Abstract
Summary
This study evaluated bone features of PHPT using HR-pQCT. The results showed both cortical and trabecular bones were significantly impaired in PHPT patients. Male and female PHPT patients suffered similar damages in bone. HR-pQCT indices were not observed to differ in MEN1 and sporadic PHPT patients.
Introduction
High-resolution peripheral quantitative CT is a novel imaging technique used to separately assess trabecular and cortical bone status of the radius and tibia in vivo. Using HR-pQCT, we aimed to evaluate bone features of primary hyperparathyroidism patients in a Chinese population and reveal similarities and differences in bone features in multiple endocrine neoplasia type 1–related PHPT and sporadic PHPT patients in the Chinese population.
Methods
A case-control study was designed. In 58 PHPT patients and 58 sex- and age-matched healthy controls, the distal radius and tibia were scanned using HR-pQCT. Areal bone mineral density (aBMD) was also determined in PHPT patients using dual-energy X-ray absorptiometry (DXA).
Results
In comparison with controls, PHPT patients were observed to exhibit reduced volumetric BMD at the cortical and trabecular compartments, thinner cortices, and more widely spaced trabeculae. Significant differences were still observed when comparing data of female and male patients with age-matched controls separately. MHPT patients (n = 11) were found to have lower aBMD Z-scores in the lumbar spine, trochanteric region, and total hip compared with sporadic PHPT patients (n = 47), while no differences were observed in HR-pQCT indices between the two groups. In multiple linear regression models, no significant correlations were identified between PTH and HR-pQCT indices. However, height was found to positively correlate with HR-pQCT-derived trabecular indices at both the radius and tibia.
Conclusions
PHPT affects geometry, volumetric density, and microstructure in both the cortical and trabecular bones in both male and female Chinese patients. MHPT patients were observed to have reduced aBMD as determined by DXA in the lumbar spine and hip in comparison with sporadic PHPT patients. However, HR-pQCT indices were not observed to differ.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Primary hyperparathyroidism (PHPT) is a common endocrine disorder that is characterized by hypercalcemia combined with inappropriate elevated serum parathyroid hormone (PTH) levels. Bone is considered to be one of the most common target organs that is damaged by chronic, persistent excess PTH. PHPT patients have been classically considered to experience preferential bone loss in the cortical bone with a relative preservation of the trabecular bone. This observation has always been interpreted as anabolic effects of PTH on the trabecular bone and catabolic effects on the cortical bone, as demonstrated using DXA [1,2,3,4] and histomorphometry [5,6,7]. However, these results do not explain the increased risk of fracture at vertebral sites (vertebrae, approximately 3-fold), which are enriched in the trabecular bone, as well as nonvertebral sites (forearm, approximately 2-fold) PHPT in patients [8]. High-resolution peripheral computed tomography (HR-pQCT) represents a novel approach for the non-invasive assessment of both cortical and trabecular bone regarding bone geometry, volumetric density, and microarchitecture at the distal radius and tibia. Previous studies [9,10,11] using HR-pQCT have demonstrated that not only the cortical but also the trabecular bone were adversely affected by excess PTH. Currently, two studies using HR-pQCT have reported improvements in both the cortical and trabecular bone following parathyroidectomy [11, 12]. However, current HR-pQCT data regarding PHPT are limited to Caucasian females. Because bone involvement was observed to be more common and more severe in Chinese PHPT patients compared with that in Caucasians [13], and bone microstructural differences were observed in Chinese American women versus Caucasian women in HR-pQCT studies [14, 15], HR-pQCT data from Chinese patients with PHPT are needed. In addition, HR-pQCT data of male PHPT patients are also required.
Multiple endocrine neoplasia type 1 (MEN1) is an autosomal dominant syndrome that is characterized by the occurrence of multifocal neoplasias in two or more endocrine organs, and accounts for approximately 70% of hereditary PHPT cases [16]. Skeletal manifestations of MEN1-related PHPT (MHPT) are not exactly identical to those of sporadic PHPT. This is perhaps due to different clinical characteristics, including earlier disease onset, milder biochemical presentation, and an increased frequency of multiglandular parathyroid hyperplasia instead of parathyroid adenoma [17]. However, the involvement of other endocrine organs which also affect bone metabolism in MEN1 results in an increased complexity of skeletal manifestations in MHPT. Data regarding skeletal manifestations of MHPT were primarily based on aBMD measured using DXA, which produced inconsistent results [17,18,19,20]. In these studies, lower or similar BMD values of lumbar spine (LS) and femoral neck (FN) were observed in MHPT patients compared with sporadic PHPT patients [17,18,19]. Comparative data regarding bone features as assessed by HR-pQCT between MHPT and sporadic PHPT patients remain to be carried out.
