Abstract
Summary
We investigated the association between bisphosphonate treatment and the risk of stroke using a large routine clinical dataset. We found no association between bisphosphonate treatment and risk of stroke, after adjusting for large number of clinical and demographic confounders.
Introduction
There is conflicting evidence on the link between bisphosphonates and stroke with studies variously showing increased, decreased or unchanged risk. We investigated the association between bisphosphonate treatment and the risk of stroke using a large routine clinical dataset.
Methods
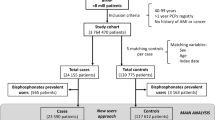
We used a matched nested case-control study design analysing routinely collected electronic data from patients registered at primary care practices in England participating in the Royal College of General Practitioners Research and Surveillance Centre. Cases were patients aged 18 years or over, either living or dead, recorded as having had a stroke in the period 1 January 2005 to 31 March 2016. Each case was matched to one control according to age, sex, general practice attended and calendar time. Data were analysed using Stata, version 14.2. and RStudio, version 1.1.463. Conditional logistic regression was used to determine odds ratios for stroke according to bisphosphonate treatment and duration in cases compared with controls. We adjusted for disease risk groups, cardiovascular risk factors, treatments, smoking status, alcohol consumption, ethnicity, bisphosphonate types, fracture and socioeconomic status using IMD (Index of Multiple Deprivation).
Results
We included 31,414 cases of stroke with an equal number of matched controls. Overall, 83.2% of cases and controls were aged 65 years or older, and there were similar proportions of females (51.5%) and males (48.5%). Bisphosphonate treatment was not associated with stroke after adjusting for the wide range of confounders considered (OR 0.86, 95% CI 0.62–1.19).
Conclusions
We found no association between bisphosphonate treatment and risk of stroke, after adjusting for other confounders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Screening, prevention and treatment of osteoporosis have increased in the UK, mainland Europe and the USA due to various factors including the need to address the increasing burden and costs of fractures, an ageing population at greater risk of fracture, increased awareness of risk factors for fracture and greater availability of screening tests (bone scans) and screening algorithms [1].
According to national guidance in the UK and USA, bisphosphonate drugs (alendronate, pamidronate, risedronate, ibandronate, zoledronic acid) have largely replaced the use of vitamin D with or without supplemental calcium for preventing fragility fractures NICE [2] in those deemed to be at-risk [3, 4], mainly due to lack of evidence of effectiveness of the latter [5, 6]. Bisphosphonates prevent bone loss by slowing down the cells that break down and reabsorb old bone.
There have also been conflicting systematic reviews about the association with cardiovascular disease (CVD) of treatments for osteoporosis. Neither calcium [7] nor vitamin D [8], which have been used for treatment of osteoporosis has been shown to be associated with cardiovascular benefits or adverse effects. Bisphosphonates, on the other hand, have shown conflicting evidence of CVD risk.
Previous observational studies have suggested an increased risk, albeit small, of fatal stroke with bisphosphonates [9], whereas other studies have not found such an association [10] or found a reduction in risk of stroke with these agents [11]. Similar early reviews suggested that some bisphosphonates could be associated with atrial fibrillation, and although this is a heart rhythm disorder which in some cases can trigger stroke, these studies showed no association with stroke [12, 13]. More recent reviews have shown no adverse effect on stroke, no reduction in cardiovascular outcomes overall [14], but a modest increase in risk of atrial fibrillation [15].
We aimed to investigate the association between bisphosphonate treatment and stroke (fatal and non-fatal) using a large routine clinical dataset.
Methods
Study design
We used a matched nested case-control study design to investigate the effect of bisphosphonates on the risk of stroke. We identified cases (patients with stroke) and controls (patients without stroke) and compared these for prescriptions of bisphosphonates and other risk factors for stroke prior to the date of the stroke (or an equivalent date in control patients). Stroke was defined as both ischaemic and haemorrhagic stroke together with transient ischaemic attack or TIA, which is also known as a mini-stroke. TIA is the same as a stroke, except that the symptoms last for a short amount of time and no longer than 24 h. This is because the blockage that stops the blood getting to the brain is temporary.
Key medications including bisphosphonates were defined and grouped using British National Formulary (BNF) chapter (Table 1).
