Abstract
We report a retrospective analysis of a nationwide health database to study the association between sodium-glucose cotransporter-2 inhibitor (SGLT2I) use and the incidence of adverse clinical outcomes among heart failure (HF) patients with and without atrial fibrillation (AF) stratified by CHA2DS2–VASc score. The outcome of this study was on the development of adverse events, including acute myocardial infarction (AMI), hemorrhagic stroke, ischemic stroke, cardiovascular (CV) death, and all-cause mortality. By dividing the number of adverse events by the total person-years, the incidence rate was calculated. The hazard ratio (HR) was estimated by the Cox proportional hazard model. A total of 95% confidence interval (CI) was also presented to show the risk of adverse events for HF patients with and without AF taking SGLT2I. SGLT2I users had a lower risk of AMI (adjusted HR = 0.83; 95% CI = 0.74, 0.94), CV death (adjusted HR = 0.47; 95% CI = 0.42, 0.51), and all-cause death (adjusted HR = 0.39; 95% CI = 0.37, 0.41). Considering HF patients without AF and SGLT2I as the reference group, HF patients without AF but with SGLT2I had a reduced risk of adverse outcomes of 0.48 (95% CI = 0.45, 0.50), and HF patients with AF and SGLT2I had the decreased hazard ratio of 0.55 (95% CI = 0.50, 0.61). The adjusted HR of adverse outcomes for HF patients with CHA2DS2–VASc score less than 2 and SGLT2I without and with AF relative to HF patients without AF nor SGLT2I were 0.53 (95% CI = 0.41, 0.67) and 0.24 (95% CI = 0.12, 0.47), respectively. Compared to HF patients with no history of AF and SGLT2I, if patients additionally with SGLT2I and CHA2DS2–VASc score ≥ 2, the risk of the adverse outcomes was reduced with adjusted HR of 0.48 (95% CI = 0.45, 0.50); if patients additionally with AF and CHA2DS2–VASc score ≥ 2, the risk of the adverse outcomes was decreased with adjusted HR of 0.88 (95% CI = 0.80, 0.97); if patients additionally with AF, SGLT2I, and CHA2DS2–VASc score ≥ 2, the risk of the adverse outcomes was diminished with adjusted HR of 0.52 (95% CI = 0.47, 0.58). We concluded that SGLT2I has a protective effect in HF patients, and the risk reduction is greater with a score of < 2 and without AF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Heart failure (HF) and atrial fibrillation (AF) are extremely closely linked (Anter et al. 2009; Lubitz et al. 2010; Kotecha and Piccini 2015; Ferreira and Santos 2015; Hu and Lin 2022). The situation would be very complicated when these two entities coexist (Anter et al. 2009; Lubitz et al. 2010; Kotecha and Piccini 2015; Ferreira and Santos 2015; Hu and Lin 2022). The vital role of sodium-glucose cotransporter-2 inhibitor (SGLT2I) in the HF population and the widespread use of SGLT2I in this population is well established (Packer et al. 2020; McMurray et al. 2019). However, a comparison of developing major adverse cardiac and cerebrovascular events (MACCE) in HF patients with and without AF who received SGLT2I remained unknown.
CHA2DS2–VASc score, once developed to quantify the comorbidity or complications in AF and potentially better predict the risk of stroke in people with AF, is widely penetrating into different risk stratification schemes currently (Hu and Lin 2019a, 2019b; Hu and Lin 2017; Yaşar et al. 2022a, 2022b). In general, it is also possible to use the above score as an indicator of patient selection for the further decision-making process.
To identify this certainly novel research question of the role of SGLT2I for primary prevention of poor outcomes in a large HF cohort, the authors extracted data from Taiwan’s National Health Insurance Research Database (NHIRD), a well-validated nationwide big database, to detect whether HF taking SGLT2I have a lower risk of adverse clinical events. Further subgroup analysis according to with and without AF and stratified by CHA2DS2–VASc score would also be performed.
Methods
Data source
In 1995, the Taiwan government promoted a single-payer National Health Insurance program to improve the national welfare. The insurance information, which contains demographic data, disease diagnosis, medicine records, and therapy records, of beneficiaries has been collected and stored in NHIRD. Currently, NHIRD involves the medical history of the residents for at least two decades. The International Classification of Diseases, Ninth & Tenth Revision, and Clinical Modification (ICD-9-CM, ICD-10-CM) are used for the coding. This study was approved by the Institutional Review Board of China Medical University Hospital Research Ethics Committee (CMUH109-REC2-031(CR-2)).