In the present study, we evaluated bone geometry, volumetric density, and microarchitecture using the second-generation HR-pQCT in both female and male PHPT patients in order to generate data regarding bone features of PHPT in the Chinese population. In addition, we compared bone structural indices between MHPT and sporadic PHPT patients in order to identify similarities and differences of bone effects in these two different disease conditions. In addition, correlations between clinical data and HR-pQCT indices were evaluated in order to understand the effect of clinical characteristics on bone parameters.
Subjects and methods
Subjects and clinical investigation
A case-control study was designed. One hundred and eight consecutive patients with PHPT were referred to the Department of Endocrinology of Peking Union Medical College Hospital (PUMCH) from November 2016 to August 2017. Ninety-two patients underwent parathyroidectomy. Patients that had used bisphosphonates, glucocorticoids, or other drugs known to influence bone metabolism, and had a history of prior parathyroidectomy were excluded from this study. Based on the foregoing criteria, 17 patients were excluded: 14 cases for reasons of using medications (bisphosphonates, 13; corticosteroids, 1) and 3 cases for having a history of prior parathyroidectomy. The remaining 75 patients were invited, of whom 58 agreed to participate in the study. Thus, the final study consisted of 58 PHPT patients. Clinical data, including age, gender, weight, height, course of disease, clinical manifestations, and biochemical indices, were obtained from medical chart reviews. In our cohort, MEN1 was routinely screened in PHPT patients and clinically diagnosed if the presence of two or more major MEN1-associated endocrine tumors was confirmed and the MEN1 mutation was detected. Sporadic PHPT was defined as cases presenting with isolated PHPT and a lack of family history. Asymptomatic PHPT is defined as hyperparathyroidism in the absence of specific symptoms or signs that results from hypercalcemia or PTH excess.
The 58 controls used in this study were selected from the healthy database of HR-pQCT in our center, which came from a population-based study of HR-pQCT in the mainland Chinese population (641 normal individuals recruited from communities in Beijing between the year of 2015 and 2017). Healthy controls were matched for sex and age, with an age span of 10 years, and possessed no history of PHPT or fragility fractures. Biochemical markers, including liver and renal functions, serum calcium, phosphorus, alkaline phosphatase, and PTH levels were determined to be within normal ranges in control subjects. All control subjects included were free of other diseases or drugs known to influence bone metabolism. The present study was approved by the Ethics Committee of Peking Union Medical College Hospital. Written informed content was obtained from all subjects, and this study was carried out according to the principles defined in the Declaration of Helsinki.
Biochemical measurements
Blood samples were drawn in a fasting state. Biochemical tests were performed within 1 week of DXA and HR-pQCT scan. Serum calcium, serum ionized calcium, serum phosphate, alkaline phosphatase (ALP), 25-hydroxyvitamin D (25OHD), parathyroid hormone (PTH), and β-C-terminal telopeptide region of collagen type 1 (β-CTX) were all tested in the Department of Clinical Laboratory of Peking Union Medical College Hospital by standard methods.
Dual-energy X-ray absorptiometry
BMD was determined using DXA (GE-Lunar, USA) at the lumbar spine (L1–L4) and right hip (femoral neck, trochanteric region, and total hip) in all PHPT patients in this study. The coefficient of variations (CV) of measurements was 0.9% for lumbar spine, 1.6% for femoral neck, and 0.7% for total hip. Z-scores (age- and sex-matched comparison in SD units) and T-scores (comparison from the mean BMD value in a healthy young reference population, in SD units) of BMD were calculated using the normal reference database from our center [21]. According to the International Society for Clinic Densitometry (ISCD) criteria, T-scores lower than − 2.5 at any site indicate osteoporosis, and Z-scores lower than − 2.0 were defined as reduced BMD.
