Abstract
Bladder afferent outflow, linked to sensation, plays a critical role in bladder pathology: abnormal outflow results in altered sensation, leading to increased voiding frequency, urge and often incontinence. β3-adrenoceptor agonists have been suggested to be beneficial in treating these symptoms. However, the absence of a significant sympathetic innervation of the detrusor and only a modest relaxation of bladder muscle by β3 agonists has questioned the therapeutic site of action of β3 agonists in the bladder. The present study was done to explore the possibility that β3-adrenoceptors might be located in the pelvic plexus. Using the rat, where the pelvic plexus is located primarily within a single ganglion, the major pelvic ganglion (MPG), immuno-histochemical approaches were used to identify structures expressing β3-adrenoceptor immuno-reactivity (β3AR-IR). The only structures found to express β3AR-IR were small-diameter tyrosine hydroxylase and vesicular mono-amine transporter immuno-reactive (TH-IR and vmat-IR) neurones. These neurones, found in clusters or singly on the periphery of the ganglion, or dispersed in smaller clumps throughout the MPG, are similar to the small intensely fluorescent (SIF) cells described previously. Not all small cells expressed β3AR-IR. A population of the small cells were also immuno-reactive to the type 3 muscarinic receptor (M3R-IR) and the P2X3 purinergic receptor (P2X3-IR). Clumps of small cells were associated with calcitonin gene-related peptide immuno-reactive (CGRP-IR) nerve fibres (putative sensory fibres) and a small number were contacted by putative cholinergic nerves expressing immuno-reactivity to vesicular acetylcholine transporter (vacht-IR). These observations are consistent with the idea that small cells are interneurons and one of the components making up complex neural circuits within the MPG. The precise physiological role of these neural elements in the MPG is unknown. However, as one therapeutic action of β3-adrenoceptor agonists is to modulate sensation, it is possible that these neural circuits may be involved in the regulation of afferent outflow and sensation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The site and specific mode of action of β3-adrenoceptor agonists in the management of the over active bladder (OAB) has become the centre of considerable research interest. Originally conceived to relax the detrusor via a direct action on β3-adrenoceptors at or near the bladder smooth muscle, there is now a growing body of data to suggest that other sites for β3-adrenoceptors should be considered to explain the therapeutic actions of these agents. At therapeutic doses of 25 or 50 mg/day, the plasma concentrations of mirabegron are in the region of 30–75 nM (Krauwinkel et al. 2012). In this concentration range, little relaxation can be seen in isolated strips of human bladder (Svalø et al. 2013). Therefore, additional β3-adrenoceptor-operated mechanisms associated with the lower urinary tract should be considered as potential targets for this drug.
In a rat model of detrusor overactivity (partial bladder outflow obstruction, pBOO), mirabegron, at similar doses to those used in humans, was reported to reduce the non-voiding activity (NVA) observed throughout the filling phase during cystometry in conscious animals but not to affect the voiding contractions (Gillespie et al. 2012). It has been argued that the mechanisms underlying NVA might be an alternative therapeutic target for β3-adrenoceptor agonists (Gillespie et al. 2012). NVA is thought to be the motor component of a motor-sensory system linked to bladder sensation (Sherrington 1892; Starling 1905; Iggo 1955; Vaughan and Satchell 1995; Gillespie 2004; Eastham and Gillespie 2013). Reducing NVA by β3-adrenoceptor activation might reduce bladder sensation and alleviate the symptoms of OAB (Eastham and Gillespie 2013).
Exploration of isolated bladder tissues from the rat revealed that mirabegron, in concentrations comparable to those in plasma using therapeutic doses, had little effect on intrinsic micro-contractile activity, nerve-mediated contractions or agonist-induced contractions (Gillespie et al. 2015a, b). These studies also suggested that the inhibition of micro-contractile activity appears to be influenced by a β1-adrenoceptor-dependent mechanism not β3. Consequently, despite attempts to identify β3-adrenoceptor mechanisms on contractile events within the rat bladder, no clear effect has yet been demonstrated. Therefore, there is a need to identify other elements within the LUT that might be a target for the therapeutic actions of β3-adrenoceptor activation.
For many years, it has been known that the peripheral ganglia played a key role in bladder physiology and pathology (Langley and Anderson 1895a, b, 1896; Gabella 1990; De Groat and Booth 1993; Uvelius and Gabella 1995). In almost all species, the pelvic plexus consists of a large number of diffuse small ganglia located close to the pelvic organs (Langley and Anderson 1895a). Also, in some species, ganglia are found in the bladder wall (intra-mural ganglia: Gosling and Dixon 1974; (Gosling and Dixon 1974; Dixon et al. 1983; Gabella 1990; Smet et al. 1996; Zhou and Ling 1998; Gosling et al. 1999; Gillespie et al. 2006). Simplistically, they have been proposed to operate as a relay point for the parasympathetic nervous system (De Groat and Booth 1980, 1993). However, the diversity of nerve types within these ganglia (Keast et al. 1989; De Groat and Booth 1993), the possibilty of complex synaptic circuitry (Dail et al. 1975) and the presence of possible intra-ganglionic inter-neurones, small intensely fluorescent (SIF) cells (Dail et al. 1975; Eränkö 1976, 1978), has led to a growing realisation that there are likely to be, as yet, unrecognised physiological systems operating in the ganglia.