We searched routinely collected electronic records from patients in England registered at primary care practices who are members of the Royal College of General Practitioners (RCGP) Research and Surveillance Centre (RSC) [16]. This is a large computerised, anonymised database representative of and comprising 2.9% of the population of England [17] including demographic information, data on health behaviours, referrals and treatment outcomes, with good clinical information including stroke and stroke deaths. [18] The study observational period was 1 January 2005 to 31 March 2016.
Selection of cases and controls
The study cohort included patients drawn from all RCGP RSC practices over 10 years. Cases were patients aged 18 or over, either living or dead, recorded with standard computer codes for stroke.
Each case of stroke was matched to one control according to age, sex, general practice attended and calendar time. Controls were patients registered at the same practice during the study period identified at the same index date as the corresponding case to account for possible seasonal effects and effects due to the duration of observation for events. Controls were selected at random (and before their exposure status was known to reduce selection bias) from the pool of eligible matched controls for each case using incidence density sampling according to person-time at risk [19]. Controls had to be alive and not transferred out of the practice or dead prior to the index date of their matched case. All cases and controls that had less than 5 years of clinical records before the index date on the dataset were excluded to ensure completeness of recording of exposures and confounding variables. Those with a previous diagnosis of stroke were also excluded. For identified cases, the index date was the date of the first stroke/TIA suffered by the patient. For the control, the index date was the date the patient they are matched to suffered their first stroke within the study period. The case was only stopped if it had deceased during the observational period.
Outcomes, exposures, confounder and effect modifiers
Outcome measures were unadjusted and adjusted odds ratios and 95% confidence intervals for stroke associated with bisphosphonate treatment prior to the index date. Quintiles of the Index of Multiple Deprivation (IMD) were used as it ranks every small area in England from 1 to 32,844 (most deprived area to least deprived area) and Charlson Comorbidity Index (CCI) was used as a proxy for level of risk and frailty [1]. We adjusted for known confounding variables, in particular disease risk groups associated with stroke, cardiovascular risk factors, treatments and other factors (ethnicity, Charlson comorbidity index, Index of Multiple Deprivation (IMD score) recorded with a computer (Read or EMIS) code. Fractures and bisphosphonate types were also included as confounding variables.
Data analysis
Data were analysed using Stata, version 14.2 initially with some work done during the revision period using Rstudio version 1.1.463. Descriptive statistics were given in terms of frequencies for categorical variables and means with standard deviations for continuous variables. We used conditional logistic regressions for matched case-control studies, calculating unadjusted and adjusted odds ratios with 95% confidence intervals for stroke according to bisphosphonate treatment and duration in cases compared with controls. Adjusted analysis accounted for disease risk groups, cardiovascular risk factors, treatments, smoking status, alcohol consumption, fracture types, bisphosphonate types, ethnicity and socioeconomic status using the Index of Multiple Deprivation. All the confounding variables are listed in Tables 2, 3 and 4. Fracture types, hip, osteonecrosis of the jaw (ONJ), vertebral and other fractures were grouped together. Bisphosphonate types were derived from Table 1.
Ethical approval
We obtained ethical approval from Lincolnshire Community Health Services NHS Trust and the University of Lincoln, School of Health and Social Sciences Ethics Committee; the research protocol was approved by RCGP RSC.
Results
Unadjusted analysis
We included 31,414 cases of stroke with an equal number of matched controls (Table 2). Overall, 83.2% in both cases and controls were aged 65 years or older, and there were similar proportions of females and males (51.5% females and 48.5% males).
All the disease risk groups included in the analysis had a negative impact on the risk of stroke, with atrial fibrillation, peripheral arterial disease and hemiplegia being the groups with the highest impact on stroke (unadjusted OR of 2.13, 2.04 and 5.45 respectively; see Table 3). For cardiovascular risk factors (Table 2), being an ex-smoker, never smoker or non-drinker was associated with a reduced risk of stroke (unadjusted OR of 0.86, 0.82 and 0.82 respectively). The remaining cardiovascular risk factors also had a negative impact on the risk of stroke, except high-density lipoprotein (HDL) cholesterol.
