Abstract
Purpose: The purpose of the present study was to investigate the preventive effect of l-arginine (ARG) and carnosine (CAR) on hypoxia-induced neurotoxicity in rats. The impact on neuro-inflammation, apoptosis, angiogenesis, and the brain levels of monoamines and GABA were investigated. Methods: Rats were divided into the following: normal control, hypoxia model induced by sodium nitrite (75 mg/kg s.c), and hypoxic rats pre-treated with CAR (250 mg/kg), ARG (200 mg/kg), and their combination. Results: Data revealed that hypoxia induced significant elevation of hypoxia inducible factor-1α (HIF-1α), vascular endothelial growth factor (VEGF), and its receptor reflecting the stimulation of angiogenesis. Hypoxia also resulted in increased inflammatory mediators-including nuclear factor kappa B (NF-κB), tumor necrosis factor-alpha (TNF-α), and interleukin-6 (IL-6). In addition, hypoxia initiates cerebral apoptosis as revealed by increased caspase-3 and BAX with reduced Bcl-2. These changes were associated with reduced brain levels of GABA and monoamines including noradrenaline (NADR), dopamine (DOP), and serotonin (SER). Pre-treatment with ARG and/or CAR significantly mitigated the neural changes induced by hypoxia and attenuated the elevated levels of NF-κB, TNF-α, IL-6, caspase-3, and BAX, while ameliorated the reduced levels of Bcl-2, NADR, DOP, SER, and GABA, with the best improvement observed with the combination. Further elevation of the angiogenic markers was observed indicating their role in boosting oxygen delivery to brain. Conclusion: CAR, ARG, and, importantly, their combination could effectively protect against hypoxia-induced neurotoxicity, via their angiogenic, anti-inflammatory, and anti-apoptotic properties in addition to reversing the effect on GABA and monoamines.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hypoxia is a condition characterized by insufficient oxygen supply to tissues (Gore et al. 2007). The brain is the second body organ, after the heart, that needs continuous oxygen supply to maintain its functions. Therefore, any oxygen depletion causes severe cerebral hypoxia that eventually leads to activation of apoptotic factors initiating the cascade of cell death (Saikumar et al. 1998) and brain damage (Majmundar et al. 2010). Several factors contribute to hypoxia-induced brain damage including reduced ATP production, enhanced activity of excitatory amino acids (e.g., glutamate), uncontrolled nitrosative and oxidative stress, and inflammation (Hota et al. 2008; Abdel Baky et al. 2010). Because of its low antioxidant capacity together with the increased oxygen consumption, the brain is easily susceptible to the damage by the above factors (Sorce and Krause 2009).
Cells respond to hypoxic conditions by activating hypoxia-inducible factor (HIF), a transcription factor that regulates the response to oxygen deficiency (Dirnagl et al. 2009). For example, HIF activates several genes involved in cell survival and angiogenesis, the formation of new blood vessels, to facilitate better oxygenation of the tissue (Majmundar et al. 2010). HIF consists of an oxygen-sensitive α subunit (HIF-α) and oxygen-insensitive β subunit (Majmundar et al. 2010). Three isoforms of HIF-α are found in mammals: 1α, 2α, and 3α. Only HIF-1α is found in all cell types, and it is the main regulator of the aforementioned genes (Dirnagl et al. 2009; Majmundar et al. 2010). HIF-1α is more active during short, intense hypoxia, while HIF-2α is predominant during prolonged, mild hypoxia (Koh et al. 2011). In the present study, HIF-1α has been determined as a potential target for neuroprotection against acute hypoxia. In addition to HIF activation, it has been reported that the brain-resident macrophages (microglial cells) respond to hypoxic conditions via producing pro-inflammatory mediators such as tumor necrosis factor (Yao et al. 2013). In addition, some authors reported that hypoxia is a potential cause of tissue inflammation through the activation of nuclear factor κB (NFκB), in the tissue macrophages (Al-Rasheed et al. 2016; Rius et al. 2008).
The biogenic amines, dopamine (DOP), noradrenaline (NADR), and serotonin (SER) are preferably distributed in the brain where they regulate several behavioral, physiological, and pharmacological functions. They play an essential role in sleep, mood, anxiety, motor coordination, learning, and memory (Torda 2004; Hritcu et al. 2007; Cools 2008; Yadav et al. 2010). However, their levels in the brain are reduced in neurodegenerative conditions involving hypoxia, leading to neurochemical and behavioral abnormalities (Premanand and Ganesh 2010; Yadav et al. 2010; Biradar et al. 2013; Biradar and Joshi 2014; Rizk et al. 2017). Furthermore, it is documented that hypoxic stress leads to exaggerated release of glutamate, an excitatory neurotransmitter that causes neuronal injury (Takagi et al. 1993; Nelson et al. 2003) and contributes to seizure susceptibility in hypoxic models in rats (Rakhade et al. 2008) and mice (Grosenbaugh et al. 2018). It was shown that hypoxia-induced seizures in a neonatal rat model induce rapid phosphorylation of serine 831 and serine 845 sites of glutamate receptor, and consequently neuronal hyperexcitability and epilepsy (Rakhade et al. 2008). In addition, it is reported that pimonidazole (a marker of hypoxia)-immunopositive neurons in the brain of rats suffering from recurrent seizure supports the hypothesis that hypoxia could occur in vivo in relation to epileptic activity (Gualtieri et al. 2013). However, this neurotoxicity is antagonized by the inhibitory amino acids including gamma aminobutyric acid (GABA), suggesting the neuroprotective role of GABA against ischemic injury (Schwartz-Bloom and Sah 2001). Therefore, reduced levels of GABA may participate in the brain damage. Previous study indicates that downregulation of GABA after hypoxia-induced seizures in neonatal rats may contribute to higher epileptic susceptibility in later life (Wang et al. 2011). Collectively, the impact on the brain levels of monoamines and GABA could be a therapeutic target of the neuroprotective agents in hypoxic conditions.
Sodium nitrite (NaNO2) is commonly used for induction of hypoxia in experimental animal models (Naik et al. 2006; Attia et al. 2009; Abdel Baky et al. 2010). That is because sodium nitrite is highly reactive with hemoglobin, oxidizing Fe+2 to Fe+3 and causing methemoglobinemia, a condition in which hemoglobin has no ability to carry oxygen leading to hypoxia (Kohn et al. 2002). The administration of sodium nitrite causes oxidative stress with subsequent inflammation, apoptosis, and impaired energy metabolism, which finally aggravate organ injury including brain damage (Naik et al. 2006; Attia et al. 2009; Abdel Baky et al. 2010).
A growing body of evidences indicated that compounds having antioxidant potency are able to reduce many adverse effects of hypoxia, thereby reducing the risk of tissue injury and organ dysfunction (Naik et al. 2006; Attia et al. 2009; Abdel Baky et al. 2010; Tsai et al. 2010). In this regard, we aimed to test the beneficial effects of two natural antioxidants, carnosine (CAR) and l-arginine (ARG) on the consequences of hypoxia including inflammation, angiogenesis, and apoptosis as well as the modulatory effects on monoamines and GABA levels.
l-Arginine (ARG) is a basic amino acid that has many functions in the human body. ARG has antioxidant and anti-inflammatory activities (Ivanov et al. 2008) and can protect the tissue against ischemic–reperfusion injury (Krauss et al. 2009). The protective effects of ARG against hypoxia-induced liver and kidney damage have been reported (Ali et al. 2012; Al-Rasheed et al. 2016). Importantly, ARG elicited neuroprotection on cerebral hemic hypoxia through nitric oxide generation, antioxidant mechanisms, and the improvement of energy production in the brain (Abdel Baky et al. 2010). However, its modulating roles on the neuro-inflammation, apoptosis, angiogenesis, and the levels of neurotransmitters in hypoxic rat brain have not studied yet.
Carnosine (CAR; β-alanyl-l-histidine) is a dipeptide that is highly concentrated in mammalian tissues, particularly muscles and brain (Boldyrev et al. 2013). It possesses several properties including antioxidant (Boldyrev et al. 2004; Boldyrev et al. 2013), anti-inflammatory (Boldyrev et al. 2013), and membrane-protecting activities (Tsai et al. 2010). Previous studies revealed the beneficial role of CAR in preventing hypoxic and ischemic injuries in the liver (Fouad et al. 2007), brain (Pekcetin et al. 2009), and kidney (Al-Rasheed et al. 2016). Because of its few side effects and its ability to penetrate the blood-brain barrier (BBB) easily, the neuroprotective potentials of CAR have attracted great attention. In vitro studies demonstrated that CAR protected the neuronal cells against reactive oxygen species (ROS) (Boldyrev et al. 2004) and elicited protection against neurotoxicity in PC12 cells (Tabakman et al. 2002; shen et al. 2007). In addition, the neuroprotective effects of CAR have been demonstrated against ischemic (Stvolinskii et al. 2003; Rajanikant et al. 2007; Baek et al. 2014; Afshin-Majd et al. 2015) and hypoxic rat models (Fedorova et al. 2006), mainly via antioxidant effects. However, and like ARG, its impact on apoptosis, angiogenesis, inflammation, and the levels of monoamines and GABA in hypoxic rats’ brain have not been elucidated. Therefore, in the present work, the role of CAR, ARG, and their combination in altering the aforementioned markers was investigated.