In rats, the pelvic plexus is not a distributed network of ganglia. Unusually, the peripheral neurones are collected into a single large ganglion, containing both sympathetic and parasympathetic neurones (approximately 50:50). In male rats, this ganglion is known as the major pelvic ganglion (MPG) and in the female equivalent is a paracervical ganglion (Frankenhauser’s ganglion) (Langworthy 1965; El-Badawi and Schenk 1968; el-Badawi and Shenk 1968; Dail et al. 1975; Keast et al. 1989; De Groat and Booth 1993). Few, if any ganglia are found within the bladder wall of the rat (Uvelius and Gabella 1995). Thus, the MPG of the rat provides an opportunity to explore the peripheral neurological elements of the lower urinary tract.
Since evidence for functional β3-adrenoceptor mechanisms within the bladder wall of the rat is tenuous, the present experiments were done to explore the possibility that β3-adrenoceptor mechanisms might be operating within the MPG. In this study, immuno-histochemical techniques were employed to identify structures that might express β3-adrenoceptor immuno-reactivity (β3-IR) as well as immuno-reactivity to other signalling elements, e.g. the cholinergic, prostanoid and purinergic systems.
Methods
Tissue extraction and preparation
Wistar rats (male, n = 17 weight 250–270 g) were killed by stunning and cervical dislocation (Approved UK Home Office: Scheduled 1 killing). MPG were surgically removed and immediately immersed in 4 % paraformaldehyde made up in phosphate buffer saline (PBS) for 120 min at 4 °C. Tissues were then washed in PBS and incubated in solutions with progressively higher sucrose solutions (10, 20 and 30 %) to act as cryo-preservant. Tissue was subsequently ‘snap frozen’ using isopentane cooled to freezing point with liquid nitrogen. Frozen tissue was then kept at −80 °C until needed. Tissue sections (7–8 μm) were cut at −25 °C and subsequently placed on poly-lysine-coated slides. Tissue morphology was examined using a light microscope to confirm that gross structural features were intact. Slides were labelled and stored at −80 °C until used.
Staining procedures
Slides were removed from the freezer and maintained in a dry environment for 120 min. They were then washed in tris-buffer saline (TBS), tris-buffer saline tween (TBS-T) and TBS wash cycle for 5 min at each stage. Primary antibodies were diluted with 1× PBS or PBS with triton-X (1 %), pH 7.4. Combinations of primary antibodies (1°Abs) were then put on each slide and incubated overnight at 4 °C.
Primary polyclonal antibodies included against calcitonin gene-related peptide (CGRP) (1:500; Santa Cruz, Cat No. sc-57053), cyclooxygenase 1 (COX1) (1:100; Santa Cruz, Cat No. sc-1752), protein gene product 9.5 (PGP 9.5) (1:2,000; Seratec, Cat No. 7863-0604), neuronal nitric oxide synthase (NOS) (1:500; Santa Cruz, Cat No. 648), β3-AR (1:200; Santa Cruz, Cat No. sc-1473), tyrosine hydroxylase (TH) (1:5,000; Santa Cruz, Cat No, 14007), purinergic receptor P2X3 (P2X3) (1:200; Santa Cruz, Cat No. 25694), neuro-filament H protein (NF-H) (1:1,000; Abcam, Cat No. 9640796), muscarinic receptor type 3 (M3) (1:100; Santa Cruz, Cat No. sc-9108) and vesicular mono-amine transporter (vmat) (1:100; Santa Cruz, Cat No. sc-7721). These antibodies were chosen since they have been characterised at the molecular level and used in papers published in the literature (see manufacturers data sheets for more information).
For two of two of the key antibodies used in this study, β3-AR and muscarinic receptor type 3 (M3), specific characterisations have been published that give confidence in their epitope specificity (Grol et al. 2009; Cernecka et al. 2014).
After overnight incubation, sections were washed in TBS, TBS-T, TBS wash cycles each for 20 min. Sections were then incubated with appropriate secondary fluorescent antibodies: mouse, goat and rabbit primary antibodies were visualised using donkey anti-mouse/goat/rabbit IgG antibody conjugate (Molecular Probes) Alexa Fluor 488 or 594.2°Abs were applied in PBS and used at 1:500 dilutions. The secondary antibodies were applied sequentially and were applied for 1 h at room temperature. After each incubation, slides were washed three times in TBS, TBS-T and TBS. After the final wash, sections were covered with Vectashield hard-set mounting medium with DAPI (nucleic acid molecular probe stain) and over-laid with a cover-glass (24 × 60 mm). Varnish was applied to the cover-glass to preserve slides.
Image and microscope analysis
Sections were viewed using an Olympus BX61 fluorescence microscope with × 10, ×20 and × 60 objectives. Images were captured using an Olympus XM10 monochrome camera in 16-bits digital format and examined further using Image J software (Java-based image processing program—National Institutes of Health (US)).