High-resolution peripheral quantitative computed tomography
The nondominant distal radius and tibia were measured using the second-generation HR-pQCT system (Xtreme CT II, Scanco Medical AG, Brüttisellen, Switzerland). At each site, 3-dimensional (3D) bone images of 10.2 mm in the axial direction were obtained, with a voxel size of 61 μm. An anteroposterior scout view was utilized to define the measurement region. The reference line was manually placed at the endplate of the radius and tibia. A stack of 168 parallel CT slices was obtained, with the first CT slice 9 mm and 22 mm proximal to the reference line for the radius and tibia, respectively. X-ray photon attenuation data were then converted to equivalent hydroxyapatite (HA) densities. An automated threshold-based algorithm was used to separate the cortical and trabecular compartments. Images were manually graded for motion artifacts on a scale of 1 (no motion artifact) to 5 (extreme motion artifact). No images had a grade of 4 or 5; thus, all images were included [22].
The parameters were as follows: indices of bone geometry included total bone area (Tt.Ar), trabecular area (Tb.Ar), cortical area (Ct.Ar), and cortical perimeter (Ct.Pm). Indices of volumetric density included total volumetric BMD (Tt.vBMD), trabecular volumetric BMD (Tb.vBMD), and cortical volumetric BMD (Ct.vBMD). Indices of bone microarchitecture included trabecular bone volume fraction (BV/TV), trabecular number (Tb.N), trabecular thickness (Tb.Th), trabecular separation (Tb.Sp), cortical thickness (Ct.Th), and cortical porosity (Ct.Po).
Statistical analysis
All statistics were carried out using SPSS software version 17.0 (SPSS, Chicago, USA). Continuous variables, including normally distributed variables and non-normally distributed variables, are presented as the mean ± standard deviation (SD) and median (range), respectively. Between-group differences were analyzed using independent-samples t tests for normally distributed variables, while the Mann-Whitney U test was carried out in the case of non-normally distributed variables. Categorical variables were presented as percentages and were compared using the Pearson χ2 test or Fisher exact test, as appropriate. Covariance analysis was used for age adjustment. Spearman correlation test and multiple linear regression analysis were used to examine the correlations between the clinical data and the HR-pQCT indices. In the case of all analyses, p values < 0.05 were considered to be statistically significant.
Results
Demographic, clinical, and biochemical characteristics
The 58 patients with PHPT (41 females and 17 males) were included, with a mean age of 49.9 ± 15.1 years. There were 26 postmenopausal women in both the PHPT group and the control group. In the PHPT group, the median course of disease was 3.0 (0.08,34) years; 5 cases suffered fragility fractures with a incidence of 8.6% (5/58). Serum calcium and PTH levels in the PHPT group were 2.80 ± 0.28 mmol/L (normal range 2.13–2.70 mmol/L) and 171.6 (39.0, 1891.5) pg/mL (normal range13–65 pg/mL), respectively. The average serum 25OHD level was 13.58 ± 6.45 ng/mL, and 90% (52/58) of cases had vitamin D deficiency (25OHD below 20 ng/mL).
Among the 58 patients included in this study, 11 cases were clinically and genetically diagnosed as MEN-1, 9 of them were probands. All of the MEN1 patients were found to present with PHPT. Among these patients, there were a total of eight with pancreatic neuroendocrine tumors, four with prolactinoma, and three with non-functional pituitary adenoma.
Comparisons of clinical characteristics and bone indices between PHPT patients and healthy controls
As depicted in Table 1, PHPT patients were observed to be comparable with healthy controls in respect to age, sex, weight, height, and body mass index (BMI). In regard to the indices assessed using HR-pQCT, for the geometry, PHPT patients had reduced Ct.Ar (p < 0.001) in the radius and increased Tb.Ar (p = 0.021) in the tibia compared with controls. For the vBMD measurements, reduced Tt.vBMD, Tb.vBMD, and Ct.vBMD (all p < 0.001) were found in both the radius and tibia in PHPT patients. For the trabecular microarchitecture, PHPT patients had reduced BV/TV, Tb.N and increased Tb.SP (all p < 0.001) in both radius and tibia. For the cortical microarchitecture, Ct.Th was lower in both radius and tibia in PHPT patients compared with controls (p < 0.001 and p = 0.009, respectively), whereas Ct.Po was similar between the two groups. Representative 3D images of the distal radius and tibia in PHPT patients in comparison with control subject are shown in Fig. 1.
