Abstract
Ochratoxin A (OTA) and aristolochic acid (AA) are toxins that can frequently contaminate cereals and cereals-based products. The present study has realized a comparison between the effect of OTA and AA on oxidative stress and inflammation in both the liver and kidney of pigs as major organs involved in the metabolism of xenobiotics. Fifteen pigs (five pigs/group) were randomly distributed in three groups (control, OTA, and AA) and were fed diets contaminated or not with 250 μg toxin/kg for 28 days. Consumption of a diet contaminated with OTA and AA increase the concentration of serum creatinine as compared with the control group. The exposure of piglets to AA decrease the activity of enzymes involved in the oxidative stress response: catalase (CAT), superoxide dismutase (SOD), and glutathione peroxydase (GPx) in the liver and kidney while OTA decrease only GPx activity and only in the kidney. The consumption of the diets contaminated with AA increase in the liver the synthesis of tumor necrosis factor (TNF) alpha, interferon (IFN) gamma, Interleukin (IL)-1 beta, IL-6, and IL-8 synthesis, while IL-4 was increase by OTA and decreased by AA. In the kidney, AA increase the TNF alpha and IFN gamma synthesis as compared with the control. In conclusion, our results have shown that beside the alteration of serum markers, much known indicators for nephropathy, OTA and AA can induce inflammation and oxidative stress. In conclusion, the inflammatory effects were more pronounced for AA and at the liver level, while oxidative stress was induced both in the liver and kidney.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
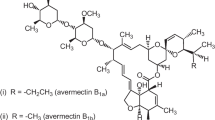
Ochratoxin A (OTA) and aristolochic acid (AA) are two of the etiological factors supposed to be at the origin of the Balkan endemic nephropathy (BEN), a tubulo-interstitial nephropathy with unknown origin described in Balkan Peninsula and in Romania (Peraica et al. 2008). The disease is associated with various forms of upper urinary tract cancer (Cukuranovic et al. 2010). Intoxications with OTA and AA occurred constantly in human population, due to the consumption of contaminated food commodities (Wu and Wang 2013). OTA and AA are toxic compounds with different chemical structure (Fig. 1) and origin. OTA is a toxic metabolite produced by fungus belonging to Aspergillus and Penicillium genera (Cabañes et al. 2010; el Khoury and Atoui 2010). AA is synthesized by Aristolochia clematitis, a weed that can grow in wheat fields in the Balkan region (Stiborová et al. 2016; Wu and Wang 2013). OTA can contaminate a large number of food commodities as wheat, oats, rice, and other food products such as grapes, raisins, wine, corn, soy, coffee, and beer (Bui-Klimke and Wu 2015; Vettorazzi et al. 2014). AA was frequently found in cereals and cereal products, as well as in Chinese medicinal products (Hranjec et al. 2005; Wu and Wang 2013).
The kidney and urothelial tract are the primary target organs for both toxins, but OTA and AA can induce other toxic effects as mutagenicity, teratogenicity, hepatotoxicity, neurotoxicity, immunotoxicity, etc. (Kuiper-Goodman and Scott 1989). AA was reported to be among the 2% most potent of known carcinogens, being classified as carcinogenic to humans (group 1) by the International Agency for Research on Cancer (IARC) (Arlt et al. 2002; IARC 2002). Also, OTA was classified by IARC as a possible human carcinogen (group 2b) (Ostry et al. 2017) but there are new evidences that can support the classification in group 2a of toxicity (Kuiper-Goodman 1996; Ostry et al. 2017). Kidneys and livers play essential roles in drug and toxin metabolism (van Montfoort et al. 2003). Even the renal toxicity of both OTA and AA was demonstrated, few studies have investigated the involvement of these two toxins in liver toxicity. For example, the interference with the pathways involved in liver damage and in metabolic disease OTA was shown to be responsible for early hepatotoxicity (Qi et al. 2014). Also, a subchronic intoxication in pigs with low dose of OTA-induced hepatocellular injury in intoxicated animals. AA-DNA adducts were detected in the liver (Schmeiser et al. 1988) and recent studies detected AA-like mutational patterns in hepatocellular carcinoma, which suggests an underappreciated carcinogenic role for AA in a subset of liver cancers (Poon et al. 2013).
Pigs and humans have anatomical and physiological similarities and therefore, the pig can be used as valuable preclinical model for medical research (Kobayashi et al. 2012). For example, the establishment of the provisional tolerable weekly intake of OTA for humans had been based on nephrotoxicity studies in pig model (Walker and Larsen 2005).
Oxidative stress has a critical role in the pathophysiology of several liver and kidney diseases, and many complications of these diseases are mediated by oxidative stress, oxidative stress-related mediators, and inflammation (Li et al. 2015; Ozbek 2012). Recent studies have attributed an important role of oxidative stress and inflammation to OTA and AA mediated toxicity (Marin et al. 2017a, b).
The present study has realized a comparison between the effect of OTA and AA on oxidative stress and inflammation in both the liver and kidney of pigs as the major organs involved in the metabolism of xenobiotics.
Material and methods
Reagents
All chemicals, immunological reagents, and media components were purchased from Sigma (Sigma-Aldrich, Steinheim, Germany) unless otherwise stated.