Results
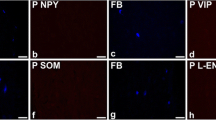
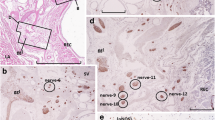
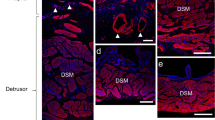
Figure 1 illustrates the cell types observed in the MPG. The general architecture, with large and small nerve cell bodies and cell processes, is seen in panel a, where all structures stain with the non-specific neuronal marker PGP (Wilson et al. 1988). It is noteworthy that a small number of neurones receive fibres that are immuno-reactive for CGRP (CGRP-IR: green, arrow) (see also panels c and d). In keeping with previous studies (Keast et al. 1989), approximately half of the neurones demonstrated tyrosine hydroxylase immuno-reactivity (TH-IR) or vesicular mono-amine transporter immuno-reactivity (vmat-IR) (panels b and c), suggesting that they are adrenergic. The remainder of the large neurones, showing weak immuno-reactivity to vacht, are likely to be cholinergic (see (Keast 1995). Many of the large adrenergic neurones are surrounded by vacht-IR fibres (panel b, (asterisk)). Other large neurones, weakly vacht-IR, are also surrounded by stronger vacht-IR fibres (panels b and d, (rhombus)), suggesting that these cells also are contacted by vacht-IR nerves. Large neurones, that are NOS-IR, are also found (panels e and f). Some of these neurones have NOS-IR terminals on their surface ((rhombus) panel e), suggesting the presence of nitrergic signalling between neurones. Panels f–h illustrate a further neuronal type found in the MPG. These are small-diameter TH-IR neurones (see arrowed structures in panels f, g and h). Based on the number and size, these are cells that have been previously described as the small intensely fluorescent cells (Dail et al. 1975; Eränkö 1976, 1978). Panel g shows that these cells are associated with CGRP-IR fibres. Importantly, panel h shows that these TH-IR small cells are also immuno-reactive to a β3-adrenoceptor antibody (β3AR-IR).
Illustrations of the major cell types observable in the major pelvic ganglion (MPG) of the rat. The antibody combinations used were: a, PGP 9.5 (red) and calcitonin gene related peptide (CGRP: green); b, vesicular mono-amine transporter (vmat: green) and vesicular acetylcholine transporter (vacht: red); c, tyrosine hydroxylase (TH: red) and CGRP (green): d, vacht (red) and CGRP (green): e, neuronal nitric oxide synthase (NOS: red) and CGRP (green); f, NOS (red) and TH (green); g, TH (red) and CGRP (green); h, TH (red) and β3-adrenoceptor (green). Arrows and symbols indicate specific features (see text). Sections e and h are also stained with the nuclear stain dapi (blue). Calibration bars: a and c 50 μm; b, f, g and h 30 μm; and d and e 20 μm
Figure 2a suggests that the only cells that demonstrate β3AR-IR in the MPG are the SIF cells (star). No large neurones were observed with β3AR-IR. Panel b shows a region of panel a demonstrating that the β3AR-IR cells (star) are contacted by CGRP-IR fibres (square). Figure 2c, d shows that not all TH-IR small cells are β3AR-IR suggesting that the population of small cells is heterogeneous. Figure 3 illustrates this heterogeneity again, but shows regional variation within the MPG. Collections of SIF cells are found with mixed TH-IR and β3AR-IR (area (b)), while other areas (a) are predominantly TH-IR. The heterogeneity is emphasised in Fig. 4 that shows images at higher magnification, β3AR-IR cells are seen in close contact to TH-IR only small cells (Fig. 4a). Also, in small clumps of SIF cells, single β3AR-IR are often observed (Fig. 4b).
Illustrations of staining associated with small-diameter SIF cells in the MPG. a demonstrates the observation that the only β3-adrenoceptor immuno-reactive cells (β3AR-IR: red) are SIF cells. Some β3AR-IR cells are in close apposition to nerve fibres that are immuno-reactive for CGRP (CGRP-IR: green). b shows a section of the image in a at higher magnification. c and d show a collection of SIF cells stained for TH (red) and β3 AR (green). Some cells are predominately TH-IR (red: rhombus) while there is a sub-population that are also β3AR-IR (green: star). These cells appear yellow indicative of co-localisation. Sections in c and d are also stained with the nuclear stain dapi (blue). Calibration bars: a and c 30 μm; b 20 μm; d 10 μm
Illustration of a regional variation within collections of SIF cells on the periphery of a MPG. a was stained to show tyrosine hydroxylase immuno-reactivity (TH-IR: red), β3-adrenoceptor immuno-reactivity (β3AR-IR: green) and dapi (blue). Predominantly TH-IR cells are indicated (rhombus) and cells with β3AR-IR (star). Regions of the image (boxes: a and b) are illustrated in the panels below where the images are separated into the component images. Note that within these large clumps, all SIF cells are TH-IR, while only a sub-population are β3AR-IR. Arrows indicate specific examples of cells or where they are present but demonstrate no immuno-reactivity. Calibration bars 15 μm
Illustrations of the heterogeneity of small clumps of small SIF cells. a shows a section illustrating TH-IR (red) and β3AR-IR (green) elements. Symbols and arrows indicate predominantly TH-IR (rhombus) and β3AR-IR (star) cells. b shows a region of a section stained for TH (red) and β3 AR (green). Part of this image (dotted rectangle) is shown in panel a with the component images (b) and (c). Note in (b) 4 TH-IR cells are seen (rhombus) but that only 1 cell is β3AR-IR positive (star). Calibration bars: a and b, 20 μm (small panels 10 μm)
Using a characterised antibody to the type 3 muscarinic receptor (M3R) (Grol et al. 2009), a sub-population of the SIF cells were seen to be immuno-reactive for the M3 receptor (M3-IR). Figure 5a illustrates a collection of small cells showing both TH-IR (red) and M3R-IR (green). Clearly two populations are seen: TH-IR and M3R-IR and TH-IR alone. The intensity of the M3R-IR appears to vary from strong to weak. Part of the image is shown along with the separate images. It is clear that some small cells express TH-IR and M3R-IR while others only express TH-IR.