In an effort to provide further data regarding skeletal features of male patients, we compared male patients with age-matched healthy controls. Considering the effect of menopausal status on bone, we also separately compared premenopausal female patients and postmenopausal female patients with age and menopausal status–matched controls. These results are depicted in Supplement Table 1, 2 and 3. Bone indices in male and premenopausal/postmenopausal female patients showed approximately similar abnormalities as in the general population. The percentage comparisons of HR-pQCT results in the male and the whole female group relative to age-matched controls were depicted in Fig. 2.
Percentage comparisons of HR-pQCT indices in male and female group relative to controls in radius (a) and tibia (b). *Represents significant differences between cases and controls (p < 0.05). #Represents significant differences for comparisons of the percentage difference between male and female (p < 0.05). Tt.Ar, total bone area; Tb.Ar, trabecular area; Ct.Ar, cortical area; Ct.Pm, cortical perimeter; Tt.vBMD, total bone volumetric BMD; Tb.vBMD, trabecular volumetric BMD; Ct.vBMD, cortical volumetric BMD; BV/TV, trabecular bone volume fraction; Tb.N, trabecular number; Tb.Th, trabecular thickness; Tb.Sp, trabecular separation; Ct.Th, cortical thickness; Ct.Po, cortical porosity
Comparisons of clinical characteristics, biochemical indices, aBMD, and bone indices between MHPT and sporadic PHPT patients
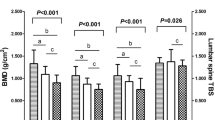
As shown in Table 2, MEN-1 patients were found to be younger than sporadic PHPT patients (p = 0.005). No differences were observed in sex, height, weight, BMI, course of disease, biochemical indices, or incidence of asymptomatic PHPT between these two groups. As depicted in Table 2, BMD Z-scores of the trochanteric region, the total hip, and the lumbar spine were found to be significantly lower in MHPT patients compared with those in sporadic PHPT patients (p = 0.047, p = 0.042, and p = 0.042, respectively). In regard to the HR-pQCT parameters, no significant differences of indices of bone geometry, vBMD, and microarchitecture were observed between the two groups following adjustment by age (Supplement Table 4).
Correlations between clinical characteristics and HR-pQCT indices in sporadic PHPT patients
The results from the Spearman correlation analysis is shown in Supplement Table 5. Age and sex were found to correlate with the majority of the HR-pQCT indices. PTH levels were found to positively correlate with Ct.Ar at the radius and Ct.Th at the tibia (r = 0.275 and r = 0.290, respectively, p < 0.05). No significant correlations were observed between BMI or serum 25(OH)D level and HR-pQCT indices.
Multiple linear regression analyses were carried out in order to further study these correlations in sporadic PHPT patients (n = 47). The results are depicted in Table 3. Aging was found to negatively correlate with Tb.vBMD, BV/TV in the radius and Tt.vBMD, and BV/TV in the tibia. Height was observed to be a positive predictor for Tb.vBMD, BV/TV, Tb.N, Tt.Ar, and Tb.Ar and a negative predictor for Tb.Sp at the both the radius and tibia. Male gender was determined to be a positive predictor for Ct.Ar at both the radius and tibia. The course of the disease was found to only positively correlate with Tb.Sp and to negatively correlate with Tb.N at the radius. No significant correlations were observed between PTH levels and HR-pQCT indices in these models. When multiple linear regression analyses were examined in female sporadic PHPT patients (n = 33, Supplement Table 6), only height and course of disease were found to have significant correlations with some HR-pQCT indices. No significant correlations were observed between PTH levels or menopause status and HR-pQCT indices in the models studied here.
Discussion
HR-pQCT is as an advanced bone imaging technique that provides an in vivo assessment of bone features of both cortical and trabecular bones, separately. In this study, we utilized HR-pQCT to study skeletal effects of PHPT in the Chinese population, and the effect of gender differences on bone features was first studied in PHPT patients using HR-pQCT. In addition, to our knowledge, this represents the first pilot study carried out to compare bone features between MHPT and sporadic PHPT patients using HR-pQCT.