Study population
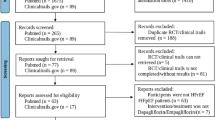
Patients with at least three times of outpatient visits or one admission record of HF (ICD-9-CM code 428; ICD-10CM code I50) were enrolled for the study population in this cohort study. We further divided participants into SGLT2I users and non-users. The index date of the SGLT2I users was the first prescription day of SGLT2I, and that of the SGLT2I non-users was a random date after the diagnosis date of HF. The study period was between 2016 and 2019. Patients who were aged below 20, without information of gender, with an index date before 2016 or after 2018, or who developed outcomes before the index date were eliminated. SGLT2I non-users with similar characteristics, which is according to the propensity score calculated by the logistic model with covariates of sex, age, comorbidities, and medicines, to the SGLT2I users, were selected as the control group. The matched ratio was 1:1.
Main outcome and confounders
The primary outcome of the study was defined as patients with adverse events, including acute myocardial infarction (AMI) (ICD-9-CM code 410; ICD-10CM code I21, I22), hemorrhagic stroke (ICD-9-CM code 431,432; ICD-10-CM code I61, I62), ischemic stroke (ICD-9-CM code 433, 434, 436; ICD-10-CM code I63, I65, I66, I67.89), cardiovascular (CV) death, and all-cause mortality. Patients who developed any one of the events will be counted as the outcome occurs and the follow-up time will be recorded to the day of the first outcome. The following comorbidities which related to outcomes and developed before the index date were included for the adjustment, AF (ICD-9-CM code 427.3; ICD-10-CM code I48), diabetes (ICD-9-CM code 250; ICD-10-CM code E08-E13), hyperlipidemia (ICD-9-CM code 272; ICD-10-CM code E77, E78), hypertension (ICD-9-CM code 410–405; ICD-10-CM code I10-I15), chronic kidney disease (ICD-9-CM code 585; ICD-10-CM code N18), chronic obstructive pulmonary disease (COPD) (ICD-9-CM code 491, 492, 496; ICD-10-CM code J41-J44), AMI (ICD-9-CM code 410; ICD-10-CM code I21, I22), and stroke (ICD-9-CM code 430–438; ICD-10-CM code I60-I69). Medicines such as aspirin, colopidogrel, warfarin, novel oral anticoagulant drugs (NOACs), amiodarone, dronedarone, angiotensin-converting enzyme inhibitors(ACEIs), angiotensin II receptor blockers (ARBs), α-blockers, β-blockers, calcium channel blockers (CCBs), diuretics, sacubitril/valsartan, and statins used before the index date were considered too.
Statistical analysis
Baseline variables about the case group and control group were summarized by number with percentage for categorical variables and mean with standard deviation for continuous variables. To examine the difference in the characteristics between SGLT2I users and non-users, the standard mean difference was computed. By dividing the number of adverse events by the total person-years, we had the incidence rate. The hazard ratio (HR) was estimated by the Cox proportional hazard model. A total of 95% confidence interval (CI) was also presented. The univariable model was used for crude HR, and the multivariable model was used for adjusted HR. Kaplan–Meier method was adopted to plot the cumulative incidence curves of the outcomes. And the curves were asses by the Log-rank test. All statistical analyses were performed by SAS software, version 9.4 (SAS Institute Inc., Cary, NC). A significance level was set as a p-value less than 0.05.
Results
The cohort study consisted of 17,588 SGLT2I users and 17,588 SGLT2I non-users. As shown as Table 1, the distributions of gender and age group within two groups were similar. The proportions of each comorbidities had no difference between SGLT2I users and non-users. Besides, diabetes, hypertension, and hyperlipidemia were the most common comorbidities in this study. The drug prescription pattern in the two group was similar, and the most common medicines were ARBs. The mean of the follow-up time for SGLT2I users was 1.75(± 1.01) years and that for SGLT2I non-users was 1.99(± 0.88) years.