Illustration of TH-IR and muscarinic type 3 receptor immuno-reactivity (M3R-IR) in SIF cells in the MPG. a illustrates a large and small clump of SIF cells on the periphery of a ganglion: TH-IR (rhombus) and M3 -IR (star). The region (a) is shown below (panel a) illustrating the combined and component images. M3R-IR and TH-IR positive cells (star: yellow) and TH-IR only cells (rhombus, red) cells can be identified. Calibration bars: a 25 μm and (a) 15 μm
It is likely that some of the small cells express both M3R-IR and β3AR-IR. Control experiments, using specific blocking peptides to these antibodies, were done to check this. By incubating each antibody with an excess of the specific peptide to which it was raised, then all specific antibody-binding sites are removed. Any residual staining is therefore non-specific. Figure 6 shows examples using serial sections to determine the extent of both M3R-IR and β3AR-IR with and without the respective blocking peptides. Figure 6a shows that the staining with the β3 AR antibody is removed by the blocking peptide. Figure 6b shows that the staining with the M3 antibody is also removed by blocking with its respective peptide. Thus, weight is given to the conclusion that the antibodies are detecting specifically M3 receptors and β3 AR on SIF cells.
Illustration of the effects of pre-incubation of the β3 AR and M3R antibodies with their respective blocking peptides on the detection of β3AR-IR and M3R-IR in small cells of the MPG. a (a) shows an image from a section stained showing vmat-IR (red) and β3AR-IR (green) (co-localising cells appear yellow). Individual stainings are shown in (b) and (c). Panels (d–e) show the same region in the next section. Here, the tissue was incubated with the same vmat antibody but now in conjunction with the β3 AR antibody plus blocking peptide. Images (c) and (e) were taken with the same exposure. b shows a similar experiment on serial sections examining the effects of the M3R blocking peptide. Note, comparison of panels (c) and (e) show the loss of M3R-IR in the presence of blocking peptide. Calibration bars: a 25 μm, b 20 μm
Figure 7 examines in more detail the close apposition of CGRP-IR fibres on β3AR-IR SIF cells. When present, these fibres give rise to multiple discrete foci of CGRP-IR. This pattern is seen on both β3AR-IR and TH-IR small cells. Not all SIF cells receive CGRP-IR fibres (Fig. 7f) although CGRP-IR fibres may run close by.
Examples of the close apposition of CGRP-IR processes to β3AR-IR cells (a–c) and TH-IR (d–f) SIF cells. A shows a small clump in which all cells are surrounded by CGRP-IR nerve processes. Adjacent to this is a single SIF cell with no CGRP-IR processes (square). b and c show magnified images illustrating the nature of the CGRP-IR processes on the SIF cells. Discrete punctate collections of CGRP-IR are readily seen. d and e illustrate TH-IR SIF cells in close apposition to fibres that are CGRP-IR. In f, a small clump of TH-IR cells is seen with no associated CGRP-IR structures. However, note the CGRP-IR fibres surrounding an adjacent large TH-IR positive neuron. Calibration bars: a 20 μm; b and c 10 μm; d, e, f and e 10 μm
Since there appears to be a population of the small cells that express M3R-IR, a series of experiments were done to see if cholinergic nerves were associated with small cells (Fig. 8). Using an antibody to vesicular acetylcholine transporter (vacht), vacht-IR could be detected in fibres within clumps of small cells (Fig. 8). Note that not all clumps of these cells show vacht-IR fibres.
Example of further complexities of the signalling elements that might impinge on SIF cells. a shows vesicular acetylcholine immuno-reactive (vacht-IR) nerve fibres in close apposition to SIF cells. vmat-IR large neurones (square: green) are seen to be surrounded by vacht-IR fibres (red). vmat-IR negative large neurones (putative cholinergic neurones) are also contacted by vacht-IR fibres (star, red). The boxes delineated by (a) and (b) are shown at higher magnification. vmat-IR positive SIF cells (green) are seen to be in close proximity to vacht-IR fibres (red). Only a small number of SIF cell clumps exhibit vacht-IR fibres. b shows further examples of small-diameter SIF cells that are not contacted by vacht-IR fibres and clumps of cells that are. Calibration bars: a 50 μm (insets 10 μm), b 20 μm (insets 10 μm)
Figure 9 illustrates additional observations made on small cells in the MPG. Firstly, these cells stain for an antibody to the P2X3 receptor. P2X3-IR was observed on the majority of small cells. Also, using an antibody to the enzyme responsible for production of prostaglandin (cyclooxygenase: COX1) COX1-IR was also detected. Finally, using an antibody to neuro-filament (NF), it was noted that the small cells did not express NF-IR in contrast to the large neurones in the ganglion.