Animals and treatments
For this study, a total number of 15 cross-bred TOPIG hybrid [(landrace × large white) × (Duroc × Pietrain)] pigs with an average body weight of 10.9 ± 0.77 kg were allocated to three experimental groups (five pigs per group). Animals were cared for in accordance with the Romanian law 206/2004 and decision 28/2011 for handling and protection of the animals used for experimental purposes. The piglets were exposed to one of the three treatments: control group (C), ochratoxin group (OTA), and aristolochic acid (AA) for 28 days. The piglets were fed with a maize-soybean-meal-based diet (Table 1) contaminated or not with 250 μg OTA and respectively AA/kg feed (Sigma). Blood samples were aseptically collected on day 28, by jugular vein puncture. Plasma was obtained from blood after centrifugation at 3000 rpm; 20 min was used for the assessment of biochemical parameters. Pigs had free access to feed and water during the experimental period. At the end of the experiment (day 28), animals were slaughtered by exsanguination in an EU-licensed abattoir according to the EU Council directive 2010/63/CE. After slaughtering, samples of the liver and kidney were taken on ice and stored at − 80 °C until analyzed for cytokine concentration, activity of enzymes involved in oxidative stress, total antioxidant capacity, and lipid peroxidation. The study protocol was approved by the Ethical Committee of the National Research-Development Institute for Biology and Animal Nutrition, Balotesti Romania.
Mycotoxins analyses
The content of OTA was analyzed by high-performance liquid chromatography (HPLC) with fluorescence detection after clean-up with an immune-affinity column (Ochraprep, R-BIOPHARM) and a detection limit of 0.2 ppb. The concentration of OTA was 2.52 ppb in the control feed and 49.62 ppb in the OTA contaminated feed. Other mycotoxins concentration (DON, ZEN, FB1, FB2, T-2, HT-2, DAS, AFB1, AFB2, AFG1, AFG 2) were also analyzed by HPLC (Rommer Labs, Austria) with a detection limit of 50, 10, 25, 25, 25, 50, 40, 0.3, 0.1, 0.1, and 0.1 ppb respectively and with the exception of a low concentration of FB1 (88 ppb) the other mycotoxins were below the limit of detection.
Plasma biochemical parameters
Plasma was obtained from blood after centrifugation at 3000 rpm; 20 min was used for the assessment of biochemical parameters. Plasma concentrations of parameters reflecting the lipid (cholesterol, triglycerides) protein (total protein, albumin,), carbohydrate (glucose) metabolism, mineral status (phosphorus, calcium, magnesium, iron), liver functionality (total bilirubin), activity of alanine aminotransferase (ALAT), aspartate aminotransferase (ASAT), alkaline phosphatase (AP), and gamma-glutamyl transferase (GGT), as well as kidney functionality (creatinine, urea) were determined spectrophotometrically from plasma on a BS-130 Chemistry analyzer (BioMedical Electronics Co., LTD, China) using ACCENT kits (Cayman, Poland).
Determination of total antioxidant status
Total antioxidant capacity (TAC) assay was based on the absorption of ABTS+ cation [2,20-azinobis-(3-ethylbenzothiazoline- 6-sulfonic acid)] as already described (Marin et al. 2013b) in samples of plasma, the liver, and kidney, and inhibition percentages were converted into trolox equivalent antioxidant capacity (TEAC), expressed as μmol TEAC/g tissue.
Determination of nitric oxide concentration
Evaluation of the NO concentration in plasma was done using the Griess assay, based on transformation of NO2- into an azo-compound, in the presence of sulphanyl amide and napthylethlene-diamide (Marin et al. 2013a).
TBARS assessment
For the determination of thiobarbituric acid reactive substances (TBARS), frozen liver and kidney samples were homogenized in Tris HCL buffer containing thiobarbituric acid, as already described (Marin et al. 2017b). The absorbance at 532 nm was measured using a photometer (Tecan Sunrise, Austria). TBARS are reported as nmol/mg protein.
Cytokine measurement
Samples of frozen liver and kidney for each animal were homogenized in phosphate buffer containing 1% igepal, 0.5% sodium deoxycholate, 0.1% SDS, and complete (EDTA-free) protease inhibitor cocktail tablets, as already described (Marin et al. 2017b). The homogenates were kept 30 min on ice, and then centrifuged at 10,000 g at 4 °C for 10 min. The supernatants were frozen at − 20 °C, until analyzed for cytokine content by ELISA. Total protein content was measured using Bradford assay. Monoclonal anti-porcine antibody from the following: (i) R&D Systems (Minneapolis, USA): IL-1β (MAB6811), IL-10 (MAB6931), IL-6 (DuoSet ELISA, DY686), IL-8 (MAB5351), and TNF-α (MAB6902) or (ii) Invitrogen (Camarillo, Canada): IFN gamma (ASC4934) and IL-4 (ASC0944) were used as capture antibody in conjunction with anti-porcine cytokines-biotinylated antibodies: IL-1 β (BAF 681), IL-10 (BAF 693), IL-6 (DuoSet ELISA, DY686), IL-8 (BAF535), IFNγ (ASC4839), IL-4 (ASC0849), and TNF-α (BAF690). Streptavidin-HRP (Invitrogen, Camarillo, USA) and TMB (tetramethylbenzidine) were used for detection. Absorbance was read at 450 nm using a microplate reader (SUNRISE TECAN, Austria). Recombinant swine IL-1β, IL-10, IL-6, IL-8, IFN-γ, IL-4, and TNF-α were used as standards and results were expressed as picograms of cytokine/mL, after normalization to the total protein content of the samples.