In the current study, structural indices demonstrated that both cortical and trabecular bones were significantly impaired in PHPT patients, with reduced volumetric BMD observed at the cortical and trabecular compartments, thinner cortices, and more widely spaced trabeculae. The results also demonstrated that the radius and tibia were almost equally damaged in PHPT patients. However, the previous two studies that assessed the bone involvement in female PHPT patients using HR-pQCT showed greater abnormalities in the radius compared with the tibia [9, 10]. In addition to a limited sample size, site-specific differences in mechanical loading have been considered to represent one of the factors involved in the difference between the radius and tibia [9]. Mechanical stimuli is a promoting factor for PTH-mediated bone formation [23, 24]. Therefore, the radius, a non-weight-bearing site, is generally found to be adversely affected more than the tibia, a weight-bearing site [9, 10]. Nevertheless, this difference observed between the radius and tibia was not observed in our findings. Due to the prevalence of lower BMI, less exercise, and a more severe PHPT phenotype in the Chinese population compared with the Caucasian population, the protection of mechanical loading in the tibia in the Chinese population could be less obvious compared with the Caucasian population [15]. Our study also identified a significant increase in Tb.Ar along with an insignificantly reduction in Tt.Ar and Ct.Ar at the tibia in PHPT patients, which has been considered to be a reflection of endocortical resorption (trabecularization) [9, 11]. In contrast to significantly reduced cortical vBMD, we did not observe a significant increase in Ct.Po in PHPT patients, similarly with the results in previous study [9, 10]. The inability to demonstrate difference in Ct.Po could be due to an inferior resolution of HR-pQCT to capture Ct.Po and a lack of power given the relatively small sample size.
When analyzing male and female data separately, we observed significant abnormalities in both cortical and trabecular indices in both groups. These results indicated that male and female PHPT patients suffered similar damages in bone features, with even the majority of the variations of these indices observed to be similar between male and female patients. Numerous previous studies demonstrated that male patients with PHPT were more commonly asymptomatic [25, 26]. In regard to bone involvement, the majority of aBMD studies demonstrated that osteoporosis was less common in male patients [25,26,27,28], despite one study that showed male patients presenting with higher serum calcium and PTH levels in comparison with female patients [25]. The differences observed between our results and previous studies could be related to racial differences, disease severity, and different evaluation technologies. Nevertheless, the limited sample size (17 males) should also be taken into consideration.
In the present study, the aBMD Z-scores of lumbar spine, trochanteric region, and total hip in MHPT patients were found to be significantly lower than in sporadic PHPT patients. The results are consistent with that from previous studies that have shown severe trabecular bone mineral loss in MEN1 [17,18,19,20]. Numerous previous studies have demonstrated that there is no correlation between PTH and BMD in MEN1 patients [17, 19], in contrast to the inverse correlation observed in sporadic PHPT patients [17]. Therefore, increased severity of bone loss in MHPT patients could be partially attributed to the combination of other endocrine dysfunction components, including hyperprolactinemia, hypercortisolism, hypogonadism, and GH deficiency, which also exert negative effects on bone mineralization, especially in the case of trabecular bone [28]. In addition, MHPT often presents with an earlier onset age, typically two to three decades earlier than sporadic PHPT. This earlier onset could interfere with the normal formation of peak bone mass [20]. In the present study, we provided for the first time comparative data regarding bone features as assessed using HR-pQCT between MHPT and sporadic PHPT. While significantly lower aBMD levels were observed in MHPT patients, no between-group differences were observed in bone indices as measured using HR-pQCT. The site-to-site differences in bone features at different anatomical regions could partly lead to the different results obtained by DXA and HR-pQCT measurements. Considering the limited sample size of our study, a larger sample size may yield significant differences in the HR-pQCT indices between groups.
In the current study, we observed no significant correlations between PTH and HR-pQCT indices using the multiple linear regression models. Height was found to be an obvious positive predictor for HR-pQCT-derived trabecular indices at both the radius and the tibia. Since taller person had more distally positioned fixed region of interest (ROI) than shorter person when scanning, and more distally, the bone was assembled with larger cross-sectional area and larger medullary void volume containing more trabecular bone [29]; therefore, the positive correlations between height and trabecular indices may be partly due to the result of the positioning of the ROI. Because of the limited sample size in our current study, the effect of clinical characteristics on bone features must be evaluated using a larger sample-sized study.