Materials and methods
Chemicals
CAR, ARG, and sodium nitrite were purchased from Sigma-Aldrich Chemical Co (St. Louis, MO, USA). Rat ELISA kits for the assay of tumor necrosis factor-α (TNF-α) and interleukin-6 (IL-6) were obtained from R&D company (Minneapolis, MN, USA). ELISA kits for the assay of heat shock protein-70 (HSP-70), monoamines, and GABA were purchased from MyBioSource, Inc. (San Diego, CA, USA). Rat ELISA kit for the determination of brain levels of caspase-3 was purchased from Cloud-Clone Corp Co. (Houston, TX, USA). A colorimetric kit for determination of hemoglobin (Hb) was obtained from United Diagnostic Industry Co. (UDI, Dammam, Saudi Arabia). Sodium nitrite and CAR solutions were prepared by dissolving in normal saline, while ARG was suspended in 1% gum acacia/normal saline.
Animals
Fifty Wistar adult male albino rats weighing 170–200 g were obtained from the Experimental Animal house, College of Pharmacy, King Saud University, Saudi Arabia. Animals were housed in cages (five rats per cage), kept at 12-h light/dark cycle, temperature (20–22 °C), and 60% humidity. Rats were fed with standard rat pellet chow with free access to water. The experimental protocol was performed according to the National Institute of Health Guide for Animal Care and approved by the Experimental Animal Ethics Committee at King Saud University, Saudi Arabia.
Experimental design
Following overnight fast, rats were randomly divided into five groups (ten rats each) as follows: group 1: normal control administered normal saline, group 2: untreated hypoxic rats injected with sodium nitrite only (75 mg/kg, s.c.) (Naik et al. 2006; Ali et al. 2012), group 3: hypoxic rats pre-treated with ARG (200 mg/kg, i.p.) (Ali et al. 2012); group 4: hypoxic group pre-treated with CAR (250 mg/kg) (Pekcetin et al. 2009; Al-Rasheed et al. 2016); group 5: hypoxic rats pre-treated with a combination of ARG and CAR at the same doses. ARG and CAR were administered 24 h and 1 h before sodium nitrite injection.
Blood sampling and brain tissue preparation
One hour following injection of sodium nitrite, rats were anesthetized using isoflurane and sacrificed by decapitation. Blood was collected and aliquoted into two portions; one portion was collected into EDTA-containing tubes for Hb determination, and the second portion was used for serum preparation after coagulation and centrifugation. Sera were stored at − 80 °C for biochemical determinations. Rats’ brain tissues were carefully separated and gently homogenized in phosphate buffer to obtain 20% homogenate. Parts of at least three brain tissues from each group were fixed overnight in formalin, and then embedded in paraffin for staining with hematotoxylin and eosin (H & E).
Biochemical assays
Colorimetric assay of blood Hb
Hb was determined using Drabkin’s reagent (sodium bicarbonate, potassium ferricyanide, and potassium cyanide) according to the method of Kjeldsberg (1993). Briefly, 5 mL of Drabkin’s solution was mixed with 20 μL of blood. The mixture was incubated for 15 min at room temperature, and the absorbance of the produced color was read at 540 nm against blank (Drabkin’s reagent itself). The assay is based on the oxidation of Hb by potassium ferricyanide into methemoglobin which in turn reacts with potassium cyanide to form cyanomethemoglobin, which has maximum absorption at 540 nm.
ELISA assays for inflammatory markers and caspase-3
Brain levels of TNF-α, IL-6, and caspase-3 as well as the serum levels of HSP-70 were measured using Rat ELISA kits according to the instructions of the manufacturers.
Assay of gamma-amino butyric acid (GABA), noradrenaline (NADR), serotonin (SER), and dopamine (DOP)
Quantitative estimation of NADR, SER, DOP, and GABA concentrations in brain tissues was performed using ELISA kits, according to the manufacturer’s protocol. The Rat ELISA kits were obtained from MyBiosource Co. (NADR, Cat # MBS023557), serotonin (Cat # MBS725497), DOP (Cat # MBS725908), and GABA (Cat # MBS045103). Briefly, brain tissues were rinsed in phosphate buffered saline (PBS, pH 7.0) to remove excess blood. For the assay of DOP and SER, homogenate were prepared 1:1 w/v (500 mg of brain tissue homogenized in 500 μL of PBS on ice) while for determining NADR/GABA, homogenate were prepared 1:10 (10 mg tissue to 100 μL PBS). After that, the homogenates were centrifuged for 15 min at 4000 rpm. The assay is based on competitive enzyme immunoassay technique using polyclonal anti-DOP/SER/NADR/GABA antibodies and DOP/SER/NADR/GABA-HRP conjugates. 100 μL of brain sample, standard or BPS (as blank) were incubated with 50 μL DOP/SER/NADR/GABA-HRP conjugates in pre-coated plate for one hour at 37 °C. After incubation, the wells were decanted and washed five times. After washing, 100 μL of substrate for HRP enzyme was added to each well and the plate was incubated for 15 min in the dark until blue color is produced. Finally, 50 μL of stop solution was added, which will turn the solution yellow. The intensity of color was measured spectrophotometrically at 450 nm in a microplate reader. A standard curve is plotted relating the intensity of the color to the concentration of standards. The DOP/SER/NADR/GABA concentration in each sample was interpolated from this standard curve.
Quantitative real-time polymerase chain reaction (qRT-PCR) for the assay of relative mRNA levels of NF-κB (inflammatory marker), BAX (apoptotic factor), Bcl-2 (anti-apoptotic marker), and HIF-1α, VEGF&VEGF-R1 (angiogenic markers) in brain tissues
Total rat RNA was extracted from approximately 100 mg of brain tissue homogenates using RNeasy Purification Kit (Qiagen, Valencia, CA, USA), according to the manufacturer’s instructions. After verification of RNA integrity, 2 μg of RNA were reverse transcribed into cDNA using SuperScript III First-Strand Synthesis System according to the manufacturer’s protocol (Waltham, MA, USA). The quantitative RT-PCR was performed using the following primer sets for NF-κB, BAX, Bcl-2, VEGF, and VEGF-R1.
Primer name | Primer sequence |
|---|---|
NF-κB | |
Forward 5′-CATGAAGAGAAGACACTGACCATGGAAA-3′ | (329 bp) |
Reverse 5′-TGGATAGAGGCTAAGTGTAGACACG-3′ | |
BAX | |
Forward 5′-GTTGCCCTCTTCTACTTTG-3′ | (194 bp) |
Reverse 5′-AGCCACCCTGGTCTTG-3′ | |
Bcl-2 | |
Forward 5′-CGGGAGAACAGGGTATGA-3′ | (224 bp) |
Reverse 5′-CAGGCTGGAAGGAGAAGAT-3′ | |
VEGF | |
Forward 5′-GGCTCTGAAACCATGAACTTTCT-3′ | (165 bp) |
Reverse 5′-GCAGTAGCTGCGCTGGTAGAC-3′ | |
VEGFR-1 | |
Forward 5′-CAAGGGACTCTACACTTGTC-3′ | (267 bp) |
Reverse 5′-CCGAATAGCGAGCAGATTTC-3′ | |
β-actin | |
Forward 5′-GAGACCTTCAACACCCCAGC-3′ | (263 bp) |
Reverse 5′-ATGTCACGCACGATTTCCC-3′ | |
For a final volume of 25 μL, the reaction mixture contained 12.5 μL of 2X SYBR® Green Master Mix (Applied Biosystems, CA, USA), 5 μL of cDNA, 200 ng of each primer, and 5 μL RNase-free water. The amplification conditions were as follows: 1 cycle at 50 °C for 30 min, 1 cycle at 95 °C for 15 min, 40 cycles of 95 °C for 20 s, 60 °C for 30 s, and 72 °C for 30 s and finally an extension incubation at 72 °C for 5 min. Gene expression was calculated using the relative expression method (Livak; 2–ΔΔCT).Values were normalized to β-actin as the control housekeeping gene.
