stature, waddling gait, necrosis of the femoral head and early-onset hip osteoarthritis [5,6].
The gene that encodes COMP, also known as thrombospondin-5, is located at 19p13.11 and has 19 exons, producing a 757-amino acid polypeptide [7]. The monomer structure of COMP comprises an N-terminal domain (NTD), four epidermal-growth factor-like domains (EGF-like domains, also called T2), eight calmodulin-like domains (CLDs, also called T3), and a C-terminal domain (CTD) [8]. Five COMP monomers aggregate through disulfide bonds to form a pentameric glycoprotein with a molecular weight of 524 kDa that localizes to the extracellular matrix [9,10,11]. The protein is abundantly expressed in the chondrocyte extracellular matrix and is found in tendons, ligaments, smooth muscle, synovium and osteoblasts [12,13]. COMP is a noncollagenous protein that maintains the stability of the cartilage structure by interacting with other extracellular matrix proteins or mediating interactions between chondrocytes and the extracellular matrix through integrin and its receptors [8,14]. COMP is known to bind to heparin, chondroitin sulfates, and heparan sulfate in the presence of calcium [15] and to collagen I, II and IX in the presence of zinc [16].
The objective of this study was to analyze clinical, anthropometrical, biochemical, radiological, genetic and therapeutic data for patients with short stature from 14 families, including 12 probands with PSACH and 2 probands with MED1. Clinical manifestation and radiology scoring systems were initially established to evaluate the severity of the phenotypes. In addition, we report four novel variants of COMP, expanding the mutation profile.
Materials and Methods
Subjects
Fourteen patients were admitted to our hospital mainly because of short stature or waddling gait. Family history, clinical information, and biochemical and radiological data of all these patients were collected. Peripheral blood and serum from patients as well as some of their family members were collected for analysis; serum was also obtained from sex- and age-matched healthy controls. All subjects signed the informed consent form. The study was performed with the approval of the Ethics Committee of Peking Union Medical College Hospital (JS-1689).
Evaluation Standard of Anthropometric Data
Z-scores of height, weight and body mass index (BMI) were calculated according to “growth charts for Chinese children and adolescents aged 0 to 18 years” [17,18].
Biochemical Assessment
Serum phosphorus, calcium, alkaline phosphatase (ALP), total 25-hydroxyl vitamin D (25OHD), C-terminal cross-linking telopeptide of type I collagen (β-CTX), growth hormone (GH) and insulin-like growth factor 1 (IGF-1) levels were measured using automated analyzers. The Kidney Disease Outcomes Quality Initiative (KDOQI) guideline was used as the reference for serum phosphorus and calcium in patients below 18 years of age [19]; the β-CTX level each of these patients was measured, and further evaluated based on sex- and age-specific reference ranges [20]. The serum of 10 patients with PSACH and 10 healthy subjects was collected and stored at − 80 °C for further assessment of COMP levels using a Quantikine® ELISA Human COMP Immunoassay Kit (DCMP0, R&D Systems, USA) according to the manufacturer's protocol and a microplate reader set to 450 nm, with 562 nm as the correction wavelength. The reference range of serum samples from donors without a medical history was 66.8–409 ng/ml. Each sample was assayed in duplicate.
Scoring Systems of Clinical Manifestations and Radiological Characteristics
To evaluate the severity of the disorder, clinical and radiological scoring systems were established according to the specific clinical manifestations and radiological characteristics of patients with COMP gene variants. The evaluation dimensions in the clinical scoring system included 18 key items, such as waddling gait, growth retardation, joint laxity, osteoarticular pain, and skeletal deformities (Supplementary Materials Table 1). The radiological scoring system focused on 12 key features, including abnormal shape of the vertebrae, brachydactyly, scoliosis, and lumbar lordosis (Supplementary Materials Table 2). Some dimensions were assigned a score of 0 or 1, with 0 representing patients without the characteristic and 1 representing those with the characteristic. Other dimensions were assigned a score of 0, 1 or 2, with 0 representing patients without the characteristics and 1 and 2 representing mild and severe manifestations, respectively. The converted score, was the actual score divided by the total score, multiplied by 100. The clinical and radiological scores were evaluated by two experienced clinicians and radiologists, respectively, and the final average score was calculated. The intraclass correlation coefficient (ICC) of clinical and radiological scoring systems were 0.921 (p < 0.001) and 0.962 (p < 0.001), respectively.
DNA Extraction and COMP Gene Sequencing
A QIAamp DNA Mini Kit (51304, QIAGEN, Germany) was used to extract DNA from 200 µl peripheral blood. Genomic DNA from the proband of every family was amplified by polymerase chain reaction (PCR) to detect variants in exons 8 to 19 of the COMP gene. The reference sequence of the COMP gene was NM_000095.3, as provided by the National Center for Biotechnology Information (NCBI). Information for the primers used to amplify COMP is shown in Supplementary Materials Table 3. The total PCR volume was 20 µl, including 10 µl of 2 × Taq PCR Master Mix, 6 µl of double-distilled water, 2 µl of genomic DNA, and 1 µl of forward and reverse primers (10 µmol/l). The PCR amplification was as follows: 94 °C for 4 min; 35 cycles at 94 °C for 30 s, appropriate annealing temperatures for 30 s and 72 °C for 1 min; and one cycle at 72 °C for 4 min followed by storage at 4 °C. The same site of the COMP gene in each family member was verified based on the results for the proband.