Examples of additional immuno-reactivity of small cells in the MPG. a, b and c shows respectively staining with antibodies to the purinergic receptor P2X3, the enzyme cyclooxygenase (COX1) and to neuro-filament (NF). Note that the small cells do not stain with the NF antibody. Calibration bars: 50 μm
Discussion
The present study has identified a population of small-diameter neurones in the MPG of the rat that express β3AR-IR and M3R-IR. This conclusion relies on the specificity of the antibodies used. Since both antibodies have been characterised using a number of approaches (Grol et al. 2009; Cernecka et al. 2014) and here using specific blocking peptides, the observations described here may be looked upon with some confidence. If the detection of β3AR and M3R immuno-reactivity can be taken as evidence for the expression of functional receptors, then these observations support the idea that these cells are sensitive to both adrenergic and cholinergic agonists.
A population of small neurones within the MPG has been described previously (see De Groat and Booth 1993 for an overview). Because these cells were intensely fluorescent when viewed after formaldehyde fixation, they were described as ‘small intensely fluorescent’ cells. It is postulated that the small-diameter cells seen in this study, expressing β3AR-IR and M3R-IR, are SIF cells.
In early work, the presence of nerve fibres contacting SIF cells with small electron transparent vesicles was taken as indicative of a cholinergic input (Eränkö 1976). Also, using formaldehyde-induced fluorescence, adrenergic nerve terminals were proposed to surround SIF cells, suggestive of an adrenergic input. Similarly, catecholamines, derived from adjacent SIF cell processes or from the circulation, may also provide an input to SIF cells (Eränkö 1976). The present observations support these observations, showing nerve fibres in close apposition to SIF cells containing vacht, indicative of cholinergic transmission, and the presence of M3 receptors suggesting a responsiveness to acetylcholine. The presence of β3-adrenoceptors supports the idea that SIF cells can respond to catecholamines. Thus, there is now compelling evidence for a cholinergic and adrenergic signalling system associated with SIF cells of the MPG. What is important from this study is the identification of specific β3AR and M3R sub-types. It is noteworthy that not all SIF cells co-express β3AR-IR and M3R-IR, suggesting that there might be different populations of these cells. Indeed, two populations of SIF cells has already been suggested, type I and type II: type I have been suggested to be interneurons, while type II have properties more akin to neuro-endocrine cells (Owman et al. 1983; Taxi et al. 1983; De Groat and Booth 1993).
The present observations also show that SIF cells, in large and small clumps, are in close contact with CGRP-IR nerves. When associated with SIF cells, these CGRP-IR fibres appear as diffuse collections of small varicose structures, reminiscent of synaptic contacts. It is generally accepted that CGRP is found in afferent nerves. Afferent nerves from the bladder pass through the MPG en route to the dorsal root ganglia and the central nervous system. The CGRP-IR fibres, observed to contact SIF cells and also a population of large cholinergic and adrenergic neurones, are suggestive of a sensory input into neurones of the ganglia. This may constitute part of a reflex arc within the ganglion. Alternatively, the possibility exists that these CGRP fibres are not afferent and that they might originate from elsewhere, for example, the spinal cord. Evidence for this possibility remains to be obtained.
The complexity of the MPG and other peripheral ganglia has been recognised and has led to the suggestion that they are more than simple relay stations, having the machinery and capacity for information processing and modulated output. In relation to bladder function, this possibilty of complex circuitry has been explored primarily in relation to the control of functions associated with voiding (de Groat and Booth 1980; De Groat and Booth 1993). This is questionable. Although there is some evidence to suggest that there may be some modulation of efferent pathways, this does not appear to be a major site to modulate voiding.
There is evidence for information processing in other peripheral ganglia involved in motor-sensory systems in the gut, for example in the prevertebral ganglion (PVG). Here, systems modulating motility are linked to sensory processing. Mechano-sensory afferents fibres, passing through PVG send collaterals to sympathetic neurones. These peripheral inputs are then integrated with central inputs in a complex reflex system modulating gut motility and so indirectly influencing afferent outflow from the gut (Crowcroft et al. 1971; Szurszewski 1981; Szurszewski et al. 2002). The present study leads to speculation that similar reflex interactions within the MPG might modulate bladder systems that generate and modulate motor systems linked to afferent outflow, involved in motor control (Sugaya and de Groat 2007; Sugaya and De Groat 2009) and possibly bladder sensation (Eastham and Gillespie 2013) (see below).
It has been proposed that β3 agonists are effective in relieving the symptoms of OAB (Sacco and Bientinesi 2012; Sacco 2014). Specific β3-adrenoceptor agonists such as mirabegron were developed with the idea that they mimicked the effects of the sympathetic system in the bladder wall, to cause a relaxation of the detrusor and so reduce or remove activity associated with OAB. Indeed, there is evidence demonstrating the presence of β3-adrenoceptors in the bladder of both humans and rats (Seguchi et al. 1998; Fujimura et al. 1999). Also, that these receptors are coupled to adenylyl cyclase and that this system can relax pre-contracted strips of human and rat bladder (Igawa et al. 1998; Seguchi et al. 1998; Fujimura et al. 1999). Thus, a possible therapeutic mode of action of this class of drug was put forward. However, there is a difficulty with this proposed therapeutic mode of action of the β3-adrenoceptor agonists. In both humans and rats, the adrenergic innervation of the detrusor is sparse with large areas of the muscle having no adrenergic nerves (Watanabe and Yamamoto 1979; Dixon et al. 1992). Therefore, a function of physiological sympathetic regulation of the detrusor in the main body of the bladder wall is open for discussion.