Histopathological examination
Small pieces of excised brain were obtained using microtome and then fixed in formalin at 4 °C for 24 h, dehydrated in ascending grades of alcohol and embedded into paraffin. Paraffin blocks were cut to prepare 5-μm-thick paraffin sections. These sections were deparaffinised, rehydrated using descending concentrations of ethanol, stained with H&E, and examined by light microscope to detect structural changes.
Statistical analysis
The data were expressed as the means ± standard error of mean (SEM). Differences between groups were determined using one-way analysis of variance (ANOVA) followed by Tukey’s Kramer multiple comparison post hoc test using GraphPad Prism 4 software (San Diego, CA, USA). The differences were considered statistically significant at P < 0.05.
Results
Effect of CAR and/or ARG on Hb concentration and serum HSP-70 levels in hypoxic rats (Table 1)
Sodium nitrite induced a highly significant decrease in Hb concentration in the hypoxic rats compared to normal control (P < 0.001). ARG, CAR, and their combination significantly attenuated this reduction compared to hypoxic rats (P < 0.001) with the best improvement observed with the combination group where the Hb concentration nearly reaches the normal levels. The combined treatment of ARG and CAR showed significant improvement in Hb concentration compared to CAR-pretreated group (P < 0.05), while no significant difference was observed compared with ARG.
The serum levels of HSP-70 were significantly higher in the untreated hypoxic rats compared to normal control (P < 0.05). The pre-treatment with ARG alone or CAR alone resulted in further increase of HSP-70, which is significant, compared to untreated hypoxic rats (P < 0.05). The combined therapy of ARG and CAR showed marked increase in HSP-70 compared to untreated hypoxic rats (P < 0.001), ARG- (P < 0.05), and CAR-(P < 0.05) treated groups.
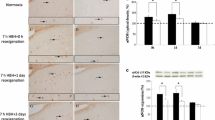
Effect of CAR and/or ARG on the pathological changes in hypoxic rats’ brain (Fig. 1)
As shown in Fig. 1, normal control brain sections from cerebellum revealed normal appearance of brain nerve cells (arrowhead) and neuropil (nerve fibers and glial cells and extracellular substances) (arrow), while marked neuronal cellular degeneration (arrowhead) and vascular congestion were manifested in brains of hypoxic rats (panel B). Rats pretreated with ARG alone or CAR alone showed prevention of the hypoxia-induced neuronal degeneration (panels C and D, respectively). The best improvement of brain tissue was observed in the brain of rat received combination of ARG and CAR (panel E) in which many normal neurons (arrowhead) and nerve fibers and glial cells (arrow) were detected.
Light photomicrographs of brain (cerebellum) from rats stained with hematoxylin and eosin in which (a), represent normal brain nerve cells (arrowhead) and nerve fibers (arrow). (b) Section of brain from rat exposed to hypoxia showing marked degeneration of many neurons (arrowhead) while the nerve fibers and glial cells are not affected (arrow). (c and d) Sections of brain from rat exposed to hypoxia and received arginine alone or carnosine alone respectively, showing few normal healthy nerve cells (arrowhead) and nerve fibers (arrow). (e) Brain from rat exposed to hypoxia and received combination of arginine and carnosine showing many normal neurons (arrowhead) and nerve fibers and glial cells (arrow); (scale bar: 50 μm)
Effect of CAR and/or ARG on the levels of inflammatory markers in hypoxic rats (Fig. 2)
The brain concentration of inflammatory cytokines, TNF-α and IL-6 as well as mRNA levels of NF-κB, the transcription factor that regulates genes involved in inflammation, were markedly elevated in the hypoxic rats compared to normal control (P < 0.001). The enhanced levels TNF-α and IL-6 significantly ameliorated by the pretreatment with ARG (P < 0.01), CAR (P < 0.01), and their combination (P < 0.001) compared to untreated hypoxic rats. In addition, the upregulation of NF-κB mRNA levels was attenuated by the administration of ARG, CAR, and their combination (P < 0.001). Compared to ARG alone or CAR alone, the combined treatment of ARG and CAR showed significant improvement in the levels of TNF-α (P < 0.05) and IL-6 (P < 0.01). As well, the mRNA levels of NF-κB were significantly lower in the combination group compared to ARG alone (P < 0.001) or CAR alone (P < 0.01).
Effect of CAR and/or ARG on the levels of inflammatory markers in hypoxic rats including mRNA expression of nuclear factor κB (NF-κB), and brain levels of tumor necrosis factor- α (TNF-α) and interleukin-6 (IL-6). a Significantly different from normal control, b significantly different from untreated hypoxic group, c significantly different from Hyp + ARG-treated group, d significantly different from Hyp + CAR-treated group. *P ˂ 0.05; **P ˂ 0.01;***P ˂ 0.001 using one-way ANOVA followed by Tukey Kramer post-test. ARG, l-arginine; CAR, carnosine; Hyp, hypoxic group
Effect of CAR and/or ARG on the mRNA levels of HIF-1α and angiogenic markers in hypoxic rats’ brain (Fig. 3)
As revealed in Fig. 3, untreated hypoxic rats showed a significant increase in mRNA levels of HIF-1α (P < 0.01), VEGF (P < 0.05), and VEGFR-1 (P < 0.01) compared to normal control rats. Moreover, the mRNA levels of HIF-1α, VEGF, and VEGFR-1 were significantly higher in ARG-treated rats (P < 0.001), CAR-treated group (P < 0.01), and the combination-treated group (P < 0.001) compared to untreated hypoxic rats. The mRNA expression of HIF-1α is significantly higher in the rats pre-treated with ARG alone and the combination compared to CAR alone (P < 0.05), while the mRNA levels of VEGF and VEGFR-1 were higher in the combination group compared to ARG alone (P < 0.01) and CAR alone (P < 0.001).
Effect of CAR and/or ARG on the mRNA levels of hypoxia inducible factor-1α (HIF-1α) and angiogenic markers; vascular endothelial growth factor (VEGF) and its receptor type I (VEGF-R-1) in hypoxic rats’ brain. a Significantly different from normal control, b significantly different from untreated hypoxic group, c significantly different from Hyp + ARG-treated group, d significantly different from Hyp + CAR-treated group. *P ˂ 0.05; **P ˂ 0.01;***P ˂ 0.001 using one-way ANOVA followed by Tukey Kramer post-test. ARG, l-arginine; CAR, carnosine, Hyp, hypoxic group
Effect of CAR and/or ARG on the levels of apoptotic markers (caspase-3, BAX, Bcl-2) and the ratio of BAX to Bcl-2 in hypoxic rats’ brain (Fig. 4)
The brain concentration of caspase-3 (the executive apoptotic protein) and mRNA levels of BAX were markedly upregulated (P < 0.001), while the mRNA expression of Bcl-2 were significantly reduced (P < 0.001) in the untreated hypoxic rats compared to normal control. In addition, the ratio of BAX to Bcl-2 was significantly higher in untreated hypoxic group (P < 0.001) indicating predominance of BAX, and hence the apoptosis. The enhanced expression of caspase-3 and BAX, and the reduced mRNA levels of Bcl-2 were significantly attenuated by the treatment of ARG alone, CAR alone, and the combination treatment (P < 0.01, P < 0.001). Additionally, the elevated ratio of BAX to Bcl-2 was significantly alleviated by the pre-treatment with ARG and/or CAR. The combination therapy exhibited significant improvement in the concentration of caspase-3 (P < 0.05) and mRNA expression of BAX (P < 0.001) compared to the individual treatment by either ARG or CAR, while no significant difference was detected in Bcl-2 expression. The BAX to Bcl-2 ratio was lowered significantly by the combined therapy compared to ARG alone (P < 0.05) or CAR alone (P < 0.01).
Effect of CAR and/or ARG on the mRNA levels of apoptotic markers (caspase-3, BAX, Bcl-2 and the ratio of BAX to Bcl-2) in hypoxic rats’ brain. a Significantly different from normal control, b significantly different from untreated hypoxic group, c significantly different from Hyp + ARG-treated group, d significantly different from Hyp + CAR-treated group. *P ˂ 0.05; **P ˂ 0.01;***P ˂ 0.001 using one-way ANOVA followed by Tukey Kramer post-test. ARG, l-arginine; CAR, carnosine, Hyp, hypoxic group
Effect of CAR and/or ARG on the brain concentration of monoamines (NADR, DOP, and SER) and GABA in hypoxic rats (Fig. 5)
Figure 5 revealed that hypoxia resulted in marked reduction in the brain levels of DOP, NADR, SER, and GABA (P < 0.001). Pretreatment with ARG alone or CAR alone significantly alleviated this depletion in the brain levels of DOP (P < 0.05), NADR (P < 0.01), SER (P < 0.01), and GABA (P < 0.01) compared to untreated hypoxic rats. These reduced levels were also attenuated, but to greater extent, by the use of the combined treatment of ARG and CAR (P < 0.001 for NADR, SER, and GABA; P < 0.01 for DOP). In comparison with the individual treatment (either ARG or CAR), the combination therapy showed significant increase in the brain levels of DOP (P < 0.05), NADR (P < 0.001), SER (P < 0.01), and GABA (P < 0.01).
