Abstract
To investigate the biological characteristics of monoclonal antibodies (mAbs) against avian influenza virus (AIV) and the possible mechanism of AIV-related kidney injury. BALB/c mice were immunized with inactivated H5N1 AIV to prepare monoclonal antibody H5-32, and its subtype, titer and cross-reactivity with other influenza viruses were identified. The reactivity of monoclonal antibody with normal human tissue was analyzed by immunohistochemistry. Immunofluorescence and confocal laser scanning technique were used to detect the binding sites between mAb and human renal cortical cells, and Western blotting was used to detect the size of binding fragments. Immunohistochemical analysis confirmed that monoclonal antibody H5-32 cross-reacted with normal human kidney tissue. In human kidney, mAb H5-32 was localized in the cytoplasm of human renal tubular epithelial cells, and its binding fragment size was about 43 kDa. H5N1 AIV appears to bind to human renal tubular epithelial cells, which may be one of the mechanisms of kidney injury caused by AIV infection.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The influenza virus is a type of enveloped negative-strand RNA virus belonging to the orthomyxoviridae family, and it can infect a variety of hosts. The highly pathogenic avian influenza viruses (AIVs), including H5N1, H7N9, and other subtypes, have the ability to infect humans and can cause fatal disease, and is therefore considered a major threat to public health (Adlhoch et al. 2023; Kniss et al. 2022). Since the first cases of the H5N1 influenza virus infection were reported in 1997, thousands of cases have been detected, and the fatality rate is extremely high (Abubakar et al. 2016; Zhao et al. 2023). The H5N1 virus mainly affects the lungs and lower respiratory tract of humans, but there have been reports of the virus spreading outside the lungs. In relatively rare or severe cases, the virus has been detected in the brain, intestine, and lymphoid tissue (Gu et al. 2007; Zhang et al. 2022; Sangsiriwut et al. 2021). Furthermore, there have been reports of an association between H5N1 avian influenza virus infection and effects in multiple organs other than the lungs, with disorders including local steatosis, hepatic congestion edema, kidney hyperemia edema, and acute tubular necrosis, among others (Gao et al. 2010).
In our previous work, we found that monoclonal antibody (mAb) H5-32 against H5N1 avian influenza virus can cross-reacts with human kidney tissue (Li et al. 2017). On further investigation, we confirmed the cross-reactivity of mAb H5-32 with renal tubular epithelial cells, which may provide some clues to the mechanism of acute kidney injury caused by influenza virus.
Materials and methods
Materials
H5N1 avian influenza virus (Re-5 + Re-4) was purchased from Qingdao Yibang Biotech Co. Ltd. (Qingdao, China). RPMI-1640 medium was a customized product from Hyclone Company (Utah State, USA). Fetal bovine serum (FBS) was from Sijiqing Company (Hangzhou, China). Horseradish peroxidase (HRP)-conjugated goat anti-mouse IgG was provided by Thermo Fisher Company (Massachusetts, USA). Two types of human tissue microarray were used in this study: one contained 33 cases of different normal human tissue, and another included 21 samples of normal human kidney tissues (Shaanxi Chaoying Biotech Co. Ltd., Xi’an, China). Immunohistochemical staining kits were purchased from Beijing Jinqiao Biological Technology Company (Xi’an, China). Human kidney cortexes were obtained from FengHui Biotechnology Company (Xi’an, China). Cy3 (Cy3-labeled goat anti-mouse IgG [H + L]) antibody was purchased from Kangwei Century Biotechnology Company (Xi’an, China). 4-6-Diamino-2-phenyl indole (DAPI) staining kits were purchased from Bioworld Technology Company (Beijing, China). SBA Clonotyping™ System/HRP kit was purchased from Southern Biotech Company (Alabama, USA). Institutional animal care and the committee of Shaanxi provincial people’s hospital approved the animal experiment.