In the rat, it has been shown that β3-adrenoceptor agonists are capable of modulating storage function. In one model of bladder over activity, intra-vesical infusion of PGE2, it was shown that the β3-adrenoceptor agonist CL316,243 prolonged bladder filling time and so reduced voiding frequency (Takeda et al. 2002). Also, in a decerebrate rat model, to study bladder function, plasma concentrations of mirabegron of 100 nM were sufficient to modulate bladder function (Sadananda et al. 2013). Therefore, in the rat, as in human, there is evidence for actions of β3-adrenoceptor agonists at low concentrations that are not mediated via sympathetic supply to the bladder wall or relaxation of the detrusor.
In a study using a different model of bladder over activity, cystometry in conscious rats with partial bladder outflow obstruction, it was shown that mirabegron and the M3R antagonist tolterodine had effects on the NVA observed during bladder filling: both mirabegron and tolterodine reducing NVA (Gillespie et al. 2012). It has been argued that NVA is part of a motor-sensory system operating in the bladder: the motor activity being coupled to afferent nerve discharge (Iggo 1955; Gillespie 2004). As the bladder fills, the motor activity increases, afferent outflow increases and, possibly, sensation is increased (Starling 1905; Iggo 1955; Vaughan and Satchell 1995; Gillespie 2004; Eastham and Gillespie 2013). Based on these observations, it was proposed that NVA and sensation were modulated by cholinergic excitatory and β adrenergic inhibitory inputs. However, where this regulation takes place is unknown.
The observations presented here, that SIF cells possess both β3AR-IR and M3R-IR, might provide some further insight. The SIF cells of the MPG appear to be a primary site for the expression of β3-adrenoceptors in structures associated with the organs of the lower pelvis. Since no major effects of β3-adrenoceptor agonists or M3 receptor antagonists have been noted on gut, prostate and penile function (Sacco and Bientinesi 2012; Chapple 2014; Chapple et al. 2014; Sacco 2014), it seems plausible that the β adrenergic system in which they operate is the bladder. Therefore, SIF cells may be a key element in the control of bladder function, possibly in the control of afferent outflow and sensation. As SIF cells express both β3AR-IR and M3R-IR, it is possible that these collections of cells in the pelvic ganglion are the site for the physiological integration of both cholinergic and adrenergic inputs. The SIF cells are potentially part of a greater neural network, consisting of afferent inputs from the bladder wall and CNS that has the capability to influence the generation and regulation of NVA. The reflex pathways and the intra-ganglionic elements possibly involved in this motor-sensory regulation are illustrated in Fig. 10b. Thus, it can be hypothesised that the site of peripheral and central modulation of the motor system involved in generating afferent outflow from the bladder in the rat resides in the MPG.
Cartoons summarising the key observations. d shows that clumps of SIF cells of different sizes are readily found within all regions of the MPG. All cells are TH-IR and vmat-IR. There is the indication that all cells may also be COX1-IR and P2X3-IR. In addition, there appear to be sub-populations that are β3AR-IR or M3R-IR or may express both β3AR-IR and M3R-IR. The largest clumps and the majority of smaller clumps are associated with fibres showing CGRP-IR. Some clumps show no CGRP-IR. A small number of small clumps also appear to have fibres that are vacht-IR, suggesting the presence of cholinergic nerve fibres. Single, isolated SIF cells are also found. b suggests (1) possible complex interactions that might occur within the MPG and between the different components and (2) possible physiological systems that such interactions and neural circuitry might involve. Such circuitry is similar to that described in the inferior mesenteric ganglion (Szurszewski et al. 2002). SIF cells are likely to have inputs from sympathetic adrenergic neurones [ref] and cholinergic fibres (vacht-IR). These fibres may be involved in the activation of β3 AR and M3R on sub-populations of SIF cells. They also have inputs from afferent fibres (CGRP-IR). As SIF cells also express TH-IR and vmat-IR, there is the likelihood that they can release catecholamines, suggesting that they can act in a paracrine manner on adjacent cells within the clumps. Based on observations on isolated tissues and the whole animals using β3 AR agonists (Gillespie et al. 2012; Gillespie et al. 2015b), it is proposed that this system may function to modulate motor activity during the filling phase: non-voiding activity. This system is in addition to but different from that involved in activation of the detrusor during voiding
If this analysis for the situation we observed in rats, in spite of the anatomical differences brought up earlier in this paper, is translatable to the human situation, it implies a concept that there are mechanisms located in the periphery, capable of modulating bladder afferent outflow. The possibility of having both excitatory and inhibitory inputs suggests that it could function to increase or decrease afferent outflow from the bladder. If so, then this represents a possible mechanism that would allow a degree of control of bladder sensation. It is part of everyday experience that sensations of bladder fullness can increase and decrease, despite there being no change in bladder volume. Almost certainly, such modulation will have a central component. However, the modulation of sensation by β3-adrenoceptor agonists and specific M3 cholinergic antagonists, the identification of β3AR-IR and M3R-IR on SIF cells and the possibility that these elements are involved in regulating a motor-sensory system suggest that there are also mechanisms in the periphery involved in the modulation of bladder sensation (Eastham and Gillespie 2013).