In relation to treatments (Table 4), we found that all were associated with a higher risk of stroke, with aspirin, statins and oral anticoagulants having the strongest association (unadjusted odds ratios of 1.79, 1.45 and 1.47, respectively). The unadjusted analysis also showed that a greater number of comorbidities were associated with a higher risk of stroke. Finally, the Index of Multiple Deprivation (IMD score) showed that people living in the most deprived areas had a higher risk of stroke than those living in the least deprived ones (without considering any other confounding).
The number of patients who had received bisphosphonates was greater for the cases than for controls: 9.3% of cases were prescribed bisphosphonates, while 7.6% of patients in the control group had received a prescription. The unadjusted odds ratio (OR) for the bisphosphonate treatment was 1.27, indicating that patients taking bisphosphonates were 27% more likely to suffer stroke than patients with no treatment, without considering any confounding variables.
Alendronate, Ibandronate and Risedronate showed reduced risk (unadjusted OR 0.78, 0.66 and 0.84 respectively) of association with stroke, and fracture types were not statistically significant for the unadjusted analysis. Most patients with lower CCI index took Alendronate followed by Risedronate and Ibandronate, (Fig. 1). Alendronate remained the preferred bisphosphonate of choice even as CCI index increased, showing the highest prescription number for the first CCI index.
Adjusted analysis
Table 5 shows the results of the adjusted analysis, where we included all the variables in the same regression to adjust for other confounders. The adjusted OR for the bisphosphonate treatment was 0.86 (95% CI 0.62–1.19) indicating the absence of a relationship between the drug and stroke, once all other confounding variables had been taken into account.
Among the disease risk groups, hemiplegia, atrial fibrillation and peripheral arterial disease were the variables with the highest effect on the risk of having stroke (OR 4.59, 1.98 and 1.48, respectively). Some of the disease risk groups included in the analysis, such as hyperlipidaemia, diabetes, chronic renal disease, chronic obstructive pulmonary disease (COPD), mild liver disease, peptic ulcer and rheumatological disease, showed a non-significant effect on the risk of stroke, when they were considered in the adjusted analysis.
Alcoholism (OR 1.43, 95% CI 1.30–1.57) and most deprived IMD (OR 1.27, 95% CI 1.18–1.37) were the risk factors showing the highest association with risk of stroke. Being a safe drinker was associated with a lower risk of stroke (OR 0.84, 95% CI 0.80–0.88) compared with someone who had never drank alcohol, as were those on warfarin (OR 0.40, 95% CI 0.37–0.59).
The treatment associated with the highest risk of stroke was aspirin (OR 1.44, 95% CI 1.38–1.50), whereas antihypertensive treatment was associated with a reduced risk of stroke (OR 0.92). Finally, looking at IMD score, we found that patients living in the most deprived areas were more likely to suffer stroke compared with those living in the least deprived areas, as previously shown in the unadjusted analysis. The CCI showed a lower gradient than for the unadjusted analysis but still showed slight increase in odds ratio as number of comorbidities increased.
Analysis performed using R package survival [21]
Discussion
Main findings
We found no association between bisphosphonate treatment and risk of stroke, after adjusting for age, sex, ethnicity, index of multiple deprivation, Charlson index, fracture status, clinical and treatment variables.
Strengths and limitations
The limitations of the case-control approach include confounding and residual unmeasured confounding. The large validated database we used enabled us to adjust for important confounders including clinical risk groups, cardiovascular risk factors and differences in treatment between cases and controls. We also adjusted for additional comorbidities using the Charlson Index. Although great care was taken to ensure all stroke/TIAs were correctly coded, around 20% of all stroke patients’ are those who have temporary symptoms of TIA episodes [22]. These are difficult to diagnose as they depend on patient history. Because the duration of the episode is short, patients’ symptoms are likely to have resolved by the time of assessment, and the absence of an established biomarker makes the diagnosis difficult. Information about physical activity and diet were not available, and these factors may be a source of residual confounding.
Comparison with previous studies
The previous contradictory evidence linking bisphosphonates and stroke provided the rationale for this study. Although bisphosphonates have been associated with atrial fibrillation, presumed to be an idiosyncratic adverse effect which can sometimes lead to an embolic stroke due to thrombus generated in the abnormally contracting atrium blocking a narrowed carotid artery, there was no association with stroke in these studies [12, 13].