Statistical analysis
All the results are expressed as mean ± standard error of the mean (SEM). ANOVA tests followed by a Fisher PSLD test were used to analyze the differences (StatView software 6.0, SAS Institute, Cary, NC). Values of P < 0.05 were considered significant.
Results
Plasma biochemistry parameters and antioxidant capacity
Compared with the control, consumption of a diet contaminated with 250 μg/kg OTA affect the protein metabolism, as resulting from the significant increase of the concentration of total protein, albumin, and creatinine in the OTA group with 14%, 10%, and 17% respectively as compared with the control group (Table 2). An increased concentration of triglycerides (23%) was induced by OTA but not by AA. Intoxication with 250 μg/kg AA, significantly increased only the creatinine concentration with 4.3% as compared with the control. The concentration of other investigated parameters: glucose, cholesterol, total bilirubin, urea, phosphorus, calcium, magnesium, iron, or the activity of enzymes: alanine aminotransferase, aspartate aminotransferase, alkaline phosphatase, and gamma-glutamyl transferase were not affected by both OTA and AA. Also, the intoxication with either OTA or AA does not interfere with the total antioxidant capacity of plasma and the nitric oxide concentration (Table 2).
Toxin-contaminated diet differentially modulated the oxidative status in the liver and kidney
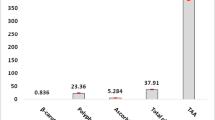
As compared with the control piglets, the exposure of piglets to AA significantly decrease (P < 0.05) the activity of enzymes involved in the oxidative stress response: CAT (− 37% in the liver; − 34% in the kidney); SOD (− 12% in the liver; − 13% in the kidney); GPx (− 64% in the liver; − 78% in the kidney). Two hundred micrograms per kilogram of OTA significantly decrease only GPx activity and only in the kidney (Fig. 2). When the total antioxidant capacity was investigated in the liver and kidney of the piglets, both OTA and AA induced a decrease of TAC by − 27% (P = 0.0003) and − 21% (P < 0.0001) respectively in the liver and by − 41% (P < 0.0001) and − 16% (P < 0.0001) respectively in the kidney. Lipid peroxidation as resulted from the assessment of thiobarbituric acid reactive substances was increased by both OTA and AA by 50% (P = 0.122) and by 43% (P = 0.235) respectively in the liver and by 70% (P = 0.0007) and by 173% (P < 0.0001) respectively in the kidney, as compared with the control. Also, the lipid peroxidation induced by AA was significantly increased (P < 0.0001) in the kidney when compared with OTA.
Effects of OTA and AA on cytokine synthesis in the kidney. The synthesis of TNF alpha, IFN gamma, IL-1 beta, IL-4, IL-6, IL-8, and IL-10 cytokines was analyzed by ELISA in the kidney of control and intoxicated piglets. Data are means ± SEM for six animals/group. *Indicate significant differences (P < 0.05) between groups
Intoxication of piglets with OTA or AA differentially affect the cytokine synthesis
The consumption of the diets contaminated with AA significantly increase the synthesis of TNF alpha (P = 0.001), IFN gamma (P = 0.007), IL-1 beta (P = 0.0004), IL-6 (P = 0.015), and IL-8 (P = 0.044) in the liver, decrease the synthesis of IL-4 (P < 0.0001), while has no effect on IL-10 synthesis as compared with the control (Fig. 3). Significantly higher concentration of TNF alpha (69 ± 1 vs. 54 ± 1 pg/mL), IFN gamma (5282 ± 407 vs. 4202 ± 232 pg/mL), IL-1 beta (2122 ± 132 vs. 2727 ± 145 pg/mL) were quantified in the liver of AA-intoxicated animals versus OTA-intoxicated ones. OTA exposure leaded to an increase of IL-4 synthesis in the liver of the intoxicated animals. In a similar manner, AA exposure was responsible in the kidney for an increase of TNF alpha (76 ± 5 vs. 96 ± 5 pg/mL) and IFN gamma (4976 ± 358 vs. 5692 ± 189 pg/mL), while no difference from the control was observed for IL-1 beta, IL-4, IL-6, IL-8, or IL-10 (Fig. 4). Also, AA exposure induced significantly higher concentration of TNF alpha (P = 0.042), IL-1 beta (P = 0.025), and IL-4 (P = 0.031) in the kidney of intoxicated animals as compared with OTA-intoxicated animals.
Effects of OTA and AA on cytokine synthesis in the liver. The synthesis of TNF alpha, IFN gamma, IL-1 beta, IL-4, IL-6, IL-8, and IL-10 cytokines was analyzed by ELISA in the liver of control and intoxicated piglets. Data are means ± SEM for six animals/group. *Indicate significant differences (P < 0.05) between groups
Effects of OTA and AA on oxidative stress. The activity of enzymes involved in oxidative stress response (CAT, GPx, SOD), total antioxidant capacity (TAC), and lipid peroxidation (TBARS) was analyzed in the kidney and liver of control and intoxicated piglets. Data are means ± SEM for six animals/group. *Indicate significant differences (P < 0.05) between groups. **Indicate significant differences (P < 0.0001) between groups
Discussion
The carcinogenic activity of both OTA and AA was well established (Pfohl-Leszkowicz 2009). In the risk assessment of carcinogenic substances, consideration of the mode of action is essential and despite many trials aiming to discover the mechanism that lead to the nephropathy progression, the sequence of events is still not clear. Inflammation and oxidative stress represents key factors in carcinogenesis, but the effect of OTA and AA on these two complex processes have been less investigated. Also, there are new evidences showing that beside the kidney, OTA and AA have important toxic effects on the liver (Marin et al. 2017a) (Poon et al. 2013). Swine could provide a good model for toxicological studies due to both anatomical and physiological similarities with humans (Swindle et al. 2012).