Methods
Preparation and characterization of the mAb
The H5N1 avian influenza virus was extracted by isobutanol and purified by centrifuge speed (106 g) and sucrose gradient centrifugation. Purified H5N1 antigen combined with complete Freund’s adjuvant and injected into BALB/c mice. Afterward, positive hybridomas were screened by an indirect ELISA method and then cloned by limited dilution to establish stable hybridoma cell line with expanded culture and cryopreserved in liquid nitrogen. BALB/c mice were injected intraperitoneally with liquid paraffin. After 1 week, they were intraperitoneally inoculated with the hybridoma cell lines, and ascites produced by the mice were collected and purified (Zhang 2012; Walls et al. 1986). The SBA Clonotyping™ System/HRP kit was used to identify the subtypes of antibodies. Western blotting determined the reactivity of purified antibodies with H5N1 antigen.
Immunohistochemical reaction of human tissues with the mAb H5-32
Human tissue microarray chips were used to detect the binding of mAb H5-32 with normal human tissue by immunohistochemical staining. Briefly, paraffin sections were dewaxed, hydrated, and treated with 3% H2O2 to eliminate endogenous peroxidase, heated by microwave for 10 min in citrate buffer (pH 6.0), and cooled to room temperature. After blocking with 10% goat serum solution, sections were treated with diluted primary antibody (1:500 dilution for mAb H5-32) at 4 ℃ overnight and washed with PBS three times before HRP-labeled goat anti-mouse secondary antibody (1:1000) was added. Sections were incubated for 1 h at 37 ℃ and then washed three times with PBS, then exposed to DAB for 10 min at room temperature. Finally, the sections were counterstained with hematoxylin, dehydrated, sealed, and observed under a microscope.
Immunohistochemical reaction of HKC cells with the H5-32 mAb
Human renal tubular epithelial cells (HKC) were cultured on slides overnight. On the second day, the cells were washed with PBS for three times, and then immunohistochemical experiments were performed. The cells were fixed with 4% paraformaldehyde for 20 min. Then, HKC cells were washed with PBS three times again, and then covered with normal goat serum for about 30 min. The goat serum was discarded and diluted mAb H5-32 was added overnight at 4 ℃. The next day, the cells were washed with PBS three times, and then goat anti-mouse secondary antibody labeled with HRP (1:1000) was incubated at 37 ℃ for 1 h. After washing with PBS for three times, DAB was added. Finally, the sections were counterstained with hematoxylin, dehydrated, sealed, and observed under a microscope. The staining results were evaluated according to Yu's standard score (Yu et al. 2009).
The immunofluorescence test of mAb H5-32 and HKC cell
Slides of cultured HKC cells were placed in culture dishes and washed with PBS for three times. 4% paraformaldehyde was cold fixed for about 20 min, washed three times with PBS, and covered with normal goat serum for about 30 min. The serum was poured out, diluted monoclonal antibody H5-32 was added and incubated at 37 ℃ for 2 h, then the liquid was discarded, washed three times with PBS, and diluted secondary antibody (Cy3-coupled mice) was added and incubated at 37 ℃ for 1 h in the dark. Diluted DAPI (1:5000) was stained at room temperature for 30 min, washed with PBS for 5 min four times, sealed, and observed under fluorescence microscope.
The technique of confocal laser scanning microscopy of mAb H5-32 and HKC cells
The HKC cells were spread on slides and washed twice with PBS 12 h later. The cells were fixed with 4% precooled paraformaldehyde for 10 min. After being washed once with PBS, the slides were incubated for 2 min with PBS containing 0.1% Triton X-100 in ice. The sections were then placed in PBS containing 2% goat serum and covered for 1 h at 37 ℃. The fluid was then poured off, and 50 µL of mAb H5-32 (1:500 dilutions) was added to cover cells, followed by incubation at 37 ℃ for 2 h. The cell smears were removed from the H5-32 solution, washed in PBS for 3 min three times. With light exposure being avoided, 50 µL of secondary antibody (goat anti-mouse Cy3 red fluorescence, 1:200 dilution) was added to cover the sections, which were then incubated for 40 min at room temperature. After three washes with PBS, 50 µL of DAPI staining fluid (1:5000 dilutions) was added to cover the sections, which were then kept at room temperature for 5 min. After five times washes with PBS for 3 min each, the HKC cells were sealed by adding 20 µL of liquid seal, and then observed by confocal laser scanning microscopy.