References
Cernecka H, Pradidarcheep W, Lamers WH, Schmidt M, Michel MC (2014) Rat beta(3)-adrenoceptor protein expression: antibody validation and distribution in rat gastrointestinal and urogenital tissues. Naunyn Schmiedebergs Arch Pharmacol 387(11):1117–1127
Chapple C (2014) Mirabegron the first beta3 -adrenoceptor agonist for overactive bladder (OAB): a summary of the phase III studies. BJU Int 113(6):847–848
Chapple CR, Nitti VW, Khullar V, Wyndaele JJ, Herschorn S, van Kerrebroeck P et al. (2014) Onset of action of the beta3-adrenoceptor agonist, mirabegron, in Phase II and III clinical trials in patients with overactive bladder. World J Urol 32:1565–1572
Crowcroft PJ, Holman ME, Szurszewski JH (1971) Excitatory input from the distal colon to the inferior mesenteric ganglion in the guinea-pig. J Physiol 219(2):443–461
Dail WG Jr, Evan AP Jr, Eason HR (1975) The major ganglion in the pelvic plexus of the male rat—a histochemical and ultrastructural study. Cell Tissue Res 159(1):49–62
De Groat W, Booth AM (1993) Synaptic transmission in pelvic ganglia. In: Nervous control of the urogenital system. CA Maggi editor: Harwood academic publishers
de Groat WC, Booth AM (1980) Inhibition and facilitation in parasympathetic ganglia of the urinary bladder. Fed Proc 39(12):2990–2996
Dixon JS, Gilpin SA, Gilpin CJ, Gosling JA (1983) Intramural ganglia of the human urinary bladder. Br J Urol 55(2):195–198
Dixon JS, Gosling JA, Canning DA, Gearhart JP (1992) An immunohistochemical study of human postnatal paraganglia associated with the urinary-bladder. J Anat 181:431–436
Eastham JE, Gillespie JI (2013) The concept of peripheral modulation of bladder sensation. Organogenesis 9(3):177–186
el-Badawi A, Shenk EA (1968) A new theory of the innervation of bladder musculature. 1. Morphology of the intrinsic vesical innervation apparatus. J Urol 99(5):585–587
El-Badawi A, Schenk EA (1968) The peripheral adrenergic innervation apparatus - I. Intraganglionic and extraganglionic adrenergic ganglion cells. Zeitschrift für Zellforschung und Mikroskopische Anatomie 87(2):218–225
Eränkö O (1976) SIF cells, chromaffin cells, granule-containing cells, and interneurons. In: Eränkö O (ed) SIF cells structure and function of the small, intensely fluorescent sympathetic cells. Raven Press, New York, pp 1–7
Eränkö O (1978) Small intensely fluorescent (SIF) cells and nervous transmission in sympathetic ganglia. Annu Rev Pharmacol Toxicol 18:417–430
Fujimura T, Tamura K, Tsutsumi T, Yamamoto T, Nakamura K, Koibuchi Y et al (1999) Expression and possible functional role of the β3-adrenoceptor in human and rat detrusor muscle. J Urol 161(2):680–685
Gabella G (1990) Intramural neurons in the urinary-bladder of the guinea-pig. Cell Tissue Res 261(2):231–237
Gillespie JI (2004) The autonomous bladder: a view of the origin of bladder overactivity and sensory urge. BJU Int 93(4):478–483
Gillespie JI, Markerink-Van Ittersum M, De Vente J (2006) Sensory collaterals, intramural ganglia and motor nerves in the guinea-pig bladder: evidence for intramural neural circuits. Cell Tissue Res 325(1):33–45
Gillespie JI, Rouget C, Palea S, C. G, Korstanje C (2015) Beta adrenergic modulation of spontaneous microcontractions and electrical field-stimulated contractions in isolated strips of the rat bladder from normal animals and animals with partial bladder outflow obstruction NSAP - Submitted Ref No -NSAP-D-14-00220
Gillespie JI, Palea S, Guilloteau V, Guerard M, Lluel P, Korstanje C (2012) Modulation of non-voiding activity by the muscarinergic antagonist tolterodine and the beta(3)-adrenoceptor agonist mirabegron in conscious rats with partial outflow obstruction. BJU Int 110(2 Pt 2):E132–E142
Gillespie JI, Rouget C, Palea S, Granato C, Birder L, Korstanje C (2015). The characteristics of intrinsic complex micro-contractile activity in isolated strips of the rat bladder NSAP - Submitted Ref No -NSAP-D-14-00219
Gosling JA, Dixon JS (1974) Sensory nerves in mammalian urinary-tract—evaluation using light and electron-microscopy. J Anat 117:133–144
Gosling JA, Dixon JS, Jen PYP (1999) The distribution of noradrenergic nerves in the human lower urinary tract. Rev Eur Urol 36(1):23–30
Grol S, Essers PBM, Van Koeveringe GA, Martinez-Martinez P, De Vente J, Gillespie JI (2009) M 3 muscarinic receptor expression on suburothelial interstitial cells. BJU Int 104(3):398–405
Igawa Y, Yamazaki Y, Takeda H, Akahane M, Ajisawa Y, Yoneyama T et al (1998) Possible β3-adrenoceptor-mediated relaxation of the human detrusor. Acta Physiol Scand 164(1):117–118
Iggo A (1955) Tension receptors in the stomach and the urinary bladder. J Physiol 128(3):593–607
Keast JR (1995) Visualization and immunohistochemical characterization of sympathetic and parasympathetic neurons in the male rat major pelvic ganglion. Neuroscience 66(3):655–662