Statistical Analysis
Statistical analysis was performed using SPSS version 25.0. The Shapiro–Wilk test was employed to assess the normality of the data. Normally distributed data are presented as the mean ± standard deviation (M ± SD); nonnormally distributed data are described as the median (interquartile range, IQR). For two groups of normally distributed data, an independent-sample t test was used to determine differences between two groups. Pearson or Spearman correlation analysis was applied to determine correlation between two parameters. p < 0.05 indicated a significantly statistical difference.
Results
General Characteristics of the Patients in the Cohort
The cohort included 39 patients from 14 families with clinical or genetic diagnosis, among whom 20 patients had a definitive genetic diagnosis. The ratio of males to females was 0.77, with 17 males and 22 females. The mean age of first clinical manifestations occurred at 1.62 ± 0.80 years for 13 probands, and the median age at diagnosis was 8.15 years [IQR 4.38–13.75 years old (y.o.), n = 14]. Eight families had a history of short stature, accounting for 57.1% (8/14). Detailed pedigrees of these 14 families were shown in Fig. 1 of Supplementary Materials. There were 22 patients with PSACH (including 12 probands) and 17 patients (including 2 probands) with the MED1 phenotype.
Clinical Manifestations of Patients with COMP Variants
For PSACH patients with available data, the mean birth weight was 3.20 ± 0.66 kg (n = 8), and the mean birth length was 50.00 ± 0.89 cm (n = 6). Three patients were born by cesarean section because of the small pelvis of their PSACH mother. All patients with PSACH (n = 13) had short stature, growth retardation, waddling gait, long and tubular bones that were short, genu varum or valgum, and bracelet and anklet signs. Other common manifestations such as lumbar lordosis, kyphosis, joint laxity, osteoarthropathy, scoliosis were listed in Table 1. Only two patients had atlantoaxial dislocation and hip dislocation. However, none of the patients exhibited craniofacial malformation, mental retardation or dental dysplasia. Two patients with MED1 were prepubertal males with the main manifestations of waddling gait, short stature and mild skeletal abnormalities. One MED1 patient had osteoarticular pain, short neck, kyphosis and brachydactyly, and the other presented with mild short limbs and limited carpal joint movement without other skeletal deformity. Among the 13 patients with PSACH, there was no correlation between the clinical manifestation score and age at evaluation (Spearman analysis, r = 0.362, p = 0.224).
Anthropometric Data of Patients with COMP Variants
For 18 patients with PSACH, the mean Z-score of height was − 8.06 ± 3.62. The height Z-scores of males and females were − 6.38 ± 3.80 (n = 7) and − 9.13 ± 3.22 (n = 11), respectively (p = 0.119; Fig. 1A). The Z-scores of height were − 5.89 ± 2.49 (n = 10) for individuals below 18 y.o. and − 10.77 ± 2.95 (n = 8) for adults, and the difference was 4.88 (95% confidence interval 2.16–7.59, p = 0.002; Fig. 1B). Absolute height and its Z-score of adult PSACH patients were listed in Table 2. Furthermore, there was a negative correlation between the height Z-score and age at evaluation in 17 patients with PSACH (Pearson analysis, r = − 0.603, p = 0.01; Fig. 1C). Overall, height impairment was not severe in the MED1 patients, with the height Z-scores of two patients being − 2.01 and − 0.50. Moreover, in some of the PSACH and MED1 patients, the Z-score of height correlated negatively with the clinical manifestation score (Pearson analysis, n = 14, r = − 0.556, p = 0.039), but there was no correlation between the Z-score of height and the radiology score (Spearman analysis, n = 12, r = − 0.266, p = 0.404). Regarding other anthropometric parameters for PSACH patients with available data, the ratio of arm span to height was 0.88 ± 0.03 (n = 5), and the median weight Z-score was − 2.25 (IQR − 2.78 to − 0.96, n = 12). The mean BMI of 12 of the patients with PSACH was 21.24 ± 5.36 kg/m2, with a Z-score of 1.51 ± 1.72. According to the Z-score of BMI, the proportions of individuals with underweight, normal weight, overweight and obese statuses accounted for 8.3% (1/12), 33.3% (4/12), 33.3% (4/12) and 25.0% (3/12), respectively.
Evaluation of height and correlation analysis among age, height Z-score, clinical manifestation score and radiology score in patients with PSACH. A and B The difference in height Z-scores in PSACH patients by sex and age. C Correlation analysis between age at evaluation and height Z-score in 17 PSACH patients. PSACH pseudoachondroplasia. **p = 0.01
Biochemical Parameters and the Level of Serum COMP
In total, 38.5% (5/13) of the patients had a diagnosis of vitamin D deficiency (a total 25OHD level < 20 ng/ml). Nonetheless, the levels of calcium, phosphorus, alkaline phosphatase, parathyroid hormone, β-CTX, glucose, lipid, hepatic and renal functions were almost within the normal ranges matched to age and sex. One patient with PSACH was diagnosed with GH deficiency, with a peak level of 3.55 ng/ml and an IGF-1 level of 214 ng/ml (Z-score 1.04).