Other studies have suggested that bisphosphonates may prevent cardiovascular disease including stroke and myocardial infection mediated through a reduction in vascular calcification or reduced atherosclerosis through a number of mechanisms [23]. Vestergaard and colleagues, in a large cohort study in Denmark, found a reduction in overall risk of cardiovascular events but an increase in fatal strokes, but the variability in effect for different drugs and the differences in risk observed were small. [9]
One study showed no association between prior bisphosphonate therapy and 30-day mortality from stroke. [24] The most recently published meta-analysis, from Kim and colleagues, concluded that ‘bisphosphonates do not have beneficial or harmful effects on atherosclerotic cardiovascular events, but zoledronic acid may modestly increase the risk of atrial fibrillation’. [15]
Bisphosphonate compliance
There is a question about those patients who are possibly at a higher risk may have been less likely to take the bisphosphonates, (Fig. 1). Generally, there is a problem with compliance as Park and colleagues have shown that compliance and persistence with oral bisphosphates in patients with rheumatoid arthritis were suboptimal in real practice, thereby limiting the efficacy of osteoporosis treatment [25]. This may be true for our study as well.
Implications for policy, practice and research
This study suggests that bisphosphonate as a group of drugs are not associated with increased risk of stroke. This and evidence of effectiveness for prevention of osteoporosis supports their use first-line for prevention of osteoporosis in those deemed to be at high risk [2]. Clinicians will continue to use these drugs but greater consideration is being given to the time to stop [26] because of a lack of benefit beyond this time. There is limited evidence that bisphosphonates can cause painful, hard-to-treat osteonecrosis damage to the jaw bone, as well as very rare fractures of the mid-femur, further research is needed in these areas to shed more light. Our study finds no evidence for excess ONJ fracture due to bisphosphonates; however, there were noticeably more hip and other fractures present in the cases. Finally, we recommend further research to incorporate other confounders, to conduct studies which overcome unknown or unmeasured confounders for example using self-controlled case series designs.
Conclusion
We found no association between bisphosphonate treatment and risk of stroke, after adjusting for other confounders. Bisphosphonates are considered first-line for prevention of osteoporosis and fragility fractures, and this study supports their safety in people at risk of stroke.
References
Quan H, Li B, Couris CM, Fushimi K, Graham P, Hider P, Januel JM, Sundararajan V (2011) Updating and validating the Charlson comorbidity index and score for risk adjustment in hospital discharge abstracts using data from 6 countries. Am J Epidemiol 173(6):676–682
NICE (2017) Bisphosphonates for treating osteoporosis. National Institute for Health and Clinical Excellence, London
NICE (2012) Osteoporosis: Assessing the risk of fragility fracture. National Institute for Health and Clinical Excellence, London
Qaseem A, Forciea MA, McLean RM, Denberg TD, for the Clinical Guidelines Committee of the American College of Physicians (2017) Treatment of low bone density or osteoporosis to prevent fractures in men and women: a clinical practice guideline update from the American College of Physicians. Ann Intern Med 166(11):818–839
Reid IR, Bolland MJ, Grey A (2014) Effects of vitamin D supplements on bone mineral density: a systematic review and meta-analysis. Lancet 383(9912):146–155
Kahwati LC, Weber RP, Pan H, Gourlay M, LeBlanc E, Coker-Schwimmer M, Viswanathan M (2018) Vitamin D, calcium, or combined supplementation for the primary prevention of fractures in community-dwelling adults: evidence report and systematic review for the US preventive services task force. JAMA 319(15):1600–1612