Table 2 presents the associated of the covariates and the adverse outcomes. The adjusted hazard ratio of adverse events for SGLT2I users relative to SGLT2I non-users was 0.50 (95% CI = 0.48 0.53). Male patients were more likely to have an adverse outcome compared to female patients, and the adjusted HR was 1.18 (95% CI = 1.12, 1.25). If we consider patients younger than 50 years old as a reference group, 50–59-year-old patients and greater than 60-year-old patients increase the risk of adverse outcomes by 1.11 folds (95% CI = 1.00, 1.23) and 1.59 folds (95% CI = 1.45, 1.74), respectively. Patients with diabetes (adjusted HR = 1.25; 95% CI = 1.10, 1.41), chronic kidney disease (adjusted HR = 1.65; 95% CI = 1.56, 1.73), COPD (adjusted HR = 1.08; 95% CI = 1.03, 1.14), AMI (adjusted HR = 1.36; 95% CI = 1.28, 1.44), and stroke (adjusted HR = 1.56; 95% CI = 1.49, 1.64) will increase the risk of adverse outcomes. Patients with hyperlipidemia (adjusted HR = 0.84; 95% CI = 0.80, 0.89) reduce the risk of adverse outcomes. For the medications, clopidogrel (adjusted HR = 1.15; 95% CI = 1.09, 1.21), amiodarone (adjusted HR = 1.24; 95% CI = 1.16, 1.31), ACEIs (adjusted HR = 1.09; 95% CI = 1.04, 1.14), CCBs (adjusted HR = 1.08; 95% CI = 1.00, 1.16), and diuretics (adjusted HR = 2.22; 95% CI = 2.02, 2.43) were the risk factors of adverse outcomes. However, dronedarone (adjusted HR = 0.75; 95% CI = 0.59, 0.96), ARBs (adjusted HR = 0.87; 95% CI = 0.81, 0.94), β-blockers (adjusted HR = 0.90; 95% CI = 0.86, 0.95), and statins (adjusted HR = 0.84; 95% CI = 0.79, 0.89) were the protection factors of the adverse outcomes.
To look into the risk of the individual adverse outcome, SGLT2I users had a lower risk of AMI (adjusted HR = 0.83; 95% CI = 0.74, 0.94), CV death (adjusted HR = 0.47; 95% CI = 0.42, 0.51), and all-cause death (adjusted HR = 0.39; 95% CI = 0.37, 0.41), see Table 3. The cumulative incidence of adverse outcomes in SGLT2I users were lower than that of the SGLT2I non-users, see Fig. 1.
According to Table 4, patients who used SGLT2I for 1–447 days had a reduced risk of adverse outcomes (adjusted HR = 0.88, 95% CI = 0.84, 0.93), and SGLT2I users for more than 448 days had a lower risk of adverse outcomes (adjusted HR = 0.15, 95% CI = 0.14, 0.17) compared to SGLT2I non-users.
Table 5 illustrates the relationship between SGLT2I and adverse outcomes stratified by AF and CHA2DS2-VASc score. When considering HF patients without AF and SGLT2I as the reference group, HF patients without AF but used SGLT2I reduce the risk of adverse outcomes to 0.48 (95% CI = 0.45, 0.50), and HF patients with AF and SGLT2I had the adjusted HR of 0.55 (95% CI = 0.50, 0.61). The adjusted HR of adverse outcomes for HF patients with CHA2DS2-VASc score less than 2 and SGLT2I without and with AF relative to HF patients without AF nor SGLT2I were 0.53 (95% CI = 0.41, 0.67) and 0.24 (95% CI = 0.12, 0.47), respectively. Compared to HF patients with no history of AF and SGLT2I, if patients additionally with SGLT2I and CHA2DS2-VASc score ≥ 2, the risk of the adverse outcomes was reduced with adjusted HR of 0.48 (95% CI = 0.45, 0.50); if patients additionally with AF and CHA2DS2-VASc score ≥ 2, the risk of the adverse outcomes was diminished with adjusted HR of 0.88 (95% CI = 0.80, 0.97); if patients additionally with AF, SGLT2I, and CHA2DS2-VASc score ≥ 2, the risk of the adverse outcomes was decreased with adjusted HR of 0.52 (95% CI = 0.47, 0.58).
Discussion
In this study, the authors tried to evaluate the effect of SGLT2I on adverse events risk among patients with HF with/without AF. The authors reported that the use of SGLT2I in HF patients carried a lower risk for CV events, but not cerebrovascular events.