The level of serum COMP in the PSACH patients was significantly lower than that in the control group, with medians of 16.75 ng/ml (IQR 1.83–23.48 ng/ml) and 98.53 ng/ml (IQR 63.70–162.03 ng/ml) (p < 0.001; Fig. 2A). Serum COMP levels in the PSACH and control groups were 13.43 ± 10.07 ng/ml and 108.88 ± 63.60 ng/ml, respectively, in the minors group (p = 0.027) and 17.36 ± 17.31 ng/ml and 150.14 ± 121.20 ng/ml (p = 0.042), respectively, in adults (Fig. 2B). However, in both the PSACH (p = 0.673) and control (p = 0.519) groups, there were no significant differences in COMP levels between adults and individuals under 18 y.o. (Fig. 2B). Moreover, there were no correlations between serum COMP level and Z-scores of height (r = 0.166, p = 0.669) or BMI (r = − 0.074, p = 0.889) in the patients with PSACH, and biochemical markers, including Ca, P, ALP, β-CTX, and 25OHD, showed no correlations with serum COMP in PSACH patients (Supplementary Materials Table 4). Similarly, no correlation between COMP levels and the clinical manifestation score (r = 0.189, p = 0.685) or radiology score (r = 0.616, p = 0.193) were detected.
Results and correlation analysis of serum COMP levels in patients with PSACH. A Serum COMP levels were significantly different between patients with PSACH (n = 10) and healthy controls (n = 10). B Stratified by age and regardless of age, the serum COMP levels of PSACH patients were lower than those of healthy controls, but there was no significant difference between adults and individuals under 18 years of age among PSACH patients or healthy controls. PSACH pseudoachondroplasia. *p < 0.05, ***p < 0.001
Radiological Characteristics of Patients with COMP Variants
The X-ray results of 11 patients with PSACH showed that the most common features were deformities of the spine, vertebrae, acetabulum and metaphysis of the long and tubular bones (Fig. 3A–G). Only 60% (6/10) of the PSACH patients had scoliosis. The exact proportions of the radiological characteristics of the PSACH patients are listed in Table 3. The classic vertebral abnormalities were anterior and posterior vertebral flattening, with beak-shaped or transverse vase-like vertebrae, but this feature was not observed in all patients with PSACH. Some of the vertebrae showed posterior flattening or superior and inferior depression. In general, the radiological features of the MED1 patients were milder than those of the PSACH patients. The X-ray for one of the MED1 patients indicated only an irregular acetabulum and an irregular and small femoral neck, and the other MED1 patient had an atypical irregular acetabulum, slight scoliosis, and mild disorganized and expansive metaphysis of the long bone (Fig. 3H–L); neither patient had brachydactyly. Eight patients, including one with MED1, underwent bone age assessment, and 62.5% (5/8) had a delayed bone age.
Typical features of X-rays of PSACH and MED1. A–G are X-rays of PSACH patients. A Proband in family 11, M/10.5 years old, lumbar lordosis, kyphosis, cuppy sign of the front rib and beak-like vertebrae. B Proband in family 3, M/4 years old, parentheses sign of rib in anteroposterior spine X-ray, and beak-like vertebrae in lateral spine X-ray. C Proband in family 1, M/4.67 years old, scoliosis, irregular and small femoral head and irregular acetabulum. D Proband in family 11, M/10.5 years old, severe disorganization and expansion of metaphysis of long bones. E Proband in family 12, F/24 years old, inclination of articular surface in long bone. F Proband in family 6, M/30 years old, brachydactyly and inclination of articular surface in carpal joint. G Proband in family 11, M/10.5 years old, brachydactyly and disorganization and expansion of metaphysis of long bones. H–L are X-rays of the MED1 proband from family 5, M/7.1 years old, slight scoliosis and lordosis in lumbar spine, anterior edge of vertebrae flattened in T11–L5, and mild disorganization of metaphysis of in lower extremities. PSACH pseudoachondroplasia, MED1 multiple epiphyseal dysplasia type 1, M male, F female
Summary of COMP Variants
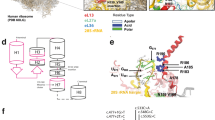
Twelve heterozygous variants of the COMP gene, including four novel variants, were detected in 14 families (Table 4). There were 10 missense mutations and two deletions, and all variants were located from exons 8 to 14, corresponding to the T3 and CTD domains. The proportion of de novo mutations was 41.7% (5/12). Among the variants, c.1417_1419delGAC was the hotspot variant, as detected in three families.
The PSACH patients were divided into group 1 (variants in T3-6, T3-7 and T3-8) and group 2 (variants in T3-1, T3-2 and CTD) according to the COMP domain in which the mutation occurs. The median height Z-score of group 1 was significantly lower than that of group 2, at − 7.64 (IQR − 11.94 to − 6.72) and − 3.08 (IQR − 7.47 to − 2.21), respectively (p = 0.02; Fig. 4A). Moreover, the level of serum COMP in group 1 was 3.08 ng/ml (IQR 0.96–15.39 ng/ml), which was significantly lower than that in group 2 (25.21 ng/ml, IQR 21.17–37.91 ng/ml) (p = 0.005; Fig. 4B).
Differences in height and serum COMP levels in PSACH patients carrying different variants. PSACH patients were divided into two groups according to the domains in which the mutations occurred, with group 1 including mutations in domains T3-6, T3-7 and T3-8 and group 2 including mutations in domains T3-1, T3-2 and the CTD. A The height Z-score in group 1 was lower than that in group 2. B The serum COMP level of group 1 was significantly lower than that of group 2. PSACH pseudoachondroplasia, T3 calmodulin-like domain, CTD C-terminal domain. *p < 0.05, **p < 0.01
Treatment and Prognosis
With regard to treatment, two patients with PSACH accepted recombinant human growth hormone (rhGH) therapy, but the efficacy was not ideal. One patient was injected with rhGH for 8 months but had no obvious height gain. The other patient, whose IGF-1 was above the mean level of the normal reference, was diagnosed with GH deficiency and accepted rhGH therapy for a year; the growth velocity of this patient increased from 2.5 cm/year to 5.5 cm/year, but rhGH was later withdrawn due to aggravation caused by lower-limb bending. One PSACH patient was treated with atlantoaxial fixation. Three PSACH patients underwent orthopedic surgery for two lower limbs: the height of one adult female patient improved from 127 cm to 137 cm, and the genu varus of the other two children improved, with gait becoming stable.