Chung M, Tang AM, Fu Z, Wang DD, Newberry SJ (2016) Calcium intake and cardiovascular disease risk: an updated systematic review and meta-analysis. Ann Intern Med 165(12):856–866
Ford JA et al (2014) Cardiovascular disease and vitamin D supplementation: trial analysis, systematic review, and meta-analysis. Am J Clin Nutr 100(3):746–755
Vestergaard P, Schwartz K, Pinholt EM, Rejnmark L, Mosekilde L (2011) Stroke in relation to use of raloxifene and other drugs against osteoporosis. Osteoporos Int 22(4):1037–1045
Christensen S, Mehnert F, Chapurlat RD, Baron JA, Sørensen HT (2011) Oral bisphosphonates and risk of ischemic stroke: a case-control study. Osteoporos Int 22(6):1773–1779
Kang JH, Keller JJ, Lin HC (2012) A population-based 2-year follow-up study on the relationship between bisphosphonates and the risk of stroke. Osteoporos Int 23(10):2551–2557
Sharma A, Einstein AJ, Vallakati A, Arbab-Zadeh A, Walker MD, Mukherjee D, Homel P, Borer JS, Lichstein E (2014) Risk of atrial fibrillation with use of oral and intravenous bisphosphonates. Am J Cardiol 113(11):1815–1821
Sharma A, Chatterjee S, Arbab-Zadeh A, Goyal S, Lichstein E, Ghosh J, Aikat S (2013) Risk of serious atrial fibrillation and stroke with use of bisphosphonates: evidence from a meta-analysis. Chest 144(4):1311–1322
Kranenburg G, Bartstra JW, Weijmans M, de Jong PA, Mali WP, Verhaar HJ, Visseren FLJ, Spiering W (2016) Bisphosphonates for cardiovascular risk reduction: a systematic review and meta-analysis. Atherosclerosis 252:106–115
Kim DH, Rogers JR, Fulchino LA, Kim CA, Solomon DH, Kim SC (2015) Bisphosphonates and risk of cardiovascular events: a meta-analysis. PLoS One 10(4):e0122646
Correa A, Hinton W, McGovern A, van Vlymen J, Yonova I, Jones S, de Lusignan S (2016) Royal College of General Practitioners Research and Surveillance Centre (RCGP RSC) sentinel network: a cohort profile. BMJ Open 6(4):e011092
de Lusignan S, Correa A, Pathirannehelage S, Byford R, Yonova I, Elliot AJ, Lamagni T, Amirthalingam G, Pebody R, Smith G, Jones S, Rafi I (2017) RCGP Research and Surveillance Centre annual report 2014-2015: disparities in presentations to primary care. Br J Gen Pract 67(654):e29–e40
Hinton W, McGovern A, Coyle R, Han TS, Sharma P, Correa A, Ferreira F, de Lusignan S (2018) Incidence and prevalence of cardiovascular disease in English primary care: a cross-sectional and follow-up study of the Royal College of General Practitioners (RCGP) Research and Surveillance Centre (RSC). BMJ Open 8(8):e020282
Knol MJ, Vandenbroucke JP, Scott P, Egger M (2008) What do case-control studies estimate? Survey of methods and assumptions in published case-control research. Am J Epidemiol 168(9):1073–1081
Team, R (2018) RStudio: Integrated development for R. RStudio, B. Inc., MA URL, ed
T, T (2015) A Package for Survival Analysis in S_ version 2:38
Fitzpatrick T et al How do neurologists diagnose transient ischemic attack: a systematic review. Int J Stroke. https://doi.org/10.1177/1747493018816430
Caffarelli C, Montagnani A, Nuti R, Gonnelli S (2017) Bisphosphonates, atherosclerosis and vascular calcification: update and systematic review of clinical studies. Clin Interv Aging 12:1819–1828
Christensen DH, Horváth-Puhó E, Schmidt M, Christiansen CF, Pedersen L, Langdahl BL, Thomsen RW (2015) The impact of preadmission oral bisphosphonate use on 30-day mortality following stroke: a population-based cohort study of 100,043 patients. Clin Epidemiol 7:381–389
Park J-H et al (2017) Compliance and persistence with oral bisphosphonates for the treatment of osteoporosis in female patients with rheumatoid arthritis. BMC Musculoskelet Disord 18(1):152
Paskins Z, Warburton L (2016) Bisphosphonates beyond five years. BMJ 352:i264
Funding
The authors declare no competing financial interests.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Asghar, Z., Godoy Caballero, A., Pathirannehelage, S. et al. Saving bones without risking brain—bisphosphonates and risk of stroke: matched case-control study. Osteoporos Int 30, 1845–1854 (2019). https://doi.org/10.1007/s00198-019-05045-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-05045-z