Serum creatinine and urea (or blood urea nitrogen - BUN) are routinely used in the minimal invasive clinical chemical analysis for the detection and monitoring of renal function (Zhang et al. 2014). Urea and creatinine are nitrogenous end products of protein metabolism, urea being the primary metabolite derived from dietary protein and tissue protein turnover, while creatinine is the product of muscle creatine catabolism (Stefanovic et al. 2007). Increased serum creatinine levels, mild tubular proteinuria, normoglycemic glucosuria, and anemia were observed in patients with endemic nephropathy (Pepeljnjak and Klaric 2010). Also, our results have shown that exposure of piglets to the two toxins for 28 days significantly increased the serum creatinine, albumin and total protein level for OTA and only the serum creatinine level for AA. The exposure of piglets to a higher concentration of OTA (300–2500 μg OTA/kg of feed) for 30 days resulted also in significantly higher serum levels of creatinine and urea (Harvey et al. 1994; Stoev et al. 2012). No studies were performed with AA in swine, but in rats, the AA intoxication (10 mg/kg b.w./day for 35 days) induced elevated serum creatinine levels associated with proximal tubule necrosis, microproteinuria, and glycosuria, resulting in interstitial renal fibrosis (Debelle et al. 2002). However, the sensitivity of serum creatinine and BUN as early markers of nephropathy is very poor and it has been observed that a reduction of renal functionality occurs only after approximately two thirds of renal biomass has been lost (Fuchs and Hewitt 2011).
Mechanisms for drug-induced nephrotoxicity include inflammation besides changes in glomerular hemodynamics, tubular cell toxicity, crystal nephropathy, rhabdomyolysis and thrombotic micro-angiopathy (Ferguson et al. 2008; Kim and Moon 2012). Nephrotoxic drugs often induce inflammation in glomerulus, proximal tubules, and surrounding cellular matrix and then fiberize the kidney tissue (Kim and Moon 2012), but few studies have investigated the role of AA and OTA in the inflammation. Many studies have shown a strong link between inflammation and carcinogenesis due to the fact that various types of cancer arise in the setting of chronic inflammation (Grivennikov et al. 2010). Our results have shown that AA and not OTA induces a significant increase of TNF alpha and IFN gamma in the kidney of exposed animals. Recent studies (Zhao et al. 2015) have shown that AA activate the pro-inflammatory pathways in the kidney of rats receiving 20 mg AA/kg b.w/week for 12 weeks through an increase in p-IκB and nuclear translocation of p65 subunits of NF-κB. We also have shown that AA has a high inflammatory effect in the liver as shown by the increase of TNF alpha, IFN gamma, IL-1 beta, IL-8, and IL-6, and a decrease of IL-4 in the liver. AA was classified by IARC as a potent carcinogen and oral administration of AA to rats resulted in neoplastic lesions of the kidney, forestomach, renal pelvis, urinary bladder, ear duct, thymus, small intestine, and pancreas (Cosyns et al. 1999; Cui et al. 2005; Hadjiolov et al. 1993). There are less evidence concerning the ability of AA to induce liver cancer. For example, Rossiello (Rossiello et al. 1993) has shown that single intraperitoneal injection of AA (10 mg/kg b.w.) increased the incidence of liver neoplastic nodules in rats when coupled with the liver tumor promoter orotic acid. The liver is one of the major organs for toxin biotransformation (Gu and Manautou 2012; Qi et al. 2014). The development of hepatocellular carcinoma (HCC) is one of the most extensively investigated inflammation-based carcinogenic processes because more than 90% of HCCs develop in the context of chronic liver damage and inflammation (Nakagawa and Maeda 2012). The toxins accumulate in the liver in concentrations similar to those found in the kidney (Vettorazzi et al. 2011), so there are high possibilities that inflammation could have an important role in the hepatocarcinogenic potential of AA. Indeed, AA-DNA adducts were detected in the liver (Schmeiser et al. 1988) and AA-like mutational patterns were identified in hepatocellular carcinoma (Poon et al. 2013).
Proximal tubule cells are exposed to toxins in the process of concentration and reabsorption through the glomerulus (Perazella 2005). The increase in oxidative stress by generation of free radicals represents one of the first cytotoxic effects observed in cells of proximal tubule (Markowitz and Perazella 2005; Zager 1997). On the other side, the liver is the target of xenobiotics because of its central role in xenobiotic metabolism, its portal location within the circulation, and its anatomic and physiologic structure (Sturgill and Lambert 1997). Abnormal ROS generation results in structural and functional abnormalities in the liver through the interaction with the cellular structures of hepatocytes (Cichoz-Lach and Michalak 2014). In general, an increased level of oxidative cell damage may be the result of an impairment of the antioxidant system, and this process could lead to carcinogenesis (Halliwell 2007).