Effect of CAR and/or ARG on the brain concentration of noradrenaline, dopamine serotonin and GABA in hypoxic rats. a Significantly different from normal control, b significantly different from untreated hypoxic group, c significantly different from Hyp + ARG-treated group, d significantly different from Hyp + CAR-treated group. *P ˂ 0.05; **P ˂ 0.01;***P ˂ 0.001 using one-way ANOVA followed by Tukey Kramer post-test. ARG, l-arginine; CAR, carnosine; Hyp, hypoxic group
Discussion
High dose of sodium nitrite is widely used as an experimental model of hemic hypoxia. In blood, nitrite binds to oxy-Hb displacing the bound oxygen and yielding hydrogen peroxide and nitrogen dioxide, which oxidizes ferrous Hb to ferric producing methemoglobin (Met-Hb), as well as the generation of ferryl Hb radicals (Kohn et al. 2002). Met-Hb has reduced ability to transport oxygen to tissue and thus hypoxia (Gluhcheva et al. 2012). Oxy-Hb concentration in the current study was significantly reduced after sodium nitrite administration, confirming this phenomenon. Because of the oxygen deprivation and free radical generation, sodium nitrite leads to oxidative stress, depleted energy production, and eventually brain injury (Attia et al. 2009; Abdel Baky et al. 2010). Brain damage was observed in the current study via H&E stain, which revealed neuronal cellular degeneration and vascular congestion. Pre-treatment with ARG, CAR, and their combination significantly increased Hb concentration in hypoxic rats, which was associated with alleviation of the brain injury as observed by H&E stain. The prominent effect was achieved by the combination, which nearly reverses the anemia induced by sodium nitrite. Although the antioxidant power is extensively studied as a mechanism for the neuroprotective effects of ARG and CAR in hypoxic brain, other mechanisms such as induction of angiogenesis, anti-inflammatory, and anti-apoptotic, as well as the effect on biogenic amines and GABA has not studied yet.
The cytoprotective role of stress-inducible-proteins such as HSP-70 during low oxygen conditions has been studied in vivo and in vitro (Lee et al. 2001; Matsumori et al. 2005; Zhang et al. 2009). In these conditions, HSP-70 is increased and contributes to cell survival (Didelot et al. 2006) via different mechanisms including antioxidant and anti-inflammatory properties (Guo et al. 2007; Zheng et al. 2008) as well as the inactivation of caspase-3 (Ying et al. 2016). Accordingly, the high levels of serum HSP-70 in the current study in hypoxic rats could be a compensatory mechanism to counteract the hypoxia-induced inflammation and apoptosis. ARG, CAR, and, to a lager extent, their combination resulted in further elevation of HSP-70, which could contribute to many protective mechanisms exhibited by these two amino acids in the present study as discussed later.
The lack of oxygen is usually accompanied by inflammatory response, which could be related to many reasons, including oxidative stress (Prabhakar et al. 2001; Attia et al. 2009; Abdel Baky et al. 2010) and the activation of NF-κB, which leads to the release inflammatory mediators such as TNF-α and interleukins (Bai et al. 2018). In addition, the innate immune cells in the central nervous system, especially the microglia, are usually activated in response to hypoxia leading to the release of inflammatory cytokines, which are closely related to brain damage (de Vries et al. 1996; Deng et al. 2008; Wang et al. 2018). Our results agree with the previous data where the brain levels of TNF-α and IL-6 as well as mRNA levels of NF-κB significantly augmented in hypoxic rats compared to normal group. On the other hand, pre-treatment with ARG, CAR, and their combination alleviated this inflammation. Similarly, the supplementation of either CAR or ARG revealed anti-inflammatory potency in different pathological conditions (Huang et al. 2008; Ivanov et al. 2008; Tsai et al. 2010; Al-Rasheed et al. 2016). Since HSP-70 can protect the tissues by inhibiting various inflammatory mediators (Zheng et al. 2008); therefore, ARG and CAR may exhibit their anti-inflammatory effects via enhancing the levels of HSP-70 (Table 1).
Twenty-four hours after onset of hypoxia, our results showed an elevation of mRNA levels of HIF-1α in the brain of hypoxic rats and this result is consistent with that of Molina et al. (2013) who reported increased expression of HIF-1α in rats brain exposed to acute hypoxia. HIF-1α is also detected in the brain shortly after onset of hypoxia (Chávez et al. 2000). Kaur et al. (2006) and Molina et al. (2017) have also described similar results. It is reported that HIF-1α increased immediately due to the hypoxic inhibition of prolyl hydroxylase, the enzyme that is responsible for the continuous degradation of HIF-1α under normoxic conditions (Guzy et al. 2005). Hypoxia-induced ROS formation may play a role in this inhibition of prolyl hydroxylase enzyme (Guzy et al. 2005). HIF-1α immunoreactivity was detected in cerebral samples obtained from rats presenting with spontaneous seizures and patients affected by pharmacoresistant epilepsy, and interestingly, this immunoreactvity in rats was also found in all pimonidazole-immunopositive neurons, suggesting the induction of HIF-1α in epilepsy as a consequence of hypoxia (Gualtieri et al. 2013). This could also suggest the relation between increased HIF-1α and the alteration in the neurotransmitters such as glutamate and GABA in hypoxic state.
Hypoxic studies explained the increase of HIF-1α as an adaptive neuroprotective mechanism to drive oxygen delivery to the hypoxic brain via the induction of angiogenesis; the formation of new vessels that allow increased oxygen availability (Molina et al. 2013; Yu et al. 2014). In hypoxia, HIF regulates a great number of target genes involved in angiogenesis. VEGF, the most potent angiogenic factor, is a direct target of HIF-1α and this data could explain our results in which the mRNA expression of VEGF and VEGFR-1 are enhanced after 24 h of hypoxia. In agreement of our results, Molina et al. (2013) have shown the following: (i) the expression of both HIF-1α and VEGF is upregulated immediately after short term hypoxia; (ii) such upregulation is a neuroprotective mechanism to hypoxia in order to maintain an adequate blood supply to the hypoxic tissue, thereby minimizing the adverse effects of oxygen deprivation. Moreover, in traumatic brain injury, the treatment with HIF activator leads to an increase in VEGF and a subsequent neuroprotection (Sen and Sen 2016). The upregulation of VEGF under hypoxic conditions is also reported in rat brain (BaniHashemi et al. 2008), rat cerebellum (Kaur et al. 2006), and mouse brain (Kuo et al. 1999). In our study, pre-treatment with ARG, CAR, and their combination resulted in significant higher levels of HIF-1α, VEGF, and VEGFR-1 compared to hypoxic rats suggesting their neuroprotective effects via boosting the oxygen supply to hypoxic brain tissues. Concerning ARG, the increase in HIF-1α, and subsequently VEGF, could be also attributed to the production of nitric oxide (NO). Under hypoxic conditions, NO released by ARG blocked HIF-1α degradation by prolyl hydroxylase and upregulated the mRNA expression of VEGF in primary astrocytes (Brix et al. 2012; Shi et al. 2016).
Apoptosis is another adaptive mechanism following hypoxia. Severe hypoxia causes a reduced activity of DNA repair system, particularly mismatch repair (Greijer and Van der Wall 2004), leading to high mutation rate. Therefore, to prevent the accumulation of these mutations, the cell initiates the cascade of apoptotic cell death (Greijer and Van der Wall 2004). Hyper-permeability of the inner mitochondrial membrane (Saikumar et al. 1998) and excessive ROS production and inflammatory response (Xie et al. 2017) triggers the apoptosis. Apoptosis is initiated by cascade of events that eventually leads to the activation of the apoptotic proteins called caspases, among them; caspase-3 is the executive apoptotic protein that triggers the cell death. In the present study, after 24 h of hypoxia, the brain levels of caspase-3 were obviously elevated in hypoxic brains supporting the apoptotic adaptive mechanism induced by hypoxia. It is reported that, two groups of proteins regulate the apoptotic pathway; pro-apoptotic proteins such as BAX and anti-apoptotic proteins including Bcl-2 (Gross et al. 1999). The balance between pro- and anti-apoptotic proteins determines whether the cell undergoes apoptosis or survival. For example, the ratio of BAX to Bcl-2 is considered as a critical factor in cell survival or death (Lee et al. 2017). In this study, the mRNA expression levels of Bcl-2 significantly decreased, while that of BAX and the ratio of BAX to Bcl-2 were increased. This indicates that the pro-apoptotic effect of BAX was greater than the anti-apoptotic effect of Bcl-2, which eventually leads to apoptosis.