In this retrospective cohort study using the Taiwan NHIRD, HF patients were classified according to cormorbid AF or not stratified by a score of < 2 and ≥ 2. Even in patients with HF with AF, SGLT2I has been shown to improve the outcomes. In this study, the authors use CHA2DS2–VASc score as a surrogate marker for disease severity. The authors found that patients with a score ≥ 2 had a lower risk reduction rate of developing adverse outcomes if they were treated with SGLT2I. It seems that the risk reduction rate was attenuated in those with AF and especially in the score of ≥ 2.
There is sample data from randomized controlled trials on the value of SGLT2I in events protection (Packer et al. 2020; McMurray et al. 2019). Nonetheless, a properly conducted real-world study making a significant contribution is indeed important.
Observational big-data studies can be valuable resources for teasing out signals regarding rare or unexpected outcomes. SGLT2I is indicated in HF patients according to the current practice guidelines (Li et al. 2021; Heidenreich et al. 2022). This analysis of Taiwan’s large health database is important as it confirms the protective effect of SGLT2I in HF patients. In addition, the sufficiencies in the study’s methodology and statistical planning empowered the confidence in the stated conclusions.
Concerning the role of SGLT2I therapy in HF ± AF and stratified by CHA2DS2–VASc score, there is no significant data from randomized controlled trial or mendelian studies or prospective observational studies. Thus, using the Taiwan NHI database, the aim of the study might be powerful, full of interest for the scientific community, and also be important for everyday clinical practice, and SGLT2I-associated risk reduction phenomenon was reported. The reasons for the alleviated protective effect of SGLT2I in patients with the higher scores or AF might be due to the diluted effect resulting from multiple comorbid illnesses. Moreover, the protective effect of the medication can be achieved over enough time.
Taken together, it was understood that the study suggested that the onset of adverse events in HF patients could be prevented and that SGLT2I prescription might be involved, especially in cases with no AF and with lower scores. Our observation further emphasizes the important role of this drug in HF patients for adverse outcomes prevention and SGLT2I should be initiated in the HF population as early as possible so that the beneficial effect would not be attenuated.
Limitations
Despite its large population, this claimed database is severely limited in that no detailed laboratory information is available.
In addition, the lack of data regarding the disease duration and severity which might probably make an inconclusive result. Finally, the authors collected the study population simply by ICD-9/ICD-10 codes but not by left ventricular ejection fraction per se. Other echocardiografic parameters such as left atrium volume, akinesia, hypokinesia, and thickness of the interventricular septum were also unavailable. Moreover, there is not any mention about forms of AF. Furthermore, the events of death were also collected only by ICD codes which should be underestimated such as out-of-hospital events.
Conclusions
SGLT2I is beneficial in HF population, and the effect is greater for those with a CHA2DS2–VASc score of < 2 and with no AF.
Data availability
Data are available upon reasonable request.
References
Anter E, Jessup M, Callans DJ (2009) Atrial fibrillation and heart failure: treatment considerations for a dual epidemic. Circulation 119(18):2516–2525
Ferreira JP, Santos M (2015) Heart failure and atrial fibrillation: from basic science to clinical practice. Int J Mol Sci. 16(2):3133–47
Heidenreich PA, Bozkurt B, Aguilar D, Allen LA, Byun JJ, Colvin MM, Deswal A, Drazner MH, Dunlay SM, Evers LR, Fang JC, Fedson SE, Fonarow GC, Hayek SS, Hernandez AF, Khazanie P, Kittleson MM, Lee CS, Link MS, Milano CA, Nnacheta LC, Sandhu AT, Stevenson LW, Vardeny O, Vest AR, Yancy CW (2022) 2022 AHA/ACC/HFSA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Joint Committee on clinical practice guidelines. Circulation 145(18):e895–e1032