Discussion
PSACH and MED1, two phenotypes caused by COMP gene variants, are characterized by varying degrees of linear growth retardation and skeletal deformities [21]. To date, research on these two disorders has focused mainly on gene variants, pathogenic mechanisms, clinical phenotypes (in case reports), and novel therapeutic interventions [22,23,24]. In contrast, few researchers have paid attention to anthropometric parameters such as the BMI of patients with COMP variants or have analyzed relationships between genotype and phenotype in detail. Therefore, this study recruited 14 probands, evaluated in detail the severity of their clinical manifestations and radiological characteristics by using two scoring systems, measured serum COMP levels, identified COMP variants and explored correlations among those items.
Several basic studies have shown that Comp-null mice in which the Comp gene has been knocked out exhibit no abnormalities in anatomy, histology or ultrastructure, and there are no clinical manifestations associated with PSACH or MED1 [25]. Nonetheless, mutant Comp mice including T585M-knock in and D469del-knock in mice have typical phenotypes, such as hip dysplasia and articular cartilage erosion, suggesting that COMP variants have dominant negative effects that result in the phenotype of PSACH [26,27]. Variants of COMP occur mainly in the T3 domain, interfering with COMP binding to calcium ions and protein folding. The mutant product accumulates in the endoplasmic reticulum (ER) of chondrocytes in the growth plate, leading to abnormal chondrocytes in a state of inflammation and oxidative stress, eventually resulting in early death of these cells and impairment of linear growth in long bones [23]. Moreover, DNA damage inducible transcript 3 (DDIT3, also known as CHOP) is a transcription factor related to ER stress and can promote chondrocyte apoptosis [28,29]. The pathogenic mechanism of COMP variants in CTD is slightly different; that is, mutant COMP does not accumulate in the ER, but the unfolded protein and cell stress response promote a reduction in chondrocyte proliferation and an increase in apoptosis [26]. Interfering with the formation and assembly of other extracellular matrix proteins, including collagen, aggrecan, fibronectin and matrilin, is another pathogenic mechanism of mutant COMP [8].
Most patients harboring COMP variants are mostly born with a normal appearance and birth length and weight, regardless of the PSACH or MED1 phenotype [4]. Although the proportion of patients with a positive family history for these two disorders in the whole population is unknown, it was over 50% in the current cohort, which can be explained by selection bias. In addition, the onset age was approximately 1.5 years in this cohort, although the median age of definitive diagnosis was approximately 8 years, with a 6.5-year delay. The three most common chief complaints are linear growth retardation, waddling gait and bending of the lower limbs. The prominent clinical manifestations of PSACH are disproportionate short stature accompanied by severe skeletal deformities, including lumbar lordosis, sacrum kyphosis, genu valgum/varum; shortened long bones and tubular bones; and even joint dislocation [30]. Overall, the clinical characteristics of MED1 patients include mainly mild-to-moderate short stature and early-onset arthritis [31], especially in the hip [32], and skeletal deformities are milder than those of PSACH patients, even without notable skeletal deformities [30].
Regarding height, PSACH patients can be extremely short. In this cohort, the mean Z-score was − 8.06, and the height of the adult patients was more severely affected than that of the minors. The final adult height of PSACH is always less than 142 cm [33], but a height of 155 cm was reached in male patients [34]. It is worth mentioning that the height Z-score of PSACH correlates significantly negatively with age at evaluation and the clinical manifestation score, which indicates that the height of these individuals continues to fall behind that of their peers as they grow older and that the more severe the clinical manifestation is, the greater the height impairment. Compared with that of PSACH patients, the height of MED1 patients is less impaired, with the final adult height usually being over 150 cm [33]. Over half of the PSACH patients in this cohort appeared to be overweight or obese, which might be related to a reduction in activity ability and shorter duration of activity due to the lessened ability to engage in it or due to the influence and regulation of COMP in adipose tissue. A murine study found that accumulation of mutant COMP protein in cells can upregulate the expression of miR-223, interfering with the balance of adipogenesis and osteogenesis and reducing bone mineral density, bone mass, bone mechanical strength and subchondral bone thickness [35]. Thus, it is necessary to pay attention to problems such as obesity and metabolism in patients with COMP variants in the long term.
In PSACH patients, biochemical markers, especially bone metabolic markers, are usually within the normal range, although some have vitamin D deficiency. Although measurement of serum COMP levels is an effective way to differentiate PSACH patients, it has not been applied in clinical practice to date. In general, circulating COMP levels of PSACH and MED1 patients are significantly lower than those in the normal population [33,36,37]. Mabuchi et al. reported that the plasma COMP levels of patients with COMP variants, including PSACH and MED1 phenotypes, were significantly lower than those of control subjects; there was no difference in plasma COMP levels between PSACH and MED1, but among patients with MED, the plasma COMP level was higher in those with COMP variants than in those without COMP variants [33]. It has been proposed that as the level of mutant COMP accumulation in the ER increases, the level of COMP released into the circulation decreases, leading to a more severe patient condition. Thus, correlations between serum COMP levels and important parameters, including Z-scores of height and BMI, the clinical manifestation score and radiological score, were analyzed, but showed no significant correlations.