Pre-treatment with ARG, CAR, and, particularly, their combination successfully attenuated the abnormalities in caspase-3, BAX, Bcl-2, and BAX/ Bcl-2 ratio reflecting their prophylactic effect against hypoxia-induced apoptosis. The observed anti-apoptotic effects of ARG and CAR may be attributable to their augmentation effect on HIF-1α because Guo (2007) found that HIF-1α ameliorates brain damages during ischemia reperfusion through reduction of cell apoptosis and enhancing the cell survival. Furthermore, the role HIF-1α on the anti-apoptotic potency of berberine in neurons during hypoxia/ischemia is documented (Zhang et al. 2012). In addition to its ability to induce vessel growth, a growing body of evidence showed that VEGF is a survival factor that can enhance neuronal cell survival and reduce infarct size in the brain (Kaya et al. 2005). Therefore, it is suggested that the anti-apoptotic effects of CAR and ARG on hypoxic brain could be related to their angiogenic action and the elevation of VEGF and VEGFR-1. The anti-apoptotic effect of ARG and CAR could be also attributed to their powerful antioxidant effects and the elevated levels of HSP-70 (Table 1). Moreover, ARG is the precursor of NO that exerts protective anti-apoptotic actions (De Nadai et al. 2000). The neuroprotective effects of CAR via anti-apoptotic mechanisms were previously reported in a model of hemorrhagic stroke (Xie et al. 2017) and against 6-hydroxydopamine toxicity in hemi parkinsonian rat (Afshin-Majd et al. 2015).
Biogenic amines are important regulators of various physiological and pharmacological functions in the brain and any alterations in their brain levels may affect the signaling process and behavioral functions Torda 2004; Hritcu et al. 2007; Cools 2008). Reductions in the levels of brain catecholamines, serotonin, and their metabolites have been observed in chemical-induced neurodegeneration and neurodegenerative diseases involving hypoxia (Premanand and Ganesh 2010; Yadav et al. 2010; Rizk et al. 2017). Consistent with previous works, our model of hypoxia-induced brain damage resulted in reduced levels of DOPA, NADR, and SER, the effect which could be related to the increased activity of monoamine oxidase-A (MAO-A) induced by sodium nitrite leading to degradation of monoamines and their depletion in brain (Premanand and Ganesh 2010; Biradar et al. 2013; Biradar and Joshi 2014). Apart from the effect on MAO, hypoxia itself leads to decreased activity of tyrosine hydroxylase and tryptophan hydroxylase, the key enzymes in the biosynthesis of catecholamines and SER (Hedner and Lundborg 1979).
Pre-treatment of hypoxic rats with ARG, CAR, and their combination successfully alleviated the depleted levels of monoamines compared to untreated hypoxic rats. The increase in brain monoamines levels with CAR may be a consequence of the reduced activities of MAO-A (Banerjee and Poddar 2015; Banerjee et al. 2015) in rat’s brain; therefore, CAR may reverse the action of sodium nitrite on MAO-A delaying the metabolism of DOPA, NADR, and SER and enhances their action. Banerjee and his colleagues (Banerjee et al. 2015) have shown that treatment with CAR attenuated the aging-induced increase activity of brain MAO-A activity and restored the serotonergic parameters towards their normal levels that observed in young control rats. In addition, it is suggested that the increase in histamine release after administration of CAR may play a role in modulating the release the neurotransmitters such as dopamine (Gong et al. 2007). On the other hand, the effect of ARG on monoamines could be attributed to its role as precursor of NO production (Abdel Baky et al. 2010). NO is an important intercellular messenger in the brain and has been found to increase the release of SER and DOP in different brain regions (Lorrains and Hull 1993; Kaehler et al. 1999; Sinner et al. 2001; Philippu 2016). This explanation could be supported by the data stating that NO synthase inhibitor blocked the rise in monoamines induced by NO and that NO donors, including ARG, reversed the decrease in striatal dopamine levels (Bishnoi et al. 2009). Furthermore, Volz and Schenk (2004) revealed that ARG increases dopamine transporter activity in rat striatum via a NO synthase-dependent mechanism. Literature reports suggest that NO participates in the regulation of dopaminergic neurotransmission, possibly through interaction with cysteine residues of the dopamine transporter. Collectively, these studies suggest the protective role of ARG is probably via its function as a precursor of NO. Our results suggest that ARG and CAR, particularly their combination, may provide neuroprotection against hypoxia via preserving the biogenic amine brain levels.
Exaggerated release of the excitatory neurotransmitters such as glutamate has been documented in the hypoxic conditions (Takagi et al. 1993; Nelson et al. 2003), leading to neuronal damage. However, GABA as inhibitory amino acid antagonizes this neurotoxicity providing neuroprotection (Schwartz-Bloom and Sah 2001). Therefore, the detected reduced brain levels of GABA in the present study may participate in the brain damage shown in H&E stain of hypoxic rats. The reduced GABA in our model of hypoxia is consistent with Anju et al. (2011) in which GABA content and their receptors were decreased significantly in the cerebellum and brain stem of hypoxic neonatal rats compared to control. The diminished levels of GABA in hypoxic state may be a consequence of reduced glutamate transporters. That is because the glutamate transporters provide more glutamate as a substrate for GABA synthesis from glutamate; however, during hypoxia, the glutamate transporter expression and activity are downregulated leading to decreased GABA levels and the subsequent neurotoxicity. Moreover, the decreased levels of GABA may be attributed to the hypoxia-induced downregulation of glutamate decarboxylase expression in the brain, which in turn results in the inhibition of GABA synthetic pathway, which involves glutamate decarboxylation (Anju et al. 2011). On the other hand, pre-treatment with CAR and ARG alleviated the depletion of GABA and this effect may contribute to their neuroprotective effects. Similarly, ARG-induced elevation of NO concentration was accompanied by the increase of GABA levels in cerebral cortex (Kuriyama and Ohkuma 1995), hippocampus (Lonart et al. 1992), and striatum (Segovia and Mora 1998; Paul and Ekambaram 2005). The NO-induced increase in GABA could be related to the reduced activity of GABA transaminase (GABA-T) (Paul and Jayakumar 2000). Rasgado et al. (2018) reported that GABA-T activity and brain GABA levels are inversely related and that NO generated by neuronal NO synthase had a direct influence on GABA-T activity and thereby on brain GABA levels. Concerning CAR, previous findings suggest that regulating GABA levels are involved in the CAR-induced neuroprotection (Ouyang et al. 2016). Ouyang et al. (2016) demonstrated that CAR markedly increased GABA level and upregulated the mRNA level of neuronal glutamate transporter EAAC1 in neuron/astrocyte co-cultures exposed to oxygen glucose deprivation /recovery. In a model of hemorrhagic stroke, application of CAR on slices before autoblood influence (blood clot) leads to restoration of the activity of GABA receptors that are inhibited in the presence of autoblood (Khama-Murad et al. 2011). Our results concerning monoamines and GABA in this model of hemic hypoxia in brain may provide a perspective for investigating the mechanisms of neuroprotection by CAR and ARG.
It is noted that the combination of CAR and ARG has superior prophylactic effect against the inflammation, the apoptosis, and the downregulation of biogenic amines and GABA induced by hypoxic brain. The induction of angiogenesis also predominates with the combination treatment. In conclusion, supplementation with CAR, ARG, and, more effectively, their combination elicit neuroprotection in hypoxic rats via variable mechanisms beyond their antioxidant power. These mechanisms include anti-inflammatory, anti-apoptosis, induction of HIF-1α, and angiogenesis as well as the attenuation of reduced levels of biogenic amines and GABA.