We note that our study also possessed some limitations. First, because the HR-pQCT technique was not been developed in our center until recently, the sample size included in the present study was limited. A large-scale study will be required in the future. Second, DXA measurements were not carried out at the forearm in all of the subjects used in this study. Therefore, we could not simultaneously analyze aBMD and vBMD data at the same skeletal site. Third, the aBMD data were absent in healthy controls. Therefore, we were unable to compare aBMD between PHPT patients and controls in this study. Instead, Z-scores of aBMD were calculated in order to evaluate the status of bone mass loss. Finally, microstructural finite-element analysis (μFEA) was not carried out as a mechanism to estimate bone stiffness and strength in this study. Further studies to evaluate biomechanical characteristics using μFEA are needed.
In conclusion, in the present study, we demonstrated that PHPT affects bone geometry, volumetric BMD, and microarchitecture in both the cortical and trabecular bone in the Chinese population. Both female and male PHPT patients exhibited impaired bone structures, and seemed to have similar variations of HR-pQCT indices. MHPT patients exhibited reduced aBMD as assessed using DXA in the lumbar spine and hip. However, similar indices were assessed using HR-pQCT in both the radius and tibia when compared with sporadic PHPT patients.
References
Chen Q, Kaji H, Iu MF et al (2003) Effects of an excess and a deficiency of endogenous parathyroid hormone on volumetric bone mineral density and bone geometry determined by peripheral quantitative computed tomography in female subjects. J Clin Endocrinol Metab 88(10):4655–4658
Silva BC, Costa AG, Cusano NE, Kousteni S, Bilezikian JP (2011) Catabolic and anabolic actions of parathyroid hormone on the skeleton. J Endocrinol Investig 34(10):801–810
Dempster DW, Muller R, Zhou H et al (2007) Preserved three-dimensional cancellous bone structure in mild primary hyperparathyroidism. Bone 41(1):19–24
Minisola S, Rosso R, Romagnoli E et al (2002) Uneven deficits in vertebral bone density in postmenopausal patients with primary hyperparathyroidism as evaluated by posterior-anterior and lateral dual-energy absorptiometry. Osteoporos Int 13(8):618–623
Parisien M, Silverberg SJ, Shane E et al (1990) The histomorphometry of bone in primary hyperparathyroidism: preservation of cancellous bone structure. J Clin Endocrinol Metab 70(4):930–938
Christiansen P, Steiniche T, Brockstedt H, Mosekilde L, Hessov I, Melsen F (1993) Primary hyperparathyroidism: iliac crest cortical thickness, structure, and remodeling evaluated by histomorphometric methods. Bone 14(5):755–762
Uchiyama T, Tanizawa T, Ito A, Endo N, Takahashi HE (1999) Microstructure of the trabecula and cortex of iliac bone in primary hyperparathyroidism patients determined using histomorphometry and node-strut analysis. J Bone Miner Metab 17(4):283–288
Khosla S, Melton LR, Wermers RA, Crowson CS, O’Fallon W, Riggs B (1999) Primary hyperparathyroidism and the risk of fracture: a population-based study. J Bone Miner Res 14(10):1700–1707
Hansen S, Beck JJ, Rasmussen L, Hauge EM, Brixen K (2010) Effects on bone geometry, density, and microarchitecture in the distal radius but not the tibia in women with primary hyperparathyroidism: a case-control study using HR-pQCT. J Bone Miner Res 25(9):1941–1947
Stein EM, Silva BC, Boutroy S et al (2013) Primary hyperparathyroidism is associated with abnormal cortical and trabecular microstructure and reduced bone stiffness in postmenopausal women. J Bone Miner Res 28(5):1029–1040
Vu TD, Wang XF, Wang Q et al (2013) New insights into the effects of primary hyperparathyroidism on the cortical and trabecular compartments of bone. Bone 55(1):57–63
Hansen S, Hauge EM, Rasmussen L, Jensen JE, Brixen K (2012) Parathyroidectomy improves bone geometry and microarchitecture in female patients with primary hyperparathyroidism: a one-year prospective controlled study using high-resolution peripheral quantitative computed tomography. J Bone Miner Res 27(5):1150–1158