Keast JR, Booth AM, De Groat WC (1989) Distribution of neurons in the major pelvic ganglion of the rat which supply the bladder, colon or penis. Cell Tissue Res 256(1):105–112
Krauwinkel W, van Dijk J, Schaddelee M, Eltink C, Meijer J, Strabach G et al (2012) Pharmacokinetic properties of mirabegron, a β3-adrenoceptor agonist: results from two phase I, randomized, multiple-dose studies in healthy young and elderly men and women. Clin Ther 34(10):2144–2160
Langley JN, Anderson HK (1895a) The innervation of the pelvic and adjoining viscera. Part 1. The lower portion of the intestine. J Physiol(London) 18(:67–105
Langley JN, Anderson HK (1895b) The innervation of the pelvic and adjoining viscera. Part 2. The bladder. J Physiol(London) 19:71–84
Langley JN, Anderson HK (1896) The innervation of the pelvic and adjoining viscera. Part 7. Anatomical observations. J Physiol(London) 20:372–406
Langworthy OR (1965) Innervation of the pelvic organs of the rat. Invest Urol 2:491–511
Owman C, Alm P, Sjoberg N (1983) Pelvic autonomic ganglia: structure, transmitters, function and steroid influence. In: Elfvin LG (ed) Autonomic Ganglia. John Wiley and Sons Ltd, New York
Sacco E (2014) Discovery history and clinical development of mirabegron for the treatment of overactive bladder and urinary incontinence. Expert Opin Drug Discov EPub Ahead of print
Sacco E, Bientinesi R (2012) Mirabegron: a review of recent data and its prospects in the management of overactive bladder. Ther Adv Urol 4(6):315–324
Sadananda P, Drake M, Paton J, Pickering A (2013) A functional analysis of the influence of beta 3-adrenoceptors on the rat micturition cycle. J Pharmacol Exp Ther 347:506–515
Seguchi H, Nishimura J, Zhou Y, Niiro N, Kumazawa J, Kanaide H (1998) Expression of β3-adrenoceptors in rat detrusor smooth muscle. J Urol 159(6):2197–2201
Sherrington CS (1892) Notes on the arrangement of motor fibers in the lumbo-sacral plexus. J Physiol 13:621–772
Smet PJ, Edyvane KA, Jonavicius J, Marshall VR (1996) Neuropeptides and neurotransmitter-synthesizing enzymes in intrinsic neurons of the human urinary bladder. J Neurocytol 25(2):112–124
Starling EH (1905) Elements of human physiology, 7th edn. London, Churchill
Sugaya K, de Groat WC (2007) Bladder volume-dependent excitatory and inhibitory influence of lumbosacral dorsal and ventral roots on bladder activity in rats. Biomed Res 28(4):169–175
Sugaya K, De Groat WC (2009) Excitatory and inhibitory influence of pathways in the pelvic nerve on bladder activity in rats with bladder outlet obstruction. Lower Urinary Tract Symptoms 1(1):51–55
Svalø J, Nordling J, Bouchelouche K, Andersson KE, Korstanje C, Bouchelouche P (2013) The novel β3-adrenoceptor agonist mirabegron reduces carbachol-induced contractile activity in detrusor tissue from patients with bladder outflow obstruction with or without detrusor overactivity. Eur J Pharmacol 699(1-3):101–105
Szurszewski JH (1981) Physiology of mammalian prevertebral ganglia. Ann Rev Physiol 43:53–68
Szurszewski JH, Ermilov LG, Miller SM (2002) Prevertebral ganglia and intestinofugal afferent neurones. Gut 51(1):i6–i10
Takeda H, Yamazaki Y, Igawa Y, Kaidoh K, Akahane S, Miyata H et al (2002) Effects of β3-adrenoceptor stimulation on prostaglandin E2-induced bladder hyperactivity and on the cardiovascular system in conscious rats. Neurourol Urodyn 21(6):558–565
Taxi J, Derer M, Domich A (1983) Morphology and histophysiology of SIF cells in the autonomic ganglia. In: Elfin L (ed) Autonomic ganglia. John Wiley and Sons Ltd, New York, pp 67–95
Uvelius B, Gabella G (1995) Intramural neurones appear in the urinary bladder wall following excision of the pelvic ganglion in the rat. NeuroReport 6(16):2213–2216
Vaughan CW, Satchell PM (1995) Urine storage mechanisms. Prog Neurobiol 46(2-3):215–237
Watanabe H, Yamamoto TY (1979) Autonomic innervation of the muscles in the wall of the bladder and proximal urethra of male rats. J Anat 128(4):873–886
Wilson PO, Barber PC, Hamid QA, Power BF, Dhillon AP, Rode J et al (1988) The immunolocalization of protein gene product 9.5 using rabbit polyclonal and mouse monoclonal antibodies. Br J Exp Pathol 69(1):91–104
Zhou Y, Ling EA (1998) Colocalization of nitric oxide synthase and some neurotransmitters in the intramural ganglia of the guinea pig urinary bladder. J Comp Neurol 394(4):496–505
Compliance with ethical standards
This manuscript has been prepared to comply with all required ethical standards. There are no conflicts of interest to be declared.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Eastham, J., Stephenson, C., Korstanje, K. et al. The expression of β3-adrenoceptor and muscarinic type 3 receptor immuno-reactivity in the major pelvic ganglion of the rat. Naunyn-Schmiedeberg's Arch Pharmacol 388, 695–708 (2015). https://doi.org/10.1007/s00210-015-1122-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-015-1122-5