References
Abdel Baky NA, Zaidi ZF, Fatani AJ, Sayed-Ahmed MM, Yaqub H (2010) Nitric oxide pros and cons: the role of L-arginine, a nitric oxide precursor, and idebenone, a coenzyme-Q analogue in ameliorating cerebral hypoxia in rat. Brain Res Bull 83(1-2):49–56. https://doi.org/10.1016/j.brainresbull.2010.07.004
Afshin-Majd S, Khalili M, Roghani M, Mehranmehr N, Baluchnejadmojarad T (2015) Carnosine exerts neuroprotective effect against 6-hydroxydopamine toxicity in hemiparkinsonian rat. Mol Neurobiol 51(3):1064–1070. https://doi.org/10.1007/s12035-014-8771-0
Ali SA, Aly HF, Faddah LM, Zaidi ZF (2012) Dietary supplementation of some antioxidants against hypoxia. World J Gastroenterol 18(44):6379–6386. https://doi.org/10.3748/wjg.v18.i44.6379
Al-Rasheed NM, Fadda L, Mohamed AM, Attia HA, Al-Rasheed NM (2016) Regulating effect of carnosine and /or L-arginine on the expression of inflammatory molecules induced nephropathy in the hypoxic rat model. Braz Arch Biol Technol 59:e16150622
Anju TR, Jayanarayanan S, Paulose CS (2011) Decreased GABAB receptor function in the cerebellum and brain stem of hypoxic neonatal rats: role of glucose, oxygen and epinephrine resuscitation. J Biomed Sci 18(1):31. https://doi.org/10.1186/1423-0127-18-31
Attia HA, AL-Rasheed NM, Faddah LM, AL-Rasheed NM, Ahmed AA (2009) Ameliorating effect of idebenone and/or melatonin against oxidative stress and energy depletion in brain of hypoxic rats. Res J Sci Med Sci 4(2):263–277
Baek SH, Noh AR, Kim KA, Akram M, Shin YJ, Kim ES, Yu SW, Majid A, Bae ON (2014) Modulation of mitochondrial function and autophagy mediates carnosine neuroprotection against ischemic brain damage. Stroke 45:2438–2443. https://doi.org/10.1161/STROKEAHA.114.005183
Bai W, Zhou J, Zhou N, Liu Q, Cui J, Zou W, Zhang W (2018) Hypoxia-increased RAGE expression regulates chemotaxis and pro-inflammatory cytokines release through nuclear translocation of NF-κ B and HIF1α in THP-1 cells. Biochem Biophys Res Commun 495(3):2282–2288. https://doi.org/10.1016/j.bbrc.2017.12.084
Banerjee S, Poddar MK (2015) Carnosine: effect on aging-induced increase in brain regional monoamine oxidase-A activity. Neurosci Res 92:62–70. https://doi.org/10.1016/j.neures.2014.09.009
Banerjee S, Ghosh TK, Poddar MK (2015) Carnosine reverses the aging-induced down regulation of brain regional serotonergic system. Mech Ageing Dev 152:5–14. https://doi.org/10.1016/j.mad.2015.09.002
BaniHashemi S, Braun J, Bernhardt WM, Rascher W, Dötsch J, Trollmann R (2008) HIF-1alpha subunit and vasoactive HIF-1-dependent genes are involved in carbon monoxide-induced cerebral hypoxic stress response. Eur J Appl Physiol 104:95–102. https://doi.org/10.1007/s00421-008-0776-9
Biradar SM, Joshi H (2014) The influence of ethanolic extract of seeds of Peganum harmala Linn. on behavioral and biochemical studies in cognitive deficit mice. Int J Pharm Phytopharmacol Res 4(1):25–33
Biradar SM, Joshi H, Tarak KC (2013) Cerebroprotective effect of isolated harmine alkaloids extracts of seeds of Peganum harmala L. on sodium nitrite-induced hypoxia and ethanol-induced neurodegeneration in young mice. Pak J Biol Sci 16(23):1687–1697
Bishnoi M, Chopra K, Kulkarni SK (2009) Co-administration of nitric oxide (NO) donors prevents haloperidol-induced orofacial dyskinesia, oxidative damage and change in striatal dopamine levels. Pharmacol Biochem Behav 91(3):423–429. https://doi.org/10.1016/j.pbb.2008.08.021
Boldyrev A, Bulygina E, Leinsoo T, Petrushanko I, Tsubone S, Abe H (2004) Protection of neuronal cells against reactive oxygen species by carnosine and related compounds. Comp Biochem Physiol Biochem Mol Biol 137:81–88
Boldyrev AA, Aldini G, Derave W (2013) Physiology and pathophysiology of carnosine. Physiol Rev 93:1803–1845. https://doi.org/10.1152/physrev.00039.2012
Brix B, Mesters JR, Pellerin L, Johren O (2012) Endothelial cell-derived nitric oxide enhances aerobic glycolysis in astrocytes via HIF-1alpha-mediated target gene activation. J Neurosci 32:9727–9735
Chávez JC, Agani F, Pichiule P, LaManna JC (2000) Expression of hypoxic inducible factor 1α in the brain of rats during chronic hypoxia. J Appl Physiol 89:1937–1942. https://doi.org/10.1152/jappl.2000.89.5.1937
Cools R (2008) Role of dopamine in the motivational and cognitive control of behavior. Neuroscientist 14(4):381–395. https://doi.org/10.1177/1073858408317009
De Nadai C, Sestili P, Cantoni O et al (2000) Nitric oxide inhibits tumor necrosis factor-alpha-induced apoptosis by reducing the generation of ceramide. Proc Natl Acad Sci U S A 97:5480–5485. https://doi.org/10.1073/pnas.070062397
de Vries HE, Blom-Roosemalen MC, van Oosten M, de Boer AG, van Berkel T, Breimer DD, Kuiper J (1996) The influence of cytokines on the integrity of the blood-brain barrier in vitro. J Neuroimmunol 64:37–43
Deng Y, Lu J, Sivakumar V, Ling EA, Kaur C (2008) Amoeboid microglia in the periventricular white matter induce oligodendrocyte damage through expression of proinflammatory cytokines via MAP kinase signalling pathway in hypoxic neonatal rats. Brain Pathol 18:387–400
Didelot C, Schmitt E, Brunet M, Maingret L, Parcellier A, Garrido C (2006) Heat shock proteins: endogenous modulators of apoptotic cell death. Handb Exp Pharmacol 172:171–198
Dirnagl U, Becker K, Meisel A (2009) Preconditioning and tolerance against cerebral ischaemia: from experimental strategies to clinical use. Lancet Neurol 8:398–412. https://doi.org/10.1016/S1474-4422(09)70054-7
Fedorova TN, Macletsova MG, Kulikov AV, Stepanova MS, Boldyrev AA (2006) Carnosine protects from the oxidative stress induced by prenatal hypoxia. Dokl Biol Sci 408:207–210
Fouad AA, El-Rehany MAA, Maghraby HK (2007) The hepatoprotective effect of carnosine against ischemia/reperfusion liver injury in rats. Eur J Pharmacol 572:61–68
Gluhcheva Y, Ivanov I, Petrova E, Pavlova E, Vladova I (2012) Sodium nitrite-induced hematological and hemorheological changes in rats. Ser Biomech 27(3-4):53–58
Gong YX, Wang HJ, Zhu YP, Zhang WP, Dai HB, Zhang SH, Wei EQ, Chen Z (2007) Carnosine ameliorates morphine-induced conditioned place preference in rats. Neurosci Lett 422(1):34–38. https://doi.org/10.1016/j.neulet.2007.05.048
Gore CJ, Clark SA, Saunders PU (2007) Nonhematological mechanisms of improved sea level performance after hypoxic exposure. Med Sci Sports Exerc 39(9):1600–1609. https://doi.org/10.1249/mss.0b013e3180de49d3
Greijer A, Van der Wall E (2004) The role of hypoxia inducible factor 1 (HIF-1) in hypoxia induced apoptosis. J Clin Pathol 57(10):1009–1014
Grosenbaugh DK, Ross BM, Wagley P, Zanelli SA (2018) The role of Kainate receptors in the pathophysiology of hypoxia-induced seizures in the neonatal mouse. Sci Rep 8(1):7035. https://doi.org/10.1038/s41598-018-24722-3
Gross A, Yin XM, Wang K, Wei MC, Jockel J, Milliman C, Erdjument-Bromage H, Tempst P, Korsmeyer SJ (1999) Caspase cleaved BID targets mitochondria and is required for cytochrome c release, while BCL-XL prevents this release but not tumor necrosis factor-R1/Fas death. J Biol Chem 274:1156–1163
Gualtieri F, Marinelli C, Longo D, Pugnaghi M, Nichelli PF, Meletti S, Biagini G (2013) Hypoxia markers are expressed in interneurons exposed to recurrent seizures. Neuromolecular Med 15(1):133–146. https://doi.org/10.1007/s12017-012-8203-0