Results
Characterization of mAb H5-32
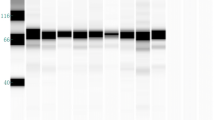
Monoclonal antibody H5-32 was obtained by immunizing mice with H5N1 avian influenza virus using traditional hybridoma cell technique (Zhang 2012). The light chain and heavy chain of monoclonal antibody H5-32 were identified as type λ and IgM, respectively. ELISA assay showed no cross reactivity with other pathogenic microorganisms such as influenza A virus H1N1 (Table 1). Western blotting analysis confirmed a specific reaction between mAb H5-32 and H5N1 antigen, with a binding fragment size of about 60 kDa, as shown in Fig. 1.
Western blotting assay of mAb H5-32. The image on the left shows the specificity of mAb H5-32 reaction with the H5N1 virus lysate, with the binding fragment size of about 60 kDa. The image on the right shows the cross-reactivity of mAb H5-32 with HKC cells, with a binding fragment size of about 43 kDa
Immunohistochemical results of mAb H5-32 and human tissues
Immunohistochemical results showed that mAb H5-32 was bound to kidney tissue in 33 kinds of human tissue microarray, as shown in Fig. 2a. Moreover, identified by the microarray containing 21 different human kidneys tissue, we found that mAb H5-32 can bind to human renal tubules to varying degrees (Fig. 2b).
Cross-reactivity of mAb H5-32 with human kidney tissue. a Immunohistochemistry results of mAb H5-32 reactions with human tissue microarray. b Results of mAb H5-32 reactions with the microarray containing 21 different normal human kidney tissues. TMAs: tissue microarrays. Relative quantification 0: negative; 1: weakly positive; 2: moderately positive; 3: strongly positive. The results show that mAb H5-32 binding with the human kidney tissue to varying degrees. c Immunohistochemical staining of the renal tissues samples (400×). From the staining pattern, the mAb H5-32 was stained around the renal tubules. The sections were counterstained with hematoxylin (mAb H7N9-58 used as a negative control)
Cross-reactivity of mAb H5-32 with renal tubular epithelial cells
According to the immunohistochemical and immunofluorescent staining results, we found that mAb H5-32 cross-reaction with HKC cells, as shown in Fig. 3a, b. The cytoplasm is stained red by Cy3 antibodies and the nucleus is stained blue by DAPI. Scanning with confocal laser scanning microscopy revealed that mAb H5-32 non-specifically cross-reacted with the cytoplasm of HKC cells, as shown in Fig. 3c.
Cross-reactivity of mAb H5-32 with HKC cells. a Immunohistochemistry results of mAb H5-32 reaction with HKC cells (400×). The image on the left shows HKC cells were dyed brown and the image on the right shows PBS used as a negative staining control. b Immunofluorescence results of mAb H5-32 reaction with HKC cell (400×). Cy3: HKC cells stained red; DAPI: nuclei stained blue; Merge: composite image. c Confocal laser scanning microscopy results of mAb H5-32 reactions with HKC cells (400×). Cy3 stained red HKC cells (left), DAPI stained blue nuclei (middle), and composite images (right)
Western blotting of mAb H5-32 with HKC cells
Western blotting assay was performed after HKC cells were lysed with RIPA buffer solution, and the results showed that mAb H5-32 cross-reacted with HKC cells, with the size of binding fragment about 43 kDa. This is significantly different from the 60 kDa fragment size of mAb H5-32 binding to the H5N1 antigen, as shown in Fig. 1.
Discussion
Currently, humans have little immunity to avian influenza strains, and highly pathogenic avian influenza H5N1 remains a persistent threat to the public. Given the potential for H5N1 virus to trigger a pandemic (Herfst et al. 2012; Imai et al. 2012), there is an urgent need to develop new therapeutic interventions to control potential outbreaks. Prevention and treatment strategies for influenza mainly include the use of vaccines and antiviral drugs, but the fact of the influenza epidemic proves that vaccine effectiveness is highly variable and vaccines need to be often changed to keep pace with persistent mutations in the influenza virus genome. In addition, antiviral resistance has been reported in many pandemic strains, including the 2013 H7N9 influenza virus (Itoh et al. 2015; Chen et al. 2013). Influenza viruses can target and hijack multiple host cell pathways to facilitate their survival and replication, thereby affecting viral infection, immune response, and pathology (Vlahos et al. 2011; Yatmaz et al. 2013). Although influenza virus infection has been well studied in animal models (Cameron et al. 2008; Muramoto et al. 2014), human cytological research has lagged due to the lack of available human anatomical materials, especially from patients infected with highly pathogenic AIV.