The X-ray features of PSACH indicate that almost all bones, except for the skull, are affected [38], and the changes mainly include cup-shaped changes in both ends of the ribs on chest plain film, lumbar lordosis, kyphosis, scoliosis, vertebra double-convex deformation and a corresponding widening of the intervertebral space on spine lateral film, a small pelvis, irregular acetabular margin, shortening of long tubular bones, metaphyseal dilation and structural disorders, and articular surface inclination. The X-ray characteristics of MED1 are not as severe as those of PSACH, with the main features of late ossifying and irregular epiphyses, brachydactyly, and short metacarpals being evident with MED1; however, disorganization of the metaphysis in long bones is not as common in MED1 [5]. Moreover, the incidence of spinal involvement in MED1 is notably low, and the shape of the vertebrae and spinal curvature are usually normal [39]. Despite little value in predicting the height impairment of patients, the radiological scoring system may be helpful for differentiating PSACH and MED1. Unfortunately, there is no related research evaluating bone mineral density or bone microarchitecture in these patients. However, an animal study showed that the bone mineral density of the femur, trabecular number, trabecular thickness, cortical thickness and mechanical properties of Comp-mutant mice were lower than those of wild-type mice [35]. The long-term bone health condition of patients deserves further attention.
In this study, 12 COMP gene variants were detected in 14 affected families, including 4 novel variants. The percentage of de novo variants in this cohort reached 41.7%. Kennedy et al. reported that at least 22% of individuals with COMP pathogenic variants carry de novo mutations [40], while other literature reports a rate of 70–80% [24]. The hotspot variant is c.1417_1419delGAC (p.Asp473del), accounting for 16–30% of all cases worldwide [1,3,37]. Briggs summarized 300 types of COMP variants and found that missense variants in the T3-6/7/8 domains are significantly associated with the PSACH phenotype and that missense variants in the T3-4/5 domains are significantly associated with the MED1 phenotype [1]. Based on this, variants in our cohort were divided into the T3-6/7/8 group and T3-1/2/CTD group. Both the height Z-score and serum COMP level were lower in the former than in the latter, indicating that the condition of the patients with COMP T3-6/7/8 domain variants might be more severe. COMP is the only pathogenic gene for PSACH known to date; it accounts for 50% of the etiologies of multiple epiphyseal dysplasia [41], and other pathogenic genes causing multiple epiphyseal dysplasia include COL9A1, COL9A2, COL9A3, SLC26A2, CANT1 and MATN3 [12,42]. Because it is difficult to distinguish mild PSACH from severe MED1 and considering that both are caused by COMP variants and show overlap in clinical phenotype, these two phenotypes might be combined and termed “spondyloepiphyseal dysplasia, COMP type”.
At present, treatment for patients with COMP variants is limited and involves mainly symptomatic treatment. rhGH injection does not seem to be the ideal therapy for PSACH patients; indeed, in this study, one patient showed no height gain after rhGH therapy, and the other withdrew from rhGH therapy due to worsened bending of the lower limbs. As early as 2003, Kanazawa et al. reported that rhGH does not improve the height or growth rate effectively in patients with PSACH, although the levels of IGF-1 in PSACH patients significantly improved [43]. Moreover, rhGH therapy can promote bone growth but can also result in adverse events such as worsened kyphosis and lumbar lordosis due to weak ligaments and matrix, which cannot support muscle tonus or withstand the effects of gravity [43]. Thus, rhGH therapy is not recommended for patients with PSACH. Analgesics may be used for patients with joint pain, and some patients undergo functional reconstruction operations, such as hip or knee replacement and lower-limb orthopedic surgery. Novel and potential therapies for PSACH include anti-inflammatory/antioxidant drugs such as aspirin and resveratrol, antisense oligonucleotides, and even gene therapy via a knockdown approach [24,44].
The strengths of this study are as follows. Clinical manifestation and radiological scoring systems for disorders with COMP variants are proposed for the first time. The BMI of these patients was also considered, and attention should be given to the long-term metabolic function of these patients. Moreover, the levels of serum COMP in patients with PSACH were measured and compared with those in healthy controls, and further correlations with anthropometric parameters, bone metabolic markers, and clinical and radiological scores were analyzed. In addition, four novel variants were identified, and the relationship between phenotype and genotype was explored. However, there are also some limitations. First, the number of cases was limited, and this was especially so for the MED1 cases, the number of which was insufficient for distinguishing the two phenotypes by means of the scoring systems. Second, the clinical manifestation and radiological scoring systems are still in the initial stage of application, and the scoring items and algorithms need to be improved. Third, at present, the measurement of serum COMP has been used only for scientific research and has not been widely applied in clinical practice. Finally, there is no further study on the metabolism, bone mineral density, bone microarchitecture or body composition of these patients.
In conclusion, patients with COMP variants are characterized by short stature with skeletal deformities and osteoarthropathy to different degrees. Scoring systems of clinical manifestations and radiology, serum COMP level detection and the domain in which the mutation is located may be helpful to evaluate the severity of a patient's condition. Four novel COMP gene variants were identified in this cohort, involving the phenotypes of PSACH and MED1. Overall, PSACH and MED1 are suggested to combine to produce “spondyloepiphyseal dysplasia, COMP type”. Current therapies for these patients are limited, and new therapies need to be developed for clinical application.
Data Availability
The raw datasets generated and/or analyzed during this study are not publicly available but are available from the corresponding author upon reasonable request.
Change history
04 March 2023
Missing ESM files has been added in the article.