Oxidative stress is a disturbance in the balance between the production of reactive oxygen species (ROS) and the antioxidant defense, and is often associated with toxin exposure (Nita and Grzybowski 2016). ROS can stimulate proliferation, invasiveness, angiogenesis, and metastasis, and inhibit apoptosis being considered as a pro-neoplastic factor (Halliwell 2007). Cells of eukaryote organisms have created defense mechanisms as antioxidant enzymes in the purpose to limit the damage caused by the action of free radicals (Lobo et al. 2010). When the system fails and the antioxidant control mechanisms are exhausted or overrun, the cellular redox potential shifts toward an oxidative and nitrosative stress, which leads to DNA mutations and genomic instability (Federico et al. 2007). Our results show that the defense mechanisms of the piglets were seriously damaged by the exposure to AA, resulting from the significant decrease of the activity of CAT, SOD, and GPx, and the decrease of the total antioxidant capacity in the kidney and liver of intoxicated animals. OTA induced a lower effect by decreasing the TAC in the liver and kidney and GPx activity only in the kidney.
Excepting our previous results (Marin et al. 2017a, b) that were lower dose of OTA (50 μg/kg feed) have increased the SOD activity in the liver and kidney of intoxicated animals; few studies concerning the oxidative stress induced by OTA were performed in swine. For example, it was shown that in swine, OTA was responsible for the decrease of the antioxidant capacity in blood and the kidney of weaned piglets (Zhang et al. 2016) and a significantly lower glutathione peroxidase activity in the liver and in the kidney of intoxicated animals (Balogh et al. 2007). A decrease of heme oxigenase (HO)-1 mRNA in the kidney, an indicative for cells stress, was observed in weaned pigs fed 181 μg/kg OTA (Bernardini et al. 2014). In other species, many studies have shown the capacity of OTA and AA to induce oxidative stress (Chen et al. 2010; Marin-Kuan et al. 2011). It looks like both AA and OTA can induce depletion of antioxidant defense by inhibition of Nrf2 responsible of response to the oxidative stress (Boesch-Saadatmandi et al. 2009; Cavin et al. 2007). Activation of the Nrf2-antioxidant signaling pathway represents a major mechanism in the cellular defense against oxidative stress (Ma 2013). The activation of Nrf2 pathway induce the expression of genes whose protein products are involved in the detoxication and elimination of reactive oxidants and enhance the cellular antioxidant capacity (Nguyen et al. 2009). In our study, the Nrf2 repression was associated with significant increase in Keap1 (a repressor of Nrf2 activation) and with a decrease in the Nrf2 targets (NQO1, GCLC, etc.) in both renal and hepatic cells (Cavin et al. 2007; Zhao et al. 2015). This alteration of the defense mechanism was associated with an increase of lipid peroxidation in the liver and kidney induced by both OTA and AA (Fig. 2). Lipid peroxidation has been found to play an important role in the toxicity and carcinogenesis of many carcinogens and marked increases in lipid peroxide levels and a concomitant decrease in enzymatic antioxidant levels after exposure to toxins in both the liver and kidney (Liu et al. 2009; Rastogi et al. 2001).
In conclusion, our results have shown that beside the alteration of serum markers, much known indicators for nephropathy, OTA, and AA can induce inflammation and oxidative stress. For the same experimental conditions, in terms of inflammation, the effects were more pronounced for AA and at the liver level, while oxidative stress was induced both in the liver and kidney but the effect was again more important for AA.
References
Arlt VM, Stiborova M, Schmeiser HH (2002) Aristolochic acid as a probable human cancer hazard in herbal remedies: a review. Mutagenesis 17(4):265–277. https://doi.org/10.1093/mutage/17.4.265
Balogh K, Hausenblasz J, Weber M, Erdelyi M, Fodor J, Mezes M (2007) Effects of ochratoxin A on some production traits, lipid peroxide and glutathione redox status of weaned piglets. Acta Vet Hung 55(4):463–470. https://doi.org/10.1556/AVet.55.2007.4.5
Bernardini C, Grilli E, Duvigneau JC, Zannoni A, Tugnoli B, Gentilini F, Bertuzzi T, Spinozzi S, Camborata C, Bacci ML, Piva A, Forni M (2014) Cellular stress marker alteration and inflammatory response in pigs fed with an ochratoxin contaminated diet. Res Vet Sci 97(2):244–250. https://doi.org/10.1016/j.rvsc.2014.07.018