The mAb H5-32 prepared in our laboratory was of IgM subtype and Western blotting assay showed specific binding bands of the mAb H5-32 and H5N1 virus around 60 kDa. Meanwhile, mAb H5-32 cross-reacted with the microarray containing 21 different human renal tissues, with individual differences in the degree of binding. Immunohistochemical and immunofluorescence tests consistently revealed cross-reactivity between mAb H5-32 and HKC, and confocal laser scanning microscopy revealed that the binding reaction was located in the cytoplasm. Western blotting showed that mAb H5-32 cross-reacted with HKC cells and the binding fragment size was 43 kDa. The results show that mAb H5-32 binds to both H5N1 AIV and HKC cells, which may provide therapeutic targets for antiviral drugs.
As pathogenic microorganisms, viruses can stimulate the production of antibodies in the body, and antibodies against the virus may also react with cells of the host itself. Monsalvo et al. (2011) found cross-reactive antibodies in sera of patients with 2009 H1N1 influenza and suggested that cross-reactive antibodies were associated with immune complex mediated disease after influenza A infection. Our results suggest that severe disease caused by H5N1 influenza viruses may be due to influenza viruses having similar or identical antigenic epitopes as those found in human cells. After influenza virus infects the human body, immune cross-recognition activates the immune system of the infected person, causing excessive reactions, leading to cytokine storm or complement abnormalities, resulting in tissue and organ damage and death.
In brief, this study found that the mAb H5-32 against H5N1 AIV can bind to human kidney tissue, especially in the cytoplasm of renal tubular epithelial cells. This finding suggests that there may be antigenic epitope similarities between influenza viruses H5N1 and HKC cells that hijack the patient's own immune system and cause tissue damage. This may be one of the possible pathogenic mechanisms of AIV, and may also provide experimental basis for the prevention and control of H5N1 AIV and related vaccine research. Subsequent studies using co-immunoprecipitation and mass spectrometry to identify specific proteins that react with H5N1 AIV monoclonal antibodies will be very necessary and meaningful.
Data availability
The data and material used to support the findings of this study are available from the corresponding author upon request.
References
Abubakar A, Malik M, Pebody RG, Elkholy AA, Khan W, Bellos A et al (2016) Burden of acute respiratory disease of epidemic and pandemic potential in the WHO Eastern Mediterranean Region: a literature review. East Mediterr Health J 22(7):513–526
Adlhoch C, Fusaro A, Gonzales JL, et al. European Food Safety Authority; European Centre for Disease Prevention and Control; European Union Reference Laboratory for Avian Influenza; Avian influenza overview December 2022–March 2023. EFSA J. 2023; 21(3):e07917.
Cameron CM, Cameron MJ, Bermejo-Martin JF et al (2008) Gene expression analysis of host innate immune responses during Lethal H5N1 infection in ferrets. J Virol 82:11308–11317
Chen Y, Liang W, Yang S et al (2013) Human infections with the emerging avian influenza A H7N9 virus from wet market poultry: clinical analysis and characterisation of viral genome. Lancet 381:1916–1925
Gao R, Dong L, Dong J, Wen L, Zhang Y, Yu H et al (2010) A systematic molecular pathology study of a laboratory confirmed H5N1 human case. PLoS ONE 5(10):e13315
Gu J, Xie Z, Gao Z, Liu J, Korteweg C, Ye J et al (2007) H5N1 infection of the respiratory tract and beyond: a molecular pathology study. Lancet 370(9593):1137–1145
Herfst S, Schrauwen EJ, Linster M et al (2012) Airborne transmission of influenza A/H5N1 virus between ferrets. Science 336:1534–1541
Imai M, Watanabe T, Hatta M et al (2012) Experimental adaptation of an influenza H5 HA confers respiratory droplet transmission to a reassortant H5 HA/H1N1 virus in ferrets. Nature 486:420–428
Itoh Y, Shichinohe S, Nakayama M et al (2015) Emergence of H7N9 influenza A virus resistant to neuraminidase inhibitors in nonhuman primates. Antimicrob Agents Chemother 59:4962–4973
Kniss K, Sumner KM, Tastad KJ, Lewis NM, Jansen L, Julian D, et al. Risk for infection in humans after exposure to birds infected with highly pathogenic avian influenza A(H5N1) virus, United States, 2022. Emerg Infect Dis. 2023. https://doi.org/10.3201/eid2906.230103.