Abbreviations
- PSACH:
-
Pseudoachondroplasia
- MED1:
-
Multiple epiphyseal dysplasia type 1
- COMP:
-
Cartilage oligomeric matrix protein
- NTD:
-
N-terminal domain
- T2:
-
Epidermal-growth factor-like domains
- T3:
-
Calmodulin-like domains
- CTD:
-
C-terminal domain
- BMI:
-
Body mass index
- KDOQI:
-
Kidney Disease Outcomes Quality Initiative
- PCR:
-
Polymerase chain reaction
- M ± SD:
-
Mean ± standard deviation
- IQR:
-
Interquartile range
- y.o.:
-
Years old
- GH:
-
Growth hormone
- IGF-1:
-
Insulin-like growth factor 1
- Ca:
-
Calcium
- P:
-
Phosphorus
- ALP:
-
Alkaline phosphatase
- β-CTX:
-
C-terminal cross-linking telopeptide of type I collagen
- 25OHD:
-
25-Hydroxyvitamin D
- rhGH:
-
Recombinant human growth hormone
- ER:
-
Endoplasmic reticulum
References
Briggs MD, Brock J, Ramsden SC, Bell PA (2014) Genotype to phenotype correlations in cartilage oligomeric matrix protein associated chondrodysplasias. Eur J Hum Genet 22:1278–1282. https://doi.org/10.1038/ejhg.2014.30
Briggs MD, Hoffman SM, King LM, Olsen AS, Mohrenweiser H, Leroy JG, Mortier GR, Rimoin DL, Lachman RS, Gaines ES et al (1995) Pseudoachondroplasia and multiple epiphyseal dysplasia due to mutations in the cartilage oligomeric matrix protein gene. Nat Genet 10:330–336. https://doi.org/10.1038/ng0795-330
Hecht JT, Nelson LD, Crowder E, Wang Y, Elder FF, Harrison WR, Francomano CA, Prange CK, Lennon GG, Deere M et al (1995) Mutations in exon 17B of cartilage oligomeric matrix protein (COMP) cause pseudoachondroplasia. Nat Genet 10:325–329. https://doi.org/10.1038/ng0795-325
Briggs MD, Wright MJ (1993) Pseudoachondroplasia. In: Adam MP, Ardinger HH, Pagon RA, Wallace SE, Bean LJH, Stephens K, Amemiya A (eds) GeneReviews((R)). University of Washington, Seattle (Updated 16 Aug 2018)
Unger S, Bonafe L, Superti-Furga A (2008) Multiple epiphyseal dysplasia: clinical and radiographic features, differential diagnosis and molecular basis. Best Pract Res Clin Rheumatol 22:19–32. https://doi.org/10.1016/j.berh.2007.11.009
Briggs MD, Wright MJ, Mortier GR (1993) Multiple epiphyseal dysplasia, autosomal dominant. In: Adam MP, Ardinger HH, Pagon RA, Wallace SE, Bean LJH, Stephens K, Amemiya A (eds) GeneReviews((R)). University of Washington, Seattle (Updated 25 April 2019)
Posey KL, Hayes E, Haynes R, Hecht JT (2004) Role of TSP-5/COMP in pseudoachondroplasia. Int J Biochem Cell Biol 36:1005–1012. https://doi.org/10.1016/j.biocel.2004.01.011
Acharya C, Yik JH, Kishore A, Van Dinh V, Di Cesare PE, Haudenschild DR (2014) Cartilage oligomeric matrix protein and its binding partners in the cartilage extracellular matrix: interaction, regulation and role in chondrogenesis. Matrix Biol J Int Soc Matrix Biol 37:102–111. https://doi.org/10.1016/j.matbio.2014.06.001
Tan K, Duquette M, Joachimiak A, Lawler J (2009) The crystal structure of the signature domain of cartilage oligomeric matrix protein: implications for collagen, glycosaminoglycan and integrin binding. FASEB J Off Publ Fed Am Soc Exp Biol 23:2490–2501. https://doi.org/10.1096/fj.08-128090
Newton G, Weremowicz S, Morton CC, Copeland NG, Gilbert DJ, Jenkins NA, Lawler J (1994) Characterization of human and mouse cartilage oligomeric matrix protein. Genomics 24:435–439. https://doi.org/10.1006/geno.1994.1649
Kleerekoper Q, Hecht JT, Putkey JA (2002) Disease-causing mutations in cartilage oligomeric matrix protein cause an unstructured Ca2+ binding domain. J Biol Chem 277:10581–10589. https://doi.org/10.1074/jbc.M109944200
Unger S, Hecht JT (2001) Pseudoachondroplasia and multiple epiphyseal dysplasia: new etiologic developments. Am J Med Genet 106:244–250
Di Cesare PE, Fang C, Leslie MP, Tulli H, Perris R, Carlson CS (2000) Expression of cartilage oligomeric matrix protein (COMP) by embryonic and adult osteoblasts. J Orthop Res Off Publ Orthop Res Soc 18:713–720. https://doi.org/10.1002/jor.1100180506
Chen FH, Thomas AO, Hecht JT, Goldring MB, Lawler J (2005) Cartilage oligomeric matrix protein/thrombospondin 5 supports chondrocyte attachment through interaction with integrins. J Biol Chem 280:32655–32661. https://doi.org/10.1074/jbc.M504778200
Chen FH, Herndon ME, Patel N, Hecht JT, Tuan RS, Lawler J (2007) Interaction of cartilage oligomeric matrix protein/thrombospondin 5 with aggrecan. J Biol Chem 282:24591–24598. https://doi.org/10.1074/jbc.M611390200