Guo S, Wharton W, Moseley P, Shi H (2007) Heat shock protein 70 regulates cellular redox status by modulating glutathione-related enzyme activities. Cell Stress Chaperones 12:245–254
Guzy RD, Hoyos B, Robin E, Chen H, Liu L, Mansfield KD, Simon MC, Hammerling U, Schumacker PT (2005) Mitochondrial complex III is required for hypoxia-induced ROS production and cellular oxygen sensing. Cell Metab 1(6):401–408. https://doi.org/10.1016/j.cmet.2005.05.001
Hedner T, Lundborg P (1979) Regional changes in monoamine synthesis in the developing rat brain during hypoxia. Acta Physiol Scand 106(2):139–143
Hota SK, Barhwal K, Ray K, Singh SB, Ilavazhagan G (2008) Ceftriaxone rescues hippocampal neurons from excitotoxicity and enhances memory retrieval in chronic hypobaric hypoxia. Neurobiol Learn Mem 89(4):522–532. https://doi.org/10.1016/j.nlm.2008.01.003
Hritcu L, Clicinschi M, Nabeshima T (2007) Brain serotonin depletion impairs short-term memory, but not long-term memory in rats. Physiol Behav 91(5):652–657. https://doi.org/10.1016/j.physbeh.2007.03.028
Huang CC, Tsai SC, Lin WT (2008) Potential ergogenic effects of L-arginine against oxidative and inflammatory stress induced by acute exercise in aging rats. Exp Gerontol 43:571–577
Ivanov V, Cha J, Ivanova S et al (2008) Essential nutrients suppress inflammation by modulating key inflammatory gene expression. Int J Mol Med 22:731–741
Kaehler ST, Singewald N, Sinner C, Philippu A (1999) Nitric oxide modulates the release of serotonin in the rat hypothalamus. Brain Res 835(2):346–349
Kaur C, Sivakumar V, Zhang Y, Ling EA (2006) Hypoxia-induced astrocytic reaction and increased vascular permeability in the rat cerebellum. Glia 54:826–839
Kaya D, Gürsoy-Ozdemir Y, Yemisci M, Tuncer N, Aktan S, Dalkara T (2005) VEGF protects brain against focal ischemia without increasing blood-brain permeability when administered intracerebroventricularly. J Cereb Blood Flow Metab 25(9):1111–1118. https://doi.org/10.1038/sj.jcbfm.9600109
Khama-Murad AK, Mokrushin AA, Pavlinova LI (2011) Neuroprotective properties of l-carnosine in the brain slices exposed to hemorrhagic stroke model autoblood in the in vitro. Regul Pept 167(1):65–69. https://doi.org/10.1016/j.regpe
Kjeldsberg CR (1993) Principles of hematologic examination. In: Lee GR, Bittell TC, Foerster J, Athens JW, Lukens JN (eds) Wintrobe's clinical hematology, vol 1. London, Philadelphia, pp 7–37
Koh MY, Lemos R Jr, Liu X, Powis G (2011) The hypoxia-associated factor switches cells from HIF-1alpha- to HIF-2alpha-dependent signaling promoting stem cell characteristics, aggressive tumor growth and invasion. Cancer Res 71:4015–4027. https://doi.org/10.1158/0008-5472.CAN-10-4142
Kohn MC, Melnick RL, Ye F, Portier CJ (2002) Pharmacokinetics of sodium nitrite-induced methemoglobinemia in the rat. Drug Metab Dispos 30(6):676–683
Krauss H, Jablecka A, Sosnowski P, Bogdanski P (2009) Influence of l-arginine on the nitric oxide concentration and level of oxidative stress during ischemia–reperfusion injury in a rat model. Int J Clin Pharmacol Ther 47:533–538
Kuo NT, Benhayon D, Przybylski RJ, Martin RJ, LaManna JC (1999) Prolonged hypoxia increases vascular endothelial growth factor mRNA and protein in adult mouse brain. J Appl Physiol 86:260–264
Kuriyama K, Ohkuma S (1995) Role of nitric oxide in central synaptic transmission: effects on neurotransmitter release. Jpn J Pharmacol 69:1–8. https://doi.org/10.1254/jjp.69.1
Lee JE, Yenari MA, Sun GH, Xu L, Emond MR, Cheng D, Steinberg GK, Giffard RG (2001) Differential neuroprotection from human heat shock protein 70 overexpression in in vitro and in vivo models of ischemia and ischemia-like conditions. Exp Neurol 170:129–139
Lee HJ, Lee EK, Seo YE, Shin YH, Kim HS, Chun YH, Yoon JS, Kim HH, Han MY, Kim CK et al (2017) Roles of Bcl-2 and caspase-9 and -3 in CD30-induced human eosinophil apoptosis. J Microbiol Immunol Infect 50:145–152. https://doi.org/10.1016/j.jmii.2015.05.017
Lonart G, Wang J, Johnson KM (1992) Nitric oxide induces neurotransmitter release from hippocampal slices. Eur J Pharmacol 220:271–272. https://doi.org/10.1016/0014-2999(92)90759-W
Lorrains DS, Hull EM (1993) Nitric oxide increases dopamine and serotonin release in the medial preoptic area. Neuroreport 5:87–89
Majmundar AJ, Wong WJ, Simon MC (2010) Hypoxia-inducible factors and the response to hypoxic stress. Mol Cell 40:294–309. https://doi.org/10.1016/j.molcel.2010.09.022
Matsumori Y, Hong SM, Aoyama K, Fan Y, Kayama T, Sheldon RA, Vexler ZS, Ferriero DM, Weinstein PR, Liu J (2005) Hsp70 overexpression sequesters AIF and reduces neonatal hypoxic/ischemic brain injury. J Cereb Blood Flow Metab 25:899–910. https://doi.org/10.1038/sj.jcbfm.9600080
Molina F, Rus A, Peinado MA, Del Moral ML (2013) Short-term hypoxia/reoxygenation activates the angiogenic pathway in rat caudate putamen. J Biosci 38(2):363–371
Molina F, Del Moral ML, Peinado MÁ, Rus A (2017) Angiogenesis is VEGF-independent in the aged striatum of male rats exposed to acute hypoxia. Biogerontology 18(5):759–768. https://doi.org/10.1007/s10522-017-9709-5
Naik SR, Pilgaonkar VW, Panda VS (2006) Evaluation of antioxidant activity of ginkgo biloba phytosomes in rat brain. Phytother Res 20:1013–1016. https://doi.org/10.1002/ptr.1976
Nelson RM, Lambert DG, Green AR, Hainsworth AH (2003) Pharmacology of ischemia- induced glutamate efflux from rat cerebral cortex in vitro. Brain Res 964:1–8
Ouyang L, Tian Y, Bao Y, Xu H, Cheng J, Wang B, Shen Y, Chen Z, Lyu J (2016) Carnosine decreased neuronal cell death through targeting glutamate system and astrocyte mitochondrial bioenergetics in cultured neuron/astrocyte exposed to OGD/recovery. Brain Res Bull 124:76–84. https://doi.org/10.1016/j.brainresbull.2016.03.019
Paul V, Ekambaram P (2005) Effects of sodium nitroprusside, a nitric oxide donor, on gamma-aminobutyric acid concentration in the brain and on picrotoxin-induced convulsions in combination with phenobarbitone in rats. Pharmacol Biochem Behav 80:363–370
Paul V, Jayakumar AR (2000) A role of nitric oxide as an inhibitor of gamma-aminobutyric acid transaminase in rat brain. Brain Res Bull 51(1):43–46
Pekcetin C, Kiray M, Ergur BU, Tugyan K, Bagriyanik HA, Erbil G, Baykara B, Camsari UM (2009) Carnosine attenuates oxidative stress and apoptosis in transient cerebral ischemia in rats. Acta Biol Hung 60:137–148. https://doi.org/10.1556/ABiol.60.2009.2.1
Philippu A (2016) Nitric oxide: a universal modulator of brain function. Curr Med Chem 23(24):2643–2652
Prabhakar NR, Fields RD, Baker T, Fletcher EC (2001) Intermittent hypoxia: cell to system. Am J Physiol Lung Cell Mol Physiol 281:L524–L528. https://doi.org/10.1152/ajplung.2001.281.3.L524
Premanand R, Ganesh T (2010) Neuroprotective effects of Abrus precatorius Linn. aerial extract on hypoxic neurotoxicity induced rats. Int J Chem Pharm Sci 1(1):9–15
Rajanikant GK, Zemke D, Senut MC, Frenkel MB, Chen AF, Gupta R, Majid A (2007) Carnosine is neuroprotective against permanent focal cerebral ischemia in mice. Stroke 38:3023–3037
Rakhade SN, Zhou C, Aujla PK, Fishman R, Sucher NJ, Jensen FE (2008) Early alterations of AMPA receptors mediate synaptic potentiation induced by neonatal seizures. J Neurosci 28(32):7979–7990. https://doi.org/10.1523/JNEUROSCI.1734-08.2008