Boesch-Saadatmandi C, Wagner AE, Graeser AC, Hundhausen C, Wolffram S, Rimbach G (2009) Ochratoxin A impairs Nrf2-dependent gene expression in porcine kidney tubulus cells. J Anim Physiol Anim Nutr 93(5):547–554. https://doi.org/10.1111/j.1439-0396.2008.00838.x
Bui-Klimke TR, Wu F (2015) Ochratoxin A and human health risk: a review of the evidence. Crit Rev Food Sci Nutr 55(13):1860–1869. https://doi.org/10.1080/10408398.2012.724480
Cabañes FJ, Bragulat MR, Castellá G (2010) Ochratoxin A producing species in the genus Penicillium. Toxins 2(5):1111–1120. https://doi.org/10.3390/toxins2051111
Cavin C, Delatour T, Marin-Kuan M, Holzhauser D, Higgins L, Bezencon C, Guignard G, Junod S, Richoz-Payot J, Gremaud E, Hayes JD, Nestler S, Mantle P, Schilter B (2007) Reduction in antioxidant defenses may contribute to ochratoxin A toxicity and carcinogenicity. Toxicol Sci 96(1):30–39. https://doi.org/10.1093/toxsci/kfl169
Chen YY, Chung JG, Wu HC et al (2010) Aristolochic acid suppresses DNA repair and triggers oxidative DNA damage in human kidney proximal tubular cells. Oncol Rep 24(1):141–153. https://doi.org/10.3892/or_00000839
Cichoz-Lach H, Michalak A (2014) Oxidative stress as a crucial factor in liver diseases. World J Gastroenterol 20(25):8082–8091. https://doi.org/10.3748/wjg.v20.i25.8082
Cosyns JP, Jadoul M, Squifflet JP, Wese FX, van Ypersele de Strihou C (1999) Urothelial lesions in Chinese-herb nephropathy. Am J Kidney Dis: Off J Natl Kidney Found 33(6):1011–1017. https://doi.org/10.1016/s0272-6386(99)70136-8
Cui M, Liu ZH, Qiu Q, Li H, Li LS (2005) Tumour induction in rats following exposure to short-term high dose aristolochic acid I. Mutagenesis 20(1):45–49. https://doi.org/10.1093/mutage/gei007
Cukuranovic R, Ignjatovic I, Visnjic M, Velickovic LJ, Petrovic B, Potic M, Stefanovic V (2010) Characteristics of upper urothelial carcinoma in an area of Balkan endemic nephropathy in South Serbia. A fifty-year retrospective study. Tumori 96(5):674–679. https://doi.org/10.1177/030089161009600505
Debelle FD, Nortier JL, De Prez EG et al (2002) Aristolochic acids induce chronic renal failure with interstitial fibrosis in salt-depleted rats. J Am Soc Nephrol: JASN 13(2):431–436
el Khoury A, Atoui A (2010) Ochratoxin A: general overview and actual molecular status. Toxins 2(4):461–493. https://doi.org/10.3390/toxins2040461
Federico A, Morgillo F, Tuccillo C, Ciardiello F, Loguercio C (2007) Chronic inflammation and oxidative stress in human carcinogenesis. Int J Cancer 121(11):2381–2386. https://doi.org/10.1002/ijc.23192
Ferguson MA, Vaidya VS, Bonventre JV (2008) Biomarkers of nephrotoxic acute kidney injury. Toxicology 245(3):182–193. https://doi.org/10.1016/j.tox.2007.12.024
Fuchs TC, Hewitt P (2011) Biomarkers for drug-induced renal damage and nephrotoxicity-an overview for applied toxicology. AAPS J 13(4):615–631. https://doi.org/10.1208/s12248-011-9301-x
Grivennikov SI, Greten FR, Karin M (2010) Immunity, inflammation, and cancer. Cell 140(6):883–899. https://doi.org/10.1016/j.cell.2010.01.025
Gu X, Manautou JE (2012) Molecular mechanisms underlying chemical liver injury. Expert Rev Mol Med 14:e4. https://doi.org/10.1017/s1462399411002110
Hadjiolov D, Fernando RC, Schmeiser HH, Wiessler M, Hadjiolov N, Pirajnov G (1993) Effect of diallyl sulfide on aristolochic acid-induced forestomach carcinogenesis in rats. Carcinogenesis 14(3):407–410
Halliwell B (2007) Oxidative stress and cancer: have we moved forward? Biochem J 401(1):1–11. https://doi.org/10.1042/bj20061131
Harvey RB, Kubena LF, Elissalde MH, Rottinghaus GE, Corrier DE (1994) Administration of ochratoxin A and T-2 toxin to growing swine. Am J Vet Res 55(12):1757–1761
Hranjec T, Kovac A, Kos J, Mao W, Chen JJ, Grollman AP, Jelaković B (2005) Endemic nephropathy: the case for chronic poisoning by aristolochia. Croat Med J 46(1):116–125
IARC (2002) Some traditional herbal medicines, some mycotoxins, naphthalene and styrene. IARC Monogr Eval Carcinog Risks Hum 82:1–556
Kim SY, Moon A (2012) Drug-induced nephrotoxicity and its biomarkers. Biomol Ther 20(3):268–272. https://doi.org/10.4062/biomolther.2012.20.3.268
Kobayashi E, Hishikawa S, Teratani T, Lefor AT (2012) The pig as a model for translational research: overview of porcine animal models at Jichi Medical University. Transp Res 1:8–8. https://doi.org/10.1186/2047-1440-1-8
Kuiper-Goodman T (1996) Risk assessment of ochratoxin A: an update. Food Addit Contam 13(Suppl):53–57
Kuiper-Goodman T, Scott PM (1989) Risk assessment of the mycotoxin ochratoxin a. Biomed Environ Sci: BES 2(3):179–248