Thur J, Rosenberg K, Nitsche DP, Pihlajamaa T, Ala-Kokko L, Heinegard D, Paulsson M, Maurer P (2001) Mutations in cartilage oligomeric matrix protein causing pseudoachondroplasia and multiple epiphyseal dysplasia affect binding of calcium and collagen I, II, and IX. J Biol Chem 276:6083–6092. https://doi.org/10.1074/jbc.M009512200
Li H, Ji C, Zong X, Zhang Y (2009) Height and weight standardized growth charts for Chinese children and adolescents aged 0 to 18 years. Chin J Pediatr 47:487–492
Li H, Ji C, Zong X, Zhang Y (2009) Body mass index growth carves for Chinese children and adolescents aged 0 to 18 years. Chin J Pediatr 47:493–498
KW Group (2009) KDOQI Clinical Practice Guideline for Nutrition in Children with CKD: 2008 update. Executive summary. Am J Kidney Dis Off J Natl Kidney Found 53:S11-104. https://doi.org/10.1053/j.ajkd.2008.11.017
Rauchenzauner M, Schmid A, Heinz-Erian P, Kapelari K, Falkensammer G, Griesmacher A, Finkenstedt G, Högler W (2007) Sex- and age-specific reference curves for serum markers of bone turnover in healthy children from 2 months to 18 years. J Clin Endocrinol Metab 92:443–449. https://doi.org/10.1210/jc.2006-1706
Briggs MD, Chapman KL (2002) Pseudoachondroplasia and multiple epiphyseal dysplasia: mutation review, molecular interactions, and genotype to phenotype correlations. Hum Mutat 19:465–478. https://doi.org/10.1002/humu.10066
Yu WJ, Zhang Z, He JW, Fu WZ, Wang C, Zhang ZL (2016) Identification of two novel mutations in the COMP gene in six families with pseudoachondroplasia. Mol Med Rep 14:2180–2186. https://doi.org/10.3892/mmr.2016.5486
Posey KL, Veerisetty AC, Liu P, Wang HR, Poindexter BJ, Bick R, Alcorn JL, Hecht JT (2009) An inducible cartilage oligomeric matrix protein mouse model recapitulates human pseudoachondroplasia phenotype. Am J Pathol 175:1555–1563. https://doi.org/10.2353/ajpath.2009.090184
Posey KL, Hecht JT (2017) Novel therapeutic interventions for pseudoachondroplasia. Bone 102:60–68. https://doi.org/10.1016/j.bone.2017.03.045
Svensson L, Aszodi A, Heinegard D, Hunziker EB, Reinholt FP, Fassler R, Oldberg A (2002) Cartilage oligomeric matrix protein-deficient mice have normal skeletal development. Mol Cell Biol 22:4366–4371. https://doi.org/10.1128/MCB.22.12.4366-4371.2002
Pirog-Garcia KA, Meadows RS, Knowles L, Heinegard D, Thornton DJ, Kadler KE, Boot-Handford RP, Briggs MD (2007) Reduced cell proliferation and increased apoptosis are significant pathological mechanisms in a murine model of mild pseudoachondroplasia resulting from a mutation in the C-terminal domain of COMP. Hum Mol Genet 16:2072–2088. https://doi.org/10.1093/hmg/ddm155
Posey KL, Coustry F, Hecht JT (2018) Cartilage oligomeric matrix protein: COMPopathies and beyond. Matrix Biol J Int Soc Matrix Biol 71–72:161–173. https://doi.org/10.1016/j.matbio.2018.02.023
Posey KL, Coustry F, Veerisetty AC, Liu P, Alcorn JL, Hecht JT (2012) Chop (Ddit3) is essential for D469del-COMP retention and cell death in chondrocytes in an inducible transgenic mouse model of pseudoachondroplasia. Am J Pathol 180:727–737. https://doi.org/10.1016/j.ajpath.2011.10.035
Pirog KA, Irman A, Young S, Halai P, Bell PA, Boot-Handford RP, Briggs MD (2014) Abnormal chondrocyte apoptosis in the cartilage growth plate is influenced by genetic background and deletion of CHOP in a targeted mouse model of pseudoachondroplasia. PLoS ONE 9:e85145. https://doi.org/10.1371/journal.pone.0085145
Jackson GC, Mittaz-Crettol L, Taylor JA, Mortier GR, Spranger J, Zabel B, Le Merrer M, Cormier-Daire V, Hall CM, Offiah A, Wright MJ, Savarirayan R, Nishimura G, Ramsden SC, Elles R, Bonafe L, Superti-Furga A, Unger S, Zankl A, Briggs MD (2012) Pseudoachondroplasia and multiple epiphyseal dysplasia: a 7-year comprehensive analysis of the known disease genes identify novel and recurrent mutations and provides an accurate assessment of their relative contribution. Hum Mutat 33:144–157. https://doi.org/10.1002/humu.21611
Sakamoto Y, Yamamoto T, Kajino Y, Kabata T, Tsuchiya H, Miyake N, Iwamoto Y, Matsumoto N, Ikegawa S (2017) Multiple epiphyseal dysplasia mimicking osteoarthritis due to acetabular dysplasia: a report of a familial case with a COMP mutation. J Orthop Sci Off J Jpn Orthop Assoc 22:967–971. https://doi.org/10.1016/j.jos.2016.01.010
Shao J, Zhao S, Yan Z, Wang L, Zhang Y, Lin M, Yu C, Wang S, Niu Y, Li X, Qiu G, Zhang J, Wu Z, Wu N (2020) A novel COMP mutation in a Chinese family with multiple epiphyseal dysplasia. BMC Med Genet 21:115. https://doi.org/10.1186/s12881-020-01040-y