Rasgado LA, Reyes GC, Díaz FG (2018) Role of nitric oxide synthase on brain GABA transaminase activity and GABA levels. Acta Pharma 68:349–359. https://doi.org/10.2478/acph-2018-0022
Rius J, Guma M, Schachtrup C, Akassoglou K, Zinkernagel AS, Nizet V, Johnson RS, Haddad GG, Karin M (2008) NF-kappa B links innate immunity to the hypoxic response through transcriptional regulation of HIF-1alpha. Nature 453:807–811. https://doi.org/10.1038/nature06905
Rizk HA, Masoud MA, Maher OW (2017) Prophylactic effects of ellagic acid and rosmarinic acid on doxorubicin-induced neurotoxicity in rats. J Biochem Mol Toxicol 31(12). https://doi.org/10.1002/jbt.21977
Saikumar P, Dong Z, Patel Y, Hall K, Hopfer U, Weinberg JM, Venkatachalam MA (1998) Role of hypoxia-induced Bax translocation and cytochrome c release in reoxygenation injury. Oncogene 17:3401–3415. https://doi.org/10.1038/sj.onc.1202590
Schwartz-Bloom RD, Sah R (2001) Gamma-aminobutyric acid (A) neurotransmission and cerebral ischemia. J Neurochem 77:353–371
Segovia G, Mora F (1998) Role of nitric oxide in modulating the release of dopamine, glutamate, and GABA in striatum of the freely moving rat. Brain Res Bull 45:275–279. https://doi.org/10.1016/S0361-9230(97)00402-4
Sen T, Sen N (2016) Treatment with an activator of hypoxia-inducible factor 1, DMOG provides neuroprotection. Neuropharmacology 107:79–88. https://doi.org/10.1016/j.neuropharm.2016.03.009
Shen Y, Hu WW, Fan YY, Dai HB, Fu QL, Wei EQ, Luo JH, Chen Z (2007) Carnosine protects against NMDA-induced neurotoxicity in differentiated rat PC12 cells through carnosine–histidine–histamine pathway and H(1)/H(3) receptors. Biochem Pharmacol 73:709–717
Shi Q, Liu X, Wang N, Zheng X, Fu J, Zheng J (2016) Nitric oxide from brain microvascular endothelial cells may initiate the compensatory response to mild hypoxia of astrocytes in a hypoxia-inducible factor-1α dependent manner. Am J Transl Res 8(11):4735–4749 eCollection 2016
Sinner C, Kaehler ST, Philippu A, Singewald N (2001) Role of nitric oxide in the stress-induced release of serotonin in the locus coeruleus. Naunyn Schmiedeberg's Arch Pharmacol 364(2):105–109
Sorce S, Krause KH (2009) NOX enzymes in the central nervous system: from signaling to disease. Antioxid Redox Signal 11:2481–2504. https://doi.org/10.1089/ARS.2009.2578
Stvolinskii SL, Fedorova TN, Yuneva MO, Boldyrev AA (2003) Protective effect of carnosine on Cu, Zn-superoxide dismutase during impaired oxidative metabolism in the brain in vivo. Bull Exp Biol Med 135:130–132
Tabakman R, Lazarovici P, Kohen R (2002) Neuroprotective effects of carnosine and homocarnosine on pheochromocytoma PC12 cells exposed to ischemia. J Neurosci Res 68:463–469. https://doi.org/10.1002/jnr.10228
Takagi K, Ginsberg MD, Globus MY, Dietrich WD, Martinez E, Kraydieh S, Busto R (1993) Changes in amino acid neurotransmitters and cerebral blood flow in the ischemic penumbral region following middle cerebral artery occlusion in the rat: correlation with histopathology. J Cereb Blood Flow Metab 13:575–585. https://doi.org/10.1038/jcbfm.1993.75
Torda C (2004) Effects of catecholamines on behavior. J Neurosci Res 2(3):193–202. https://doi.org/10.1002/jnr.490020303
Tsai SJ, Kuo WW, Liu WH, Yin MC (2010) Antioxidative and anti-inflammatory protection from carnosine in the striatum of MPTP-treated mice. J Agric Food Chem 58(21):11510–11516. https://doi.org/10.1021/jf103258p
Volz TJ, Schenk JO (2004) L-arginine increases dopamine transporter activity in rat striatum via a nitric oxide synthase-dependent mechanism. Synapse 54(3):173–182. https://doi.org/10.1002/syn.20075
Wang Y, Zhan L, Zeng W, Li K, Sun W, Xu ZC, Xu E (2011) Downregulation of hippocampal GABA after hypoxia-induced seizures in neonatal rats. Neurochem Res 36(12):2409–2416. https://doi.org/10.1007/s11064-011-0565-4
Wang C, Yan M, Jiang H, Wang Q, He S, Chen J, Wang C (2018) Mechanism of aquaporin 4 (AQP 4) up-regulation in rat cerebral edema under hypobaric hypoxia and the preventative effect of puerarin. Life Sci 193:270–281. https://doi.org/10.1016/j.lfs.2017.10.021
Xie RX, Li DW, Liu XC, Yang MF, Fang J, Sun BL, Zhang ZY, Yang XY (2017) Carnosine attenuates brain oxidative stress and apoptosis after intracerebral hemorrhage in rats. Neurochem Res 42(2):541–551. https://doi.org/10.1007/s11064-016-2104-9
Yadav RS, Shukla RK, Sankhwar ML, Patel DK, Ansari RW, Pant AB, Islam F, Khanna VK (2010) Neuroprotective effect of curcumin in arsenic-induced neurotoxicity in rats. Neurotoxicology 31(5):533–539. https://doi.org/10.1016/j.neuro.2010.05.001
Yao L, Kan EM, Lu J, Hao A, Dheen ST, Kaur C, Ling EA (2013) Toll-like receptor 4 mediates microglial activation and production of inflammatory mediators in neonatal rat brain following hypoxia: role of TLR4 in hypoxic microglia. J Neuroinflammation 10:23. https://doi.org/10.1186/1742-2094-10-23
Ying GY, Jing CH, Li JR, Wu C, Yan F, Chen JY, Wang L, Dixon BJ, Chen G (2016) Neuroprotective effects of valproic acid on blood-brain barrier disruption and apoptosis-related early brain injury in rats subjected to subarachnoid hemorrhage are modulated by heat shock protein 70/matrix metalloproteinases and heat shock protein 70/AKT pathways. Neurosurgery 79:286–295. https://doi.org/10.1227/NEU.0000000000001264
Yu JH, Seo JH, Lee JE, Heo JH, Cho SR (2014) Time-dependent effect of combination therapy with erythropoietin and granulocyte colony-stimulating factor in a mouse model of hypoxic-ischemic brain injury. Neurosci Bull 30(1):107–117. https://doi.org/10.1007/s12264-013-1397-9
Zhang K, Zhao T, Huang X, Liu ZH, Xiong L, Li MM, Wu LY, Zhao YQ, Zhu LL, Fan M (2009) Preinduction of HSP70 promotes hypoxic tolerance and facilitates acclimatization to acute hypobaric hypoxia in mouse brain. Cell Stress Chaperones 14:407–415
Zhang Q, Qian Z, Pan L, Li H, Zhu H (2012) Hypoxia-inducible factor 1 mediates the anti-apoptosis of berberine in neurons during hypoxia/ischemia. Acta Physiol Hung 99(3):311–323. https://doi.org/10.1556/APhysiol.99.2012.3.8
Zheng Z, Kim JY, Ma H, Lee JE, Yenari MA (2008) Anti-inflammatory effects of the 70 kDa heat shock protein in experimental stroke. J Cereb Blood Flow Metab 28:53–63. https://doi.org/10.1038/sj.jcbfm.9600502
Acknowledgements
The authors extend their appreciation to the Deanship of Scientific Research at King Saud University for funding this work through research group NO. (RG-1438-061).
Limitation of the study
One of the important limitations in the current study is the assay of this array of markers in the whole brain homogenate. Therefore, in future study, our plan is to determine in which cerebral region these markers are induced.
Author information
Authors and Affiliations
Contributions
HA and LF designed the research. All authors participate in conducting experiments. HA analyzed data and wrote the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Attia, H., Fadda, L., Al-Rasheed, N. et al. Carnosine and l-arginine attenuate the downregulation of brain monoamines and gamma aminobutyric acid; reverse apoptosis and upregulate the expression of angiogenic factors in a model of hemic hypoxia in rats. Naunyn-Schmiedeberg's Arch Pharmacol 393, 381–394 (2020). https://doi.org/10.1007/s00210-019-01738-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-019-01738-8