Li T, Na R, Yu P et al (2015) Effects of dietary supplementation of chitosan on immune and antioxidative function in beef cattle. Czech J Anim Sci 60(1):38–44. https://doi.org/10.17221/43/2014-CJAS
Liu J, Qu W, Kadiiska MB (2009) Role of oxidative stress in cadmium toxicity and carcinogenesis. Toxicol Appl Pharmacol 238(3):209–214. https://doi.org/10.1016/j.taap.2009.01.029
Lobo V, Patil A, Phatak A, Chandra N (2010) Free radicals, antioxidants and functional foods: impact on human health. Pharmacogn Rev 4(8):118–126. https://doi.org/10.4103/0973-7847.70902
Ma Q (2013) Role of Nrf2 in oxidative stress and toxicity. Annu Rev Pharmacol Toxicol 53:401–426. https://doi.org/10.1146/annurev-pharmtox-011112-140320
Marin-Kuan M, Ehrlich V, Delatour T, Cavin C, Schilter B (2011) Evidence for a role of oxidative stress in the carcinogenicity of ochratoxin A. J Toxicol 2011:645361–645315. https://doi.org/10.1155/2011/645361
Marin DE, Braicu C, Gras MA, Pistol GC, Petric RC, Berindan Neagoe I, Palade M, Taranu I (2017a) Low level of ochratoxin A affects genome-wide expression in kidney of pig. Toxicon : Off J Int Soc Toxinology 136:67–77. https://doi.org/10.1016/j.toxicon.2017.07.004
Marin DE, Pistol GC, Gras MA, Palade ML, Taranu I (2017b) Comparative effect of ochratoxin A on inflammation and oxidative stress parameters in gut and kidney of piglets. Regul Toxicol Pharmacol: RTP 89:224–231. https://doi.org/10.1016/j.yrtph.2017.07.031
Marin DE, Pistol GC, Neagoe IV, Calin L, Taranu I (2013a) Effects of zearalenone on oxidative stress and inflammation in weanling piglets. Food Chem Toxicol 58:408–415. https://doi.org/10.1016/j.fct.2013.05.033
Marin DE, Pistol GC, Neagoe IV, Calin L, Taranu I (2013b) Effects of zearalenone on oxidative stress and inflammation in weanling piglets. Food Chem Toxicol: Int J Published Br Ind Biol Res Assoc 58:408–415. https://doi.org/10.1016/j.fct.2013.05.033
Markowitz GS, Perazella MA (2005) Drug-induced renal failure: a focus on tubulointerstitial disease. Clinica Chimica Acta; Int J Clin Chem 351(1–2):31–47. https://doi.org/10.1016/j.cccn.2004.09.005
Nakagawa H, Maeda S (2012) Inflammation- and stress-related signaling pathways in hepatocarcinogenesis. World J Gastroenterol 18(31):4071–4081. https://doi.org/10.3748/wjg.v18.i31.4071
Nguyen T, Nioi P, Pickett CB (2009) The Nrf2-antioxidant response element signaling pathway and its activation by oxidative stress. J Biol Chem 284(20):13291–13295. https://doi.org/10.1074/jbc.R900010200
Nita M, Grzybowski A (2016) The role of the reactive oxygen species and oxidative stress in the pathomechanism of the age-related ocular diseases and other pathologies of the anterior and posterior eye segments in adults. Oxidative Med Cell Longev 2016:3164734–3164723. https://doi.org/10.1155/2016/3164734
Ostry V, Malir F, Toman J, Grosse Y (2017) Mycotoxins as human carcinogens-the IARC monographs classification. Mycotoxin Res 33(1):65–73. https://doi.org/10.1007/s12550-016-0265-7
Ozbek E (2012) Induction of oxidative stress in kidney. Int J Nephrol 2012:465897–465899. https://doi.org/10.1155/2012/465897
Pepeljnjak S, Klaric MS (2010) <<Suspects>> in etiology of endemic nephropathy: aristolochic acid versus mycotoxins. Toxins 2(6):1414–1427. https://doi.org/10.3390/toxins2061414
Peraica M, Domijan AM, Saric M (2008) Mycotoxic and aristolochic acid theories of the development of endemic nephropathy. Arhiv za higijenu rada i toksikologiju 59(1):59–65. https://doi.org/10.2478/10004-1254-59-2008-1865
Perazella MA (2005) Drug-induced nephropathy: an update. Expert Opin Drug Saf 4(4):689–706. https://doi.org/10.1517/14740338.4.4.689
Pfohl-Leszkowicz A (2009) Ochratoxin A and aristolochic acid involvement in nephropathies and associated urothelial tract tumours. Arhiv za higijenu rada i toksikologiju 60(4):465–483. https://doi.org/10.2478/10004-1254-60-2009-2000
Poon SL, Pang ST, McPherson JR et al (2013, 5) Genome-wide mutational signatures of aristolochic acid and its application as a screening tool. Sci Transl Med (197):197ra101. https://doi.org/10.1126/scitranslmed.3006086
Qi X, Yang X, Chen S, He X, Dweep H, Guo M, Cheng WH, Xu W, Luo Y, Gretz N, Dai Q, Huang K (2014) Ochratoxin A induced early hepatotoxicity: new mechanistic insights from microRNA, mRNA and proteomic profiling studies. Sci Rep 4. https://doi.org/10.1038/srep05163
Rastogi R, Srivastava AK, Rastogi AK (2001) Long term effect of aflatoxin B(1) on lipid peroxidation in rat liver and kidney: effect of picroliv and silymarin. Phytother Res: PTR 15(4):307–310. https://doi.org/10.1002/ptr.722