Hu WS, Lin CL (2017) CHA2DS2-VASc score in the prediction of ischemic bowel disease among patients with atrial fibrillation: insights from a nationwide cohort. Int J Cardiol Int J Cardiol 15(235):56–60
Hu WS, Lin CL (2019a) Acute coronary syndrome, ischemic stroke and mortality prediction in patients with heart failure: a comparison of CHA2DS2-VASc and AHEAD scores. J Interv Card Electrophysiol 55(2):225–231
Hu WS, Lin CL (2019b) Comparison of CHA2DS2-VASc and AHEAD scores for the prediction of incident dementia in patients hospitalized for heart failure: a nationwide cohort study. Intern Emerg Med 14(3):395–402
Hu WS, Lin CL (2022) Weekend vs. weekday admission and clinical outcomes in heart failure patients with and without atrial fibrillation in Taiwan. Eur Heart J Cardiovasc Pharmacother 8(4):346–352
Kotecha D, Piccini JP (2015) Atrial fibrillation in heart failure: what should we do? Eur Heart J 36(46):3250–7
Li S, Vandvik PO, Lytvyn L, Guyatt GH, Palmer SC, Rodriguez-Gutierrez R, Foroutan F, Agoritsas T, Siemieniuk RAC, Walsh M, Frere L, Tunnicliffe DJ, Nagler EV, Manja V, Åsvold BO, Jha V, Vermandere M, Gariani K, Zhao Q, Ren Y, Cartwright EJ, Gee P, Wickes A, Ferns L, Wright R, Li L, Hao Q, Mustafa RA (2021) SGLT-2 inhibitors or GLP-1 receptor agonists for adults with type 2 diabetes: a clinical practice guideline. BMJ 11(373):n1091
Lubitz SA, Benjamin EJ, Ellinor PT (2010) Atrial fibrillation in congestive heart failure. Heart Fail Clin. 6(2):187–200
McMurray JJV, DeMets DL, Inzucchi SE, Køber L, Kosiborod MN, Langkilde AM, Martinez FA, Bengtsson O, Ponikowski P, Sabatine MS, Sjöstrand M, Solomon SD, DAPA-HF committees and investigators (2019) A trial to evaluate the effect of the sodium-glucose co-transporter 2 inhibitor dapagliflozin on morbidity and mortality in patients with heart failure and reduced left ventricular ejection fraction (DAPA-HF). Eur J Heart Fail. 21(5):665–675. https://doi.org/10.1002/ejhf.1432
Packer M, Anker SD, Butler J, Filippatos G, Pocock SJ, Carson P, Januzzi J, Verma S, Tsutsui H, Brueckmann M, Jamal W, Kimura K, Schnee J, Zeller C, Cotton D, Bocchi E, Böhm M, Choi DJ, Chopra V, Chuquiure E, Giannetti N, Janssens S, Zhang J, Gonzalez Juanatey JR, Kaul S, Brunner-La Rocca HP, Merkely B, Nicholls SJ, Perrone S, Pina I, Ponikowski P, Sattar N, Senni M, Seronde MF, Spinar J, Squire I, Taddei S, Wanner C, Zannad F, EMPEROR-reduced trial investigators (2020) Cardiovascular and renal outcomes with empagliflozin in heart failure. N Engl J Med. 383(15):1413–1424. https://doi.org/10.1056/NEJMoa2022190
Yaşar E, Akalın Y, Aktaş İ, Çakmak T, Karakuş Y, Bayramoğlu A (2022a) The CHA2DS2-VASc risk score predicts successful endovascular treatment in patients with acute ischemic stroke. Acta Neurol Scand 145(4):407–413
Yaşar E, Bayramoğlu A, Karakuş Y, Çakmak T (2022b) The CHA2DS2-VASc risk score predicts total occlusion in infarct-related arteries in patients with non-ST elevation myocardial infarction. Angiology 73(4):380–386
Funding
This study was supported in part by the Taiwan Ministry of Health and Welfare Clinical Trial and Research Center of Excellence (MOHW109-TDU-B-212–114004), China Medical University (CMU110-AWARD-01), and China Medical University Hospital (DMR-HHC-110–4, DMR-112–009).
Author information
Authors and Affiliations
Contributions
All authors contributed to the manuscript. All were involved in the design of the study, collected the data, performed statistical analysis, and wrote the manuscript, and all authors were involved in the final approval of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
This study was approved by the Institutional Review Board of China Medical University Hospital Research Ethics Committee (CMUH109-REC2-031(CR-2)).
Consent to participate
Not required.
Consent for publication
Not required.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hu, WS., Lin, CL. Clinical outcomes in heart failure patients with and without atrial fibrillation receiving sodium-glucose cotransporter-2 inhibitor. Naunyn-Schmiedeberg's Arch Pharmacol 396, 1977–1986 (2023). https://doi.org/10.1007/s00210-023-02425-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-023-02425-5