Li JL, Zhang HX, Feng YM, et al. Identification on biological characteristics of AIV H5N1 monoclonal antibody. Chin J Immunol. 2017;33(3):398–400, 406.
Monsalvo AC, Batalle JP, Lopez MF et al (2011) Severe pandemic 2009 H1N1 influenza disease due to pathogenic immune complexes. Nat Med 17:195–199
Muramoto Y, Shoemaker JE, Le MQ et al (2014) Disease severity is associated with differential gene expression at the early and late phases of infection in nonhuman primates infected with different H5N1 highly pathogenic avian influenza viruses. J Virol 88:8981–8997
Sangsiriwut K, Noisumdaeng P, Uiprasertkul M, Prasertsopon J, Payungporn S, Auewarakul P et al (2021) Full genomic sequences of H5N1 highly pathogenic avian influenza virus in human autopsy specimens reveal genetic variability and adaptive changes for growth in MDCK Cell cultures. Biomed Res Int 22(2021):3890681
Vlahos R, Stambas J, Bozinovski S et al (2011) Inhibition of Nox2 oxidase activity ameliorates influenza A virus-induced lung inflammation. PLoS Pathog 7:e1001271
Walls HH, Harmon MW, Slagle JJ et al (1986) Characterization and evaluation of monoclonal antibodies developed for typing influenza A and influenza B viruses. J Clin Microbial 23(2):240–245
Yatmaz S, Seow HJ, Gualano RC et al (2013) Glutathione peroxidase-1 reduces influenza A virus-induced lung inflammation. Am J Respir Cell Mol Biol 48:17–26
Yu J, Kane S, Wu J et al (2009) Mutation-specific antibodies for the detection of EGFR mutations in non-small-cell lung cancer. Clin Cancer Res 15:3023–3028
Zhang C (2012) Hybridoma technology for the generation of monoclonal antibodies. Methods Mol Biol 901:117–135
Zhang L, Liu K, Su Q, Chen X, Wang X, Li Q et al (2022) Clinical features of the first critical case of acute encephalitis caused by the avian influenza A (H5N6) virus. Emerg Microbes Infect 11(1):2437–2446
Zhao N, Wang S, Wang L, Shi Y, Jiang Y, Tseng TJ et al (2023) Epidemiological features and trends in the mortality rates of 10 notifiable respiratory infectious diseases in China from 2004 to 2020: Based on national surveillance. Front Public Health 17(11):1102747
Acknowledgements
We gratefully acknowledge to Shaanxi Engineering Research Center of Cell Immunology for their generous assistance, as well as to Liting Yan and Xiaoyan Huang for their invaluable cooperation of in the research process.
Funding
This study was supported by the Natural Science Basic Research Program of Shaanxi (Grant No. 2023-JC-QN-0844) and the Key Research and Development Project of Shaanxi (Grant No. 2021ZDLSF01-03).
Author information
Authors and Affiliations
Contributions
HX Zhang, NN Wang and J Hu designed the experiments. HX Zhang, JY Sun, YM Feng, JL Li, NN Wang, XR Zhao and Y Li conducted the experiments. LJ Sun and CX Xu analyzed the data. HX Zhang, JY Sun and NN Wang wrote the paper. All authors approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Communicated by Ran Wang.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, H., Sun, J., Feng, Y. et al. A murine monoclonal antibody against H5N1 avian influenza virus cross-reacts with human kidney cortex cells. Arch Microbiol 205, 373 (2023). https://doi.org/10.1007/s00203-023-03693-8
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00203-023-03693-8