Rossiello MR, Laconi E, Rao PM, Rajalakshmi S, Sarma DS (1993) Induction of hepatic nodules in the rat by aristolochic acid. Cancer Lett 71(1–3):83–87. https://doi.org/10.1016/0304-3835(93)90101-E
Schmeiser HH, Schoepe KB, Wiessler M (1988) DNA adduct formation of aristolochic acid I and II in vitro and in vivo. Carcinogenesis 9(2):297–303. https://doi.org/10.1093/carcin/9.2.297
Stefanovic V, Jelakovic B, Cukuranovic R, Bukvic D, Nikolic J, Lukic L, Gluhovschi G, Toncheva D, Polenakovic M, Cosyns JP (2007) Diagnostic criteria for Balkan endemic nephropathy: proposal by an international panel. Ren Fail 29(7):867–880. https://doi.org/10.1080/08860220701600732
Stiborová M, Arlt VM, Schmeiser HH (2016) Balkan endemic nephropathy: an update on its aetiology. Arch Toxicol 90(11):2595–2615. https://doi.org/10.1007/s00204-016-1819-3
Stoev SD, Gundasheva D, Zarkov I, Mircheva T, Zapryanova D, Denev S, Mitev Y, Daskalov H, Dutton M, Mwanza M, Schneider YJ (2012) Experimental mycotoxic nephropathy in pigs provoked by a mouldy diet containing ochratoxin A and fumonisin B1. Exp Toxicol Pathol: Off J Ges fur Toxikologische Pathol 64(7–8):733–741. https://doi.org/10.1016/j.etp.2011.01.008
Sturgill MG, Lambert GH (1997) Xenobiotic-induced hepatotoxicity: mechanisms of liver injury and methods of monitoring hepatic function. Clin Chem 43(8 Pt 2):1512–1526
Swindle MM, Makin A, Herron AJ, Clubb FJ Jr, Frazier KS (2012) Swine as models in biomedical research and toxicology testing. Vet Pathol 49(2):344–356. https://doi.org/10.1177/0300985811402846
van Montfoort JE, Hagenbuch B, Groothuis GM, Koepsell H, Meier PJ, Meijer DK (2003) Drug uptake systems in liver and kidney. Curr Drug Metab 4(3):185–211. https://doi.org/10.2174/1389200033489460
Vettorazzi A, de Troconiz IF, Gonzalez-Penas E et al (2011) Kidney and liver distribution of ochratoxin A in male and female F344 rats. Food Chem Toxicol 49(9):1935–1942. https://doi.org/10.1016/j.fct.2011.04.021
Vettorazzi A, Gonzalez-Penas E, de Cerain AL (2014) Ochratoxin A kinetics: a review of analytical methods and studies in rat model. Food Chem Toxic: Int J Published Br Ind Biol Res Assoc 72:273–288. https://doi.org/10.1016/j.fct.2014.07.020
Walker R, Larsen JC (2005) Ochratoxin A: previous risk assessments and issues arising. Food Addit Contam 22(Suppl 1):6–9. https://doi.org/10.1080/02652030500309343
Wu F, Wang T (2013) Risk assesement of upper tract urothelial carcinoma related to aristolochic acid. Cancer Epidemiol Biomark Prev 22(5):812–820. https://doi.org/10.1158/1055-9965.epi-12-1386
Zager RA (1997) Pathogenetic mechanisms in nephrotoxic acute renal failure. Semin Nephrol 17(1):3–14
Zhang Q, Davis KJ, Hoffmann D, Vaidya VS, Brown RP, Goering PL (2014) Urinary biomarkers track the progression of nephropathy in hypertensive and obese rats. Biomark Med 8(1):85–94. https://doi.org/10.2217/bmm.13.106
Zhang Z, Gan F, Xue H, Liu Y, Huang D, Khan AZ, Chen X, Huang K (2016) Nephropathy and hepatopathy in weaned piglets provoked by natural ochratoxin A and involved mechanisms. Exp Toxicol Pathol: Off J Ges fur Toxikologische Pathol 68(4):205–213. https://doi.org/10.1016/j.etp.2015.12.002
Zhao YY, Wang HL, Cheng XL, Wei F, Bai X, Lin RC, Vaziri ND (2015) Metabolomics analysis reveals the association between lipid abnormalities and oxidative stress, inflammation, fibrosis, and Nrf2 dysfunction in aristolochic acid-induced nephropathy. Sci Rep 5:12936. https://doi.org/10.1038/srep12936
Funding
This work was financed through the Nucleus Program thought the project PN 16 41 0202 financed by Romanian Ministry of Research.
Author information
Authors and Affiliations
Contributions
DM and IT conceived and designed the research. MG, DM, GP, and IT performed the in vivo experiments. GP and MP performed the ex vivo analysis (assessment of plasma biochemistry, oxidative stress parameters and cytokine synthesis). DM write the paper and performed the statistical analysis. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
The study protocol was approved by the Ethical Committee of the National Research-Development Institute for Biology and Animal Nutrition, Balotesti Romania.
Rights and permissions
About this article
Cite this article
Marin, D.E., Pistol, G.C., Gras, M. et al. A comparison between the effects of ochratoxin A and aristolochic acid on the inflammation and oxidative stress in the liver and kidney of weanling piglets. Naunyn-Schmiedeberg's Arch Pharmacol 391, 1147–1156 (2018). https://doi.org/10.1007/s00210-018-1538-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-018-1538-9