Bilezikian JP, Meng X, Shi Y, Silverberg SJ (2000) Primary hyperparathyroidism in women: a tale of two cities—New York and Beijing. Int J Fertil Womens Med 45(2):158–165
Boutroy S, Walker MD, Liu XS et al (2014) Lower cortical porosity and higher tissue mineral density in Chinese American versus white women. J Bone Miner Res 29(3):551–561
Walker MD, Liu XS, Stein E et al (2011) Differences in bone microarchitecture between postmenopausal Chinese-American and white women. J Bone Miner Res 26(7):1392–1398
Thakker RV et al (2012) Clinical practice guidelines for multiple endocrine neoplasia type 1 (MEN1). J Clin Endocrinol Metab 97(9):2990–3011
Thakker RV, Newey PJ, Walls GV et al (2009) Sporadic and MEN1-related primary hyperparathyroidism: differences in clinical expression and severity. J Bone Miner Res 24(8):1404–1410
Kong J, Wang O, Nie M et al (2016) Clinical and genetic analysis of multiple endocrine neoplasia type 1-related primary hyperparathyroidism in Chinese. PLoS One 11(11):e0166634
Lourenco DJ, Toledo RA, Mackowiak II et al (2008) Multiple endocrine neoplasia type 1 in Brazil: MEN1 founding mutation, clinical features, and bone mineral density profile. Eur J Endocrinol 159(3):259–274
Lourenco DJ, Coutinho FL, Toledo RA, Montenegro FL, Correia-Deur JE, Toledo SP (2010) Early-onset, progressive, frequent, extensive, and severe bone mineral and renal complications in multiple endocrine neoplasia type 1-associated primary hyperparathyroidism. J Bone Miner Res 25(11):2382–2391
Yu W, Qin MW, Xu L (1996) Bone mineral analysis of 445 normal subjects assessed by dual X-ray absorptiometry. Chin J Rad 30:625–629
Pauchard Y, Liphardt AM, Macdonald HM, Hanley DA, Boyd SK (2012) Quality control for bone quality parameters affected by subject motion in high-resolution peripheral quantitative computed tomography. Bone 50(6):1304–1310
Kim CH, Takai E, Zhou H et al (2003) Trabecular bone response to mechanical and parathyroid hormone stimulation: the role of mechanical microenvironment. J Bone Miner Res 18(12):2116–2125
Hagino H, Okano T, Akhter MP, Enokida M, Teshima R (2001) Effect of parathyroid hormone on cortical bone response to in vivo external loading of the rat tibia. J Bone Miner Metab 19(4):244–250
Mazeh H, Sippel RS, Chen H (2012) The role of gender in primary hyperparathyroidism: same disease, different presentation. Ann Surg Oncol 19(9):2958–2962
Shah VN, Bhadada SK, Bhansali A, Behera A, Mittal BR, Bhavin V (2012) Influence of age and gender on presentation of symptomatic primary hyperparathyroidism. J Postgrad Med 58(2):107–111
De Lucia F, Minisola S, Romagnoli E et al (2013) Effect of gender and geographic location on the expression of primary hyperparathyroidism. J Endocrinol Investig 36(2):123–126
Kann PH, Bartsch D, Langer P et al (2012) Peripheral bone mineral density in correlation to disease-related predisposing conditions in patients with multiple endocrine neoplasia type 1. J Endocrinol Investig 35(6):573–579
Ghasem-Zadeh A, Burghardt A, Wang XF et al (2017) Quantifying sex, race, and age specific differences in bone microstructure requires measurement of anatomically equivalent regions. Bone 101:206–213
Acknowledgments
The authors thank the patients for their participation in the study.
Funding
This work was financially supported by the Chinese Academy of Medical Sciences (CAMS) Initiative for Innovative Medicine (CAMS-I2M) and the National Natural Science Foundation of China (No. 81100559).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
The present study was approved by the Ethics Committee of Peking Union Medical College Hospital. Written informed content was obtained from all subjects, and this study was carried out according to the principles defined in the Declaration of Helsinki.
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 53 kb)
Rights and permissions
About this article
Cite this article
Wang, W., Nie, M., Jiang, Y. et al. Impaired geometry, volumetric density, and microstructure of cortical and trabecular bone assessed by HR-pQCT in both sporadic and MEN1-related primary hyperparathyroidism. Osteoporos Int 31, 165–173 (2020). https://doi.org/10.1007/s00198-019-05186-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-05186-1