Mabuchi A, Momohara S, Ohashi H, Takatori Y, Haga N, Nishimura G, Ikegawa S (2004) Circulating COMP is decreased in pseudoachondroplasia and multiple epiphyseal dysplasia patients carrying COMP mutations. Am J Med Genet A 129:35–38. https://doi.org/10.1002/ajmg.a.30164
Guo BB, Jin JY, Yuan ZZ, Zeng L, Xiang R (2021) A novel COMP mutated allele identified in a Chinese family with pseudoachondroplasia. BioMed Res Int 2021:6678531. https://doi.org/10.1155/2021/6678531
Coustry F, Posey KL, Maerz T, Baker K, Abraham AM, Ambrose CG, Nobakhti S, Shefelbine SJ, Bi X, Newton M, Gawronski K, Remer L, Veerisetty AC, Hossain MG, Chiu F, Hecht JT (2018) Mutant cartilage oligomeric matrix cartilage (COMP) compromises bone integrity, joint function and the balance between adipogenesis and osteogenesis. Matrix Biol J Int Soc Matrix Biol. https://doi.org/10.1016/j.matbio.2017.12.014
Tufan AC, Satiroglu-Tufan NL, Jackson GC, Semerci CN, Solak S, Yagci B (2007) Serum or plasma cartilage oligomeric matrix protein concentration as a diagnostic marker in pseudoachondroplasia: differential diagnosis of a family. Eur J Hum Genet 15:1023–1028. https://doi.org/10.1038/sj.ejhg.5201882
Liu FX, Li ZL, Wei ZJ, Meng Y, Ren CA, Zhang XD, Yu MX, Huang SZ (2010) Genetic analysis and serum level of cartilage oligomeric matrix protein in patients with pseudoachondroplasia. Chin Med J 123:2181–2184
Weiner DS, Guirguis J, Makowski M, Testa S, Shauver L, Morgan D (2019) Orthopaedic manifestations of pseudoachondroplasia. J Child Orthop 13:409–416. https://doi.org/10.1302/1863-2548.13.190066
Mabuchi A, Manabe N, Haga N, Kitoh H, Ikeda T, Kawaji H, Tamai K, Hamada J, Nakamura S, Brunetti-Pierri N, Kimizuka M, Takatori Y, Nakamura K, Nishimura G, Ohashi H, Ikegawa S (2003) Novel types of COMP mutations and genotype–phenotype association in pseudoachondroplasia and multiple epiphyseal dysplasia. Hum Genet 112:84–90. https://doi.org/10.1007/s00439-002-0845-9
Kennedy J, Jackson G, Ramsden S, Taylor J, Newman W, Wright MJ, Donnai D, Elles R, Briggs MD (2005) COMP mutation screening as an aid for the clinical diagnosis and counselling of patients with a suspected diagnosis of pseudoachondroplasia or multiple epiphyseal dysplasia. Eur J Hum Genet 13:547–555. https://doi.org/10.1038/sj.ejhg.5201374
Anthony S, Munk R, Skakun W, Masini M (2015) Multiple epiphyseal dysplasia. J Am Acad Orthop Surg 23:164–172. https://doi.org/10.5435/JAAOS-D-13-00173
Balasubramanian K, Li B, Krakow D, Nevarez L, Ho PJ, Ainsworth JA, Nickerson DA, Bamshad MJ, Immken L, Lachman RS, Cohn DH (2017) MED resulting from recessively inherited mutations in the gene encoding calcium-activated nucleotidase CANT1. Am J Med Genet A 173:2415–2421. https://doi.org/10.1002/ajmg.a.38349
Kanazawa H, Tanaka H, Inoue M, Yamanaka Y, Namba N, Seino Y (2003) Efficacy of growth hormone therapy for patients with skeletal dysplasia. J Bone Miner Metab 21:307–310. https://doi.org/10.1007/s00774-003-0425-7
Posey KL, Coustry F, Veerisetty AC, Hossain M, Alcorn JL, Hecht JT (2015) Antioxidant and anti-inflammatory agents mitigate pathology in a mouse model of pseudoachondroplasia. Hum Mol Genet 24:3918–3928. https://doi.org/10.1093/hmg/ddv122
Acknowledgements
Our deepest thanks to all of the participants in this study and Dr. Yuelun Zhang for whose kind help in statistics. This study was supported by the National Natural Science Foundation of China (Nos. 81900811, 81170805, and 81670714), and the Chinese Academy of Medical Sciences-CAMS Innovation Fund for Medical Sciences (CAMS-2016–12 M-3-003).
Author information
Authors and Affiliations
Contributions
WBX designed the study and revised the manuscript. HTL and YFH analyzed the genetic results. HTL draft the manuscript. QQP sampled the serum. YJ, OW, ML, XPX and HJZ collected the clinical information of the patients. HTL and WBX are responsible for the integrity of the data analysis. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical Approval
The study was performed with the approval of the Ethics Committee of Peking Union Medical College Hospital (JS-1689).
Informed Consent
All of the subjects agreed to participate in this study and signed informed consent forms.
Consent to Publication
All of the authors agreed to publish the manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liang, H., Hou, Y., Pang, Q. et al. Clinical, Biochemical, Radiological, Genetic and Therapeutic Analysis of Patients with COMP Gene Variants. Calcif Tissue Int 110, 313–323 (2022). https://doi.org/10.1007/s00223-021-00920-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00223-021-00920-6